Abstract
Objective
The objective of this study is to determine placental transfusion blood volumes with intact and cut umbilical cord milking in term newborns.
Study design
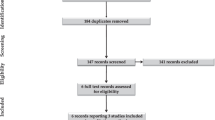
Sixty women at ≥37 weeks’ gestation were enrolled. Following delivery, the umbilical cord was immediately clamped and cut to separate the newborn. Either intact umbilical cord milking (I-UCM) of the placental–umbilical cord unit or cut umbilical cord milking (C-UCM) of the cut umbilical cord segment was performed. For I-UCM, the cord underwent milking three or four times while being attached to placental circulation. For C-UCM, a 10, 20, or 30 cm cord segment was cut separately and milked four times. Blood volumes were compared between I-UCM and C-UCM methods.
Results
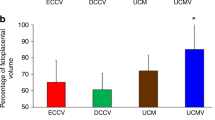
Mean blood volume with I-UCM (×4) was increased compared to the 30 cm C-UCM technique (48.5 ± 19.0 vs. 24.8 ± 4.0 mL, P < 0.001). For C-UCM, blood volume increased proportionally to cord length and, by the second milking, 98.1 ± 4.5% of blood volume was delivered.
Conclusion
I-UCM provides a greater blood volume than C-UCM. With C-UCM, milking the cord more than twice offers no additional advantage.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
McDonald SJ, Middleton P, Dowswell T, Morris PS. Effect of timing of umbilical cord clamping of term infants on maternal and neonatal outcomes. Cochrane Database Syst Rev. 2013;7:CD004074.
Raju TN. Timing of umbilical cord clamping after birth for optimizing placental transfusion. Curr Opin Pediatr. 2013;25:180–87.
Rabe H, Diaz-Rossello JL, Duley L, Dowswell T. Effect of timing of umbilical cord clamping and other strategies to influence placental transfusion at preterm birth on maternal and infant outcomes. Cochrane Database Syst Rev. 2012;8:CD003248.
WHO Guidelines Approved by the Guidelines Review Committee. Guideline: delayed umbilical cord clamping for improved maternal and infant health and nutrition outcomes. Geneva: World Health Organization; 2014.
Weiner G. Textbook of neonatal resuscitation. 7th ed. Elk Grove Village, Il: American Academy of Pediatrics; 2016.
Wyllie J, Perlman JM, Kattwinkel J, Wyckoff MH, Aziz K, Guinsburg R, et al. Part 7: neonatal resuscitation: 2015 international consensus on cardiopulmonary resuscitation and emergency cardiovascular care science with treatment recommendations. Resuscitation. 2015;95:e169–201.
Committee Opinion No. 684. Delayed umbilical cord clamping after birth. Obstet Gynecol. 2017;129:e5–10.
Al-Wassia H, Shah PS. Efficacy and safety of umbilical cord milking at birth: a systematic review and meta-analysis. JAMA Pediatr. 2015;169:18–25.
Dang D, Zhang C, Shi S, Mu X, Lv X, Wu H. Umbilical cord milking reduces need for red cell transfusions and improves neonatal adaptation in preterm infants: meta-analysis. J Obstet Gynaecol Res. 2015;41:890–95.
Patel S, Clark EA, Rodriguez CE, Metz TD, Abbaszadeh M, Yoder BA. Effect of umbilical cord milking on morbidity and survival in extremely low gestational age neonates. Am J Obstetr Gynecol. 2014;211:519 e511–17.
Katheria AC, Truong G, Cousins L, Oshiro B, Finer NN. Umbilical cord milking versus delayed cord clamping in preterm infants. Pediatrics. 2015;136:61–9.
Katheria A, Blank D, Rich W, Finer N. Umbilical cord milking improves transition in premature infants at birth. PLoS ONE. 2014;9:e94085.
Rabe H, Sawyer A, Amess P, Ayers S. Brighton perinatal study G. neurodevelopmental outcomes at 2 and 3.5 years for very preterm babies enrolled in a randomized trial of milking the umbilical cord versus delayed cord clamping. Neonatology. 2016;109:113–19.
March MI, Hacker MR, Parson AW, Modest AM, de Veciana M. The effects of umbilical cord milking in extremely preterm infants: a randomized controlled trial. J Perinatol. 2013;33:763–67.
Sweet DG, Carnielli V, Greisen G, Hallman M, Ozek E, Plavka R, et al. European consensus guidelines on the management of respiratory distress syndrome - 2016 update. Neonatology. 2017;111:107–25.
Yadav AK, Upadhyay A, Gothwal S, Dubey K, Mandal U, Yadav CP. Comparison of three types of intervention to enhance placental redistribution in term newborns: randomized control trial. J Perinatol. 2015;35:720–24.
Bora R, Akhtar SS, Venkatasubramaniam A, Wolfson J, Rao R. Effect of 40-cm segment umbilical cord milking on hemoglobin and serum ferritin at 6 months of age in full-term infants of anemic and non-anemic mothers. J Perinatol. 2015;35:832–36.
Hosono S, Mugishima H, Takahashi S, Takahashi S, Masaoka N, Yamamoto T, et al. One-time umbilical cord milking after cord cutting has same effectiveness as multiple-time umbilical cord milking in infants born at <29 weeks of gestation: a retrospective study. J Perinatol. 2015;35:590–94.
Kumar B, Upadhyay A, Gothwal S, Jaiswal V, Joshi P, Dubey K. Umbilical cord milking and hematological parameters in moderate to late preterm neonates: a randomized controlled trial. Indian Pediatr. 2015;52:753–57.
Jaiswal P, Upadhyay A, Gothwal S, Chaudhary H, Tandon A. Comparison of umbilical cord milking and delayed cord clamping on cerebral blood flow in term neonates. Indian J Pediatr. 2015;82:890–95.
Rabe H, Jewison A, Alvarez RF, Crook D, Stilton D, Bradley R, et al. Milking compared with delayed cord clamping to increase placental transfusion in preterm neonates: a randomized controlled trial. Obstet Gynecol. 2011;117(2 Pt 1):205–11.
Katheria AC, Lakshminrusimha S, Rabe H, McAdams R, Mercer JS. Placental transfusion: a review. J Perinatol. 2017;37:105–11.
Fanaroff and Martin's Neonatal-Perinatal Medicine. Diseases of the fetus and infant. 10th ed. Philadelphia, PA: Saunders; 2015.
Hosono S, Hine K, Nagano N, Taguchi Y, Yoshikawa K, Okada T, et al. Residual blood volume in the umbilical cord of extremely premature infants. Pediatr Int. 2015;57:68–71.
Hooper SB, Binder-Heschl C, Polglase GR, Gill AW, Kluckow M, Wallace EM, et al. The timing of umbilical cord clamping at birth: physiological considerations. Matern Health Neonatol Perinatol. 2016;2:4.
Acknowledgements
We gratefully acknowledge the technical assistance of Jan Hamanishi in preparing the figures and the statistical advice provided by Jens Eickhoff. There were no sources of funding for this project. Data from this study were presented as a poster at the ACOG Annual Clinical and Scientific Meeting in San Diego, CA, in May 2017 and the Pediatric Academic Society Meeting in San Francisco, CA, in May 2017.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interest
The authors declare that they have no competing financial interest.
Rights and permissions
About this article
Cite this article
McAdams, R.M., Fay, E. & Delaney, S. Whole blood volumes associated with milking intact and cut umbilical cords in term newborns. J Perinatol 38, 245–250 (2018). https://doi.org/10.1038/s41372-017-0002-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-017-0002-x
This article is cited by
-
Cut umbilical cord milking (C-UCM) as a mode of placental transfusion in non-vigorous preterm neonates: a randomized controlled trial
European Journal of Pediatrics (2023)
-
What does the evidence tell us? Revisiting optimal cord management at the time of birth
European Journal of Pediatrics (2022)
-
The effect of placental transfusion on hemodynamics in premature newborns: a randomized controlled trial
European Journal of Pediatrics (2022)
-
Umbilical cord milking versus delayed cord clamping in term infants: a systematic review and meta-analysis
Journal of Perinatology (2021)
-
Effects of blood sampling stewardship and erythropoietin administration in extremely low birth weight infants—a quality improvement non-controlled before-and-after retrospective study
European Journal of Pediatrics (2021)