Abstract
Intrauterine growth restricted (IUGR) infants have increased susceptibility to infection associated with higher risk of illness and death. Dual specificity phosphatase 1 (DUSP1), which is transcribed in the thymus, increases in quantity as T cells mature and differentiate into CD4+ cells. Little is known about how IUGR affects DUSP1 levels and T-cell subpopulations over time. We hypothesized that IUGR would decrease cell count, CD4+ and CD8+ subpopulations of T lymphocytes, and DUSP1 levels in IUGR rat thymus and spleen. Bilateral uterine artery ligation produced IUGR rats. Thymus and spleen were harvested at P0 and P21. Flow cytometry was used to compare CD4+ and CD8+ lymphocyte populations. Real-time RT-PCR and Western blotting were used to determine DUSP1 quantity. IUGR significantly decreased total cell count in P0 and P21 IUGR male and female thymus. IUGR significantly increased CD4+ cells in IUGR P0 males and females, significantly decreased CD4+ cells in P21 female thymus, and significantly altered DUSP1 levels in the IUGR female thymus at P0 and P21, although it is not yet known whether the change in DUSP1 levels is due to a change in the level per cell or to a change in cellular composition of the thymus.
Similar content being viewed by others
Main
Intrauterine growth restriction (IUGR) refers to the failure of a fetus to reach its genetic growth potential. In humans and rats, IUGR leads to multiple postnatal morbidities, including defects in immune function. The leading cause of IUGR in developed countries is uteroplacental insufficiency (UPI) (1). The association between IUGR and defective immune function is an important public health issue because UPI affects 5–9% of all pregnancies (2,3).
Humans studies examining IUGR and/or LBW infants at term demonstrate persistent immunological impairment throughout childhood. This is associated with higher risk of illness and death due to increased susceptibility to infections (4–6). Full-term IUGR infants have a 7-fold higher mortality rate and a 4-fold higher hospitalization rate than their appropriate for GA counterparts (7). This increased mortality and morbidity is primarily because of diarrheal illness and respiratory tract infections occurring from the neonatal period through adulthood (8). In addition, there is evidence of long-term deficiencies in adaptive immune competence in IUGR infants from developing countries (9,10).
The thymus plays a crucial role in adaptive immunity and the development, proliferation, and differentiation of mature T cells, with thymic size being a predictor of immune function (11,12). CD4+ cells are cytokine-producing helper cells that function in host defense against extracellular microbes. CD8+ cells are cytotoxic cells whose major function is to recognize and kill host cells infected with intracellular microbes (13). Human studies examining cellular immunity in IUGR infants have shown a decrease in peripheral T lymphocytes (14) and decreases in CD4+ and CD8+ T-lymphocyte subpopulations (15).
One regulator of CD4+ and CD8+ differentiation, and of the proinflammatory response, is dual specificity phosphatase 1 (DUSP1). DUSPs can regulate mitogen-activated protein kinases (MAPKs) by dephosphorylation of tyrosine and threonine residues (16). DUSP1, which is expressed in most tissues, is expressed at significantly higher levels in the murine thymus than the other members of the DUSP family. The transcription of DUSP1 increases thymocyte transition from an immature CD4+CD8+ double-positive stage to the mature CD4+ single positive stage (17). In addition to its role in thymocyte differentiation, DUSP1 serves as a feedback control regulator of proinflammatory cytokine production including TNFα, IL-1β, and the anti-inflammatory cytokine IL-10 (18). DUSP1 is expressed in the spleen, and mRNA levels are increased after lipopolysaccharide (LPS) challenge in splenocytes. Furthermore, a knockout of DUSP1 (Mkp−/−) sensitizes mice to endotoxic shock induced by LPS (19). This dual role of DUSP1 in both thymocyte differentiation and control of the inflammatory response makes it a likely player in the immune dysfunction seen in IUGR. Despite the widespread nature of this problem, little is known about how IUGR affects DUSP1 levels and the CD4+ and CD8+ subpopulations over time.
In light of the connection between IUGR and immune dysfunction, in these preliminary experiments, we hypothesized that UPI-induced IUGR would 1) decrease thymus and spleen organ weight and cell count, 2) decrease the CD4+ and CD8+ T-lymphocyte subpopulations in the thymus and subsequently the spleen (used as a proxy for peripheral CD4+ and CD8+ population), 3) decrease whole thymic levels of DUSP1, and 4) decrease in levels of whole spleen DUSP1 leading to an increase in the cytokines TNFα, IL-1β, and IL-10 after LPS challenge. We used a well-characterized rat model of IUGR to test this hypothesis (20,21). We examined the effect of IUGR on the rat at birth (P0) and at a prepubescent age (P21). We measured thymus weight and nucleated cell count at P0 and P21 and spleen weight and nucleated cell count at P21. We also measured proportional changes in the T-lymphocyte subpopulations of CD4+ and CD8+ cells. We examined DUSP1 mRNA and protein levels in P0 and P21 thymus and P21 spleen. Finally, we examined change in mRNA levels of TNFα, IL-1β, and IL-10 in isolated splenocytes after LPS stimulation at P21.
METHODS
Animals.
IUGR was induced by bilateral uterine artery ligation of pregnant Sprague-Dawley rats as previously described (20,21). All procedures were approved by the University of Utah Animal Care Committee and are in accordance with the American Physiological Society's Guiding Principles (22). In brief, on d 19.5 of gestation, pregnant dams were anesthetized and both inferior uterine arteries ligated. Control dams underwent identical anesthetic procedures.
At term gestation (21.5 d), P0 pups were delivered by cesarean section, weighed, and decapitated. To generate juvenile pups, dams were allowed to deliver spontaneously, litters were randomly culled to six pups, and the dams raised the pups. At P21, pups were anesthetized and killed. For both time points, tissue was harvested and frozen or used immediately for flow cytometry or cytokine stimulation studies. For each experiment, each group (control and IUGR) had six male pups and six female pups, unless otherwise noted. Pups within each group were derived from different litters.
Real-time RT-PCR.
Thymus and spleen mRNA levels of DUSP1 were measured on P0 and P21 as previously described (21). P0 samples were pooled to provide sufficient RNA for analysis. The following Assay-on-Demand primer/probes assays were used: DUSP1, Rn00678341_g1; TNFα, Rn99999017_m1; IL-1β, Rn00580432_m1; and IL-10, Rn99999012_m1 (Applied Biosystems). The sequences for GAPDH were forward: 5-CAAGATGGTGAAG-GTCGGTGT-3; reverse: 5-CAAGAGAAGGCAGCCCTGGT-3; and probe: 5-GCGTCCGATACGGCCAAATCCG-3.
Immunoblotting.
Immunoblotting was performed as previously described (21) using the following antibodies: anti-DUSP1 (Abcam, Cambridge, MA) and anti-GAPDH (Abcam).
Total cell count.
Single-cell suspensions from a whole spleen (P21 only) and thymus (P0 and P21) were obtained by teasing the organ into RPMI 1640 medium and filtered using a 100-μm sterile nylon mesh (BD Biosciences, San Jose, CA). Lymphocyte-rich cells were further washed with medium to remove the traces of ammonium chloride, and the viability was assessed by trypan blue dye exclusion (data not shown). Cells were counted using a hemocytometer and then multiplied by volume of cell suspension. P0 spleen was not reliably harvested because of its small size. Cell numbers were divided by organ weight.
Immunostaining.
Two million cells per sample (both IUGR and control groups) were counted and characterized by flow cytometry (BD Biosciences) after staining with FITC-conjugated, phycoerythrin (PE), or peridinin chlorophyll protein complex (PerCP)-conjugated antibodies to cell surface markers CD4 and CD8 (PharMingen, San Diego, CA). The results were analyzed with Cell Quest software (BD Biosciences).
Splenocyte activation and cytokine production.
A single cell suspension of P21 spleen was obtained as described above and standardized to 5 × 106 cells/mL per well in RPMI media. Nucleated cells were then incubated with 100 ng/mL of LPS (Sigma Chemical Co.-Aldrich, St. Louis, MO). Cell pellets were collected at 0, 1, 3, and 6 h for both LPS and controls. mRNA quantification was performed as described above.
Statistics.
All data presented are expressed as mean ± SEM. ANOVA (Fisher's protected least significant difference) and the Student's unpaired t test determined statistical significance. We accepted p < 0.05 for statistical significance.
RESULTS
P0 and P21 pup weight and organ weight.
All data are presented as mean ± SEM. At P0, IUGR significantly decreased thymus weight in both females (0.006 ± 0.002 g versus 0.011 ± 0.002 g, p = 0.03) and males (0.007 ± 0.001 g versus 0.013 ± 0.002 g, p = 0.03). The P0 female and male IUGR thymuses were 46% smaller than the control thymuses. Thymus weight returned to control weight in both genders by P21 (Fig. 1a). The P21 IUGR spleen was significantly smaller than control in both females (0.27 ± 0.02 g versus 0.36 ± 0.02 g, p = 0.02) and males (0.28 ± 0.02 g versus 0.36 ± 0.02 g, p = 0.02). At P0, the IUGR females and males weighed significantly less than controls (2.81 ± 0.9 g versus 3.36 ± 0.22 g, p = 0.002; 3.1 ± 0.9 g versus 3.6 ± 0.54 g, p = 0.002). The P0 IUGR female and male pups were 19% and 14% smaller than control pups. At P21, the IUGR males continued to weigh significantly less than the male controls (57.5 ± 3.3 g versus 63.3 ± 1.0 g, p = 0.01; Fig. 1B).
The effect of IUGR on rat pup and organ weight. (A) IUGR significantly decreased thymus weight at P0 and spleen weight at P21 (B) IUGR significantly decreased pup weight at P0 and male pup weight at P21. Data are expressed as weight ± SEM (* indicates a p < 0.05). ▪, control female; □, IUGR female;  , control male;
, control male;  , IUGR male.
, IUGR male.
P0 and P21 organ cell count.
At P0, IUGR significantly decreased thymus cell count in females (3.6 ± 0.2 × 107 cells versus 7.5 ± 1.2 × 107 cells, p = 0.03) and males (7.0 ± 0.9 × 107 cells versus 12.6 ± 1.8 × 107 cells, p = 0.005). IUGR continued to significantly decrease thymus cell counts, compared with gender-matched controls, at P21 in both females (404 ± 30 × 107 cells versus 571 ± 43 × 107 cells, p = 0.008) and males (423 ± 37 × 107 cells versus 581 ± 37 × 107 cells, p = 0.01). IUGR also significantly decreased the cell count in the P21 spleen in females (11.3 ± 1.0 × 107 cells versus 15.5 ± 1.9 × 107 cells, p = 0.05) and males (7.8 ± 1.2 × 107 cells versus 14.9 ± 1.3 × 107 cells, p = 0.004; Fig. 2).
P0 thymus CD4+ and CD8+ cell populations.
IUGR significantly increased the percentage of CD4+ lymphocytes in the thymus, with females (3.1 ± 0.5% versus 1.2 ± 0.2%, p = 0.0003) more affected than males (2.6 ± 0.3% versus 1.5 ± 0.2%, p = 0.02). The resulting CD4+ to CD8+ ratio was similarly increased. There was a significant decrease in the immature CD4+CD8+ cells in IUGR females compared with gender-matched controls (80.6 ± 1.1% versus 84.8 ± 0.6% p = 0.004). There was no significant change in the immature CD4-CD8 double-negative cells when compared with controls (Fig. 3a). The total CD4+ cell count was similar to controls in IUGR males and females, with the total CD8+ cell count decreased when compared with controls. The total CD4+ to CD8+ ratio is increased in IUGR female and males when compared with controls (Table 1).
The effect of IUGR on T lymphocyte CD4+ and CD8+ cell percentages as measured by flow cytometry. (A) IUGR significantly increased the percentage of CD4+ lymphocytes and CD4+:CD8+ ratio in females and males at P0. (B) IUGR significantly decreased the percentage of CD4+ lymphocytes in P21 females. Data are expressed as a % ± SEM (* indicates a p < 0.05). ▪, control female; □, IUGR female;  , control male;
, control male;  , IUGR male.
, IUGR male.
P21 thymus CD4+ and CD8+ cell populations.
IUGR significantly decreased the percentage of CD4+ cells in the female thymus (4.5 ± 0.1% versus 6.3 ± 0.4%, p = 0.02) with no significant difference in males. There was also a significant increase in the female CD4+CD8+ cell population (91.7 ± 0.3% versus 88.4 ± 0.4%, p = 0.016) with no significant difference in the male. There was no significant change in the CD4-CD8- or the CD4+:CD8+ ratio in males or females (Fig. 3B). The total CD8+ cell count was similar to controls in IUGR males, with all other cell populations decreased when compared with controls in IUGR males and females (Table 1).
P0 spleen CD4+ and CD8+ cell populations.
IUGR did not significantly change the CD4+ or CD8+ cell populations. However, in the rodent, as opposed to the human, the thymus has not yet populated the spleen at P0, and <6% of all splenocytes were CD4+ or CD8+ (Fig. 4A).
The effect of IUGR on T lymphocyte CD4+ and CD8+ cell percentages as measured by flow cytometry. (A) IUGR had no significant effect on the P0 CD4+ and CD8+ lymphocytes in either males or females (B). At P21, IUGR significantly increased the percentage of CD4+ lymphocytes. Data are expressed as ± SEM (* indicates a p < 0.05). ▪, control female; □, IUGR female;  , control male;
, control male;  , IUGR male.
, IUGR male.
P21 spleen CD4+ and CD8+ cell populations.
IUGR significantly increased P21 CD4+ cell percentage in the spleen of both females (14.61 ± 0.9% versus 12.3 ± 0.3%, p = 0.03) and males (15.7 ± 0.6% versus 12.9 ± 0.6%, p = 0.01). IUGR did not affect the CD8+ cell subpopulation percentage in the spleen at this time point (Fig. 4B). The total CD4+ cell count was similar to controls in IUGR males and females, with the CD8+ populations decreased when compared with controls in both IUGR males and females (Table 1).
P0 and P21 thymus DUSP1 mRNA and protein levels.
IUGR significantly increased DUSP1 mRNA levels (0.006 ± 0.0004 versus 0.004 ± 0.0002, p = 0.0008) in the P0 female thymus. However, IUGR did not affect mRNA levels of DUSP1 in P21 male or female thymus (Fig. 5A). At P0, IUGR significantly increased DUSP1 protein levels in the female thymus (1.2 ± 0.05 versus 0.24 ± 0.04, p = 0.045) and decreased DUSP1 protein levels in the P21 female thymus (2.1 ± 0.2 versus 3.1 ± 0.6, p = 0.0375) with no significant difference in the P21 male (Fig. 5B).
The effect of IUGR on DUSP1 mRNA and protein in the rat thymus. (A) IUGR significantly increased DUSP1 mRNA in the P0 female. (B) IUGR significantly increased DUSP1 protein levels in the P0 female and decreased DUSP1 protein levels in the P21 female. Data are expressed as relative met intensity ± SEM (* indicates a p < 0.05). ▪, control female; □, IUGR female;  , control male;
, control male;  , IUGR male.
, IUGR male.
P21 spleen DUSP1 mRNA and protein levels.
IUGR did not significantly affect mRNA of DUSP1 in male or female spleen (Fig. 6A). However, IUGR significantly decreased DUSP1 protein levels in the female (1.7 ± 0.2 versus 2.5 ± 0.1, p = 0.0093; Fig. 6B).
The effect of IUGR on DUSP1 mRNA and protein in the rat thymus and spleen. (A) There were no significant differences mRNA levels at P21. (B) IUGR significantly decreased DUSP1 protein levels in the P21 female rat spleen. Data are expressed as relative met intensity ± SEM (* indicates a p < 0.05). ▪, control female; □, IUGR female;  , control male;
, control male;  , IUGR male.
, IUGR male.
P21 spleen cytokine analysis.
After 100 ng/mL LPS stimulation, there was a significant increase in stimulation curve of IL-1β mRNA at 1 and 3 h poststimulation in the IUGR female. In the IUGR male, there were significant changes in mRNA levels at 1 and 6 h, but not at the peak time point of 3 h (Fig. 7A and B). There were no significant differences in peak mRNA levels of TNFα or IL-10 (data not shown).
The effect of IUGR on cytokine production. (A) IUGR significantly increased the peak IL-1β mRNA levels in the female prepubescent rat spleen after stimulation with 100 ng/mL of LPS. (B) IUGR significantly increased IL-1β mRNA at the 1- and 3-h time points in the male prepubescent rat spleen. Data are expressed as 2−ΔCT ± SEM (* indicates a p < 0.05). ▪, control female; ♦, IUGR female; ▴, control male; •, IUGR male.
DISCUSSION
We demonstrated four novel and significant findings in our rat model of IUGR. First, IUGR decreased thymus cell count both at birth and in the juvenile period. This change in thymic cell populations was further demonstrated by the decreased nucleated cell population of the spleen, which also persisted into the juvenile period. Second, IUGR altered the population percentage of CD4+ in the female thymus at birth and in the juvenile, again leading to changes in the splenic population in the juvenile period. Third, IUGR altered levels of DUSP1 in females at P0 and P21 thymus and in the female P21 spleen were consistent with the changes seen in the CD4+ populations. Finally, IUGR increased the IL-1β mRNA stimulation curve in LPS challenged juvenile spleen in both male and females, with a significant difference in peak levels in the IUGR female. To our knowledge, this is the first time persistent changes in the immune system have been demonstrated in an animal model of UPI-induced IUGR. These findings may explain some of the immune dysregulation seen in IUGR.
Our finding of decreased cell count and organ weight in our IUGR model is consistent with studies in IUGR humans at birth of decreased thymus size (11,12) and decreased total white blood cell count (14). The thymus size in the P0 IUGR pups was decreased to a greater extent than the decrease in IUGR pup weight, demonstrating that the thymus was preferentially affected by UPI. The potential impact of UPI on thymus weight and cell count makes sense based on both human and rodent embryology, because many of the principal components of the immune system develop early in fetal life. In humans, by 15–16 wk the architecture of the fetal thymus resembles that of the neonate (23). In the rodent thymus, the first T-cell precursors colonize the thymus by d 13–14 of a 21.5-d gestation (24). Therefore, T-cell precursors in the thymus are present and susceptible to a late gestational insult, making it a potential target for prenatal stress-induced changes.
The persistent decrease in organ size and cell count we observed through d 21 may partially explain the increased susceptibility to infections seen in previous studies. The decreased overall cell count, and therefore decreased population of CD4+ and CD8+ cells, leaves the rat pup in a relatively immunocompromised state when compared with controls. Given that the cell populations return to control percentages at P21, the decrease in cell count is likely a result of increased apoptosis or cell death across all cell populations. However, the decreased percentage of CD4+ lymphocytes in P21 female thymus may be compensated by an increase in CD4+ lymphocytes in P21 spleen, therefore preserving immune function. This overall decrease in lymphocytes lasts from birth to the juvenile age in our model.
Although several rodent models have recently looked at the effects of maternal psychosocial stress on the immune system of the offspring, none of these models looked at the effect of UPI-induced IUGR. These models include repeated stimulation of maternal rats to confrontation (25), acute immobilization (26), bright light (27,28), and loud noise (29,30). These studies have shown a decrease in total peripheral leukocyte count (26,31) and decreases in the peripheral CD4+ and CD8+ T-cell subsets in older rats (31). Other studies showed only a decrease in the CD8+ subsets (26) or a gender difference in splenocyte response to mitogens, but no difference in the T-lymphocyte subsets (30). Prenatal stress is also associated with an altered response to stimulation with LPS (28) or the potent mitogen concanavalin A (27,29). The wide spectrum of results seen in these studies is likely a function of the model variance in type, onset, and duration of stress. However, it also demonstrates the susceptibility of the immune system to in utero stressors.
We chose to examine a model of IUGR produced by surgical UPI and prenatal stress for a number of reasons. First, UPI is the most prevalent cause of IUGR in western society. Second, surgical UPI exposes the rat fetus to a late gestation, in utero hypoxic, hypoglycemic, and acidotic environment (20,32) similar to that experienced by the human infant exposed to placental dysfuntion (33,34). In this study, we demonstrated that changes in the immune system of IUGR rat pups are present at birth, after the stress of UPI. Importantly, we have also demonstrated that IUGR pups continue to have immune system alterations that persist at the prepubescent age.
We have shown that levels of DUSP1, a key regulator of several aspects of the immune system, are altered in IUGR thymus and spleen. An important consideration, however, is that alterations in whole organ DUSP1 levels could reflect only the altered cellular makeup of the thymus and spleen and not be a function of changes in DUSP1 expression in any one cell type. It will be important to determine DUSP1 expression in individual cell types in future studies. Similarly, examination of downstream targets, such as extracellular signal-regulated kinases (ERKs), in isolated cells will also be important to establish the functional consequences of IUGR on the immune system.
Some limitations of our study are important to consider. First, in this preliminary study, we have focused on T cells only. Numbers and proportions of the other splenocyte populations may also be altered by IUGR and warrant further investigation. Moreover, as mentioned above, we looked at whole organ extracts with differing cell populations, which may confound the differences we see in DUSP1 and IL-1β levels. In addition, caution is always necessary when attempting to apply data from a rat model to human pathophysiology. Of note, however, in this model of UPI where the fetal rat is exposed to a severe insult relatively late in gestation, the effects on the immune system are similar to those seen in human studies. The rat UPI-induced IUGR model will be an invaluable tool in future studies elucidating mechanisms involved in IUGR and immune dysfunction.
In summary, UPI and subsequent IUGR lead to decreased thymus and spleen size and lymphocyte counts, as well as alterations in CD4+ and CD8+ populations. We saw alterations in the CD4+ subpopulation of cells in our IUGR model. It is feasible that increased CD4+ percentages in P0 thymus and P21 spleen reflect an attempt in the IUGR rat to compensate for the decreased total lymphocyte counts to maintain a stable CD4+ count. Further studies will be needed to determine whether the changes seen in DUSP1 and IL-1β are a result of the heterogenous cell populations or occur as a result of IUGR stress.
Abbreviations
- DUSP1:
-
dual specificity phosphatase 1
- LPS:
-
lipopolysaccharide
- UPI:
-
uteroplacental insufficiency
References
Gortner L, Wauer RR, Stock GJ, Reiter HL, Reiss I, Jorch G, Hentschel R, Hieronimi G 1999 Neonatal outcome in small for gestational age infants: do they really better?. J Perinat Med 27: 484–489
Witlin AG, Sibai BM 1997 Hypertension in pregnancy: current concepts of preeclampsia. Annu Rev Med 48: 115–127
Zhang J, Zeisler J, Hatch MC, Berkowitz G 1997 Epidemiology of pregnancy-induced hypertension. Epidemiol Rev 19: 218–232
Chandra RK 1979 Nutritional deficiency and susceptibility to infection. Bull World Health Organ 57: 167–177
Victora CG, Smith PG, Vaughan JP, Nobre LC, Lombardi C, Teixeira AM, Fuchs SM, Moreira LB, Gigante LP, Barros FC 1988 Influence of birth weight on mortality from infectious diseases: a case-control study. Pediatrics 81: 807–811
Moore SE, Collinson AC, Tamba N′Gom P, Aspinall R, Prentice AM 2006 Early immunological development and mortality from infectious disease in later life. Proc Nutr Soc 65: 311–318
Lira PI, Ashworth A, Morris SS 1996 Low birth weight and morbidity from diarrhea and respiratory infection in northeast Brazil. J Pediatr 128: 497–504
Ashworth A 1998 Effects of intrauterine growth retardation on mortality and morbidity in infants and young children. Eur J Clin Nutr 52: S34–S41
McDade TW, Beck MA, Kuzawa C, Adair LS 2001 Prenatal undernutrition, postnatal environments, and antibody response to vaccination in adolescence. Am J Clin Nutr 74: 543–548
Moore SE, Jalil F, Ashraf R, Szu SC, Prentice AM, Hanson LA 2004 Birth weight predicts response to vaccination in adults born in an urban slum in Lahore, Pakistan. Am J Clin Nutr 80: 453–459
Cromi A, Ghezzi F, Raffaelli R, Bergamini V, Siesto G, Bolis P 2009 Ultrasonographic measurement of thymus size in IUGR fetuses: a marker of the fetal immunoendocrine response to malnutrition. Ultrasound Obstet Gynecol 33: 421–426
Hartge R, Jenkins DM, Kohler HG 1978 Low thymic weight in small-for-dates babies. Eur J Obstet Gynecol Reprod Biol 8: 153–155
Abbas AK, Lichtman AH, Pillai S 2007 Cellular and Molecular Immunology. Saunders Elsevier, Philadelphia, pp 114–118
Ferguson AC 1978 Prolonged impairment of cellular immunity in children with intrauterine growth retardation. J Pediatr 93: 52–56
Thilaganathan B, Plachouras N, Makrydimas G, Nicolaides KH 1993 Fetal immunodeficiency: a consequence of placental insufficiency. Br J Obstet Gynaecol 100: 1000–1004
Mustelin T, Alonso A, Bottini N, Huynh H, Rahmouni S, Nika K, Louis-dit-Sully C, Tautz L, Togo SH, Bruckner S, Mena-Duran AV, al-Khouri AM 2004 Protein tyrosine phosphatases in T cell physiology. Mol Immunol 41: 687–700
Tanzola MB, Kersh GJ 2006 The dual specificity phosphatase transcriptome of the murine thymus. Mol Immunol 43: 754–762
Liu Y, Shepherd EG, Nelin LD 2007 MAPK phosphatases—regulating the immune response. Nat Rev Immunol 7: 202–212
Hammer M, Mages J, Dietrich H, Servatius A, Howells N, Cato AC, Lang R 2006 Dual specificty phosphatase 1 (DUSP1) regulates a subset of LPS-induced genes and protects mice from lethal endotoxin shock. J Exp Med 203: 15–20
Ogata ES, Swanson SL, Collins JW, Finley SL 1990 Intrauterine growth retardation: altered hepatic energy and redox states in the fetal rat. Pediatr Res 27: 56–63
Baserga M, Hale MA, Ke X, Wang ZM, Yu X, Callaway CW, McKnight RA, Lane RH 2006 Uteroplacental insufficiency increases p53 phosphorylation without triggering the p53-MDM2 functional circuit response in the IUGR rat kidney. Am J Physiol Regul Integr Comp Physiol 291: R412–R418
World Medical Association American Physiological Society 2002 Guiding principles for research involving animals and human beings. Am J Physiol Regul Integr Comp Physiol 283: R281–R283
Klein J, Hořejší V 1997 Immunology. Blackwell Science, Oxford, pp 32–36
Vicente A, Varas A, Acedón RS, Jiménez E, Muñoz JJ, Zapata AG 1998 Appearance and maturation of T-cell subsets during rat thymus ontogeny. Dev Immunol 5: 319–331
Götz AA, Wittlinger S, Stefanski V 2007 Maternal social stress during pregnancy alters immune function and immune cell numbers in adult male Long-Evans rat offspring during stressful life-events. J Neuroimmunol 185: 95–102
Llorente E, Brito ML, Machado P, González MC 2002 Effect of prenatal stress on the hormonal response to acute and chronic stress and on immune parameters in the offspring. J Physiol Biochem 58: 143–149
Klein SL, Rager DR 1995 Prenatal stress alters immune function in the offspring of rats. Dev Psychobiol 28: 321–336
Hashimoto M, Watanabe T, Fujioka T, Tan N, Yamashita H, Nakamura S 2001 Modulating effects of prenatal stress on hyperthermia induced in adult rat offspring by restraint or LPS-induced stress. Physiol Behav 73: 125–132
Sobrian SK, Vaughn VT, Ashe WK, Markovic B, Djuric V, Jankovic BD 1997 Gestational exposure to loud noise alters the development and postnatal responsiveness of humoral and cellular components of the immune system in offspring. Environ Res 73: 227–241
Kay G, Tarcic N, Poltyrev T, Weinstock M 1998 Prenatal stress depresses immune function in rats. Physiol Behav 63: 397–402
Götz AA, Stefanski V 2007 Psychosocial maternal stress during pregnancy affects serum corticosterone, blood immune parameters and anxiety behaviour in adult male rat offspring. Physiol Behav 90: 108–115
Ogata ES, Bussey ME, LaBarbera A, Finley S 1985 Altered growth, hypoglycemia, hypoalaninemia, and ketonemia in the young rat: postnatal consequences of intrauterine growth retardation. Pediatr Res 19: 32–37
Economides DL, Nicolaides KH 1989 Blood glucose and oxygen tension levels in small-for-gestational-age fetuses. Am J Obstet Gynecol 160: 385–389
Nicolaides KH, Economides DL, Soothill PW 1989 Blood gases, pH, and lactate in appropriate- and small-for-gestational-age fetuses. Am J Obstet Gynecol 161: 996–1001
Author information
Authors and Affiliations
Corresponding author
Additional information
Supported by the Children's Health Research Center (CHRC).
Rights and permissions
About this article
Cite this article
Contreras, Y., Yu, X., Hale, M. et al. Intrauterine Growth Restriction Alters T-Lymphocyte Cell Number and Dual Specificity Phosphatase 1 Levels in the Thymus of Newborn and Juvenile Rats. Pediatr Res 70, 123–129 (2011). https://doi.org/10.1203/PDR.0b013e31821f6e75
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/PDR.0b013e31821f6e75
This article is cited by
-
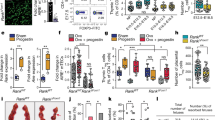
Dentate granule progenitor cell properties are rapidly altered soon after birth
Brain Structure and Function (2018)
-
Effects of intrauterine growth retardation and Bacillus subtilis PB6 supplementation on growth performance, intestinal development and immune function of piglets during the suckling period
European Journal of Nutrition (2017)
-
Increased Fetal Thymocytes Apoptosis Contributes to Prenatal Nicotine Exposure-induced Th1/Th2 Imbalance in Male Offspring Mice
Scientific Reports (2016)
-
Impairment of cellular immunity is associated with overexpression of heat shock protein 70 in neonatal pigs with intrauterine growth retardation
Cell Stress and Chaperones (2012)