Abstract
Fetal growth restriction (FGR) remains a cause of perinatal brain injury, sometimes leading to neurological and intellectual impairment. Although the mechanisms and pathophysiology of CNS injuries have not been elucidated completely, it is possible carbohydrate and energy metabolism may have an important role in the FGR brain. In this study, FGR was induced in rats by administration of synthetic thromboxane A2 (STA2). Pups were delivered by cesarean section. After killing, samples were obtained from the fetuses of both control and FGR rats for evaluation of carbohydrate and energy metabolism in brain tissue. Lactate and pyruvate levels in brain were reduced significantly in the FGR group. Glucose content in brain tissue tended to be increased in the FGR group. In contrast, glycogen content in brain tissue tended to be lower in the FGR group. However, these differences in glucose and glycogen content did not reach statistical significance. Brain high-energy reserves, including ATP, ADP, AMP, and phosphocreatine (P-Cr), were similar in the control and FGR groups. Gluconeogenesis compensated for chronic fetal hypoxia and decreased glycogen storage. Energy metabolism in the FGR brain is likely to be disrupted as a consequence of lower reserves of energy substrates.
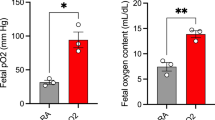
Similar content being viewed by others
Main
Fetal growth restriction (FGR) is an important cause of perinatal morbidity and mortality. Surviving small-for-GA (SGA) infants have a higher incidence of neurological impairments including mental retardation and educational and/or behavioral problems (1–3). Several authors have reported that perinatal hypoxic ischemic brain damage may contribute to an increased prevalence of motor, cognitive, and affective disabilities in children born with FGR (4–6). However, the mechanisms underlying these disabilities have not yet been fully elucidated.
Various prenatal factors may affect fetal growth. Pregnancy- induced hypertension (PIH) is an especially important factor in FGR fetuses. In PIH, increasing umbilical vessel resistance causes limitations in uteroplacental blood flow. As a consequence, the supply of oxygen and nutrition to the fetus may decrease (7). FGR fetuses are frequently hypoxic and hypoglycemic (8). During labor, uterine contractions can further compromise placental blood flow and oxygen supply to the FGR fetus, thereby increasing the risk of an intrapartum hypoxic-ischemic event and subsequent brain injury (9). Several authors have also reported that FGR fetuses are not only at great risk of perinatal hypoxic ischemic events but also may be more susceptible to hypoxic-ischemic brain damage, compared with appropriate-for-GA (AGA) fetuses (9,10).
Several studies have investigated the mechanisms of brain injuries in FGR model animals (11–13). Manipulations to induce FGR in animal models included surgical ligation of vessels supplying the uteroplacental unit (12) and maternal starvation (11). However, these models do not necessarily reflect the pathophysiology of FGR. It has been suggested that plasma levels of thromboxane, a potent vasoconstrictor, may exceed prostacycline levels in PIH, whereas in normal gestation, the opposite is true (14–16). This prostacycline-thromboxane imbalance may be of primary importance in the pathophysiology of uteroplacental vascular insufficiency and resultant fetal growth retardation. We have developed an FGR model induced by maternal administration of thromboxane A2 (17) and consider that this model may more closely resemble the pathophysiology of human FGR compared with other models generated by uterine artery ligation (18) or maternal undernutrition (19). Our FGR model exhibits not only physical growth restriction but also a significant delay in postnatal neurological development (20). The phenotype of our FGR model is therefore very similar to severe human FGR associated with severe PIH.
In general, FGR infants suffer from hypoglycemia. There is evidence that hypoglycemia affects psychomotor development in SGA infants (21). Changes in energy metabolism associated with adaptation of the FGR fetus to chronic hypoxia and hypoglycemia in utero may therefore be an important determinant of susceptibility to perinatal hypoxic ischemic brain injury in FGR neonates. Accordingly, it is important to clarify the alterations that occur in carbohydrate and energy metabolism in growth-retarded fetal brains. We hypothesize that the content of substrates in FGR brains is lower than in brains of AGA infants. However, we speculate the energy status in FGR is normal as the majority of FGR infants do not have neurological symptoms. In this study, we examined cerebral carbohydrate and energy metabolism and used our model of FGR to clarify the mechanism of brain damage in this condition.
MATERIALS AND METHODS
The protocol for this study was approved by the Ethical Committee of the Center for the Promotion of Medical Research and Education, Nagoya University Graduate School of Medicine.
Preparation of FGR rats.
Dated pregnant Sprague-Dawley rats were purchased from Chubu Kagaku Shizai, Nagoya, Japan, and osmotic pumps, Model 2Ml1 from Alza Corporation, Palo Alto, CA. Synthetic thromboxane A2 (STA2) analog was kindly gifted by Ono Pharmaceutical Company, Osaka, Japan. All reagents and enzymes used in the study were of the highest commercial grade available. The maternal rats were housed individually and fed ad libitum under controlled light cycle (12-h light and 12-h darkness) and temperature conditions. The FGR model rats were produced using our previously reported method (17). In brief, on the 13th day of pregnancy, an osmotic pump filled with STA2 was implanted into the peritoneal cavity under general anesthesia with pentobarbital. The mean delivery rate of STA2 was 20 ng/h. On the 20th day of gestation, the fetuses were delivered by cesarean section under ether anesthesia. The fetuses were stabilized for 1 h after birth and then weighed. To avoid hypothermia, the environmental temperature was regulated using a temperature-controlled bath. After decapitation, blood samples were collected for analysis of blood glucose levels. The whole brains were then removed and weighed, and saved for the experiments.
Six pregnant rats were divided into two groups, with three rats being administrated STA2 to induce FGR, whereas the remaining three animals had no intervention. None of the maternal rats died during pregnancy, and there was no intrauterine/neonatal death of the pups in the study. We were unable to obtain sufficient quantities of tissue from several pups. The lactate and pyruvate content was measured in whole brains of 10 FGR pups from a litter of 13 and also in 14 control pups from a litter of 14. Glucose and glycogen contents in whole brains were evaluated in 7 FGR rats from a litter of 10 and in 13 controls from a litter of 13, whereas energy status in whole brains was evaluated in 9 FGR rats from 1 litter of 12 and in 9 controls from a litter of 13. The total number of pups in the FGR and control groups were 26 and 36, respectively. A proportion of the experimental animals was used to measure plasma glucose levels (10 FGR rats and 13 controls).
Preparation of brain tissue.
For determination of lactate and pyruvate contents, the whole brains were removed and homogenized immediately in 2 mL of 0.6% perchloric acid using a Potter-Elvehjem glass homogenizer to achieve optimal preservation of the labile metabolites. The combined procedures of decapitation, brain removal, and homogenization were carried out within 13–15 s. The homogenate was centrifuged at 28,000 × g for 30 min and the resultant supernatant adjusted to pH 6.0 with 3 N potassium carbonate containing 0.5 M triethanolamine, followed by centrifugation at 28,000 × g for 30 min. The final supernatant was stored at −80°C until analyzed. To measure glucose and glycogen contents, the homogenate of the whole brain was added to 50 volumes of 0.03 N HCl and then heated for 10 min at 100°C in sealed tubes. The boiled suspension was used in the assays (22).
Whole brains were homogenized with 10 volumes of ice-cold 6% perchloric acid to evaluate ATP, ADP, AMP, and phosphocreatine (P-Cr) levels. Sampling of the brain tissue was carried out using the same methods as for pyruvate and lactate. After centrifugation of the homogenate at 10,000 × g for 10 min, 0.1 mL of 1 M dibasic potassium phosphate was added to 1 mL of the supernatant. The mixture was then neutralized with 3 N potassium hydroxide and centrifuged at 10,000 × g for 10 min. The supernatant was stored at −80°C until analysis.
Laboratory measurements.
Measurement of glucose and pyruvate contents in whole brains were essentially those described by Lowry and Passonneau (23), whereas lactate and glycogen contents were determined by the method of Vannucci and Duffy (22).
The fluorometric methods for ATP, ADP, AMP, and P-Cr were essentially those described by Lowry and Passonneau (23). Determination of adenine nucleotide concentrations allows estimation of the ATP/ADP ratio and adenylate charge ratio, (ATP + 1/2ADP)/(ATP + ADP + AMP). The former approximates energy availability, whereas the latter reflects the equilibrium between high-energy adenine nucleotides mediated by adenylate kinase (24). Plasma glucose was analyzed by the glucose oxidase method using an Ascensia Breeze2 Blood Glucose Meter (Bayer HealthCare, Japan).
Statistical analysis.
The results were expressed as median and range. The Mann-Whitney U test was used to evaluate the statistical significance of differences between the FGR and control groups. A p < 0.05 was considered statistically significant.
RESULTS
Evaluation of fetal growth.
The median body weights of pups in the FGR and control groups were 3.64 g (3.35–4.09 g) and 4.18 g (3.74–4.69 g), respectively. Fetuses with FGR were significantly smaller than those in the control group (p < 0.0001). The median brain weight in the FGR group was significantly lower than that in the control group [167 mg (144–186 mg) versus 180 mg (156–192 mg), p < 0.0001].
Evaluation of carbohydrate metabolism.
Carbohydrate substrates and metabolites in the whole brains are shown in Fig. 1. The median lactate content in the brains was significantly lower in the FGR group compared with the control group [0.69 μmol/g (0.34–1.67 μmol/g) versus 1.19 μmol/g (0.81–1.63 μmol/g), p = 0.017]. The median pyruvate content in the brains was also significantly lower in the FGR group than in controls [0.24 μmol/g (0.12–0.43 μmol/g) versus 0.31 μmol/g (0.26–0.43 μmol/g), p = 0.004]. Total glucose content tended to be higher in FGR rat brains [1.24 μmol/g (0.54–1.96 μmol/g) versus 0.58μmol/g (0.37–1.78 μmol/g), p = 0.081]. In contrast, total glycogen content in the brains tended to be lower in the FGR pups compared with controls [1.29 μmol/g (1.15–1.66 μmol/g) versus 1.53 μmol/g (1.11–1.85 μmol/g), p = 0.075]. These differences in glucose and glycogen contents in the whole brains were not statistically significant.
Comparison of carbohydrate substrates in whole brains of the control and FGR groups. (A) Lactate contents in control (n = 10) and FGR (n = 14) pups. (B) Pyruvate contents in control (n = 10) and FGR (n = 14) pups. (C) Glucose contents in control (n = 7) and FGR (n = 13) pups. (D) Glycogen contents in control (n = 7) and FGR (n = 13) pups. The horizontal bars within the boxes correspond to the median, the upper and lower bars of the boxes to the first and third quartiles, respectively, and the upper and lower whiskers to the 90th and 10th percentiles, respectively. The observations marked by an open circle were considered extreme outliers. *p < 0.01, **p < 0.05.
Median plasma glucose was significantly lower in FGR rats compared with controls [24.8 mg/dL (18.0–30.5 mg/dL) versus 43.8 mg/dL (39.0–60.5 mg/dL), p < 0.0001].
Evaluation of energy status in the brain.
The energy state in brain tissue was evaluated by measuring ATP, ADP, AMP, and P-Cr concentrations (Table 1). There were no significant differences in cerebral high-energy reserves, as total ATP, ADP, AMP, and P-Cr contents were similar in the two groups. The ATP/ADP and charge ratio in the FGR brains were also similar to those in the controls.
DISCUSSION
In this study, we evaluated carbohydrate substrates and energy status in the brains of rats with FGR induced by STA2. Pyruvate and lactate contents in the brain were decreased significantly in FGR rats. Although glucose content tended to be increased in FGR rat brains compared with controls, glycogen content tended to be lower. These differences in glucose and glycogen content in whole brains, however, did not reach statistical significance. There was also no significant difference in cerebral high-energy reserves such as total ATP, ADP, AMP, and P-Cr contents between the two groups. Our results suggest that a normal energy state is maintained in FGR brains even when serum glucose levels are low. However, energy metabolism may be disrupted easily when there is a decreased supply of carbohydrate substrates in the FGR brains. This suggests that FGR brains may be more susceptible to hypoxic-ischemic events.
In view of the known predisposition for human FGR infants to develop neonatal hypoglycemia, glucose metabolism was the subject of early investigations in FGR models. We measured carbohydrate substrates in the brain, and as expected, showed pyruvate and lactate levels were decreased in FGR rats. Glycogen levels tended to be lower in FGR rats compared with controls, although this difference was not statistically significant. In contrast, glucose content in FGR brains tended to be higher when compared with controls. In general, glucose transportation across the placenta and the blood-brain-barrier is facilitated by carrier-mediated diffusion that is dependent on the concentration gradient. Ogata et al.(25) showed that growth-retarded fetuses had significantly diminished plasma glucose concentrations 10 and 240 min after uterine artery ligation, which recovered to normal ranges by the 21st gestational day. Our results support the hypothesis that fetal glycogen degradation with resultant hyperglycemia ensures an adequate supply of substrates to vital tissues such as the brain, and provides, at least, some measure of fetal tolerance to interruptions in placental oxygen transport (26).
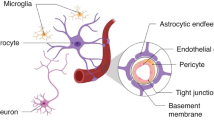
Brain glycogen is contained predominantly in astrocytes, although its concentration is low compared with that in the liver (27). When brain blood flow is interrupted completely, theoretically energy may become depleted within a few minutes. However, it is possible that glucose utilization is considerably slower in newborn rats (28), and therefore glycogen may be an important substrate in fetal and neonatal brains during periods of asphyxia even when the amount of glycogen stored is small. A reduction in umbilical blood flow results in a decrease in fetal glucose and oxygen uptake. Anaerobic glycolysis is then stimulated by hypoxia to maintain optimal cellular energy balance despite oxygen debt. Glycogenolysis with resulting availability of glucose is an obviously important pathway that contributes to glucose homeostasis during the perinatal period. As glycogen storage in fetal brains is minimal (27), the supply of free glucose via glycogenolysis from glycogen storage tissues such as the liver and kidney plays an important role in the survival of the fetus during times of stress. It has been demonstrated that accumulation of fetal hepatic glycogen is decreased in animal models of FGR (25), and in our study we also observed that FGR brains had lower glycogen content. Taken together, these experimental data suggest that FGR brains may have a low tolerance to the effects of undernutrition and adaptive glycogenolysis.
The significance of gluconeogenesis in fetal carbohydrate metabolism remains controversial. Townsend et al. (29) showed that gluconeogenic capacity is not expressed in utero under unperturbed circumstances, and that the contribution of gluconeogenesis from lactate, pyruvate, or alanine to glucose was quantitatively negligible. The FGR newborn also has depressed activity of enzymes necessary for gluconeogenesis (30). However, another report presented evidence that suggested that three carbon substrates, such as lactate, pyruvate, and alanine are likely to be precursors for hepatic glycogen (31). In experiments on fasted sheep, fetal glucose utilization did not decline to the same degree as the decrease in umbilical uptake, suggesting compensatory glucose production by the fetus (32). Rudolph et al. (33) also showed an increase in net glucose production in fetal sheep livers during acute umbilical cord compression.
The substrates in the FGR brain also remain controversial. Kliegman et al. (11) examined brain substrates in FGR dogs and showed the levels of lactate, pyruvate, and glycogen were higher in brain tissue of FGR dogs than in controls. However, glucose levels were similar in the FGR dogs and controls. Lin et al. (12) also reported high levels of pyruvate and glucose in the brains of FGR rats. By using magnetic resonance spectroscopy, Moxon-Lester et al. (13) demonstrated that lactate levels in the brain of FGR piglets and controls were similar. However, in our study, both lactate and pyruvate levels were reduced significantly in the brains of FGR rats. Uteroplacental blood flow reduction induced by STA2 may stimulate gluconeogenesis at the expense of lactate and pyruvate to adapt to the chronic reduction in delivery of oxygen and substrates. This priority for endogenous fuel provision to vital tissues leads to impaired fetal growth. The reasons for the different results in the analysis of brain substrates between studies are not clearly understood, although we speculate that differences between species and the methodologies used in the FGR animal models may have influenced the results.
In this study, serum glucose levels were significantly lower in FGR rats compared with controls. We did not evaluate glycogen storage in the liver or plasma insulin levels in this study. However, Ogata et al. (25) measured serum glucose and insulin levels and glycogen content in FGR rats and showed that insulin levels were low, despite glucose levels and glycogen storage both being decreased. Therefore, we speculate that the cause of hypoglycemia in FGR rats may be due to reduced storage of glycogen.
Regarding brain energy metabolism, no significant difference was observed in the high-energy reserves, ATP, ADP, AMP, and P-Cr between FGR rats and controls. According to a study by Brown and Vannucci (34) using the Wiggleworth FGR model, the concentrations of various cerebral substrate metabolites including glycogen, glucose, lactate, ATP, and P-Cr were not altered in spite of a significant reduction in brain weight. They ascribed these findings to the absence of hypoxia at the level required to disrupt oxidative metabolism and the energy state of the brain. Kliegman et al. (11) demonstrated using a maternal canine starvation model that cerebral charge in FGR neonates was unaffected, whereas their calculated energy reserve was lower than that of controls. Theoretically, depression of oxygen delivery to respiring tissues increases the ADP to ATP ratio (ADP/ATP). This, in turn, acts to stimulate glycolysis (i.e. the Pasteur effect), with a subsequent increase in anaerobic ATP production. In this study, the charge ratio in FGR rat brains was similar to that in controls. This result demonstrates that the energy state in FGR brains can be compensated by stimulation of glycolysis under chronic hypoxic conditions, but that FGR fetuses do not revert totally to anaerobic metabolism.
In summary, chronic disturbance in uteroplacental blood flow stimulates fetal glucose production mainly by increasing gluconeogenesis to maintain a normal energy state in the brain. Energy metabolism in the FGR brain will be liable to disruption and stressed further because of decreased storage of carbohydrate substrates.
Abbreviations
- FGR:
-
fetal growth restriction
- P-Cr:
-
phosphocreatine
- PIH:
-
pregnancy-induced hypertension
- STA2:
-
synthetic thromboxane A2
REFERENCES
Bergvall N, Iliadou A, Johansson S, Tuvemo T, Cnattingius S 2006 Risks for low intellectual performance related to being born small for gestational age are modified by gestational age. Pediatrics 117: e460–e467
Peng Y, Huang B, Biro F, Feng L, Guo Z, Slap G 2005 Outcome of low birthweight in China: a 16-year longitudinal study. Acta Paediatr 94: 843–849
Walker DM, Marlow N 2008 Neurocognitive outcome following fetal growth restriction. Arch Dis Child Fetal Neonatal Ed 93: F322–F325
Anderson P, Doyle LW 2003 Neurobehavioral outcomes of school-age children born extremely low birth weight or very preterm in the 1990s. JAMA 289: 3264–3272
Jarvis S, Glinianaia SV, Torrioli MG, Platt MJ, Miceli M, Jouk PS, Johnson A, Hutton J, Hemming K, Hagberg G, Dolk H, Chalmers J 2003 Cerebral palsy and intrauterine growth in single births: European collaborative study. Lancet 362: 1106–1111
Thordstein CM, Sultan BL, Wennergren MM, Tornqvist E, Lindecrantz KG, Kjellmer I 2004 Visual evoked potentials in disproportionately growth-retarded human neonates. Pediatr Neurol 30: 262–270
Ghidini A 1996 Idiopathic fetal growth restriction: a pathophysiologic approach. Obstet Gynecol Surv 51: 376–382
Soothill PW, Nicolaides KH, Campbell S 1987 Prenatal asphyxia, hyperlacticaemia, hypoglycaemia, and erythroblastosis in growth retarded fetuses. BMJ (Clin Res Ed) 294: 1051–1053
Thordstein M, Kjellmer I 1988 Cerebral tolerance of hypoxia in growth-retarded and appropriately grown newborn guinea pigs. Pediatr Res 24: 633–638
Burke C, Gobe G 2005 Pontosubicular apoptosis (“necrosis”) in human neonates with intrauterine growth retardation and placental infarction. Virchows Arch 446: 640–645
Kliegman RM 1986 Cerebral metabolic intermediate response following severe canine intrauterine growth retardation. Pediatr Res 20: 662–667
Lin CH, Gelardi NL, Cha CJ, Oh W 1998 Cerebral metabolic response to hypoglycemia in severe intrauterine growth-retarded rat pups. Early Hum Dev 52: 1–11
Moxon-Lester L, Sinclair K, Burke C, Cowin GJ, Rose SE, Colditz P 2007 Increased cerebral lactate during hypoxia may be neuroprotective in newborn piglets with intrauterine growth restriction. Brain Res 1179: 79–88
Magness RR, Mitchell MD, Rosenfeld CR 1990 Uteroplacental production of eicosanoids in ovine pregnancy. Prostaglandins 39: 75–88
Sibai BM 1992 An aspirin a day to prevent prematurity. Clin Perinatol 19: 305–317
Wallenburg HC, Rotmans N 1987 Prevention of recurrent idiopathic fetal growth retardation by low-dose aspirin and dipyridamole. Am J Obstet Gynecol 157: 1230–1235
Hayakawa M, Takemoto K, Nakayama A, Saito A, Sato Y, Hasegawa M, Ieda K, Mimura S 2006 An animal model of intrauterine growth retardation induced by synthetic thromboxane A2. J Soc Gynecol Investig 13: 566–572
Wigglesworth JS 1964 Experimental growth retardation in the foetal rat. J Pathol Bacteriol 88: 1–13
Mellor DJ, Matheson IC 1979 Daily changes in the curved crown-rump length of individual sheep fetuses during the last 60 days of pregnancy and effects of different levels of maternal nutrition. Q J Exp Physiol Cogn Med Sci 64: 119–131
Saito A, Matsui F, Hayashi K, Watanabe K, Ichinohashi Y, Sato Y, Hayakawa M, Kojima S, Oohira A 2009 Behavioral abnormalities of fetal growth retardation model rats with reduced amounts of brain proteoglycans. Exp Neurol 219: 81–92
Duvanel CB, Fawer CL, Cotting J, Hohlfeld P, Matthieu JM 1999 Long-term effects of neonatal hypoglycemia on brain growth and psychomotor development in small-for-gestational-age preterm infants. J Pediatr 134: 492–498
Vannucci RC, Duffy TE 1974 Influence of birth on carbohydrate and energy metabolism in rat brain. Am J Physiol 226: 933–940
Lowry OH, Passonneau JV 1972 A Flexible System of Enzymatic Analysis. Academic Press, New York
Atkinson DE, Walton GM 1967 Adenosine triphosphate conservation in metabolic regulation. Rat liver citrate cleavage enzyme. J Biol Chem 242: 3239–3241
Ogata ES, Swanson SL, Collins JW Jr, Finley SL 1990 Intrauterine growth retardation: altered hepatic energy and redox states in the fetal rat. Pediatr Res 27: 56–63
Philipps A 1992 Carbohydrate metabolism of the fetus. In: Polin R, Fox W (eds) Fetal and Neonatal Physiology. WB Saunders Company, Philadelphia, pp 373–384
Brown AM, Tekkok SB, Ransom BR 2003 Glycogen regulation and functional role in mouse white matter. J Physiol 549: 501–512
Moore TJ, Lione AP, Regen DM, Tarpley HL, Raines PL 1971 Brain glucose metabolism in the newborn rat. Am J Physiol 221: 1746–1753
Townsend SF, Rudolph CD, Wood CE, Rudolph AM 1989 Perinatal onset of hepatic gluconeogenesis in the lamb. J Dev Physiol 12: 329–335
Pollak A, Susa JB, Stonestreet BS, Schwartz R, Oh W 1979 Phosphoenolpyruvate carboxykinase in experimental intrauterine growth retardation in rats. Pediatr Res 13: 175–177
Levitsky LL, Paton JB, Fisher DE 1988 Precursors to glycogen in ovine fetuses. Am J Physiol 255: E743–E747
Hay WW Jr, Sparks JW, Wilkening RB, Battaglia FC, Meschia G 1984 Fetal glucose uptake and utilization as functions of maternal glucose concentration. Am J Physiol 246: E237–E242
Rudolph CD, Roman C, Rudolph AM 1989 Effect of acute umbilical cord compression on hepatic carbohydrate metabolism in the fetal lamb. Pediatr Res 25: 228–233
Brown JD, Vannucci RC 1978 Cerebral oxidative metabolism during intrauterine growth retardation. Biol Neonate 34: 170–173
Acknowledgements
We dedicate this report to Dr. S Mimura who designed the study protocol but died before its the completion.
Author information
Authors and Affiliations
Corresponding author
Additional information
Supported, in part, by a Grant-in-Aid for Scientific Research (No. 20591296) from the Ministry of Education, Culture, Sports, Science, and Technology.
Rights and permissions
About this article
Cite this article
Hayakawa, M., Sato, Y., Hattori, T. et al. Carbohydrate and Energy Metabolism in the Brain of Rats With Thromboxane A2-Induced Fetal Growth Restriction. Pediatr Res 70, 21–24 (2011). https://doi.org/10.1203/PDR.0b013e31821b9d7c
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/PDR.0b013e31821b9d7c
This article is cited by
-
Role for the thromboxane A2 receptor β-isoform in the pathogenesis of intrauterine growth restriction
Scientific Reports (2016)
-
Acute hypoglycemia results in reduced cortical neuronal injury in the developing IUGR rat
Pediatric Research (2015)