Abstract
The mucopolysaccharidoses (MPS) are inherited metabolic disorders resulting from the defective catabolism of glycosaminoglycans. In this report, we find that the stimulation of MPS connective tissue cells by the inflammatory cytokines causes enhanced secretion of several matrix-degrading metalloproteinases (MMPs). In addition, expression of tissue inhibitor of metalloproteinase-1 was elevated, consistent with the enhanced MMP activity. These findings were not restricted to one particular MPS disorder or species, and are consistent with previous observations in animal models with chemically induced arthritis. Bromodeoxyuridine incorporation studies also revealed that MPS chondrocytes proliferated up to 5-fold faster than normal chondrocytes, and released elevated levels of transforming growth factor-beta, presumably to counteract the marked chondrocyte apoptosis and matrix degradation associated with MMP expression. Despite this compensatory mechanism, studies of endochondral ossification revealed a reduction in chondro-differentiation in the growth plates. Thus, although MPS chondrocytes grew faster, most of the newly formed cells were immature and could not mineralize into bone. Our studies suggest that altered MMP expression, most likely stimulated by inflammatory cytokines and nitric oxide, is an important feature of the MPS disorders. These data also identify several proinflammatory cytokines, nitric oxide, and MMPs as novel therapeutic targets and/or biomarkers of MPS joint and bone disease. This information should aid in the evaluation of existing therapies for these disorders, such as enzyme replacement therapy and bone marrow transplantation, and may lead to the development of new therapeutic approaches.
Similar content being viewed by others
Main
The accumulation of partially degraded glycosaminoglycans (GAGs) in late endosomes and lysosomes of connective tissue cells is characteristic of a family of heritable lysosomal storage diseases known as the mucopolysaccharidoses (MPS) (1). The MPS family consists of 12 chronic and progressive syndromes, each with a specific enzyme deficiency leading to a characteristic pattern of accumulating GAGs within lysosomes. Among the different MPS disorders, there are several clinical characteristics present in most affected individuals. These include anterior hypoplasia of lumbar vertebrae, enlarged diaphyses of the long bones, underdeveloped epiphyseal centers, marked dwarfism, degenerative joint disease, dysostosis multiplex, facial dysmorphia, organomegaly, corneal clouding, and in most syndromes mental retardation (1). Cartilage is a major site of pathology in these diseases, leading to painful joints, poor joint mobility, poor bone growth, and an abnormal larynx and trachea producing breathing abnormalities often requiring tracheotomies.
There are numerous MPS animal models available for study, either naturally occurring or generated through targeted disruption of the corresponding mouse gene (e.g., 2–5). These animal models have biochemical and pathologic features that are similar to their human counterparts, and their availability has facilitated the evaluation of various therapeutic approaches and a better understanding of the disease pathogenesis.
Using these animals, several therapies have been investigated for the treatment of the MPS disorders, including bone marrow transplantation (BMT) (6–8), enzyme replacement therapy (ERT) (9–12), and gene therapy (13). Varying results have been obtained from these endeavors, in part due to differences in the procedures used and/or specific issues related to the particular disease and animal model studied. Currently, for human patients BMT is undertaken for several of the MPS disorders, and ERT is available for MPS I and under evaluation for MPS II and VI (14). However, these therapies have proven to be very limited in their ability to prevent or reverse most of the serious bone and cartilage complications. In addition, few biomarkers exist to monitor the severity of bone and joint involvement in these disorders, or the effects of therapies.
In part, the lack of effective bone-directed therapies is due to the poorly characterized underlying pathophysiology. Morphologic analysis of MPS growth plates has revealed clusters of enlarged, GAG-containing cells that disrupt the normal columnar architecture of the growth plate cartilage, presumably leading, in part, to the bone growth abnormalities (15,16). This has led to the suggestion that the main tissue site of pathology in these disorders is the cartilage, rather than the bone itself. The articular cartilage also is thicker in MPS VI and VII animals with a hyperplastic synovium, suggesting that there are also abnormalities in articular cartilage matrix formation and function (17).
Our previous studies have demonstrated increased apoptosis of MPS chondrocytes, leading to a depletion of proteoglycans and total collagen in the cartilage of MPS animals (18). During the course of this work, we also observed that many analogies could be made between the cartilage of MPS individuals and those with osteo- or rheumatoid arthritis (OA and RA, respectively). Similarities exist in the secretion of proinflammatory cytokines, such as tumor necrosis factor-alpha (TNF-α) and IL-1 beta (IL-1β), nitric oxide (NO) production, apoptosis of chondrocytes, and reduced proteoglycan content in the extracellular matrix (ECM). Matrix metalloproteinases (MMPs) are key enzymes involved in ECM degradation, and enhanced MMP activity is an important feature of arthritis. MMP transcription is regulated by growth factors and cytokines, while specific tissue inhibitors of metalloproteinase (TIMPs) regulate their translation and proenzyme activation (19,20). In arthritis, tissue destruction often correlates with the imbalance of MMPs over TIMPs. For example, in RA, synovial fluid contains elevated levels of MMP-2 and MMP-9, both of which degrade the joint matrix because of their gelatinase activities (21). In addition to proinflammatory cytokines, NO production has also been shown to act as a proinflammatory mediator leading to enhanced MMP production (22).
Herein, we report the further characterization of joint and bone disease in MPS animal models. Enhanced expression of MMP-2 and MMP-9 was observed in the MPS animals, and was associated with abnormal expression of TIMP-1. In addition, we show that increased expression of TGF-β in MPS cartilage leads to enhanced proliferation of chondrocytes in these tissues, but that a majority of these newly formed cells remain immature and cannot mineralize into bone. Based on these findings, we suggest that further research on the treatment of MPS joint and bone degeneration should be based on the emerging picture of inflammatory disease in these disorders, and its particular effects on cartilage. In addition, we suggest that many of the molecules we have identified in the course of these studies may serve as new biomarkers to monitor MPS disease progression and treatment, as they have in arthritis, and may also be important therapeutic targets. Lastly, we suggest that the MPS animal models may be useful to the arthritis research community since they are naturally occurring and relatively homogeneous, and could serve as adjuncts to the chemically induced arthritis models that are currently used.
METHODS
Animals.
The MPS VI cat and rat models, and MPS VII dog model have been previously described (2–4). Affected and control animals were raised under National Institutes of Health and USDA guidelines for the care and use of animals in research. Rats were maintained at the Mount Sinai School of Medicine, while the larger animal models were maintained at the University of Pennsylvania School of Veterinary Medicine. The animals were housed with ad libitum food and water, 12-h light cycles at 21°C, with 12–15 air changes per hour. Euthanasia was performed on cats and dogs using 80 mg/kg of sodium pentobarbital (Veterinary Laboratories, Lenexa, KS) in accordance with the American Veterinary Medical Association guidelines. Euthanasia of rats was performed using carbon dioxide inhalation. Breeding colonies were maintained under IACUC approved protocols and genotyped by clinical/pathologic screening of WBC and by PCR-based methods (23,24).
Sample isolation and chondrocyte cultures.
Proximal humeri, femurs, and proximal tibias were collected from age-matched normal and MPS animals and placed in either PBS (PBS) for chondrocyte isolation or fixed in neutral buffered 10% formalin (Sigma Chemical Co. Chemical, St. Louis, MO) for immunohistochemical assessment (see below). For immunohistochemistry, the formalin-fixed bones were decalcified in 8% formic acid (Sigma Chemical Co. Chemical) for 5 d, embedded in paraffin, and sectioned (5 μm). The tissues were obtained from four animals in each age group, ranging from 2 wk to 12 mo in the rats, 3 to 60 mo in the cats, and 2 to 6 mo in dogs.
To establish primary chondrocyte cultures, the articular cartilage was sliced from the underlying bone, and washed in minimal essential medium (MEM, Invitrogen, Carlsbad, CA). The cartilage was minced and digested with 1% hyaluronidase for 1 h at 37°C, washed three times with PBS containing 1 mM EDTA, and sequentially incubated with 2.5% trypsin (Invitrogen) and 0.01 M EDTA for 1 h at 37°C, followed by further digestion at 37°C for 8 h with 0.2% collagenase (Sigma Chemical Co.) prepared in MEM containing 10% FCS. Cells were isolated by centrifugation (450 g), washed twice, and plated in 96 well plates at a concentration of 7 × 104 cells in MEM containing 10% fetal bovine serum, 1% glutamine, penicillin (150 units/mL), and streptomycin (50 μg/mL). After 24 h, the media was changed to serum-free, and then collected after 48 h and either immediately analyzed or stored at −20°C.
Samples of synovial fluid also were obtained from the joints of normal and MPS VII dogs. Dogs were euthanized and the joints were examined to confirm the lack or presence of gross pathologic changes. Samples of synovial fluid were collected from the following joints: stifle, elbow, shoulder and coxofemoral. After isolation, synovial samples were divided into aliquots and stored frozen at −70°C until analyzed. Synovial membranes from MPS VII and normal dogs also were collected from stifle following euthanasia, embedded in OCT media (Sakura Finetek, Torrance, CA), frozen, and stored at −70°C until analyzed.
Immunohistochemical staining.
Bone sections were deparaffinized, rehydrated in a series of descending ethanol concentrations, and digested for 1 h with testicular hyaluronidase (2 mg/mL, Sigma Chemical Co.) in PBS. Immunohistochemistry for MMP-2 was performed using an anti-mouse MMP-2 (72 kD collagenase IV) MAb (NeoMarkers, Fremont, CA), while MMP-9 was detected using an anti-rat MMP-9 (95 kD collagenase/gelatinase B) MAb (Chemicon International, Temecula, CA). Immunohistochemical detection of osteonectin was carried out using an anti-human osteonectin antibody (Chemicon International). Dilutions of the specific antisera were applied in PBS containing 1% BSA, and the sections were incubated overnight at 4°C. After several rinses with PBS, visualization was performed using the streptavidin-biotin complex method (Histostain-Plus kit, Zymed, San Francisco, CA). Biotin conjugated secondary antibodies were applied and incubated for 10 min at room temperature. The slides were washed twice with PBS, incubated with streptavidin-conjugated horseradish peroxidase for 10 min, stained with diaminobenzidine, and counterstained with hematoxylin.
Reverse transcription-polymerase chain reaction (RT-PCR).
Total RNA was extracted from cultured chondrocytes using the Rneasy Mini Kit (Qiagen, Valencia, CA) and processed according to the manufacturers instructions. Total RNA was reverse transcribed into first-strand cDNA (cDNA) using the SuperScript II RT kit (Invitrogen) utilizing random hexanucleotide primers. For cDNA amplification, 1.0 μg of cDNA, 10× PCR buffer (100 mM Tris-HCl, 500 mM KCl, 25 mM MgCl2), 2.5 mM dNTPs, 20 pmol of sense and anti-sense primers, and recombinant Taq polymerase (Invitrogen) was mixed in a total reaction volume of 25 μL. PCR amplification was performed using oligonucleotides corresponding to cDNA sequences for MMP-2 (25), MMP-9 (25), and TIMP-1 (26).
In situ gelatinase activity in synovial membranes.
A method of fluorescent substrate overlay was used to detect in situ proteinase activity in sections of intact frozen tissues (27). Synovial membranes from MPS VII and normal dogs were snap-frozen and embedded in OCT media (Sakura Finetek). Transverse sections (6 μm) were immediately overlaid with 20 μL of FITC-labeled gelatin (2 μg/mL in 50 mM Tris-HCl, pH 7.6) (Molecular Probes, Eugene, OR). Coverslips were applied, and samples were incubated in a humidified chamber at 37°C for 3 h. Areas of proteolytic activity observed during microscopic examination were compared with areas from serial sections in which MMP activity was inhibited with 1,10-phenanthroline monohydrate. Images were captured by a Nikon E600 fluorescent microscope (Nikon Inc, Melville, NY) and associated Phase III Image Pro analyzer software (Phase III, PA).
Proliferation assays.
Chondrocytes from normal and MPS age-matched animals were seeded at 1–4 × 105 cells/mL into 96 well culture plates and grown for 72 h in the presence of bromodeoxyuridine (BrdU). A cell proliferation assay kit (Calbiochem, SanDiego, CA) was used to detect BrdU incorporation into newly synthesized DNA of proliferating cells.
Immunoassays.
Il-1β, TIMP-1, TGF-β, and TNF-α protein expression was quantified by immunoassays using normal and MPS plasma, conditioned chondrocyte media, and/or synovial fluid using rat and human Quantikine® immunoassay kits (R&D Systems, Minn. MN) according to the manufacturer's protocols. MMP-2 and -9 enzymatic activities also were measured using commercial assay kits (Chemicon International) according to the manufacturer's protocol. Before use, samples for the MMP assays were activated with 5 mM p-aminophenylmercuric acetate (Sigma Chemical Co. Chemical) at 37°C for 30 min. All immuno- and enzymatic assay experiments were performed in duplicates and for each experiment at least three samples were studied per animal. The student's 2-tailed t test was used to calculate the statistical significance of the difference between the two groups.
RESULTS
Gelatinase expression.
Abnormal regulation of gelatinase activity is an important factor in arthritic bone disease. To assess total gelatinase activity in tissues from MPS animals (MPS VI rats and cats, and MPS VII dogs), cartilage and synovial membranes were subjected to in situ gelatinase assays. As shown for the synovial membranes of MPS VII dogs (Fig. 1), markedly enhanced gelatinase activity was observed in tissues from each of these MPS models. High levels of MMP activity were present in the synoviocytes, as well as in the extracellular spaces of the underlying synovial membranes (Fig. 1B). The majority of this enhanced activity was attributable to MMPs because co-incubation with 1,10 phenanthrolene, a metalloprotease inhibitor, reduced the in situ gelatinase staining (Fig. 1C).
In situ gelatinase activity in normal and MPS VII dog synovial membranes. (A) Gelatin overlay of synovium from normal one-year old dog. (B) Gelatin overlay of age-matched MPS VII dog synovium showing enhanced MMP activity concentrated in the synoviocytes and the underlying extracellular matrix of the hyperplastic synovium. (C) Gelatin overlay of MPS VII dog synovium treated with an MMP inhibitor (1,10-phenanthroline monohydrate), resulting in quenching of the activity. Magnification 60×.
MMP associated gelatinase activity also was evaluated in serum free-conditioned media obtained from primary chondrocytes of each MPS animal model. The MPS conditioned media had from 67.8% to 330% more MMP gelatinase activity when compared with media from normal cells. To investigate these findings further, immunohistochemical staining for MMP-2 and -9 was carried out using tissues from the MPS animals. As shown in Figs. 2 and 3, enhanced MMP immunostaining was seen in the cartilage and bone marrow of the MPS animals, confirming the in situ and in vitro gelatinase assays. Enhanced MMP expression was primarily detected in the superficial and intermediate zones, and bone marrow osteoclasts and osteoblasts. Neutrophils and macrophages in the bone marrow also stained positive for the two MMPs. In most cases, the MMP immunostaining was intracellular and/or pericellular.
Immunostaining of MMP-2 in rat tibia. (A) MMP-2 staining in superficial and intermediate cartilage of normal 6-month old rats. (B) MMP-2 staining in the superficial and intermediate cartilage from age-matched MPS VI rats. Note that most of the MMP-2 staining is intracellular with slight staining of the extracellular matrix. (C) MMP-2 staining in subchondral bone of normal 6-month old rats. (D) MMP-2 staining in age-matched MPS VI rat subchondral bone. Note that most of the enhanced immunostaining is observed in the bone marrow and within osteoblasts (arrow). Magnification 60×.
Immunostaining of MMP-9 in rat tibia. (A) Normal, 6-month old rat tibia. (B) Age-matched MPS VI rat tibia showing enhanced MMP-9 staining in multi-nuclear osteoclasts (arrow) Magnification 40×. (C) MPS VI rat tibia showing MMP-9 staining in neutrophils (arrowhead) and osteoblasts (arrow) Magnification 100×.
To confirm the protein expression results, MMP gene expression also was examined in the MPS animals by RT-PCR analysis. As shown in Fig. 4, expression of the MMP-2 and -9 genes was significantly enhanced in articular chondrocytes, consistent with enhanced MMP gelatinase activity.
TIMP-1 expression.
TIMP-1 is an important component of the complex regulatory pathway that controls gelatinase activity, and a balance of gelatinase and TIMP-1 is required for normal bone homeostasis. In arthritis, elevated gelatinase activity is associated with elevated TIMP-1, however the net ratio of gelatinase activity to TIMP-1 is significantly increased, leading to enhanced bone degradation (21,28,29). TIMP-1 expression was measured in serum free conditioned media obtained from primary MPS VI rat chondrocyte cultures, and was found to be elevated ~35% compared with cultures established from age-matched normal animals (Fig. 5A). Similarly, RT-PCR analysis revealed slightly elevated TIMP-1 gene expression in chondrocytes (Fig. 5B). These results are similar to those found in arthritis, and are consistent with elevations of proinflammatory cytokines that we have previously shown in these animals (18). A 3-fold TIMP-1 elevation also was observed in synovial fluid from MPS VII animals (data not shown).
TIMP-1 expression in rats. (A) TIMP-1 concentration in supernatants from normal (open box) and MPS VI (solid box) rat chondrocytes. Data represent median values obtained from 4 individual animals. (B) TIMP-1 mRNA expression in tibial plateau cartilage. Equivalent amounts of DNA (1 μg) from 6-month old normal and MPS VI rats were used as templates for the PCR.
Cell proliferation and TGF-β expression.
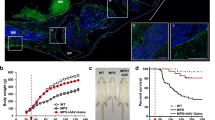
In our previous work we observed marked apoptotic cell death in MPS cartilage (18). However, despite increased chondrocyte death, no significant cell loss was observed. To address this apparent contradiction, we determined the proliferation rate of MPS chondrocytes in culture. As shown in Fig. 6 for MPS VI rats and cats, but also observed for MPS VII dogs, BrdU incorporation studies revealed a markedly increased proliferation rate of these cells (up to 5-fold), perhaps explaining why little cell loss was observed in the MPS cartilage despite massive cell death.
Chondrocyte proliferation studies in MPS VI animals. 6-month-old MPS VI rat (A) and one-year-old MPS VI cat (B) chondrocytes were grown in the presence of BrdU for 72 h, and proliferation rates were compared with chondrocytes grown from age-matched normal animals. Closed and open boxes represent MPS and normal animals, respectively. Data represents median values obtained from four independent experiments. MPS VI rat chondrocytes showed a 2-fold increase in proliferation rate, whereas MPS VI cat chondrocytes showed up to a 5-fold increase.
TGF-β is an important growth factor involved in regulating cell proliferation, and also plays an important role in the control of TIMP-1 gene expression (30). As shown in Fig. 7, TGF-β levels in serum free conditioned media from primary MPS VI articular chondrocyte cultures was significantly elevated, consistent with the enhanced cell proliferation rate and elevated TIMP-1 and gelatinase expression. However, despite the fact that MPS chondrocytes were proliferating at a rapid rate (presumably to compensate for the enhanced apoptosis), the functional capacity and developmental program of these newly formed cells remained unknown. We also carried out immunostaining for osteonectin, a marker of maturing chondrocytes, on growth plate cartilage from MPS VI rats. As can be seen in Fig. 8, osteonectin staining was markedly reduced in the MPS animals, suggesting that the newly formed chondrocytes were not mature, and thus, could not undergo hypertrophy and develop into bone.
TGF-β activity in MPS VI chondrocytes. TGF-β concentrations were determined in serum-free culture supernatants after 48 h. Data represent median value of 4 individual animals. (A) Chondrocytes were obtained from 6-month old MPS VI rats (solid box) and normal age matched controls (open box). (B) Chondrocytes were obtained from one-year old MPS VI cats (solid box) and age-matched, MPS VI heterozygous cats (hatched box).
DISCUSSION
We previously reported enhanced chondrocyte apoptosis in the articular cartilage of MPS animal models, and found that the levels of IL-1β, TNF-α, and NO were markedly increased in the media of MPS chondrocyte cultures compared with normal cells. Furthermore, these levels were significantly greater in cells from older MPS animals when compared with young (18). To explain why, despite the very high apoptosis rate, the overall chondrocyte cell number was not markedly reduced in these animals, we postulated that TGF-β release might also be enhanced. TGF-β is known to have a mitogenic effect on cells and to counteract the effects of apoptosis (31). Indeed, as described above, this was found to be the case, and proliferation studies performed on normal and MPS VI articular chondrocytes using BrdU immunolabeling revealed that the MPS cells were proliferating up to 5-fold faster than normal cells. Thus, MPS animals appear to be compensating for enhanced cell death in the cartilage by increasing cell proliferation.
However, despite this compensation mechanism, marked bone and joint abnormalities are still observed in the MPS animals. Nuttall et al. (32) has suggested that the osteopenia observed in MPS VI may be due to a delayed turnover of hypertrophic chondrocytes in the growth plate. Therefore, we used osteonectin as a marker for proliferating and differentiating chondrocytes and chondroid matrix formation, and observed a marked reduction in hypertrophic cells in the epiphyseal plate of MPS VI rats. While the mechanism for the reduced hypertrophy remains unknown, intriguingly, TGF-β inhibits terminal differentiation of immature chondrocytes (30,33), and enhanced expression of TGF-β in the MPS animals may, in part, be responsible for this observation. In addition, osteonectin, which is required for forming bone from cartilage, is a substrate for MMP-2 and -9, both of which are elevated in MPS bones and joints (see Figs. 1–4). Clearly, whatever the underlying mechanism, one component of the osteopenia in this MPS model appears to arise from a defect in bone production due to a reduction in hypertrophic chondrocytes available for mineralization into bone.
There are numerous analogies between our findings in the MPS animal models and arthritis. For example, MMPs are particularly important in the chondrolytic processes that contribute to degenerative changes in arthritis, and arthritic chondrocytes release elevated levels of MMP-2 and -9 (34). MMPs are secreted from cells as inactive zymogens, and the pro-forms are activated by serine proteinases and other classes of MMPs. In addition, MMP activities are reduced by tissue inhibitors of metalloproteinases (e.g., TIMP-1) (35), while NO and proinflammatory cytokines induce their synthesis and/or activate them (36,37). Thus, the precise regulation of MMP activity is crucial for maintaining the proper balance of tissue remodeling and damage. In fact, abnormal articular extracellular matrix remodeling in RA is due, in part, to abnormalities in this precise MMP regulation pathway (22).
Similar to RA, in the MPS disorders synoviocytes and chondrocytes are the primary source of NO (38,39). Cytokines, such as IL-1β and TNF-α, also are produced by MPS chondrocytes, synoviocytes, and macrophages, and significantly up-regulate MMP gene expression (this manuscript), as they do in arthritis. Notably, we also found an increase in TIMP-1 gene and protein expression in cultured MPS cells, but we presume that this TIMP-1 cannot effectively compensate for the dramatic over-expression of MMP-2 and MMP-9, thus leading to enhanced matrix degradation. This observation was similar to the situation in OA, where TIMP-1 mRNA and protein expression is up-regulated, although its activity is reduced.
Our results suggest that strategies that use inhibition of cytokines, over-expression of TIMPs (or TIMP activation), and/or the prevention of apoptosis should be explored as treatments for the bone and joint disease in the MPS disorders. While these approaches will not address the underlying GAG storage abnormalities and may not be completely effective alone, in combination with ERT or gene therapy, they may be useful adjuncts. Our results also provide further documentation that the degenerative joint and bone disease in MPS animals is remarkably similar to that occurring in chemically induced animal models of arthritis. Thus, the MPS animals represent naturally occurring, somewhat inbred models that should be useful to the arthritis research community. Investigators in this area have been severely limited by their reliance on chemically induced models that are not homogenous and nonphysiologic. Lastly, this research has revealed several molecules (e.g., NO, proinflammatory cytokines, MMPs, TIMP-1) that could be used as biomarkers to monitor disease severity and treatment in MPS patients (Table 1). Several of these markers can be easily measured in synovial fluid and/or serum, and may be a more direct measure of changes in the joints and bones than GAG release into urine, which is currently used.(40–44).
Abbreviations
- BMT:
-
bone marrow transplantation
- BrdU:
-
bromodeoxyuridine
- ECM:
-
extracellular matrix
- ERT:
-
enzyme replacement therapy
- GAGs:
-
glycosaminoglycans
- IL1-β:
-
interleukin 1-beta
- MMPs:
-
matrix metalloproteinases
- MPS:
-
mucopolysaccharidoses
- NO:
-
nitric oxide
- OA:
-
osteoarthritis
- RA:
-
rheumatoid arthritis
- TGF-β:
-
transforming growth factor-beta
- TIMP:
-
tissue inhibitor of metalloproteinase
- TNF-α:
-
tumor necrosis factor-alpha
References
Neufeld EF, Muenzer J 2001 The Metabolic and Molecular Bases of Inherited Disease. McGraw-Hill, New York, pp 3421–3452
Jezyk PF, Haskins ME, Patterson DF, Mellman WJ, Greenstein M 1977 Mucopolysaccharidosis in a cat with arylsulfatase B deficiency: a model of Maroteux-Lamy syndrome. Science 198: 834–836
Haskins ME, Desnick RJ, DiFerrante N, Jezyk PF, Patterson DF 1984 Beta-glucuronidase deficiency in a dog: a model of human mucopolysaccharidosis VII. Pediatr Res 18: 980–984
Yoshida M, Noguchi J, Ikadai H, Takahashi M, Nagase S 1993 Arylsulfatase B-deficient mucopolysaccharidosis in rats. J Clin Invest 91: 1099–1104
Haskins M, Casal M, Ellinwood NM, Melniczek J, Mazrier H, Giger U 2002 Animal models for mucopolysaccharidoses and their clinical relevance. Acta Paediatr Suppl 91: 88–97
Gasper PW, Thrall MA, Wenger DA, Macy DW, Ham L, Dornsife RE, McBiles K, Quackenbush SL, Kesel ML, Gillette EL et al. 1984 Correction of feline arylsulfatase B deficiency (mucopolysaccharidosis VI) by bone marrow transplantation. Nature 312: 467–469
Sands MS, Barker JE, Vogler C, Levy B, Gwynn B, Galvin N, Sly WS, Birkenmeir E 1993 Treatment of murine mucopolysaccharidosis type VII by syngeneic bone marrow transplantation in neonates. Lab Invest 68: 676–686
Simonaro C, Haskins ME, Kunieda T, Evans SM, Visser JW, Schuchman E 1997 Bone marrow transplantation in newborn rats with mucopolysaccharidosis type VI: biochemical, pathological, and clinical findings. Transplantation 63: 1386–1393
Shull RM, Kakkis ED, McEntee MF, Kania SA, Jonas AJ, Neufeld EF 1994 Enzyme replacement in a canine model of Hurler syndrome. Proc Natl Acad Sci USA 91: 12937–12941
Kakkis ED, McEntee MF, Schmidtchen A, Neufeld EF, Ward DA, Gompf RE, Kania S, Bedolla C, Chien SL, Shull RM 1996 Long-term and high-dose trials of enzyme replacement therapy in the canine model of mucopolysaccharidosis I. Biochem Mol Med 58: 156–167
Kakkis ED, Schuchman E, He X, Wan Q, Kania S, Wiemelt S, Hasson CW, O'Malley T, Weil MA, Aguirre GA, Brown DE, Haskins ME 2001 Enzyme replacement in feline mucopolysaccharidosis type I. Mol Genet Metab 72: 199–208
Simonaro CM, Haskins ME, Abkowitz JL, Brooks DA, Hopwood JJ, Zhang J, Schuchman EH 1999 Autologous transplantation of retrovirally transduced bone marrow or neonatal blood cells into cats can lead to long-term engraftment in the absence of myeloablation. Gene Ther 6: 107–113
Ellinwood NM, Vite CH, Haskins ME 2004 Gene therapy for lysosomal storage diseases: the lessons and promise of animal models. J Gene Med 6: 481–506
Desnick RJ 2004 Enzyme replacement and enhancement therapies for lysosomal diseases. J Inherit Metab Dis 27: 385–410
Norrdin RW, Moffat KS, Thrall MA, Gasper PW 1993 Characterization of osteopenia in feline mucopolysaccharidosis VI and evaluation of bone marrow transplantation therapy. Bone 14: 361–367
Abreu S, Hayden J, Berthold P, Shapiro IM, Decker S, Patterson D, Haskins M 1995 Growth plate pathology in feline mucopolysaccharidosis VI. Calcif Tissue Int 57: 185–190
Byers S, Crawley AC, Brumfield LK, Nuttall JD, Hopwood JJ 2000 Enzyme replacement therapy in a feline model of MPS VI: modification of enzyme structure and dose frequency. Pediatr Res 47: 743–749
Simonaro CM, Haskins ME, Schuchman EH 2001 Articular chondrocytes from animals with a dermatan sulfate storage disease undergo a high rate of apoptosis and release nitric oxide and inflammatory cytokines: a possible mechanism underlying degenerative joint disease in the mucopolysaccharidoses. Lab Invest 81: 1319–1328
Tetlow LC, Adlam DJ, Wooley DE 2001 Matrix metalloproteinase and proinflammatory cytokine production by chondrocytes of human osteoarthritic cartilage: associations with degenerative changes. Arthritis Rheum 44: 585–594
Visse R, Nagase H 2003 Matrix metalloproteinases and tissue inhibitors of metalloproteinases: structure, function and biochemistry. Circ Res 92: 827–839
Yoshihara Y, Nakamura H, Obata K, Yamada H, Hayakawa T, Fujikawa K, Okada Y 2001 Matrix metalloproteinases and tissue inhibitors of metalloproteinases in synovial fluids from patients with rheumatoid arthritis or osteoarthritis. Ann Rheum Dis 59: 455–461
Hirai Y, Migita K, Honda S, Ueki Y, Yamasaki S, Urayama S, Kamachi M, Kawakami A, Ida H, Fukuda T, Shibatomi K, Kawabe Y, Aoyagi T, Eguchi K 2001 Effects of nitric oxide on matrix metalloproteinase-2 production by rheumatoid synovial cells. Life Sci 68: 913–920
Kunieda T, Simonaro CM, Yoshida M, Ikadai H, Levan G, Desnick RJ, Schuchman EH 1995 Mucopolysaccharidosis type VI in rats: isolation of cDNAs encoding arylsulfatase B, chromosomal localization of the gene, and identification of the mutation. Genomics 29: 582–587
Beratis NG, Turner BM, Weiss R, Hirschhorn K 1975 Arylsulfatase B deficiency in Maroteaux-Lamy syndrome: cellular studies and carrier identification. Pediatr Res 9: 475–480
Ijima Y, Kobayashi M, Kubota E 2001 Role of interleukin-1 in induction of matrix metalloproteinases synthesized by rat temporomandibular joint chondrocytes and disc cells. Eur J Oral Sci 109: 50–59
Flannelly J, Chambers MG, Dudhia J, Hembry RM, Murphy G, Mason RM, Bayliss MT 2002 Metalloproteinase and tissue inhibitor of metalloproteinase expression in the murine STR/ort model of osteoarthritis. Osteoarthritis Cartilage 10: 722–733
Sarment DP, Korostoff J, D'Angelo M, Polson AM, Feldman RS, Billing PC In Situ localization and characterization of active proteases in chronically inflamed and healthy human gingival tissues. J Periodontol 70: 1303–1312, 1999
Ishiguro N, Ito T, Miyazaki K, Iwata H 1999 Matrix metalloproteinases, tissue inhibitors of metalloproteinases, and glycosaminoglycans in synovial fluid from patients with rheumatoid arthritis. J Rheumatol 26: 34–40
Keyszer G, Lambiri I, Nagel R, Keysser C, Keysser M, Gromnica-Ihle E, Franz J, Burmester GR, Jung K 1999 Circulating levels of matrix metalloproteinases MMP-3 and MMP-1, tissue inhibitor of metalloproteinases I (TIMP-1) and MMP-1/TIMP-1 complex in rheumatic disease. Correlation with clinical activity of rheumatoid arthritis versus surrogate markers. J Rheumatol 26: 251–258
Gunther M, Haubeck HD, van de Leur E, Blaser J, Bender S, Gutgemann I, Fischer DC, Tschesche H, Greiling H, Heinrich PC 1994 Transforming growth factor beta 1 regulates tissue inhibitor of metalloproteinase-1 expression in differentiated human articular chondrocytes. Arthritis Rheum 37: 395–405
Kawakami A, Eguchi K, Matsuoka N, Tsuboi M, Kawabe Y, Aoyagi T, Nagataki S 1996 Inhibition of Fas antigen-mediated apoptosis of rheumatoid synovial cells in vitro by transforming growth factor beta 1. Arthritis Rheum 39: 1267–1276
Nuttall JD, Brumfield LK, Fazzalari NL, Hopwood JJ, Byers S 1999 Histomorphometric analysis of the tibial growth plate in a feline model of mucopolysaccharidosis type VI. Calcif Tissue Int 65: 47–52
Serra R, Johnson M, Filvaroff EH, LaBorde J, Sheehan DM, Derynck R, Moses HL 1997 Expression of a truncated, kinase-defective TGF-beta type II receptor in mouse skeletal tissue promotes terminal chondrocyte differentiation and osteoarthritis. J Cell Biol 139: 541–552
Hembry RM, Bagga MR, Dingle JT, Thomas PP, Reynolds JJ 1994 Metalloproteinase production by rabbit articular cartilage: comparison of the effects of interleukin-1 alpha in vitro and in vivo.. Virchows Arch 425: 413–424
Cawston TE, Galloway WA, Mercer E, Murphy G, Reynolds JJ 1981 Purification of rabbit bone inhibitor of collagenase. Biochem J 195: 159–165
Sasaki K, Hattori T, Fujisawa T, Takahashi K, Inoue H, Takigawa M 1998 Nitric oxide mediates interleukin-1-induced gene expression of matrix metalloproteinases and basic fibroblast growth factor in cultured rabbit articular chondrocytes. J Biochem (Tokyo) 123: 431–439
Iannone F, Lapadula G 2003 The pathophysiology of osteoarthritis. Aging Clin Exp Res 15: 364–372
Amin AR, Attur M, Abramson SB 1999 Nitric oxide synthase and cyclooxygenases: distribution, regulation, and intervention in arthritis. Curr Opin Rheumatol 11: 202–209
McInnes IB, Leung BP, Field M, Wei XQ, Huang FP, Sturrock RD, Kinninmonth A, Weidner R, Mumford R, Liew FY 1996 Production of nitric oxide in the synovial membrane of rheumatoid and osteoarthritis patients. J Exp Med 184: 1519–1524
Kahle P, Saal JG, Schaudt K, Zacher J, Fritz P, Pawelec G 1992 Determination of cytokines in synovial fluids: correlation with diagnosis and histomorphological characteristics of synovial tissue. Ann Rheum Dis 51: 731–734
Giannelli G, Erriquez R, Iannone F, Marinosci F, Lapadula G, Antonaci S 2004 MMP-2, MMP-9, TIMP-1 and TIMP-2 levels in patients with rheumatoid arthritis and psoriatic arthritis. Clin Exp Rheumatol 22: 335–338
Masuhara K, Nakai T, Yamaguchi K, Yamasaki S, Sasaguri Y 2002 Significant increases in serum and plasma concentrations of matrix metalloproteinases 3 and 9 in patients with rapidly destructive osteoarthritis of the hip. Arthritis Rheum 46: 2625–2631
Lotito AP, Muscara MN, Kiss MH, Teixeira SA, Novaes GS, Laurindo IM, Silva CA, Mello SB 2004 Nitric oxide-derived species in synovial fluid from patients with juvenile idiopathic arthritis. J Rheumatol 31: 992–997
Schlaak JF, Pfers I, Meyer Zum Buschenfelde KH, Marker-Hermann E 1996 Different cytokine profiles in the synovial fluid of patients with osteoarthritis, rheumatoid arthritis and seronegative spondylarthropathies. Clin Exp Rheumatol 14: 155–162
Acknowledgements
The authors wish to thank Yi Ge and Scott Roger for expert technical assistance, and Patty O'Donnell and Karyn J. Cullen for animal care and postmortem tissue collection
Author information
Authors and Affiliations
Corresponding author
Additional information
NIH grant RO1 DK 25759 and a grant from the National MPS Society to CS.
Rights and permissions
About this article
Cite this article
Simonaro, C., D'Angelo, M., Haskins, M. et al. Joint and Bone Disease in Mucopolysaccharidoses VI and VII: Identification of New Therapeutic Targets and BioMarkers Using Animal Models. Pediatr Res 57, 701–707 (2005). https://doi.org/10.1203/01.PDR.0000156510.96253.5A
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/01.PDR.0000156510.96253.5A
This article is cited by
-
Comparison of growth dynamics in different types of MPS: an attempt to explain the causes
Orphanet Journal of Rare Diseases (2022)
-
Recent trends in mucopolysaccharidosis research
Journal of Human Genetics (2019)
-
Recommendations for the management of MPS VI: systematic evidence- and consensus-based guidance
Orphanet Journal of Rare Diseases (2019)
-
Growth patterns in children with mucopolysaccharidosis I and II
World Journal of Pediatrics (2015)
-
Pain: a prevalent feature in patients with mucopolysaccharidosis. Results of a cross‐sectional national survey
Journal of Inherited Metabolic Disease (2015)