Abstract
Background:
To assess trends in the distribution of patients for radical prostatectomy in Germany from 2006 to 2013 and the impact of robotic surgery on annual caseloads. We hypothesized that the advent of robotics and the establishment of certified prostate cancer centers caused centralization in the German radical prostatectomy market.
Methods:
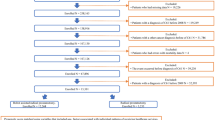
Using remote data processing we analyzed the nationwide German billing data from 2006 to 2013. We supplemented this database with additional hospital characteristics like the prostate cancer center certification status. Inclusion criteria were a prostate cancer diagnosis combined with radical prostatectomy. Hospitals with certification or a surgical robot in 2009 were defined as ‘early’ group. Linear covariant-analytic models were applied to describe trends over time.
Results:
Annual radical prostatectomy numbers declined from 28 374 (2006) to 21 850 (2013). High-volume hospitals (⩾100 cases) decreased from 87 (22.0%) in 2006 to 43 (10.4%) in 2013. Low-volume hospitals (<50 cases) increased from 193 (48.7%) to 280 (67.4%). Mean radical prostatectomy caseloads of hospitals with early vs without certification declined from 155 to 130 vs 77 to 39 (P=0.021 for trend comparison). Early robotic hospitals maintained their volume >200 cases per year contrary to the overall trend (P<0.001 for trend comparison). A multivariate model for caseload numbers of 2013 indicated a robotic system to be the most important factor for higher caseloads (multiplication factor 7.3; 95% confidence interval: 6.6–8.0). A prostate cancer center certification (multiplication factor 1.6; 95% confidence interval: 1.50–1.59) had a much smaller impact.
Conclusions:
We found decentralization of radical prostatectomy in Germany. The driving force for this development might consist in the overall decline of radical prostatectomy numbers. The most important factor for achieving higher caseloads was the presence of a robotic system. In order to optimize outcomes of radical prostatectomy additional health policy measures might be necessary.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Sriprasad S, Feneley MR, Thompson PM . History of prostate cancer treatment. Surg Oncol 2009; 18: 185–191.
Ritch CR, Graves AJ, Keegan KA, Ni S, Bassett JC, Chang SS et al. Increasing use of observation among men at low risk for prostate cancer mortality. J Urol 2015; 193: 801–806.
Trinh QD, Sammon J, Sun M, Ravi P, Ghani KR, Bianchi M et al. Perioperative outcomes of robot-assisted radical prostatectomy compared with open radical prostatectomy: results from the nationwide inpatient sample. Eur Urol 2012; 61: 679–685.
Basto M, Sathianathen N, Te Marvelde L, Ryan S, Goad J, Lawrentschuk N et al. Patterns-of-care and health economic analysis of robot-assisted radical prostatectomy in the Australian public health system. BJU Int 2015; 117: 930–939.
Hager B, Kraywinkel K, Keck B, Katalinic A, Meyer M, Zeissig SR et al. Integrated prostate cancer centers might cause an overutilization of radiotherapy for low-risk prostate cancer: a comparison of treatment trends in the United States and Germany from 2004 to 2011. Radiother Oncol 2015; 115: 90–95.
Huland H, Graefen M . Changing trends in surgical management of prostate cancer: The end of overtreatment? Eur Urol 2015; 68: 175–178.
Weeks WB, Paraponaris A, Ventelou B . Geographic variation in rates of common surgical procedures in France in 2008-2010, and comparison to the US and Britain. Health Policy 2014; 118: 215–221.
Chang SL, Kibel AS, Brooks JD, Chung BI . The impact of robotic surgery on the surgical management of prostate cancer in the USA. BJU Int 2015; 115: 929–936.
Barocas DA, Mitchell R, Chang SS, Cookson MS . Impact of surgeon and hospital volume on outcomes of radical prostatectomy. Urol Oncol 2010; 28: 243–250.
Gilbert SM, Dunn RL, Miller DC, Daignault S, Ye Z, Hollenbeck BK . Mortality after urologic cancer surgery: impact of non-index case volume. Urology 2008; 71: 906–910.
Hanchanale VS, McCabe JE, Javle P . Radical prostatectomy practice in England. Urol J 2010; 7: 243–248.
Cathcart P, Sridhara A, Ramachandran N, Briggs T, Nathan S, Kelly J . Achieving quality assurance of prostate cancer surgery during reorganisation of cancer services. Eur Urol 2015; 68: 22–29.
Holt P, Thompson MM . Centralisation: putting patients first. Eur J Vasc Endovasc Surg 2010; 40: 580–581.
National_Institute_for_Clinical_Excellence. Guidance on cancer services: improving outcomes in urological cancers. Treatment for specific cancers: prostate cancer 2002.
Fichtner J, Kowalski C, Wesselmann S, Albers P . [Indicator analysis of prostate cancer centers certified by the German Cancer Society 2015]. Urologe A 2015 54: 1530–1536.
Kalble T, Fichtner J . [Treatment quality of prostate cancer centers: Analysis of the 2014 annual report of the German Cancer Society]. Urologe A 2015; 54: 1523–1529.
Begg CB, Riedel ER, Bach PB, Kattan MW, Schrag D, Warren JL et al. Variations in morbidity after radical prostatectomy. N Engl J Med 2002; 346: 1138–1144.
Ellison LM, Heaney JA, Birkmeyer JD . The effect of hospital volume on mortality and resource use after radical prostatectomy. J Urol 2000; 163: 867–869.
Ramirez A, Benayoun S, Briganti A, Chun J, Perrotte P, Kattan MW et al. High radical prostatectomy surgical volume is related to lower radical prostatectomy total hospital charges. Eur Urol 2006; 50: 58–62 discussion 62-53.
Benchimol EI, Smeeth L, Guttmann A, Harron K, Moher D, Petersen I et al. The REporting of studies Conducted using Observational Routinely-collected health Data (RECORD) statement. PLoS Med 2015; 12: e1001885.
Hanchanale VS, Javle P . Impact of hospital provider volume on outcome for radical urological cancer surgery in England. Urol Int 2010; 85: 11–15.
Trinh QD, Bjartell A, Freedland SJ, Hollenbeck BK, Hu JC, Shariat SF et al. A systematic review of the volume-outcome relationship for radical prostatectomy. Eur Urol 2013; 64: 786–798.
Tilki D, Huland H, Graefen M . Centralization and quality control of elective surgery improve outcome: aren't we ethically obliged to force the pace of creating high-volume centers? Eur Urol 2015; 68: 30–31.
Ridic G, Gleason S, Ridic O . Comparisons of health care systems in the United States, Germany and Canada. Mater Sociomed 2012; 24: 112–120.
Huber J, Groeben C, Wirth MP, Hoffmann F . [Minimum caseload requirements in urologic oncology: not without evidence from health services research]. Urologe A 2014; 53: 1753–1757.
Peschke D, Nimptsch U, Mansky T . Achieving minimum caseload requirements—-an analysis of hospital discharge data from 2005-2011. Dtsch Arztebl Int 2014; 111: 556–563.
Acknowledgements
Data source: Research data centers of the federal and state statistical offices, DRG-statistics 2006 to 2013, own calculations. We thank Stefanie Uhrich for continuously supporting data retrieval. Funding: Med-Drive Grant of the medical faculty Carl Gustav Carus, TU Dresden.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Groeben, C., Koch, R., Baunacke, M. et al. Robots drive the German radical prostatectomy market: a total population analysis from 2006 to 2013. Prostate Cancer Prostatic Dis 19, 412–416 (2016). https://doi.org/10.1038/pcan.2016.34
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/pcan.2016.34
This article is cited by
-
Robotic-assisted surgery for prostatectomy – does the diffusion of robotic systems contribute to treatment centralization and influence patients’ hospital choice?
Health Economics Review (2023)
-
Hospital rating websites play a minor role for uro-oncologic patients when choosing a hospital for major surgery: results of the German multicenter NAVIGATOR-study
World Journal of Urology (2023)
-
Versorgungswirklichkeit der urologischen Endoprothetik in Deutschland von 2006 bis 2016
Der Urologe (2021)
-
Centralization tendencies of retroperitoneal lymph node dissection for testicular cancer in Germany? A total population-based analysis from 2006 to 2015
World Journal of Urology (2020)
-
Multicenter evaluation of guideline adherence for pelvic lymph node dissection in patients undergoing open retropubic vs. laparoscopic or robot assisted radical prostatectomy according to the recent German S3 guideline on prostate cancer
World Journal of Urology (2018)