Abstract
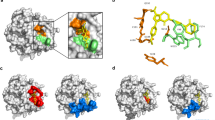
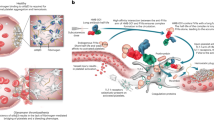
Inhibitors of coagulation factor Xa (fXa) have emerged as a new class of antithrombotics but lack effective antidotes for patients experiencing serious bleeding. We designed and expressed a modified form of fXa as an antidote for fXa inhibitors. This recombinant protein (r-Antidote, PRT064445) is catalytically inactive and lacks the membrane-binding γ-carboxyglutamic acid domain of native fXa but retains the ability of native fXa to bind direct fXa inhibitors as well as low molecular weight heparin–activated antithrombin III (ATIII). r-Antidote dose-dependently reversed the inhibition of fXa by direct fXa inhibitors and corrected the prolongation of ex vivo clotting times by such inhibitors. In rabbits treated with the direct fXa inhibitor rivaroxaban, r-Antidote restored hemostasis in a liver laceration model. The effect of r-Antidote was mediated by reducing plasma anti-fXa activity and the non–protein bound fraction of the fXa inhibitor in plasma. In rats, r-Antidote administration dose-dependently and completely corrected increases in blood loss resulting from ATIII-dependent anticoagulation by enoxaparin or fondaparinux. r-Antidote has the potential to be used as a universal antidote for a broad range of fXa inhibitors.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Lassen, M.R. et al. Rivaroxaban versus enoxaparin for thromboprophylaxis after total knee arthroplasty. N. Engl. J. Med. 358, 2776–2786 (2008).
Granger, C.B. et al. Apixaban versus warfarin in patients with atrial fibrillation. N. Engl. J. Med. 365, 981–992 (2011).
Weitz, J.I. et al. Randomised, parallel-group, multicentre, multinational phase 2 study comparing edoxaban, an oral factor Xa inhibitor, with warfarin for stroke prevention in patients with atrial fibrillation. Thromb. Haemost. 104, 633–641 (2010).
Connolly, S.J. et al. Apixaban in patients with atrial fibrillation. N. Engl. J. Med. 364, 806–817 (2011).
Chawla, L.S., Moore, G. & Seneff, M.G. Incomplete reversal of enoxaparin toxicity by protamine: implications of renal insufficiency, obesity, and low molecular weight heparin sulfate content. Obes. Surg. 14, 695–698 (2004).
Crowther, M.A. & Warkentin, T.E. Bleeding risk and the management of bleeding complications in patients undergoing anticoagulant therapy: focus on new anticoagulant agents. Blood 111, 4871–4879 (2008).
Crowther, M.A. & Warkentin, T.E. Managing bleeding in anticoagulated patients with a focus on novel therapeutic agents. J. Thromb. Haemost. 7 (suppl. 1), 107–110 (2009).
Bershad, E.M. & Suarez, J.I. Prothrombin complex concentrates for oral anticoagulant therapy-related intracranial hemorrhage: a review of the literature. Neurocrit. Care 12, 403–413 (2010).
Levi, M., Bijsterveld, N.R. & Keller, T.T. Recombinant factor VIIa as an antidote for anticoagulant treatment. Semin. Hematol. 41 (suppl. 1), 65–69 (2004).
Lauritzen, B. et al. Recombinant human factor VIIa and a factor VIIa-analogue reduces heparin and low molecular weight heparin (LMWH)-induced bleeding in rats. J. Thromb. Haemost. 6, 804–811 (2008).
Pryzdial, E.L. & Kessler, G.E. Kinetics of blood coagulation factor Xaα autoproteolytic conversion to factor Xaβ. Effect on inhibition by antithrombin, prothrombinase assembly, and enzyme activity. J. Biol. Chem. 271, 16621–16626 (1996).
Pryzdial, E.L. & Kessler, G.E. Autoproteolysis or plasmin-mediated cleavage of factor Xaα exposes a plasminogen binding site and inhibits coagulation. J. Biol. Chem. 271, 16614–16620 (1996).
Sinha, U. et al. Antithrombotic activity of PRT54021, a potent oral direct factor Xa inhibitor, can be monitored sing a novel prothrombinase inhibition bioassay. Blood 108 Abstract 907 (2006).
Perzborn, E. et al. In vitro and in vivo studies of the novel antithrombotic agent BAY 59–7939–an oral, direct Factor Xa inhibitor. J. Thromb. Haemost. 3, 514–521 (2005).
Pinto, D.J. et al. Discovery of 1-(4-methoxyphenyl)-7-oxo-6-(4-(2-oxopiperidin-1-yl)phenyl)-4,5,6,7-tetrahydro-1H -pyrazolo[3,4-c]pyridine-3-carboxamide (apixaban, BMS-562247), a highly potent, selective, efficacious, and orally bioavailable inhibitor of blood coagulation factor Xa. J. Med. Chem. 50, 5339–5356 (2007).
Sinha, U. et al. Expression, purification, and characterization of inactive human coagulation factor Xa (Asn322Ala419). Protein Expr. Purif. 3, 518–524 (1992).
Izaguirre, G. et al. Mechanism by which exosites promote the inhibition of blood coagulation proteases by heparin-activated antithrombin. J. Biol. Chem. 282, 33609–33622 (2007).
Mann, K.G. et al. Surface-dependent reactions of the vitamin K–dependent enzyme complexes. Blood 76, 1–16 (1990).
Huntington, J.A. Mechanisms of glycosaminoglycan activation of the serpins in hemostasis. J. Thromb. Haemost. 1, 1535–1549 (2003).
Olson, S.T., Bjork, I. & Bock, S.C. Identification of critical molecular interactions mediating heparin activation of antithrombin: implications for the design of improved heparin anticoagulants. Trends Cardiovasc. Med. 12, 198–205 (2002).
Andrassy, K., Eschenfelder, V. & Weber, E. Neutralization of the anticoagulant activity of low molecular weight heparin LU 47311 (Clivarin) in man by protamine chloride. Thromb. Res. 73, 85–93 (1994).
Bang, C.J., Berstad, A. & Talstad, I. Incomplete reversal of enoxaparin-induced bleeding by protamine sulfate. Haemostasis 21, 155–160 (1991).
Crowther, M.A. et al. Mechanisms responsible for the failure of protamine to inactivate low-molecular-weight heparin. Br. J. Haematol. 116, 178–186 (2002).
Dementiev, A. et al. The ternary complex of antithrombin-anhydrothrombin-heparin reveals the basis of inhibitor specificity. Nat. Struct. Mol. Biol. 11, 863–867 (2004).
Kuziej, J. et al. In vivo neutralization of unfractionated heparin and low-molecular-weight heparin by a novel salicylamide derivative. Clin. Appl. Thromb. Hemost. 16, 377–386 (2010).
Bianchini, E.P. et al. Development of a recombinant antithrombin variant as a potent antidote to fondaparinux and other heparin derivatives. Blood 117, 2054–2060 (2011).
Mega, J.L. et al. Rivaroxaban in patients with a recent acute coronary syndrome. N. Engl. J. Med. 366, 9–19 (2012).
Eerenberg, E.S. et al. Reversal of rivaroxaban and dabigatran by prothrombin complex concentrate: a randomized, placebo-controlled, crossover study in healthy subjects. Circulation 124, 1573–1579 (2011).
Smith, T.W. et al. Reversal of advanced digoxin intoxication with Fab fragments of digoxin-specific antibodies. N. Engl. J. Med. 294, 797–800 (1976).
Carothers, A.M. et al. Structure of the dihydrofolate reductase gene in Chinese hamster ovary cells. Nucleic Acids Res. 11, 1997–2012 (1983).
Carothers, A.M. et al. Splicing mutations in the CHO DHFR gene preferentially induced by (+/−)-3 α,4 β-dihydroxy-1 α,2 α-epoxy-1,2,3,4- tetrahydrobenzo[c]phenanthrene. Proc. Natl. Acad. Sci. USA 87, 5464–5468 (1990).
Di Scipio, R.G., Hermodson, M.A. & Davie, E.W. Activation of human factor X (Stuart factor) by a protease from Russell's viper venom. Biochemistry 16, 5253–5260 (1977).
Paolucci, F. et al. Fondaparinux sodium mechanism of action: identification of specific binding to purified and human plasma-derived proteins. Clin. Pharmacokinet. 41 (suppl. 2), 11–18 (2002).
Godier, A. et al. Evaluation of prothrombin complex concentrate and recombinant activated factor VII to reverse rivaroxaban in a rabbit model. Anesthesiology 116, 94–102 (2012).
Dejana, E., Villa, S. & de Gaetano, G. Bleeding time in rats: a comparison of different experimental conditions. Thromb. Haemost. 48, 108–111 (1982).
Author information
Authors and Affiliations
Contributions
G. Lu, S.J.H. and U.S. conceived of the study, designed experiments and wrote the manuscript. G. Lu, F.R.D., M.J.K., K.A., G. Lee, P.L., A.H. and M.I. designed and conducted experiments. P.B.C. discussed and interpreted data with G. Lu, M.J.K. and P.L. D.R.P. provided expertise, designed experiments and interpreted data.
Corresponding author
Ethics declarations
Competing interests
G. Lu, F.R.D., S.J.H., M.J.K., K.A., G. Lee, P.L., A.H., M.I., P.B.C., D.R.P. and U.S. are current or former employees of Portola Pharmaceuticals Inc.
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–4 (PDF 316 kb)
Rights and permissions
About this article
Cite this article
Lu, G., DeGuzman, F., Hollenbach, S. et al. A specific antidote for reversal of anticoagulation by direct and indirect inhibitors of coagulation factor Xa. Nat Med 19, 446–451 (2013). https://doi.org/10.1038/nm.3102
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nm.3102
This article is cited by
-
Update der Point-of-care-basierten Gerinnungstherapie
Die Anaesthesiologie (2024)
-
An update on applications and limitations of direct oral anticoagulants
The Egyptian Journal of Internal Medicine (2023)
-
The methods for removal of direct oral anticoagulants and heparins to improve the monitoring of hemostasis: a narrative literature review
Thrombosis Journal (2023)
-
Andexanet alfa versus four-factor prothrombin complex concentrate for the reversal of apixaban- or rivaroxaban-associated intracranial hemorrhage: a propensity score-overlap weighted analysis
Critical Care (2022)
-
A DNA origami-based aptamer nanoarray for potent and reversible anticoagulation in hemodialysis
Nature Communications (2021)