Abstract
Objective:
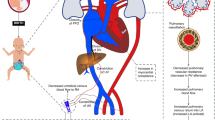
The objective of the study was to study the effect of short-term left-lateral position on cardiovascular parameters in hemodynamically stable newborns.
Study Design:
Cardiac output (CO), stroke volume (SV), systemic vascular resistance index (SVRI) and heart rate (HR) were measured by electric velocimetry in hemodynamically stable newborns without respiratory support in the supine, left-lateral and back-to-supine positions, each kept for 10 min.
Results:
Thirty-two newborns were enrolled, birth weight 2134 (1818 to 2460) g, gestational age 34.5±2.4 weeks. CO and SV decreased significantly from supine to left-lateral position (CO supine: 193.4 (168.0 to 229.6) ml kg−1min−1; CO left-lateral: 172.0 (154.9 to 201.6) ml kg−1min−1, P<0.0001; SV supine: 3.0 (2.7 to 4.0) ml; SV left-lateral: 2.7 (2.4 to 3.2) ml, P<0.0004). Conversely, SVRI increased in left-lateral position: SVRI supine: 18865±9244 dyns cm−5 m−2; SVRI left-lateral: 21203±10059 dyns cm−5 m−2, P<0.0001). All variables returned to the initial value when infants were back in the supine position. HR and blood pressure did not change.
Conclusion:
In stable infants, CO and SV decrease and SVRI increases, in left-lateral position.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Gouna G, Rakza T, Kuissi E, Pennaforte T, Mur S, Storme L . Positioning effects on lung function and breathing pattern in premature newborns. J Pediatr 2013; 162: 1133–1137.
Grenier IR, Bigsby R, Vergara ER, Lester BM . Comparison of motor self-regulatory and stress behaviors of preterm infants across body positions. Am J Occup Ther 2003; 57: 289–297.
Ewer AK, James ME, Tobin JM . Prone and left lateral positioning reduce gastro-oesophageal reflux in preterm infants. Arch Dis Child Fetal Neonatal Ed 1999; 81: F201–F205.
Corvaglia L, Rotatori R, Ferlini M, Aceti A, Ancora G, Faldella G . The effect of body positioning on gastroesophageal reflux in premature infants: evaluation by combined impedance and pH monitoring. J Pediatr 2007; 151: 591–596.
Stenke E, Kieran EA, McCarthy LK, Dawson JA, Van Vonderen JJ, Kamlin CO et al. A randomised trial of placing preterm infants on their back or left side after birth. Arch Dis Child Fetal Neonatal Ed 2016; 101: F397–F400.
Task Force on Sudden Infant Death Syndrome Task Force on Sudden Infant Death Syndrome, Moon RY . SIDS and other sleep-related infant deaths: expansion of recommendations for a safe infant sleeping environment. Pediatrics 2011; 128: 1030–1039.
de Boode WP . Cardiac output monitoring in newborns. Early Hum Dev 2010; 86: 143–148.
Osthaus WA, Huber D, Beck C, Winterhalter M, Boethig D, Wessel A et al. Comparison of electrical velocimetry and transpulmonary thermodilution for measuring cardiac output in piglets. Paediatr Anaesth 2007; 17: 749–755.
Norozi K, Beck C, Osthaus WA, Wille I, Wessel A, Bertram H . Electrical velocimetry for measuring cardiac output in children with congenital heart disease. Br J Anaesth 2008; 100: 88–94.
Zoremba N, Bickenbach J, Krauss B, Rossaint R, Kuhlen R, Schälte G . Comparison of electrical velocimetry and thermodilution techniques for the measurement of cardiac output. Acta Anaesthesiol Scand 2007; 51: 1314–1319.
Noori S, Drabu B, Soleymani S, Seri I . Continuous non-invasive cardiac output measurements in the neonate by electrical velocimetry: a comparison with echocardiography. Arch Dis Child Fetal Neonatal Ed 2012; 97: F340–F343.
Grollmuss O, Demontoux S, Capderou A, Serraf A, Belli E . Electrical velocimetry as a tool for measuring cardiac output in small infants after heart surgery. Intens Care Med 2012; 38: 1032–1039.
Grollmuss O, Gonzalez P . Non-invasive cardiac output measurement in low and very low birth weight infants: a method comparison. Front Pediatr 2014; 2: 16.
Torigoe T, Sato S, Nagayama Y, Sato T, Yamazaki H . Influence of patent ductus arteriosus and ventilators on electrical velocimetry for measuring cardiac output in very-low/low birth weight infants. J Perinatol 2015; 35: 485–489.
Song R, Rich W, Kim JH, Finer NN, Katheria AC . The use of electrical cardiometry for continuous cardiac output monitoring in preterm neonates: a validation study. Am J Perinatol 2014; 31: 1105–1110.
Ma M, Noori S, Maarek JM, Holschneider DP, Rubinstein EH, Seri I . Prone positioning decreases cardiac output and increases systemic vascular resistance in neonates. J Perinatol 2015; 35: 424–427.
Osypka MJ, Bernstein DP . Electrophysiologic principles and theory of stroke volume determination by thoracic electrical bioimpedance. AACN Clin Issues 1999; 10: 385–399.
Hsu KH, Wu TW, Wang YC, Lim WH, Lee CC, Lien R . Hemodynamic reference for neonates of different age and weight: a pilot study with electrical cardiometry. J Perinatol 2016; 36: 481–485.
Fujita M, Miyamoto S, Tambara K, Budgell B . Trepopnea in patients with chronic heart failure. Int J Cardiol 2002; 84: 115–118.
Kamenik M . The influence of left lateral position on cardiac output changes after head up tilt measured by impedance cardiography. J Clin Monit Comput 1999; 15: 519–523.
Bembich S, Oretti C, Travan L, Clarici A, Massaccesi S, Demarini S . Effects of prone and supine position on cerebral blood flow in preterm infants. J Pediatr 2012; 160: 162–164.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Paviotti, G., Todero, S. & Demarini, S. Cardiac output decreases and systemic vascular resistance increases in newborns placed in the left-lateral position. J Perinatol 37, 563–565 (2017). https://doi.org/10.1038/jp.2016.251
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2016.251