Abstract
Objective:
To describe the characteristics of small for gestational age (SGA) and non-SGA infants with bronchopulmonary dysplasia (BPD) and to ascertain whether respiratory outcomes and health-care utilization patterns in these two populations differ.
Study Design:
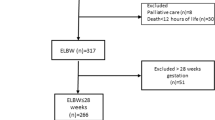
Three hundred and twenty-five infants with BPD born at <32 weeks gestation were recruited in the outpatient setting. Sociodemographic data and indicators of respiratory morbidity were collected via questionnaire and retrospective chart review.
Result:
SGA infants were on average 1 month older than non-SGA infants at discharge from the neonatal intensive care unit and were more likely to have a weight less than 10th percentile at first clinic visit. History of SGA was associated with increased risk of emergency department visits as well as with caregiver perception of poor weight gain.
Conclusion:
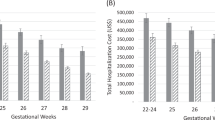
SGA status in infants with BPD is associated with increased health-care utilization, including length of initial hospitalization and emergency department visits.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Horbar JD, Badger GJ, Carpenter JH, Fanaroff AA, Kilpatrick S, LaCorte M, et al. Trends in mortality and morbidity for very low birth weight infants, 1991–1999. Pediatrics 2002; 110 (1): 143–151.
Berger TM, Bachmann II, Adams M, Schubiger G . Impact of improved survival of very low-birthweight infants on incidence and severity of bronchopulmonary dysplasia. Biol Neonate 2004; 86 (2): 124–130.
Northway WH, Rosan RC, Porter DY . Pulmonary disease following respiratory therapy of hyaline membrane disease: bronchopulmonary dysplasia. N Engl J Med 1967; 276: 357–368.
Regev RH, Reichman B . Prematurity and intrauterine growth retardation—double jeopardy? Clin Perinatol 2004; 453–473.
Jobe AH, Bancalari E . NICHD/NHLBI/ORD Workshop Summary: Bronchopulmonary Dysplasia. Am J Respir Crit Care Med 2001; 163: 1723–1729.
Ehrenkranz RA, Walsh MC, Vohr BR, Jobe AH, Wright LL, Fanaroff AA, et al. Validation of the National Institutes of Health Consensus Definition of Bronchopulmonary Dysplasia. Pediatrics 2005; 116 (6): 1353–1360.
Lal MK, Manktelow BN, Draper ES, Field DJ . Chronic lung disease of prematurity and intrauterine growth retardation: a population-based study. Pediatrics 2003; 111 (3): 483–487.
Egreteau L, Pauchard JY, Semama DS, Matis J, Liska A, Romeo B, et al. Chronic oxygen dependency in infants born at less than 32 weeks’ gestation: incidence and risk factors. Pediatrics 2001; 108 (2): E26.
Cooke RW . Conventional birth weight standards obscure fetal growth restriction in preterm infants. Arch Dis Child Fetal Neonatal Ed 2007; 92: F189.
Joyce BJ, Louey S, Davey MG, Cock ML, Hooper SB, Harding R . Compromised respiratory function in postnatal lambs after placental insufficiency and intrauterine growth restriction. Pediatr Res 2001; 50 (5): 641–649.
Maritz GS, Cock ML, Louey S, Suzuki K, Harding R . Fetal growth restriction has long-term effects on postnatal lung structure in sheep. Pediatr Res 2004; 55 (2): 287–295.
Rozance PJ, Seedorf GJ, Brown A, Roe G, O’Meara MC, Gien J, et al. Intrauterine growth restriction decreases pulmonary alveolar and vessel growth and causes pulmonary artery endothelial cell dysfunction in vitro in fetal sheep. Am J Physiol Lung Cell Mol Physiol 2011; 301: L860–L871.
Bose C, Van Marter LJ, Laughon M, O’Shea TM, Allred EN, Karna P, et al. Fetal growth restriction and chronic lung disease among infants born before the 28th week of gestation. Pediatrics 2009; 124 (3): e450–e458.
Klinger G, Sirota L, Lusky A, Reichman B . Bronchopulmonary dysplasia in very low birth weight infants is associated with prolonged hospital stay. J Perinatol 2006; 26: 640–644.
Greenough A, Limb E, Marston L, Marlow N, Calvert S, Peacock J . Risk factors for respiratory morbidity in infancy after very premature birth. Arch Dis Child Fetal Neonatal Ed 2005; 90: F320–F323.
Greenough A, Cox S, Alexander J, Lenney W, Turnbull F, Burgess S, et al. Health care utilisation of infants with chronic lung disease, related to hospitalisation for RSV infection. Arch Dis Child 2001; 85: 463–468.
Oken E, Kleinman KP, Rich-Edwards J, Gillman MW . A nearly continuous measure of birth weight for gestational age using a United States national reference. BMC Pediatr 2003; 3: 6.
Wang LY, Luo HJ, Hsieh WS, Hsu CH, Hsu HC, Chen PS, et al. Severity of bronchopulmonary dysplasia and increased risk of feeding desaturation and growth delay in very low birth weight preterm infants. Pediatr Pulmonol 2010; 45: 165–173.
Bernstein IM, Horbar JD, Badger GJ, Ohlsson A, Golan A . Morbidity and mortality among very-low-birthweight neonates with intrauterine growth restriction. Am J Obstet Gynecol 2000; 182 (1,part 1): 198–206.
Padula MA, Grover TR, Brozanski B, Zaniletti I, Nelin LD, Asselin JM, et al. Therapeutic interventions and short-term outcomes for infants with severe bronchopulmonary dysplasia born at <32 weeks’ gestation. J Perinatol 2013; 33(11): 877–881.
Acknowledgements
This work was funded by the Thomas Wilson Foundation, the Flight Attendant Medical Research Institute and the American Academy of Pediatrics Julius B Richmond Center. We thank the patients and families who participated in this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Johnson, J., Ryan, T., Aherrera, A. et al. The influence of small for gestational age status on outpatient bronchopulmonary dysplasia outcomes. J Perinatol 35, 72–76 (2015). https://doi.org/10.1038/jp.2014.142
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2014.142