Abstract
Gaucher disease (GD) is an inherited metabolic disorder that involves accumulation of glycolipid glucocerebroside in monocyte–macrophage cells, which can result in multiple organ damage. Enzyme replacement and substrate reduction therapies have improved the potential for early diagnosis and treatment. Determining the true incidence of this rare disease is critical for relevant policy establishment. Newborn screening allows for early diagnosis and an comparatively accurate incidence of GD. A fluorometric method to detect acid β-glucocerebrosidase (GBA) activity on a dried blood spot punch was developed. Validity and feasibility of the fluorometric method was demonstrated by examining 116 healthy controls, 19 confirmed GD patients and 19 obligate carriers. GBA activity was measured on dried blood spots of 80 855 newborns. Samples from positively screened newborns were reanalyzed by a leukocyte GBA activity test and GBA gene analysis. Plasma glucosylsphingosine level was determined as a biomarker of the pathophysiology of GD. GD patients were distinguished from healthy controls and obligate carriers using the fluorometric method. Mean GBA activity in newborn screening specimens was 145.69±44.76 μmol l−1 h−1 (n=80 844). Three children had low GBA activity, of which one child had low GBA activity on the second dried blood spot specimen. Leukocyte, genetic and biomarker analysis confirmed the diagnosis and indicated that this child was in the early stages of GD. In conclusion, the incidence of GD in Shanghai of China is approximately 1 in 80 855. Screening for GD by fluorometric analysis of GBA activity is an efficient and feasible technology in newborns.
Similar content being viewed by others
Introduction
Gaucher disease (GD) is an inherited metabolic disorder that results from deficiency of acid β-glucocerebrosidase (GBA, EC 3.2.1.45). Progressive accumulation of glycolipid glucocerebroside, which would otherwise be decomposed by GBA, can occur in the monocyte–macrophage cells throughout the body and results in multiple organ damage.1 Patients with GD exhibit a broad range of phenotypes and cases were conventionally divided into three main forms based on the severity of neurological presentations.2 Type I is chronic and non-neuropathic and accounts for the majority of GD cases. Type II is the rarest form with severe and rapid progressive neurological involvement. Type III is a less acute form with slowly progressive neurological presentations.2 The incidence of GD varies in different ethnic populations and is estimated to be 1/20 000–1/200 000 in the general population.3 However, it has a much higher incidence in the Ashkenazi Jewish population, where the incidence reaches to 1/1000–12 000.4
The GBA gene is located on chromosome 1q21 and consists of 11 exons and 10 introns.1 A nonfunctional pseudogene GBAP is located 16 000 bp downstream of the functional GBA gene and they share 96% exonic homology.5 More than 440 different mutations, including missense mutations, small insertions, deletions, as well as recombinations between GBA and GBAP, have been reported in the Human Gene Mutation Database.
Treatment of GD usually aims directly at symptomatic care of secondary complications. However, enzyme replacement therapy, substrate reduction therapy and hematopoietic stem cell transplantation therapy have made GD etiologically treatable with the exception of the neurological deterioration associated with types II and III.6, 7 Three enzyme replacement therapy products, imiglucerase, velaglucerase and taliglucerase, have already been approved for commercial use by the American Food and Drug Administration.6 As some of the damage is irreversible, treatment may be more effective when started earlier, even at an asymptomatic stage, especially for GD type I.8 Thus, presymptomatic diagnosis and early treatment of GD are of high importance. Some countries have already incorporated GD into newborn screening by tandem mass spectrometry (MS/MS).9, 10, 11, 12 However, due to its heterogeneous nature, newborn screening for GD has raised ethical concerns, for example, treatment challenge for a late-onset phenotype, implications of being a carrier of Gaucher.9, 13 More data in this field are critical.
Standard diagnostic procedures of GD include measurement of GBA activity, genetic analysis, as well as detection of biomarkers such as chitotriosidase, chemokine (C-C motif) ligand 18 (CCL18) and glucosylsphingosine.14 Early diagnosis of GD may be promoted through suitable techniques. Nestor Chamoles and his group developed the use of artificial fluorescent 4-methylumbelliferone-tagged (4-MU-tagged) substrates for analysis of lysosomal enzymes in dry blood spots (DBSs). This fluorometric method dependably and sensitively measured GBA activities in DBS and reliably differentiated GD patients from healthy newborns.15, 16
Although a newborn screening study for GD by MS/MS had been reported in Taiwan, the incidence and prevalence of GD in mainland China is unknown.12 A large-scale newborn screening of GD by fluorometric assay is absent although limited-scale screening on high-risk population has achieved success.17 The fluorometric assay has been successfully applied to newborn screening for Pompe disease, Fabry disease and mucopolysachridosis type I.18, 19, 20 In this study, we investigated a large sample size of newborn screening for GD using a modified fluorometric method. Our objective was to evaluate the utility of this fluorometric method for the detection of GBA activity on DBS of newborns and to explore the incidence of GD in the Chinese neonatal population.
Materials and methods
Study population and sample preparation
DBS samples from 116 healthy individuals (2–46 years old), 19 previously diagnosed GD patients (6 months to 14 years old) and 19 obligate carriers (20–50 years old) were collected to validate the fluorometric method. A total of 80 855 DBSs from newborns were provided by the Neonatal Screening Center of Shanghai China. Blood samples were recommended to be collected on filter paper after the third day of life and dried at room temperature for at least 4 h. Filter paper was sealed in a plastic bag and stored desiccated at 4 °C for 1 week and −20 °C for longer periods. Suspected results were retested in duplicates and positive cases were confirmed by GBA activity in leukocytes and GBA gene analysis.
DBS test
GBA activity was measured by modifying the method proposed by Chamoles et al.15 One 3 mm diameter blood spot (approximately 3.2 μl) from each DBS sample was punched into 96-well polystyrene plates (Corning, Corning, NY, USA) using a DBS Puncher. Each plate contained at least two blank filter papers. We prepared 0.2 mol l−1 citrate-phosphate buffer (pH 5.2, containing 0.9% taurodeoxycholate and 0.15% Triton-X 100) as elution buffer. Fifty microliters of 5 mmol l−1 4-methyl-umbelliferyl-β-d-glucopyranoside distilled in the elution buffer as a substrate was added to each well. Plates were sealed with an adhesive film (Corning) and incubated (400 r.p.m. shaking, 37 °C, 20 h; Labsystems iEMS, Finland). The seal was removed and the reaction was stopped with 200 μl glycine-carbonate buffer (0.17 mol l−1, pH 10.5). Samples (200 μl) were transferred to a new 96-well polystyrene plate to avoid interference of the filter paper with fluorescence. Fluorescence was detected in a Wallac 1420 victor2 microplate reader (excitation 355 nm, emission 460 nm; Perkin Elmer, Waltham, MA, USA). After correcting readings with blanks, we used the 4-MU calibration curve to convert fluorescence readings into moles of 4-MU. Enzymatic activity was expressed as micromoles of 4-MU hydrolyzed substrate per liter of blood per hour. Reagents used above were obtained from Sigma (St Louis, MO, USA).
Quality control and data analysis
Inter- and intra-assay precisions were calculated by performing three quality controls from US Centers for Disease Control and Prevention that showed low, medium and high enzyme activity. We determined intra-assay precision by measuring five punches of each control in one day. We calculated inter-assay precision by collecting enzyme activity of each control on five consecutive days. We judged the validity of our test by using enzyme activities of quality controls. All data were analyzed with SPSS (version 19, IBM, Armonk, NY, USA).
Leukocyte GBA activity
GBA activity in leukocytes was measured with an artificial fluorogenic substrate 4-methyl-umbelliferyl-β-d-glucopyranoside, as described previously.21 Leukocytes were isolated from fresh heparinized blood and protein concentration of homogenate was determined by the method of Lowry et al.22 We added the substrate to the 0.2 mol l−1 citrate-phosphate buffer (pH 5.8, containing 0.3% sodium taurocholate and 0.15% Triton-X 100) to achieve a final concentration of 5 mmol l−1. A mixture of 20 μl substrate and 10 μl homogenate was incubated at 37 °C for 2 h. We then added 200 μl glycine-carbonate buffer (0.17 mol l−1, pH 10.5) to stop the reaction. Fluorescence was measured (excitation 355 nm, emission 460 nm) and GBA activity was expressed as nmol h−1 per mg protein.
Sequence analysis
Genomic DNA was isolated from peripheral blood using an e.Z.N.A. blood DNA Kit (OMEGA, Norwalk, CA, USA) according to the manufacturer’s instructions. In order to amplify the functional GBA gene without amplifying the pseudogene GBAP, we used the nested polymerase chain reaction with appropriate primers, as described previously.23 Primer sequences are available upon request. PCR products were sequenced by Sangon Biotech (Shanghai, China). Data from Sanger sequencing were compared with the NCBI Reference Sequence NM_000157. PolyPhen-2 (http://genetics.bwh.harvard.edu/pph2/index.shtml) for amino acid substitution and MutationTaster (http://www.mutationtaster.org/) were applied to evaluate pathogenicity.
Plasma glucosylsphingosine level
Plasma glucosylsphingosine level was measured on an ultra performance liquid chromatography (UPLC) system with Xevo TQ-S detector (Waters, USA). Plasma samples were collected in EDTA tubes and stored frozen at −20 °C before analysis. Plasma sample (30 μl) was added to 120 μl of internal standard solution in a 1.5 ml vial. Samples were vortexed and centrifuged (13 300 r.p.m., 5 min), and then supernatant was transferred to a 96-well plate. Analytes were separated on an Acquity BEH C18 reversed phase column (column dimensions 2.1 × 50 mm, particle size 1.7 μm; Waters). Mass spectrometry was performed in the positive ionization mode using electrospray ionization source. The glucosylsphingosine standard and the internal standard were purchased from Matreya Inc. (Pleasant Gap, PA, USA). The normal range of glucosylsphingosine is 0.17–1.18 ng ml−1 (n=30, mean 0.58 ng ml−1).
Results
Precision analysis of enzyme assay with blood spots
Enzyme activities of quality controls provided by the Centers for Disease Control and Prevention were measured to calculate the precision of our experiment. Blank filter paper spots were used for background modification. The intra- and inter-assay coefficients of variation (CV) for GBA were in the range of 4.28–25.62% (Table 1), which was similar to the inter-assay CV of an MS/MS study.24
GBA activity in healthy controls, confirmed patients and obligate carriers
Overview of GBA activities in healthy individuals (n=116), confirmed patients (n=19) and obligate carriers (n=19) are shown in Figure 1 and Table 2. All patients with GD had GBA activities lower than those in healthy controls and obligate carriers. Our test was sensitive enough to distinguish GD patients from healthy volunteers.
Enzyme activities in dried blood spots among healthy controls, obligate carriers and confirmed patients. Boxes represent interquartile ranges. Top and bottom bars indicate limits of the ranges and central bars within the boxes represent median values. A full color version of this figure is available at the Journal of Human Genetics journal online.
GBA activity in newborn screening
We screened a total of 80 855 neonatal samples. We set our threshold for normal activity at 30.07 μmol h−1 l−1 based on the 0.01 percentile of 80 852 samples with removal of three samples of obviously abnormal low values (see below). Enzyme activity in healthy newborns was 145.69±44.76 μmol h−1l−1 (Table 2).
During the first screening, we detected enzyme activities below the threshold (30.07 μmol h−1 l−1) in 11 newborns. We retested these samples from the same DBS card and the enzyme activities were again low. Eight newborns were regarded as heterozygous or as normal individuals with comparatively low GBA activities because their enzyme activities were in the range of obligate carriers as described in Figure 1, which were derived from 116 healthy individuals and 19 obligate carriers (Figure 2 and Table 2). Three samples, whose values were not included when calculating the threshold of normal newborns, were identified as disease-suspected newborns (Figure 2 and Table 2).
Enzyme activities in newborns. Dotted line represents threshold for normal activity. Boxes represent interquartile ranges. Top and bottom bars indicate limits of the ranges and central bars represent median values. A full color version of this figure is available at the Journal of Human Genetics journal online.
GBA activities in disease-suspected newborns
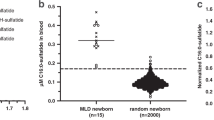
A second dried blood spot specimen was collected from three suspected newborns (Figure 3). Two of them had enzyme activities within the normal range, at 111.74 and 97.99 μmol h−1 l−1, and were considered false positives. The other sample had a GBA activity of 4.26 μmol h−1 l−1 on the second DBS card, and was highly suspected of being affected by GD.
Confirmatory tests
The GBA activity in peripheral leukocytes of this true positive individual was 2.64 nmol h−1 mg−1 of protein (normal range was 6.56–55.10 nmol h−1 mg−1 of protein). Through analysis of the GBA gene, one known mutation c.1448T>C (L483P) and one novel variation c.907C>A (L303I), inherited from each parent, were identified. L483P is a hot missense mutation in the Chinese population and its homoallelism may be associated with neurological symptoms.25 L303I was detected in trans with L483P, and was not found in 1000 Genomes or ExAC databases. Interestingly, two separate computational sources, PolyPhen-2 and MutationTaster, predicted that the L303I mutation is ‘possibly damaging’ and ‘disease-causing’, respectively. Furthermore, missense variants in the GBA gene often cause disease and the rate of benign missense variation is low.26 Based on this evidence, we concluded that L303I is likely pathogenic according to 2015 ACMG standards and guidelines.27
However, this true positive individual did not experience any clear clinical symptoms at 2 years old, such as hepatosplenomegaly or thrombocytopenia. The plasma glucosylsphingosine value was predicted to reflect GD pathophysiological impact on patients. While the plasma glucosylsphingosine values were 266.3±175 ng ml−1 (n=8) in adult type I GD patients and 4.65 ng ml−1 in this child, which is mildly yet significantly elevated compared with the normal range (0.17–1.18 ng ml−1). Therefore, this child was confirmed to have GD and should continue routine follow-up with a genetic metabolism clinic. The positive predictive value for GD in our screening was 33.33% (Figure 3).
Discussion
In this paper, we investigated the efficiency and validity of measuring the GBA activity on DBS using a fluorometric method. First, we used the technique to differentiate healthy volunteers from known carriers and GD patients. Second, we used the technique to screen a large population of newborns in mainland China and suspected one had GD. Based on the leukocyte GBA activity, GBA gene mutations and elevated plasma glucosylsphingosine level, we concluded that this child did have GD. One affected baby identified though this study demonstrated the feasibility of this fluorometric assay in newborn screening.
We began by comparing enzyme activities among healthy controls, previously confirmed GD patients and obligate carriers. Mean enzyme activity found in GD patients was significantly lower than those in healthy individuals. A clear separation between GD patients and healthy controls was evident. Thus, we suspected that the method has the potential to identify potential GD patients in a large population of newborns.
Obligate carriers had enzyme activities in a range that was lower than normal controls and higher than confirmed GD patients, generating a heterozygous range. Previous research concluded that normal newborns and obligate carriers could not be distinguished based on solely enzyme activity.15 Consistent with these previous reports, we found an overlap in the GBA activity reference range between normal newborns and obligate carriers of GBA gene mutations. However, GBA activities on DBS than were substantially lower in GD patients than in obligate carriers. Thus, the method we used is able to distinguish potential GD patients from heterozygous carriers, which could help us significantly decrease the recall rate.
A total of 80 855 newborns were screened over 12 months. To our knowledge, this is the largest screening of GD in mainland China. Considering the incidence of GD in other populations, including Taiwanese, we predicted the incidence of GD in mainland China would be below 1:10 000. Therefore, we set the threshold at 0.01 percentile (30.07 μmol h−1 l−1) to distinguish potential patients from normal newborns.
Out of 80 855 newborns, enzyme activities in 11 samples were below the threshold. Eight were suspected to be heterozygous carriers, as their GBA activities were within the range of obligate carriers (Figure 2 and Table 2). To decrease psychological burden incurred by retesting, we did not recall suspected carrier samples. The enzyme activities of the remaining three samples were 3.83, 2.94 and 5.34 μmol h−1 l−1, within the range generated from confirmed GD patients. Thus, only three newborns were suspected to be at risk of having GD and were retested. The recall rate was 0.0037% (3/80 855), which was significantly lower than those reported previously.9, 11, 12 After testing by other methods, only one patient was confirmed to have GD.
The reported incidence of GD is 1:103 134 in Taiwan, 1:17 368 in Australia and 1:13 341 in Hungary.9, 11, 12 In our study, we found an incidence of approximately 1:80 855 newborns in mainland China, which was lower than that in Australia and Hungary and similar to that in Taiwan.12
Over the past decade, MS/MS and digital microfluidics have been introduced into newborn screening programs in some countries.10, 11, 12, 28 However, MS/MS requires an additional mass spectrometry system and is technique-demanding and time-consuming. Digital microfluidics also requires specific equipment to run the assay. The fluorometric method used in our study could be easily applied to the general newborn screening laboratory. Additionally, the recall rate of our study had been decreased significantly compared with the MS/MS method in Taiwan and Hungary study.11, 12
One of the three cases reanalyzed had low GBA activity in leukocytes and two pathological mutations at the GBA gene, and was thus regarded as true positive case. We followed this patient for 2 years; however, no abnormal clinical manifestations, for example, hepatosplenomegaly, anemia and thrombocytopenia, was identified. Thus, a biochemical biomarker that reflects the pathophysiology of GD was measured to verify the diagnosis of GD. Plasma chitotriosidase and CCL18 levels are routine biomarkers used to support the diagnosis of GD. Patients with GD usually display increased chitotriosidase or CCL18 levels; however, elevated chitotriosidase and CCL18 have also been correlated with a variety of other diseases.14 Dekker et al.29 introduced glucosylsphingosine as a novel biomarker for GD, which not only correlates with a diagnosis of GD, but also reflects the progress of the disease. We detected mildly elevated glucosylsphingosine in the suspected GD patient, which supported his early GD diagnosis.
In this study, we had two false-positive cases. When we took their history, it was revealed that both of the false-positive patients experienced adverse events as newborns and had been cared for in neonatal critical care units for several days. The GBA enzyme on the blood cards may have been destroyed for unknown reasons before blood cards arrived at our newborn screening center.
In conclusion, the modified fluorometric assay is a reliable and practical method for GD newborn screening, which could be easily adopted by newborn screening laboratories. We obtained a comparatively accurate incidence of GD in mainland China using this method.
References
Mattosova, S., Chandoga, J., Hlavata, A., Saligova, J. & Macekova, D. Spectrum of GBA mutations in patients with Gaucher disease from Slovakia: identification of five novel mutations. Isr. Med. Assoc. J. 17, 166–170 (2015).
Mistry, P. K., Cappellini, M. D., Lukina, E., Ozsan, H., Mach Pascual, S., Rosenbaum, H. et al. A reappraisal of Gaucher disease-diagnosis and disease management algorithms. Am. J. Hematol. 86, 110–115 (2011).
Huang, W., Zhang, X. & Chen, W. Gaucher disease: a lysosomal neurodegenerative disorder. Eur. Rev. Med. Pharmacol. Sci. 19, 1219–1226 (2015).
Zhao, H., Keddache, M., Bailey, L., Arnold, G. & Grabowski, G. Gaucher’s disease: identification of novel mutant alleles and genotype-phenotype relationships. Clin. Genet. 64, 57–64 (2003).
Horowitz, M., Wilder, S., Horowitz, Z., Reiner, O., Gelbart, T. & Beutler, E. The human glucocerebrosidase gene and pseudogene: structure and evolution. Genomics 4, 87–96 (1989).
Rosenbloom, B. & Weinreb, N. Gaucher disease: a comprehensive review. Crit. Rev. Oncog. 18, 163–175 (2013).
Ito, S. & Barrett, A. J. Gauchers disease—a reappraisal of hematopoietic stem cell transplantation. Pediatr. Hematol. Oncol. 30, 61–70 (2013).
Desnick, R. & Schuchman, E. Enzyme replacement therapy for lysosomal diseases: lessons from 20 years of experience and remaining challenges. Annu. Rev. Genomics Hum. Genet. 13, 307–335 (2012).
Thomas, P., Susanne, S., Thomas, F., Víctor, R., Susanne, G., Arnold, P. et al. Neonatal screening for lysosomal storage disorders: feasibility and incidence from a nationwide study in Austria. Lancet 379, 335–341 (2012).
Han, M., Jun, S., Song, S., Park, K., Kim, J. & Song, J. Use of tandem mass spectrometry for newborn screening of 6 lysosomal storage disorders in a Korean population. Korean J. Lab. Med. 31, 250–256 (2011).
Wittmann, J., Karg, E., Turi, S., Legnini, E., Wittmann, G., Giese, A. et al. Newborn screening for lysosomal storage disorders in Hungary. JIMD Rep. 6, 117–125 (2012).
Liao, H. C., Chiang, C. C., Niu, D. M., Wang, C. H., Kao, S. M., Tsai, F. J. et al. Detecting multiple lysosomal storage diseases by tandem mass spectrometry—a national newborn screening program in Taiwan. Clin. Chim. Acta 431, 80–86 (2014).
Zimran, A., Altarescu, G. & Elstein, D. Screening for Gaucher disease: new challenges. Isr. Med. Assoc. J. 16, 723–724 (2014).
Rolfs, A., Giese, A., Grittner, U., Mascher, D., Elstein, D., Zimran, A. et al. Glucosylsphingosine is a highly sensitive and specific biomarker for primary diagnostic and follow-up monitoring in Gaucher disease in a non-Jewish, Caucasian cohort of Gaucher disease patients. J. Med. Genet. 8, e79732 (2013).
Chamoles, N. A., Blanco, M., Gaggioli, D. & Casentini, C. Gaucher and Niemann–Pick diseases—enzymatic diagnosis in dried blood spots on filter paper: retrospective diagnoses in newborn-screening cards. Clin. Chim. Acta 317, 191–197 (2002).
Olivova, P., Cullen, E., Titlow, M., Kallwass, H., Barranger, J., Zhang, K. et al. An improved high-throughput dried blood spot screening method for Gaucher disease. Clin. Chim. Acta 398, 163–164 (2008).
Herrera, D., Monaga, M., Campos, D., Pampin, Y., Gonzalez, E. C. & Lavaut, K. Ultramicro-fluorometric assay for the diagnosis of Gaucher disease in dried blood spots on filter paper. J. Neonatal Perinatal Med. 6, 61–67 (2013).
Chien, Y. H., Chiang, S. C., Zhang, X. K., Keutzer, J., Lee, N. C., Huang, A. C. et al. Early detection of Pompe disease by newborn screening is feasible: results from the Taiwan screening program. Pediatrics 122, e39–e45 (2008).
Spada, M., Pagliardini, S., Yasuda, M., Tukel, T., Thiagarajan, G., Sakuraba, H. et al. High incidence of later-onset fabry disease revealed by newborn screening. Am. J. Hum. Genet. 79, 31–40 (2006).
Lin, S. P., Lin, H. Y., Wang, T. J., Chang, C. Y., Lin, C. H., Huang, S. F. et al. A pilot newborn screening program for Mucopolysaccharidosis type I in Taiwan. Orphanet J. Rare Dis. 8, 147 (2013).
Chabás, A., Cormand, B., Grinberg, D., Burguera, J., Balcells, S., Merino, J. et al. Unusual expression of Gaucher’s disease: cardiovascular calcifications in three sibs homozygous for the D409H mutation. J. Med. Genet. 32, 740–742 (1995).
Lowry, O., Rosebrough, N., Farr, A. & Randall, R. Protein measurement with the Folin phenol reagent. J. Biol. Chem. 193, 265–275 (1951).
Jeong, S. Y., Park, S. J. & Kim, H. J. Clinical and genetic characteristics of Korean patients with Gaucher disease. Blood Cells Mol. Dis. 46, 11–14 (2011).
De Jesus, V., Zhang, X., Keutzer, J., Bodamer, O., Mühl, A., Orsini, J. et al. Development and evaluation of quality control dried blood spot materials in newborn screening for lysosomal storage disorders. Clin. Chem. 55, 158–164 (2009).
Tajima, A., Yokoi, T., Ariga, M., Ito, T., Kaneshiro, E., Eto, Y. et al. Clinical and genetic study of Japanese patients with type 3 Gaucher disease. Mol. Genet. Metab. 97, 272–277 (2009).
Montfort, M., Chabas, A., Vilageliu, L. & Grinberg, D. Functional analysis of 13 GBA mutant alleles identified in Gaucher disease patients: pathogenic changes and ‘modifier’ polymorphisms. Hum. Mutat. 23, 567–575 (2004).
Richards, S., Aziz, N., Bale, S., Bick, D., Das, S., Gastier-Foster, J. et al. Standards and guidelines for the interpretation of sequence variants: a joint consensus recommendation of the American College of Medical Genetics and Genomics and the Association for Molecular Pathology. Genet. Med. 17, 405–424 (2015).
Sista, R. S., Wang, T., Wu, N., Graham, C., Eckhardt, A., Bali, D. et al. Rapid assays for Gaucher and Hurler diseases in dried blood spots using digital microfluidics. Mol. Genet. Metab. 109, 218–220 (2013).
Dekker, N., van Dussen, L., Hollak, C., Overkleeft, H., Scheij, S., Ghauharali, K. et al. Elevated plasma glucosylsphingosine in Gaucher disease: relation to phenotype, storage cell markers, and therapeutic response. Blood 118, e118–e127 (2011).
Acknowledgements
Jiande Zhou in Shanghai Institute for Pediatric Research provided help in newborn recalling. This project is supported by NSFC (81570516, 81270936), Shanghai Municipal Education Commission-Gaofeng Clinical Medicine Grant Support (20152520) and Shanghai Science and Technology Committee (16JC1404600) to HZ.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Kang, L., Zhan, X., Gu, X. et al. Successful newborn screening for Gaucher disease using fluorometric assay in China. J Hum Genet 62, 763–768 (2017). https://doi.org/10.1038/jhg.2017.36
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jhg.2017.36
This article is cited by
-
Patient centered guidelines for the laboratory diagnosis of Gaucher disease type 1
Orphanet Journal of Rare Diseases (2022)
-
Ambroxol improves skeletal and hematological manifestations on a child with Gaucher disease
Journal of Human Genetics (2020)
-
A pilot screening of high-risk Gaucher disease children using dried blood spot methods in Shandong province of China
Orphanet Journal of Rare Diseases (2018)