Abstract
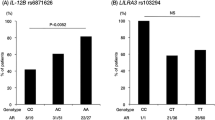
Chronic thromboembolic pulmonary hypertension (CTEPH) is characterized by pulmonary hypertension caused by thromboembolism of the pulmonary artery. Etiology of CTEPH may be heterogeneous and is largely unknown, but genetic factors are considered to be involved in the etiology. It has been reported that deep vein thrombosis (DVT) and/or coagulation factor variants are predisposing factors to CTEPH. However, more than half of the CTEPH patients, especially the Japanese, do not have prior DVT or coagulation abnormality, suggesting that there should be other risk factors for CTEPH. Moreover, there are several reports on the association between CTEPH and human leukocyte antigen (HLA). To further clarify the HLA-linked gene(s) controlling the susceptibility to CTEPH, 160 patients (99 without DVT and 61 with DVT) and 380 healthy controls were analyzed for polymorphisms in 15 microsatellite markers and 5 genes in the HLA region. We found a strong association of HLA markers with the DVT-negative CTEPH, DPB1*0202 (odds ratio (OR)=5.07, 95% confidence interval (CI)=2.52–10.19, P=0.00000075, corrected P-value (Pc)=0.00014), IKBL-p*03 (OR=2.33, 95% CI=1.49–3.66, P=0.00017, Pc=0.033) and B*5201 (OR=2.47, 95% CI=1.56–3.90, P=0.000086, Pc=0.016), whereas no significant association was observed for the DVT-positive CTEPH. The comparison of clinical characteristics of patients stratified by the presence of susceptibility genes implied that the DPB1 gene controlled the severity of the vascular lesion, whereas the IKBL gene (NFKBIL1) was associated with a relatively mild phenotype.
Similar content being viewed by others
Introduction
Chronic thromboembolic pulmonary hypertension (CTEPH) is characterized by persistent pulmonary embolism, which causes pulmonary hypertension and consequent right heart failure.1, 2, 3 CTEPH is a rare disease with an estimated annual incidence of 500–2500 patients in USA.2 It is further rare in Japan,4 where the prevalence of CTEPH was estimated to be 450 patients, which is about one-tenth of that in the United States (http://www.nanbyou.or.jp/sikkan/081.htm). It is accepted that continuous influx of venous thrombi mainly leads to the formation and progression of pulmonary thromboembolism, and that deep vein thrombosis (DVT) and/or coagulation factor variants are predisposing factors of CTEPH.1, 2, 3 From this point of view, anticoagulants are often prescribed to CTEPH patients, but the effect is not always sufficient for the prevention of disease progression. In addition, more than half of the patients do not show coincidence or apparent history of DVT. An especially lower prevalence rate of DVT in Japanese patients as compared with Caucasian patients (12–38% in Japan vs 35–45% in the United States) has been reported, implying the presence of different clinical categories, that is, DVT-positive CTEPH and DVT-negative CTEPH, and/or ethnic difference in the etiology of CTEPH.2, 4, 5, 6
The human leukocyte antigen (HLA) locus spans about 4 Mb on chromosome 6p21.3 and contains more than 200 genes, including genes for HLA molecules that are involved in the immune responsiveness to foreign and self-antigens.7, 8, 9 It is well known that HLA genes are highly polymorphic and their allelic distributions are different among different ethnic groups; diseases can be associated with different HLA alleles among different ethnic groups, and there is a possibility that the different HLA alleles may contribute to the difference in pathogenesis based on ethnicity.9, 10 Recently, de Bakker et al.11 reported a high-resolution single nucleotide polymorphism (SNP) mapping of the HLA region, which showed the ethnicity-specific complexity of HLA haplotypes.
It was reported that the circulating levels of monocyte chemoattractant protein-1, tumor necrosis factor α and interleukin-1β were high in CTEPH.12 In addition, several risk factors for CTEPH have been identified, including chronic inflammatory disorders, myeloproliferative syndromes and splenectomy.4, 13 These observations implied that inflammatory or immune-related mechanisms might be involved in the pathogenesis of CTEPH. In accordance with this hypothesis, HLA analyses had been done in patients with primary pulmonary hypertension, and it was reported that certain types of HLA antigens or HLA alleles, such as HLA-B35, -DR3, -DR6, -DR52, -DQ2 and -DQ7, were associated with the disease in Caucasoid populations.14, 15, 16, 17, 18 On the other hand, we reported significant associations of CTEPH with HLA-DPB1*0202 and B*5201 in the Japanese.19 These observations suggest that HLA-linked gene(s) may control the susceptibility to CTEPH. However, it remains to be clarified whether the HLA-linked gene(s) were related to the pathogenesis of CTEPH itself or to specific conditions of CTEPH, such as DVT. It is also unknown whether the reported disease-associated HLA class I (HLA-B) alleles and class II (HLA-DR, DQ, and DP) alleles contributed equally to the disease or whether they were simple reflections of linkage disequilibrium (LD) among the alleles of HLA genes or non-HLA genes.
To further clarify the HLA-linked susceptibility gene(s) involved in CTEPH, we analyzed a total of 160 patients (61 DVT-positive patients and 99 DVT-negative patients) and 380 controls for polymorphisms in the genetic markers distributed within the HLA region. We found that the association with HLA was confined to DVT-negative CTEPH, and that there were at least two different HLA-linked disease susceptibility genes for DVT-negative CTEPH.
Materials and methods
Subjects
We recruited CTEPH patients from Chiba University Hospital, National Cardiovascular Center, and Tohoku University Hospital. In addition to 80 patients (21 DVT-positive and 59 DVT-negatives) analyzed earlier for some HLA genes,19 80 patients (40 DVT-positive and 40 DVT-negative) were newly recruited in this study. Chronic pulmonary hypertension was defined as mean pulmonary artery pressure (Ppa) ⩾25 mm Hg, with normal wedge pressure in patients who had symptoms at least for 6 months.6, 19 Chronic thromboembolic findings were confirmed by pulmonary angiography.20 The disease could be divided into two categories, the central predominant type and the peripheral predominant type, according to the location of thrombi by angiographies and spiral computed tomography angiographies. The central predominant type was defined by the thrombi of lobar arteries or proximal location, whereas the peripheral predominant type was defined by the thrombi in segmental arteries or distal location.19 All patients were examined for DVT by contrast venography or venous ultrasonography. Three hundred and eighty unrelated healthy Japanese subjects (273 males and 107 females, age 35.5±1.5) selected at random from medical staff, students, or blood donors were used as controls. All patients and controls were residents of Honshu or Kyushu islands, two main islands of Japan, and it is well known that there is no significant difference in allele frequencies of genes in the HLA region among residents of four main islands in Japan.21, 22 It is also well known that there was no age-related or gender-related difference in the allele frequencies of HLA genes. Therefore, the control group was neither age-matched nor gender-matched to the patient groups. Allele frequencies of all tested markers in the control population were in Hardy–Weinberg equilibrium. Blood samples were derived from subjects after obtaining informed consent from them. The study protocol was approved by the Ethics Reviewing Committees of The Medical Research Institute of Tokyo Medical and Dental University, Chiba University School of Medicine, National Cardiovascular Center and Tohoku University School of Medicine.
HLA typing and microsatellite marker typing
Genomic DNA was obtained from peripheral leukocytes by using a QIAamp DNA blood minikit (Qiagen, Germany). Fifteen microsatellite markers in the HLA region, D6S1680, D6S439, TAP, DQCARII, DQCAR, D6S273, TNFd, TNFa, C1_2_A, MICA, MIB, C1_4_1, C1_2_5, C3_2_11, and D6S276, were described earlier.23, 24, 25 Polymorphisms of microsatellite markers were investigated using the fluorescence-conjugated PCR primer method, as reported earlier.24, 25 DNA typing of HLA-A, -B, and -DRB1 was carried out using the RELI-typing kit based on the sequence-specific oligonucleotide probe method (Dynal, Norway). DNA typing of HLA-DPB1 was done by the restriction enzyme fragment length polymorphism technique26, 27 using eight restriction enzymes, RsaI, Sau96I, BsrBI, DdeI, BsaJI, BssHII, SacI and BsgI, which enabled us to detect all the DPB1 alleles with allele frequencies >0.005 in the Japanese.21, 22 The promoter polymorphism of IKBL gene (IKBLp allele) located in the HLA class I and class III boundary regions was also analyzed as a genetic marker, as described earlier.28
Statistical analysis
Frequencies of alleles in the patients were compared with those in the controls. Odds ratio (OR) was calculated to evaluate the strength of association from a 2 × 2 contingency table, and the statistical significance was evaluated by chi-square test or Fisher’s exact test when it was appropriate. To reduce the statistical type 1 error, Bonferroni's correction was done; the corrected P-value (Pc) was calculated by multiplying the P-value by 191, which is the total number of alleles found in Japanese controls with frequencies of >0.005: HLA-A (n=9), -B (n=23), -DPB1 (n=15), -DRB1 (n=26), IKBLp (n=5), D6S1680 (di-nucleotide repeat, range 180–198, n=5), D6S439 (di-nucleotide repeat, range 274–288, n=4), TAP (di-nucleotide repeat, range 190–202, n=4), DQCARII (di-nucleotide repeat, range 185–207, n=9), DQCAR (di-nucleotide repeat, range 103–123, n=7), D6S273 (di-nucleotide repeat, range 126–136, n=5), TNFd (di-nucleotide repeat, range 126–138, n=6), TNFa (di-nucleotide repeat, range 95–119, n=8), C1_2_A (di-nucleotide repeat, range 236–256, n=10), MICA (tri-nucleotide repeat, range 179–194, n=5), MIB (di-nucleotide repeat, range 326–350, n=8), C1_4_1 (tetra-nucleotide repeat, range 213–229, n=5), C1_2_5 (di-nucleotide repeat, range 178–218, n=15), C3_2_11 (di-nucleotide repeat, range 197–229, n=14), and D6S276 (di-nucleotide repeat, range 198–226, n=8). A Pc <0.05 was considered to be significant. Values for clinical characteristics were compared between patient groups by Student’s unpaired t-test (two-tailed), with P-value <0.05 as a set point for significance. Linkage disequilibria among the disease-associated alleles were evaluated by pairwise D′ and r2 values calculated using the Haploview software (http://www.broad.mit.edu/mpg/haploview/index.php).
Results
Analysis of microsatellite markers in the HLA region
A total of 160 CTEPH patients were investigated in this study and they were divided into two groups according to the presence or absence of DVT. Demographic and clinical characteristics of the patients grouped by the presence or absence of DVT are shown in Table 1. Japanese patients showed dominance of the female and central predominant type, especially in DVT-negative CTEPH. These findings were consistent with the characteristics of Japanese patients reported earlier.4, 5, 19 When the clinical characteristics were compared between the DVT-positive patients and the DVT-negative patients, there was no statistically significant difference (Table 1).
First, we analyzed fifteen microsatellite markers in the HLA region. As our earlier study showed association of CTEPH with HLA-B and DPB1 alleles,19 microsatellite markers mapped within about 1 Mb from the HLA-B or DPB1 genes were selected (Figure 1). As shown in Table 2, there was no significant association between any alleles of the microsatellite markers and DVT-positive CTEPH. In clear contrast, we found definite associations in DVT-negative CTEPH; significant associations (Pc<0.05) were found with an allele of C1_2_A (allele *238, OR=2.77 and Pc=0.002) and an allele of C3_2_11 (*207, OR=2.51 and Pc=0.017). C1_2_A and C3_2_11 were mapped with the class III–class I boundary and the class I region, respectively (Figure 1), indicating at least one susceptibility gene within the class III or the class I region. In addition, other microsatellite markers, including TAP (allele*192, OR=2.04, P=0.004 and Pc=0.82) near the HLA-DPB1 gene and alleles of several microsatellite markers around the class III–class I boundary to the class I regions, TNFa (allele*119, OR=2.27, P=0.0004 and Pc=0.078), MIB (allele*326, OR=2.25, P=0.0011 and Pc=0.21), and C1_2_5 (allele*208, OR=2.14, P=0.0013 and Pc=0.25), showed marginal associations (P-value was <0.05, but it did not reach statistical significance after the Bonferroni’s correction of the P-value).
Schematic representation of genetic markers in the HLA region. Names and positions of fifteen microsatellite markers (upper panel) and five HLA markers (lower panel) analyzed for polymorphisms are schematically shown along with the approximate regions of class I, II and III. Arrows indicate the markers showing significant associations with DVT-negative CTEPH.
Analysis of genes in the HLA region
To further explore the susceptibility genes to the DVT-negative CTEPH, we investigated polymorphisms in the possible susceptibility genes: HLA-DPB1 in the DPB1 locus, NFKBIL1 in the class III–class I boundary region and HLA-B in the class I locus (Figure 1). In addition, HLA-DRB1 and HLA-A genes were analyzed as out-markers. As shown in Table 2, significant associations were observed with alleles of DPB1 (DPB1*0202, OR=5.07 and Pc=0.00014), NFKBIL1 (IKBLp*03, OR=2.33, and Pc=0.033) and HLA-B (B*5201, OR=2.47, and Pc=0.016). On the other hand, no significant association was observed with DRB1 and HLA-A genes, although a marginal association was found with DRB1*1502 (Table 2). This marginal association was considered to be a reflection of strong LD between DRB1*1502 and IKBLp*03 in the Japanese.28 In contrast, no association with any alleles of the HLA genes was observed with DVT-positive CTEPH, further indicating that there was no association between HLA and DVT-positive CTEPH (Table 2).
We found significant associations of DVT-negative CTEPH with DPB1*0202, IKBLp*03, C1_2_A*238, HLA-B*5201 and C3_2_11*207. As there was tight LD among the alleles of HLA and non-HLA genes in the HLA region, which extended over several mega-bases (Mb) in some haplotypes,11, 28 we have evaluated LD among these disease-associated alleles in the controls, DVT-negative patients and DVT-positive patients (Table 3). It was found that DPB1*0202 was not in LD with the other disease-associated alleles in both controls and patients (for example, between DPB1*0202 and IKBLp*03, D′=0.26 and r2=0.00 in controls, and D′=0.49 and r2=0.01 in DVT-negative patients). On the other hand, IKBLp*03, C1_2_A*238, B*5201 and C2_3_11*207 were in LD, albeit not strong, in both controls and patients. For example, LD values between the IKBLp*03 and C2_3_11*207, which were apart by 0.9 Mb (Figure 1), were D′=0.63 and r2=0.29 in controls and D′=0.73 and r2=0.40 in patients. Moreover, IKBLp*03 and B*5201 showed strong LD in both controls (D′=0.67 and r2=0.30) and patients (D′=1.00 and r2=0.76).
Owing to the strong LD, it was difficult to determine whether IKBLp*03 or B*5201 (or both of them) was primarily associated with the disease. In addition, haplotype analysis showed that IKBLp*03-B*5201 haplotype was associated with DVT-negative CTEPH (OR=2.75, 95% CI 1.76–4.30, and P=0.0000055). These HLA analyses showed that the susceptibility to DVT-negative CTEPH and not to DVT-positive CTEPH was related to the genes within the class II region (DPB1*0202) and the class III–class I boundary region (IKBLp*03 and/or B*5201).
When the frequencies of HLA markers were compared between DVT-negative and DVT-positive patients, IKBLp*03 showed a significant association (OR=3.68, P=0.0002 and Pc=0.04), whereas the associations with DPB1*0202 (OR=4.59, P=0.011 and Pc>0.05) and B*5201 (OR=3.79, P=0.0004 and Pc>0.05) were of marginal significance. The observations suggested that IKBLp*03 might be of larger contribution than B*5201 in controlling the susceptibility to DVT-negative CTEPH.
Analysis of clinical data in association with HLA
The HLA analyses showed that specific HLA alleles or haplotypes were associated with the susceptibility to DVT-negative CTEPH, suggesting that they could be used as markers to investigate the etiology and/or pathogenesis of the disease at least for the DVT-negative CTEPH. To analyze the possible difference in clinical phenotypes of CTEPH depending on these genetic markers, we compared the clinical characteristics of patients stratified by carrying or not carrying HLA-DPB1*0202 and/or IKBLp*03. In this analysis, we chose IKBLp*03 as a marker of the class III–class I boundary region, though we could not rule out the involvement of B*5201, as IKBLp*03 and B*5201 were in tight LD (Table 3). The clinical characteristic in each subgroup was statistically compared with that in the DVT-positive patients who carried neither HLA-DPB1*0202 nor IKBLp*03 as the reference.
As shown in Table 4, patients carrying HLA-DPB1*0202 but not IKBLp*03 (group 1) showed a significantly lower value of PaO2 and AaDO2, and a higher value of total pulmonary vascular resistance than the reference. On the other hand, patients carrying IKBL-p*03 but not DPB1*0202 (group 2) showed a significantly lower mean pulmonary artery pressure than the reference. Group 4 patients also showed a significantly lower value of arterial carbon dioxide tension (PaCO2) and larger AaDO2 than the reference. These observations suggested that DPB1*0202 was associated with the severity of vascular lesions, whereas IKBLp*03 was associated with relatively mild phenotypes.
Discussion
We earlier reported the significant association of CTEPH with alleles of two different HLA genes, DPB1*0202 and B*5201, in the Japanese.19 In addition, we showed that the CTEPH patients carrying HLA-B*5201 or HLA-DPB1*0202 had a low prevalence of DVT.19 On the other hand, earlier HLA studies in Caucasoid populations showed that some HLA alleles were associated with pulmonary arterial hypertension, but the results were not consistent with each other,14, 15, 16, 17, 18 implying that the observed associations with HLA were specific to the investigated ethnic groups because the complexity of HLA region depends on the nature of ethnic groups.11 It is also possible that these reports might be false-positive findings owing to the type I error in the statistical analyses, because none of the earlier studies was concerned about multiple testing. However, the possibility remains that the association with HLA might be confined to a specific category of CTEPH, because the etiology and pathogenesis of CTEPH were heterogeneous. In this study, we investigated HLA markers in patients with CTEPH stratified by the presence of DVT, that is, DVT-positive CTEPH and DVT-negative CTEPH. We first compared clinical characteristics between the DVT-positive and DVT-negative cases and found that there was no major difference in the clinical phenotypes.
The fact that significant association with HLA markers was observed for the DVT-negative and not for the DVT-positive CTEPH suggested that DVT-negative CTEPH was a characteristic clinical type under specific control by the HLA-linked susceptibility genes. The lack of association with HLA markers in the DVT-positive group might be because of the lack of statistical power to detect the association. However, power calculations under the condition using parameters obtained from our earlier study (frequency of high-risk DPB1 and HLA-B alleles were 0.18 and 0.39, whereas genotype-associated risks were 3.4 and 2.1, respectively, and the prevalence of disease was 0.0001)19 showed that the power was 0.77 (DPB1*0202) and 0.69 (B*5201). Therefore, although the statistical power was not low, we could not exclude the possibility of type I error in the detection of association between HLA and DVT-positive CTEPH. Further study with a large cohort of DVT-positive patients is required to obtain a definite conclusion about the lack of association.
We found significant association of DVT-negative CTEPH with alleles of HLA and non-HLA genes in the HLA region, suggesting that there were at least two susceptibility loci: one was the DPB1 locus and the other was near the class III–class I boundary. When the frequencies of the alleles in DVT-negative patients were compared with the controls, DPB1*0202, IKBL*03 and B*5201 showed significant association. In addition, when the comparison was made within the patient populations (between the DVT-negatives and DVT-positives), IKBLp*03 showed significant association even though the number of patients was not so large, implying that IKBLp*03 might be the primary allele within the class III–class I boundary that was associated with DVT-negative CTEPH. Nevertheless, DPB1*0202 and IKBLp*03 were used as the genetic markers to investigate the etiopathological mechanisms underlying the DVT-negative CTEPH, and stratification of CTEPH by these genetic markers implied that DPB1*0202 and IKBLp*03 contributed differently to the susceptibility.
As there was a gender difference in the susceptibility to CTEPH in the Japanese,4 and it was also true in our subjects as shown in Table 1, the association with HLA might depend on the gender. However, the frequencies of DPB1*0202 in DVT-negative CTEPH patients were 13/76 (17.1%) in females and 6/23 (26.1%) in males. Moreover, the frequencies of IKBLp*03 and B*5201 were 42/76 (55.3%) and 34/76 (44.7%) in female patients and 12/23 (52.2%) and 9/23 (39.1%) in male patients, respectively. In the control group, frequencies of DPB1*0202, IKBLp*03 and B*5201 were 6/148 (4.1%), 49/148 (33.1%) and 36/148 (24.3%) in females and 11/232 (4.7%), 80/232 (34.5%) and 60/232 (25.9%) in males, respectively. Therefore, the associations between DVT-negative CTEPH and DPB1*0202, IKBLp*03 or B*5201 could be slightly different in females (OR: 4.88, 3.27 and 2.52; P-value: 0.001, 0.0004 and 0.002, respectively) and males (OR: 7.15, 2.07 and 1.84, P-value: 0.00001, 0.09 and 0.17, respectively). It should be noted that the OR for DPB1*0202 was higher in males, whereas those for IKBLp*03 and B*5201 were higher in females, suggesting that the role of HLA-linked susceptibility gene(s) to DVT-negative CTEPH might be different between males and females.
To reveal the genetic contribution to disease, standard linkage analysis could be used successfully for simple Mendelian disorders. However, such a family-based linkage study was difficult to apply for multifactorial diseases, especially for rare diseases with possible heterogeneity in etiology, because multiplex families cannot be found easily and the disease status linked to specific loci cannot be defined clearly.29 One powerful strategy for mapping the susceptibility gene(s) in multifactorial diseases is the association study using multiple genetic markers including microsatellite markers and SNPs. We first used microsatellite markers to investigate the HLA-linked susceptibility loci. These microsatellite markers were used in earlier studies to discover the susceptibility loci of various diseases, including chronic rheumatoid arthritis,24, 30, 31 Takayasu arteritis,28, 32 and autoimmune pancreatitis,26 which suggested that these markers might capture specific haplotypes of HLA or non-HLA genes. However, because we investigated only 15 microsatellite markers, these markers might not be enough to capture all the susceptibility genes for DVT-negative CTEPH. Therefore, we cannot exclude the possibility that there may be additional susceptibility genes in the HLA region.
The HLA region contains a number of genes that control inflammation and immune responsiveness to antigens, which might be underlying the process of susceptibility to immune-related disorders.10, 33 The observation that the susceptibility genes to CTEPH were mapped within the HLA region suggested that the pathogenesis of DVT-negative , but not DVT-positive, CTEPH, was through an inflammatory process. As CTEPH occurred in the absence of DVT and could be coincident with anticardiolipin antibody syndrome, chronic inflammatory disorders, myeloproliferative syndromes and splenectomy,4, 12, 13 inflammation might be involved in the pathogenesis of CTEPH at least in part of the DVT-negative cases. A possibility that DVT-negative CTEPH patients had DVT in the acute phase, which was but resolved in the chronic phase, could not be excluded. However, it was speculated that inflammation-related genes might contribute to the persistence of thromboemboli attached to lesions of CTEPH in DVT-negative cases.
In conclusion, we showed that the association with HLA was confined to the DVT-negative CTEPH and that there were at least two different HLA-linked disease susceptibility genes for the DVT-negative CTEPH: one was within the DPB1 locus (DPB1*0202) and the other was mapped near the class III–class I boundary (presumably IKBLp*03).
References
Moser, K. M., Auger, W. R. & Fedullo, P. F. Chronic major-vessel thromboembolic pulmonary hypertension. Circulation 81, 1735–1743 (1990).
Fedullo, P. F., Auger, W. R., Kerr, K. M. & Rubin, L. J. Chronic thromboembolic pulmonary hypertension. N. Engl. J. Med. 345, 1465–1472 (2001).
Hoeper, M. H., Mayer, E., Simonneau, G. & Rubins, L. J. Chronic thromboembolic pulmonary hypertension. Circulation 113, 2011–2020 (2006).
Nakamura, M., Okada, O., Sakuma, M., Nakanishi, N., Miyahara, Y., Yamada, N. et al. Incidence and clinical characteristics of chronic pulmonary thromboembolism in Japan compared to acute pulmonary embolism—results of multicenter registry of the Japanese society of pulmonary embolism research. Circ. J. 66, 257–260 (2003).
Kunieda, T., Naito, M., Ookubo, S., Yoshioka, K., Nakanishi, N. & Oobayashi, Y. Clinical aspects and diagnosis of pulmonary thromboembolism. Jpn. J. Thorac. Dis. 26, 463–472 (1988).
Tanabe, N., Okada, O., Nakagawa, Y., Masuda, M., Kato, K., Nakajima, N. et al. The efficacy of pulmonary thromboendarterectomy on long-term gas exchange. Eur. Respir. J. 10, 2066–2072 (1977).
Beck, S. & Trowsdale, J. The human major histocompatibility complex: lessons from the DNA sequence. Ann. Rev. Hum. Genet. 01, 117–137 (2000).
Fedullo, P. F., Auger, W. R., Kerr, K. M. & Rubin, L. J. Chronic thromboembolic pulmonary hypertension. Clin. Chest Med. 22, 561–581 (2001).
Geraphty, D. E., Daza, R., Williams, L. M., Yu, Q. & Ishitani, A. Genetics of the immune response: identifying immune variation within the MHC and throughout the genome. Immunol. Rev. 190, 69–85 (2002).
Shiina, T., Inoko, H. & Kulsky, J. K. An update of the HLA genomic region, locus information and disease associations: 2004. Tissue Antigens 64, 631–649 (2004).
de Bakker, P. I. W., McVean, G., Sabeti, P. C., Miretti, M. M., Green, T., Marchini, J. et al. A high-resolution HLA and SNP haplotype map for disease association studies in the extended human MHC. Nat. Genet. 38, 1166–1172 (2006).
Kimura, H., Okada, O., Tanabe, N., Tanaka, Y., Terai, M., Takiguchi, Y. et al. Plasma MCP-1 and pulmonary vascular resistance in chronic thromboembolic pulmonary hypertension. Am. J. Respir. Crit. Care Med. 164, 319–324 (2001).
Auger, W. R., Permpikul, P. & Moser, K. M. Lupus anticoagulant, heparin use and thrombocytopenia in patients with chronic thromboembolic pulmonary hypertension: a preliminary report. Am. J. Med. 99, 392–396 (1995).
Langevitz, P., Buskila, D., Gladman, D. D., Darlington, G. A., Farewell, V. T. & Lee, P. HLA alleles in systemic sclerosis: association with pulmonary hypertension and outcome. Br. J. Rheumatol. 31, 609–613 (1992).
Grigolo, B., Mazzetti, I., Meliconi, R., Bazzi, S., Scorza, R., Candela, M. et al. Anti-topoisomerase II α autoantibodies in systemic sclerosis-association with pulmonary hypertension and HLA-B35. Clin. Exp. Immunol. 121, 539–543 (2000).
Morse, J. H., Barst, R. J., Fotino, M., Zhang, Y., Flaster, E., Gharavi, A. E. et al. Primary pulmonary hypertension, tissue plasminogen activator antibodies, and HLA-DQ7. Am. J. Respir. Crit. Care Med. 155, 274–278 (1997).
Barst, R. J., Flaster, E. R., Menon, A., Fotino, M. & Morse, J. H. Evidence for the association of unexplained pulmonary hypertension in children with the major histocompatibility complex. Circulation 85, 249–258 (1992).
Morse, J. H., Barst, R. J., Itescu, S., Flaster, E. R., Sinha, G., Zhang, Y. et al. Primary pulmonary hypertension in HIV infection: an outcome determined by particular HLA class II alleles. Am. J. Respir. Crit. Care Med. 153, 1299–1301 (1996).
Tanabe, N., Kimura, A., Amano, S., Okada, O., Kasahara, Y., Tatsumi, K. et al. Association of clinical features with HLA in chronic pulmonary thromboembolism. Eur. Respir. J. 25, 131–138 (2005).
Auger, W. R., Fedullo, P. F., Moser, K. M., Buchbinder, M., Peterson, K. L. Chronic major-vessel thromboembolic pulmonary artery obstruction: appearance at angiography. Radiology 182, 393–398 (1992).
Saito, S., Ota, S., Yamada, E., Inoko, H. & Ota, M. Allele frequencies and haplotypic associations defined by allelic DNA typing at HLA class I and class II loci in the Japanese population. Tissue Antigens 56, 522–529 (2000).
Nakajima, F., Nakamura, J. & Yokota, T. Analysis of HLA haplotype in Japanese, using high resolution allele typing. MHC 8, 1–32 (2001).
Foissac, A., Salhi, M. & Cambon-Thomsen, A. Microsatellites in the HLA region: 1999 update. Tissue Antigens 55, 477–509 (2000).
Tamiya, G., Shiina, T., Oka, A., Tomizawa, M., Ota, M., Katsuyama, Y. et al. Twenty-six new polymorphic microsatellite markers around the HLA-B, -C, and -E loci in the human MHC class I lesion. Tissue Antigens 51, 337–346 (1998).
Ota, M., Katsuyama, Y., Hamano, H., Umemura, T., Kimura, A., Yoshizawa, K. et al. Two critical genes (HLA-DRB1 andABCF1) in the HLA region are associated with the susceptibility to autoimmune pancreatitis. Immunogenetics 59, 45–52 (2007).
Ota, M., Seki, T., Nomura, N., Sugimura, K., Mizuki, N., Fukushima, H. et al. Modified PCR-RFLP method for HLA-DPB1 and -DQA1 genotyping. Tissue Antigens 38, 60–71 (1991).
Fleischhauer, K., Zino, E., Bordignon, C. & Benazzi, E. Complete generic and extensive fine-specificity typing of the HLA-B locus by the PCR-SSOP method. Tissue Antigens 46, 281–292 (1995).
Shibata, H., Yasunami, M., Obuchi, N., Takahashi, M., Kobayashi, Y., Numano, F. et al. Direct determination of SNP haplotype of NFKBIL1 promoter polymorphism by DNA conformation analysis and its application to association study of chronic inflammatory diseases. Hum. Immunol. 67, 363–373 (2006).
Lander, E. S. & Schork, N. J. Genetic dissection of complex traits. Science 265, 2037–2048 (1994).
Ota, M., Katsuyama, Y., Kimura, A., Tsuchiya, K., Kondo, M., Naruse, T. et al. A second susceptibility gene for developing rheumatoid arthritis in the human MHC is located within a 70 kb interval telomeric of the TNF genes in the HLA class III region. Genomics 71, 263–270 (2001).
Okamoto, K., Makino, S., Yoshikawa, Y., Takaki, A., Nagatsuka, Y., Ota, M. et al. Identification of IkBL as the second MHC-linked susceptibility locus for rheumatoid arthritis. Am. J. Hum. Genet. 72, 303–312 (2003).
Kimura, A., Ota, M., Katsuyama, Y., Ohbuchi, N., Takahashi, M., Kobayashi, Y. et al. Mapping of the HLA-linked genes controlling the susceptibility to Takayasu's arteritis. Int. J. Cardiol. 75, 105–110 (2000).
McCluskey, J. & Peh, C. A. The human leukocyte antigens and clinical medicine: and overview. Rev. Immunogenet. 1, 3–20 (1999).
Acknowledgements
We thank Professor H Inoko, Mr D Shichi, Ms H Kawada, Ms E Kikkawa and Ms M Nakajima for their contributions in the genotyping of a part of the control subjects. This study was partly supported in part by Grant-in-Aids from the Ministry of Education, Science, Sports, Culture and Technology (MEXT) of Japan, the program of Founding Research Centers for Emerging and Reemerging Infection Disease supported by MEXT, Japan, research grants including that for the Research Committee of Intractable Respiratory Failure, a research grant for cardiovascular disease(14-5) from the Ministry of Health, Labor and Welfare, Japan, and a research grant from the Japan Health Science Foundation.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kominami, S., Tanabe, N., Ota, M. et al. HLA-DPB1 and NFKBIL1 may confer the susceptibility to chronic thromboembolic pulmonary hypertension in the absence of deep vein thrombosis. J Hum Genet 54, 108–114 (2009). https://doi.org/10.1038/jhg.2008.15
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jhg.2008.15
Keywords
This article is cited by
-
Chronic Thromboembolic Pulmonary Hypertension: the End Result of Pulmonary Embolism
Current Cardiology Reports (2015)
-
DDX39B (BAT1), TNF and IL6 gene polymorphisms and association with clinical outcomes of patients with Plasmodium vivax malaria
Malaria Journal (2014)
-
Susceptibility to chronic thromboembolic pulmonary hypertension may be conferred by miR-759 via its targeted interaction with polymorphic fibrinogen alpha gene
Human Genetics (2010)