Abstract
Purpose
Anti-VEGF treatment has a potent vasoconstrictive effect. Early changes of retinal blood flow velocity (RBFV) measured using the Retinal Function Imager (RFI) combined with indicators of vascular status may help in predicting the visual outcome 1 month post injection in patients with neovascular age-related macular degeneration (nvAMD) under ranibizumab treatment. To develop a simple prediction model based on the change in RBFV 3 days post injection and indicators of a patient’s vascular status to assess the probability of a successful visual outcome 1 month post injection.
Methods
RBFV measured using RFI were prospectively collected pre-injection and 3 days post injection in 18 eyes of 15 patients. Indicators of vascular status (history of hypertension, diabetes mellitus without retinal affection, and smoking) were assessed by medical history. By univariate analyses, parameters associated with visual outcome were weighted (−1 to 6 points). A multivariate logistic regression model with the categorized visual outcome parameter (≥0 letters gained after 1 month) as the dependent variate and the sum score as the independent variate (continuous scale) was used to estimate the score value-specific probabilities of letters gained ≥0 1 month post injection.
Results
The indicators of vascular status negatively influenced the likelihood of a letter gain ≥0 whereas an increase in the arterial RBFV strongly increased it. The area under the receiver operating characteristics curve for these parameters investigated was 0.71 (95% CI: 0.43–1.00).
Conclusion
Changes in the arterial RBFV following 3 days after ranibizumab injection combined with three indicators of the vascular status identified nvAMD patients with favorable visual outcome accurately.
Similar content being viewed by others
Introduction
Early changes in retinal blood flow velocity (RBFV) measured with the Retinal Function Imager (RFI) may help in predicting the visual outcome of patients under ranibizumab treatment for neovascular age-related macular degeneration (nvAMD), but the evidence is sparse.1, 2 It has been demonstrated that intravitreal ranibizumab injection (IVRI) in patients with nvAMD causes a significant vasoconstriction in retinal arterioles.3, 4 This effect can be explained by the inhibition of vascular endothelial growth factor (VEGF), which functions as a vasodilator by activating endothelial nitric oxide synthase, resulting in the production of the potent vasodilator nitric oxide.5 In order to maintain the retinal blood flow in case of vasoconstriction following IVRI, RBFV is expected to increase (flow=cross-section area × RBFV). Assuming that this is the case, the effect of a ranibizumab therapy would be expressed by a gain in arterial RBFV.
Retinal function imaging is a new, noninvasive diagnostic concept that allows to perform a quantitative mapping of RBFV.6, 7, 8 The RBFV is measured by direct observation of erythrocyte movement. The RFI has proven to be a valuable tool in investigating various retinal conditions9, 10, 11, 12, 13, 14, 15, 16 as well as in evaluating the medical treatment.17 We hypothesize that the extent of RBFV gain early after injection could be used as a proxy for an anti-VEGF treatment effect. Therefore, in this study we quantified the early changes in RBFV measured by RFI following ranibizumab injection and examined the association with visual outcomes after 1 month of follow-up.
Materials and methods
This study received the approval of the ethics committee of Canton Lucerne (#13103) and was performed according to the standards of good clinical practice.
Setting and recruitment
In this prospective and longitudinal study, patient records of individuals with nvAMD admitted to the Lucerne Eye Clinic for monthly check-up in the pro re nata regimen were screened. If patients met the inclusion criteria, they were informed about the study and included if interested. Written informed consent was obtained by all participating patients.
Inclusion and exclusion criteria
A total of 18 eyes of 15 patients were included. We included patients with nvAMD who have been treated with ≥3 intravitreal injections of only ranibizumab in the study eye. Indication for and conduction of retreatment on the actual visit were mandatory. If both eyes of one individual qualified for inclusion, both eyes were investigated.
All patients with history of epileptic or any other type of seizure (n=0) were excluded as the RFI works with a stroboscopic flash light. To guarantee an optimal image quality, patients with optical media opacity (n=2), poorly dilating pupil (n=1), or high refractive error (≥+10dpt or −6dpt) (n=0) were excluded. Factors possibly altering RBFV that accounted for exclusion were eye surgery or trauma within ≤3 months (n=1), diabetic retinopathy (n=0), and intraocular pressure (IOP) >21 mm Hg (n=1).
Clinical assessments
The data evaluated in this study derived from three visits per patient.
On the first (T0) and third (T1m) visit, approximately 1 month after T0, patients underwent testing of best-corrected visual acuity (BCVA) by Early Treatment of Diabetic Retinopathy Scale (ETDRS) and a Spectralis-Optical Coherence Tomography (OCT) (Heidelberg Engineering GmbH, Heidelberg, Germany) in follow-up mode was conducted by the optometrist to obtain central macular thickness (CFT) and total macular volume (TMV) (version 1.7.1.0., 2012, Heidelberg Engineering GmbH, Germany).
Indication for retreatment was determined by a resident physician using the retreatment criteria based on the PrONTO-Studies.18, 19 In addition any intra- and subretinal fluid assessed by OCT was treated.
Before IVRI (T0) and 3 days after IVRI (T3) images were taken with the RFI after dilatation (tropicamide 0.5% gtt) to analyze the changes in the arterial, venous, and mean RBFV.
Indicators of vascular status and physiological parameters
On the first visit (T0), we assessed the history of hypertension, diabetes mellitus without retinal affection, and smoking. Moreover, systolic and diastolic blood pressure, mean arterial pressure (MAP), pulse frequency, IOP, and mean ocular perfusion pressure (MOPP) were assessed.
RFI measurements
Details of RFI measurements have been described elsewhere.6 In brief, the device calculates the cross-correlation of moving patterns of erythrocytes and single erythrocytes over eight consecutive pictures and quantifies the RBFV of venules and arterioles.
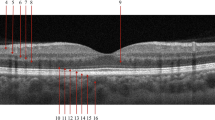
The first RBFV measurement (T0) was performed minutes before the injection, the second measurement was conducted 3 days after IVRI (T3). The field of vision was set to 35 degrees. The three series of best image quality, each with at least four consecutive images, were included for the RBFV analysis. For quality assurance, segments with coefficients of variance >0.45 were excluded. In each hemisphere three arterioles and three venules were measured using the automated integrated software, resulting in a total of 12 vessel segment measurements per patient, 6 venules and 6 arterioles (Supplementary Figure 1).
Statistical analysis
Dichotomous variates were described with percentages and continuous variates with means and standard deviations (SD). We measured the changes in arterial, venous, and mean RBFV between T0 and T3 with a paired t-test. In the same manner, the outcomes (change in BCVA, CMT, and TMV) were assessed. To quantify the association between history of hypertension, diabetes mellitus, any smoking and the three RFI parameters (arterial, venous, and mean RBFV difference between T0 and T3), we performed univariate analyses.
Multivariate analysis
For each patient we calculated the vascular score as the sum of positive vascular risk factors. Values of this score could range from 0 (no history of hypertension, diabetes, and smoking) up to a value of 3 (all risk factors present). In a multivariate analysis (using a random intercept model with subject as the random factor to adjust for the fact that three patients provided data on both eyes), we assessed the association of the two independent variates, arterial RBFV and vascular score, with the visual outcome parameter (≥0 letters gained after 1 month) as the dependent variate.
Prediction score
The arterial blood flow velocity was categorized into two groups (RFI >=1 vs else) and a score value was attributed to each category as follows: Each of the three vascular parameters (hypertension, diabetes mellitus without retinal affection, and smoking history) received 1 minus point and the velocity parameter received 6 points. Thus, the sum score could theoretically reach values between −3 and 6 points and was calculated for each patient. A univariate logistic regression model with the categorized visual outcome parameter (≥0 letters gained after 1 month) as the dependent variate and the prediction score as the independent variate (continuous scale) was used to estimate score value-specific probabilities of letters gained ≥0 using the following formula:

where α=intercept and β=regression coefficient for score variate.
The corresponding estimated probabilities are shown in Table 2. The area under the receiver operator curve (aROC) was estimated. A P-value of <0.05 was considered statistically significant. Analyses were performed using the Stata 11.2 statistics software package (StataCorp LP, College Station, TX, USA).
Results
Patients’ characteristics
Patients’ characteristics are listed in Table 1a. Mean age was 80.4 years (SD±4.8), 67% of eyes were female, and 44% was right eyes. On average, patients have received 13.7 injections (SD±9.0) before inclusion into the study. Overall, 39% of patients were suffering from a treated hypertension and 17% were suffering from a diabetes mellitus without retinal affection, whereof 67% were insulin dependent and 33% treated with oral anti-diabetics. Also, 56% of eyes came from former or current smokers, with an average pack years of 12.8 (SD±18.9).
Changes in clinical parameters
RFI
Before anti-VEGF injection, the average RBFV of all patients studied was 3.68 mm/s for arterial, 3.08 mm/s for venous, and 3.38 mm/s for mean arterio-venous RBFV. Three days after the injection, the RBFV measurements increased to 4.27 mm/s (+16%) for the arterial RBFV, 3.24 mm/s (+5%) for the venous RBFV, and 3.85 mm/s (+14%) the mean arterial-venous RBFV. Although the arterial and mean RBFV increased significantly 3 days following the injection (P=0.023, P= 0.042), venous RBFV only increased to a nonsignificant level (P=0.464).
In the subgroup of patients with stable gaining of vision, the RBFV values increased from 3.63 (SD 1.14) to 4.79 (SD 1.41) mm/s for the arterial RBFV, from 3.38 (SD 1.16) to 3.28 (SD 0.38) mm/s for the venous RBFV, and from 3.50 (SD 1.10) to 4.03 (SD 0.83) mm/s for the mean arterial-venous RBFV before and 3 days after the treatment, respectively. In contrast, in the subgroup of patients losing vision the RFFV readings changed from 3.72 (SD 0.74) to 3.94 (SD 1.21) mm/s for the arterial RBFV, from 2.89 (SD 0.81) to 3.22 (SD 0.97) mm/s for the venous RBFV and from 3.30 (SD 0.69) to 3.74 (SD 1.04) mm/s for the mean arterial-venous RBFV before and 3 days after treatment. The difference in changes of arterial RBFV was statistically significant (P=0.048), whereas those of the venous (P=0.344) and mean RBFV (P=0.486) were not.
Visual acuity and morphologic parameters
Overall, BCVA decreased slightly, but non-significantly, from 75.6 letters (SD±7.8) to 74.9 letters (SD±7.3) (P=0.517) after 1 month. Letter gain 1 month post injection was significantly influenced by the arterial RBFV (coef. 1.23, 95% CI: 0.23–2.23, P=0.016). At the same time, a significant decrease in the morphologic parameters CFT (−17.72 (SD 23.73); P=0.006) and TMV (−0.08 μm3 (SD 0.16); P=0.044) was observed; however, it was not influenced by the arterial RBFV (coef. −1.21, 95% CI: −13.81 to 11.39, P=0.841; and −0.004, 95% CI: −0.088 to 0.081, P=0.931). The eyes of patients with diabetes without retinal affection were associated with a lower decrease in CFT (coef. −27.27, 95% CI: −56.71 to 2.17). The changes in clinical parameters are summarized in Table 1b.
Physiological parameters
All physiological parameters (systolic and diastolic blood pressure, pulse frequency, MAP, and MOPP) except for IOP (P= 0.039) were comparable at T0 and T3.
The changes in all parameters are summarized in Table 1b.
Prediction model
Full model
The regression coefficients of the full model were: β0= −0.76 (95% CI: −2.56 to 1.05); βvasc.status=−0.42 (95% CI: −1.59 to 0.75); and βaRBFV=1.23 (95% CI: 0.00–2.46). The corresponding aROC of this model was 0.82 (95% CI: 0.56–1.00). The estimated probabilities ranged from 10.8 to 81.8%. Goodness-of-fit and the comparison between observed and estimated probabilities are shown in Supplementary Figures 2 and 3.
Score
An increase in arterial RBFV of ≥1 mm/s strongly increased the likelihood for a letter gain ≥0 one month post injection, whereas the history of hypertension, diabetes mellitus without retinal affection, and smoking decreased this likelihood. ROC plot is depicted in Figure 1 with the aROC amounting to 0.71 (95% CI: 0.43–1.00). A comparison between observed probabilities and corresponding estimated probabilities generated by the simple prediction score are shown in Table 2.
Discussion
Main findings
A simple score including changes in arterial RBFV following 3 days after ranibizumab injection combined with three indicators of vascular status (history of hypertension, diabetes mellitus, and smoking) predicted nvAMD patients with a favorable visual outcome after 1 month accurately. Arterial RBFV increased 3 days after ranibizumab injection, while most physiological parameters remained stable, rendering chances of confounding of RBFV changes low. The finding of a major increase of RBFV occurring in arterioles supports the theory of vasoconstriction being the major driver of increase in RBFV.20, 21 In this set of patients, we found only a weak association between changes in IOP and blood flow velocity (data not shown). We therefore conclude that changes in RBFV were not substantially affected by changes in IOP. As treatment success was strongly positively influenced by increase in RBFV, thus vasoconstriction, and negatively influenced by suboptimal vascular conditions (history of hypertension, diabetes mellitus without retinal affection, and smoking) probably only allowing restricted response by vasoconstriction, one can conclude that treatment success as visual outcome is directly influenced by vessel response. Morphologic findings in OCT did not correspond to our indicators, which is why the prediction model was based on visual development solely.
Results in context with the existing literature
Finger et al22 in a review classified possible predictors of anti-VEGF treatment outcome as genetic, clinical, and behavioral, where they found that clinical parameters are likely to majorly contribute to treatment outcome. Although the levels of pretreatment visual acuity and several morphologic parameters in OCT have been assessed in detail as possible predictors for treatment outcome,23 the role of factors of retinal hemodynamics indicating at a treatment response are ill understood. We are aware of only one study by Barak et al17 that looked into the short-term effects of bevacizumab (Avastin) on RBFV. Stimulated by their findings, we focused on the vascular response to ranibizumab. Our findings contribute to a better understanding the extent to which RBFV may be useful in the prediction of a ranibizumab treatment success.
Strengths and limitations
The strengths of this study lie in its prospective design presenting a uniform and typical cohort of nvAMD patients in terms of mean age (80.4 years, SD±4.8), female predominance24 (67%), and ranibizumab history (13.7 injections, SD±9.0). The simple score that was derived is easy to use and has an acceptable goodness-of-fit particularly in higher probability regions. Where are the limitations? This prediction model does only take into account the outcome of functional success, ie, visual acuity. Anatomic features, such as CMT and TMV, that do contribute to a fair degree to definition of treatment success and are commonly used for indication for retreatment18, 19 were not included. Also, the sample size was rather small and further exploration of its usefulness is certainly warranted.
Implications for research and practice
Further studies should validate our score and our findings in their settings and with their patients. It might be necessary to calibrate the parameters for specific clinical circumstances. The prediction model could contribute as a puzzle piece to the ongoing quest of early definition of therapy response to anti-VEGF treatment.22, 25, 26 Randomized trials comparing a therapeutic strategy based on the prediction model with standard care are necessary to assess the clinical impact of the score in the clinical management. If, by the score, treatment is expected to be successful, the treatment interval until the next check-up could possibly be stretched out, combined with means of patient empowerment and self-monitoring of their disease in the meantime.27
Conclusions
To our knowledge, the developed prediction score is the first tool allowing an estimation of visual treatment success as early as 3 days post injection in nvAMD therapy with ranibizumab. In regard to the current research to predict responders and nonresponders of anti-VEGF therapy, we believe that our findings make a valuable contribution in creating the full picture of early detection of treatment success. If confirmed in cross validations this simple score based on RBFV and clinical information could assist ophthalmologists optimizing nvAMD management of individual patients.

References
Rosenfeld PJ, Brown DM, Heier JS, Boyer DS, Kaiser PK, Chung CY et al. Ranibizumab for neovascular age-related macular degeneration. N Engl J Med 2006; 355 (14): 1419–1431.
Brown DM, Michels M, Kaiser PK, Heier JS, Sy JP, Ianchulev T . Ranibizumab versus verteporfin photodynamic therapy for neovascular age-related macular degeneration: Two-year results of the ANCHOR study. Ophthalmology 2009; 116 (1): 57–65 e5.
Papadopoulou DN, Mendrinos E, Mangioris G, Donati G, Pournaras CJ . Intravitreal ranibizumab may induce retinal arteriolar vasoconstriction in patients with neovascular age-related macular degeneration. Ophthalmology 2009; 116 (9): 1755–1761.
Micieli JA, Tsui E, Lam WC, Brent MH, Devenyi RG, Hudson C . Retinal blood flow in response to an intravitreal injection of ranibizumab for neovascular age-related macular degeneration. Acta ophthalmol 2012; 90 (1): e13–e20.
Chen Y, Medhora M, Falck JR, Pritchard KA Jr, Jacobs ER . Mechanisms of activation of eNOS by 20-HETE and VEGF in bovine pulmonary artery endothelial cells. American journal of physiology. Am J Physiol Lung Cell Mol physiol 2006; 291 (3): L378–L385.
Izhaky D, Nelson DA, Burgansky-Eliash Z, Grinvald A . Functional imaging using the retinal function imager: direct imaging of blood velocity, achieving fluorescein angiography-like images without any contrast agent, qualitative oximetry, and functional metabolic signals. Jpn J Ophthalmol 2009; 53 (4): 345–351.
Landa G, Jangi AA, Garcia PM, Rosen RB . Initial report of quantification of retinal blood flow velocity in normal human subjects using the Retinal Functional Imager (RFI). Int Ophthalmol 2012; 32 (3): 211–215.
Nelson DA, Burgansky-Eliash Z, Barash H, Loewenstein A, Barak A, Bartov E et al. High-resolution wide-field imaging of perfused capillaries without the use of contrast agent. Clin Ophthalmol. 2011; 5: 1095–1106.
Burgansky-Eliash Z, Barash H, Nelson D, Grinvald A, Sorkin A, Loewenstein A et al. Retinal blood flow velocity in patients with age-related macular degeneration. Curr Eye Res 2014; 39 (3): 304–311.
Burgansky-Eliash Z, Barak A, Barash H, Nelson DA, Pupko O, Lowenstein A et al. Increased retinal blood flow velocity in patients with early diabetes mellitus. Retina 2012; 32 (1): 112–119.
Beutelspacher SC, Serbecic N, Barash H, Burgansky-Eliash Z, Grinvald A, Krastel H et al. Retinal blood flow velocity measured by retinal function imaging in retinitis pigmentosa. Graefes Arch Clin Exp Ophthalmol 2011; 249 (12): 1855–1858.
Burgansky-Eliash Z, Nelson DA, Bar-Tal OP, Lowenstein A, Grinvald A, Barak A . Reduced retinal blood flow velocity in diabetic retinopathy. Retina 2010; 30 (5): 765–773.
Landa G, Amde W, Haileselassie Y, Rosen RB . Cilioretinal arteries in diabetic eyes are associated with increased retinal blood flow velocity and occurrence of diabetic macular edema. Retina 2011; 31 (2): 304–311.
Birger Y, Blumenfeld O, Bartov E, Burgansky-Eliash Z . Reduced retinal blood flow-velocity in severe hyperlipidemia measured by the retinal function imager. Graefes Arch Clin Exp Ophthalmol 2011; 249 (10): 1587–1590.
Gutfreund S, Izkhakov E, Pokroy R, Yaron M, Yeshua H, Burgansky-Eliash Z et al. Retinal blood flow velocity in metabolic syndrome. Graefes Arch Clin Exp Ophthalmol 2013; 251 (6): 1507–1513.
Feng X, Kedhar S, Bhoomibunchoo C . Retinal blood flow velocity in patients with active uveitis using the retinal function imager. Chin Med J(Engl) 2013; 126 (10): 1944–1947.
Barak A, Burgansky-Eliash Z, Barash H, Nelson DA, Grinvald A, Loewenstein A . The effect of intravitreal bevacizumab (Avastin) injection on retinal blood flow velocity in patients with choroidal neovascularization. Eur J Ophthalmol 2012; 22 (3): 423–430.
Lalwani GA, Rosenfeld PJ, Fung AE, Dubovy SR, Michels S, Feuer W et al. A variable-dosing regimen with intravitreal ranibizumab for neovascular age-related macular degeneration: year 2 of the PrONTO Study. Am J Ophthalmol 2009; 148 (1): 43–58 e1.
Fung AE, Lalwani GA, Rosenfeld PJ, Dubovy SR, Michels S, Feuer WJ et al. An optical coherence tomography-guided, variable dosing regimen with intravitreal ranibizumab (Lucentis) for neovascular age-related macular degeneration. Am J Ophthalmol 2007; 143 (4): 566–583.
Toklu Y, Cakmak HB, Raza S, Anayol A, Asik E, Simsek S . Short-term effects of intravitreal bevacizumab (Avastin((R))) on retrobulbar hemodynamics in patients with neovascular age-related macular degeneration. Acta Ophthalmol 2011; 89 (1): e41–e45.
Fontaine O, Olivier S, Descovich D, Cordahi G, Vaucher E, Lesk MR . The effect of intravitreal injection of bevacizumab on retinal circulation in patients with neovascular macular degeneration. Invest Ophthalmol Vis Sci 2011; 52 (10): 7400–7405.
Finger RP, Wickremasinghe SS, Baird PN, Guymer RH . Predictors of anti-VEGF treatment response in neovascular age-related macular degeneration. Surv Ophthalmol 2014; 59 (1): 1–18.
Ying GS, Huang J, Maguire MG, Jaffe GJ, Grunwald JE, Toth C et al. Baseline predictors for one-year visual outcomes with ranibizumab or bevacizumab for neovascular age-related macular degeneration. Ophthalmology 2013; 120 (1): 122–129.
Rudnicka AR, Jarrar Z, Wormald R, Cook DG, Fletcher A, Owen CG . Age and gender variations in age-related macular degeneration prevalence in populations of European ancestry: a meta-analysis. Ophthalmology 2012; 119 (3): 571–580.
Otsuji T, Nagai Y, Sho K, Tsumura A, Koike N, Tsuda M et al. Initial non-responders to ranibizumab in the treatment of age-related macular degeneration (AMD). Clin Ophthalmol 2013; 7: 1487–1490.
Krebs I, Glittenberg C, Ansari-Shahrezaei S, Hagen S, Steiner I, Binder S . Non-responders to treatment with antagonists of vascular endothelial growth factor in age-related macular degeneration. Br J Ophthalmol 2013; 97 (11): 1443–1446.
Faes L, Bodmer NS, Bachmann LM, Thiel MA, Schmid MK . Diagnostic accuracy of the Amsler grid and the preferential hyperacuity perimetry in the screening of patients with age-related macular degeneration: systematic review and meta-analysis. Eye (Lond) 2014; 28 (7): 788–796.
Acknowledgements
Dr Böhni’s and Dr Bittner’s work was funded via an unrestricted educational grant from Novartis AG, Switzerland.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on Eye website
Supplementary information
Rights and permissions
About this article
Cite this article
Böhni, S., Howell, J., Bittner, M. et al. Blood flow velocity measured using the Retinal Function Imager predicts successful ranibizumab treatment in neovascular age-related macular degeneration: early prospective cohort study. Eye 29, 630–636 (2015). https://doi.org/10.1038/eye.2015.10
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/eye.2015.10
This article is cited by
-
The retinal function imager and clinical applications
Eye and Vision (2018)