Abstract
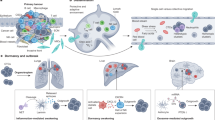
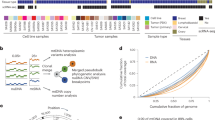
Microsatellite alterations can be found in a number of tumors. There are two types of alterations: loss of heterozygosity (LOH), which can be detected in the majority of colorectal cancers (CRC), and microsatellite instability (MSI). MSI occurs in about 15% of CRC with a mutator phenotype and are the hallmark of hereditary nonpolyposis colorectal cancers (HNPCC). Furthermore, MSI can also be detected in other tumors which are part of the HNPCC tumor spectrum (eg, gastric, ovarian, and endometrial carcinomas). Usually, a set of microsatellite markers is amplified by PCR followed by gel or capillary electrophoresis to separate PCR amplicons and by detection of the markers using autoradiography (Thibodeau et al, 1993), silver staining (Schlegel et al, 1996), or fluorescence techniques (Gyapay et al, 1996; Mansfield et al, 1994). We have established a technique to detect MSI by LightCycler PCR and melting point analysis using sequence-specific hybridization probes (HyProbes) labeled with LightCycler dyes, LCRed640 and LCRed705. Amplification of microsatellites by real-time PCR is followed by melting point analysis to display alterations in the length of repetitive sequences, thereby avoiding any electrophoretical separation of amplified DNA. Two mononucleotide markers (BAT25 and BAT26) were tested in 81 formalin-fixed and paraffin-embedded colorectal cancer samples with matched normal tissues from 21 MSI tumors and 60 tumors with microsatellite stability. Amplification and melting point determination of BAT26 and BAT25 was possible in 129/162 (80%) and 123/162 (76%) formalin-fixed and paraffin-embedded tissue samples, respectively. MSI could be detected specifically with both BAT25 and BAT26 markers only in MSI-high tumors (≥40% MSI rate, determined with microsatellite reference panel, BAT25, BAT26, D5S346, D2S123, D17S250; Boland et al, 1998; Dietmaier et al, 1997). This new technique allows MSI detection within less than a hour and provides a basis for fast, high-throughput MSI analysis.
Similar content being viewed by others
Main
Microsatellite instability (MSI) status from 81 tumors and matching normal tissues was first characterized by the analysis of reference microsatellite markers with conventional microsatellite PCR (Hereditary Nonpolyposis Colorectal Cancer Microsatellite Instability Test-Kit; Roche GmbH, Mannheim, Germany) followed by automatic fragment analysis (ABI310, Perkin Elmer Biosystems, Weiterstadt, Germany). In addition, all tissue samples were analyzed for hMSH2, hMLH1, and hMSH6 mismatch repair protein expression by immunohistochemistry (hMSH2: AB-2, clone FE11, Calbiochem, San Diego, California; hMLH1: clone G168-15, Pharmingen, Hamburg, Germany; hMSH6: clone 44, Transduction Laboratories, Lexington, Kentucky). Sixty microsatellite stable (MSS) tumors and 21 microsatellite instability-high (MSI-H) tumors were used for LightCycler (Roche GmbH, Mannheim, Germany) microsatellite PCR and melting point analysis with BAT25 and BAT26, which are described as the most sensitive markers for MSI detection (Cravo et al, 1999; Dietmaier et al, 1997; Hoang et al, 1997; Loukola et al, 2001; Stone et al, 2000). Tumor tissue and normal mucosa were microdissected from 5-μm sections of formalin-fixed, paraffin-embedded tissues by laser assisted (P.A.L.M., Bernried, Germany) or manual microdissection. DNA preparation was done using the High Pure PCR Preparation Kit (Roche GmbH), and the quality of DNA was checked by electrophoresis (1.3% agarose gel).
Two microliters of high-molecular-weight DNA (50–100 ng) were mixed with 13 μl amplification solution, resulting in a final concentration of 3 mm MgCl2, 0.5 μm BAT26-U (5′ TGA CTA CTT TTG ACT TCA GCC 3′) and BAT26-D (5′ AAC CAT TCA ACA TTT TTA ACC 3′) primers, 0.15 μm BAT26donor-HyProbe (5′ GCA GCA GTC AGA GCC CTT AAC CT-Fluorescein 3′) and BAT26accept-HyProbe (5′ LC-Red640-TCA GGT AAA AAA AAA AAA AAA AAA AAA AAA AA-Phosphate 3′), and × 1 LightCycler DNA Master Hybridization Probes-Mix (Roche Molecular Biochemicals). Alternatively, 0.5 μm BAT25-U (5′ TCG CCT CCA AGA ATG TAA GT 3′) and BAT25-D (5′ TCT GCA TTT TAA CTA TGG CTC 3′) primers and 0.15 μm BAT25donor-HyProbe (5′ CAA AAA AAA AAA AAA AAA AAA AAA AAT CA-Fluorescein 3′) and BAT25accept-HyProbe (5′ LC-Red-705-AAC AAA ACA CAA AAC TCT TTA GAG AAT C-Phosphate 3′) were used for BAT25 LightCycler PCR. The PCR amplification program started with a single denaturation step at 95° C for 90 seconds and proceeded with 50 cycles of 95° C/0 seconds (denaturation), 60° C/10 seconds (annealing), 50° C/3 seconds (fluorescence signal detection), and 72° C/10 seconds (elongation). Subsequent melting point analysis was done by denaturating the amplicons at 95° C/0 seconds, incubating at 35° C/30 seconds (BAT26) and 30° C/30 seconds (BAT25), respectively, for HyProbe annealing, and increasing the temperature to 95° C at a rate of 0.2°/second, with continuous F2 (Bat26) and F3 (BAT25) measuring, respectively. Fluorescence settings for BAT26 were F2 channel, 1 (F1 Gain), 10 (F2 Gain), 1 (F3 Gain) and for BAT25 were F3 channel, 1 (F1 Gain), 1 (F2 Gain), 10 (F3 Gain).
Amplification and melting point analysis of BAT26 was successful in 80% of tumor samples (65/81; 16 MSI, 49 MSS tumors) and in 79% of normal mucosa samples (64/81). BAT 25 analysis was possible in 78% of tumor samples (63/81; 15 MSI, 48 MSS tumors) and in 74% of normal mucosa samples (60/81). Successful amplification of these markers depends on the quality of isolated DNA and might be improved by using mainly intact high-molecular-weight DNA controlled by agarose gel electrophoresis. In some cases the use of a 10-fold diluted DNA might further improve the PCR because the concentration of potential PCR inhibitors would be lowered. BAT26 melting point analysis showed a melting temperature (Tm) of 51.0 to 51.5° C for DNA from normal mucosa tissue, blood, or MSS tumors (Fig. 1A), whereas the Tm of MSI-H tumors with either defective hMSH2, hMLH1, or hMSH6 protein expression and MSI-H phenotype was shifted to 42 to 50° C (Fig. 1B). The Tm alterations are due to shortenings of 3 to 12 nucleotides in a stretch of 26 repetitive adenosine nucleotides within BAT26 marker as determined by automatic fragment analysis using the ABI310 sequencer (Fig. 1C). Tm of BAT25 was 45 to 46° C in DNA from blood, normal mucosa, and MSS tumor tissue (Fig. 2A) and 42.5 to 43.7° C in the MSI-H tumors (Fig. 2B). These Tm shifts correspond to a shortening of 5 to 7 nucleotides within 25 repetitive nucleotides of BAT25 marker as shown by automatic fragment analysis (Fig. 2C). The high resolution of melting point analysis could be demonstrated in hMSH6-defective MSI-H Tumor 1, which shows a shortening of only a single nucleotide in BAT25 (Fig. 2C) and a Tm shift of −2° C in melting point analysis (Fig. 2B). In this case, detection of BAT25 instability was more evident with melting point analysis than with automatic fragment analysis. As observed in some samples, the accuracy of Tm determination might be further improved by diminishing the rate of temperature increase in the melting point analysis step from 0.2° C/second to 0.05° C/second. All tumors with MSS in conventional fragment analyses had the same melting points as the normal tissue.
Microsatellite melting point analysis allows a fast microsatellite analysis of the two most sensitive and specific markers for MSI detection in colorectal cancer. Because MSI-H is defined as at least two unstable microsatellites from five markers (Boland et al, 1998; Dietmaier et al, 1997), this LightCycler-based microsatellite PCR technique can rapidly detect MSI-H in most colorectal tumors. Furthermore, this technique avoids the need of time-consuming DNA fragment analysis by electrophoresis and can detect MSI reproducibly, accurately, sensitively, and specifically. Thus, microsatellite melting point analysis allows MSI detection within 1 hour, starting with PCR setup, and is an ideal technique for high throughput MSI screening analyses.
References
Boland CR, Thibodeau SN, Hamilton SR, Sidransky D, Eshleman JR, Burt RW, Meltzer SJ, Rodriguez-Bigas MA, Fodde R, Ranzani GN, and Srivastava S (1998). A National Cancer Institute Workshop on Microsatellite Instability for cancer detection and familial predisposition: Development of international criteria for the determination of microsatellite instability in colorectal cancer. Cancer Res 58: 5248–5257.
Cravo M, Lage P, Albuquerque C, Chaves P, Claro I, Gomes T, Gaspar C, Fidalgo P, Soares J, and Nobre-Leitao C (1999). BAT-26 identifies sporadic colorectal cancers with mutator phenotype: A correlative study with clinico-pathological features and mutations in mismatch repair genes. J Pathol 188: 252–257.
Dietmaier W, Wallinger S, Bocker T, Kullmann F, Fishel R, and Ruschoff J (1997). Diagnostic microsatellite instability: Definition and correlation with mismatch repair protein expression. Cancer Res 57: 4749–4756.
Gyapay G, Ginot F, Nguyen S, Vignal A, and Weissenbach J (1996). Genotyping Procedures in Linkage Mapping. Methods 9: 91–97.
Hoang JM, Cottu PH, Thuille B, Salmon RJ, Thomas G, and Hamelin R (1997). BAT-26, an indicator of the replication error phenotype in colorectal cancers and cell lines. Cancer Res 57: 300–303.
Loukola A, Eklin K, Laiho P, Salovaara R, Kristo P, Jarvinen H, Mecklin JP, Launonen V, and Aaltonen LA (2001). Microsatellite marker analysis in screening for hereditary nonpolyposis colorectal cancer (HNPCC). Cancer Res 61: 4545–4549.
Mansfield DC, Brown AF, Green DK, Carothers AD, Morris SW, Evans HJ, and Wright AF (1994). Automation of genetic linkage analysis using fluorescent microsatellite markers. Genomics 24: 225–233.
Schlegel J, Vogt T, Munkel K, and Ruschoff J (1996). DNA fingerprinting of mammalian cell lines using nonradioactive arbitrarily primed PCR (AP-PCR). Biotechniques 20: 178–180.
Stone JG, Tomlinson IP, and Houlston RS (2000). Optimising methods for determining RER status in colorectal cancers. Cancer Lett 149: 15–20.
Thibodeau SN, Bren G, and Schaid D (1993). Microsatellite instability in cancer of the proximal colon. Science 260: 816–819.
Acknowledgements
We thank Dr. Arndt Hartmann for revising the manuscript and Ms. Lisa Weber for excellent technical assistance.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Dietmaier, W., Hofstädter, F. Detection of Microsatellite Instability by Real Time PCR and Hybridization Probe Melting Point Analysis. Lab Invest 81, 1453–1456 (2001). https://doi.org/10.1038/labinvest.3780358
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1038/labinvest.3780358
This article is cited by
-
Microsatellite instability assessment is instrumental for Predictive, Preventive and Personalised Medicine: status quo and outlook
EPMA Journal (2023)
-
Microsatellite instability testing in colorectal cancer using the QiaXcel advanced platform
BMC Cancer (2018)
-
Microsatellite instability typing in serum and tissue of patients with colorectal cancer: comparing real time PCR with hybridization probe and high-performance liquid chromatography
Molecular Biology Reports (2014)
-
Genetic alterations of APC, K-ras, p53, MSI, and MAGE in Korean colorectal cancer patients
International Journal of Colorectal Disease (2007)
-
Lack of Association between Microsatellite Instability and Benign Adrenal Tumors
World Journal of Surgery (2006)