Abstract
It is still unclear which membrane-bound regulatory proteins (mCRP) are important in vivo to protect tumor cells from complement-mediated damage. To address this question, the expression levels of CD46, CD55, and CD59 were measured semi-quantitatively in situ on renal cell carcinomas and compared with the expression level and cellular distribution of these mCRP in proximal tubuli within each patient (n = 31). It was also determined whether the expression of mCRP on tumor cells is associated with deposition of C3d and C5b-9. CD46 expression was decreased on tumor cells; in contrast, CD55 was expressed on tumor cells (12 out of 31 samples), while it was not detected on proximal tubular epithelial cells (PTEC). Also, expression of CD59 on tumor cells was increased as compared with its expression on PTEC. Furthermore, the localization on the cell surface of mCRP as observed on PTEC was altered on tumor cells. Because expression of mCRP may limit a complement-mediated anti-tumor response, we determined whether complement deposition was associated with the expression level of CD46, CD55, and CD59. The presence of C3d on tumor cells was associated with a low expression level of CD46 (p < 0.02). The expression level of CD46 was also associated with a low tumor stage (p < 0.04). The results suggest that in vivo CD46 plays a role in the protection of human renal tumor cells from complement-mediated injury.
Similar content being viewed by others
Introduction
Renal cell carcinoma (RCC) is the most common renal malignancy, accounting for 3% of malignancies in men (Bukowski, 1997; Figlin, 1999). RCC can be subdivided into clear cell carcinoma, papillary carcinoma, chromophobe carcinoma, and collecting duct carcinoma based upon morphology and genetics (Störkel et al, 1997). The most common of these is the clear cell carcinoma, which accounts for 70% to 80% of RCC. RCC is resistant to both chemo- and radiotherapy (Pittman and Selby, 1994). At present, radical nephrectomy is the main therapy for primary RCC. In a few cases the occurrence of spontaneous regressions of advanced disease after nephrectomy has been observed. This suggests that the host immune system is involved in tumor eradication (Pittman and Selby, 1994). Thus, RCC may be a suitable target for immunotherapy.
Thus far, immunotherapy with the cytokine IL-2 is the only effective treatment for metastatic RCC (Hrouda et al, 1997). In addition to clinical trials for improvement of cytokine therapy (Bono and Lovisolo, 1997; Bukowski et al, 1997; Motzer et al, 1996), clinical trials have been undertaken to study the effect of mAb-mediated immunotherapy for RCC (Oosterwijk et al, 1993; Steffens et al, 1997). One of the most promising mAb for mAb-mediated immunotherapy of RCC is G250. This complement-activating mAb is directed against the renal tumor-associated antigen G250 and has shown minor cross-reactivity with normal tissue (Blok et al, 1998; Oosterwijk et al, 1986). The complement system can either directly lyse tumor cells through formation of the membrane-attack complex or can promote cellular cytotoxicity through opsonization of tumor cells with C3 fragments. In addition, chemotactic factors are released during complement activation that can attract leukocytes to the tumor site (Gorter and Meri, 1999).
The level of complement activation on the tumor cell surface is regulated by the expression of mCRP, which protects normal and tumor cells from uncontrolled complement-mediated injury. It comprises complement receptor 1 (CR1, CD35), membrane cofactor protein (MCP, CD46), decay-accelerating factor (DAF, CD55), and homologous restriction factor 20 (HRF20, CD59) (Liszewski et al, 1996). CD35, CD46, and CD55 inhibit the deposition of C3 fragments on the cell surface and thereby limit complement-dependent cell-mediated cytotoxicity. CD59 prevents the formation of the membrane-attack complex and the subsequent osmotic lysis of the target cell. Several studies have shown that in situ tumor cells overexpress mCRP (Kumar et al, 1993; Mäenpää et al, 1996; Niehans et al, 1996). The overexpression of the mCRP on tumor cells may down-regulate an efficient local immune response. This may partially explain the disappointing results found thus far with mAb-mediated immunotherapy of solid tumors (Dillman, 1994).
Only a few studies have examined the deposition of complement components in association with mCRP (reviewed by Gorter and Meri, 1999). From these studies it is unclear which mCRP is important in vivo to protect human tumor cells from complement-mediated damage. To clarify this question, we determined the expression level and cellular distribution of CD46, CD55, and CD59 on renal clear cell carcinoma cells and PTEC in situ in each patient, and we correlated the presence of cell surface deposited C3d and C5b-9 with the expression of these mCRP.
Results
Analysis of mCRP Expression on Renal Carcinoma Cells
To establish a correlation between mCRP expression on renal carcinoma cells and complement deposition, we first measured semi-quantitatively the expression level of CD46, CD55, and CD59 in situ on RCC, using immunohistochemistry. The 31 RCC specimens revealed intra- and inter-tumor heterogeneity in both the level of expression (intensity) of mCRP and the number of tumor cells (% positive cells; Table 1) that expressed mCRP. All tumor specimens expressing mCRP demonstrated circumferential expression of CD46, CD55, and CD59 on the tumor cell membrane.
Of the 31 tumor specimens, 12 specimens showed a weak homogeneous, 9 specimens moderate homogeneous, and 2 specimens a strong homogeneous expression of CD46 on the tumor cell membrane (Fig. 1A). Heterogeneous tumor staining was observed in seven specimens. In one tumor specimen CD46 was not detected (Patient 31). From the 23 tumor specimens with a homogeneous expression of CD46, 8 specimens expressed CD46 on all tumor cells. On the other specimens the percentage of cells that expressed CD46 varied between 6% and 75%.
Expression of mCRP in renal cell carcinoma, as detected by immunohistochemistry. A, Expression of CD46. B, Expression of CD55. The tumor shown is heterogeneous for CD55 expression. A small part of the specimen with moderate expression of CD55 is shown. C, Expression of CD59. D, Control mAb, no immunoreactivity was seen in the negative control. Magnification, ×32. The cellular distribution of mCRP in this patient (Patient 12) is representative for the series.
CD55 expression could not be demonstrated on 19 tumors. Nine specimens showed a weak and one specimen (patient no. 14) a moderate homogeneous expression of CD55 on the tumor cell membrane (Table 1). In two specimens a heterogeneous membrane staining pattern was observed (Fig. 1B). In only one of the tumor specimens, all of the tumor cells expressed CD55 (Patient 27). The other nine specimens expressed CD55 on 6% to 75% of the tumor cells.
A strong homogenous expression of CD59 was observed on 22 tumor specimens (Fig. 1C). A heterogeneous staining pattern was displayed by nine specimens (Table 1). One tumor section could not be evaluated. In some tumor sections a weak to moderate expression of CD59 was also observed in the cytoplasm.
It is generally assumed that the sensitivity of immunohistochemistry is relatively low compared with that of flow cytometry. Thus, absence of CD55 expression on particular tumor specimens measured with immunohistochemistry does not exclude the possibility that tumor cells may express low amounts of CD55. To substantiate this argument, the expression of CD46, CD55, and CD59 was measured by triple-color flow cytometric analysis on six freshly isolated tumor cell suspensions derived from the same tumors as those used for immunohistochemistry. Tumor cells were discriminated from other cells in the cell suspension by selecting only cells that were positive for the renal tumor-associated antigen G250 using the G250 mAb. Three cases that had scored negatively for expression of CD55 by immunohistochemistry (Patients 19, 29, 30) expressed CD55 as measured with flow cytometry (Table 2). This suggests that flow cytometry is indeed more sensitive than immunohistochemistry. The order of mCRP expression intensities found by flow cytometry corresponded to that observed by immunohistochemistry (CD59>>CD46>CD55).
Comparison of the mCRP Expression Levels in Renal Clear Cell Carcinomas and PTEC
An increased expression level of mCRP on tumor cells would further protect tumor cells from complement-mediated damage, either induced as a local humoral anti-tumor response or by immunotherapy with mAb. Therefore, we investigated whether the expression levels of mCRP on renal clear cell carcinomas are increased as compared with the expression on normal renal tissue. Because clear cell carcinomas are thought to be derived from PTEC (Bander et al, 1989; Holthöfer et al, 1983), the expression of mCRP was determined on PTEC at a site within each patient distant from the clear cell carcinoma (Table 3). Because we not only observed that the intensities, but also the cellular distribution of mCRP seemed to be altered, the exact localization of mCRP expression on PTEC was determined and compared with that of clear cell carcinomas by immunofluorescent staining and subsequent analysis by confocal laser microscopy. For this purpose, material from two patients (No. 8 and 27) representative of the specimens in the series were stained and analyzed. Moderate expression of CD46 was observed on PTEC (Table 3). In general, more than 50% of PTEC in a specimen showed a positive reaction with the anti-CD46 mAb. This expression of CD46 was found essentially at the basal side of PTEC with a weak, diffuse staining into the cytoplasm (Fig. 2A). The basal lamina surrounding the tubuli was negative for expression of CD46 (Fig. 2B). Out of the 18 PTEC specimens investigated, one showed a moderate, basolateral expression of CD46. In one specimen a weak staining of the brush border of the proximal tubuli was detected. PTEC were completely negative for expression of CD55 (Fig. 2C). This was not due to lack of mAb binding, because expression of CD55 in cortical renal tissue was observed on the peritubular vascular endothelium. In contrast, expression of CD59 was found on all proximal tubuli. In most specimens, staining intensity was moderate (Table 3). In two specimens a strong reactivity with the anti-CD59 mAb was observed, while six specimens showed a heterogeneous reaction pattern varying from moderate to strong. Expression of CD59 on PTEC was localized to the brush border (Fig. 2D). Also, a weak to moderate homogeneous cytoplasmic staining was observed in six specimens.
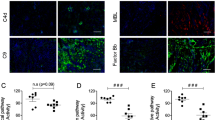
Cellular localization of mCRP in PTEC, as detected by immunofluorescence (Patient 8) and subsequent analysis with confocal fluorescence microscopy. A, Expression of CD46. B, (zoom) The basal lamina surrounding the tubuli (arrowhead) is negative for expression of CD46. C, Expression of CD55. Note the expression of CD55 on peritubular capillaries. D, Expression of CD59. Note the strong expression on peritubular capillaries. No immunoreactivity was seen in negative controls (not shown). Bars = 25 μm.
When comparing the expression pattern of mCRP on renal clear cell carcinomas and PTEC from the renal tissue of patients, it is clear that CD55 is enhanced on a proportion of tumors because it was expressed weakly to moderately in 44% (8 of 18) of the clear cell carcinomas, whereas distant PTEC did not show expression of CD55 (Tables 3 and 4). From our immunohistochemical data we could extract that the level of CD46 and CD59 expression on tumor cells differed from the expression level on PTEC (Table 4). To confirm this observation in a semi-quantitative way, the intensities of the immunofluorescent signals (Patients 8 and 27) were analyzed by means of pseudocolors. Pseudocolor analysis substantiated that the expression of CD46 was decreased on tumor cells as compared with the expression on PTEC (Fig. 3, A and B). In contrast, expression of CD59 was enhanced on renal tumor cells as compared with their expression on PTEC (Fig. 3, C and D).
Difference in expression level of mCRP on PTEC and renal tumor cells, as detected by immunofluorescence. The intensity of the fluorescent signal is presented as pseudocolors, with the signal increasing from blue to white. Expression of CD46 is decreased on renal tumor cells (B) as compared with the expression of CD46 on PTEC (A) (Patient 8). In contrast, the expression of CD59 is increased on tumor cells (D) as compared with PTEC (C) (Patient 27). Note that polarization of both CD46 and CD59 expression is lost on tumor cells. L, lumen.
Association Between Expression of mCRP and Tumor Grade or Tumor Stage
We also investigated whether these differences in the level of expression of CD46, CD55, and CD59 between tumor cells and PTEC could be related to the differentiation (grade) or progression (stage) of the tumors (Table 1). Expression of CD46 was significantly associated with tumor stage (p < 0.04). Tumors with low CD46 expression were predominantly (82%) of low stage (T1 and T2). Although expression of CD55 or CD59 was not significantly associated with tumor stage, we observed that the two tumors with moderate expression levels of CD55 were stage T3 tumors, whereas most of the tumors with low or absent CD55 expression (71%) were stage T1 and T2 tumors. No significant association was found between any mCRP and tumor grade.
Presence of C3 and C5b-9 in RCC
The presence of C3d and C5b-9 on renal tumor cells was analyzed by immunohistochemistry (Table 1). In general, tumor specimens showed a weak to moderate reactivity for C3d on the membrane of tumor cells (Fig. 4A). In six specimens a heterogeneous pattern of C3d deposition was observed. In most of the tumor specimens the tumor cell membranes did not stain for C5b-9 deposition. Only five tumors showed a weak cell membrane staining with reactivity on 6% to 50% of the tumor cells (Fig. 4B).
Association Between Expression of mCRP and Complement Deposition
When we correlated the expression of mCRP with the presence of C3d and C5b-9, a significant negative association between CD46 expression on tumor cells and deposition of C3d (p < 0.02) was found (Table 1). In two tumors with a heterogeneous expression pattern of CD46 and deposition of C3d, we observed microscopically a low intensity of C3d in areas with a high expression of CD46 and vice versa (data not shown). Expression of CD55 on RCC was not significantly associated with complement deposition. Although no deposition of C3d was detected on the two tumors from our series with a moderate expression of CD55, C3d was detected on 21 (72%) of the 29 tumors with a low or absent CD55 expression. The number of tumors with moderate expression of CD55 was too low for a statistically significant correlation. No significant association between expression of CD59 and deposition of C5b-9 nor an association between any (combination of) mCRP and C3d or C5b-9 was observed.
Discussion
The presence of mCRP on different types of tumors has been reported frequently (reviewed by Gorter and Meri, 1999). Also the function of mCRP in protecting normal and tumor cells in vitro from complement-mediated damage has been amply demonstrated (Gorter and Meri, 1999). Therefore, it is surprising that the relative importance of mCRP on tumor cells and their level of expression compared with normal tissue in vivo is still ill defined. To elucidate this question, the expression level of CD46, CD55, and CD59 on renal tumor cells and their association with the presence of C3d and C5b-9 in situ on RCC was investigated.
To establish whether mCRP are overexpressed in vivo on the most common type of RCC, the level of mCRP expression on renal clear cell carcinomas was compared semi-quantitatively with the level of expression on PTEC of the same patient, using different methods. In general, the expression pattern of CD46, CD55, and CD59 as observed on PTEC corresponds to that found in other studies (Ichida et al, 1994; Nakanishi et al, 1994). The expression of CD55 and CD59 was enhanced on renal clear cell carcinomas as compared with their expression on PTEC. Also other studies on RCC (Niehans et al, 1996), melanoma (Brasoveanu et al, 1995), and lung cancer (Varsano et al, 1995) observed an enhanced expression of CD55 and/or CD59. In contrast to the results of the study of Niehans et al (1996), who detected a focal moderate expression of CD55 on the interface between tumor cell nests and stroma, we were able to detect weak homogeneous membrane expression on CD55-positive renal tumor cells by immunohistochemistry. CD55 expression was confirmed by flow cytometric analysis of tumor cell suspensions derived from these tumors. The difference between the results of our study and that of Niehans et al (1996) might be explained by the fact that we used the EnVision+ (Dako, A/S, Glostrup, Denmark) detection system, which is more sensitive than the widely used peroxidase detection system. The enhanced signal generated by this system enabled us to visualize antigens with a low expression level. In addition, the limited number of RCC (n = 10) studied by Niehans et al (1996), may account for the observed difference in detection of CD55 on tumor cells.
In accordance with our immunohistochemical data, flow cytometric analysis of mCRP expression in tumor cell suspensions showed that on RCC the expression of CD59 was the highest, whereas CD55 expression was low or absent. These observations are also consistent with our data on renal tumor cell lines (Gorter et al, 1996). However, we noted that the mean expression level of mCRP on freshly isolated tumor cells was 15 to 40 times lower than that on tumor cell lines. Nevertheless, the ratio between the expression level of CD46, CD55, and CD59 on renal tumor cell lines and the expression level of these mCRP on freshly isolated renal tumor cells is similar.
In our immunohistochemical study, a significantly negative association between the level of CD46 expression and the intensity of C3d deposition on tumor cells was found. However, in a preceding study with renal tumor cell lines, we did not find an effect on C3 deposition after blocking of CD46 (Blok et al, 1998). This latter finding was in accordance with prior data suggesting that CD46 is mainly involved in regulation of the alternative pathway (Devaux et al, 1999). However, protection of classical pathway activation by CD46 expression on tumor cell lines has been shown previously (Azuma et al, 1995), although mainly CD55 and CD59 have been implicated as being important for classical pathway activation (Bjørge et al, 1997; Brasoveanu et al, 1996; Cheung et al, 1988); Gorter et al, 1996; Venneker et al, 1998). We propose, in view of our present results, that CD46 is able to regulate the amplification loop of the classical pathway when the expression of CD55 is low or absent.
A significant association between expression of CD46 and tumor stage was found. A high expression level of CD46 may protect tumor cells entering the circulation during the metastatic process. Because deposition of C3b and inactivated C3b on these tumor cells is low or absent, the elimination by CR1- or CR3-positive effector cells through recognition of these C3 fragments will be reduced.
The presence of C3d and C5b-9 on renal tumor cells demonstrated that complement activation at the tumor site had occurred. It has been shown that large numbers of macrophages are present in the cellular infiltrate of renal cell carcinoma (Van Ravenswaay Claasen et al, 1992). These cells have been shown to be involved in eradication of tumor cells opsonized with C3 fragments (Bara and Lint, 1987). Despite the presence of C3 fragments on the tumor cell membrane, the RCC are not eradicated by the immune system. This suggests that complement-mediated responses at the tumor site (eg, opsonisation of tumor cells with C3b or inactivated C3b, production of the anaphylatoxin C5a, and cell lysis) may be limited because of overexpression of mCRP on the renal tumor cells.
In conclusion, the results of this study have shown that the expression of CD55 and CD59 is increased in renal clear cell carcinoma, which may contribute to the progression of these tumors. Furthermore, frequently C3d and occasionally C5b-9 were present on renal tumor cells in situ, suggesting that the complement system is involved in the immune reaction against RCC. A statistically significant association was observed between a high C3d deposition and a low expression level of CD46. The expression level of CD46 was found to be significantly associated with tumor stage. Based upon these results, we suggest that it is important to develop strategies to functionally block or down-regulate mCRP, to enhance the efficacy of potential mAb-mediated immunotherapy of RCC.
Materials and Methods
Tissue Specimens and Processing
Human RCC specimens and matching normal renal tissue were obtained from 31 patients who underwent radical nephrectomy. The following RCC subtypes were investigated: 18 clear cell carcinomas, 12 chromophobe carcinomas, and 1 mixed carcinoma (clear cell and chromophobe) (Störkel et al, 1997). Tumor grade was defined as nuclear-differentiation grade 1 to 4, according to Fuhrman et al (1982). The tumors used were staged as T1 and T2 (tumor limited to the kidney; noninvasive) and stage T3 (invasive), according to the most recent TNM staging for renal cell carcinoma (Hermanek et al, 1997). After surgical removal, the kidney was placed on ice. Macroscopically normal tissue was obtained at a site distant from the tumor. Tumor specimens for flow cytometric analysis of mCRP expression were minced and treated overnight with collagenase 1A (Sigma, St. Louis, Missouri) and DNAse (Sigma), according to the method described by Terachi et al (1991). The dissociated tumor specimen was filtered through a wire sieve. Erythrocytes were removed from the suspension by treatment for 5 minutes at 4° C) with a solution of 0.16 M NH4Cl, 10 mm KHCO3, and 0.13 mm EDTA. Cell suspensions were stored at −70° C in 80% heat-inactivated fetal bovine serum/20% DMSO until use. Both tumor and normal tissue were snap-frozen in liquid isopentane on dry ice and stored at −70° C until use.
Antibodies
The following antibodies were used: J4–48 (IgG1), directed against CD46 (CLB, Amsterdam, The Netherlands); BRIC216 (IgG1), directed against CD55, and BRIC229 (IgG2b), directed against CD59 (BPL Commercial Department, Elstree, United Kingdom); G250 mAb (IgG2a), directed against the renal tumor-associated antigen G250 (developed at our department) (Oosterwijk et al, 1986); CLB-T200/1,15D9 (IgG1) directed against CD45 (CLB); anti-human C3d (IgG1) (Quidel Corporation, San Diego, California); aE11 (IgG2a), directed against human C5b-9 (Dako); isotype-specific anti-asparagus mAb (Dako); FITC-labeled goat F(ab′)2 anti-mouse IgG1, FITC-labeled goat F(ab′)2 anti-mouse IgG2b, and PE-labeled goat F(ab′)2 anti-mouse IgG2a (Biotechnology Associate, Birmingham, Alabama); Alexa 594-labeled goat-anti-mouse IgG (Molecular Probes, Leiden, The Netherlands); and horseradish peroxidase (HRP) rabbit-anti-mouse Ig EnVision+ kit (Dako).
Treatment of tissue specimens
Immunohistochemistry
Cryostat sections of 5 μm were dried for 1 hour at 50° C and subsequently placed overnight in a 60° C oven. Sections were fixed in acetone for 10 minutes. Sections were washed twice with PBS for 5 minutes and then incubated with predetermined concentrations of primary antibody diluted in PBS containing 1% BSA (PBS/1%BSA) for 1 hour. Sections were washed three times for 5 minutes with PBS. Subsequently sections were incubated for 30 minutes with HRP and rabbit-anti-mouse Ig both coupled to the Dako EnVision+ system. After three washes with PBS, sections were washed once with 0.05 M Tris-HCl, pH 7.6. Sections were developed with diamino-benzidine-tetrahydrochloride for 10 minutes. The reaction was stopped with PBS. Sections were counterstained with Mayer’s hematoxylin. The intensity of the color was scored as negative (0), weak (1), moderate (2), or strong (3) staining. The percentage of positive cells was scored as sporadic (1, 1–5%), local (2, 6–25%), occasional (3, 26–50%), majority (4, 51–75%), or large majority (5, 76–100%) (Ruiter et al, 1998). Isotype-specific anti-asparagus mAb did not show reactivity with the tissue sections. Sections in which the primary mAb was omitted were included in all experiments as negative controls. As a positive control for the presence of C3d and C5b-9 mAb, kidney tissue from a patient with glomerulonephritis was used.
Immunofluorescence
Cryostat sections of 5 μm were dried for 1 hour at 50° C and subsequently placed overnight in a 60° C oven. Sections were fixed in acetone for 10 minutes. Nonspecific binding was blocked with PBS/1% BSA for 1 hour. Sections were incubated with primary antibody diluted in PBS/1%BSA for 2 hours. After washing five times with PBS (5 minutes/wash), sections were incubated with Alexa 594-labeled secondary antibody for 1 hour. Subsequently, sections were washed five times with PBS (12 minutes/wash), rinsed three times in milli-Q water, and dried overnight. Finally, sections were mounted in Vectashield (Vector Laboratories, Inc., Burlingame, California) and analyzed with the BRC-600 confocal system (Bio-Rad Laboratories, Richmond, California), equipped with a Nikon fluorescence microscope (Nikon Europe B.V., Badhoevedorp, The Netherlands). Photos were taken at a constant pinhole and after 10 Kalman. Sections in which the primary mAb was omitted were included in all experiments as negative controls. The intensity of immunofluorescent signals was converted to pseudocolors, using the Photostyler 2.0 program (Adobe Systems Inc, Seattle, Washington).
Flow Cytometry
Cells (2 4 × 105) were incubated with a 100 μl mixture of primary antibodies diluted in PBS/0.5%BSA for 30 minutes at 4° C. Cells were washed twice with PBS/0.5%BSA and incubated with 100 μl of a mixture of secondary antibodies for 30 minutes at 4° C. After washing, the cells were resuspended in 250 μl PBS/0.5%BSA containing 1 μg/ml propidium iodide (PI) to stain dead cells. Isotype-specific negative control mAb were used to correct for nonspecific reactivity. Specimens were measured on the FACSCalibur (Becton Dickinson, San Jose, California). Ten thousand events of G250-positive tumor cells were counted. FITC-positive cells were measured on FL1:BP530/30 nm (green fluorescence). PE-positive cells were measured on FL2: BP585/42 nm (orange fluorescence). PI-positive (dead) cells were measured on FL3: LP 650 nm (red fluorescence). Fluorescence compensation was used to correct for spectral cross-talk between the fluorescent signals. Data are expressed in molecules of equivalent soluble fluorescence values calculated on the basis of a flow cytometry standardization kit, Quantum 25 FITC (Flow Cytometry Standards Europe, Leiden, The Netherlands). Tumor cells were distinguished from other cells by selecting only cells positive for the renal tumor-associated antigen G250. The fraction of PI-negative cells in the cell suspension consisted of G250-positive tumor cells (10–25%), leukocytes (approximately 50%), and the remaining cell population (25–40%) probably containing stromal cells (fibroblasts) and endothelial cells.
Statistical Analysis
Associations between mCRP expression and tumor stage, tumor grade, or complement deposition were evaluated by Fisher’s exact test; p values less than 0.05 were considered statistically significant.
References
Azuma A, Yamano Y, Yoshimura A, Hibino T, Nishida T, Yagita H, Okumura K, Seya T, Kannagi R, Shibuya M, and Kudoh S (1995). Augmented lung adenocarcinoma cytotoxicity by the combination of a genetically modified anti-Lewis Y antibody and antibodies to complement regulatory proteins. Scand J Immunol 42: 202–208.
Bander NH, Finstad CL, Cordon Cardo C, Ramsawak RD, Vaughan ED, Jr ., Whitmore WF, Jr ., Oettgen HF, Melamed MR, and Old LJ (1989). Analysis of a mouse monoclonal antibody that reacts with a specific region of the human proximal tubule and subsets renal cell carcinomas. Cancer Res 49: 6774–6780.
Bara S and Lint TF (1987). The third component of complement (C3) bound to tumor target cells enhances their sensitivity to killing by activated macrophages. J Immunol 138: 1303–1309.
Bjørge L, Hakulinen J, Wahlström T, Matre R, and Meri S (1997). Complement-regulatory proteins in ovarian malignancies. Int J Cancer 70: 14–25.
Blok VT, Daha MR, Tijsma O, Harris CL, Morgan BP, Fleuren GJ, and Gorter A (1998). Bispecific monoclonal antibody directed against both the membrane-bound complement regulator CD55 and the renal tumor-associated antigen G250 enhances C3 deposition and tumor cell lysis by complement. J Immunol 160: 3437–3443.
Bono AV and Lovisolo JAJ (1997). Renal cell carcinoma-Diagnosis and treatment: State of the art. Eur Urol 31: 47–55.
Brasoveanu LI, Altomonte M, Gloghini A, Fonsatti E, Coral S, Gasparollo A, Montagner R, Cattarossi I, Simonelli C, Cattelan A, Attadia V, Carbone A, and Maio M (1995). Expression of protectin (CD59) in human melanoma and its functional role in cell- and complement-mediated cytotoxicity. Int J Cancer 61: 548–556.
Brasoveanu LI, Altomonte M, Fonsatti E, Colizzi F, Coral S, Nicotra MR, Cattarossi I, Cattelan A, Natali PG, and Maio M (1996). Levels of cell membrane CD59 regulate the extent of complement-mediated lysis of human melanoma cells. Lab Invest 74: 33–42.
Bukowski RM (1997). Natural history and therapy of metastatic renal cell carcinoma: the role of interleukin-2. Cancer 80: 1198–1220.
Bukowski RM, Olencki T, Wang Q, Peereboom D, Budd GT, Elson P, Sandstrom K, Tuason L, Rayman P, Tubbs R, McLain D, Klein E, Novick A, and Finke J (1997). Phase II trial of interleukin-2 and interferon-a in patients with renal cell carcinoma: Clinical results and immunologic correlates of response. J Immunother 20: 301–311.
Cheung N-KV, Walter EI, Smith-Mensah WH, Ratnoff WD, Tykocinski ML, and Medof ME (1988). Decay-accelerating factor protects human tumor cells from complement-mediated cytotoxicity in vitro. J Clin Invest 81: 1122–1128.
Devaux P, Christiansen D, Fontaine M, and Gerlier D (1999). Control of C3b and C5b deposition by CD46 (membrane cofactor protein) after alternative but not classical complement activation. Eur J Immunol 29: 815–822.
Dillman RO (1994). Antibodies as cytotoxic therapy. J Clin Oncol 12: 1497–1515.
Figlin RA (1999). Renal cell carcinoma: Management of advanced disease. J Urol 161: 381–386.
Fuhrman SA, Lasky LC, and Limas C (1982). Prognostic significance of morphologic parameters in renal cell carcinoma. Am J Surg Pathol 6: 655–663.
Gorter A, Blok VT, Haasnoot WHB, Ensink NG, Daha MR, and Fleuren GJ (1996). Expression of CD46, CD55, and CD59 on renal tumor cell lines and their role in preventing complemented-mediated tumor cell lysis. Lab Invest 74: 1039–1049.
Gorter A and Meri S (1999). Immune evasion of tumor cells using membrane-bound regulatory proteins. Immunol Today 20: 576–582.
Hermanek P, Hutter RVP, Sobin LH, Wagner G, and Wittekind Ch (1997). Urological tumours: Kidney. In: Hermanek P, Hutter RVP, Sobin LH, Wagner G, and Wittekind Ch, editors. TNM Atlas: Illustrated guide to the TNM/pTNM classification of malignant tumours. 4th ed. Berlin, Heidelberg, New York: Springer-Verlag, 296–302.
Holthöfer H, Miettinen A, Paasivuo R, Lehto VP, Linder E, Alfthan O, and Virtanen I (1983). Cellular origin and differentiation of renal carcinomas. A fluorescence microscopic study with kidney-specific antibodies, antiintermediate filament antibodies, and lectins. Lab Invest 49: 317–326.
Hrouda D, Muir GH, and Dalgleish AG (1997). The role of immunotherapy for urological tumours. Br J Urol 79: 307–316.
Ichida S, Yuzawa Y, Okada H, Yoshioka K, and Matsuo S (1994). Localization of the complement regulatory proteins in the normal human kidney. Kidney Int 46: 89–96.
Kumar S, Vinci JM, Pytel BA, and Baglioni C (1993). Expression of messenger RNAs for complement inhibitors in human tissues and tumors. Cancer Res 53: 348–353.
Liszewski MK, Farries TC, Lublin DM, Rooney IA, and Atkinson JP (1996). Control of the complement system. Adv Immunol 61: 201–283.
Mäenpää A, Junnikkala S, Hakulinen J, Timonen T, and Meri S (1996). Expression of complement membrane regulators membrane cofactor protein (CD46), decay accelerating factor (CD55), and protectin (CD59) in human malignant gliomas. Am J Pathol 148: 1139–1152.
Motzer RJ, Bander NH, and Nanus DM (1996). Renal-cell carcinoma. N Engl J Med 335: 865–875.
Nakanishi I, Moutabarrik A, Hara T, Hatanaka M, Hayashi T, Syouji T, Okada N, Kitamura E, Tsubakihara Y, Matsumoto M, and Seya T (1994). Identification and characterization of membrane cofactor protein (CD46) in the human kidneys. Eur J Immunol 24: 1529–1535.
Niehans GA, Cherwitz DL, Staley NA, Knapp DJ, and Dalmasso AP (1996). Human carcinomas variably express the complement inhibitory proteins CD46 (membrane cofactor protein), CD55 (decay-accelerating factor), and CD59 (protectin). Am J Pathol 149: 129–142.
Oosterwijk E, Ruiter DJ, Hoedemaeker PJ, Pauwels EKJ, Jonas U, Zwartendijk J, and Warnaar SO (1986). Monoclonal antibody G250 recognizes a determinant present in renal cell carcinoma and absent from normal kidney. Int J Cancer 38: 489–494.
Oosterwijk E, Bander NH, Divgi CR, Welt S, Wakka JC, Finn RD, Carswell EA, Larson SM, Warnaar SO, Fleuren GJ, Oettgen HF, and Old LJ (1993). Antibody localization in human renal cell carcinoma: a phase I study of monoclonal antibody G250. J Clin Oncol 11: 738–750.
Pittman K and Selby P (1994). The management of renal cell carcinoma. Crit Rev Oncol Hematol 16: 181–200.
Ruiter DJ, Ferrier CM, Van Muijen GNP, Henzen-Logmans SC, Kennedy S, Kramer MD, Nielsen BS, Schmitt M, and Eur BIOMED-1 Concert Act Clin Relev (1998). Quality control of immunohistochemical evaluation of tumour-associated plasminogen activators and related components. Eur J Cancer 34: 1334–1340.
Steffens MG, Boerman OC, Oosterwijk-Wakka JC, Oosterhof GON, Witjes JA, Koenders EB, Oyen WJG, Buijs WCAM, Debruyne FMJ, Corstens FHM, and Oosterwijk E (1997). Targeting of renal cell carcinoma with iodine-131-labeled chimeric monoclonal antibody G250. J Clin Oncol 15: 1529–1537.
Störkel S, Eble JN, Adlakha K, Amin M, Blute ML, Bostwick DG, Darson M, Delahunt B, and Iczkowski K (1997). Classification of renal cell carcinoma: Workgroup No. 1. Union Internationale Contre le Cancer (UICC) and the American Joint Committee on Cancer (AJCC). Cancer 80: 987–989.
Terachi T, Stanescu G, Pontes JE, Medof ME, and Caulfield MJ (1991). Coexistence of autologous antibodies and decay-accelerating factor, an inhibitor of complement, on human renal tumor cells. Cancer Res 51: 2521–2523.
Van Ravenswaay Claasen HH, Kluin PM, and Fleuren GJ (1992). Tumor infiltrating cells in human cancer: On the possible role of CD16+ macrophages in antitumor cytotoxicity. Lab Invest 67: 166–174.
Varsano S, Frolkis I, and Ophir D (1995). Expression and distribution of cell-membrane complement regulatory glycoproteins along the human respiratory tract. Am J Respir Crit Care Med 152: 1087–1093.
Venneker GT, Vodegel RM, Okada N, Westerhof W, Bos JD, and Asghar SS (1998). Relative contributions of decoy accelerating factor (DAF), membrane cofactor protein (MCP) and CD59 in the protection of melanocytes from homologous complement. Immunobiology 198: 476–484.
Acknowledgements
The authors thank Ms. Colette M.A.N. Blonk-Beckers for technical assistance, and Dr. M. Veselic-Charvath and Dr. V.T.H.B.M. Smit for determining tumor grade.
This study was supported by the Dutch Kidney Foundation, grant C94.1374.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Blok, V., Daha, M., Tijsma, O. et al. A Possible Role of CD46 for the Protection In Vivo of Human Renal Tumor Cells from Complement-Mediated Damage. Lab Invest 80, 335–344 (2000). https://doi.org/10.1038/labinvest.3780038
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1038/labinvest.3780038
This article is cited by
-
Context-dependent roles of complement in cancer
Nature Reviews Cancer (2019)
-
Expression of complement regulatory proteins: CD46, CD55, and CD59 and response to rituximab in patients with CD20(+) non-Hodgkin’s lymphoma
Medical Oncology (2010)
-
The Inhibitory Effect of CD46, CD55, and CD59 on Complement Activation After Immunotherapeutic Treatment of Cervical Carcinoma Cells with Monoclonal Antibodies or Bispecific Monoclonal Antibodies
Laboratory Investigation (2002)