Abstract
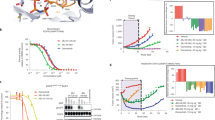
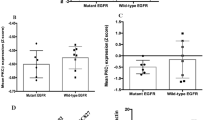
Mutations in the kinase domain of epidermal growth factor receptor (EGFR) are associated with clinical responsiveness to gefitinib in patients with non-small-cell lung cancers (NSCLC). Recently, we have identified many novel EGFR mutations in NSCLC tissues. In this study, we found that gefitinib could suppress the tyrosine phosphorylation of most EGFR mutants better than the wild-type receptor. However, gefitinib had quite variable growth-suppressive effects on different EGFR mutant-expressing cells. All tested EGFR mutants have high basal phosphorylation at multiple tyrosine residues. Upon EGF stimulation, the mutated EGFRs did not have apparently stronger phosphorylation at tyrosines 845, 992, 1068, and 1173 than the wild-type receptor. However, stronger phosphorylation at tyrosine 1045 was observed in the S768I, L861Q, E709G, and G719S mutants. The E746-A750 deletion mutant was less responsive to EGF than the wild-type and other mutant receptors. The S768I, L861Q, E709G, and G719S mutants were refractory to EGF-induced ubiquitination and had more sustained tyrosine phosphorylation. E709G and G719S also lacked EGF-induced receptor downregulation. Our results indicate that, in addition to sensitivity to gefitinib, EGFR mutations also caused various changes in EGFR's regulatory mechanisms, which may contribute to the constitutive activation of EGFR mutants and oncogenesis in NSCLC.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 50 print issues and online access
$259.00 per year
only $5.18 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout








Similar content being viewed by others
Accession codes
Abbreviations
- EGF:
-
epidermal growth factor
- EGFR:
-
EGF receptor
- FCS:
-
fetal calf serum
- HA:
-
hemagglutinin
- IC50:
-
concentration of 50% inhibition
- NSCLC:
-
non-small-cell lung cancer
- TGF-α:
-
transforming growth factor-α
- Tyr:
-
tyrosine
References
Amann J, Kalyankrishna S, Massion PP, Ohm JE, Girard L, Shigemastsu H et al. (2005). Cancer Res 65: 226–235.
Brabender J, Danenberg KD, Metzger R, Schneider PM, Park JS, Salonga D et al. (2001). Clin Cancer Res 7: 1850–1855.
Chen Y-R, Han J, Kori R, Tan T-H . (2002). J Biol Chem 277: 39334–39342.
Duan L, Miura Y, Dimri M, Majumder B, Dodge IL, Reddi AL et al. (2003). J Biol Chem 278: 28950–28960.
Fabian MA, Biggs WHI, Treiber DK, Ateridge CE, Azimioara MD, Benedetti MG et al. (2005). Nat Biotechnol 23: 329–336.
Fontanini G, De Laurentiis M, Vignati S, Chine S, Lucchi M, Silvestri V et al (1998). Clin Cancer Res 4: 241–249.
Fukuoka M, Yano S, Giaccone G, Tamura T, Nakagawa K, Douillard JY et al. (2003). J Clin Oncol 21: 2237–2246.
Haglund K, Sigismund S, Polo S, Szymkiewics I, Di Fiore PP, Dikic I . (2003). Nat Cell Biol 5: 461–466.
Herbst RS, Bunn PAJ . (2003). Clin Cancer Res 9: 5813–5824.
Herbst RS, Maddox AM, Rothenberg ML, Small EJ, Rubin EH, Baselga J et al. (2002). J Clin Oncol 20: 3815–3825.
Hirsch FR, Varella-Garcia M, Bunn PA, Di Maria MV, Veve R, Bremmes RM et al. (2003). J Clin Oncol 21: 2237–2246.
Holbro T, Hynes NE . (2003). Ann Rev Pharmacol Toxicol 44: 195–217.
Huang S-F, Liu H-P, Li L-H, Ku Y-C, Fu Y-N, Tsai H-Y et al. (2004). Clin Cancer Res 10: 8195–8203.
Jiang X, Sorkin A . (2003). Traffic 4: 529–543.
Kosaka T, Yatabe Y, Endoh H, Kuwano H, Takahashi T, Mitsudomi T . (2004). Cancer Res 64: 8919–8923.
Kris MG, Natale RB, Herbst RS, Lynch TJJ, Prager D, Belani CP et al. (2003). JAMA 290: 2149–2158.
Lai WW, Chen FF, Wu M, Chow NH, Su WC, Ma MC et al. (2001). Ann Throac Surg 72: 1868–1876.
Levkowitz G, Waterman H, Ettenberg SA, Katz M, Tsygankov AY, Alroy I et al. (1999). Mol Cell 4: 1029–1040.
Lynch TJ, Bell DW, Sordella R, Gurubhagavatula S, Okimoto RA, Brannigan BW et al. (2004). N Engl J Med 350: 2129–2139.
Mitsudomi T, Kosaka T, Endoh H, Horio Y, Hida T, Mpri S et al. (2005). J Clin Oncol 23: 2513–2520.
Mosesson Y, Shtiegman K, Katz M, Zwang Y, Vereb G, Szollosi J et al. (2003). J Biol Chem 278: 21323–21326.
Nakagawa KTT, Negoro S, Kudoh S, Yamamoto N, Yamamoto N, Takeda K et al. (2003). Ann Oncol 14: 922–930.
Nicholson RI, Gee JM, Harper ME . (2001). Eur J Cancer 37: S9–S15.
Paez JG, Janne PA, Lee JC, Tracy S, Greulich H, Gabriel S et al. (2004). Science 304: 1497–1500.
Pao W, Miller V, Zakowski MF, Doherty J, Politi K, Sarkara I et al. (2004). Proc Natl Acad Sci USA 101: 13306–13311.
Pierce JH, Ruggiero M, Fleming TP, Di Fiore PP, Greenberger JS, Varticovski L et al. (1988). Science 239: 628–631.
Rusch V, Baselga J, Cordon-Cardo C, Orazem J, Zaman M, Hoda S et al. (1993). Cancer Res 53: 2379–2385.
Sigismund S, Woelk T, Puri C, Maspero E, Tacchetti C, Transidico P et al. (2005). Proc Natl Acad Sci USA 102: 2760–2765.
Sordella R, Bell DW, Haber DASJ . (2004). Science 305: 1163–1167.
Acknowledgements
We are grateful to AstraZeneca for providing gefitinib, to Drs M-C Hung and L-M Wang for the generous gift and helpful discussion, to Dr K-D Lee for technical assistance to this research, to Dr H-M Shih for valuable suggestions, to Ms L-M Huang and Ms C-W Kang for secretarial help. This work was supported by grants from National Health Research Institutes (MG-093-PP-08 and MG-093-PP-07 to SF Huang and Y-R Chen, respectively), Department of Health (DOH94-TD-G-111-016 to Y-R Chen), and National Science Council, Taiwan (NHRI92A1-NSCCA16-5 to S-F Tsai).
Author information
Authors and Affiliations
Corresponding author
Additional information
Supplementary Information accompanies the paper on Oncogene website (http://www.nature.com/onc)
Rights and permissions
About this article
Cite this article
Chen, YR., Fu, YN., Lin, CH. et al. Distinctive activation patterns in constitutively active and gefitinib-sensitive EGFR mutants. Oncogene 25, 1205–1215 (2006). https://doi.org/10.1038/sj.onc.1209159
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.onc.1209159
Keywords
This article is cited by
-
DUSP3 regulates phosphorylation-mediated degradation of occludin and is required for maintaining epithelial tight junction
Journal of Biomedical Science (2022)
-
Investigation of therapeutic modalities of G719X, an uncommon mutation in the EGFR gene in non-small cell lung cancer
Oncology and Translational Medicine (2019)
-
The exon 19-deleted EGFR undergoes ubiquitylation-mediated endocytic degradation via dynamin activity-dependent and -independent mechanisms
Cell Communication and Signaling (2018)
-
Efficacy of EGFR tyrosine kinase inhibitors in non-small cell lung cancer patients harboring different types of EGFR mutations: A retrospective analysis
Current Medical Science (2017)
-
Combined analysis of rearrangement of ALK, ROS1, somatic mutation of EGFR, KRAS, BRAF, PIK3CA, and mRNA expression of ERCC1, TYMS, RRM1, TUBB3, EGFR in patients with non-small cell lung cancer and their clinical significance
Cancer Chemotherapy and Pharmacology (2016)