Abstract
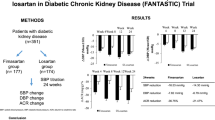
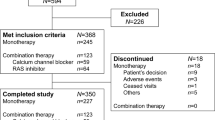
We examined the effects of increasing the recommended initial doses of angiotensin-converting enzyme inhibitors (ACEIs) or angiotensin receptor blockers (ARBs), or of switching to combination therapy with both drugs, on diabetic nephropathy. Hypertensive type 2 diabetic patients with urinary albumin excretion (ACR) between 100 and 300 mg/g creatinine (Cre) were assigned to the following five groups in which an antihypertensive drug was administered at a recommended initial dose for 48 weeks, and then either the dose was doubled or an additional drugs was added to regimen for the following 48 weeks: N, nifedipine-CR (N) 20 mg/day (initial dose); T, ACEI temocapril (T) 2 mg/day; C, ARB candesartan (C) 4 mg/day; T+C, T first and then addition of C; C+T, C first and then addition of C. ACR decreased in the T (n=34), C (n=40), T+C (n=37) and C+T (n=35) groups, but not in the N group (n=18). However, the anti-proteinuric effect was less in the T than in the C, T+C or C+T groups, while no differences existed among the latter three. In each group, there were significant linear relationships between attained BP and ACR; however, the regression lines were shifted toward lower ACR level in the renin-angiotensin system–inhibition groups compared with the N group. These results indicate that an ACEI and/or ARB is superior to a CCB in retarding diabetic nephropathy, while the combination of low doses of ACEI and ARB has effects similar to those of high-dose ARB. Even among patients treated with an ACEI and/or ARB, lowering BP is important.
Similar content being viewed by others
Article PDF
References
Taguma Y, Kitamoto Y, Futaki G, et al: Effect of captopril on heavy proteinuria in azotemic diabetics. N Engl J Med 1985; 26: 1617–1620.
Brenner BM, Cooper ME, de Zeeuw D, et al, RENAAL Study Investigators : Effects of losartan on renal and cardiovascular outcomes in patients with type 2 diabetes and nephropathy. N Engl J Med 2001; 12: 861–869.
Rossing K, Schjoedt KJ, Jensen BR, et al, Collaborative Study Group: Renoprotective effect of the angiotensin-receptor antagonist irbesartan in patients with nephropathy due to type 2 diabetes. N Engl J Med 2001; 12: 851–860.
Viberti G, Wheeldon NM, MicroAlbuminuria Reduction with VALsartan (MARVAL) Study Investigators : Microalbuminuria reduction with valsartan in patients with type 2 diabetes mellitus: a blood pressure–independent effect. Circulation 2002; 6: 672–678.
Horita Y, Tadokoro M, Taura K, et al: Low-dose combination therapy with temocapril and losartan reduces proteinuria in normotensive patients with immunoglobulin a nephropathy. Hypertens Res 2004; 27: 693–970.
Parving HH, Lehnert H, Brochner-Mortensen J, et al, Irbesartan in Patients with Type 2 Diabetes and Microalbuminuria Study Group: The effect of irbesartan on the development of diabetic nephropathy in patients with type 2 diabetes. N Engl J Med 2001; 12: 870–878.
Rossing K, Schjoedt KJ, Jensen BR, Boomsma F, Parving HH : Enhanced renoprotective effects of ultrahigh doses of irbesartan in patients with type 2 diabetes and microalbuminuria. Kidney Int 2005; 3: 1190–1198.
Mogensen CE, Neldam S, Tikkanen I, et al: Randomised controlled trial of dual blockade of renin-angiotensin system in patients with hypertension, microalbuminuria, and non-insulin dependent diabetes: the candesartan and lisinopril microalbuminuria (CALM) study. BMJ 2000; 321: 1440–1444.
Andersen NH, Poulsen PL, Knudsen ST, et al: Long-term dual blockade with candesartan and lisinopril in hypertensive patients with diabetes: the CALM II study. Diabetes Care 2005; 2: 273–277.
Rossing K, Christensen PK, Jensen BR, et al: Dual blockade of the renin-angiotensin system in diabetic nephropathy: a randomized double-blind crossover study. Diabetes Care 2002; 1: 95–100.
Ferrari P, Marti HP, Pfister M, et al: Additive antiproteinuric effect of combined ACE inhibition and angiotensin II receptor blockade. J Hypertens 2002; 1: 125–130.
Cetinkaya R, Odabas AR, Selcuk Y : Anti-proteinuric effects of combination therapy with enalapril and losartan in patients with nephropathy due to type 2 diabetes. Int J Clin Pract 2004; 5: 432–435.
Adler AI, Stevens RJ, Manley SE, et al, UKPDS Group: Development and progression of nephropathy in type 2 diabetes: the United Kingdom Prospective Diabetes Study (UKPDS 64). Kidney Int 2003; 1: 225–232.
Chobanian AV, Bakris GL, Black HR, et al, National Heart, Lung, and Blood Institute Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure; National High Blood Pressure Education Program Coordinating Committee : The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure: the JNC 7 report. JAMA 2003; 19: 2560–2572.
Casas JP, Chua W, Loukogeorgakis S, et al: Effect of inhibitors of the renin-angiotensin system and other antihypertensive drugs on renal outcomes: systematic review and meta-analysis. Lancet 2005; 366: 2026–2033.
Nosadini R, Tonolo G : Cardiovascular and renal protection in type 2 diabetes mellitus: the role of calcium channel blockers. J Am Soc Nephrol 2002; 13: S216–S223.
Schrier RW, Estacio RO, Esler A, et al: Effects of aggressive blood pressure control in normotensive type 2 diabetic patients on albuminuria, retinopathy and strokes. Kidney Int 2002; 3: 1086–1097.
Ruggenenti P, Fassi A, Ilieva AP, et al, Bergamo Nephrologic Diabetes Complications Trial (BENEDICT) Investigators : Preventing microalbuminuria in type 2 diabetes. N Engl J Med 2004; 19: 1941–1951.
Dahlof B, Devereux RB, Kjeldsen SE, et al: Cardiovascular morbidity and mortality in the Losartan Intervention For Endpoint reduction in hypertension study (LIFE): a randomised trial against atenolol. Lancet 2002; 359: 995–1003.
Sato A, Hayashi K, Naruse M, et al: Effectiveness of aldosterone blockade in patients with diabetic nephropathy. Hypertension 2003; 1: 64–68.
Miyazaki M, Takai S : Role of chymase on vascular proliferation. J Renin Angiotensin Aldosterone Syst 2000; 1: 23–26.
MacFadyen RJ, Lee AF, Morton JJ, et al: How often are angiotensin II and aldosterone concentrations raised during chronic ACE inhibitor treatment in cardiac failure? Heart 1999; 1: 57–61.
Fujisawa T, Ikegami H, Ono M, et al: Combination of half doses of angiotensin type 1 receptor antagonist and angiotensin-converting enzyme inhibitor in diabetic nephropathy. Am J Hypertens 2005; 1: 13–17.
Liu YH, Yang XP, Sharov VG, et al: Effects of angiotensin-converting enzyme inhibitors and angiotensin II type 1 receptor antagonists in rats with heart failure. Role of kinins and angiotensin II type 2 receptors. J Clin Invest 1997; 8: 1926–1935.
Wiemer G, Scholkens BA, Becker RH : Converting enzyme inhibitor–stimulated formation of nitric oxide and prostacyclin in endothelial cells from bovine aorta is mediated by endothelium-derived bradykinin. Agents Actions Suppl 1992; 38: 196–200.
Kohno M, Yokokawa K, Minami M, et al: Plasma levels of nitric oxide and related vasoactive factors following long-term treatment with angiotensin-converting enzyme inhibitor in patients with essential hypertension. Metabolism 1999; 10: 1256–1259.
Rasoul S, Carretero OA, Peng H, et al: Antifibrotic effect of Ac-SDKP and angiotensin-converting enzyme inhibition in hypertension. J Hypertens 2004; 3: 593–603.
Rhaleb NE, Peng H, Harding P, et al: Effect of N-acetyl-seryl-aspartyl-lysyl-proline on DNA and collagen synthesis in rat cardiac fibroblasts. Hypertension 2001; 3: 827–832.
Ogawa S, Mori T, Nako K, et al: Angiotensin II type 1 receptor blockers reduce urinary oxidative stress markers in hypertensive diabetic nephropathy. Hypertension 2006; 47: 699–705.
Yagi S, Morita T, Katayama S, et al: Combined treatment with an AT1 receptor blocker and angiotensin converting enzyme inhibitor has an additive effect on inhibiting neointima formation via improvement of nitric oxide production and suppression of oxidative stress. Hypertens Res 2004; 27: 129–135.
Gaede P, Tarnow L, Vedel P, et al: Remission to normoalbuminuria during multifactorial treatment preserves kidney function in patients with type 2 diabetes and microalbuminuria. Nephrol Dial Transplant 2004; 19: 2784–2788.
Rossing K, Christensen PK, Hovind P, et al: Remission of nephrotic-range albuminuria reduces risk of end-stage renal disease and improves survival in type 2 diabetic patients. Diabetologia 2005; 11: 2241–2247.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ogawa, S., Takeuchi, K., Mori, T. et al. Effects of Monotherapy of Temocapril or Candesartan with Dose Increments or Combination Therapy with Both Drugs on the Suppression of Diabetic Nephropathy. Hypertens Res 30, 325–334 (2007). https://doi.org/10.1291/hypres.30.325
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1291/hypres.30.325
Keywords
This article is cited by
-
Efficacy and Safety of Dual Blockade of the Renin–Angiotensin–Aldosterone System in Diabetic Kidney Disease: A Meta-Analysis
American Journal of Cardiovascular Drugs (2019)
-
Chapter 6. Hypertension associated with organ damage
Hypertension Research (2014)
-
The impact of renin–angiotensin–aldosterone system inhibitors on Type 1 and Type 2 diabetic patients with and without early diabetic nephropathy
Kidney International (2012)
-
Early Treatment With Olmesartan Prevents Juxtamedullary Glomerular Podocyte Injury and the Onset of Microalbuminuria in Type 2 Diabetic Rats
American Journal of Hypertension (2012)
-
Reno-protective effects of renin–angiotensin system blockade in type 2 diabetic patients: a systematic review and network meta-analysis
Diabetologia (2012)