Case Study

PART 1 Oral cavity, pharynx and esophagus
GI Motility online (2006) doi:10.1038/gimo80
Published 16 May 2006
A patient with dysphagia to solids and liquids
Ikuo Hirano, M.D.
About the contributor
Case description
The patient is a 43-year-old man with hypertension and a 5-year history of dysphagia. Foods, especially solids but occasionally liquids, are sticking at the level of his upper sternum with every meal. He is usually able to get the food down with repeated swallows or by drinking water. More recently, he has noticed the spontaneous regurgitation of clear, foamy liquid and undigested food into his mouth, especially when bending over after dinner. His wife has noted that he coughs at night and has lost 7 to 8 lb.
Additional complaints include episodes of chest "seizures," characterized as a squeezing pain without radiation, that can occur at any time of day. These episodes last for several minutes to 1 hour and are unrelated to physical activity or meals. Drinking cold water sometimes helps alleviate the pain.
The patient denies either heartburn or odynophagia but does report an inability to belch. He traveled to Mexico one month before the onset of the dysphagia. His past medical history is unremarkable, but he does have a smoking history of 20 packs per year. His physical examination is unremarkable.
Q1. What is the mostly likely diagnosis and differential diagnosis?
Barium swallow and esophageal motility studies were obtained.
Q2. Is the selection of these tests appropriate?
The barium swallow is shown in Figure 1.
Q3. What is your interpretation of the barium swallow?
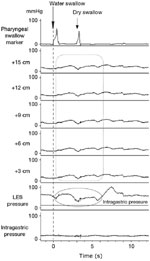
The esophageal motility study is shown in Figure 2.
Q4. What is your interpretation of the esophageal motility study?
Q5. What is your differential diagnosis after these studies?
Q6. Explain the pathophysiology of this condition.
Q7. What are possible explanations for the episodes of chest pain?
Q8. Discuss the treatment options available.
After detailed discussions on the various treatment options, the patient undergoes an uneventful laparoscopic Heller myotomy with Dor fundoplasty. He is discharged on postoperative day 1. On follow-up 4 weeks later, the patient reports substantial improvements in his dysphagia but does note some delay in the transit of solid food in his lower chest region. The food usually passes after several seconds and is aided by drinking liquid. He denies heartburn although he has been taking a proton pump inhibitor since the surgery. The chest pain episodes remain unchanged in terms of frequency or severity. His nocturnal coughing and postprandial regurgitation have completely resolved and he has been gradually gaining weight.
Q9. Why is empiric therapy with a proton pump inhibitor a reasonable recommendation for the patient?
A follow-up barium swallow is performed and demonstrates free passage of barium through a patent gastroesophageal junction with intact fundoplasty. The patient is reassured and scheduled for follow-up in 1 year.
Ten years later, the patient is referred again by his primary care physician with complaints of increasing dysphagia, predominantly for solid food. His symptoms have been worsening over the past few months. His prior chest pain is now very infrequent and of lesser severity. He denies weight loss.
Q10. What are the causes of postoperative dysphagia?