Abstract
Obsessive-compulsive disorder (OCD) is one of the most debilitating psychiatric conditions. An extensive body of the literature has described some of the neurobiological mechanisms underlying the core manifestations of the disorder. Nevertheless, most reports have focused on individual modalities of structural/functional brain alterations, mainly through targeted approaches, thus possibly precluding the power of unbiased exploratory approaches. Eighty subjects (40 OCD and 40 healthy controls) participated in a multimodal magnetic resonance imaging (MRI) investigation, integrating structural and functional data. Voxel-based morphometry analysis was conducted to compare between-group volumetric differences. The whole-brain functional connectome, derived from resting-state functional connectivity (FC), was analyzed with the network-based statistic methodology. Results from structural and functional analysis were integrated in mediation models. OCD patients revealed volumetric reductions in the right superior temporal sulcus. Patients had significantly decreased FC in two distinct subnetworks: the first, involving the orbitofrontal cortex, temporal poles and the subgenual anterior cingulate cortex; the second, comprising the lingual and postcentral gyri. On the opposite, a network formed by connections between thalamic and occipital regions had significantly increased FC in patients. Integrative models revealed direct and indirect associations between volumetric alterations and FC networks. This study suggests that OCD patients display alterations in brain structure and FC, involving complex networks of brain regions. Furthermore, we provided evidence for direct and indirect associations between structural and functional alterations representing complex patterns of interactions between separate brain regions, which may be of upmost relevance for explaining the pathophysiology of the disorder.
Similar content being viewed by others
Introduction
Obsessive-compulsive disorder (OCD) is one of the most disabling psychiatric conditions, impacting occupational, academic and social functioning1 and affecting 2 to 3% of the worldwide population.2 OCD is characterized by the occurrence of obsessions (intrusive, persistent and inappropriate thoughts, urges or images) and compulsions (repetitive or ritualistic behaviors or mental acts performed to reduce the anxiety caused by the obsessions).3, 4 Despite the availability of pharmacological and cognitive-behavioral interventions, these treatments are not effective for a significant number of patients.5 This highlights the limited understanding of the neurobiological mechanisms of OCD.6
The pathophysiology of OCD has been widely conceptualized within the cortico-striato-thalamo-cortical (CSTC) model.7 According to this model, tracts from frontal regions project to the striatum and then, travel through direct and indirect pathways to the thalamus and project back to the frontal regions. This model has been corroborated by several reports of structural and functional alterations observed in magnetic resonance imaging (MRI) studies. In particular, volumetric alterations within the orbitofrontal cortex (OFC), anterior cingulate cortex (ACC) and thalamus have been reported in patients (for example, refs. 8, 9, 10). Furthermore, early evidence from functional imaging studies indicated an increased metabolism and hyperactivity in several brain regions in OCD patients during task performance, including the basal ganglia (BG),11, 12 OFC13 and ACC.14 On the opposite, a decreased activation in the dorsolateral prefrontal cortex (DLPFC)15 and parietal cortex16, 17, 18, 19 has been described. Emerging evidence suggests a broader cortical dysfunction, involving structural and functional alterations of the anterior insula, lateral and medial temporal lobe regions.20 Furthermore, recent multimodal meta-analytic evidence highlights the relevance of the cerebellum and the parietal cortex for the OCD pathophysiology.21
Resting-state fMRI (rs-fMRI) studies have also provided important biomarkers of OCD. For instance, alterations in the normal patterns of functional connectivity (FC) in resting-state networks (RSNs) have been reported in children with OCD, including a significantly increased connectivity between the dorsal striatum and ventromedial frontal cortex, and a decreased FC between dorsal striatum and medial dorsal thalamus to rostral and dorsal ACC, respectively.22 In addition, increased FC within the auditory and cingulate networks was also reported in a pediatric sample.23 Adult OCD individuals exhibited decreased FC of the dorsal striatum and lateral PFC, and of the ventral striatum with ventral tegmental area,24 as well as a decreased dorsal ACC-right anterior operculum FC during rest.25 Altered FC in the default-mode network (DMN) has been reported, particularly its connections with OFC and ACC,25, 26 and with middle frontal gyrus and putamen.26 Moreover, FC alterations between frontoparietal/ventral attention network (VAN) and the structures comprising the DMN, thalamus, lateral frontal cortex and somatosensory/motor regions were observed.20 Using a graph-theory approach, drug-free patients were found to present a diminished FC between the DMN and frontoparietal regions;27 interestingly, these alterations were abolished after SSRI treatment.
Altogether, the abovementioned results suggest that a large variety of brain areas and circuits are involved in the pathophysiology of the disease. In particular, FC abnormalities have been mainly observed in orbitofrontal, cingulate, striatal and default-mode regions. Nevertheless, these results were observed using theoretically driven investigations. To the best of our knowledge, the use of whole-brain exploratory approaches to assess FC patterns in OCD patients is scarce, with few notable exceptions.28, 29In these studies, OCD patients were characterized by a reduced FC within the lateral prefrontal cortex and an increased FC within the dorsal striatum and thalamus, as well as with a hyperconnectivity between basal ganglia and cerebellar regions. Nevertheless, none of the abovementioned strategies integrated structural findings in their analyses. Thus, despite the variety of studies investigating structural and functional MRI patterns in OCD patients, a comprehensive integration of distinct modalities is still unclear. The use of this multimodal/integrative approach may be of upmost relevance, as it may provide useful information on how distinct MRI modalities (that is, brain structure and function) are associated with each other.30 Consequently, it will enable a further exploration of our understanding of the pathophysiological core features of OCD. With this purpose, we conducted a multimodal study, using voxel-based morphometry and whole-brain functional connectivity analyses, respectively, in which structural and FC data were integrated in mediation models. We hypothesize that OCD patients will be characterized by disrupted structural and FC patterns of large-scale brain networks, as manifested by alterations at the whole-brain level. Furthermore, in accordance with recent developments on the study of OCD, it is anticipated that FC alterations will be observed in networks comprising regions outside of the CSTC model.
Materials and methods
Participants
A sample of 80 subjects (40 OCD patients, 40 controls) participated in this study. Healthy controls were recruited to match OCD patients for age, sex, educational level and ethnical origin. All the participants were right-handed and had no history of neurological or comorbid disorders. OCD patients were characterized with a comprehensive clinical assessment. The diagnosis of the disorder was established by experienced psychiatrists, using a semi-structured interview based on Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition (DSM-IV)-TR. Then, the Mini-International Neuropsychiatric Interview (MINI), a short structured diagnostic interview, was administered to confirm OCD diagnosis and to identify any current psychiatric (non-OCD) comorbidity. Patients that met criteria for additional Axis I psychiatric disorders at the time of the study were not included in this study. The severity of the disease was assessed using the Yale–Brown Obsessive–Compulsive Scale (Y-BOCS31). Hamilton Anxiety Rating Scale (HAM-A) and Hamilton Depression Rating Scale (HAM-D) were used to assess anxiety and depression symptoms, respectively. All OCD patients were under medication: the majority of patients (72.2%) was receiving SSRI medication (fluxomanine, 150–300 mg day−1; fluoxetine, 40–80 mg day−1; sertraline: 100–200 mg day−1), 11.1% of the sample was receiving TCA (clomipramine, 150–300 mg day−1), 16.7% was receiving combined pharmacological intervention. All the patients were receiving stable doses for at least three months prior to the imaging session. The sample characterization is presented on Table 1.
The study was conducted according to the Declaration of Helsinki principles and was approved by the Ethics Committee of Hospital de Braga (Portugal). The study goals were explained, and written informed consent was obtained from each participant.
MRI protocol
The imaging sessions were performed at Hospital de Braga using a clinically approved 1.5 T Siemens Magnetom Avanto MRI scanner (Siemens, Erlangen, Germany) equipped with a standard 12 channel receive-only head coil. Details on the imaging parameters are described in the Supplementary Information.
Volumetric analysis
Before any data processing and analysis, all the acquisitions were visually inspected to confirm that they were not affected by significant artifacts and that participants had no gross anatomical abnormalities. For the volumetric analysis, a Voxel-Based Morphometry (VBM) analysis was performed with FSL-VBM (ref. 32, http://fsl.fmrib.ox.ac.uk/fsl/fslwiki/FSLVBM), an optimized VBM protocol33 implemented using tools from the FMRIB Software Library (FSL v5.0.9, www.fmrib.ox.ac.uk/fsl), using the recommended analytical pipeline (Supplementary Information).
Data preprocessing of functional data
Data preprocessing was performed using FSL tools. Images were corrected for slice timing using the first slice as reference and then motion corrected by aligning every volume with the mean volume using a rigid-body (six degrees of freedom) spatial transformation. As a means to further reduce the possible contamination of motion on functional connectivity, motion scrubbing was performed, to identify and exclude time points in which head motion could have a critical impact. Following the recommendations from Van Dijk et al.,34 only participants with <20 outlier time points were included in the analysis, ensuring that more than 5 min of motion-free data was obtained for each subject. None of the participants exceeded head motion higher than 2 mm in translation or 1° in rotation. Images were non-linearly normalized to the MNI standard space using an indirect procedure (Supplementary Information). Linear regression of motion parameters, mean white-matter (WM) and cerebrospinal fluid (CSF) signal and motion outliers was performed to reduce motion related variance in fMRI signals and the residuals of the regression were used for the subsequent analysis.35, 36 Finally, images were spatially smoothed with a Gaussian kernel of 8 mm full-width at half-maximum (FWHM) and band-pass filtered (0.01–0.08 Hz).
Whole-brain connectome
Whole-brain functional connectomes were built by extracting the mean time-series of 116 cortical, subcortical and cerebellar regions from the Anatomical Automatic Labelling (AAL) atlas.37 A symmetric adjacency matrix R was then produced, where each cell rij corresponded to the correlation coefficient (r) between the time-series of regions i and j. This matrix was then transformed with Fisher’s r-to-Z transformation to convert Pearson coefficients r to normally distributed Z-values. Individual matrices were then aggregated for further statistical analysis.
Statistical analysis
Statistical group comparisons on volumetric and functional MRI data were conducted using two-samples t-tests, adjusted for confounding effects. For the different analysis, sex and age were used as between-subjects’ covariates.
VBM analysis was performed voxel-wise with a General Linear Model (GLM) using a non-parametric permutation procedure as implemented in the randomise tool from FSL.38 Threshold-free cluster enhancement (TFCE) was used to detect widespread significant differences, whereas controlling the family-wise error rate (FWE-R) at α=0.05. Each contrast underwent 5.000 permutations.
The identification of significantly different FC subnetworks between groups at the whole-brain connectome was performed through the network-based statistic (NBS) procedure, implemented with NBS.39 The differences between the adjacency matrices of each group were estimated with 5.000 random permutations, based on two different thresholds for significance: α=0.001 and α=0.0001. Networks were considered significant at α=0.05 family-wise error (FWE) corrected. BrainNet Viewer (http://www.nitrc.org/projects/bnv) was used to display significant networks.40
Associations between symptoms’ severity and structural/functional findings were evaluated computing Pearson correlations between total Y-BOCS score and findings significantly different between groups.
With the goal of integrating structural and functional findings, mediation models were established. For these models, direct (that is, the impact of the independent on the dependent variable) and indirect effects (that is, the impact of one proposed mediator variable on the key relationship) were evaluated. For both approaches, bootstrap sampling was implemented to generate bias-corrected 95% confidence intervals to estimate indirect and interactive effects.
An overview of the methodological pipeline is summarized on Figure 1.
Overview of the methodological approach. Structural and functional magnetic resonance imaging (MRI) sequences were acquired. For the structural acquisitions, a voxel-based morphometry analysis was conducted to detect clusters with significantly between-group differences. For the functional acquisitions, the time-series of Anatomical Automatic Labelling (AAL) cortical and subcortical brain regions was extracted to create group-specific matrices, corresponding to the correlation between regions. Afterwards, a network-based statistic approach was implemented to detect networks with significantly different functional connectivity between groups. As the final step, the structural and functional results were analyzed in integrative models, using mediation analyses.
Results
Sample characteristics
As shown in Table 1, the groups are similar with respect to sex, age and education level. As represented, all the participants were taking medication. The Y-BOCS total score ranged from 11 to 35 (M=24.93, s.d.=5.69). The groups did not differ on the number of motion outliers (t(78)=−1.23, P=0.224).
Volumetric analysis
Results from the VBM analysis revealed that OCD patients had significantly reduced volumes in one cluster comprising 394 voxels with peak on the right temporal middle gyrus, extending to the superior temporal gyrus (Figure 2). We will refer to this region as the superior temporal sulcus (STS). No results of volumetric increases in OCD patients were found.
Whole-brain functional connectivity
Using the most restrict threshold (P<0.0001), it was noted that OCD patients displayed significantly reduced FC in two subnetworks with short-range configurations: the first subnetwork (orbitofrontal-temporal pole subnetwork, OFC-TM) comprised anterior regions, including the bilateral medial orbitofrontal cortex (mOFC), bilateral temporal poles and the subgenual anterior cingulate cortex (sgACC) (Figure 3a; P=0.010); the second subnetwork (occipital-sensorimotor, Occ-SM) was formed by the connection between left postcentral and bilateral lingual gyri (Figure 3a; P=0.045). Using the less restrict threshold (P<0.001), it was observed that these subnetworks were aggregated in a main single network with wide-range properties, which was also constituted by edges connecting occipital and sensorimotor brain regions and also involving edges connecting the temporal middle gyrus to the mOFC (Figure 3b; P=0.039). In contrast, even though no networks with significantly different FC patterns were identified with the more restrict threshold, using the less restrict threshold, a network (thalamic-occipital, Thal-Occ) with marginally significant increased FC (P=0.057) in OCD patients was identified, encompassing edges connecting the thalamus to occipital inferior, lingual and fusiform gyri (Figure 3d).
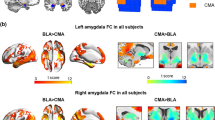
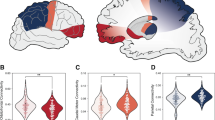
Whole-brain networks with altered functional connectivity (FC) in obsessive-compulsive disorder (OCD) patients, using two primary thresholds: networks with significantly decreased FC (blue) in OCD patients at P<0.0001 (a) and P<0.001 (b) levels are presented on the top; (c) no networks with significantly increased FC was found at the P<0.0001 level; (d) a network with significantly increased FC (red) was found in OCD patients at P<0.001 level. Bar graphs correspond to individual levels of mean FC in each group. On the middle, the t-statistic corresponding to each individual edge is represented for networks with increased and decreased FC levels.
Associations between symptom’s severity and structural/functional findings
The Y-BOCS total score revealed a significant negative association with the fronto-temporal subnetwork with decreased FC in OCD patients (r=−0.325, P=0.040). No associations between symptoms’ severity and the other functional and volumetric findings were found.
Mediation effects between structural and functional findings
Bivariate correlations revealed that the volumetric and FC findings were significantly associated (Supplementary Table 1), enabling the test for mediation effects. Different models were conducted, using the volumetric differences as either independent or dependent variables. It was observed that, controlling for confounding effects (sex and age), the mean FC of the OFC-TP subnetwork significantly mediated the association between volumetric differences and the mean FC of the Occ-SM subnetwork (Figure 4a), as observed by a significant indirect between these variables. On the other hand, we could also observe that there was a significant indirect effect of the mean FC of the Thal-Occ subnetwork on volumetric differences within the STS, which was mediated by two mediator variables, corresponding to the mean FC of the Occ-SM and OFC-TP subnetworks (Figure 4b).
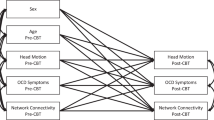
Mediation models. (a) Mediator effects of the orbitofrontal-temporal pole subnetwork (OFC-TP) on the association between volumetric differences within the superior temporal sulcus (STS) and the mean functional connectivity (FC) of the occipito-sensorimotor subnetwork (Occ-SM); (b) mediator effects of the occipito-sensorimotor (Occ-SM) and orbitofrontal-temporal pole (OFC-TP) subnetworks on the association between the mean FC of the thalamic-occipital subnetwork (Thal-Occ) and volumetric differences. Both models revealed significant indirect effects between independent and dependent variables, controlling for confounding factors (sex and age). Values next to each arrow represent standardized coefficients. Values in parenthesis correspond to standardized coefficients when the effects of mediator variables are removed.
Discussion
In this work, we conducted an exploratory multimodal MRI investigation to study volumetric and FC patterns in OCD patients. We observed that OCD patients display volumetric reductions of one cluster comprising the right medial and superior temporal gyri and significantly altered FC in distinct subnetworks, particularly a reduced FC in networks connecting the medial OFC, temporal poles, lingual and postcentral gyri; and on the opposite, patients had increased FC in a network composed of connections involving the thalamus and occipital regions. Mediation analyses revealed that the association between structural findings and specific FC networks were mediated by other FC networks.
Volumetric alterations in OCD patients
We observed that OCD patients display volumetric reductions of one cluster with peak on the right STS, extending to both the medial and superior temporal gyri. This result is corroborated by previous reports, which implicated the superior temporal cortex on the pathophysiology of the disease.41 Furthermore, in a meta-analytic investigation, it was demonstrated that OCD patients display a reduction of the middle temporal gyrus during the aging process.42
Decreased functional connectivity in OCD patients
In our study, a FC network comprising connections between bilateral mOFC and bilateral temporal pole, as well as between the left temporal pole and the sgACC, revealed decreased FC in OCD patients. The mOFC is functionally connected with default-mode network, autonomic and subcortical regions, including the ventral striatum, amygdala and the hippocampus,43, 44 being relevant for multiple psychological processes, including episodic memory, reward, decision-making and fear.43, 45 Previous studies demonstrated bilateral volume reductions46 and hypo-functioning of the mOFC during extinction recall in OCD.7 Furthermore, the temporal pole, is directly linked to prefrontal brain regions, through a large white-matter tract, the uncinate fasciculus. Owing to its dense connections with the amygdala and the OFC, the temporal pole is considered an important hub of the affective brain circuit.47 The temporal pole, together with the sgACC, were implicated in the mental effort to overcome fear.48 With respect to OCD pathophysiology, these nodes have been previously associated with the severity of harm/checking symptoms49 and dysfunctional beliefs.50 A recent report also revealed a decrease in the structural connectivity among these regions in OCD, highlighting the role of emotional processing on the clinical manifestations of the disorder.51 Altogether, and due to the fact that this subnetwork was significantly associated with the severity of OCD symptoms, it seems reasonable to hypothesize that the reduced link between OFC and these ‘affective’ hubs may contribute to a deficient emotional processing and a consequent impaired regulation of the anxiety following obsessive thoughts.
Another subnetwork with decreased FC in OCD patients was composed of edges involving bilateral lingual gyrus and the left postcentral. Previous studies reported alterations in functional52 and structural53 connectivity patterns of this region in OCD patients. The lingual gyrus was proposed to be involved in the processing of emotionally charged visual stimuli54 and with the generation of somatic arousal,55 which is typically dysregulated in disorders of the obsessive-compulsive spectrum.53 It has been recently hypothesized that its activity is tightly linked to the phenomenology of OCD, where, for instance, intrusive thoughts or images of dirt, provoke strong emotional responses in patients with contamination obsessions.56 In addition, the activity of the lingual gyrus, together with the amygdala and orbital regions, was reported to be elicited by emotional, unpleasant, stimuli,57 being also activated during the visualization of fearful faces.58 Providing further evidence for this hypothesis, it has been demonstrated that the activity of this brain region is altered in psychiatric conditions characterized by anxious59 and depressive symptoms.60 Altogether, it is reasonable to hypothesize that this network of reduced FC may underlie an altered emotional processing, particularly related with fear content. Following this hypothesis, the decreased FC between visual and sensorimotor networks herein observed may be contextualized in line with a previous hypothesis suggesting that an exaggerated FC between distinct sensory regions may contribute to a heightened encoding of fear-related stimuli during task performance.61 Despite the fact that our findings are in apparent contradiction with the abovementioned report, it is important to note that whereas Wiemer’s findings were obtained while subjects were viewing emotional, fear-related stimuli, our results were obtained with the absence of stimuli, that is, during rest. As such, it is reasonable to hypothesize that the abnormal FC between these regions may be context-dependent, being highly connected during the processing of emotional information, and hypoconnected in default brain processing.
Increased functional connectivity in OCD patients: extension of the typical CTSC model
A network with marginally significant increases of FC between thalamic and occipital brain regions was observed in OCD patients. The most widely accepted neurobiological models of OCD rely on an increased cerebral metabolism in circuits involving the thalamus, OFC and the striatum—the CTSC model—which is thought to underlie behavioral alterations in multiple domains, including reward processing, action selection or habit-based functioning. This hypothesis is partially corroborated by our results in which edges with (marginally) significant increases in resting-state FC, connecting the thalamus to cortical regions were found in OCD patients. Furthermore, the involvement of other regions not included in the CTSC model also corroborates more recent models, in which parietal, occipital and cerebellar regions have been identified as relevant for the pathophysiology of the disease.21
Integration of structural and functional findings
We observed that the structural and functional findings herein obtained were significantly associated. Nevertheless, it was noted that the associations between structural and specific functional results were significantly mediated by specific FC patterns that altered the relationship between structure and function: the mean FC of OFC-TP subnetwork significantly mediated the association between volumetric differences within the STS and Occ-SM subnetwork (model 1); the mean FC of Occ-SM and OFC-TP subnetworks significantly mediated the association between the mean FC of the Thal-Occ subnetwork and volumetric differences within the STS (model 2). According to these results, two distinct hypotheses are proposed.
Hypothesis 1: Direct and indirect contributions of volumetric alterations to a decreased connectivity between the STS and the OFC, and between the OFC and posterior regions, respectively.
The results from the mediation model revealed that the association between structural findings and the mean FC of the Occ-SM subnetwork was significantly mediated by the mean FC of the OFC-TP subnetwork. One possible explanation of this mediation effect relies on the hypothesis that the structural reductions of the STS may contribute to a diminished number of tracts of the arcuate fasciculus (one subcomponent of the superior longitudinal fasciculus (SLF), connecting regions from the temporal lobe to frontal areas) in OCD patients. Consequently, this may contribute to a diminishment of the projections between the OFC and limbic areas (for example, the temporal pole, through the uncinate fasciculus), contributing to an impaired behavioral and emotional regulation. In turn, projections from the OFC to occipital brain regions (for example, the lingual gyri), and to posterior brain regions (through another subcomponent of the SLF) may in turn be diminished.
Hypothesis 2: Hyperconnectivity between thalamic-cortical projections has an impact on volumetric reductions on the superior temporal sulcus mediated by abnormal FC involving posterior and anterior regions.
Another alternative hypothesis, which follows an inverse path of the one proposed in the first hypothesis, suggests that volumetric alterations are a consequence rather than a cause of FC alterations. We have previously discussed that the Thal-Occ network may represent the aberrant CSTC loops typically described in OCD patients. This network is significantly associated with the remaining observed structural and functional between-group differences. Nevertheless, it was found that the association between this network and volumetric differences was significantly mediated by both subnetworks with decreased FC in OCD patients. In this context, one may hypothesize that the hyperconnectivity of the loops projecting from the thalamus to parietal and occipital cortical regions may have an impact on the occipito-sensorimotor connectivity. Projections from these regions to orbitofrontal regions, through the SLF, may disturb the functioning of the OFC and its synchrony with limbic regions and the temporal pole (linked via the uncinate fasciculus). An impaired feedback between these regions may, in turn, result in an impaired structural connectivity between the OFC and the STS (throughout the arcuate fasciculus), which may ultimately cause volumetric reductions in this area.
Strengths and limitations
It is worth to acknowledge some strengths and limitations associated with this work. The first strength is associated with the multimodal approach here implemented. With this, we could provide complementary evidence for abnormal structural and functional brain patterns in OCD patients and how they can be integrated to understand the neural mechanisms associated with the disorder. In addition, the group differences were identified using very conservative approaches, with restrict thresholds for assessing both volumetric (with non-parametric permutation testing) and whole-brain (P<0.001 and P<0.0001) differences. Thus, considering the recent debate associated with the problem of false-positive findings in neuroimaging experiments, this conservative strategy enables an additional level of confidence in the reported findings.
On the other hand, it is relevant to highlight that the network with increases in FC (the Thal-Occ network) was identified with marginally significant results. Thus, these results need to be interpreted with additional caution. Other limitations pertain to the characteristics of the sample. One aspect relies on the fact that our sample was under medication. Recent reports have demonstrated that specific FC alterations stabilize after pharmacological intervention in OCD patients.27 Consequently, it is reasonable to speculate that the pharmacological treatment could ameliorate the differences herein obtained. Nevertheless, it is important to mention that the duration of medication was not associated with the magnitude of the differences between OCD and HC groups, considering either the structural and functional alterations here described (data not shown). Another important issue pertains to the high heterogeneity observed among OCD patients. It is also important to highlight that the hypotheses raised with this work strongly rely on structural connections between particular brain regions. Thus, our theoretical model could be better sustained with the complementary characterization with diffusion tractography approaches.
Conclusions
In sum, we could detect a variety of functional and structural brain alterations in OCD patients. Using this multimodal approach, we could integrate these results in an integrated, theoretical model that may provide useful insights associated with the pathophysiology of the disorder. In addition, our results reinforce the importance of extending the CSTC model to fully understand the pathophysiology of the disease.
References
Koran LM, Thienemann ML, Davenport R . Quality of life for patients with obsessive-compulsive disorder. Am J Psychiatry 1996; 153: 783–788.
Ruscio A, Stein D, Chiu W, Kessler R . The epidemiology of obsessive-compulsive disorder in the National Comorbidity Survey Replication. Mol Psychiatry 2008; 15: 53–63.
Stein DJ . Obsessive-compulsive disorder. Lancet 2002; 360: 397–405.
Huey E, Zahn R, Krueger F, Moll J, Kapogiannis D, Wassermann E et al. A psychological and neuroanatomical model of obsessive-compulsive disorder. J Neuropsychiatry Clin Neurosci 2008; 20: 390–408.
Franklin ME, Sapyta J, Freeman JB, Khanna M, Compton S, Almirall D et al. Cognitive behavior therapy augmentation of pharmacotherapy in pediatric obsessive-compulsive disorder: the Pediatric OCD Treatment Study II (POTS II) randomized controlled trial. JAMA 2011; 306: 1224–1232.
Melloni M, Urbistondo C, Sedeño L, Gelormini C, Kichic R, Ibanez A . The extended fronto-striatal model of obsessive compulsive disorder: convergence from event-related potentials, neuropsychology and neuroimaging. Front Hum Neurosci 2012; 6: 259.
Milad MR, Rauch SL . Obsessive-compulsive disorder: beyond segregated cortico-striatal pathways. Trends Cogn Sci 2012; 16: 43–51.
Atmaca M, Yildirim H, Ozdemir H, Tezcan E, Poyraz AK . Volumetric MRI study of key brain regions implicated in obsessive–compulsive disorder. Prog Neuro-psychopharmacol Biol Psychiatry 2007; 31: 46–52.
Kang D-H, Kim J-J, Choi J-S, Kim YI, Kim C-W, Youn T et al. Volumetric investigation of the frontal-subcortical circuitry in patients with obsessive-compulsive disorder. J Neuropsychiatry Clin Neurosci 2004; 16: 342–349.
Rotge J-Y, Guehl D, Dilharreguy B, Tignol J, Bioulac B, Allard M et al. Meta-analysis of brain volume changes in obsessive-compulsive disorder. Biol Psychiatry 2009; 65: 75–83.
Friedlander L, Desrocher M . Neuroimaging studies of obsessive–compulsive disorder in adults and children. Clin Psychol Rev 2006; 26: 32–49.
Menzies L, Chamberlain SR, Laird AR, Thelen SM, Sahakian BJ, Bullmore ET . Integrating evidence from neuroimaging and neuropsychological studies of obsessive-compulsive disorder: the orbitofronto-striatal model revisited. Neurosci Biobehav Rev 2008; 32: 525–549.
Alptekin K, Degirmenci B, Kivircik B, Durak H, Yemez B, Derebek E et al. Tc-99m HMPAO brain perfusion SPECT in drug-free obsessive-compulsive patients without depression. Psychiatry Res 2001; 107: 51–56.
Molina V, Montz R, Martin-Loeches M, Jimenez-Vicioso A, Carreras J, Rubia F . Drug therapy and cerebral perfusion in obsessive-compulsive disorder. J Nucl Med 1995; 36: 2234–2238.
Nakao T, Okada K, Kanba S . Neurobiological model of obsessive–compulsive disorder: evidence from recent neuropsychological and neuroimaging findings. Psychiatry Clin Neurosci 2014; 68: 587–605.
Maltby N, Tolin DF, Worhunsky P, O'Keefe TM, Kiehl KA . Dysfunctional action monitoring hyperactivates frontal–striatal circuits in obsessive–compulsive disorder: an event-related fMRI study. Neuroimage 2005; 24: 495–503.
van den Heuvel OA, Veltman DJ, Groenewegen HJ, Witter MP, Merkelbach J, Cath DC et al. Disorder-specific neuroanatomical correlates of attentional bias in obsessive-compulsive disorder, panic disorder, and hypochondriasis. Archiv Gen Psychiatry 2005; 62: 922–933.
Viard A, Flament MF, Artiges E, Dehaene S, Naccache L, Cohen D et al. Cognitive control in childhood-onset obsessive–compulsive disorder: a functional MRI study. Psychol Med 2005; 35: 1007–1017.
Remijnse PL, Nielen MM, van Balkom AJ, Cath DC, van Oppen P, Uylings HB et al. Reduced orbitofrontal-striatal activity on a reversal learning task in obsessive-compulsive disorder. Archiv Gen Psychiatry 2006; 63: 1225–1236.
Stern ER, Fitzgerald KD, Welsh RC, Abelson JL, Taylor SF . Resting-state functional connectivity between fronto-parietal and default mode networks in obsessive-compulsive disorder. PLoS ONE 2012; 7: e36356.
Eng GK, Sim K, Chen S-HA . Meta-analytic investigations of structural grey matter, executive domain-related functional activations, and white matter diffusivity in obsessive compulsive disorder: an integrative review. Neurosci Biobehav Rev 2015; 52: 233–257.
Fitzgerald KD, Welsh RC, Stern ER, Angstadt M, Hanna GL, Abelson JL et al. Developmental alterations of frontal-striatal-thalamic connectivity in obsessive-compulsive disorder. J Am Acad Child Adolesc Psychiatry 2011; 50: 938–948. e3.
Weber AM, Soreni N, Noseworthy MD . A preliminary study of functional connectivity of medication naive children with obsessive–compulsive disorder. Prog Neuro-Psychopharmacol Biol Psychiatry 2014; 53: 129–136.
Harrison BJ, Soriano-Mas C, Pujol J, Ortiz H, López-Solà M, Hernández-Ribas R et al. Altered corticostriatal functional connectivity in obsessive-compulsive disorder. Archiv Gen Psychiatry 2009; 66: 1189–1200.
Fitzgerald KD, Stern ER, Angstadt M, Nicholson-Muth KC, Maynor MR, Welsh RC et al. Altered function and connectivity of the medial frontal cortex in pediatric obsessive-compulsive disorder. Biol Psychiatry 2010; 68: 1039–1047.
Jang JH, Kim J-H, Jung WH, Choi J-S, Jung MH, Lee J-M et al. Functional connectivity in fronto-subcortical circuitry during the resting state in obsessive-compulsive disorder. Neurosci Lett 2010; 474: 158–162.
Shin D-J, Jung WH, He Y, Wang J, Shim G, Byun MS et al. The effects of pharmacological treatment on functional brain connectome in obsessive-compulsive disorder. Biol Psychiatry 2014; 75: 606–614.
Anticevic A, Hu S, Zhang S, Savic A, Billingslea E, Wasylink S et al. Global resting-state fMRI analysis identifies frontal cortex, striatal, and cerebellar dysconnectivity in obsessive-compulsive disorder. Biol Psychiatry 2014; 75: 595–605.
Vaghi MM, Vértes PE, Kitzbichler MG, Apergis-Schoute AM, van der Flier FE, Fineberg NA et al. Specific frontostriatal circuits for impaired cognitive flexibility and goal-directed planning in obsessive-compulsive disorder: evidence from resting-state functional connectivity. Biol Psychiatry 81: 708–717.
Uludağ K, Roebroeck A . General overview on the merits of multimodal neuroimaging data fusion. NeuroImage 2014; 102 (Part 1): 3–10.
Goodman WK, Price LH, Rasmussen SA, Mazure C, Fleischmann RL, Hill CL et al. The Yale-Brown obsessive compulsive scale: I. Development, use, and reliability. Archiv Gen Psychiatry 1989; 46: 1006–1011.
Douaud G, Smith S, Jenkinson M, Behrens T, Johansen-Berg H, Vickers J et al. Anatomically related grey and white matter abnormalities in adolescent-onset schizophrenia. Brain 2007; 130: 2375–2386.
Good CD, Johnsrude IS, Ashburner J, Henson RN, Friston KJ, Frackowiak RS . A voxel-based morphometric study of ageing in 465 normal adult human brains. Neuroimage 2001; 14: 21–36.
Van Dijk KR, Hedden T, Venkataraman A, Evans KC, Lazar SW, Buckner RL . Intrinsic functional connectivity as a tool for human connectomics: theory, properties, and optimization. J Neurophysiol 2010; 103: 297–321.
Chai XJ, Castañón AN, Öngür D, Whitfield-Gabrieli S . Anticorrelations in resting state networks without global signal regression. NeuroImage 2012; 59: 1420–1428.
Power JD, Barnes KA, Snyder AZ, Schlaggar BL, Petersen SE . Spurious but systematic correlations in functional connectivity MRI networks arise from subject motion. NeuroImage 2012; 59: 2142–2154.
Tzourio-Mazoyer N, Landeau B, Papathanassiou D, Crivello F, Etard O, Delcroix N et al. Automated anatomical labeling of activations in SPM using a macroscopic anatomical parcellation of the MNI MRI single-subject brain. Neuroimage 2002; 15: 273–289.
Winkler AM, Ridgway GR, Webster MA, Smith SM, Nichols TE . Permutation inference for the general linear model. Neuroimage 2014; 92: 381–397.
Zalesky A, Fornito A, Bullmore ET . Network-based statistic: identifying differences in brain networks. Neuroimage 2010; 53: 1197–1207.
Xia M, Wang J, He Y . BrainNet Viewer: a network visualization tool for human brain connectomics. PLoS ONE 2013; 8: e68910.
Choi JS, Kim HS, Yoo SY, Ha TH, Chang JH, Kim YY et al. Morphometric alterations of anterior superior temporal cortex in obsessive-compulsive disorder. Depress Anxiety 2006; 23: 290–296.
de Wit SJ, Alonso P, Schweren L, Mataix-Cols D, Lochner C, Menchon JM et al. Multicenter voxel-based morphometry mega-analysis of structural brain scans in obsessive-compulsive disorder. Am J Psychiatry 2014; 171: 340–349.
de la Vega A, Chang LJ, Banich MT, Wager TD, Yarkoni T . Large-scale meta-analysis of human medial frontal cortex reveals tripartite functional organization. J Neurosci 2016; 36: 6553–6562.
Zald DH, McHugo M, Ray KL, Glahn DC, Eickhoff SB, Laird AR . Meta-analytic connectivity modeling reveals differential functional connectivity of the medial and lateral orbitofrontal cortex. Cereb Cortex 2014; 24: 232–248.
Morgado P, Sousa N, Cerqueira JJ . The impact of stress in decision making in the context of uncertainty. J Neurosci Res 2015; 93: 839–847.
Cardoner N, Soriano-Mas C, Pujol J, Alonso P, Harrison BJ, Deus J et al. Brain structural correlates of depressive comorbidity in obsessive–compulsive disorder. Neuroimage 2007; 38: 413–421.
Olson IR, Plotzker A, Ezzyat Y . The enigmatic temporal pole: a review of findings on social and emotional processing. Brain 2007; 130: 1718–1731.
Nili U, Goldberg H, Weizman A, Dudai Y . Fear thou not: activity of frontal and temporal circuits in moments of real-life courage. Neuron 2010; 66: 949–962.
van den Heuvel OA, Remijnse PL, Mataix-Cols D, Vrenken H, Groenewegen HJ, Uylings HB et al. The major symptom dimensions of obsessive-compulsive disorder are mediated by partially distinct neural systems. Brain 2009; 132: 853–868.
Alonso P, Orbegozo A, Pujol J, López-Solà C, Fullana MÀ, Segalàs C et al. Neural correlates of obsessive–compulsive related dysfunctional beliefs. Prog Neuro-Psychopharmacol Biol Psychiatry 2013; 47: 25–32.
Reess TJ, Rus OG, Schmidt R, de Reus MA, Zaudig M, Wagner G et al. Connectomics-based structural network alterations in obsessive-compulsive disorder. Transl Psychiatry 2016; 6: e882.
Mataix-Cols D, Wooderson S, Lawrence N, Brammer MJ, Speckens A, Phillips ML . Distinct neural correlates of washing, checking, and hoarding symptomdimensions in obsessive-compulsive disorder. Archiv Gen Psychiatry 2004; 61: 564–576.
Szeszko PR, Ardekani BA, Ashtari M, Malhotra AK, Robinson DG, Bilder RM et al. White matter abnormalities in obsessive-compulsive disorder: a diffusion tensor imaging study. Archiv Gen Psychiatry 2005; 62: 782–790.
Mitterschiffthaler MT, Kumari V, Malhi GS, Brown RG, Giampietro VP, Brammer MJ et al. Neural response to pleasant stimuli in anhedonia: an fMRI study. Neuroreport 2003; 14: 177–182.
Critchley HD, Elliott R, Mathias CJ, Dolan RJ . Neural activity relating to generation and representation of galvanic skin conductance responses: a functional magnetic resonance imaging study. J Neurosci 2000; 20: 3033–3040.
Göttlich M, Krämer UM, Kordon A, Hohagen F, Zurowski B . Decreased limbic and increased fronto‐parietal connectivity in unmedicated patients with obsessive‐compulsive disorder. Hum Brain Mapp 2014; 35: 5617–5632.
Moll J, de Oliveira-Souza R, Bramati IE, Grafman J . Functional networks in emotional moral and nonmoral social judgements. Neuroimage 2002; 16: 696–703.
Carlson JM, Reinke KS, Habib R . A left amygdala mediated network for rapid orienting to masked fearful faces. Neuropsychologia 2009; 47: 1386–1389.
Lai C-H, Wu Y-T . Decreased regional homogeneity in lingual gyrus, increased regional homogeneity in cuneus and correlations with panic symptom severity of first-episode, medication-naive and late-onset panic disorder patients. Psychiatry Res 2013; 211: 127–131.
Veer IM, Beckmann C, Van Tol M-J, Ferrarini L, Milles J, Veltman D et al. Whole brain resting-state analysis reveals decreased functional connectivity in major depression. Front Syst Neurosci 2010; 4: 41.
Wiemer J, Pauli P . Enhanced functional connectivity between sensorimotor and visual cortex predicts covariation bias in spider phobia. Biol Psychol 2016; 121 (Pt B): 128–137.
Acknowledgements
PSM is supported by the FCT fellowship grant with the number PDE/BDE/113601/2015 from the PhD-iHES program; PM is funded by the Fundação Calouste Gulbenkian (Contract Grant Number: P-139977; project ‘Better mental health during ageing based on temporal prediction of individual brain ageing trajectories (TEMPO)’); RM is supported by the FCT fellowship grant with the number PDE/BDE/113604/2015 from the PhD-iHES program. The present work was supported by SwitchBox-FP7-HEALTH-2010-grant 259772-2 and co-financed by the Portuguese North Regional Operational Program (ON.2–O Novo Norte) under the National Strategic Reference Framework (QREN), through the European Regional Development Fund (FEDER). CS-M is funded by a Miguel Servet contract from the Carlos III Health Institute of Spain (CPII16/00048). We would also like to acknowledge Patrício Costa for his aiding in the implementation of the mediation models.
Disclaimer
The paper has not been published previously, or is under consideration for publication elsewhere, in English or in any other language.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies the paper on the Translational Psychiatry website
Supplementary information
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/4.0/
About this article
Cite this article
Moreira, P., Marques, P., Soriano-Mas, C. et al. The neural correlates of obsessive-compulsive disorder: a multimodal perspective. Transl Psychiatry 7, e1224 (2017). https://doi.org/10.1038/tp.2017.189
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/tp.2017.189
This article is cited by
-
Altered neural anticipation of reward and loss but not receipt in adolescents with obsessive-compulsive disorder
BMC Psychiatry (2024)
-
Decreased gray matter volume and dynamic functional alterations in medicine-free obsessive-compulsive disorder
BMC Psychiatry (2023)
-
Comparison of resting-state spontaneous brain activity between treatment-naive schizophrenia and obsessive-compulsive disorder
BMC Psychiatry (2021)
-
Comparative analysis of default mode networks in major psychiatric disorders using resting-state EEG
Scientific Reports (2021)
-
Disrupted pathways from frontal-parietal cortex to basal ganglia and cerebellum in patients with unmedicated obsessive compulsive disorder as observed by whole-brain resting-state effective connectivity analysis – a small sample pilot study
Brain Imaging and Behavior (2021)