Abstract
Chikungunya fever (CHIKF) is a global infectious disease which can affect a wide range of age groups. The pathological and immunological response upon Chikungunya virus (CHIKV) infection have been reported over the last few years. However, the clinical profile and immune response upon CHIKV infection in children remain largely unknown. In this study, we analyzed the clinical and immunological response, focusing on the cytokine/chemokine profile in a CHIKV-infected pediatric cohort from Sarawak, Malaysia. Unique immune mediators triggered upon CHIKV infection were identified through meta-analysis of the immune signatures between this pediatric group and cohorts from previous outbreaks. The data generated from this study revealed that a broad spectrum of cytokines/chemokines is up-regulated in a sub-group of virus-infected children stratified according to their viremic status during hospitalization. Furthermore, different immune mediator profiles (the levels of pro-inflammatory cytokines, chemokines and growth and other factors) were observed between children and adults. This study gives an important insight to understand the immune response of CHIKV infection in children and would aid in the development of better prognostics and clinical management for children.
Similar content being viewed by others
Introduction
Chikungunya fever (CHIKF) is an acute illness caused by the alphavirus Chikungunya virus (CHIKV). Transmitted by Aedes mosquitoes, clinical manifestations include an abrupt high fever, rashes, myalgia and arthralgia that will appear after an incubation period of 3–7 days. However, chronic and incapacitating arthralgia can persist for months to years1. CHIKV was first identified in 1953 during a dengue-like epidemic in Tanzania, and outbreaks of CHIKF have been documented in Africa and South East Asia throughout 1960s–1990s1,2,3. Since 2005, CHIKV has caused outbreaks of an unprecedented magnitude in La Réunion with more than a third of its population infected4,5. Over 1.4 million cases have also occurred in India, South East Asia, and islands in the Pacific between 2006 and 20126,7,8,9. CHIKV has since spread to the Caribbean islands in late 201310, and as of November 2015, 8,275 laboratory-confirmed cases have been reported from these areas (http://www.cdc.gov/chikungunya/geo/united-states-2015.html). With the worldwide increased spread of the Aedes mosquitoes, CHIKV remains a major threat to public health. Thus, with no available licensed vaccine or specific treatments, CHIKV can present a social and economic burden to affected communities.
Studies on CHIKF pathogenesis have revealed that CHIKV infection induced a wide range of cytokines, chemokines and growth factors11,12. Higher levels of IL-1β and IL-6, and lower level of RANTES were also linked to severe CHIKF11. Systematic meta-analysis has also revealed the immune signatures in patients from different CHIKF cohorts during the 2007–2010 outbreaks across different geographic locations13. CHIKV infection affects all age groups. However, studies on CHIKV-induced immune mediators across cohorts have been limited to adult patients. Although CHIKV infections in children have been reported14,15,16, documentation remained limited to clinical descriptions with no information on the immune response. Symptoms such as high fever, rash, seizures, and weight loss were reported in infected neonates and infants14,15,16. Interestingly, although severe arthralgia and arthritis did occur in children, it was uncommon and usually resolved during the acute phase of disease16.
In this study, we studied the immune response of CHIKV infection by examining the disease manifestations and measuring the circulatory immune mediators during acute disease in a cohort of 86 children under the age of 12. Multiplex-microbead immunoassays were done and meta-analysis was further performed together with all available data from 2009 to 2014 relating to acute CHIKV infection in adults to identify unique immune markers explaining the different clinical manifestations between children and adults. Interestingly, a differential pattern was identified in the immune mediator response between pediatric patients with early viral clearance and those with prolonged viremia and joint pain.
Results
Clinical manifestations of a CHIKF pediatric cohort
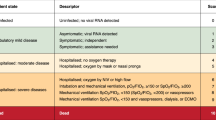
Between October 2009 and March 2010, 108 children were recruited for this study based on their presenting symptoms during hospital admission (Table 1). Patients’ admission sera (median sampling day was 1 day post illness onset) were subjected to virus isolation and tested by CHIKV-specific PCR test. IgM serology was performed to test for DENV infection17. Eighty-six children were confirmed CHIKV positive with a median age of 4.86 years, ranging from 1 week to 11 years old. The length of stay was between 2–8 days. The most reported clinical manifestations of this cohort were fever, joint pain, facial flushing, skin rash (mostly erythematous, with some cases of maculopapular rash), chills, and headache (Table 1). Many of these children also suffered from loss of appetite and were not drinking well (Table 1).
Of these 86 pediatric patients, blood samples were obtained from 64 individuals during both hospital admission and at discharge (i.e. paired samples). CHIKV was still detectable by virus isolation in 34 patients at discharge and thus classified as the prolonged viremia group (Table 1). The other 30 children with no detectable CHIKV by PCR at discharge were classified as early viral clearance group (Table 1). The remaining 22 CHIKF pediatric patients were classified as the unpaired sample group as blood samples were obtained during hospital admission only.
Profiles of immune mediators in children
We next characterized the immune mediator profiles of acute serum samples collected from the 86 children using a multiplex-microbead immunoassay11. Samples from 64 adult Singapore CHIKF patients18,19 and 8 healthy adults were included in the analysis. Both groups of patients represent the population in South-East Asia, and no major difference in disease severity was observed. The pediatric cohort induced a higher level of several immune mediators when compared to the adult cohort (Fig. 1). Pro-inflammatory cytokines: TNF-β, TRAIL, IL-5, GRO-α, IL-18, IFN-α2, IL-2Ra; chemokines: MIF, MIG, MCP-3, G-CSF; growth and others: SCGF-β, M-CSF, HGF, SCF, LIF, IL-3 were significantly higher in children compared to adults (Fig. 1). However, IL-1β; RANTES, SDF-1α, and β-NGF were significantly lower in children (Fig. 1). This observation suggests that an active production of immune mediators in children could provide a strong anti-viral environment during acute disease that could result in a better clinical outcome.
Levels of Immune mediators (Pro-inflammatory cytokines, anti-inflammatory cytokines, chemokines and growth and other factors) during acute CHIKV infection (samples collected during the admission stage of hospitalization) from two groups of patients (86 children and 64 adults) were analyzed and presented in heat map of normalized scores. In the heat map presentation, the immune mediator concentrations were scaled between 0 and 1 for each measured immune mediator and then the average scaled value computed for each group. Blue colors represent the lowest average scaled value while pink colors represent the highest average scaled value. Immune mediators levels of healthy adults (n = 8) were included as reference point. Differences between the two groups were analyzed using Mann-Whitney U-test, with Bonferroni correction.
Meta-analysis of common immune mediators between adults and children
The levels of immune mediators in adult patients with CHIKV infection have been widely reported from geographically distinct cohorts and compared systematically13. To compare the current data set in this study, a meta-analysis was performed. Source of samples, classification of immune mediators, study selection, study exclusion, and meta-analysis were done as described13. Table 2 shows an overview of the expression profiles of all immune mediators that demonstrated a significant up-regulation relative to the healthy controls. Twenty-six factors: IL-2Ra, IL-6, IFN-α2, IL-16, IL-7, IL-15, IL-12, IL-18, GM-CSF, IL-1ra, IL-10, MCP-1, IP-10, MIG, SDF-1α, G-CSF (P < 0.01); IL-12p40, TNF-α, IL-2, IFN-γ, IL-17, IL-4, MIP-1β, RANTES, MIP-1α, FGF-β (P < 0.05) were found to be age-independent factors for acute CHIKV infection. Forest plots showing the significant elevated immune mediators are summarized in Supplementary Figs S1–S4. Pro-inflammatory cytokines remain as the dominant signature for acute CHIKV infection (>50%) within the four categories of immune mediators. This suggests that a common pattern of immune signature exists from CHIKV infection across ages and cohorts.
Differential immune mediators profiles in different viremic conditions in children
The CHIKF pediatric patients were further classified based on the viremic condition during the hospitalization period, into early viral clearance and prolonged viremia groups (Table 1). Surprisingly, a distinct profile was observed in the immune mediators between these two groups (Fig. 2). Analyzes revealed that higher levels of pro-inflammatory cytokines, chemokines, growth and other factors were obtained in the early viral clearance group (Fig. 2). Profiles of pro-inflammatory cytokines, IL-12p40, IL-1α, TNF-β, TRAIL, GM-CSF, and IFN-γ were shown to be significantly higher in the early viral clearance group than in the prolonged viremia group (Fig. 2). Interestingly, the anti-inflammatory cytokine IL-10 was also significantly higher in the early viral clearance group (Fig. 2). Profiles of chemokines, CTACK, SDF-1α, IP-10, MCP-1 and MIP-1β were significantly higher in the early viral clearance group, while MCP-3 and MIP-1α were significantly higher in the prolonged viremia group (Fig. 2). Comparatively, SCGF-β, PDGF-BB and VEGF levels were significantly higher in early viral clearance group, while LIF level was significantly lower in early viral clearance group (Fig. 2). All other markers were not significantly different between the two groups (data not shown).
Levels of immune mediators during acute CHIKV infection (samples collected during the admission stage of hospitalization) were analyzed. Patients were grouped into early viral clearance (n = 30), and prolonged viremia (n = 34) groups and compared and presented in heat map of normalized scores. In the heat map presentation, the immune mediator concentrations were scaled between 0 and 1 for each measured immune mediator and then the average scaled value computed for each group. Blue colors represent the lowest average scaled value while pink colors represent the highest average scaled value. Differences between the two groups were analyzed using Mann-Whitney U-test, with Bonferroni correction.
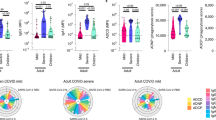
To further determine if any association exists between clinical manifestations with viral clearance, the percentage of patients with different clinical parameters were compared. Our analysis revealed that facial flushing and joint pain occurred more frequently in children in the prolonged viremia group (Table 1 and Fig. 3A). Interestingly, the manifestation of joint pain in children was associated with lower levels of the pro-inflammatory cytokine GM-CSF (Fig. 3B) observed during acute CHIKV infection.
(A) Proportions of patients with joint pain within early viral clearance (n = 25) and prolonged viremia (n = 23) group were analyzed using two-sided Fisher’s exact test. GM-CSF levels were higher in patients without joint pain. (B) Comparison of cytokine levels between patients with (n = 35) or without joint pain (n = 13). Levels are expressed in pg/mL, horizontal lines represent median values. Two-tailed, Mann-Whitney U-tests with Bonferroni correction were used to evaluate differences between the two groups of patients.
Discussion
CHIKF affects patients of different age groups and it is important to obtain a holistic view of CHIKV-induced immune mediators from multiple cohorts of all ages. Here, the profiles of several immune regulators in CHIKV-infected pediatric patients were characterized through systematic meta-analysis in order to better define CHIKV infection in children. Clinical features such as the loss of appetite and not drinking are often linked to CHIKV infection. However, these are constitutional symptoms commonly observed in many bacterial and viral infections as well as non-communicable diseases in children20. Joint-specific arthralgia (specific areas including knee, wrist and small joint of the hands and feet) is a well-characterized hallmark of CHIKF during the acute phase of disease13. Interestingly, a significantly higher percentage of children who suffered from prolonged viremia experienced joint pain. To our knowledge, this is the first study showing a clear association between the viremic phase with arthralgia in CHIKV-infected patients.
Clinicians at the Sibu hospital observed that the overall clinical outcome observed for the majority of children in this cohort is milder than adults. Arthralgia observed in the majority of children was relatively short-lived, mild and rapidly resolved with paracetamol, which was used to provide simple analgesia and treat high fever in the study cohort. At the clinic, the cardinal signs of arthralgia (redness, swelling and increased warmth of the affected joint) were only observed in approximately 20% of the CHIKV-positive children. Indeed, the parents of affected children were more concerned about the high body temperature and skin rashes than the morbidity of arthralgia. Based on the meta-analysis data, different patterns were found in the immune factors between children and adults. Specifically, the levels of pro-inflammatory cytokines such as IL-18, IFN-α2 and IL-2Ra were much higher in children. This is interesting, as children have been reported in various studies to have low basal cytokines levels under healthy physiological conditions, although some cytokines have more complex age-dependent profiles21. Therefore, the high fold increase in some of the critical immune mediators such as IL-18, IFN-α2, IL-2Ra, GRO-α, MIF, MIG, MCP-3, SCGF-β, M-CSF, HGF, SCF, LIF and IL-3 from healthy to disease state could play a role in influencing disease severity in children22. This is in contrast to adults where the basal levels of immune mediators are generally higher, due to prior exposures to a broad range of environmental factors23, infections24, and ageing25.
IL-18 is one of the most important pro-inflammatory cytokines in host defense against infection, and in NK cells activation26. It has been established that NK cells are involved in CHIKV infections27. Therefore, NK cells may have a more prominent role in inflammation and homeostasis in children. Moreover, there is mounting evidence that IL-18 could be a novel therapeutic target in treating inflammatory disease28. On the other hand, IL-2Ra is an important indicator of T cell activation29 and a marker for regulatory T cells (Tregs). More recently, selective expansion of Tregs by the JES6-1 anti-IL-2 antibody complex has been shown to ameliorate experimental CHIKV-infected joint pathology30. Therefore, the higher level of IL-2Ra in children may indicate a larger number of Tregs in children that could alleviate joint inflammation and result in a better disease outcome30,31.
It is surprising that the manifestation of joint pain in children associated with lower levels of the pro-inflammatory cytokine GM-CSF. Since GM-CSF is often described as a key component in experimental osteoarthritis and pain development32 in the IL-1β pathway32. The high levels of GM-CSF observed here could contribute to the control of viremia through its pro-inflammatory effect and this in turn could result in an early viral clearance in this subgroup of children. This raises an interesting point as the level of GM-CSF could have a role in regulating clinical outcomes such as the development of joint pain during the acute phase of CHIKV infection even without engaging the IL-1β pathway.
Previous meta-analysis studies based on CHIKV-infected adult cohorts have defined the immune signature of mediators induced in patients suffering from acute CHIKV infection13. With the inclusion of new data from this pediatric cohort, a new immune signature of acute CHIKV immune mediators was derived. All categories of immune mediators exist in similar proportions, indicating that regardless of age, acute CHIKV infection is driven mainly by an inflammatory response that will in turn exert an anti-viral activity. Once again, IFN-α is significantly up-regulated during the acute phase of disease (Fig. 1) and could be a specific indicator to distinguish between CHIKV and DENV infections as the up-regulation of IFN-α is absent in DENV infection13.
Taken together, this is the first systematic analysis of immune mediators reported in CHIKV-infected children. The addition of this new cohort redefines the significant immune signatures that can be extended to derive a new set of biomarkers specific to acute CHIKV infection in young children (IL-18, IL-2Ra, IFN-α2, G-CSF and MIG) and adult patients (SDF-1α, RANTES). Information from the recent disease outbreaks in the Americas (from Caribbean islands to South America) will be important to provide valuable data to further validate the robustness of this new immune signature and how they can be used for differentiating CHIKV-infected patients from non-CHIKV infected patients regardless of age.
Methods
Ethical Approval – Children cohort from Sarawak (2009) and Adult cohort from Singapore (2008)
Written informed consent was obtained from all participants, participants’ parents or legal guardians and study was conducted according to Declaration of Helsinki principles. For the pediatric cohort, the clinical study and the use of human samples was approved by the Malaysian Ministry of Health’s Institute Review Board (KKM/NIHSEC/08/0804/P07-197). For the adult CHIKF cohort, the study was approved by the National Healthcare Group’s Domain-Specific Ethics Review Board (DSRB Reference No. B/08/026). The methods were carried out in accordance with the approved guidelines.
Patients and Serum Collection
Sixty-four adult patients admitted with acute CHIKF to the Communicable Disease Centre at Tan Tock Seng Hospital in Singapore during the outbreak from 1 August to 23 September 2008 were included in this study18,19. Acute phase plasma specimens were collected at median 4 days post-illness onset (PIO). Clinical features definition and clinical samples were as described previously18,19. Children presented with fever or a history of fever lasting less than 7 days, one or more of the following clinical features: skin rashes, joint pain or muscle pain, and a negative blood film for malaria parasite with no apparent focal infection such as pneumonia or urinary tract infection were included into the study after obtaining informed consent from the parents or guardians. All children did not receive any medication before collection of the first blood sample and samples were taken on the day of hospital admission and at hospital discharge.
PCR and virus isolation
All clinical specimens were screened for CHIKV using either a published33 or in-house (data not shown) real time RT-PCR assay. Viruses were isolated using either the C6/36 mosquito or Vero cell lines. A total of 10 Sarawak partial E1 gene nucleotide sequences from the 2009 outbreak generated in this study were analyzed together with reference sequences obtained from GenBank. A maximum likelihood phylogenetic tree was prepared and edited using the MEGA v6.06 software34. To assess the robustness of the tree, a bootstrap re-sampling analysis of 1000 pseudo-replicate trees was performed. A preliminary phylogenetic investigation of an approximately 500 base-pair nucleotide region of the E1 gene identified the Sarawak CHIKV as part of the East/Central/South African genotype (Supplementary Fig. S5).
Multiplex-Microbead Immunoassay
Serum levels of immune mediators were measured using the Bio-Plex Pro™ human cytokine 21-plex (CTACK, GRO-α, HGF, IFN-α2, IL-12p40, IL-16, IL-18, IL-1α, IL-2Ra, IL-3, LIF, M-CSF, MCP-3, MIF, MIG, SCF, SCGF-β, SDF-1α, TNF-β, TRAIL, β-NGF) and 27-plex (Basic-FGF, Eotaxin, G-CSF, GM-CSF, IFN-γ, IL-10, IL-13, IL-15, IL-17A, IL-1β, IL-1Ra, IL-2, IL-4, IL-5, IL-6, IL-7, IL-8, IL-9, IP-10, IL-12p70, MCP-1, MIP-1α, MIP-1β, PDGF-BB, RANTES, TNF-α, VEGF) immunoassay kits (Bio-Rad) according to the manufacturer’s instruction. Briefly, magnetic beads were aliquoted in 96-well plates followed with addition of standards and sera from patients and control subjects. After an incubation period, plates were washed using a magnetic wash station according to manufacturer’s instructions, followed with addition of a detection antibody. Plates were incubated for a further 30 minutes and washed, followed with a final incubation of 10 minutes in the presence of streptavidin-PE. Results were acquired using the flexMAP™3D (Luminex corp.) with Luminex xPONENT® software, based on standard curves plotted through a 5-parameter logistic curve setting.
Meta-analysis
Meta-analysis (including search strategy, study selection, data extraction for comparison and statistical testing) was done previously13, except for the inclusion of the current data from the two cohorts. Levels of immune mediators from healthy children were obtained from published studies21,35,36,37,38,39.
Data Analysis
Continuous variables were compared between different patient groups using non-parametric Mann-Whitney U test (2-tailed) analysis, with Bonferroni correction. P-values of < 0.05 were considered statistically significant. Hierarchical clustering was done using TM4-MeV40.
Additional Information
How to cite this article: Simarmata, D. et al. Early clearance of Chikungunya virus in children is associated with a strong innate immune response. Sci. Rep. 6, 26097; doi: 10.1038/srep26097 (2016).
References
Robinson, M. C. An epidemic of virus disease in Southern Province, Tanganyika territory, in 1952–1953. Trans R Soc Trop Med Hyg. 49, 28–32 (1955).
Powers, A. M. & Logue, C. H. Changing patterns of chikungunya virus: re-emergence of a zoonotic arbovirus. J. Gen Virol. 88, 2363–2377 (2007).
Ross, R. W. The Newala epidemic. III. The virus: isolation, pathogenic properties and relationship to the epidemic. J. Hyg (Lond). 54, 177–191 (1956).
Renault, P. et al. A Major Epidemic of Chikungunya Virus Infection on Reunion Island, France, 2005 2006. Am J Trop Med Hyg. 77, 727–731 (2007).
Paquet, C. et al. Chikungunya outbreak in Reunion: epidemiology and surveillance, 2005 to early January 2006. Euro Surveill. 11, E060202.3 (2006).
Lahariya, C. & Pradhan, S. K. Emergence of chikungunya virus in Indian subcontinent after 32 years: A review. J. Vector Borne Dis. 43, 151–160 (2006).
Rezza, G. et al. Infection with chikungunya virus in Italy: an outbreak in a temperate region. Lancet 370, 1840–1846 (2007).
Hapuarachchi, H. C. et al. Re-emergence of Chikungunya virus in South-east Asia: virological evidence from Sri Lanka and Singapore. J. Gen Virol. 91, 1067–1076 (2010).
Dupont-Rouzeyrol, M. et al. Chikungunya virus and the mosquito vector Aedes aegypti in New Caledonia (South Pacific Region). Vector Borne Zoonotic Dis. 12, 1036–1041 (2012).
Leparc-Goffart, I. et al. Chikungunya in the Americas. Lancet 383, 514 (2014).
Ng, L. F. P. et al. IL-1beta, IL-6, and RANTES as biomarkers of chikungunya severity. Plos One 4, e4261 (2009).
Wauquier, N. et al. The acute phase of Chikungunya virus infection in humans is associated with strong innate immunity and T CD8 cell activation. J. Infect Dis. 204, 115–122 (2011).
Teng, T. S. et al. A Systematic Meta-analysis of Immune Signatures in Patients With Acute Chikungunya Virus Infection. J. Infect Dis. 211, 1925–1935 (2015).
Rao, G., Khan, Y. Z. & Chitnis, D. S. Chikungunya infection in neonates. Indian Pediatr. 45, 240–242 (2008).
Valamparampil, J. J. et al. Clinical profile of Chikungunya in infants. Indian J Pediatr. 76, 151–155 (2009).
Sebastian, M. R., Lodha, R. & Kabra, S. K. Chikungunya infection in children. Indian J Pediatr. 76, 185–189 (2009).
Cardosa, M. J., Wang, S. M., Sum, M. S. & Tio, P. H. Antibodies against prM protein distinguish between previous infection with dengue and Japanese encephalitis viruses. BMC Microbiol. 2, 9 (2002).
Win, M. K. et al. Chikungunya fever in Singapore: acute clinical and laboratory features, and factors associated with persistent arthralgia. J. Clin Virol. 49, 111–114 (2010).
Ng, K. W. et al. Clinical features and epidemiology of chikungunya infection in Singapore. Singapore Med J. 50, 785–790 (2009).
Dantzer, R. et al. From inflammation to sickness and depression: when the immune system subjugates the brain. Nat Rev Neurosci. 9, 46–56 (2008).
Kleiner, G. et al. Cytokine levels in the serum of healthy subjects. Mediators Inflamm. 2013, 434010 (2013).
Jiang, B. et al. Cytokines as mediators for or effectors against rotavirus disease in children. Clin Diagn Lab Immunol. 10, 995–1001 (2003).
Andiappan, A. K. et al. Genome-wide analysis of the genetic regulation of gene expression in human neutrophils. Nat Commun. 6, 7971 (2015).
Webster, R. G. & Govorkova, E. A. Continuing challenges in influenza. Ann N Y Acad Sci. 1323, 115–139 (2014).
Kim, H. O. et al. Serum cytokine profiles in healthy young and elderly population assessed using multiplexed bead-based immunoassays. J. Transl Med. 9, 113 (2011).
Chaix, J. et al. Cutting edge: Priming of NK cells by IL-18. J. Immunol. 181, 1627–1631 (2008).
Teo, T. H. et al. Caribbean and La Reunion Chikungunya Virus Isolates Differ in Their Capacity To Induce Proinflammatory Th1 and NK Cell Responses and Acute Joint Pathology. J. Virol. 89, 7955–7969 (2015).
Kanai, T., Kamada, N. & Hisamatsu, T. Clinical strategies for the blockade of IL-18 in inflammatory bowel diseases. Curr Drug Targets. 14, 1392–1399 (2013).
Rubin, L. A. et al. Soluble interleukin 2 receptors are released from activated human lymphoid cells in vitro . J. Immunol. 135, 3172–3177 (1985).
Lee, W. W. et al. Expanding regulatory T cells alleviates chikungunya virus-induced pathology in mice. J. Virol. 89, 7893–7904 (2015).
Singh, A. M. et al. Inhaled corticosteroid use is associated with increased circulating T regulatory cells in children with asthma. Clin Mol Allergy. 11, 1 (2013).
Cook, A. D. et al. Granulocyte-macrophage colony-stimulating factor is a key mediator in inflammatory and arthritic pain. Ann Rheum Dis. 72, 265–270 (2013).
Pastorino, B. et al. Development of a TaqMan(R) RT-PCR assay without RNA extraction step for the detection and quantification of African Chikungunya viruses. J. of Virological Methods. 124, 65–71 (2005).
Kumar, S., Tamura, K. & Nei, M. MEGA3: Integrated software for Molecular Evolutionary Genetics Analysis and sequence alignment. Brief Bioinform. 5, 150–163 (2004).
Ashwood, P. et al. Elevated plasma cytokines in autism spectrum disorders provide evidence of immune dysfunction and are associated with impaired behavioral outcome. Brain Behav Immun. 25, 40–45 (2010).
Ashwood, P. et al. Plasma cytokine profiles in Fragile X subjects: is there a role for cytokines in the pathogenesis? Brain Behav Immun. 24, 898–902 (2010).
Liba, Z., Kayserova, J. & Komarek, V. Th1 and Th17 but no Th2-related cytokine spectrum in the cerebrospinal fluid of children with Borrelia-related facial nerve palsy. Fluids Barriers CNS. 10, 30 (2013).
Zhang, S. Y. et al. Immunologic Characterization of Cytokine Responses to Enterovirus 71 and Coxsackievirus A16 Infection in Children. Medicine (Baltimore). 94, e1137 (2015).
Zhang, Y. et al. Comparative study of the cytokine/chemokine response in children with differing disease severity in enterovirus 71-induced hand, foot, and mouth disease. Plos One. 8, e67430 (2013).
Saeed, A. I. et al. TM4: a free, open-source system for microarray data management and analysis. Biotechniques. 34, 374–378 (2003).
Acknowledgements
We thank Drs Boon Chuan Lim, Boon Fu Lai, Beng Suan Lim, Justina Lau and See Chang Wong for their contribution in patient recruitment and sample collection. We thank the study participants and healthy volunteers for their participation, and the research and clinical staff from the Communicable Disease Centre/Tan Tock Seng Hospital for patient enrollment and care. The work was supported by the Biomedical Research Council, A*STAR, and also by operational funds from Universiti Malaysia Sarawak. The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Author information
Authors and Affiliations
Contributions
D.N., M.S., A.C., Y.S.L., D.P., J.C. and M.H.O. contributed the samples, virological and clinical data. D.S., D.P., M.H.O. and L.F.P.N. conceived and designed the experiments. D.S., Y.W.K. and Z.H. performed the experiments. D.N., D.S., Y.W.K., B.L., D.P., M.H.O. and L.F.P.N. analyzed the data. D.S., Y.W.K., D.P., M.H.O. and L.F.P.N. drafted the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Simarmata, D., Ng, D., Kam, YW. et al. Early clearance of Chikungunya virus in children is associated with a strong innate immune response. Sci Rep 6, 26097 (2016). https://doi.org/10.1038/srep26097
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep26097
This article is cited by
-
Innate immune response in patients with acute Chikungunya disease
Medical Microbiology and Immunology (2023)
-
Rheumatic manifestations of chikungunya: emerging concepts and interventions
Nature Reviews Rheumatology (2019)
-
Children with open tibial fractures show significantly lower infection rates than adults: clinical comparative study
International Orthopaedics (2019)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.