Abstract
The role of bone marrow-derived mesenchymal stem cells(BMSCs)in the pathogenesis and therapy of osteoporosis has drawn increasing attention in recent years. In the development of osteoporosis, it has been demonstrated that many changes occurred in the behavior of BMSCs. For example, the biological system of FasL pathways mediated differentiation of ERK and GSK-3β-catenin pathway was damaged. Here we found that 0.35 mg/L Licochalcone A (L-A) had a strong effect in increasing the osteogenic differentiation and mineralization of BMSCs both in vivo and in vitro by up-regulating FasL and further playing a role in regulating the ERK and GSK-3β-catenin systems. It has also demonstrated that the administration of L-A could restore the biological function of the damaged BMSCs differentiation by recovering or protecting bone mass in a disease state through activating the endosteal bone formation and partially inhibiting bone resorption in acute estrogen deficiency model. Results of our study suggested that careful titration of MSC was response to L-A and up-regulated FasL pathways mediating differentiation of ERK and GSK-3β-catenin biological systems under disease state in vivo, restore the impaired function, is one of the ways of L-A relieve or treatment osteoporosis.
Similar content being viewed by others
Introduction
Osteoporosis is a bone metabolism disease characterized by the loss of bone microarchitecture thus increasing the risk of bone fractures. The role of BMSCs in the pathogenesis and therapy of osteoporosis has drawn increasing attention in recent years1,2,3. FAS ligand (FasL) which binds to the Fas receptor is a transmembrane protein that belongs to the TNF family. It represents important apoptotic signaling in many cell types and the pathway of FasL-mediated FAS death has been extensively investigated in the interplay between immune cells, cancer cells and MSC-based immunomodulation4,5,6,7. Previous studies also showed that reduced osteoclast apoptosis might contribute to the osteoporotic phenotype and the administration of estrogen could up-regulate the FasL expression in osteoblasts to induce increased osteoclast apoptosis8,9,10.
Recent studies also showed that FasL promoted the proliferation of human BMSCs, inducing the phosphorylation of ERK1/2 in BMSCs downstream; thus concluded that the ERK1/2-dependent mechanism might be one of the pathways through which BMSCs maintained a stem cell phenotype11,12,13. ERK could inactivate the expression of GSK-3β resulting in an up-regulation of beta-catenin14. The phosphorylation of GSK-3β achieved by ERK binding to it leads to the inactivation of GSK-3β. Thus the expression of β-catenin is increased in the cytoplasm and then it translocate to the nucleus interacting with Tcf/Lefand further leading to a series reactions. So the function of ERK and GSK-3β-catenin relationship might be an important regulator in BMSCs.
During the process of aging, especially for postmenopausal females, BMSCs in bone marrow shift to adipocyte gradually with a reduction of osteogenesis and bone formation, finally resulting in osteoporosis15. In this process, many changes occurred in the behavior of BMSCs such as self-renewal and differentiation ability in addition to cell proliferation, differentiation, cell cycle phases (depending on gene modification) and the production of cytokine and growth factors16,17,18. Our team previously found that the osteogenic differentiation of BMSCs from estrogen deficiency rats with osteoporosis was decreased while the adipogenic differentiation was increased compared with normal BMSCs19. We also found that FasL significantly decreased and ERK and GSK-3β-catenin biological systems changed in BMSCs in the same model.
Some drugs, such as PTH, Bisphosphonates and vitamin D have been used in clinic to stimulate bone formation in osteoporosis patients. However, long-term trials showed that these drugs had no effect in preventing hip fracture. What was more, side-effects such as hypercalcaemia, nausea and diarrhea also happened in the long-term observation20. However, whether BMSCs respond to those drugs in vivo was unclear. As there is a growing consensus that regulating the behavior of BMSCs could increase bone formation, in this study we tried to use small molecular compounds to reverse the abnormal function of BMSCs,aiming to establish a new strategy to relieve or treat osteoporosis. Licorice, one of the most commonly used herbs in traditional medicine, Licochalcone A (L-A) derives from licorice21. It has been proven to have the ability of anti-inflammatory22, anti-parasitic23,anti-cancer24,25 and anti-browning, depigmenting26 and regulating bone metabolism27,28,29. Pharmacological activity of L-A has been broadly studied, but the molecular mechanism is not particularly clear, especially on the differentiation of BMSCs. In this study, we tried to investigate whether L-A had an effect on the osteogenic differentiation of BMSCs in vivo and in vitro. Results indicated that L-A could up-regulated the FasL expression and affect the ERK and GSK-3β-catenin pathway to rescue the differentiation disorder of osteoporotic BMSCs, suggesting a potential therapeutic strategy for osteoporosis as well as bone regenerative medicine.
Results
Effects of L-A on the osteogenic differentiation of BMSCs
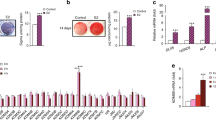
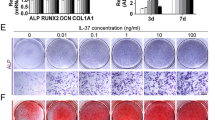
Flow-cytometry analysis showed that BMSCs highly expressed SCA-1, CD29, CD90, CD105 and CD106 while they did not express CD34 and CD45 (Figures not show). We screened different doses of L-A in the procedure of the osteogenic differentiation of BMSCs to choose the optimal dose. L-A at low concentration of 0.035 mg/L had minimal effect on the osteogenic differentiation of BMSCs, whereas higher concentration of 35 mg/L would inhibit BMSCs differentiation. L-A at the concentration ranged of 3.5 mg~0.035 mg/L would improve BMSCs osteogenic differentiation. And the 0.35 mg/L was the optimal dose which could significantly improve the osteogenic differentiation. Under this concentration, Real-time PCR showed that osteogenic marker Col1a1, OCN, Runx-2 and OSX mRNA were significantly increased in L-A treated BMSCs group (Fig. 1.b). Clearly, 0.35 mg/L is the optimum concentration for L-A and this study would carry out under this concentration. Further study revealed that treatment of L-A increased both Alkaline phosphatase (ALP) stained positive colonies and alizarin red stained mineralized nodules in BMSCs that differentiated into osteoblasts as well as the quantitative ALP activity at day 7, 14 and the volume of calcium sediment yield at day 21 of osteogenic induction(Fig. 1.c). Osteogenic marker Col1a1, OCN, Runx-2 and OSX mRNA were also detected at day 7 and day 14, L-A significantly improved the BMSCs osteogenic differentiation in osteo-inducing medium (Fig. 1.d). L-A was also administrated in the group of OVX-BMSCs and Aging-BMSCs and the same tendency was observed with previous results (Supplementary Fig. 1. a, b; Supplementary Fig. 1. a, b). These results indicated that 0.35 mg/L L-A had a pronounced ability to enhance BMSCs osteogenic differentiation and mineralization. To further confirm the role of L-A regulated FasL in BMSCs, we tested whether FasL knockdown in BMSCs rescued the function of L-A. The RT-real time PCR results showed that separate knockdown of FasL decreased the effect of L-A up-regulated MSCs (Supplementary Fig. 7. a). Notably, western blot revealed that the knockdown of FasL decreased the effect of L-A up-regulated MSCs protein level (Supplementary Fig. 7. b), suggesting that L-A up-regulated in the BMSCs functioned through their target gene FasL.
Effects of L-A on BMSCs osteogenic differentiation and mineralization.
(a) Chemical structure of L-A. (b)The ALP activity was represented by the absorbance at 520 nm, screen for the optimal concentration of L-A. Under 0.35 mg/L concentration, osteogenic marker Col1a1, OCN, Runx-2 and OSX mRNA were detected by RT-real time PCR. (c)The ALP activity detected at day 7 and day 14, ALP+ stained CFU-F colonies formed by BMSCs after 14 days culture; mineralized nodules formed by BMSCs after 21 days of culture as demonstrated by alizarin red staining and volume of calcium sediment yield also detected at day21 (L-A group: BMSCs cultured in normal medium add L-A. OS-C group: BMSCs cultured in osteogenic medium. OSL-A group: BMSCs cultured in osteogenic medium add L-A). (d) Osteogenic marker Col1a1, OCN, Runx-2 and OSX mRNA were detected by RT-real time PCR at day 7 and day 14, respectively. Key: n = 6 per group. *P < 0.05, **P < 0.01, ***P < 0.001 compared to the OS-C group. All data are shown as the mean ± s.d.
The mechanism of L-A regulating the osteogenic differentiation of BMSCs
A number of factors and signaling pathways have important roles in the differentiation and stemness maintenance of BMSCs. Factors including BMP-2, FGF, IGF, Runkl/OPG, Fas/FasL and signaling pathways including Mapks, Wnt, Notch1, Nos, Oct4 were reported to participate in the BMSCs differentiation. To investigate the mechanism of L-A regulating BMSCs osteogenic differentiation, we performed Real-time PCR to study the possible genes which may participate in the procedure. Results showed that the expression level of FasL, target gene of Mapk signaling and β-catenin was significantly up-regulated while the expression of GSK-3β was down-regulated (Fig. 2.a). To further confirm the results of real time PCR, results of western blot revealed that the protein expression of FasL, phosphorylation ERK1/2 and active-β-catenin was significantly up-regulated while GSK-3β was down-regulated at the day of 3, 7 and 14 (Fig. 2.b) than control group (OS-C group). This phenomenon was observed both in BMSCs planted in normal cultural medium (L-A group) and osteo-inducing medium (OS-L-A group) which were administrated with L-A. In addition, we also measured gene expression level of FasL, ERK1/2, catenin and GSK-3b at the day of 3, 7 and 14 and results had the same tendency with results in protein level (Fig. 2.c). It was worth noting that the protein and gene expression levels of Runx-2 were stronger in OS-L-A group than that in OS-C group (Fig. 2.b, c).The same tendency was observed with those results in OVX-BMSCs and Aging-BMSCs groups too (Supplementary Fig. 1.c, d; Supplementary Fig. 2.c, d). These results suggested that L-A could stimulate the osteoblastic differentiation of BMSCs by up-regulating the expression of FasL, phosphorylation ERK1/2, inactivated GSK-3b and activated-β-catenin.
The molecule mechanism of L-A was regulated BMSCs osteogenic differentiation.
(a) BMSCs differentiation related factors and signal pathways target gene screening by RT-real time PCR. (b) To further confirm the results of RT-real time PCR, western blot revealed that the protein of FasL, phosphorylation ERK1/2, active catenin, phosphorylation GSK-3b and Runx-2 with the time course of day 3, 7 and 14. (c) Measured gene expression level of the FasL, ERK1/2, Catenin, GSK-3b and Runx-2 at the over time of day 3, 7 and 14. Key: n = 6 per group. *P < 0.05, **P < 0.01 compared to the OS-C group. All data are shown as the mean ± s.d.
Treatment with L-A partially recovers loss of trabecular bone and increases endosteal bone formation in OVX rats
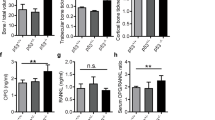
To determine whether L-A could recover bone mass in a disease state, we treated 8-week-old ovariectomized (OVX) rats with PBS or L-A 12 weeks after OVX (Fig. 3.a). OVX model was evaluated by micro CT, results revealed that the trabecular bone volume/total volume (BV/TV) and bone mineral density (BMD) were decreased and trabecular separation (Tb.Sp) was increased than Sham group (Fig. 3.b). TRAP/ALP staining results showed that the endosteal bone formation in trabecular bone in L-A treated group was increased (the black arrows indicated ALP positive) and the TRAP staining was weakly positive (the green arrows indicated) than OVX group. There was no difference in the same group between different time points over 4, 8 and 12 weeks (Fig. 3.c). At each time point, femur bone mass was also detected by micro CT and results indicated that L-A could partially recover the loss of trabecular bone (Fig. 3.d) by means of inducing a higher distal femoral trabecular bone volume (BV/TV) and bone mass (Fig. 3.f,g). The calceinfluorescent labeling of the newly formed bone observed at 4, 8 and 12 weeks (Fig. 3.e) demonstrated the same tendency. Test of loading with a maximum load to the femur and fifth lumbar vertebral bodies (LVB) was also carried out in L-A group, OVX group and Sham group treated with PBS. Results also indicated that L-A group had a stronger potent of anti-pressure load than OVX group, no difference with statistical significance was found between L-A and Sham group (Fig. 3h, i).These data suggested that L-A could activate endosteal bone formation which nearly had the same characteristic of bone tissues in normal state in acute estrogen deficiency model and increase bone mass.
Treatment with L-A partially recovers trabecular bone and increases endosteal bone formation in OVX rats.
(a) Diagram of the study and treatment methods. (b) Trabecular bone volume (BV)/tissue volume (TV), bone mineral density (BMD) and trabecular separation (Tb.Sp) were detected by micro-CT and evaluated OVX rat model. (c) TRAP/ALP staining the section samples of non-decalcified trabecular bone (2 μm thick). Black open arrows indicate new bone formation and green open arrows indicate bone resorption Right-Sidedness image Scale bar, 50 μm. (d) Femur bone mass was detected by micro CT, top; and trabecular bone three-dimensional reconstruction in red box, bottom, Scale bar, 500 μm. (e) The calceinfluorescent labeling of the newly formed bone at different time point. Scale bar, 100 μm. (f) TV/BV of Trabecular bone. (g) BMD of Trabecular bone. Greater maximum load of (h) the femur and (i) the fifth lumbar vertebral bodies (LVB) respectively in L-A group rats treated with L-A compared to OVX and Sham group treated with PBS. Key: n = 6 per group. *P < 0.05, **P < 0.01,***P < 0.001 compared to the OVX group. All data are shown as the mean ± s.d.
Treatment with L-A partially prevents trabecular bone loss and increases endosteal bone formation in OVX rats
To determine whether L-A could prevent trabecular bone loss in a disease state, we treated 8-week-old OVX rats with PBS, L-A 3 days after OVX (Fig. 4.a). OVX model was evaluated by micro CT, after ovariectomized 3 days, BV/TV, BMD and Tb.Sp was detected, there is no difference between Sham group and OVX (Fig. 4.b). The TRAP/ALP staining results showed that the TRAP positive (the green arrows indicated) is increased and ALP positive (the black arrows indicated) was decreased in OVX group at over time of 4, 8 and 12 weeks; but TRAP weakly positive and ALP stronger positive in Sham and L-A treat group at same time point (Fig. 4.c). And femur bone mass also detected by micro CT, L-A could prevent trabecular bone loss (Fig. 4.d), induced a higher distal femoral trabecular bone volume and bone mass to inhibit the bone resorption (Fig. 4.f, g). Compared to the OVX group, L-A could unremitting stimulate new bone formation and partially inhibit bone resorption. The calceinfluorescent labeling of the newly formed bone was also observed at 4, 8 and 12 weeks (Fig. 4.e), with a corresponding greater maximum load of the femur and fifth LVB respectively in L-A group rats treated with L-A compared to OVX and Sham group treated with PBS, L-A group has a stronger potent of anti-pressure load than OVX group, no significantly difference between L-A and Sham group (Fig. 4.h, i).These results suggested an activation of endosteal bone formation and partially inhibit bone resorption by L-A, that is comparable to normal rats bone formation in this acute estrogen deficiency model and increase bone mass.
Treatment with L-A partially prevents trabecular bone loss and increases endosteal bone formation in OVX rats.
(a) Diagram of the study and treatment methods. (b) BV/TV, BMD and Tb.Sp were detected by micro CT and evaluated OVX rat model. (c) TRAP/ALP staining the section samples of non-decalcified trabecular bone (2 μm thick). Black open arrows indicate new bone formation and green open arrows indicate bone resorption. Right-Sidedness image Scale bar, 50 μm. (d) Femur bone mass was detected by micro CT, top; and trabecular bone three-dimensional reconstruction in red box, bottom, Scale bar, 500 μm. (e) The calceinfluorescent labeling of the newly formed bone at different time point. Scale bar,100 μm. (f) TV/BV of Trabecular bone. (g) BMD of Trabecular bone. Greater maximum load of (h) the femur and (i) the fifth lumbar vertebral bodies (LVB) respectively in L-A group rats treated with L-A compared to OVX and Sham group treated with PBS. Key: n = 6 per group. *P < 0.05, **P < 0.01,***P < 0.001 compared to the OVX group. All data are shown as the mean ± s.d.
The effects of L-A on the BMSCs proliferation and differentiation in osteoporosis state
The osteogenic differentiation potential of BMSCs from estrogen deficiency induced osteoporosis rats was decreased and L-A could recover the potent of BMSCs osteogenic differentiation in vitro (Supplementary Fig. 1.). To determine whether L-A could effects BMSCs proliferation and differentiation in the osteoporosis state, we treated 8-week-old OVX rats with PBS, L-A 6 weeks after OVX (Fig. 5.a). OVX model was evaluated by micro CT, BV/TV and BMD were decreased and trabecular separation (Tb.Sp) was significantly increased than Sham group (Fig. 6.b). OVX rats were treated by L-A once a day, a week later, isolated BMSCs from L-A treated, Sham, OVX group rats and performed analysis at the first passage. Proliferation assay (cell clone and MTT assay) showed no difference between L-A treated rats BMSCs and Sham BMSCs, but significantly higher than OVX BMSCs (Fig. 5.b). Osteogenic differentiation assay showed OVX BMSCs formed less ALP positive clone and mineralized nodules after osteogenic induction than L-A treated rats BMSCs and Sham BMSCs, in according with ALP activity and volume of calcium sediment yield, respectively. Real-time PCR showed that osteogenic marker Col1a1, OCN, RUNX2 and OSX mRNA expression were no significantly difference between L-A treated rats BMSCs and Sham BMSCs, but significantly higher than OVX BMSCs (Fig. 5.c). Western blot revealed that the protein of FasL, phosphorylation ERK1/2 and active catenin in L-A treated rats BMSCs and Sham BMSCs is significantly up-regulated and GSK-3b is significantly down-regulated than OVX BMSCs at day7, but no difference between L-A treated rats BMSCs and Sham BMSCs. In addition, we also measured gene expression level of the FasL, ERK1/2, catenin and GSK-3b. It has the same point and tendency with the protein expression level (Fig. 5.d). These results suggested that BMSCs was response L-A in vivo, up-regulated FasL, enhanced phosphorylation ERK1/2, inactivated GSK-3b and activated catenin to restore the biological function of the damaged BMSCs.
The effects of L-A on BMSCs proliferation and differentiation in the osteoporosis state.
(a) Diagram of the study and treatment methods. (b) The first passage cell proliferation was detected by cell clone and MTT assay. Clone formation was detected by trypan blue staining and MTT detected by the absorbance at 570 nm. (c) The ALP activity detected at day 14, ALP+ stained CFU-F colonies formed by BMSCs after 14 days osteogenic culture; mineralized nodules formed by BMSCs after 21 days of osteogenic culture as demonstrated by alizarin red staining and volume of calcium sediment yield also detected at day21 (OVX group: PBS injection OVX rats. L-A group: L-A injection OVX rats. Sham: PBS injection Sham rats), osteogenic marker Col1a1, OCN, RUNX2 and OSX mRNA expression were also detected by RT-real time PCR. (d) Western blot revealed that the protein of FasL, phosphorylation ERK1/2, active catenin and phosphorylation GSK-3b at day 7. Corresponding gene expression was detected by RT-real time PCR at same times. Key: n = 6 per group. *P < 0.05, **P < 0.01 compared to the OVX group. All data are shown as the mean ± s.d.
BMSCs treated by L-A augments bone formation in OVX rats.
(a) Diagram of the study and treatment methods. (b) BV/TV, BMD and Tb.Sp were detected by micro-CT and evaluated OVX rat model. (c) TRAP/ALP staining the section samples of non-decalcified trabecular bone (2 μm thick) including OVX rats injected by OVX-BMSCs, PBS, L-A treated OVX-BMSCs, normal BMSCs and Sham rats injected by PBS, L-A treated normal BMSCs. Black open arrows indicate new bone formation and green open arrows indicate bone resorption. Right-Sidedness image Scale bar, 50 μm. (d) Femur bone mass was detected by micro CT, top; and trabecular bone three-dimensional reconstruction in red box, middle, Scale bar, 500 μm. The calceinfluorescent labeling of newly formed bone at different time point, bottom, Scale bar, 100 μm. (e, f) TV/BV and BMD of Trabecular bone after treated 4 and 8 weeks. Greater maximum load of (g) the femur and (h) the fifth lumbar vertebral bodies (LVB) respectively in OVX/Sham group rats treated with kinds BMSCs. Key: n = 6 per group. *P < 0.05, **P < 0.01,***P < 0.001 compared to the OVX group. All data are shown as the mean ± s.d.
BMSCs treated by L-A augments bone formation in OVX rats
The osteogenic differentiation of BMSCs from estrogen deficiency induced osteoporosis rats was decreased and L-A could recover the potent of BMSCs osteogenic differentiation function in vitro (Supplementary Fig. 1.). Here we performed a homo transplantation study. We intravenously injected L-A treated OVX-BMSCs, OVX-BMSCs, L-A treated Sham-BMSCs, Sham-BMSCs in OVX and Sham rats 6 weeks after surgery (Fig. 6.a). OVX model was evaluated by micro CT, BV/TV and BMD was decreased and trabecular separation (Tb.Sp) was significantly increased than Sham group (Fig. 6.b). At 4 weeks and 8 weeks after injection, TRAP/ALP staining results showed that the positive TRAP staining (the green arrows indicated) was more significant in OVX and OVX-BMSCs injection groups while positive ALP staining (the black arrows indicated) was decreased in this two groups at the same time point. In accordance, TRAP staining and ALP staining in Sham, L-A treated OVX and Sham BMSCs, normal BMSCs injection groups showed an opposite trend at the same time points (Fig. 6.c).The femur bone mass was also detected by micro CT. We observed that OVX-BMSCs injection could not recover the loss of trabecular bone compared with the OVX group; however the newly formed bone tissues in L-A treated OVX-BMSCs injection group was nearly the same with normal BMSCs injection group compared OVX injection PBS negatively control, though a little lower than that of Sham injection PBS group. Newly formed bone tissues in L-A treated normal BMSCs group were a little higher than that of Sham injection PBS, but the difference was not statistically significant. Calceinfluorescent labeling of the newly formed bone tissues was observed at 4, 8 weeks (Fig. 6.d) and the distal femoral trabecular BV/TV and BMD were also analyzed, results were in accordance with that mentioned above (Fig. 6.e, f).Test of maximum load to the femur and fifth LVB was carried out respectively in six groups. L-A treated OVX-MCSs injection OVX rats group, normal BMSCs injection OVX rats group had a stronger potent of anti-pressure load than OVX injection PBS and OVX-MCS injection OVX rats group, no difference with statistical significance was observed between Sham injection PBS and L-A treated normal BMSCs injection Sham group (Fig. 3g, h). These results suggested that L-A treated OVX-BMSCs could activate endosteal bone formation and increase bone mass. Thus L-A could restore the biological function of the damaged BMSCs to perform like normal ones.
Discussion
BMSCs within bone marrow have a multi-lineage potential and give rise to the following cell types: osteoblasts, chondrocytes and adipocytes30,31. BMSCs under going osteogenic differentiation in the bone marrow32,33 and the osteoblastic progenitors mobilizing to the bone surface area crucial steps in osteoblast maturation and forming of mineralized tissues34,35. But during the process of aging, especially for postmenopausal females, BMSCs in bone marrow shift to adipocyte gradually with a reduction of osteogenesis and bone formation, thus finally resulting in osteoporosis15,19. In such a circumstance, many changes occurred in the behavior of BMSCs including self-renewal and differentiation ability in addition to cell proliferation, cell cycle phases and production of cytokine and growth factors16,17,18. In this study we tried to use a small molecular compound to reverse the abnormal function of BMSCs aiming to establish a new strategy to treat osteoporosis. Data showed that 0.35 mg/L L-A had a pronounced ability to enhance BMSCs osteogenic differentiation and mineralization by up-regulating FasL, enhancing phosphorylation ERK1/2, inactivating GSK-3β and activating β-catenin. So we concluded that L-A could recover or protected bone mass in a disease state by activating endosteal bone formation and partially inhibiting bone resorption. And its effect was comparable to bone formation in rats in the normal state in acute estrogen deficiency model. Test of isolated L-A treated OVX rats BMSCs indicated that they were responsible to L-A in vivo through ERK and GSK-3β-catenin pathway by which to restore the biological function of the damaged BMSCs. Further study found that OVX-BMSCs from injection of L-A treatment group realized the same function recovery. So BMSCs response to L-A under disease state in vivo and recovering the impaired function was part of the possible mechanisms of L-A treating osteoporosis.
To further clear the relationship of L-A regulating FasL and BMSCs, Rodrigues et al. found that Fas, the receptor for FasL, was expressed during the procedure when MSC differentiated into osteoblasts and continued to die significantly like undifferentiated MSC, emphasizing the need for continued protection of MSC differentiating into bone cells36. But exogenously adding low level of FasL would promote proliferation of bone marrow-derived mesenchymal stem cells while higher levels inhibited their differentiation into adipocytes12. Previous studies showed that L-A can promote bone metabolism, promote osteoblast osteogenic differentiation inhibit osteoclast resorption27,28,29. Our recent research shows that L-A can promote cell-sheet secretion of extracellular matrix and osteogenic differentiation44. In this study, L-A significantly increased the expression of FasL, but no change in the expression of Fas was observed in BMSCs. We also found that decreasing of FasL in OVX-BMSCs led to a weaker cell potential for proliferation and differentiation. When BMSCs from various experimental groups including normal BMSCs, OVX-BMSCs, Aging-BMSCs were treated by L-A, the FasL expression was up-regulated and further enhanced the BMSCs osteogenic differentiation and mineralization. So it was important to maintain the stability of the FasL level or moderately increase its expression so as to keep the balance of proliferation and differentiation of BMSCs. FasL has the ability of promoting the proliferation of BMSCs, inducing the phosphorylating procedure of ERK1/2 and survival in up-regulation in BMSCs. And it was through ERK1/2-dependent mechanisms that BMSCs maintain stem cell phenotype11,12,13,37. This phenomenon was observed in all the experimental groups especially in OVX-BMSCs treated by L-A and cells from L-A injection osteoporosis rats; the effect of L-A treated MSCs to augment bone formation and increase bone mass had the same effect with that of normal BMSCs injected group. We also found that the cell proliferation and differentiation of BMSCs from L-A intraperitoneal injected osteoporosis rats were not decreased. But BMSCs from osteoporosis rats without administrating L-A would regenerate a lower bone mass than the OVX group, it is the negative control. So maintaining the stem cell phenotype of BMSCs was very crucial for bone homeostasis. Previous studies has reported that stem cell phenotype could be maintained through FasL and p-ERK pathway which would be up regulated by L-A. ERK also associates with primary GSK-3β for its inactivation resulting in up-regulation of beta-catenin14. It's worth noting that activating GSK-3β can be obtained by inhibiting Wnt dependent signaling pathway38,39,40,41. ERK through binding to GSK-3β and phosphorylating GSK-3β leads to the inactivation of it. Thus the expression of β-catenin is increased in the cytoplasm and translocats to the nucleus interacting with Tcf/Lefand further leading the series reactions downstream. As a result, it is through FasL/p-ERK and GSK-3β-catenin pathway that L-A enhance the osteogenic differentiation and mineralization of BMSCs and it would be a new pharmacology molecular mechanism of protecting bone metabolism and regulating bone regeneration.
FASL-mediated FAS death pathway has been extensively investigated in the interplay between immune cells, cancer cells and MSC-based immunomodulation4,5,6,7. To locate the migration of injected BMSCs, we observed that almost all the GFP-BMSCs were entered the spleen and bone marrow after intravenous injection 24, 48 hours, 7days and 14days while vascular walls of liver, heart and lung could only be observed only a few BMSCs; renal tissue was not detected the BMSCs (Supplementary Fig. 3.). As immune function declines under osteoporosis condition, migration of normal BMSCs into spleen and bone marrow might regulate the immune function of OVX-rats and change the microenvironment of bone metabolism, inhibiting osteoclast function and promoting bone formation. In both BMSCs injection and L-A injection treating group, FASL-mediated FAS death pathway had been activated and thus may protect the bone metabolism through regulating the immune function and maintain the balance of osteoblast/osteoclast8,9,10. We also observed the portion of the BMSCs moved on femoral growth plate and trabecular bone surface in bone marrow. It may be directly involved in the regulation procedure of the inhibition of osteoclast activity, promoting osteoblast bone formation process (Supplementary Fig. 4.White arrows indicate).
In summary, we found L-A could significantly up-regulate the expression of FasL, enhance ERK phosphorylation, making ERK further binding to GSK-3β and phosphorylating it to lead to an inactivation of GSK-3β. As a result, stabilized β-catenin in BMSCs led to enhanced or recovered function of osteogenic differentiation of damaged cells both in vivo and in vitro. The results of our study suggested that careful titration of BMSCs respond L-A in vivo may be a promising avenue for the prevention of osteoporosis or the treatment of its early stages.
Methods
Animals
All animal procedures were performed according to the guidelines of the Animal Care Committee of the Fourth Military Medical University, Xi'an, China and all experimental protocols were approved by Fourth Military Medical University. Four-2-week-old female SD rats, Four-24-month-old female SD rats were used to isolate BMSCs. One hundred and ten 8-week-old female SD rats were randomly divided into two groups and they underwent either sham surgery or bilateral ovariectomy (OVX) under general anesthesia by the dorsal approach. Then all rats were housed under specific pathogen-free conditions (22°C, 12-hour light/12-hour dark-cycles and 50–55% humidity) with free access to food pellets and tap water for6 months.
Cell culture
Primary culture of BMSCs was established as described previously42. 2-week-old,24-month-old, OVX/Sham/L-A treated female SD rats were sacrificed by dislocation of the cervical spine. Tibias and femurs were immediately dissected from attached muscles and tissues using aseptic techniques, respectively. Ends of bones were removed, marrow plugs were flushed dispersed by repeated pipetting and cells were forcefully passed through a 19-gauge needle to obtain a single cell suspension. Cells were cultured in growth medium containing a-MEM (Invitrogen, Carlsbad, CA, USA) supplemented with 10% FBS, 1% penicillin and streptomycin. The cell suspension was seeded in10-cm tissue culture dishes and grown in the growth medium in a humidified at mosphere of 5% CO2 at 37°C, respectively. The medium was changed every 2–3 days to remove non-adherent cells and adherent cells were cultured until they were confluent. At confluence, BMSCs were passaged after digestion with 0.25% trypsin/1 mM EDTA.
ALP activity measured with time course and ALP histochemical staining
BMSCs were plated in 12-well tissue culture plates. When cells were confluent, osteoinduction medium (10−8 Mdexamethasone, 10 mM b-glycerophosphate and 50 mg/ml ASAP) containing 0.0035 mg–35 mg/L L-A(Sigma-Aldrich, Cat No.58749-22-7) was changed. Equal volumes of vehicle (DMSO) were used as control. ALP activity was measured after7 and 14 days (n = 6 per time point). Cells were rinsed twice and sonicated for 15 s in 2 ml of 50 mM Tris-HCl, pH 7.2, containing 0.1% TritonX-100 and 2 mM MgCl2. ALP activity was measured using a commercial kit, as instructed (Nanjing Jiancheng Bioengineering Ltd, Nanjing, China). A modified method of King (Powell and Smith 1954) was used in the kit and results were expressed as nmol phenol/15 min/mg protein. Protein concentrations were determined using a BCA protein assay kit. To further compare the potency of different concentration L-A to stimulate osteogenic differentiation, numbers of colonies positive for ALP were also compared on day 14. Cells were fixed in 3.7% formaldehyde and 90% ethanol solution for 5 min, washed then stained a commercial kit of ALP stain, as instructed (Beyotime Institute of Biotechnology, shanghai, china). 0.35 mg/L had previously been found to be optimal concentration for L-A, to improve osteogenic differentiation.
Alizarin red staining and Calcium deposition measured
Histochemical alizarinred staining of mineralized cell nodules was carried out on day 21. Briefly, cells were fixed in 3.7% form aldehyde for 10 min and stained in 0.1% alizarin red for 1 h at 37°C. Calcium deposition measurements were performed on day 21 after osteoinduction cultured. Briefly, cultures were rinsed twice in PBS and decalcified for 24 h in 0.1 M HCl; calcium content in HCl supernatant samples was measured using a calcium colorimetric assay kit (Biovision, San Francisco, CA, USA) and results were expressed as mg/dish.
Real-time RT-PCR of mRNA expression
Total RNA was separated using Trizol reagent (Invitrogen) according to the manufacturer's standard instructions. For reverse transcription of mRNA, random-primed cDNA was synthesized from 2 mg of total RNA using a Prime Script RT reagent kit (TaKaRa, Dalian, China).Real-time PCR was performed using 2 uL of cDNA product in a 25 uL reaction volume with 7500 Real Time PCR System (Applied Biosystems, Singapore). SYBR®PremixExTaq™II (Takara Biotechnology), specific primers (see below) and 2 uL of cDNA were used in each PCR reaction (95°C for 30 s, 40 cycles of denaturation at 94°C for 5 s and annealing and extension at 60°C for 30 s).Sense and antisense primers were designed with Primer Express 5.0 based on published cDNA sequences. GAPDH was used as internal control gene. All real-time PCR reactions were performed in triplicate and results after calibration with GAPDH expression were calculated using the ΔΔCT method and are presented as fold increase, relative to non-stimulated control.
Western blot analysis
The western blot analysis was performed as previously described43,45. Whole-cell lysates were extracted with lysis buffer for western blotting. 25 ug proteins were loaded on 10% sodium dodecyl sulfatepoly acrylamide gels, transferred to polyvinylidene fluoride membranes (Millipore, Billerica, MA, USA) and blocked with 5% nonfat milk powder in PBST (PBS with0.1% Tween), respectively. The membranes were probed overnight with the following primary antibodies. The primary antibody for mouse RUNX2, p-GSK-3b (Abcam, Cambridge, MA, USA), ERK1/2, p-ERK1/2, active-catenin, b-actin (Cell Signaling, Beverly, MA, USA), FasL (Santa Cruz, Dallas, TX, USA) were used in this study. Then, the membranes were incubated with peroxidase-conjugated secondary antibody (Boster, Wuhan, China). The blots were visualized using an enhanced chemiluminescence kit (Amersham Biosciences, Piscataway, NJ, USA) according to the manufacturer's recommended instructions. The gray values of the blots in the pictures were measured with Image-Pro Plus 6.0 software (Media Cybernetics, Inc. Bethesda, MD, USA). The b-actin as internal control to verify the consistency of the amount of all of the samples, based on this, for each of the detection of the target protein, the expression level of a sample is set to “1”, compare the ratio between the different samples. Repeat the test to verify whether there is a stable protein changes in trends or consistency.
L-A treatment in vivo
Three months/days after the ovariectomy (the animal model evaluated by micro CT), the rats were injected intraperitoneally twice a week with 0.35 mg/kg body weight of L-A as the treatment group, also injected Sham and OVX sesame oil (as a vehicle control) for 12weeks. Three days before death, all rats were injected calceinwith 10 mg/kg. Three rats were sacrificed every group by dislocation of the cervical spine at 4, 8 and 12 weekend, all femurs were isolated intactly. Three left femurs used to scanning micro CT (Siemens Inveon Micro CT, Germany), then decalcified in 0.5 M EDTA and paraffin-embedded tissue sections. Three right femurs used to execute three-point bending test evaluation of the strength of rats femur, then the calceinfluorescence was observed by Leica heavy-duty sectioning and Leica SP1600 saw microtome (Leica, Germany).
Response of BMSCs on L-A in vivo
Ten weeks after the ovariectomy (the animal model evaluated by micro CT), the rats were injected intraperitoneally once a day with 0.35 mg/kg body weight of L-A as the treatment group, also injected Sham and OVX sesame PBS (as a vehicle control) for 12 weeks. 7 days later, isolated the BMSCs from Sham, OVX and L-A treated OVX group respectively. Cell proliferation was assessed by the trypan blue staining cell clone and MTT assay as previously described44,45.Cell differentiation was detected by ALP attaining and ALP activity measure, Alizarin red staining and Calcium deposition measure, osteogenic marker and signal pathway related mRNA expression were detected by RT-real time PCR. Protein expressions detected by western blot.
BMSCs treatment in vivo
Ten weeks after the ovariectomy (the animal model evaluated by micro CT), isolated Sham/OVX BMSCs and amplification cultured. The second generation of Sham/OVX BMSCs was planted 10-cm tissue culture dishes, half of dish with Sham/OVX BMSCs was treated by L-A. 1 × 106 cell/kg body weight intravenous injection, including OVX-BMSCs injected OVX rats group, Sham-BMSCs injected OVX rats group, L-A treated OVX-BMSCs injected OVX rats group, Sham-BMSCs injected Sham rats group, PBS injected OVX rats group and PBS injected Sham rats group. Three rats were sacrificed every group by dislocation of the cervical spine at 4 and 8 weekend, all femurs were isolated intactly. Three left femurs used to scanning micro CT (Siemens Inveon Micro CT, Germany), then decalcified in 0.5 M EDTA and paraffin-embedded tissue sections. Three right femurs used to execute three-point bending test evaluation of the strength of rats femur, then the calceinfluorescence was observed by Leica heavy-duty sectioning and Leica SP1600 saw microtome (Leica, Germany).
TRAP/ALP staining
Alkaline phosphatase (ALP) and tartrate-resistant acidphosphatase (TRAP) are known as marker enzymes for osteoblasts andosteoclasts, respectively. So we used TRAP/ALP staining kit (Walo Chemical USA, Inc,) to examine the state of differentiation of bone cells and the cell distribution in bone tissues by observation of the stained images of osteoblasts and osteoclasts. GMA embedded thin sample sections of non-decalcified bone (2 um thick) were applied to silan coated slides and washed with water. 0.5 mL TRAP staining soln was applied on each section in a moist chamber at room temperature for 30 minutes. Then adding sufficient distilled water to soak the sections in 3Coplin-staining jars and washing the sections in these jars for 1 min each. Later sufficient amount of 0.1 M AMPD-HCl buffer (pH 9.4) was added to soak the sections in each Coplin-staining jar for 10 minutes. After that, excessive moisture on the slides was remove and applying 0.5 mL ALP substrate soln on each section for 30 minutes in a moist chamber at room temperature. The same as previously described, add sufficient distilled water to soak the sections in 3Coplin-staining jars and wash the sections in these jars for 1 min each. Finally, add distilled water to soak the sections in a Coplin-staining jar and apply 0.5 mL nuclear staining soln on the sections. After 4~5 seconds, wash the sections by moving them up and soaking in distilled water. The sections were dried on a heater plate at 37°C. Add a sufficient amount of xylene to soak the sections in each Coplin-staining jar. Mount the sections using mounting agents such as Softmount and Malinol and observation was performed.
Transfection of FasL siRNA
The FasL siRNA was purchased from RiboBio. The cells were transfected with FasL siRNA and negative control at final concentrations of 100 nM. The Lipofectamine 2000 (Invitrogen) was used according to the manufacturer's instructions. In brief, cells were passaged in six-well plates and were 30–50% confluent at the time of transfection. The diluted oligomer was combined with the diluted Lipofectamine 2000 and added to each well. The cells were incubated at 37C in the incubator for 48 h before further assay.
Statistics
All values are the mean ± SEM. The statistics were performed with GraphPadPrism 5 software using an unpaired Student's t test to compare two independent groups or pair for sequential measurements. One-way ANOVA were performed when comparing different groups.
References
Smith, D. & Walker, M. Changes in plasma steroids and bone density inKlinefelter's syndrome, Calcif. Tissue Res. 22 Suppl225–8 (1977).
Foresta, C. et al. Testosterone andbone loss in Klinefelter syndrome. Horm. Metab. Res. 15, 56–57 (1983).
Daniell, H. Osteoporosis due to androgen deprivation therapy in men withprostate cancer. Urology. 58, 101–107 (2001).
Hohlbaum, A. M., Moe, S. & Marshak-Rothstein, A. Opposing effects of transmembrane and soluble Fas ligand expression on inflammation and tumor cell survival. J.Exp Med. 191, 1209–1220 (2000).
Zhang, Y., Xu, G., Zhang, L., Roberts, A. I. & Shi, Y. Th17 cells undergo Fas-mediated activation-induced cell death independent of IFN-gamma. J.Immunol. 181, 190–196 (2008).
Akiyama, K. et al. Mesenchymal-stem-cell-induced immunoregulation involves FAS-ligand-/FAS-mediated T cell apoptosis. Cell Stem Cell. 10, 544–55 (2012).
Micheau, O. & Tschopp, J. Induction of TNF receptor I-mediated apoptosis via two sequential signaling complexes. Cell. 114, 181–190 (2003).
Garcia, A. J. et al. ERalpha signaling regulates MMP3 expression to induce FasL cleavage and osteoclast apoptosis. J. Bone Miner Res. 28, 283–90 (2013).
Krum, S. A. et al. Estrogen protects bone by inducing Fas ligand in osteoblasts to regulate osteoclast survival. J.EMBO. 27, 535–45 (2008).
Nakamura, T. et al. Estrogen prevents bone loss via estrogen receptor alpha and induction of Fas ligand in osteoclasts. Cell. 130, 811–823 (2007).
Pricola, K., Kuhn, N., Haleem-Smith, H., Song, Y. & Tuan, R. Interleukin-6 maintains bonemarrow-derived mesenchymal stem cell stemness by an ERK1/2-dependent mechanism. J. Cell Biochem. 108, 577–588 (2009).
Rippo, M. R. et al. Low FasL levels promote proliferation of human bone marrow-derived mesenchymal stem cells, higher levels inhibit their differentiation into adipocytes. Cell Death Dis. 18, 4:e594.doi: 10 (2013).
Rojewski, M., Weber, B. & Schrezenmeier, H. Phenotypic characterization of mesenchymalstem cells from various tissues. Transfus Med Hemother. 35, 168–184 (2008).
Ding, Q. et al. Erk associates with and primes GSK-3beta for its inactivation resulting in upregulation of beta-catenin. Mol Cell. 19, 159–70 (2005).
Veronesi, F. et al. Mesenchymal stem cells in the aging and osteoporoticpopulation. Crit Rev Eukaryot Gene Expr. 21, 363–77 (2011).
Bonyadi, M. et al. Mesenchymal progenitor self-renewal deficiency leads to age-dependent osteoporosis in Sca-1/Ly-6A null mice. Proc. Natl. Acad. Sci. USA. 100, 5840–5 (2003).
Katsara, O. et al. Effects of donor age, gender and in vitro cellular aging on the phenotypic, functional and molecular characteristics of mouse bone marrow–derived mesenchymal stem cells. Stem Cells Dev. 20, 1549–61 (2011).
Stolzing, A., Jones, E., McGonagle, D. & Scutt, A. Age-related changes in human bone marrow-derived mesenchymal stem cells: consequences for cell therapies. Mech. Ageing Dev. 129, 163–173 (2008).
Liao, L. et al. Redundant miR-3077-5p and miR-705 mediate the shift of mesenchymal stem cell lineage commitment to adipocyte in osteoporosis bone marrow. Cell Death Dis. 18, 4:e600 (2013).
Rachner, T. D., Khosla, S. & Hofbauer, L. C. Osteoporosis: now and the future. Lancet. 377, 1276–1287 (2011).
Shibata, S. A drug over the millennia: pharmacognosy,chemistry and pharmacology of licorice. YakugakuZasshi 120, 849–862 (2000).
Kolbe, L. et al. Anti-inflammatory efficacy oflicochalcone A: correlation ofclinical potency and in vitro effects. Arch Dermatol Res. 298, 23–30 (2006).
Mi-Ichi, F. et al. Parasite mitochondria as a target ofchemotherapy: inhibitory effect of licochalcone A on thePlasmodium falciparum respiratory chain. Ann NY Acad Sci. 1056, 46–54 (2005).
Rafi, M. M. et al. Modulation of bcl-2 and cytotoxicity bylicochalcone-A, a novel estrogenic flavonoid. Anticancer Res. 20, 2653–2658 (2000).
Fu, Y. et al. Licochalcone-A, a novel flavonoid isolated fromlicorice root (Glycyrrhizaglabra), causes G2 and late-G1 arrestsin androgen-independent PC-3 prostate cancer cells. BiochemBiophys Res Commun. 322, 263–270 (2004).
Fu, B., Li, H., Wang, X., Lee, F. S. & Cui, S. Isolation and identificationof flavonoids in licorice and a study of their inhibitory effects ontyrosinase. J.Agric Food Chem. 53, 7408–7414 (2005).
Kim, M. H. et al. Baicalein inhibits osteoclast differentiation and induces matureosteoclast apoptosis. Food Chem Toxicol. 46, 3375–3382 (2008).
Kim, J. M. et al. Baicaleinstimulates osteoblast differentiation via coordinating activationof MAP kinases and transcription factors. J Cell Biochem. 104, 1906–1917 (2008).
Soon, N. K. et al. In vitro and in vivo osteogenic activity of licochalcone A. Amino Acids. 42, 1455–1465 (2012).
Owen, M. & Friedenstein, A. J. Stromal stem cells: marrow-derived osteogenic precursors. Ciba Found. Symp. 136, 42–60 (1988).
Bruder, S. P., Fink, D. J. & Caplan, A. I. Mesenchymal stem cells in bone development, bone repair and skeletal regeneration therapy. Cell. Biochem. 56, 283–294 (1994).
Halleux, C., Sottile, V., Gasser, J. A. & Seuwen, K. Multi-lineage potential of human mesenchymal stem cells following clonal expansion. J. Musculoskelet. Neuronal Interact. 2, 71–76 (2001).
Muraglia, A., Cancedda, R. & Quarto, R. Clonal mesenchymal progenitors from human bone marrow differentiate in vitro according to a hierarchical model. J. Cell Sci. 113, 1161–1166 (2000).
Adams, G. B. et al. Stem cell engraftment at the endosteal niche is specified by the calcium-sensing receptor. Nature. 439, 599–603 (2006).
Chen, X. D., Dusevich, V., Feng, J. Q., Manolagas, S. C. & Jilka, R. L. Extracellular matrix made by bone marrow cells facilitates expansion of marrow-derived mesenchymal progenitor cells and prevents their differentiation into osteoblasts. J Bone Miner Res. 22, 1943–1956 (2007).
Rodrigues, M., Blair, H., Stockdale, L., Griffith, L. & Wells, A. Surface tethered epidermal growth factor protects proliferating and differentiating multipotential stromal cells from FasL-induced apoptosis. Stem Cells. 31, 104–16 (2013).
Li, H. et al. Fas Ag-FasL coupling leads to ERK1/2-mediated proliferation of gastric mucosal cells. Am J PhysiolGastrointest Liver Physiol. 294, G263–75 (2008).
Cook, D. et al. Wingless inactivates glycogen synthase kinase-3 via an intracellular signalling pathway which involves a protein kinase C. EMBO J. 15, 4526–4536 (1996).
Itoh, K., Antipova, A., Ratcliffe, M. J. & Sokol, S. Interaction of dishevelled and Xenopusaxin-related protein is required forwnt signal transduction. Mol. Cell. Biol. 20, 2228–2238 (2000).
Ruel, L., Stambolic, V., Ali, A., Manoukian, A. S. & Woodgett, J. R. Regulation of the protein kinase activity of Shaggy(Zeste- white3) by components of the wingless pathway in Drosophila cellsand embryos. J. Biol. Chem. 274, 21790–21796 (1999).
Li, L. et al. Axin and Frat1interactwith dvl and GSK, bridging Dvl to GSK in Wnt-mediated regulation of LEF-1. EMBO J. 18, 4233–4240 (1999).
Nian, H. et al. Antiosteoporoticactivitof icariin in ovariectomized rats. Phytomedicine 16, 320–326 (2009).
Liu, Y. et al. MiR-17 modulates osteogenicdifferentiation through a coherent feed-forward loop in mesenchymal stem cells isolatedfrom periodontal ligaments of patients with periodontitis. Stem Cells. 29, 1804–1816 (2011).
Ming, L. G. et al. The prenyl group contributes to activities of phytoestrogen 8-prenynaringenin in enhancing bone formation and inhibiting bone resorption in vitro. Endocrinology. 154, 1202–14 (2013).
Shang, F. et al. The effect of licochalcone A on cell-aggregates ECM secretion and osteogenic differentiation during bone formation in metaphyseal defects in ovariectomized rats. Biomaterials. 35, 2789–97 (2014).
Acknowledgements
This study was supported by the grants from the National Major Scientific Research Program of China (2010CB944800 and 2011CB964700) and the Nature Science Foundation of China (81470710, 31030033, 31301062, 81300718 and 31301140).
Author information
Authors and Affiliations
Contributions
M.L., L.W., J.F. and H.P. wrote the main manuscript text; M.L., L.H., Z.L. and Y.W. prepared figures; Z.Y., M.L. and J.Y. designed experimental and analysis data. All authors reviewed the manuscript.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Electronic supplementary material
Supplementary Information
Supplementary Information
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License. The images or other third party material in this article are included in the article's Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder in order to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/4.0/
About this article
Cite this article
Ming, L., Jin, F., Huang, P. et al. Licochalcone A up-regulates of FasL in mesenchymal stem cells to strengthen bone formation and increase bone mass. Sci Rep 4, 7209 (2014). https://doi.org/10.1038/srep07209
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep07209
This article is cited by
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.