Abstract
Hepatitis C virus (HCV) is the causative agent of end-stage liver disease. Recent advances in the last decade in anti HCV treatment strategies have dramatically increased the viral clearance rate. However, several limitations are still associated, which warrant a great need of novel, safe and selective drugs against HCV infection. Towards this objective, we explored highly potent and selective small molecule inhibitors, the ellagitannins, from the crude extract of Pomegranate (Punica granatum) fruit peel. The pure compounds, punicalagin, punicalin and ellagic acid isolated from the extract specifically blocked the HCV NS3/4A protease activity in vitro. Structural analysis using computational approach also showed that ligand molecules interact with the catalytic and substrate binding residues of NS3/4A protease, leading to inhibition of the enzyme activity. Further, punicalagin and punicalin significantly reduced the HCV replication in cell culture system. More importantly, these compounds are well tolerated ex vivo and‘no observed adverse effect level’ (NOAEL) was established upto an acute dose of 5000 mg/kg in BALB/c mice. Additionally, pharmacokinetics study showed that the compounds are bioavailable. Taken together, our study provides a proof-of-concept approach for the potential use of antiviral and non-toxic principle ellagitannins from pomegranate in prevention and control of HCV induced complications.
Similar content being viewed by others
Introduction
Hepatitis C virus (HCV) is one of the main causes of chronic liver disease. It is estimated that around 170 million people are chronically infected with HCV worldwide1. Chronic infection of HCV is linked to deregulation of innate and adaptive immune signaling mechanisms as well as virus induced cytotoxicity. Error prone viral genomic replication in the hepatic micro environment permits immune evasion and facilitates viral persistence, which in turn drives the progression to liver fibrosis, cirrhosis and hepatocellular carcinoma2. The rapidly evolving HCV RNA leads to a challenge for development of specific antiviral therapies against all viral genotypes. The current therapy including a combination of pegylated IFN-α (pegIFN-α) and ribavirin with either telaprevir or boceprevir has significantly increased the sustained viral response (SVR) in genotype 1 infected patients. However, this therapy suffers some additional limitations. In particular, slow decline of viral load during triple therapy has high risk for the selection of resistance associated with variants3. Therefore, the development of more potent, safe, immune-boosting and well tolerated medications is the need of the hour.
A vast majority of natural components or dietary components are capable of modulating mitogenic signals, cell cycle regulation, angiogenesis, apoptosis and metastasis4. Few of the plant derived dietary components have been explored for their abilities to interfere with all possible stages of HCV life cycle via different mechanisms and proved valuable to HCV therapy. Recently, naringenin (grapes) has been shown to inhibit apolipoprotein B-dependent secretion of HCV particles5. Proanthocyanidin (blueberry) suppresses HCV replication, possibly by interacting with hnRNP A2/B6. Curcumin (turmeric) inhibits HCV replication via suppressing the AKT SREBP-1 pathway7 and entry of all HCV genotypes into human liver cells8. Epigallocatechin-3-gallate (green tea) inhibits HCV entry9. Also, its phenolic epicatechins (+/−) inhibit HCV replication via cyclooxygenase-2 pathway10. Similarly, quercetin has been shown to inhibit HCV by targeting the cellular heat shock proteins, HSPs 40 and 7011. It also abrogates the HCV NS3/4A protease activity in vitro as well as ex vivo12.
Pomegranate (Punica granatum) is one of the natural delicious fruit consumed worldwide. In Ayurvedic medicine, it is described under its Sanskrit name ‘dalima’ (fruit) as a blood purifier13. It has been used for centuries for treatment of variety of health disorders. Apart from its anti-inflammatory and anti-cancerous activities14, it inhibits viral infections, such as HIV15,16, influenza17, enterovirus18 etc. Fruit peel of P. granatum, comprising almost 26–30% of total fruit weight, is enriched with hydrolysable tannins (punicalin, pedunculagin, punicalagin, ellagic acid and gallic acid), anthocyanins and catechins. These compounds account for 92% of the antioxidant activity19,20. P granatum fruit extract doesn't cause side effects and not known for drug interactions; rather it prevents liver fibrosis21. However, systematic analysis of the anti-HCV properties of P. granatum and its principle ellagitannin members has not been studied so far. In this context, we explored anti-HCV properties of P. granatum fruit peel extract and its ellagitannin derivatives, punicalin (PLN), punicalagin (PGN) and ellagic acid (EA). These compounds showed dose dependent inhibition of HCV NS3/4A protease activity in vitro and considerable reduction of HCV RNA levels in HCV subgenomic replicon and infectious cell culture systems using HCV-JFH1 (genotype-2a) virus and H77S (genotype-1a) RNA. Interestingly, these active compounds were found to be systemically bioavailable and very well tolerated upto 5000 mg/kg b.wt in BALB/c mice and meet all the needs for being potent anti-HCV therapeutic molecules.
Results
Identification of bioactive compounds from P. granatum fruit peel based on bioassay guided method
The crude methanolic extract (~90%) of P. granatum fruit peel and juice were evaluated for their anti-HCV NS3 protease activity. Although both peel and juice extracts showed inhibition of NS3 protease activity, but peel extract was found to be more effective than the juice extract (Fig. 1A). Further, the HPLC analyses of crude methanolic extract of P. granatum fruit peel revealed punicalin (PLN), punicalagin (PGN) and ellagic acid (EA) as major constituents (Supplementary Fig. S1). Subsequently, this peel extract was successively partitioned by n-hexane (fraction-1), chloroform (fraction-2) and ethyl acetate (fraction-3) in a polarity gradient (Supplementary Fig. S2A) and concentrated. These fractions (fractions1-3) and left over residue (residue-3) were assessed for their potential to inhibit HCV NS3 protease activity. Among these, residual fraction (residue-3) was identified as biologically most active in inhibiting NS3 protease (Fig. 1B and Table 1). Interestingly, HPLC analysis of this residual fraction also revealed the presence of PLN, PGN and EA as major components (Supplementary Fig. S2B). The residual fraction-3 was further sub-fractionated by size exclusion column chromatography. The PLN, PGN were eluted sequentially in water (sub-fractions 1A & 1B) indicating that these are highly polar compounds whereas EA was eluted in both alcohol (sub-fraction 2A) and acetone (sub-fractions 3A & 3B). These sub-fractions were concentrated by rotary evaporator. Identities of these purified compounds were confirmed by LC ESI-MS (Supplementary Fig. S3–S5) and were authenticated by NMR, IR and UV spectroscopy studies (data not shown). These purified compounds were further evaluated for their anti-HCV properties.
P. granatum crude extract, its different fractions and ellagitannins specifically suppress HCV NS3/4A protease activity.
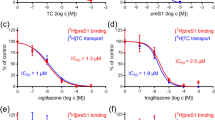
(A) The purified NS3/4A protease enzyme was pre-incubated with increasing concentrations (1, 4, 6, 8 and 10 μg/mL) of P. granatum fruit peel and juice extracts followed by addition of the substrate (EGFP-NS5A/B site-CBD fusion protein). The ability of these extracts to inhibit substrate cleavage efficiency of protease was quantified by measuring fluorescence intensity. The relative enzyme activity was normalized with the DMSO vehicle control (denoted as C). (B) Experiment similar to panel ‘A’ was performed with different fractions 1 to 3 and residue 3 (denoted as Fr 1–3 and Res-3) at a concentration of 10 μg/mL to identify the most active fraction. DMSO (vehicle) and crude fruit peel extract (denoted as CE) were used as mock and positive controls. (C) Experiment similar to panels ‘A’ and ‘B’ was performed with increasing concentrations (0.1, 0.25, 0.5, 1.0, 2.5, 5.0, 10.0 μM) of purified ellagitannins EA, PGN, PLN. Telaprevir (a known protease inhibitor) was used as positive control. ‘C’ denotes DMSO vehicle control, ‘TEL’ denotes telaprevir. (D) Cellular protease (trypsin) was incubated with its substrate FITC-casein in the presence of increasing concentrations (1.0, 2.5, 5.0, 10.0, 25.0 μM) of EA, PGN and PLN. Fluorescence intensity of cleaved product was quantified using fluorometer. Results shown as mean ± SD from three independent experiments and each were done in duplicates.
PLN, PGN and EA block HCV NS3/4A protease activity in vitro
Purified PGN, PLN and EA were tested for inhibition of NS3 protease activity. All these compounds inhibited the NS3/4A protease activity in a concentration dependent manner with IC50 values of less than 0.1 μM for PGN and PLN, whereas IC50 for EA was achieved at ~1.0 μM (Fig. 1C and Table 1).
We also compared the inhibitory potentials of laboratory purified compounds with commercially procured compounds (Fig. 1C and Supplementary Fig. S6A). No considerable difference was observed in the inhibitory activity of these compounds obtained from two different sources.
To further clarify whether only PGN, PLN and EA are the key players from P. granatum extract inhibiting NS3 protease activity, we have tested thirteen more pure compounds (quercetin, luteolin, catechin, epicatechin, gallic acid, caffeic acid, kaempferol, 3,3′-O-methyl ellagic acid -4′-O-β-D-xylopyranoside, apigenin, methyl gallate, rutin, ferulic acid and asiatic acid) present in P. granatum, for anti HCV-NS3 protease activity. Some of these compounds (such as quercetin and luteolin) showed considerable inhibition, albeit at several folds higher concentration than required by PGN, PLN and EA (Supplementary Fig. S6B and Fig. 1C). Also, the levels of these compounds (such as quercetin and luteolin) are not abundant in pomegranate. Our observations suggested that PGN, PLN and EA are major contributors present in P. granatum fruit peel extract that inhibit HCV NS3 protease.
Further, to demonstrate the specificity of these compounds to HCV NS3 protease, we have analyzed the effect of these compounds on trypsin (an unrelated porcine pancreatic cellular serine protease) activity using fluorometric assay (Fig. 1D). Our observations clearly demonstrated that these ellagitannins do not have any inhibitory effect on cellular trypsin protease activity upto 25 μM.
Structural basis of HCV NS3/4A protease inhibition by PGN, PLN and EA
Current experimental analysis showed NS3 protease inhibition by PLN, PGN and EA. The structural basis of interaction of the ligands of interest with HCV NS3 protease was also studied to understand the molecular basis of inhibition. Ligands similar to PLN, PGN and EA were found to be bound to proteins such as proteases especially serine proteases (PDB id: 1dy8, 1dy9, 1bma, 1btx, 1eld, 1ele, 1fpc, 1p01, 2est). In fact, one among the serine proteases included HCV NS3 protease bound to α-ketoacid inhibitor (1dy8, 1dy9)22. Interestingly, analysis showed that all the serine proteases were inhibited in the catalytic region and substrate binding region (competitive inhibition). Also, similarity of oxy atom in the ligands of serine proteases picked up and the ligands of interest were observed, where the oxy group interacts with the catalytic residue S139. These analyses raise the possibility of ligands of interest interacting with NS3 protease like the ligand bound serine proteases that were being compared.
Docking results showed that the ligands of interest indeed were found to interact with two of the three catalytic triad residues23 namely S139 and H57. C and O atoms of all the ligands interact with H57 by means of hydrophobic and hydrogen bonds. C and O atoms of all the ligands interact with S139 by means of hydrogen bonds which are consistent with the NS3-ligand bound complexes that were picked up. Moreover, some of the substrate interacting residues23 (L135, F154, R155, A156, A157, V158 and R161) along with other residues in NS3 were also found to interact with all ligands of interest as shown in Fig. 2. Few notable interactions are F154 which makes aromatic-aromatic contact with C,O groups with all ligands, A156 and A157 which makes hydrophobic contact with C and O groups respectively with ligand, R135 which makes hydrogen bond with C,O groups of punicalin and punicalagin. Other residues in NS3 that interact with all ligands are V132, K136 and C159. The binding energy of NS3 bound to PLN, PGN and EA were found to be −3.33 Kcal/mol, −4.46 Kcal/mol and −5.91 Kcal/mol respectively. These binding energy values suggest as favorable interaction with the protein-ligand complexes. The KI or inhibition constant values for all the NS3-ligand bound complexes were predicted to be in micromolar concentration (Fig. 2). These analyses therefore suggest that PLN, PGN and EA could interact favorably with the catalytic triad residues and the substrate interacting residues of NS3 protease, thereby causing enzyme inhibition.
Depicting the molecular docking studies of ligand protein interactions.
(A) Left side: HCV NS3 protease complexed with punicalin: Here, punicalin (yellow) interacts with catalytic residues (green), substrate interacting residues (pink) and other residues (grey) in HCV NS3 protease. Interactions such as hydrogen bonds, hydrophobic bonds and aromatic-aromatic interactions are shown as dotted lines. All the ligand bound NS3 structures are generated using PyMOL. Right side: Zoomed in view of left side figure. (B) Left side: HCV NS3 protease complexed with punicalagin: Here, punicalagin (yellow) interacts with catalytic residues (green), substrate interacting residues (pink) and other residues (grey) in HCV NS3 protease. Interactions such as hydrogen bonds, hydrophobic bonds and aromatic-aromatic interactions are represented as dotted lines. Right side: Zoomed in view of left side figure.(C) Left side: HCV NS3 protease complexed with ellagic acid: Here, ellagic acid (yellow) interacts with catalytic residues (green), substrate interacting residues (pink) and other residues (grey) in HCV NS3 protease. Interactions such as hydrogen bonds, hydrophobic bonds, aromatic-aromatic interactions are shown as dotted lines. Right side: Zoomed in view of left side figure. The structures of protein-ligand complex figures were generated using PyMOL.
Crystal structure of NS3 bound to clinically approved NS3 inhibitor- ‘telaprevir’ (PDB id: 3sv6)24 is available. However, in order to arrive at an idea of the accuracy of the modeled complex structures, we have generated a model of NS3 protease bound to telaprevir (Supplementary Fig. S7) using the protocol described in the methods section. It must be noted that we did not use any information from the crystal structure of NS3-telaprevir complex. Once the model of the complex is generated, it is compared with the crystal structure so that accuracy of the model could be ascertained (Supplementary information and Supplementary table S1). As can be seen from the supplementary section several features found in the crystal structure of NS3-telaprevir complex are also found in the modeled complex.
It is already well known that the ligand binding pocket in HCV NS3 protease is shallow and solvent exposed23. However, it has been known from the crystal structure that telaprevir is capable of interacting with NS3 through an extensive network of interactions encompassing both the substrate binding and the catalytic residues. The current study has shown that similar mode of inhibition is also been adopted by punicalin, punicalagin and ellagic acid to successfully bind and inhibit the shallow binding pocket of NS3 protease.
Additionally, the structural basis for the inability of the ligands to inhibit porcine pancreatic trypsin (PDB code for the 3-D structure of porcine trypsin: 1s81)25 was explored. Since both NS3 protease (SCOP family: b.47.1.3 - Viral proteases)26 and porcine pancreatic trypsin (SCOP family: b.47.1.2 - eukaryotic proteases) belong to different families of the same SCOP superfamily (SCOP superfamily: b.47.1 - trypsin like serine proteases), they can be considered as distant homologs. Therefore, it is safe to assume that mode of ligand binding, if it binds, to trypsin would be similar to ligand binding to NS3 protease.
NS3 protease-ligand modelled complex (Fig. 2) has been used to identify the ligand interacting residues in NS3 protease. Trypsin was structurally aligned27 with the NS3 protease bound to ligand molecule and the interface between trypsin and the ligand molecule was studied.
We noticed loss of interactions, compared to NS3 protease complex, due to amino acid substitutions (For example: hydrophobic to charged amino acid), presence of short contacts and changes in conformation in trypsin with its interaction to the ligand. (For detailed assessment of interaction between trypsin and ligands refer Supplementary tables S2, S3 and S4). It is known that the S1 pocket of NS3 protease is hydrophobic (L135, F154, A157)23 and some of these residues are also found to interact with the ligand in the NS3-ligand complex structure. However, the equivalent residues in trypsin are substituted with amino acids which are not congenial for interaction with the ligand. For example Ala 157 of NS3 is substituted by Trp in porcine trypsin leading to a short contact with the ligand. Another case of substitution of Leu 135 in NS3 to a cysteine in trypsin that is disulphide bonded with another cysteine has been observed. (Supplementary tables S2–S4). In spite of both NS3 protease and trypsin being distant homologs, several unfavorable structural and physicochemical features could preclude the interaction of the ligand molecules with trypsin, thereby not affecting its trypsin activity.
Effect of PLN, PGN and EA on HCV RNA replication and virus entry
We further evaluated the inhibitory role of PLN, PGN and EA on HCV RNA replication. Huh7 cells harbouring HCV monocistronic replicon genotype-2a were used for this purpose. Replication efficiency was assessed using real time RT- PCR at 48 hours post addition of inhibitors. It was evident from the results that PGN, PLN, EA reduce HCV negative strand RNA levels in a dose dependent manner (Supplementary Fig. S8A). The effective concentrations (EC50) of these compounds are listed Table 2.
Inhibitory effects of compounds were also demonstrated ex vivo by using genotype 2a (JFH1) or genotype 1a (H77S) based infectious cell culture systems (Fig. 3A and 3B). Results indicate that these compounds inhibit HCV replication of both the genotypes. Since it is well-known that quantitative RT-PCR alone lacks strand-specificity for HCV29, we employed more stringent strand-specific tagged primer based RT-PCR method30 and validated the replication suppression effect of the testing compounds (Supplementary Fig. S8B).
P. granatum principle ellagitannins inhibit HCV RNA replication.
(A) Huh7.5 cells were infected with HCV-JFH1 virus (genotype 2a) and treated with 150 μM of EA, PGN and PLN. At 48 h post treatment, HCV negative strand RNA synthesis was quantified using RT-qPCR. GAPDH (a house keeping gene) amplification was used as an endogenous control for normalization of data. Results are expressed in fold change of RNA levels. These results are representative of three independent experiments and are expressed as mean ± SD. (B) Huh 7.5 cells were transfected with HCV-H77S (genotype 1a) RNA and treated with PLN, PGN and EA (150 μM each). At 48 h post treatment, HCV RNA levels were quantified using RT-qPCR. (C) To determine the role of EA, PGN and PLN in inhibiting HCV entry, Huh7.5 cells were infected with the HCV-JFH1 virus in absence and presence of the compounds (150 μM each). At 72 h of post treatment, total cellular RNA was extracted and subjected to RT-qPCR. ‘C’ denotes control (no treatment). Data represent mean ± SD from three independent experiments.
As it was observed above that these ellagitannins affect HCV replication, next we have investigated the effect of these compounds on HCV entry (if any). For this, Huh7.5 cells were preincubated at 4°C and pretreated with JFH1 virus and shifted to 37°C for 3 h in the presence of the compounds (150 μM each) followed by media change. At 72 h post-treatment total cellular RNA was isolated and viral RNA levels were quantified by real time PCR. Results showed strong inhibition of HCV entry by PLN and PGN (Fig. 3C).
To rule out whether the reduction of HCV RNA replication by these ellagitannins was due to activation of cellular interferon (IFN) signalling or not, we have treated HCV-JFH1 infected cells with PGN, PLN or IFNα and checked the expression of phosphorylated signal transducer and activator of transcription 1 (pSTAT 1). PGN and PLN did not show appreciable phosphorylated form of STAT 1 compared to IFNα treatment. Our data suggest that PGN or PLN mediated suppression of HCV RNA replication might not be due to activation of cellular IFN signalling pathway (Supplementary Fig. S8C).
PGN, PLN and EA are nontoxic in cell culture
To investigate the cellular toxicity of these compounds (if any), we tested the effect of crude fruit peel extract (CE), residual fraction (Res 3), PGN, PLN and EA on cell viability. For this purpose, Huh7 cells or Huh7 harbouring replicon 2a cells were treated 0–2.5 mg/mL of CE &Res-3 (RF) and 0–5 mM of either PGN, PLN or EA (Fig. 4A, 4B and Supplementary Fig. S9). Results indicate that these compounds are non-toxic to the cells. These compounds rescued the cell death of JFH1 infected Huh7.5 cells (Fig. 4C), suggesting that these compounds are nontoxic in cell culture.
Determination of cytotoxicity of P. granatum extract and ellagitannins.
(A) Huh7 cells were incubated with increasing concentrations of crude peel extract (CE) and residue-3 (0.1, 0.5, 1.0 and 2.5 mg/mL) and cytotoxicity was determined by MTT assay. Percentage cell viability was plotted considering 100% for DMSO vehicle control (denoted by C). (B) Experiment similar to panel A was performed with increasing concentrations (0.05, 0.1, 0.5, 1.0, 2.5 and 5.0 mM) of EA, PGN and PLN. (C) JFH1 infected Huh7.5 cells were incubated with PGN, PLN and EA (150 μM) and percentage cell viability was plotted. ‘C’ denotes ‘control with no infection and no treatment’. Results represent mean ± SD from three independent experiments and each was done in duplicates.
No adverse effect was observed in oral acute toxicity in vivo
Next, we investigated the maximum tolerance levels of crude extract (CE) and purified compounds in BALB/c mice. Animals administered with an acute dose of 2000 mg/kg b.wt. did not show any adverse symptoms in terms of body weight, intake of water and food, general behavior and mortality upto 14 days post treatment period (Supplementary Fig. S10A). Moreover, further increase in the concentration of PLN, PGN and EA upto 5000 mg/kg b.wt, did not induce any toxic signs and showed high level of tolerance with increasing body weight (Supplementary Fig. S10B). Additionally, gross organ morphology and relative weights of vital organs (liver and spleen) in BALB/c mice did not change (Supplementary table S5). The LD50 for the oral administration of PGN, PLN and EA was estimated to be >5000 mg/Kg.
In contrast, a slight decrease in the survival rate was noticed when 5000 mg/kg b.wt. of CE was given to the mice. Although no delayed death was observed but approximately 30% death between 24 to 72 h was noticed (Supplementary table S5) suggesting that compounds other than PGN, PLN and EA in CE might be responsible for inducing toxicity in mice. Taken together, in accordance with Globally Harmonized Classification System (GHS) mentioned in OECD-423 guidelines, PLN, PGN and EA can be classified into category-5∞ (i.e. unclassified) demonstrating that these compounds could be considered as safe and devoid of toxicity.
No adverse effect was observed in subacute toxicity assay in vivo
Repeated oral administration of PGN, PLN and EA at 1000 mg/kg b.wt./day for 28 days separately to three different groups did not induce any obvious toxic symptoms (Supplementary Fig. S10C). Also, no difference was observed in the relative organ weights of dissected liver and spleen between the treated and control groups (Supplementary table S6).
Histological examination of mice liver and spleen showed normal histoarchitecture
Histopathological analyses of the liver sections of control (sterile distilled water) and mice treated with CE, PLN, PGN and EA (acute doses of 2000 and 5000 mg/kg b.wt.) showed normal histoarchitecture with respect to the polygonal shape of the hepatocytes, clear rounded nuclei, central veins, blood sinusoids, portal veins (Fig. 5A). Similarly, no pathological symptoms were observed in spleen sections (Supplementary Fig. S11).
(A) Histopathological examination of mice liver to determine the toxicity of inhibitors. The acute toxicity effect of vehicle control (SDW, 500 μl/animal) and test samples (5000 mg/kg b.wt of CE, punicalin, punicalagin and ellagic acid) were evaluated in comparison with normal healthy mice at intra tissue level. The histological sections of healthy control mice liver retained normal tissue architecture. The liver sections of mice treated with pure compounds and CE showed near to normal arrangement of the hepatic cords, central veins and polygonal hepatocytes. Here, (a): normal control, (b) & (c): crude extract at an acute dose of 2000 and 5000 mg/kg b.wt, (d) & (e): punicalagin 2000 and 5000 mg/kg b.wt, (f) & (g): punicalin 2000 and 5000 mg/kg b.wt, (h) & (i): ellagic acid 2000 and 5000 mg/kg b.wt. Whereas, (j), (k) & (l): punicalagin, punicalin and ellagic acid at 1000 mg/kg/day for 28 days in subacute toxicity studies. An arrow indicates minimal multifocal hepatocellular necrosis observed in liver histology upon EA treatment for 28 days. (B) Systemic bioavailability of principle ellaginnins of P. granatum in BALB/c mice after oral administration. An acute dose of 1000 mg/kg b.wt of PGN, PLN and EAwas administered orally to three different groups of BALB/c mice separately. The availability of EA (an active metabolite of PGN and PLN) in plasma at different time points of post treatment (0 to 24 h) from 3 different groups was determined by HPLC analyses. Availability of these compounds in the plasma in HPLC chromatogram was identified based on the retention time of the standard reference compounds. The total amount of EA obtained in the plasma (per mL) was determined based on the standard calibration curve for EA and AUC (Area under the curve) was plotted. Pharmacokinetics parameters including maximum plasma concentration (Cmax) and time (Tmax) of EA was calculated. Values used to plot AUC are mean ± SD from the two biologically independent experiments.
Further toxicity evaluations of PLN and PGN in subacute toxicity studies also did not reveal any change in the histoarchitecture of liver and spleen tissues after 28 days of repeated administration of 1000 mg/kg/day. However, only a minimal multifocal hepatocellular necrosis was observed in liver histology upon EA treatment for 28 days (Fig. 5A and Supplementary Fig. S11).
Orally administered PGN, PLN and EA are systemically bioavailable
For a compound to reach to tissue to exert its effects, it must be taken into the blood stream before being taken up by the target cells. Therefore, it was important to test the bioavailability of PGN, PLN and EA in the blood. For this purpose, all three compounds were administered orally at 1000 mg/kg b.wt. Based on HPLC analyses, only EA was detected in varying concentrations with PGN, PLN and EA treated mice plasma samples. In none of the plasma samples intact forms of PGN and PLN compounds were detected. This might be due to rapid metabolism of PGN and PLN into active EA by action of various digestive enzymes and gut microflora. Interestingly, relative increase of 1.9 and 1.6 folds in absorption of EA was observed in PLN (Cmax = 5.5 μg/mL) and PGN (Cmax = 4.8 μg/mL) administered groups respectively as compared to EA (Cmax = 2.9 μg/mL) plasma samples and this absorbed EA rapidly cleared out from the blood by 4th h. This increased concentration of EA in PGN, PLN treated plasma samples might be due to higher polarity and greater solubility of both of these compounds in water than EA. No corresponding EA peak was detected in the plasma collected before consumption of these components (0th hour time point) (Fig. 5B). Taken together, our pharmacokinetic evaluations revealed that these compounds are systemically absorbed from the gastrointestinal tract into blood plasma.
Discussion
Plant based remedies have a long history in the treatment of different diseases including viral infections and liver diseases. Plant derived compounds are considered as unique because of their high chemical diversity, drug-likeliness properties, biochemical specificity to different viral enzymatic assays and capacity of being absorbed and metabolized by the body with little or no toxicity than synthetic ones31. Moreover, the advancement of purification and characterization methods of active compounds become further useful in broad spectrum screening of library of plant derived compounds for anti-HCV therapy.
Our current study includes logical and stepwise elucidation process to explore the role of immune-stimulant ellagitannins derived from P. granatum in suppressing HCV infection. HCV NS3 protein, a chimera of helicase and serine protease, is involved in viral polyprotein processing and replication. This protein hijacks the host cellular machinery via mimicking the host cell proteins and directly disrupting the TLR-3 and RIG-I based antiviral signaling, which in turn results in suppression of innate immune responses32,33. Our in vitro experiments suggest that the principle components of P. granatum, PGN, PLN and EA impede the function of protease activity by directly acting on HCV NS3/4A protease. In general, tannins have the ability of complexing with metal ions and targeting macromolecular proteins and polysaccharides34. Therefore, it is possible that these compounds interact with zinc moiety present in the core region of the enzyme and thereby block its activity. Apart from this, our structural based studies also strongly prove the preferential binding of PLN, PGN and EA to the catalytic triad and substrate binding sites of NS3protease enzyme. It is also evidenced by one of the earlier reports suggesting that the galloyl residues of glucopyranose ring of polyphenols interact with Ser139, Gly137, Ala157 and Asp81 of NS3/4A protease by hydrogen bond interactions and with Ala156 and His57 by hydrophobic interactions35. The presence of galloyl residues in punicalagin and punicalin provides additional support for the inhibitory activities of these molecules against NS3/4A protease. Additionally, no inhibitory effect of these compounds on cellular serine protease (trypsin) activity upto the concentrations tested in our study, might suggest the safe use of these compounds without affecting normal host cell functions.
Although, our study clearly supports antiviral properties of PGN, PLN and EA isolated from P. granatum fruit peel extract against HCV RNA replication, the intricate mechanisms of these antiviral properties remain to be elucidated. Inhibition of NS3 protease by PGN, PLN and EA (as described above) might affect proteolytic processing of HCV polyprotein and lead to reduced levels of active viral RNA dependent RNA polymerase, thereby suppresses HCV RNA levels. Apart from this possibility, there are several evidences based on general properties of these compounds from the previous studies that correlate with their possible mechanistic roles in inhibiting viral enzyme activity and replication. HCV infection activates the expression of cyclooxgenase-2 (COX-2). Increased production of COX-2 contributes to the HCV RNA replication36. COX-2 induces HCC by activating PI3-kinase-AKT signaling pathway37, which is directly associated with the regulatory mechanism of apoptotic inhibition during acute infection, long term virus survival and transformation38. However, it is evidenced from the previous studies that principle ellagitannins of P. granatum fruit preferentially inhibit COX-2 activity39 and thereby may exert anti-inflammatory effects. The cytosolic phospholipase A2 (PLA2) is an important host factor required for HCV replication, assembly and production of infectious HCV particles. P. granatum extract and its polyphenolic constituents act synergistically against proliferation, metastatic potential and PLA2 expression in human cancer cell lines in-vitro40. Further, EA induces apoptosis in human prostatic cancer cell line via downregulation of the anti-apoptotic proteins such as HO-1 (Heme oxygenase-1), HuR (Human antigen R) and SIRT1 (silent information regulator). It also reduces the TGF-β (transforming growth factor -β) and IL-6 (interleukin-6) apoptotic markers in a prostate cancer cell line41. EA also induces the apoptosis in pancreatic cancer cells via inhibiting the NF-κB and causing mitochondrial depolarization activation42. Moreover, EA exhibits an anti-carcinogenic action via modulating oxidative stress regulated genes43. Interestingly, both PLN and PGN contain an ellagic acid core and might perform similar functions as EA and contribute to inhibition of HCV induced hepatocarcinogenesis.
Our pharmacokinetic analyses and normal histoarchitecture of liver and spleen in both acute and sub acute toxicity studies also suggested safety of these compounds for preclinical trials due to their lack of toxicity. In support of our study, an earlier report based on bioavailability and metabolism of PGN in rats showed detection of 3–6% of the ingested punicalagin as metabolites in plasma, urine and faeces44. Moreover, long-term repeated administration of PGN was demonstrated as nontoxic to rats45.
Taken together these results raised a new hope such that the vast majority of hepatoprotective properties of P. granatum fruit and its principle ellagitannins could be collectively exploited to block the HCV life cycle at different stages.
Methods
Collection and extraction of Punica granatum fruits
The fresh fruits of P. granatum were collected from the local market, washed thoroughly and fruit peel was separated from the aril. The shade dried peels were extracted with methanol (MeOH, 90%) under reflux condenser. The arils containing seeds were squeezed in MeOH. Further, these extracts were concentrated by rotary evaporator (IKA, Germany).
Isolation of bioactive principles by bioassay guided method
In order to identify the active components of the P. granatum fruit, we used the strategy illustrated in Supplementary Fig. 2A. The residual fraction (residue 3) of crude fruit peel extract was further sub-fractionated by size exclusion column chromatography using sephadex LH-20 (Sigma Aldrich, USA). The major compounds PLN, PGN and EA were eluted successively and identified by LC-ESI-MS (HPLC: Thermo Finnigan Surveyor; MS: Thermo LCQ Deca XP MAX; Software: Xcalibur). Further characterization and confirmation of their identities was done by NMR (AV III NMR spectrometer at 400 MHz and 100 MHz respectively), UV and IR spectral analyses.
Plasmid constructs
Plasmids, pYB-43 (single-chain NS3/NS4A) and pYB-44 (EGFP-NS5A/B-CBD) encoding a fusion protein containing NS3/4A cleavage site at the middle flanked by enhanced green fluorescent protein and cellulose binding domain were obtained from Dr. Itai Benhar, Tel Aviv University. The HCV JFH146 and H77s47 cDNA constructs were generous gifts from Dr. Takaji Wakita, National Institute of Infectious Diseases, Tokyo and Dr. Stanley Lemon, University of North Carolina respectively.
Cell culture
Huh7 cell line harboring HCV monocistronic replicon of genotype 2a29 was received from Dr. Ralf Bartenschlager, Heidelberg University. Huh7.5 cell line was received from Dr. Charles M. Rice, Rockefeller University. All cells were cultured in Dulbecco's modified Eagle's medium (DMEM; Sigma-Aldrich) supplemented with 10 percent heat-inactivated fetal bovine serum (Gibco), 100 U/mL of penicillin (HiMedia) and 100 μg/mL of streptomycin sulphate (HiMedia) and maintained in 5% CO2 and 37°C conditions. For stable maintenance of replicon 2a harboring Huh7 cell line, hygromycin B (25 μg/mL) was used as an additive supplement.
Compounds used for biological assay studies
All the test compounds either laboratory purified or purchased from commercial source (Natural Remedies, Bangalore, India). Telaprevir (a standard protease inhibitor approved by the US Food and Drug Administration) was purchased from MedChem Express, USA.
Preparation of test samples for in vitro and cell culture studies
Natural compounds as well as telaprevir were stored at a concentration of 10 mM in 100% dimethyl sulfoxide (DMSO). Whereas dried methanolic extract of P. granatum fruit peel and juice extracts and different fractions (fraction 1–3) as well as residue-3 were prepared in concentration of 1 mg/10 μL (w/v).
NS3 protease assay
To examine the effect of different compounds PGN, PLN, EA and crude extract on HCV NS3/4A protease activity, a fluorimetric assay was performed as described earlier48. Briefly, purified single chain NS3 protease (0.1 μM) was pre-incubated with increasing concentrations of test samples followed by the addition of purified fusion substrate protein (EGFP-NS5A/B-CBD, 0.5 μM) and incubated for another one hour at 37°C. The reaction was terminated and intensity of fluorescence signal evolved from the cleaved EGFP substrate was quantified by fluorometer (Modulus™ Microplate Multimode Reader) using excitation filter 485 nm and emission filter 538 nm.
Cellular trypsin protease assay
A simple sensitive cellular protease (trypsin) assay was performed in vitro using protease fluorescent detection kit (Sigma-Aldrich) as per manufacturer's instructions. This assay detects protease activity using casein labeled with fluorescinisothiocynate (FITC) substrate49.
Structural knowledge-based analysis and molecular docking
Ligands similar to PLN, PGN and EA were searched in PDB50, in the ligand-bound protein structures, using ligand expo51. Ligand similarity was assessed by comparing their SMILE strings (SMILES string: The simplified molecular input line-entry system: Line notation which describes the structure of chemical molecules). Ligands bound to various protein structures that were similar to the ligands of interest were analyzed for their mode of inhibition, nature of interaction using protein-ligand interaction server, LPC CSU52 and catalytic atlas53. Since the structure of EA resembled the sub-structures of PLN and PGN, the knowledge-based analysis was extrapolated for EA. Therefore the analysis helped in selectively docking the ligands of interest at the critical regions such as the catalytic region and the substrate binding region of NS3 protease (PDB id: 1dy832-active HCV serine protease complexed with co-factor NS4A). The 3D structures of the ligand compounds were obtained from TCM (Traditional Chinese medicine) database54. Protein-ligand docking was carried out using Autodock 4.255. The best ranked model with low binding energy was analyzed further and visualized using PyMOL (The PyMOL Molecular Graphics System Version 1.5.0.4)56. Telaprevir structure was used to dock on to the NS3 structure and a similar docking protocol was followed as described earlier.
Antiviral assay for subgenomic replicon cell culture system
Huh7 cells harboring HCV replicon were treated with increasing concentrations of test compounds, PGN, PLN and EA (10–150 μM) and further incubated for 48 h. Cells were harvested in TRIzol reagent (Sigma-Aldrich). Total cellular RNA was extracted followed by reverse transcription using HCV forward primer (for capturing the HCV negative strand) corresponding to IRES region (5′-TGCGGAACCGGTGAGTACA-3′). The obtained cDNA was mixed with SYBR Green PCR Master Mix and subjected to quantitative PCR. GAPDH was used as an endogenous control for normalizing results.
JFH-1 antiviral assay
HCV JFH-1 infectious virus particles were produced as described earlier46. Huh 7.5 cells were infected with JFH1 virus in the absence or presence of different test compounds, PGN, PLN and EA at 150 μM, followed by harvesting of cells at 72 h post treatment. Total cellular RNA was extracted and subjected to RT-qPCR.
H77S based replication assay
H77s-cDNA construct was linearized and H77s RNA was synthesized by run-off transcription. Huh 7.5 cells were transfected with infectious H77s RNA using lipofectamine 2000. Four hours later, cells were treated with test compounds. At 48 h post-treatment, cells were collected for total cellular RNA isolation followed by RT-qPCR.
HCV entry inhibition assay
Huh7.5 cells were seeded in 6 well plate with a cell count of 0.3 × 106. Next day, cells were preincubated at 4°C for 1 h followed by infection with the HCV-JFH1 virus at 4°C for 2 h to allow the viral particles to attach with cell surface receptors. This was followed by treatment of the cells plus virus complex with the compounds and shifted to 37°C for another 3 h. This shift allows the virus to enter the cell. At 72 h of post treatment total cellular RNA was extracted and subjected to RT-qPCR.
Cytotoxicity assay
The cytotoxic effects of different test compounds in cell culture were determined by MTT assay as described earlier57.
Ethical clearance for in vivo studies
The animal experiments were approved by ‘Institutional Animal Ethics Committee’. BALB/c mice (6 to 8 weeks old) were selected from an inbred colony and maintained under standard controlled conditions. The animals were provided with pelleted food and water ad libitum.
Preparation of drug for in vivo study
The required concentrations of CE, PLN, PGN and EA were dissolved in sterile distilled water (SDW). Only SDW without the compounds was used as a vehicle control in all in vivo experiments.
Determination of acute oral toxicity
For the safety evaluation, the acute toxicity of CE of P. granatum fruit peel and its bioactive principles, PGN, PLN and EA were determined according to Organization for Economic Co-operation and development guidelines (OECD 423)58. Female BALB/c mice were fasted for four hours. The acute doses (2000 and 5000 mg/kg body weight b.wt.) of the extract and compounds were administered orally. Animals were provided with food and water after 2 h of drug administration and monitored continuously for toxic signs. Body weight and mortality was recorded regularly till 14 days. On 14th post-treatment day, all mice from control and treated groups were sacrificed and histopathology of liver and spleen tissues were investigated using haematoxylin and eosin stains (Bioneeds India Pvt Ltd, Bangalore).
Determination of subacute toxicity
Subacute toxicity was determined as per OECD 407 guidelines59. Healthy BALB/c mice were divided into 4 groups of 3 mice each. A single dose of 1000 mg/kg b.wt/mouse/day of PGN, PLN, or EA was given continuously for 28 days to each group separately. During the treatment period general behavior, food and water intake, signs of abnormality and mortality were recorded critically. Body weight of each mouse in different groups was taken every alternative day. On 29th day, all mice were sacrificed. Liver and spleen were weighed and subjected to histopathological analyses.
Evaluation of bioavailability in BALB/c mice
Here, total of 48 mice were taken and divided into three groups of 16 mice each. A single dose (1000 mg/kg b.wt. per mouse) of PGN, PLN and EA was administered orally to each group separately. Blood samples were collected at different time points (0–24 h). Plasma was collected and analyzed for the administered drug or metabolites by analytical method as described earlier (ref. 60) with little modifications. Calibration curve of standard EA (an active metabolite of PGN and PLN) was drawn by using linear regression equation. Area under the curve (AUC) was plotted and concentration and time maxima of each compound were calculated.
Additional information
Financial Support Current work was supported by a grant from the Department of Biotechnology, India to SDand Science and Engineering Research Board, DST, India (grant SR/FT/LS-01/2011) to U.R. A.K was supported by a research fellowship from the Council of Scientific and Industrial Research, India. SD also acknowledges JC Bose fellowship from DST, India.
References
Boyer, N. & Marcellin, P. Pathogenesis, diagnosis and management of hepatitis C. J. Hepatol. 32, 98–112 (2000).
Horner, S. M. & Gale, M., Jr Regulation of hepatic innate immunity by hepatitis C virus. Nat. Med. 19, 879–888 (2013).
Guedj, J., Dahari, H., Pohl, R. T., Ferenci, P. & Perelson, A. S. Understanding silibinin's modes of action against HCV using viral kinetic modeling. J. Hepatol. 56, 1019–1024 (2012).
Trecul, A., Morceau, F., Dicato, M. & Diederich, M. Dietary compounds as potent inhibitors of signal transducers and activators of transcription (STAT) 3 regulatory network. Genes Nutr. 7, 111–125 (2012).
Nahmias, Y. et al. Apolipoprotein B-dependent hepatitis C virus secretion is inhibited by the grapefruit flavonoid naringenin. Hepatology 47, 1437–1445 (2008).
Takeshita, M. et al. Proanthocyanidin from blueberry leaves suppresses expression of subgenomic hepatitis C virus RNA. J. Biol. Chem. 284, 21165–21176 (2009).
Kim, K. et al. Curcumin inhibits hepatitis C virus replication via suppressing the Akt-SREBP-1 pathway. FEBS Lett. 584, 707–712 (2010).
Anggakusuma. et al. Turmeric curcumin inhibits entry of all hepatitis C virus genotypes into human liver cells. Gut. (2013).
Calland, N. et al. (-)-Epigallocatechin-3-gallate is a new inhibitor of hepatitis C virus entry. Hepatology 55, 720–729 (2012).
Lin, Y. T. et al. Green tea phenolic epicatechins inhibit hepatitis C virus replication via cycloxygenase-2 and attenuate virus- induced inflammation. PLoS One 8, e54466 (2013).
Gonzalez, O. et al. The heat shock protein inhibitor Quercetin attenuates hepatitis C virus production. Hepatology 50, 1756–1764 (2009).
Bachmetov, L. et al. Suppression of hepatitis C virus by the flavonoid quercetin is mediated by inhibition of NS3 protease activity. J. Viral Hepat. 19, e81–e88 (2012).
Jurenka, J. S. Therapeutic applications of pomegranate (Punica granatum L.): a review. Altern. Med. Rev. 13, 128–144 (2008).
Adams, L. S., Zhang, Y., Seeram, N. P., Heber, D. & Chen, S. Pomegranate ellagitannin-derived compounds exhibit antiproliferative and antiaromatase activity in breast cancer cells in vitro. Cancer Prev. Res. (Phila) 3, 108–113 (2010).
Neurath, A. R., Strick, N., Li, Y. Y. & Debnath, A. K. Punica granatum (Pomegrante) juice provides an HIV-1 entry inhibitor and candidate topical microbicide. BMC Infect. Dis. 4, 41 (2004).
Nonaka, G. et al. Anti-AIDS agents, 2: Inhibitory effects of tannins on HIV reverse transcriptase and HIV replication in H9 lymphocyte cells. J. Nat. Prod. 53, 587–595 (1990).
Sundararajan, A. et al. Influenza virus variation in susceptibility to inactivation by pomegranate polyphenols is determined by envelope glycoproteins. Antiviral Res. 88, 1–9 (2010).
Yang, Y., Xiu, J., Zhang, L., Qin, C. & Liu, J. Antiviral activity of punicalagin toward human enterovirus 71 in vitro and in vivo. Phytomedicine 20, 67–70 (2012).
Gil, M. I., Tomas-Barberan, F. A., Hess-Pierce, B., Holcroft, D. M. & Kader, A. A. Antioxidant activity of pomegranate juice and its relationship with phenolic composition and processing. J. Agric. Food Chem. 48, 4581–4589 (2000).
Malik, A. et al. Pomegranate fruit juice for chemoprevention and chemotherapy of prostate cancer. Proc. Natl. Acad. Sci. USA. 102, 14813–14818 (2005).
Thresiamma, K. C. & Kuttan, R. Inhibition of liver fibrosis by ellagic acid. Indian J. Physiol. Pharmacol. 40, 363–366 (1996).
Di Marco, S. et al. Inhibition of the hepatitis C virus NS3/4A protease. The crystal structures of two protease-inhibitor complexes. J. Biol. Chem. 275, 7152–7157 (2000).
Lin, C. (2006). HCV NS3-4A serine protease. In: Tan, S. L. editor. Hepatitis C viruses: Genomes and Molecular Biology. Norfolk (UK): Horizon Bioscience; 2006. Chapter 6. http://www.ncbi.nlm.nih.gov/books/NBK1623/.
Romano, K. P. et al. The molecular basis of drug resistance against hepatitis C virus NS3/4A protease inhibitors. PLoS Pathog. 8, e1002832 (2012).
Transue, T. R., Krahn, J. M., Gabel, S. A., DeRose, E. F. & London, R. E. X-ray and NMR characterization of covalent complexes of trypsin, borate and alcohols. Biochemistry. 43, 2829–2839 (2004).
Murzin, A. G., Brenner, S. E., Hubbard, T. & Chothia, C. SCOP: a structural classification of proteins database for the investigation of sequences and structures. J. Mol. Biol. 247, 536–540 (1995).
Zhang, Y. & Skolnick, J. TM-align: a protein structure alignment algorithm based on the TM-score. Nucleic Acids Res. 33, 2302–2309 (2005).
Frese, M. et al. Hepatitis C virus RNA replication is resistant to tumour necrosis factor-alpha. J. Gen. Virol. 84, 1253–1259 (2003).
Lanford, R. E., Sureau, C., Jacob, J. R., White, R. & Fuerst, T. R. Demonstration of in vitro infection of chimpanzee hepatocytes with hepatitis C virus using strand-specific RT/PCR. Virology 202, 606–614 (1994).
Craggs, J. K., Ball, J. K., Thomson, B. J., Irving, W. L. & Grabowska, A. M. Development of a strand-specific RT-PCR based assay to detect the replicative form of hepatitis C virus RNA. J. Virol. Methods 94, 111–120 (2001).
Kitazato, K., Wang, Y. & Kobayashi, N. Viral infectious disease and natural products with antiviral activity. Drug Discov. Ther. 1, 14–22 (2007).
Raney, K. D., Sharma, S. D., Moustafa, I. M. & Cameron, C. E. Hepatitis C virus non structural protein 3 (HCV NS3): a multifunctional antiviral target. J. Biol. Chem. 285, 22725–22731 (2010).
Romano, K. P. et al. Molecular mechanisms of viral and host cell substrate recognition by hepatitis C virus NS3/4A protease. J. Virol. 85, 6106–6116 (2011).
Haslam, E. Natural polyphenols (vegetable tannins) as drugs: possible modes of action. J. Nat. Prod. 59, 205–215 (1996).
Li, X., Zhang, W., Qiao, X. & Xu, X. Prediction of binding for a kind of non-peptic HCV NS3 serine protease inhibitors from plants by molecular docking and MM-PBSA method. Bioorg. Med. Chem. 15, 220–226 (2007).
Waris, G. & Siddiqui, A. Hepatitis C virus stimulates the expression of cyclooxygenase-2 via oxidative stress: role of prostaglandin E2 in RNA replication. J. Virol. 79, 9725–9734 (2005).
Leng, J., Han, C., Demetris, A. J., Michalopoulos, G. K. & Wu, T. Cyclooxygenase-2 promotes hepatocellular carcinoma cell growth through AKT activation: evidence for AKT inhibition in celecoxib-induced apoptosis. Hepatology 38, 756–768 (2003).
Cooray, S. The pivotal role of phosphotidylinositol 3-kinase-Akt signal transduction in virus survival. J. Gen. Virol. 85, 1065–1076 (2004).
Shukla, M., Gupta, K., Rasheed, Z., Khan, K. A. & Haqqi, T. M. Bioavailable constituents/metabolites of pomegranate (Punica granatum L) preferentially inhibit COX2 activity ex vivo and IL-1beta-induced PGE2 production in human chondrocytes in vitro. J. Inflamm. (Lond) 5, 9 (2008).
Lansky, E. P. et al. Possible synergistic prostate cancer suppression by anatomically discrete pomegranate fractions. Invest. New Drugs 23, 11–20 (2005).
Vanella, L. et al. Apoptotic markers in a prostate cancer cell line: effect of ellagic acid. Oncol. Rep. 30, 2804–2810 (2013).
Edderkaoui, M. et al. Ellagic acid induces apoptosis through inhibition of nuclear factor kappa B in pancreatic cancer cells. World J. Gastroenterol. 14, 3672–3680 (2008).
Mishra, S. & Vinayak, M. Anti-carcinogenic action of ellagic acid mediated via modulation of oxidative stress regulated genes in Dalton lymphoma bearing mice. Leuk. Lymphoma 52, 2155–2161 (2011).
Cerda, B., LIorach, R., Ceron, J. J., Espin, J. C. & Tomas- Barberan, F. A. Evaluation of the bioavailability and metabolism in the rat of punicalagin, anantioxidant polyphenol from pomegranate juice. Eur. J. Nutr. 42, 18–28 (2003).
Cerda, B., Ceron, J. J., Tomas-Barberan, F. A. & Espin, J. C. Repeated oral administration of high doses of the pomegranate ellagitannin punicalagin to rats for 37 days is not toxic. J. Agric. Food Chem. 51, 3493–3501 (2003).
Kato, T. et al. Cell culture and infection system for hepatitis C virus. Nat. Protoc. 1, 2334–2339 (2006).
Yi, M., Ma, Y., Yates, J. & Lemon, S. M. Compensatory mutations in E1, p7, NS2 and NS3 enhance yields of cell culture-infectious inter genotypic chimeric hepatitis C virus. J. Virol. 81, 629–638 (2007).
Berdichevsky, Y. et al. A novel high throughput screening assay for HCV NS3 serine protease inhibitors. J. Virol. Methods 107, 245–255 (2003).
Twining, S. S. Fluorescein isothiocyanate-labeled casein assay for proteaolytic enzymes. Anal. Biochem. 143, 30–34 (1984).
Bernstein, F. C. et al. The Protein Data Bank: a computer- based archival file for macromolecular structures. J. Mol. Biol. 112, 535–542 (1977).
Feng, Z. et al. Ligand Depot: a data warehouse for ligands bound to macromolecules. Bioinformatics 20, 2153–2155 (2004).
Sobolev, V., Sorokine, A., Prilusky, J., Abola, E. E. & Edelman, M. Automated analysis of interatomic contacts in proteins. Bioinformatics 15, 327–332 (1999).
Porter, C. T., Bartlett, G. J. & Thornton, J. M. The Catalytic Site Atlas: a resource of catalytic sites and residues identified in enzymes using structural data. Nucleic Acids Res. 32, D129–133 (2004).
Chen, C. Y. TCM Database@Taiwan: the world's largest traditional Chinese medicine database for drug screening in silico. PLoS One 6, e15939 (2011).
Morris, G. M. et al. AutoDock4 and AutoDockTools4: Automated docking with selective receptor flexibility. J. Comput. Chem. 30, 2785–2791 (2009).
The PyMOL Molecular Graphics System, Version 1.5.0.4 Schrodinger, LLC.
Ciofani, G., Danti, S., D'Alessandro, D., Moscato, S. & Menciassi, A. Assessing cytotoxicity of boron nitride nanotubes: Interference with MTT assay. Biochem. Biophys. Res. Commun. 394, 405–411 (2010).
OECD Guidelines for the testing of chemicals. OECD 423. Acute Oral Toxicity-Acute toxic class method. Organization for Economic Cooperation and Development, Paris (2001).
OECD. (2006). Report of the Validation of the Updated Test Guideline 407: Repeat Dose 28-day Oral Toxicity Study in Laboratory Rats. Series on Testing and Assessment No 59, ENV/JM/MONO(2006)26.
Haid, S. et al. A plant-derived flavonoid inhibits entry of all HCV genotypes into human hepatocytes. Gastroenterology 143, 213–222 (2012).
Acknowledgements
We are thankful to Drs. Itai Benhar, TakajiWakita, Stanley Lemon, Ralf Bartenschlager and Charles M. Rice for sharing plasmid constructs and cell lines. We thank Dr. K.N. Balaji for providing us useful reagent. We are also grateful to central animal facility, NMR and analytical spectroscopy facilities of IISc, Bangalore, India. Our lab members are acknowledged for helpful suggestions.
Author information
Authors and Affiliations
Contributions
U.R., R.M., A.K. and S.D. conceived and designed the study; U.R, A.K., R.M. and G.S. conducted experiments; U.R., R.M., A.K., G.S., N.S., S.D. analyzed data; U.R., R.M., A.K., G.S., N.S., S.D. wrote the paper.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Electronic supplementary material
Supplementary Information
Supplementary information
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License. The images or other third party material in this article are included in the article's Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder in order to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/4.0/
About this article
Cite this article
Reddy, B., Mullick, R., Kumar, A. et al. Small molecule inhibitors of HCV replication from Pomegranate. Sci Rep 4, 5411 (2014). https://doi.org/10.1038/srep05411
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep05411
This article is cited by
-
Punicalagin triggers ergosterol biosynthesis disruption and cell cycle arrest in Cryptococcus gattii and Candida albicans
Brazilian Journal of Microbiology (2020)
-
Oenothein B, dimeric hydrolysable tannin inhibiting HCV invasion from Oenothera erythrosepala
Journal of Natural Medicines (2019)
-
Cloning of mature pomegranate (Punica granatum) cv. Jalore seedless via in vitro shoot production and ex vitro rooting
Vegetos (2019)
-
A comprehensive overview of hepatoprotective natural compounds: mechanism of action and clinical perspectives
Archives of Toxicology (2016)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.