Abstract
Flavivirus-mediated inflammation causes neuronal death, but whether the infected neurons can evoke an innate immune response to elicit their own protection, is unknown. In an earlier study we have shown that neuronal RIG-I, play a significant role in inducing production and release of molecules that are related to inflammation. In this study, using a neuronal cell line, we show that RIG-I acts with STING in a concerted manner following its interaction with Japanese encephalitis viral RNA to induce a type 1 interferon response. Knock-down of STING showed that the expressions of various inflammatory signaling molecules were down-regulated along with increased intracellular viral load. Alternatively, over-expressing STING decreased intracellular viral load. Our results indicate that at the sub-cellular level, interaction between the pattern recognition receptor RIG-I and the adapter molecule STING, is a major contributor to elicit immunological responses involving the type 1 interferons in neurons following JEV infections.
Similar content being viewed by others
Introduction
Pattern recognition receptors (PRRs) are important effectors in the activation of the innate immune responses that recognizes microbial components including nucleic acids1. These effectors act by triggering signaling cascades, that ultimately leads to the production of proinflammatory cyto/chemokines, type-I interferons (IFNs), corresponding interferon-stimulated genes (ISGs) and activates other key regulators of innate immunity, such as nuclear factor-kappa-B (NF-κB)2. Toll-like receptors (TLRs) and retinoic acid-inducible gene I (RIG-I)-like receptors (RLRs), are two of the four major PRRs known to recognize pathogen components and directly activate immune cells.
RIG-I and melanoma differentiation-associated gene 5 (MDA5), are two cytoplasmic helicases belonging to the RLR family that senses viral RNA3. Studies on RIG-I-deficient mice have revealed that RIG-I is essential for the recognition of ssRNA viruses, such as flaviviruses, paramyxoviruses, orthomyxoviruses and rhabdoviruses, whereas MDA5 is required for recognition of a different set of RNA viruses that includes Picornaviruses4,5. Both possess two caspase recruitment domains that are required for interaction with the mitochondrial adaptor molecule called mitochondrial antiviral signaling or MAVS (also known as IPS-1, Cardif or VISA)6. This interaction leads to the activation of two cytosolic protein kinase complexes- one consisting of the ‘non-canonical’ initiation κB kinase (IKK)-related TANK binding kinase 1 (TBK1) or IKK-i associated with various adaptor proteins and the other containing IKKα, IKKβ and NF-κB essential modulator7. The TBK1 complex leads to phosphorylation of transcription factors interferon regulatory factor (IRF) 3 and IRF7 to induce the expression of type I interferons (IFNs). The IKK complex activates NF-κB that initiates expression of proinflammatory cytokines after translocating into the nucleus.
Apart from immune cells, ‘non-professional cells’ such as neurons are known to possess active cytoplasmic and endoplasmic PRRs that have multiple physiologic functions which include mounting of innate immune reactions in response to pathogen associated molecular patterns8. Following viral infections in the central nervous system (CNS), neuronal PRRs have been shown to act as the sensors that elicit an innate immune reaction9. Human neurons have been reported to mount both type-1 interferon and pro-inflammatory responses against rabies virus and herpes simplex type 1 virus infection through TLR-310; similar effects were also observed after treatment of human neurons with dsRNA, a molecular signature of virus infection11.
Flaviviruses infecting the CNS are known to trigger inflammation and cause neuronal death12,13. This is mediated in part by direct virus-induced apoptosis/necrosis or by a ‘bystander’ mechanism resulting from the inflammatory milieu. The brain has for long been referred to as an ‘immune privileged’ organ as it was believed to be out of the radar of the peripheral immune system. However, this notion has been challenged radically over the past decade or so. Among the components of the CNS, the glial cells has been known to respond to pathogenic or any foreign insults by releasing various factors that tend to cause inflammation14. The neurons on the other hand were believed to be more-or-less the victims of this chemical warfare; but as reports suggest, innate immune responses are also mounted in these cells during viral encephalitis15,16. In our earlier study, we have reported that Japanese encephalitis virus (JEV), a flavivirus with single stranded RNA, is recognized by neuronal RIG-I that leads to production and release of proinflammatory factors17. However, the exact mechanisms by which neurons are able to do so, remained unknown.
An endoplasmic reticulum transmembrane protein called Stimulator of Interferon Gene (STING) (or less commonly known as MPYS, ERIS or TMEM173 or MITA) was discovered to function downstream of MAVS in the RLR pathway18,19. This protein is also found on the outer membrane of the mitochondria. Experiments on human endothelial kidney cell lines have shown that STING plays a critical role in production of type-1 interferon via activation of interferon responsive element (IRF) 3 and NFκB. STING−/− animals were also found to be more susceptible to vesicular stomatitis virus infection which is indicative of impaired immunity20. The innate immune signaling via STING has been reported to be STAT6 dependent21.
Till date, all studies regarding STING have been limited to embryonic cells or cells of the immune or myeloid lineage. There is absolutely no report available about the expression or role of this molecule in CNS cell types, let alone neurons. In this study we are aim to elucidate the role played by neuronal STING following flaviviral encephalitis, utilizing JEV as the model virus.
Results
JEV causes upregulation of STING both in vivo and in vitro
Immunohistochemical analysis of brain sections from JEV-infected animals showed marked upregulation in the expression of STING, concomitant with severe neuronal loss. However, viral inhibition by application of 3′MO resulted in STING expression that was comparable to that observed in mock-infected animal brains ( Fig. 1 ). Immunoblotting from N2a post 6 h and 12 h of infection showed significant increase in STING levels (p<0.01), when compared to respective time-matched mock-infected cells. However, there was no significant difference in STING levels between mock-infected and JEV-infected groups 24 h post infection ( Fig. 2A–B ).
Expression of STING in brain following JEV infection.
Immunohistochemical staining from brain sections of JEV-infected mice showing increased expression of STING (Green) along with severe loss of neurons as depicted by less NeuN staining (Red). Following viral inhibition using 3′MO there was no loss of neurons and also no visibly different STING expression than that observed in mock-infected animals. Magnification ×20; scale bar is 50 µ; images are representative of 3 animals in each group.
Temporal changes in the expression of STING and proinflammatory mediators following JEV infection in neurons.
(A) Immunoblots showing STING, Cox-2, phosphoNFκB and phosphoP38MAPK expressions after 6, 12 and 24 h post infection. (B–E) Graphs representing densitometric quantification of fold change of protein bands of STING, Cox-2, phosphoNFκB and phosphoP38MAPK in JEV-infected cells over respective time matched mock-infected controls, normalized to β-actin. Data is represented as Mean ± S.D. from 3 independent experiments. *, significantly more than mock-infected, p<0.01.
Modulation in Cox-2, NFκB and p38MAPK levels following JEV infection
JEV-infection is known to cause upregulation of classical pro-inflammatory signaling molecules like p38MAPK NFκB and COX-2, both in-vivo and in-vitro. Here we found that the change in the increased levels of Cox-2, phosphoP38MAPK and phosphoNFκB was that of gradual decrease from 6 h onwards till 24 h post infection when compared to respective time-matched controls ( Fig. 2A & C–E ) (p<0.01).
JEV infection causes upregulation of IRF-3 and IRF-7 leading to type-I interferon response in neurons
Type-I interferon response is a hallmark of most viral infections. In most instances this is mediated by activation of IRF3 and 7 which regulates the IFN-α/β gene expressions. Following JEV-infection of N2a, we found significant upregulation in the levels of phosphoIRF3 both 6 h and 12 h post-infection (p<0.01), however its level at 12 h was lesser than 6 h post-infection, when compared to mock-infected cells. 24 h post infection phosphoIRF3 level showed no significant changes when compared to that from time matched mock-infected cells ( Fig. 3A & B ). Similarly level of phosphoIRF7 after 6 h post-infection showed significant increase when compared to mock-infected cells (p<0.01); but its levels were not found to be significantly different from mock-infected cells, post 12 h and 24 h of infection ( Fig. 3A & C ).
Temporal changes in the expression of type 1 interferons and interferon stimulated genes following JEV infection in neurons.
(A) Immunoblot analysis of interferon regulatory transcription factors (IRF) 3 and 7 and interferon-stimulated genes (ISG) 54 and 56 following JEV infection for different time points. (B–E) Graphs representing densitometric quantification of fold changes of proteins bands of phosphoIRF 3 & 7 and ISG 54 & 56 in JEV-infected cells over respective time matched mock-infected controls, normalized to β-actin. Data is represented as Mean ± S.D. from 3 independent experiments. *, significantly more than mock-infected, p<0.01. F, cDNA prepared from RNA extracted from mock-infected and JEV-infected cells at different time points was subjected to qRT-PCR for interferon(IFN)-α and β mRNA. Graph represents fold change of relative expression of IFN-α and β in JEV-infected cells over mock-infected after normalization with 18s rRNA internal controls. Data is represented as Mean ± S.D. from 2 independent experiments. *, significantly more than mock-infected, p<0.05.
ISG56 and ISG54 are two of the first identified proteins that are induced by type I IFNs, dsRNAs and viruses22. Immunoblot analysis of N2a infected with JEV, showed significant increases in the levels of both ISG54 and ISG56 when compared to mock-infected cells both 6 h and 12 h post infection (p<0.01), however their levels in 24 h post infected cells were not found to be different from respective mock-infected cells ( Fig. 3A, D & E ).
A similar trend was observed in the production of type I interferons following JEV infection. Quantitative real time PCR analysis from N2a revealed upsurge in levels of both IFN-α and IFN-β post 6 h and 12 h infections when compared to respective time-matched mock-infected cells (p<0.05). However, their levels post 24 h of infection showed increases, but it was only significant for IFN-α (p<0.05) when compared to mock-infected cells ( Fig. 3F ).
RIG-I detects JEV RNA and interacts with STING-IPS-1
RNA Co-IP carried out from N2a 12 h post infection with JEV revealed that viral genomic RNA interacts with RIG-I, while that with non-specific rabbit IgG showed no such interaction, confirming the RNA to be specific for RIG-I. Absence of the band specific to JEV-RNA in reaction without RT confirmed amplification is from JEV-RNA and not from any DNA contamination ( Fig. 4A ). Protein-protein CoIP carried out from cell lysates 12 h post infection showed interaction of RIG-I with STING ( Fig. 4B ) and IPS-1 with STING ( Fig. 4C ) which was found to be absent in mock-infected cells. Immunoprecipitation with non specific rabbit IgG showed no band specific for STING in either case. This interaction between RIG-I and STING was also confirmed by immunocytochemistry from N2a, post JEV infection ( Fig. 4D ).
Viral RNA interacts with RIG-I that in turn interacts with STING and IPS-1.
(A) Interactions between RIG-I and viral protein was observed by RT-PCR with RNA obtained from JEV-infected cell extracts by the method as described under experimental procedures. Viral mRNA band was visualized only in the sample which was conjugated with anti-RIG-I antibody. Image is representative of 3 independent experiments. (B–C) STING - RIG-I and STING - IPS-1 interactions following JEV infection were observed by CoIP. Protein extracts from mock-infected and JEV-infected cells were allowed to form complexes with incubated anti-RIG-I or anti-IPS-1 antibodies. The protein-antibody complexes were eluted followed by detection for STING by immunoblotting. The shown immunoblots are representative of 3 independent experiments. (D) Mock-infected and JEV-infected cells were double stained for STING and RIG-I. Merged images show clear STING and RIG-I interactions (yellow), marked by arrowheads. Un-merged images of the cell (inset) shows STING (green) and RIG-I (red) expressions, separately. Magnification ×40; scale bar is 25 µ; images are representative of 3 independent experiments.
STING ablation resulted in reduction of proinflammatory mediators following JEV-infection
JEV infection of N2a resulted in significantly increased STING expression which was found to be at basal levels in mock-infected cells (p<0.01). This was significantly inhibited (about 51%) using antisense morpholino specific for STING (STING-MO) (p<0.01). The levels of Cox-2, phosphoNFκB and phosphoP38MAPK also showed significant reduction after inhibition of STING when compared to only JEV-infected or JEV+Sc-MO group (p<0.01) ( Fig. 5A & B ). Luciferase assay done to confirm the reduced expression of COX-2 following STING knock-down showed significantly decreased transcription of COX-2 gene when compared to only JEV-infected or JEV+Sc-MO group (p<0.01) ( Fig. 5C ).
Effect of STING knock-down on proinflammatory mediators following JEV infection.
(A) Immunoblot analysis showing modulation of proinflammatory mediators following STING-MO and Sc-MO treatment. (B) Graph representing densitometric quantification of fold change of protein bands of STING, Cox-2, phosphoNFκB and phosphoP38MAPK, normalized to β-actin. Data is represented as Mean ± S.D. from 3 independent experiments. #, significantly less than JEV-infected, p<0.01. (C) Luciferase assay was done to detect change in Cox-2 expression in cells following JEV infection or after STING knock-down. Data is represented as Mean ± S.D. from 3 independent experiments. *, significantly more than mock-infected, p<0.01; #, significantly less than JEV-infected, p<0.01. (D–G) Bead array performed for the detection of released cyto/chemokines (IL-12p70, MCP-1, TNF-α and IL-6, respectively) from culture supernatants of mock-infected, JEV-infected, JEV+ STING-MO and JEV+Sc-MO groups.
The release of proinflammatory cyto/chemokines viz. IL-12, MCP-1 (CCL2), TNF-α and IL-6, were found to be significantly elevated in both JEV-infected (12 h) and JEV+Sc-MO groups when compared to that from mock-infected cells (p<0.01). However, ablation of STING resulted in significant reduction in their levels when compared to only JEV-infected or JEV+Sc-MO group (p<0.01) ( Fig. 5D–G ).
Knocking down STING resulted in altered type 1 interferon responses following JEV infection
STING ablation resulted in significant reductions in phosphoIRF3 and phosphoIRF7 levels as well as ISG54 and ISG56 levels, when compared to only JEV-infected or JEV+Sc-MO group (p<0.01) ( Fig. 6A & B ). Semi-quantitative RT-PCR for IFN-α and β showed visibly increased expression of these interferons in N2a following JEV infection. Also, ablation of STING results in marked decrease of their expression ( Fig. 6C ). Quantitative real time PCR analysis carried out to access the levels of IFN-α and β after STING ablation revealed significant reductions in their levels when compared to only JEV-infected or JEV+Sc-MO group (p<0.01) ( Fig. 6D & E ).
Effect of STING knock-down on type 1 interferon response following JEV infection.
(A) Immunoblot analysis of IRF3 & 7 and ISG 54 & 56 following STING-MO and Sc-MO treatment in JEV-infected cells. (B) Graph representing densitometric quantification of fold change of protein bands of IRF 3, IRF 7, ISG 54 and ISG 56, normalized to β-actin. Data is represented as Mean ± S.D. from 3 independent experiments. *, significantly more than mock-infected, p<0.01; #, significantly less than JEV-infected, p<0.01. (C) Semi-quantitative RT-PCR analysis showed marked decrease in the expression of IFN-α and β following STING knock-down after JEV infection. (D–E) Graphs showing qRT-PCR results done from RNA extracted from STING-MO and Sc-MO treated cells post JEV-infection represented as fold change over JEV-infected, after normalization to 18S rRNA internal control. Data is represented as Mean ± S.D. from 2 independent experiments. #, significantly less than JEV-infected, p<0.01.
Intracellular viral load is affected by modulating STING expression following JEV infection
Viral NS5 protein was found to be expressed at a significantly elevated level in cells that were treated with STING-MO as compared to only JEV-infected cells (p<0.05) ( Fig. 7A–B ), whereas over-expressing STING resulted in its significant decrease than JEV-infected group (p<0.05) ( Fig. 8G–H ). Treatment of N2a either with Sc-Mo or lipofectamine did not show significant alterations in NS5 levels when compared to only JEV-infected group ( Fig. 7A–B & 8G–H ).
Effect of STING knock-down on intracellular viral load.
(A) Immunoblot analysis for JEV NS5 following STING knock-down. (B) Graph representing densitometric quantification of fold change of protein band of JEV NS5 in STING-MO or Sc-MO treated cells that were infected with JEV over only JEV-infected cells, normalized to β-actin. Data is represented as Mean ± S.D. from 3 independent experiments. *, significantly higher than JEV-infected, p<0.05. (C) Cells were stained for Nakayama antigen and analyzed in a FACS Calibur. The representative data from 3 independent experiments are shown in the histogram; the mean fluorescence intensities of each group are mentioned within third brackets [ ]. (D) qRT-PCR was done with RNA extracted from mock-infected, JEV-infected, JEV+STING-MO and JEV+Sc-MO groups. Graph represents fold change of relative expression of JEV (GP78) mRNA in STING-MO and Sc-MO treated JEV-infected cells over only JEV-infected cells, after normalization with 18 s rRNA internal controls. Data is represented as Mean ± S.D. from 2 independent experiments.*, significantly higher than JEV-infected, p<0.05.
Effect of STING over-expression on intracellular viral load.
(A) Green fluorescence observed from N2a that were successfully transfected with vector containing GFP-tagged STING ORF (pCMV6-AC-GFP). Magnification ×20; scale bar is 50 µ. (B–D) Cells that were mock-infected, JEV-infected or transfected with different concentrations of pCMV6-AC-GFP (4 µg, 6 µg and 8 µg) and infected with JEV, were stained for JEV Nakayama antigen, analyzed using the BD FACS Calibur system and plotted as histograms. (E) The mean fluorescence intensity (MFI) in each of the different conditions were estimated and represented graphically as the averaged MFI for each condition. Data is represented as Mean ± S.D. from 3 independent experiments. #, significantly lesser than only JEV-infected, p<0.01. (F) RNA was extracted from mock-infected cells, JEV-infected cells and cells that were transfected either with pCMV6-AC-GFP (8 µg) or the empty vector and infected with JEV and was converted to cDNA. These were then subjected to qRT-PCR for JEV (GP78) mRNA. Graph represents fold change of relative expression of JEV (GP78) mRNA in STING over-expressed or empty vector transfected, JEV-infected cells over only JEV-infected cells, after normalization with 18 s rRNA internal controls. Data is represented as Mean ± S.D. from 2 independent experiments. #, significantly lesser than JEV-infected, p<0.05. (G) Immunoblot analysis for JEV NS5 following STING over-expression. (H) Graph representing densitometric quantification of fold change of protein band of JEV NS5 in STING over-expressed or empty vector transfected, JEV-infected cells over only JEV-infected cells, normalized to β-actin. Data is represented as Mean ± S.D. from 3 independent experiments. #, significantly lesser than JEV-infected, p<0.05.
Flow cytometric analysis after intracellular staining revealed that following knock-down of STING, there was a significant increase in the presence of viral antigens in the cells, than that observed from only JEV-infected cells or JEV+Sc-MO cells ( Fig. 7C ). On over-expressing STING with different plasmid concentrations (4, 6 and 8 µg), a sequential decreases in viral antigen levels were observed. (p<0.01). The viral load in JEV+only lipofectamine cells did not significantly differ from only JEV-infected cells ( Fig.8B–E ).
Quantitative real time PCR analysis was performed to assess the levels of viral RNA using primers specific for GP78 strain of JEV. It was found that after STING knock-down, amount of viral RNA was almost doubled when compared to only JEV-infected group (p<0.05), however in N2a treated with Sc-MO viral RNA was not found to be significantly altered ( Fig. 7D ). Significant reduction was observed in viral RNA levels from cells in which STING was over-expressed when compared to only JEV-infected group (p<0.05) ( Fig. 8F ).
Discussion
Encephalitis due to zoonotic flaviviral infections are a cause of major concern with frequent reports of epidemics from different regions of the globe23. From a global perspective, JEV is the most dreaded simply due to the huge number of populace living under the endemic regions. Apart from JEV, West Nile virus and Dengue virus infections are the most common causes of flaviviral epidemics. A common feature of neurotropic flaviviral infection is generation of inflammation in the CNS that is mediated mostly by glial activation and peripheral immune cell infiltration through a damaged and permeable blood brain barrier. The inflammation serves as a ‘double-edged sword’- on one hand it is necessary to counter the pathogen insult while on the other hand it is detrimental for neurons which, incidentally in adult CNS, are post-mitotic. This is indicative of the fact that survivors of flaviviral infections suffer from varying degrees of cognitive impairment due to permanent loss of neurons.
Even though the eukaryotic nervous system is known to closely co-ordinate with immune functions, neurons themselves were classically believed to be non-immunogenic. However, recent studies are producing results which indicate that following pathogenic (or antigenic) challenge, neurons activate responses that coordinate defense against the insult and facilitate antigen clearance. It has been shown that neurons possess functional PRRs8 which are necessary for pathogen detection and activation of a protein signaling cascade that ultimately leads to the generation of immune (innate) responses.
The RNA helicase RIG-I has been recently shown by us to be involved in mediation of proinflammatory responses in neurons following JEV infection17. The current study, using JEV as a model flavivirus, reports for the first time that neurons also express the endoplasmic reticular adapter molecule STING, a known interferon stimulator, which is involved in the induction of the neuronal innate immune response. Earlier studies involving viral infections have indicated the involvement of STING as a DNA sensor that led to production of interferons24,25,26 in different cell types, other than neurons. However, to the best of our knowledge, there are no reports available till date regarding the role of STING following flaviviral (RNA viruses) infections in any cell type, let alone neurons.
Immunohistochemical studies showed that STING is expressed in brain following JEV infection and also in neuronal cell lines. Interestingly, it was observed that in un-infected brain there was no STING expression, that corroborated with earlier study18, but in cultured mock-infected neuronal cells a basal expression was visible. From a time kinetic study, it was observed that STING expression was at its peak following 12 h of JEV infection, but showed gradual decline after 24 h. This also correlated with the expression of mediators such as p38MAPK, NFκB and Cox-2 and interferon stimulators such as IRF3 and 7 which prompted us to carry out subsequent studies when STING expression was at its peak. RNA-protein co-immunoprecipitation showed that there was indeed a RIG-I - viral RNA interaction that corroborates our earlier findings. Also, using protein-protein co-immunoprecipitation and immunocytochemistry it was showed that RIG-I interacts with STING in neuronal cells following JEV infection, which is a novel finding. STING-mediated interferon responses following viral (HCMV) infection has been reported to be IPS-1- independent25. However, we observed a STING - IPS-1 interaction following JEV infection in neuronal cells. The expression levels of NFκB and IRF3 and & 7 were also elevated post JEV infection which coincided with elevated IFN-α and β levels.
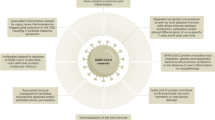
Taken together, the data indicates that the viral RNA - RIG-I complex recruits STING and IPS-1 to initiate a downstream cascade leading to the activation of the transcription factors NF-κB and IRF3, which bind to and activate the IFN promoter following nuclear translocation. Secreted IFN, binds to the type I IFN receptor (IFNAR) in an autocrine or paracrine fashion leading to activation of the JAK/STAT pathway that initiates the production of numerous IFN-inducible genes (ISGs)26. Both ISG54 and ISG56 levels were found to be elevated following JEV infection. ISG54 has been reported to be an apoptosis inducer27 while ISG56 acts as a negative feedback regulator of anti-viral interferon signaling. Specifically, ISG56 inhibits STING - IPS-1 interactions thereby preventing type 1 interferon production28.
When STING was knocked down using morpholino oligonucleotides, the IRF3 and 7 expressions were found to be significantly decreased which could be the cause of lesser induction of IFN-α and β genes. Also positively correlated to this observation was the decrease in the levels of ISG54 and 56. Hence it seems that in low STING-expressing cells, interferon responses were ablated. As a direct response to this, it was observed that in those cells the anti-viral efficacy of interferons was lacking. IFN-α is a known JEV antagonist, but on STING knock-down an increased intracellular viral load was observed. On the contrary, when STING was over-expressed, it had an antagonistic effect on the viral load.
The intracellular inflammatory mediator levels also showed modulations following STING knock-down or over-expression. As discussed above, NFκB lies downstream to STING in the signaling cascade that is activated following viral infection. NFκB is also involved in the synthesis of proinflammatory cyto/chemokines. As STING gets knocked down, NFκB expression is also decreased and concomitantly the secretions of certain proinflammatory cyto/chemokines are reduced. Expression of Cox-2, an enzyme related with synthesis of proinflammatory prostanoids, is also decreased following STING knock-down, which could be attributed to decreased IFN-α production as it is a reported antagonist29.
Our results adds to the existing knowledge and helps to chart a complete pathway regarding the mechanism by which innate immune facet of eukaryotic cells respond to flaviviral infection. This study provides conclusive evidence of an active flaviviral recognition mechanism involving the RIG-I – STING pathway in neurons. Also, the involvement of STING in the generation of an innate immune response against flaviviral infections has been indicated for the first time. There could be many implications of this study. Specifically, since it is now clear that neurons do evoke an immune response, their role in flaviviral (or any other neurotropic viral) infections needs to be studied in more detail. Also, there is a tremendous potential for the exploitation of the anti-viral actions of interferons or related genes by modulating the RIG-I – STING pathway. Finally, our study is beneficial in dissipating the age-old belief that glia are the only cell type in the CNS that are capable of contributing to immune responses.
Methods
Ethics statement
All animal experiments were approved by the Institutional Animal and Ethics Committee of the National Brain Research Centre (approval no. NBRC/IAEC/2007/36 and NBRC/IAEC/2011/66). The animals were handled in strict accordance with good animal practice as defined by the Committee for the Purpose of Control and Supervision of Experiments on Animals, Ministry of Environment and Forestry, Government of India.
Virus and cells
JEV (GP78 strain) was propagated in suckling BALB/c mice as described earlier30. Mouse neuroblastoma Neuro2a (N2a) cells were grown at 37°C in Dulbecco's modified Eagle medium (DMEM) supplemented with 3.7% sodium bi-carbonate, 10% fetal bovine serum and penicillin/streptomycin.
Animal treatment
3–4 weeks old BALB/c mice were randomly distributed into 3 groups- Mock-infected, JEV-infected and JEV-infected and treated with Vivo-morpholino (Gene Tools LLC, OR, USA) against 3′-conserved region of the viral genome (JEV+3′MO) and treated according to previously published protocol30. JEV-infected animals succumbed by 8th–9th day post infection. Animals of mock-infected and JEV + 3′MO groups were also sacrificed at same time point. Brains were excised after repeated transcardial perfusion with ice-cold 1× PBS and were processed for immunohistochemical staining.
Immunohistochemistry
To demonstrate STING expression, 10µ thick cryosections of brains from animals of different treatment groups were subjected to antigen retrieval at 70°C using antigen unmasking solution (Vector Laboratories Inc., CA, USA) followed by extensive washes with 1× PBS (pH 7.4). Sections were then blocked with 5% goat serum for 1½ h followed by overnight incubation with primary antibodies against STING (Sigma, USA; 1:200) and the neuronal marker NeuN (Chemicon, CA, USA; 1:250) in a humidified chamber at 4°C. On the next day, the sections were washed with 1× PBS followed by 1 h incubation at room temperature (r.t.) with fluorochrome-conjugated secondary antibodies. The sections were then washed extensively with 1× PBS, mounted with 4′-6-diamidino-2-phenylindole (DAPI, Vector Laboratories Inc, CA, USA) and observed under a Zeiss Axioplan 2 Fluorescence microscope31.
Infection and treatment schedule of Neuro2a
N2a were cultured in serum containing media till 70–80% confluency followed by differentiation in serum-free media. Cells were then either mock-infected or infected with JEV at multiplicity of infection (MOI) of 5 for 1½ h. Post infection, cells were washed thrice with sterile 1× PBS to remove non-internalized virus and were incubated for different time periods in serum free media.
STING over-expression and knock-down
To study the effect of STING over-expression on viral load, N2a were grown in six 90 mm culture plates. Three out of six plates were transfected with different amounts (4 µg, 6 µg and 8 µg) of mouse STING GFP-tagged open reading frame (ORF) clone commercially procured from OriGene, (MD, USA) using Lipofectamine 2000TM (Invitrogen CA, USA). The vector used for cloning and over-expression of GFP-tagged 1137 b.p. STING ORF (NCBI Reference Sequence: NM_028261.1) was pCMV-6-AC-GFP. The ORF was inserted between SgfI-MluI restriction sites in the multiple cloning site of the vector. After 24 h of transfection, these three plates, along with two others were infected with JEV as described above and kept for 12 h. One remaining plate was mock-infected. One JEV-infected plate was only treated with the empty vector, which served as reagent control.
To knock-down STING, cells were transfected with morpholino directed against STING (STING-MO; 5′ CCA ACA GCG TCT ACG AGA 3′) at 10 μM concentration along with specialized delivery moiety (endoporter) and incubated for 2 h at 37°C. Post incubation, cells were infected with JEV as described above and were then re-incubated with fresh morpholino-containing media for 12 h17. Mock-infected cells without morpholino treatments served as control, only JEV-infected cells without morpholino treatment served as positive control. A negative control was used where cells were infected with JEV but treated with a scrambled morpholino (Sc-MO; 5′ GAT AAT TCT GGT TTT AAA TTC 3′) along with the endoporter, also at 10 μM concentration. The STING-MO sequence was screened with BLAST (www.ncbi.nlm.nih.gov/BLAST/) against primate and murine mRNA sequences and the Sc-MO was additionally screened against all flaviviral sequences. Both morpholinos and endoporter were procured from Gene Tools LLC, (Philomath, OR, USA).
Immunoblotting
Cells were lysed and subjected to western blot analysis to study modulation in expression of cellular proteins, using primary antibodies against STING (Sigma, St. Louis, USA), Cox-2 (Chemicon, CA, USA), phosphoNFκB, phosphoP38MAP kinase, phosphoIRF3, phosphoIRF7 (Cell Signalling, CA, USA), ISG54 and ISG56 (Pierce, USA) and JEV NS5 (a kind gift from Dr. Chun-Jung Chen, Taichung Veterans General Hospital, Taichung, Taiwan), at 1:1000 dilutions. After extensive washes with 0.1% PBS–Tween, blots were incubated with appropriate peroxidase-conjugated secondary antibodies (Vector Laboratories, CA, USA). The blots were processed for development using chemiluminescence reagent (Millipore, CA, USA). The images were captured and analyzed using Chemigenius, Bioimaging System (Syngene, Cambridge, UK). To determine equivalent loading of samples the blots were stripped and reprobed with anti-β-actin (Sigma, St. Louis, USA).
Immunocytochemistry
N2a were cultured in 4-well chamber slides and were either mock-infected or infected with JEV as described above. 12 h post infection, the cells were fixed with 4% paraformaldehyde for 20 min followed washings with 1× PBS and then blocked with 5% goat serum in 0.01% Triton X-100-PBS. Post blocking cells were incubated overnight at 4°C with primary antibodies against STING and RIG-I (1:250; Sigma, St. Louis, USA). On the next day, the cells were washed and incubated with appropriate fluorochrome-conjugated secondary antibodies. After final washes cells were mounted with DAPI, (Vector laboratories Inc., CA, USA). The slides were observed under a Zeiss Axioplan 2 Fluorescence microscope17.
Semi-quantitative RT-PCR and Quantitative Real Time-PCR
Quantitative PCR analysis of each transcript was performed using primers specific for mouse; IFN-α (forward 5′ ATT GGC TAG GCT CTG TGC TTT 3′; reverse 5′ AGG GCT CTC CAG ACT TCT GC 3′), IFN-β (forward 5′ TTG CCA TCC AAG AGA TGC TC 3′; reverse 5′ TCA GAA ACA CTG TCT GCT GG 3′) and JEV (GP78) (forward 5′ TTG ACA ATC ATG GCA AAC G 3′; reverse 5′ CCC AAC TTG CGC TGA ATA A 3′) were used. 500 ng of cDNA was used as a template for performing qRT-PCR using SYBR Green Supermix (Bio-Rad, CA, USA) on ABI Prism 7500 sequence detection system (Applied Biosystems, CA, USA). The real time PCR results were analyzed using the iCycler Thermal Cycler Software (Applied Biosystems, CA, USA) and normalized with those from 18S rRNA internal control32.
Semi quatitative reverse transcriptase-PCR (RT-PCR) was performed using the onestep RT-PCR kit (Qiagen Biosciences; Hamburg, Germany) following the manufacturer's protocol and reactions were carried out on Applied biosystems Veriti 96 well thermal cycler. One microgram of the total RNA was used as template in 25 μl PCR reactions, containing 5× PCR buffer (5 μl), dNTPs (1 μl), enzyme mix (1 μl) and specific forward and reverse primers (5 μM) and RNase free water. The PCR products were separated on 2% agarose gel, stained with ethidium bromide and photographed using UVP Bioimaging system.
Viral intracellular staining
N2a were grown in 60 mm culture plates and were infected and treated as described above. Post infection and/or treatment, cells were collected by washing with chilled sterile 1× PBS. Cells were stained for JEV antigen by protocol described earlier30. The percentage of population of JEV-positive cells was calculated after gating the populations on a Dot plot using Cell Quest Pro Software (BD Biosciences, CA, USA).
Cytokine bead array
Mouse cytokine bead array (CBA) kit (BD Biosciences, CA, USA) was used as per manufacturers' instructions to quantitatively measure proinflammatory cyto/chemokine levels from cell culture supernatants from all treatment groups. Data were acquired using Cell Quest Pro Software in FACS Calibur and analyzed using BD CBA software (Becton Dickinson, San Diego, CA, USA)17.
Luciferase assay
Luciferase reporter gene construct pCOX301 (a kind gift from Dr. Manikuntala Kundu, Bose Institute, Kolkata, India)33 was used to study Cox-2 expression following JEV infection along with or without STING knock-down. Cells were treated with either STING-MO or Sc-MO, for 2 h before adding 1 μg of the plasmid along with 5 μL of lipofectamine 2,000 (Invitrogen, CA, USA) in Opti-MEM for 6 h. The cells were then maintained for 24 h in 5% DMEM before they were infected with JEV as described above and kept for 12 h.
Luciferase assay was done using kit (Promega, WI, USA) according to manufacturer's instructions. Reading was taken using Sirius single tube luminometer (Berthold detection systems GmBH, Germany). The luciferase units were measured as Relative Luciferase Units (RLU) and these values were normalized to protein content of samples.
RNA Co-immunoprecipitation (RNA-CoIP)
Interaction between JEV RNA and RIG-I was assayed by the method described by Riranjanakumari et al34 with slight modifications. The RNA isolated from all samples was subjected to RT-PCR for analysis. Reverse transcription reactions without reverse transcriptase (-RT) served as a control.
Co-immunoprecipitation (CoIP)
To ascertain STING-RIG-I and STING-IPS-1 interactions, co-immunoprecipitation was carried out using cell lysates containing 500 µg proteins from mock-infected and JEV-infected cells by methods described elsewhere35. Anti-RIG-I or anti-IPS-1 antibody (Sigma, St Louis, USA) were used to pull-down the immunocomplex. For detection of interaction with STING, the blots were probed with anti-STING antibody (Sigma, St. Louis, USA) followed by chemiluminescent detection as described above.
Statistical analysis
Values were calculated as the mean ± S.D. of n number of independent experiments (each n from different cell preparations). Differences between mock-infected/control and experimental samples for the accumulated data were evaluated using one-tailed Student's t test. Statistical significance was set at p <0.05 for all analyses.
References
Lee, M. S. & Kim, Y. J. Pattern-recognition receptor signaling initiated from extracellular, membrane and cytoplasmic space. Mol Cells 23, 1–10 (2007).
Saitoh, T. & Akira, S. Regulation of innate immune responses by autophagy-related proteins. J Cell Biol 189, 925–935 (2010).
Yoneyama, M. & Fujita, T. Structural mechanism of RNA recognition by the RIG-I-like receptors. Immunity 29, 178–181 (2008).
Kato, H. et al. Differential roles of MDA5 and RIG-I helicases in the recognition of RNA viruses. Nature 441, 101–105 (2006).
Gitlin, L. et al. Essential role of mda-5 in type I IFN responses to polyriboinosinic:polyribocytidylic acid and encephalomyocarditis picornavirus. Proc Natl Acad Sci U S A 103, 8459–8464 (2006).
Kawai, T. et al. IPS-1, an adaptor triggering RIG-I- and Mda5-mediated type I interferon induction. Nat Immunol 6, 981–988 (2005).
Akira, S., Uematsu, S. & Takeuchi, O. Pathogen recognition and innate immunity. Cell 124, 783–801 (2006).
Peltier, D. C., Simms, A., Farmer, J. R. & Miller, D. J. Human neuronal cells possess functional cytoplasmic and TLR-mediated innate immune pathways influenced by phosphatidylinositol-3 kinase signaling. J Immunol 184, 7010–7021 (2010).
Peterson, K. E. & Du, M. Innate immunity in the pathogenesis of polytropic retrovirus infection in the central nervous system. Immunol Res 43, 149–159 (2009).
Prehaud, C., Megret, F., Lafage, M. & Lafon, M. Virus infection switches TLR-3-positive human neurons to become strong producers of beta interferon. J Virol 79, 12893–12904 (2005).
Lafon, M., Megret, F., Lafage, M. & Prehaud, C. The innate immune facet of brain: human neurons express TLR-3 and sense viral dsRNA. J Mol Neurosci 29, 185–194 (2006).
Ghoshal, A. et al. Proinflammatory mediators released by activated microglia induces neuronal death in Japanese encephalitis. Glia 55, 483–496 (2007).
Solomon, T. Flavivirus encephalitis. N Engl J Med 351, 370–378 (2004).
Kreutzberg, G. W. Microglia: a sensor for pathological events in the CNS. Trends Neurosci 19, 312–318 (1996).
Rempel, J. D., Quina, L. A., Blakely-Gonzales, P. K., Buchmeier, M. J. & Gruol, D. L. Viral induction of central nervous system innate immune responses. J Virol 79, 4369–4381 (2005).
Reiss, C. S., Chesler, D. A., Hodges, J., Ireland, D. D. & Chen, N. Innate immune responses in viral encephalitis. Curr Top Microbiol Immunol 265, 63–94 (2002).
Nazmi, A., Dutta, K. & Basu, A. RIG-I Mediates Innate Immune Response in Mouse Neurons Following Japanese Encephalitis Virus Infection. PLoS One 6, e21761 (2011).
Ishikawa, H. & Barber, G. N. STING is an endoplasmic reticulum adaptor that facilitates innate immune signalling. Nature 455, 674–678 (2008).
Zhong, B. et al. The adaptor protein MITA links virus-sensing receptors to IRF3 transcription factor activation. Immunity 29, 538–550 (2008).
Ishikawa, H., Ma, Z. & Barber, G. N. STING regulates intracellular DNA-mediated, type I interferon-dependent innate immunity. Nature 461, 788–792 (2009).
Chen, H. et al. Activation of STAT6 by STING Is Critical for Antiviral Innate Immunity. Cell 147, 436–446 (2011).
Terenzi, F., Hui, D. J., Merrick, W. C. & Sen, G. C. Distinct induction patterns and functions of two closely related interferon-inducible human genes, ISG54 and ISG56. J Biol Chem 281, 34064–34071 (2006).
Solomon, T. Exotic and emerging viral encephalitides. Curr Opin Neurol 16, 411–418 (2003).
Castanier, C., Garcin, D., Vazquez, A. & Arnoult, D. Mitochondrial dynamics regulate the RIG-I-like receptor antiviral pathway. EMBO Rep 11, 133–138 (2010).
DeFilippis, V. R., Alvarado, D., Sali, T., Rothenburg, S. & Fruh, K. Human cytomegalovirus induces the interferon response via the DNA sensor ZBP1. J Virol 84, 585–598 (2010).
Ishikawa, H. & Barber, G. N. The STING pathway and regulation of innate immune signaling in response to DNA pathogens. Cell Mol Life Sci 68, 1157–1165 (2011).
Stawowczyk, M., Van Scoy, S., Kumar, K. P. & Reich, N. C. The interferon stimulated gene 54 promotes apoptosis. J Biol Chem 286, 7257–7266 (2011).
Li, Y. et al. ISG56 is a negative-feedback regulator of virus-triggered signaling and cellular antiviral response. Proc Natl Acad Sci U S A 106, 7945–7950 (2009).
Bostrom, P. J. et al. Interferon-alpha inhibits cyclooxygenase-1 and stimulates cyclooxygenase-2 expression in bladder cancer cells in vitro. Urol Res 29, 20–24 (2001).
Nazmi, A., Dutta, K. & Basu, A. Antiviral and neuroprotective role of octaguanidinium dendrimer-conjugated morpholino oligomers in Japanese encephalitis. PLoS Negl Trop Dis 4, e892 (2010).
Dutta, K., Kumawat, K. L., Nazmi, A., Mishra, M. K. & Basu, A. Minocycline differentially modulates viral infection and persistence in an experimental model of Japanese encephalitis. J Neuroimmune Pharmacol 5, 553–565 (2010).
Das, S., Ghosh, D. & Basu, A. Japanese encephalitis virus induce immuno-competency in neural stem/progenitor cells. PLoS One 4, e8134 (2009).
Pathak, S. K. et al. Toll-like receptor 2 and mitogen- and stress-activated kinase 1 are effectors of Mycobacterium avium-induced cyclooxygenase-2 expression in macrophages. J Biol Chem 279, 55127–55136 (2004).
Niranjanakumari, S., Lasda, E., Brazas, R. & Garcia-Blanco, M. A. Reversible cross-linking combined with immunoprecipitation to study RNA-protein interactions in vivo. Methods 26, 182–190 (2002).
Kaushik, D. K., Gupta, M., Das, S. & Basu, A. Kruppel-like factor 4, a novel transcription factor regulates microglial activation and subsequent neuroinflammation. J Neuroinflammation 7, 68 (2010).
Acknowledgements
The authors would like to thank Manish Kumar Dogra and Kanhaiya Lal Kumawat for their technical assistance. This work is supported by funding from the Council of Scientific and Industrial Research (CSIR), Govt. of India [27(1638)/10] to A.B. A.N. is a recipient of the Senior Research Fellowship from the CSIR; K.D. is a recipient of a Research Associateship in Biotechnology and Life Sciences from the Department of Biotechnology (DBT), Govt. of India. A.B. is a recipient of the National Bioscience Award for Career Development-2010 from DBT.
Author information
Authors and Affiliations
Contributions
AN, RM and KD performed all the experiments. Data was analyzed by AN and KD; AN and KD prepared the figures. The main manuscript was written by AN, KD and AB. All the authors reviewed the manuscript.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-ShareALike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Nazmi, A., Mukhopadhyay, R., Dutta, K. et al. STING Mediates Neuronal Innate Immune Response Following Japanese Encephalitis Virus Infection. Sci Rep 2, 347 (2012). https://doi.org/10.1038/srep00347
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep00347
This article is cited by
-
Reducing lipid peroxidation attenuates stress-induced susceptibility to herpes simplex virus type 1
Acta Pharmacologica Sinica (2023)
-
Duck plague virus UL41 protein inhibits RIG-I/MDA5-mediated duck IFN-β production via mRNA degradation activity
Veterinary Research (2022)
-
The crosstalk between viral RNA- and DNA-sensing mechanisms
Cellular and Molecular Life Sciences (2021)
-
Neurocognitive impacts of arbovirus infections
Journal of Neuroinflammation (2020)
-
Ab initio investigation of the cyclodehydrogenation process for polyanthrylene transformation to graphene nanoribbons
npj Computational Materials (2019)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.