Key Points
-
Biologics are medicinal products manufactured in or extracted from a biological source and include a number of human monoclonal antibodies or variant fusion proteins.
-
Highlights that dentists should be cautious when they schedule extractions in patients treated with anti-RANKL and anti-VEGF agents as they carry a risk for MRONJ and impaired wound healing.
Abstract
Biological agents – biologics, biologicals or biopharmaceuticals – are any medicinal product manufactured in, or extracted from, a biological source. They are often generated by DNA recombinant biotechnology and several dozen therapeutic monoclonal antibodies (mAbs) are now marketed for a variety of indications, increasingly in the management of inflammatory immune-mediated disorders, transplantation rejection and cancer treatments. Immunomodulatory mAbs are expensive, must be given by injection or infusion and can have adverse effects but are increasingly used and can be highly effective agents. This paper reviews these agents and their increasing relevance to oral science and healthcare.
Similar content being viewed by others
Introduction
Biopharmaceuticals – biologics, biologicals or biological agents (BAs) – are any medicinal product manufactured in or extracted from, a biological source. Biologics often target immunocytes or their products and thus specific steps in pro-inflammatory pathways.1,2 The term can include materials ranging from blood to stem cells and vaccines but it is used for gene-based and cellular biologics, often generated by DNA recombinant biotechnology. Biologics are of two main classes:
-
Biologics: nearly identical to key signalling proteins, for example, biosynthetic human insulin, erythropoeitin, colony stimulating factors, or growth hormone
-
Monoclonal antibodies (mAbs): 'custom-designed' using hybridoma or other technology, these are antibodies which aim to counteract or block a given biological substance, or to target and damage a specific cell type. Receptor constructs, also known as fusion proteins or chimeric proteins (literally, made of parts from different sources), are proteins created through the joining of two or more genes that originally coded for separate proteins. They are usually based on a monoclonal antibody (which gives specificity), linked to the immunoglobulin or a fraction of it (which gives stability). Naturally occurring fusion proteins are commonly found in cancer cells, where they may function as oncoproteins, for example bcr-abl in chronic myeloid leukaemia. In terms of a drug, chimerisation involves replacing segments of the antibody produced in a mouse that distinguish it from a human antibody, to reduce adverse reactions, and this is shown by inserting -xi- into the name – such as, abci-xi-mab. Chimerisation is for example, the basis of anti-tumour necrosis factor (anti-TNF) drugs such as etanercept, made of the combination of a TNF receptor (TNFR) with the Fc segment of IgG (immunoglobulin G1). The TNFR provides specificity for the drug target which is TNF, and the Fc segment is believed to add stability and deliverability to the drug.3,4
Biologics are often used to target immunocytes or their products and thus specific steps in pro-inflammatory pathways. Biologics may act in this way by binding directly to immunocytes (T lymphocytes, B cells, granulocytes, antigen-presenting cells [APCs], dendritic cells [DCs], macrophages or other immunocytes) or immune mediators (cytokines, chemokines, growth factors, complement components) thereby acting to:
-
Deplete them
-
Suppress their function
-
Prevent their homing to lymphoid organs and inflammatory sites
-
Induce anergy (immune unresponsiveness).
Biologics include a number of human (suffix 'mab'), humanised (suffix 'zumab') or chimeric (mouse–human; suffix 'ximab') monoclonal antibodies or variant fusion proteins (suffix 'cept'). Several dozen therapeutic mAbs are now marketed for a variety of indications, increasingly in the treatment of inflammatory immune-mediated disorders, transplantation and cancers, where tremendous advances are occurring (Table 1).5
Immunomodulatory mAbs are expensive, and must be given by injection or infusion because they are large molecules.6,7,8 Their significant difference in size and the complexity of their structure in comparison to common drugs is depicted in Figure 1, where the paracetamol molecule is juxtaposed to the molecule of infliximab an anti-TNF agent. Despite the complicated synthesis and laborious conditions for their manufacturing, the number of new available biologic agents is growing. Furthermore, as the number of biologics increases exponentially, reports of adverse effects are also increasing and it is recognised that they may have an inherent risk for adverse immune-mediated drug reactions such as infusion reactions, cytokine storms, fatigue, arthralgias, immunosuppression, autoimmunity, infections, potential malignancy and other disorders. BAs use therefore requires precautionary considerations, including screening for coexistent medical disorders; the use of strict eligibility criteria which include a) severe disease, as measured by objective measurements and b) use only where patients are refractory to/intolerant of conventional systemic therapy or where such therapy is contraindicated.6 Nevertheless, despite potential serious adverse effects, biologics are generally considered safe – in part because of good adherence to clinical recommendations based upon data from controlled and observational studies, and the fast recognition and response to safety concerns.
PubChem Compound Database; CID=1983, http://pubchem.ncbi.nlm.nih.gov/compound/1983; infliximab, http://www.drugbank.ca/drugs/DB00065. Open source figures)
Main biological agents
The three main classes of BAs are TNF-α inhibitors, lymphocyte modulators and interleukin inhibitors.
TNF-α inhibitors
TNF-α is a key pro-inflammatory cytokine central in the pathogenesis of immunologically driven disease acting via pathways to promote increased leucocyte activation and recruitment to sites of tissue inflammation. TNF acts by binding to the plasma membrane receptor TNFR, leading to inflammation, or programmed cell death (apoptosis).9
TNF-α inhibitors block the TNF effects upon target inflammatory cells (Fig. 2). TNF-α can induce apoptosis (programmed cell death) and inflammation. These are achieved via activation of various pathways. TNF initiates activity by binding to cell-surface transmembrane receptors (TNF receptors). TNF-receptor 1 is generally expressed on all cell types, while TNF-receptor 2 is expressed only on endothelial and immune cells. TNF induces apoptosis by binding to TNF-receptor 1 which activates the caspase 3-8 cascade. TNF may promote inflammation by binding to either receptor 1 or 2. Signals are then produced, and mediated through TNF receptor-associated factor 2 (TRAF2), and thereafter by activating one or more of three pathways:
-
JNK (c-Jun N-terminal kinase)-dependent kinase cascade
-
MAPK (Mitogen-activated protein kinases) kinase cascade
-
NF-κB (Nuclear factor-kappa B) transcription factor.
TNF-α inhibitors include etanercept, infliximab, golimumab and adalimumab. These drugs are generally used to control inflammatory disorders such as rheumatoid arthritis (RA) or inflammatory bowel disease.10 The most common adverse effects from TNF-α blockers are injection and infusion site reactions. However, the most important safety problem is an increased risk of infections – including upper respiratory tract infections, opportunistic infections and reactivation of tuberculosis.11 Fungal or viral infections may also be seen.12
Immune reactions to TNF-α inhibitors include skin reactions, angiooedema and autoimmune disease, both systemic (lupus erythematosus, vasculitis, sarcoidosis, antiphospholipid syndrome and inflammatory myopathies) and organ-specific (interstitial lung disease, uveitis, optic neuritis, peripheral neuropathies, multiple sclerosis, psoriasis, inflammatory bowel disease and autoimmune hepatitis).13 Demyelinating diseases or flares of existing demyelinating diseases can occur with TNF-α inhibitors.14
A further important safety problem related to BAs, such as the TNF-α blockers, is an increased risk of neoplasms. Furthermore, aplastic anaemia and/or pancytopenia may complicate treatment with etanercept or adalimumab.15
Lymphocyte action inhibitory agents
Lymphocyte modulators act on specific lymphocyte antigens (cluster of differentiation [CD] antigens).
T-cell modulators
T-cell modulators include alefacept, a chimeric fusion protein of leucocyte function-associated antigen-3 (LFA-3), and immunoglobulin G1 which targets CD2+ on T memory cells and on natural killer (NK) cells, blocking the LFA-3/CD2 interaction in antigen presentation and also inducing T cell apoptosis. Alefacept was withdrawn in US but not for safety concerns.
T-cell co-stimulators
T-cell co-stimulators (such as abatacept), approved for RA, was the first co-stimulatory blocker.16 It targets the early phase of inflammation in RA and has an acceptable safety profile – infections and risk of malignancy development are the most significant but rare adverse effects.17,18.
B-cell modulators
The most widely used B-cell modulator is rituximab, an anti-CD20 monoclonal antibody which targets CD20 on mature B cells and is approved for use in NHL (non-Hodgkin lymphoma) and RA. Rituximab has a major benefit in patients with B-cell lymphomas.19 The B-cell depletion it causes (Fig. 3) can have serious adverse effects including infections (some fatal), including progressive multifocal leukoencephalopathy (PML) caused by reactivation of latent JC virus infection. Tumour lysis syndrome (TLS) is a life-threatening complication that arises when the rapid lysis of tumour cells leads to the release of excessive quantities of cellular contents into the systemic circulation, resulting in a metabolic disturbance characterised by hyperkalaemia, hyperphosphataemia, hyperuricaemia, and hypocalcaemia and can lead to acute oliguric renal failure and cardiac arrhythmias. Cutaneous eruptions can also arise. Rituximab is currently an off- label agent used in refractory cases of pemphigus vulgaris and Sjogren syndrome (see below), but clinicians should treat such cases with caution.7,8,9,20 A newer anti–B-cell agent, belimumab, has recently been approved for the treatment of systemic lupus erythematosus.
Alemtuzumab
Alemtuzumab is a humanised anti-CD52 monoclonal antibody, used for treatment of B-cell chronic lymphocytic leukemia.21 Alemtuzumab carries a high risk for severe infections and autoimmune conditions.22
Efalizumab
Efalizumab is a recombinant humanised IgG1 monoclonal antibody which binds to CD11a, an α-subunit of lymphocyte function-associated antigen 1 (LFA-1). LFA binds to an intercellular adhesion molecule 1 (ICAM-1), also known as CD54,23 and enhances the migration of T lymphocytes.24 Efalizumab has been withdrawn since 2009 because of a link with PML.
Gemtuzumab ozogamicin
Gemtuzumab ozogamicin is a semi-synthetic end product of calicheamicin, a cytotoxic antibiotic connected to a recombinant monoclonal antibody directed against the CD33 antigen on myeloblasts in patients with acute myeloid leukaemia (AML).2 This agent was withdrawn in 2010 due to safety concerns, but newer evidence suggests some patients could benefit from low doses of gemtuzumab ozogamicin.25 Ibritumomab tiuxetan, a CD20-directed radiotherapeutic antibody, used in the treatment of NHLs26 has a box-FDA warning for serious mucocutaneous adverse reactions.27
Interleukin inhibitors
Interleukins are a group of cytokines (IL-1 to IL-35 have been identified) synthesised mainly by lymphocytes, monocytes and macrophages whose role is the regulation of the immune system.28 Interleukin inhibitors are immunosuppressive agents which inhibit various interleukins and have a broad spectrum of uses depending on the interleukin they target.29
The chimeric anti-IL-2 receptor monoclonal antibody basiliximab, attaches to the alpha chain of interleukin-2 receptors (IL-2α) on the surface of activated T-lymphocytes and blocks them,30 and is used to prevent acute renal transplantation rejection. The most usual undesirable effects of basiliximab in adult patients are constipation, infections, pain, nausea, peripheral oedema, hypertension, anaemia, headache, hyperkalaemia, hypercholesterolaemia, raised serum creatinine and hypophosphataemia.31
IL-1β blockers canakinumab rinolacept and anakinra, have great efficacy in the control of cryopyrin-associated periodic syndromes.32
The anti-IL-2 receptor antibody daclizumab, is used to prevent acute transplant rejection with a similar safety profile as basiliximab33.
A humanised monoclonal antibody against IL-5 mepolizumab, is effective for the control of severe asthma in patients who suffered from exacerbations associated with persistent eosinophilic inflammation.34
A human IgG1 monoclonal antibody that selectively binds to and neutralises IL-17A secukinumab, is currently pending FDA approval for treatment of psoriasis.35
A recombinant humanised anti-human IL-6 receptor monoclonal antibody, tocilizumab, binds soluble as well as membrane bound IL-6 receptors, and is useful for rheumatoid arthritis.36
A fully human monoclonal antibody targeting IL-12 and IL-23 ustekinumab, is used for treatment of psoriasis and psoriatic arthritis.37
Other biological agents
Anti-coagulant and anti neo–vascularisation agents
Abciximab, the Fab section of the chimeric human-murine monoclonal antibody 7E3 binds to the platelet receptor glycoprotein IIb/IIIa and is used as an antiplatelet agent. The main adverse effects are bleeding and thrombocytopenia.38
Bevacizumab (Avastin), a vascular endothelial growth factor (VEGF) inhibitor, blocks angiogenesis is used in anti-cancer chemotherapy.39 The most common adverse reactions however, are epistaxis, headache, hypertension, rhinitis, taste alterations, dry skin, rectal haemorrhage, lacrimation disorders, back pain and exfoliative dermatitis.40 It is also labelled with an FDA warning for arterial thromboembolic events, hypertension, reversible posterior leukoencephalopathy syndrome (RPLS), proteinuria, infusion reactions and ovarian failure.41,42,43
Anti- epidermal growth factor receptors
Cetuximab, is an anti-epidermal growth factor receptor (EGFR) used against head and neck (including oral) and other cancers.44,45 A common adverse effect is a severe generalised acneiform eruption.46
Panitumumab, another EGFR competitor, has an FDA box warning for severe dermatologic toxicities.47
Trastuzumab, a humanised monoclonal antibody targeting the extracellular domain of the HER-2/neu protein and used to control certain breast cancers,48 can have severe adverse effects, which include congestive heart failure and cardiac dysfunction while there are cases of patients who have developed leukaemia.49
Pertuzumab, a recombinant humanised monoclonal antibody directed at the extracellular dimerisation domain (subdomain II) of HER2, used in breast cancers,50 has an FDA box warning for foetal toxicity: common adverse effects are neutropenia and leukopenia.51
Receptor activator of nuclear factor-kappa B ligand blockers
Denosumab, is a human monoclonal antibody which targets the receptor activator of nuclear factor-kappa B ligand (RANKL) and blocks it, inhibiting osteoclast growth and action – resulting in reduced bone resorption and increasing bone density (Fig. 4).52 Denosumab is used to prevent osteoporosis but severe adverse events include skin exanthemas and infections, decreased physiological bone turnover and jaw osteonecrosis (see below).53
The signaling process is initiated by the binding of RANK-L (Receptor activator of Nuclear Factor Kappa-B Ligand) to RANK (Receptor activator of Nuclear Factor Kappa-B). Denosumab, a human monoclonal antibody that inhibits RANK-L, thus blocks RANK-L action on osteoclasts. Based on Li W-F, Hou S-X, Yu B,Ferec C,Chen J-M. Genetics of osteoporosis: perspectives for personalized medicine. Per Med 2010;7: 655–668 and also on Shoback D. Update in osteoporosis and metabolic bone disorders. J Clin Endocrinol Metab 2007;92: 747–753.
Interferons
Interferons are cytokines produced by immune cells and fibroblasts and are part of the nonspecific immune response. Interferon alpha is produced naturally by leucocytes. Interferon-beta is produced by fibroblasts. Interferon-gamma is produced by T cells and NK cells.54 Interferons are used for various therapeutic purposes such as in treatment of hepatitis C, multiple sclerosis and mastocytosis.55,56,57 Recombinant products of interferons may have adverse effects such as flu-like symptoms and psychiatric disorders, while they may also trigger immunologic phenomena.58
Anti-microbial agents
Palivizumab is a monoclonal antibody that neutralises and exerts fusion-inhibitory activity against Respiratory Syncytial Virus (RSV).59 It is indicated for premature infants and is administered during the months of high prevalence of RVS. Raxibacumab is a recombinant, fully human, IgG1λ monoclonal antibody targeting B. anthracis protective antigen and may prevent deadly outcome of anthrax in animal studies.60
Vaccines
Human papillomavirus (HPV) recombinant vaccines are 93% effective in preventing cervical pre-cancers associated with HPV 16 and 18. Currently available for women the guidelines may extend its use soon in men.61,62
An autologous CD54 + dendritic cell vaccine Sipuleucel-T directed against Prostatic Acid Phosphatase (PAP), is the first immuno-modulating agent approved for the treatment of castration resistant prostate cancer.63
Administration of biologicals
The vast majority of biological agents must be injected regularly, but administration regimens differ. Infliximab and rituximab for example, must be given as periodic intravenous infusions, while etanercept, adalimumab and ustekinumab are given as regular subcutaneous injections (bi-weekly, weekly, every two weeks or monthly), with schedules varying with the condition being treated.7,8,20
Biologic uses in oral healthcare
The use of biologics in both licenced and off-label circumstances is rapidly evolving, with new efficacy and safety data frequently being reported. Biologics are also increasingly used in oral disease, especially when there is systemic involvement.6,7,8,64 The use of biologicals in the management of inflammatory oral mucosal disease is off-label and should involve medically qualified specialists, or physicians as these agents are systemic with strict precautions indicated.6,7,8 Despite a recent suggestion that topical use of these agents in oral disease may be one strategy that could be developed further, BAs are by definition systemic and cannot be absorbed locally to any extent since they are large molecules and not absorbed, or would likely be broken down by the gastrointestinal tract.
Ulcerative disorders
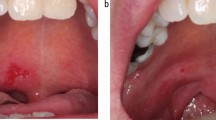
BAs are used mainly in patients with Behcet disease (BD), severe aphthous ulceration, and in vesiculobullous disease (including pemphigus and pemphigoid), and lichen planus with severe, or recalcitrant or multi-site lesions.6,8
Patients with oral ulcers as a component of BD have shown positive responses to TNF-α inhibitors, including infliximab, etanercept and adalimumab.65 Patients with RAS have been shown to respond to TNF-α inhibition with etanercept or adalimumab.66,67
Treatment-resistant autoimmune blistering skin disorders with oral involvement, such as pemphigoid and pemphigus, have responded to rituximab although significant adverse effects of rituximab therapy were reported in many of these, and similar, case-series suggesting great caution be attached to their clinical use in these mucocutaneous diseases.68 With the recognised safety concerns there would seem to be no place for rituximab for oral lesions alone. Etanercept has been effective in managing oral mucosal pemphigoid.69
Severe lichen planus (LP) has responded to alefacept and to TNF-α blockade with etanercept and adalimumab.70,71 However, LP-like eruptions are also an emerging adverse effect of TNF-α inhibitors.72
Crohn's disease and OroFacial Granulomatosis (OFG)
TNF-α inhibitors infliximab and adalimumab are increasingly used in Crohn's disease.73 Biologics may also help patients with extra-intestinal manifestations of Crohn's disease, including oral Crohn's disease and related disorders like orofacial granulomatosis74 (OFG), and allied conditions such as Melkersson-Rosenthal syndrome (MRS) and a more limited granulomatous cheilitis (described by some as a monosymptomatic form of MRS) have been reported.75 Unfortunately, not all cases of OFG with Crohn's disease (or previous intestinal disease) are responsive to infliximab. Overall, the data suggest that TNF-α inhibitors may have some role in the management of oral manifestations of Crohn's disease and similar disorders such as OFG and MRS, but while use of TNF-α inhibition in the setting of inflammatory bowel disease is considered safe, adverse effects are well recognised and include infusion reactions, infection, and increased risk of malignancy.7,8
Sjögren's syndrome
The efficacy of BAs in RA stimulated studies of their use in other autoimmune conditions, including primary Sjögren's syndrome (SS). Initial studies of TNF-α blockers in patients with SS showed promise but subsequent RCTs could not support the potential benefit for infliximab and confirmed a lack of benefit of etanercept.76 Since B-cells play a key role in the pathogenesis of SS, as seen in the array of autoantibody production, (ANA, anti-SS-A/SS-B etc), hypergammaglobulinaemia, B-cell infiltration of salivary and extrasalivary tissue, and the association with B-cell MALT lymphomas and anti-B cell monoclonals have been further studied.
Rituximab however, has produced some improved SS symptoms (xerostomia etc) and increased salivary gland function and MALT has remitted in some patients.77 There appears to be a clinical benefit from rituximab in systemic extraglandular complications of SS (fatigue, cryoglobulinaemia, pulmonary disease, polysynovitis, arthralgia and peripheral neuropathy), but little benefit in longer term improvements in SS symptoms or in salivary flow.78
Cancers
Some biologics are used in oral cancer therapy (Table 1). Biologics against angiogenesis such as VEGF inhibitors such as bevacizumab and others against epidermal growth factor receptors (anti-EGFR) agents are prime examples now in clinical use.79 Anti-EGFRs such as cetuximab have significantly improved oral cancer patients survival.80
Other impacts of biological agents on oral healthcare
Some of the BAs are now in common use and dental professionals are likely to treat many patients under such treatment. The most popular category is that of immune modulating agents. There are no official guidelines concerning patients on immune-modulating BAs who are scheduled for invasive dental procedures.7,8,9
Communication with the physician who monitors their treatment is mandatory, to agree the best approach. In general, any dental treatment that may cause bacteraemia should be scheduled before the beginning of therapy.
The commonly used medications such as amoxicillin and paracetamol, and local anaesthetics appear to have no interactions with any of the agents listed in Table 1. Of note it is not yet clear how most of these agents are metabolised and if they interfere with common CYP enzyme pathway that metabolises most drugs.
It would seem advisable to treat such patients on BAs with caution since BAs may predispose to infections, bleeding, medication-related osteonecrosis of the jaw (MRONJ) and impaired wound healing.
Infections
Extra precautions should be taken to deal with extremely urgent dental infections for example, in post-transplant patients during induction therapy, as multiple agents that suppress the immune system are administered including the anti-IL2 or the anti-CD3 agents. It is advisable that all transplant patients should be examined by dentists and any teeth that could possibly cause infections should be removed before transplant surgery.64 In case that any oral infection occurs in the induction phase it is advisable to be treated conservatively and with the advice of the transplantologist.
Bleeding tendency
The possibility of a bleeding tendency should be considered but to our knowledge there is only one patient reported who developed oral (gingival) bleeding due to abciximab related thrombocytopenia, and her condition improved after platelet concentrate transfusion.81
Jaw osteonecrosis
Osteonecrosis of the jaws (ONJ) is a particular issue following invasive dental or oral surgery, since many such procedures impact on bone. Bisphosphonates (BPs), denosumab, bevacizumab, sorafenib and sunitinib are among the drugs used in medication-related osteonecrosis of the jaws. Bisphosphonates (BPs) are potent inhibitors of osteoclast-mediated bone resorption, which is increased when cancers invade bone. BPs are an established treatment for cancer spread to bone, and effectively reduce pain and other skeletal-related events. Denosumab is a fully human monoclonal antibody with high affinity and specificity for RANKL, a cytokine that is the main final mediator of osteoclastic bone resorption. Bevacizumab, sorafenib and sunitinib are angiogenesis inhibitors that block various steps in the binding of signalling molecules, such as VEGF.82 The risk of ONJ is about 1% for cancer patients receiving intravenous BPs (zolendronate), and there is a comparable figure for cancer patients exposed to denosumab while the risk for patients on VEGF inhibitors is lower (for example, 0.2% with bevacizumab).83,84 There appears to be an increased risk in those patients combining anti-resorptive and anti-angiogenic therapy – ONJ may be as frequent as 10% in those on combined BP and sunitinib therapy.85
For patients with exposure to the above agents and in whom surgical intervention is required, cessation or interruption of anti-resorptive and anti-angiogenic medication (a drug-holiday) has been advocated to minimise the risk of developing ONJ. However, robust data on the effectiveness of drug holidays are lacking and this has been a controversial topic. A recent American Association of Oral and Maxillofacial Surgeons position paper now suggests that 'for those who have been exposed to more than four years of oral BPs therapy and whom a surgical intervention is planned, a drug-holiday of about two months before surgery and three months following surgery be undertaken to reduce the risk of ONJ'.86 This paper makes no recommendation for patients on other agents but we suggest, based on the pharmacology of denosumab, that a drug interruption of six months would possibly reduce the risk of some MRONJ.
Impaired wound healing
For VEGF inhibitors, the recommendations in the medical literature (which are adopted by surgical oncologists and plastic surgeons, to minimise wound healing impairment), might be used as a guide: bevacizumab has a median half-life of about 20 days (range 11–50 days) and on this basis a six to eight week interruption of bevacizumab treatment before surgery and four weeks after surgery, has been advocated to lower the risk of wound complications.87
Conclusions and future prospects
It is evident that biologically engineered agents are providing a new range of therapeutic solutions and may resolve several dead ends such as the antibiotic resistance and the absence of a wide range of antiviral agents. In addition, more than 900 new agents that are manufactured using biological processes are under development,88 a fact that underlies the interest of the pharmaceutical industry for this category of agents. It is therefore necessary to be aware of the progress in the biological drugs, because they will be administered more and more to our patients. The antagonising field for biologics is the newly formed class of targeted small molecules like tofacitinib, a Janus kinase inhibitor which is an oral small molecule that acts inside the cell and is approved for rheumatoid arthritis by the FDA.89 The field of targeted drug therapies is yet to offer many solutions and change the traditional therapeutics.
References
Murdaca G, Colombo B, Puppo F . Anti-TNF-alpha inhibitors: a new therapeutic approach for inflammatory immune-mediated diseases: an update upon efficacy and adverse events. Int J Immunopathol Pharmacol 2008; 22: 557–565.
Tayal V, Kalra B S . Cytokines and anti-cytokines as therapeutics - an update. Eur J Pharmacol 2008; 579: 1–12.
Grounds M D, Davies M, Torrisi J, Shavlakadze T, White J and Hodgetts S . Silencing TNFalpha activity by using Remicade or Enbrel blocks inflammation in whole muscle grafts: an in vivo bioassay to assess the efficacy of anti-cytokine drugs in mice. Cell Tissue Res 2005; 320: 509–515.
Scott D L, Wolfe F, Huizinga T W . Rheumatoid arthritis. Lancet 2010; 376: 1094–1108.
Georgakopoulou E A, Scully C . Orofacial adverse effects of biological agents. J Investig Clin Dent 2014 [Epub ahead of print].
O'Neill I D, Scully C . Biologics in oral medicine: oral Crohn's disease and orofacial granulomatosis. Oral Dis 2012; 18: 633–638.
O'Neill I D, Scully C . Biologics in oral medicine: principles of use and practical considerations. Oral Dis 2012; 18: 525–536.
O'Neill I D, C Scully . Biologics in oral medicine: ulcerative disorders. Oral Dis 2013; 19: 37–45.
Wu Y, B P Zhou . TNF-alpha/NF-kappaB/Snail pathway in cancer cell migration and invasion. Br J Cancer 2010; 102: 639–644.
Simsek I . TNF inhibitors - new and old agents for rheumatoid arthritis. Bull NYU Hosp Jt Dis 2010; 68: 204–210.
Jain A, Singh J A . Harms of TNF inhibitors in rheumatic diseases: a focused review of the literature. Immunotherapy 2013; 5: 265–299.
Bongartz T, Sutton A J, Sweeting M J, Buchan I, Matteson E L, Montori V . Anti-TNF antibody therapy in rheumatoid arthritis and the risk of serious infections and malignancies: systematic review and meta-analysis of rare harmful effects in randomized controlled trials. JAMA 2006; 295: 2275–2285.
Ramos-Casals M, Brito-Zerón P, Munoz S et al. Autoimmune diseases induced by TNF-targeted therapies: analysis of 233 cases. Medicine 2007; 86: 242–251.
Mohan N, Edwards E T, Cupps T R et al. Demyelination occurring during anti–tumor necrosis factor α therapy for inflammatory arthritides. Arthritis Rheum 2001; 44: 2862–2869.
Antoni C, Braun J . Side effects of anti-TNF therapy: current knowledge. Clin Exp Rheumatol 2002; 20(Suppl 28): S152–S157.
Teng G G, Turkiewicz A M, Moreland L W . Abatacept: a costimulatory inhibitor for treatment of rheumatoid arthritis. Expert Opin Biol Ther 2005; 5: 1245–1254.
Khraishi M, Russell A, Olszynski W P . Safety profile of abatacept in rheumatoid arthritis: a review. Clin Ther 2010; 32: 1855–1870.
Maxwell L J, Singh J A . Abatacept for rheumatoid arthritis: a Cochrane systematic review. J Rheumatol 2010; 37: 234–245.
Sehn L H, Donaldson J, Chhanabhai M et al. Introduction of combined CHOP plus rituximab therapy dramatically improved outcome of diffuse large B-cell lymphoma in British Columbia. J Clin Oncol 2005; 23: 5027–5033.
Georgakopoulou E A, Andreadis D, Arvanitidis E, Loumou P . Biologic agents and oral diseases - an update on clinical applications. Acta Dermatovenerol Croat 2013; 21: 24–34.
Quintas-Cardama A, O'Brien S . Targeted therapy for chronic lymphocytic leukemia. Target Oncol 2009; 4: 11–21.
Gilliland L K, Walsh L A, Frewin M R et al. Elimination of the immunogenicity of therapeutic antibodies. J Immunol 1999; 162: 3663–3671.
Kuehn B M . Efalizumab withdrawn. JAMA 2009; 301: 2085–2085.
Leonardi C L . Efalizumab: an overview. J Am Acad Dermatol 2003; 49: 98–104.
Ravandi F, Kantarjian H . Haematological cancer: Gemtuzumab ozogamicin in acute myeloid leukaemia. Nat Rev Clin Oncol 2012; 9: 310–311.
Witzig T E, Gordon L I, Cabanillas F et al. Randomized controlled trial of yttrium-90-labeled ibritumomab tiuxetan radioimmunotherapy versus rituximab immunotherapy for patients with relapsed or refractory low-grade, follicular, or transformed B-cell non-Hodgkin's lymphoma. J Clin Oncol 2002; 20: 2453–2463.
Johnston P B, Bondly C, Micallef I N . Ibritumomab tiuxetan for non-Hodgkin's lymphoma. Expert Rev Anticancer Ther 2006; 6: 861–869.
Liles W C, van Voorhis W C . Review: nomenclature and biologic significance of cytokines involved in inflammation and the host immune response. J Infect Dis 1995; 172: 1573–1580.
Khadka A . Interleukins in therapeutics. PharmaTutor 2014; 2: 67–72.
Nashan B, Moore R, Amlot P, Schmidt A-G, Abeywickrama K, Soulillou J-P . Randomised trial of basiliximab versus placebo for control of acute cellular rejection in renal allograft recipients. Lancet 1997; 350: 1193–1198.
Choy B, Chan T, Li F et al. IL2-receptor antagonist (basiliximab) induction therapy is associated with lower morbidity and mortality in renal transplant recipients. Transplant Proc 2003; 35: 195.
McDermott M F . Rilonacept in the treatment of chronic inflammatory disorders. Drugs Today (Barc) 2009; 45: 423–430.
Vincenti F, Kirkman R, Light S et al. Interleukin-2-receptor blockade with daclizumab to prevent acute rejection in renal transplantation. N Engl J Med 1998; 338: 161–165.
Ortega H G, Liu M C, Pavord I D et al. Mepolizumab treatment in patients with severe eosinophilic asthma. N Engl J Med 2014; 371: 1198–1207.
Papp K, Langley R, Sigurgeirsson B et al. Efficacy and safety of secukinumab in the treatment of moderate-to-severe plaque psoriasis: a randomized, double-blind, placebo-controlled phase II dose-ranging study. Br J Dermatol 2013; 168: 412–421.
Fortunet C, Pers Y-M, Lambert J et al. Tocilizumab induces corticosteroid sparing in rheumatoid arthritis patients in clinical practice. Rheumatology (Oxford) 2015; 54: 672–677.
Leonardi C L, Kimball A B, Papp K A et al. Efficacy and safety of ustekinumab, a human interleukin-12/23 monoclonal antibody, in patients with psoriasis: 76-week results from a randomised, double-blind, placebo-controlled trial (PHOENIX 1). Lancet 2008; 371: 1665–1674.
Stone G W, Grines C L, Cox D A et al. Comparison of angioplasty with stenting, with or without abciximab, in acute myocardial infarction. N Engl J Med 2002; 346: 957–966.
Hurwitz H, Fehrenbacher L, Novotny W et al. Bevacizumab plus irinotecan, fluorouracil, and leucovorin for metastatic colorectal cancer. N Engl J Med 2004; 350: 2335–2342.
Zhu X, Wu S, Dahut W L, Parikh C R . Risks of proteinuria and hypertension with bevacizumab, an antibody against vascular endothelial growth factor: systematic review and meta-analysis. Am J Kidney Dis 2007; 49: 186–193.
Glusker P, Recht L, Lane B . Reversible posterior leukoencephalopathy syndrome and bevacizumab. N Engl J Med 2006; 354: 980–982.
Stearns V, Schneider B, Henry N L, Hayes D F, Flockhart D A . Breast cancer treatment and ovarian failure: risk factors and emerging genetic determinants. Nat Rev Cancer 2006; 6: 886–893.
Ranpura V, Hapani S, Chuang J, Wu S . Risk of cardiac ischemia and arterial thromboembolic events with the angiogenesis inhibitor bevacizumab in cancer patients: a meta-analysis of randomized controlled trials. Acta oncol 2010; 49: 287–297.
Cunningham D, Humblet Y, Siena S et al. Cetuximab monotherapy and cetuximab plus irinotecan in irinotecan-refractory metastatic colorectal cancer. N Engl J Med 2004; 351: 337–345.
Bonner J A, Harari P M, Giralt J et al. Radiotherapy plus cetuximab for squamous-cell carcinoma of the head and neck. N Engl J Med 2006; 354: 567–578.
Moss J E, Burtness B . Cetuximab-associated acneiform eruption. N Engl J Med 2005; 353: e17.
Lacouture M E, Anadkat M J, Bensadoun R-J et al. Clinical practice guidelines for the prevention and treatment of EGFR inhibitor-associated dermatologic toxicities. Support Care Cancer 2011; 19: 1079–1095.
Vogel C L, Cobleigh M A, Tripathy D et al. Efficacy and safety of trastuzumab as a single agent in first-line treatment of HER2-overexpressing metastatic breast cancer. J Clin Oncol 2002; 20: 719–726.
Herrmann J, Herrmann S M, Haddad T C . New-onset heart failure in association with severe hypertension during trastuzumab therapy. Mayo Clinic Proc 2014; 89: 1734–1739.
Baselga J, Cortés J, Kim S-B et al. Pertuzumab plus trastuzumab plus docetaxel for metastatic breast cancer. N Engl J Med 2012; 366: 109–119.
Boix-Perales H, Borregaard J, Jensen K B et al. The European medicines agency review of pertuzumab for the treatment of adult patients with HER2-positive metastatic or locally recurrent unresectable breast cancer: summary of the scientific assessment of the committee for medicinal products for human use. Oncologist 2014; 19: 766–773.
Cummings S R, Martin J S, McClung M R et al. Denosumab for prevention of fractures in postmenopausal women with osteoporosis. N Engl J Med 2009; 361: 756–765.
Diz P, López-Cedrún J L, Arenaz J, Scully C (2012). Denosumab-related osteonecrosis of the jaw. J Am Dent Assoc (1939). 2012; 143: 981–984.
Stark G R, Kerr I M, Williams B R, Silverman R H, Schreiber R D . How cells respond to interferons. Annu Rev Biochem 1998; 67: 227–264.
Davis G L, Balart L A, Schiff E R et al. Treatment of chronic hepatitis C with recombinant interferon alfa. N Engl J Med 1989; 321: 1501–1506.
Kluin-Nelemans H C, Jansen J H, Breukelman H et al. Response to interferon alfa-2b in a patient with systemic mastocytosis. N Engl J Med 1992; 326: 619–623.
The IFNB Multiple Sclerosis Study Group. Interferon beta-1b is effective in relapsing-remitting multiple sclerosis I. Clinical results of a multicenter, randomized, double-blind, placebo-controlled trial. Neurology 1993; 43: 655–655.
Walther E, Hohlfeld R . Multiple sclerosis side effects of interferon beta therapy and their management. Neurology 1999; 53: 1622–1622.
Frogel M P, Stewart D L, Hoopes M, Fernandes A W, Mahadevia P J . A systematic review of compliance with palivizumab administration for RSV immunoprophylaxis. J Manag Care Pharm 2010; 16: 46–58.
Migone T-S ., Subramanian G M, Zhong J et al. Raxibacumab for the treatment of inhalational anthrax. N Engl J Med 2009; 361: 135–144.
Villa L L, Costa R L, Petta C A et al. Prophylactic quadrivalent human papillomavirus (types 6: 11, 16, and 18) L1 virus-like particle vaccine in young women: a randomised double-blind placebo-controlled multicentre phase II efficacy trial. Lancet Oncol 2005; 6: 271–278.
Saslow D, Castle P E, Cox J T et al. American Cancer Society Guideline for human papillomavirus (HPV) vaccine use to prevent cervical cancer and its precursors. CA Cancer J Clin 2007; 57: 7–28.
Wadia R, Petrylak D P . New developments in the treatment of castration resistant prostate cancer. Asian J Androl 2014; 16: 555–560.
Georgakopoulou E A, Achtari M D, Afentoulide N . Dental management of patients before and after renal transplantation. Stomatologija 2011; 13: 107–112.
Sfikakis P, Markomichelakis N, Alpsoy E et al. Anti-TNF therapy in the management of Behçet's disease—review and basis for recommendations. Rheumatology 2007; 46: 736–741.
Robinson N D, Guitart J . Recalcitrant, recurrent aphthous stomatitis treated with etanercept. Arch Dermatol 2003; 139: 1259–1262.
Vujevich J, Zirwas M . Treatment of severe, recalcitrant, major aphthous stomatitis with adalimumab. Cutis 2005; 76: 129.
Joly P, Mouquet H, Roujeau J-C . A single cycle of rituximab for the treatment of severe pemphigus. N Engl J Med 2007; 357: 545–552.
Sacher C, Rubbert A, König C, Scharffetter-Kochanek K, Krieg T, Hunzelmann N . Treatment of recalcitrant cicatricial pemphigoid with the tumor necrosis factor α antagonist etanercept. J Am Acad Dermatol 2002; 46: 113–115.
Yarom N . Etanercept for the management of oral lichen planus. Am J Clin Dermatol 2007; 8: 121–121.
Chao T J . Adalimumab in the management of cutaneous and oral lichen planus. Cutis 2009; 84: 325–328.
Asarch A, Gottlieb A B, Lee J et al. Lichen planus–like eruptions: An emerging side effect of tumor necrosis factor-α antagonists. J Am Acad Dermatol 2009; 61: 104–111.
Colombel J F, Sandborn W J, Rutgeerts P et al. Adalimumab for maintenance of clinical response and remission in patients with Crohn's disease: the CHARM trial. Gastroenterology 2007; 132: 52–65.
Elliott T, Campbell H, Escudier M et al. Experience with anti-TNF-α therapy for orofacial granulomatosis. J Oral Pathol Med 2011; 40: 14–19.
Kakimoto C, Sparks C, White A A . Melkersson-Rosenthal syndrome: a form of pseudoangioedema. Ann Allergy Asthma Immunol 2007; 99: 185–189.
Moutsopoulos N M, Katsifis G E, Angelov N et al. Lack of efficacy of etanercept in Sjögren syndrome correlates with failed suppression of tumour necrosis factor α and systemic immune activation. Ann Rheum Dis 2008; 67: 1437–1443.
Pijpe J, Van Imhoff G W, Vissink A et al. Changes in salivary gland immunohistology and function after rituximab monotherapy in a patient with Sjögren's syndrome and associated MALT lymphoma. Ann Rheum Dis 2005; 64: 958–960.
Pijpe J, Meijer J M, Bootsma H et al. Clinical and histologic evidence of salivary gland restoration supports the efficacy of rituximab treatment in Sjögren's syndrome. Arthritis Rheum 2009; 60: 3251–3256.
Cohen E E, Davis D W, Karrison T G et al. Erlotinib and bevacizumab in patients with recurrent or metastatic squamous-cell carcinoma of the head and neck: a phase I/II study. Lancet Oncol 2009; 10: 247–257.
Vermorken J B, Mesia R, Rivera F et al. Platinum-based chemotherapy plus cetuximab in head and neck cancer. N Engl J Med 2008; 359: 1116–1127.
Oh Y-J, Park T-H, Choi T-J et al. Abciximab (ReoPro)-induced thrombocytopenia diagnosed through measurement of heparin-dependent antibody. Korean Circ J 2009; 39: 75–78.
Troeltzsch M, Woodlock T, Kriegelstein S, Steiner T, Messlinger K, Troeltzsch M . Physiology and pharmacology of nonbisphosphonate drugs implicated in osteonecrosis of the jaw. J Can Dent Assoc 2012; 78: 1–7.
Guarneri V, Miles D, Robert N et al. Bevacizumab and osteonecrosis of the jaw: incidence and association with bisphosphonate therapy in three large prospective trials in advanced breast cancer. Breast Cancer Res Treat 2010; 122: 181–188.
Saad F, Brown J, Van Poznak C et al. Incidence, risk factors, and outcomes of osteonecrosis of the jaw: integrated analysis from three blinded active-controlled phase III trials in cancer patients with bone metastases. Ann Oncol 2012; 23: 1341–1347.
Beuselinck B, Wolter P, Karadimou et al. (2012). Concomitant oral tyrosine kinase inhibitors and bisphosphonates in advanced renal cell carcinoma with bone metastases. Br J Cancer 2012; 107: 1665–1671.
Ruggiero S L, Dodson T B, Fantasia J et al. American association of oral and maxillofacial surgeons position paper on medication-related osteonecrosis of the jaw - 2014 update. J Oral Maxillofac Surg 2014; 72: 1938–1956.
Sharma K, Marcus J R . Bevacizumab and wound-healing complications: mechanisms of action, clinical evidence, and management recommendations for the plastic surgeon. Ann Plast Surg 2013; 71: 434–440.
Pharmaceutical Research and Manufacturers of America. Medicines in development: biologics. 2013. Online information available at http://www.phrma.org/sites/default/files/pdf/biologicsoverview2013.pdf (accessed June 2015).
Kremer J M, Bloom B J, Breedveld F C et al. The safety and efficacy of a JAK inhibitor in patients with active rheumatoid arthritis: Results of a double-blind, placebo-controlled phase IIa trial of three dosage levels of CP-690: 550 versus placebo. Arthritis Rheum 2009; 60: 1895–1905.
Author information
Authors and Affiliations
Corresponding author
Additional information
Refereed Paper
Rights and permissions
About this article
Cite this article
Georgakopoulou, E., Scully, C. Biological agents: what they are, how they affect oral health and how they can modulate oral healthcare. Br Dent J 218, 671–677 (2015). https://doi.org/10.1038/sj.bdj.2015.439
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bdj.2015.439
This article is cited by
-
Anti-thrombotic agents
British Dental Journal (2015)