Abstract
Study design:
Retrospective and prospective observational.
Objective:
The main objective of this study was to analyse suicide attempt as a cause of traumatic spinal cord injury (tSCI) and suicide as a cause of death after tSCI.
Setting:
This study was conducted at two British spinal centres, Stoke Mandeville and Southport.
Methods:
Long-term survival of patients who were newly admitted between 1991 and 2010, had survived the first post-injury year and had neurological deficit on discharge. Follow-up was discontinued on 31 December 2014.
Results:
Among the 2304 newly admitted cases of tSCI, suicide attempt was the cause of injury in 63 cases (2.7%). By the end of 2014 there were 533 deaths of which 4.2% deaths were by suicide, with 91% of suicides happening in the first 10 years post injury. Multiple logistic regression analyses showed a higher mortality odds ratio (OR=4.32, P<0.001) and a much higher suicide OR (9.46, P<0.001) for persons injured in suicide attempts when compared with all other SCI aetiologies. The overall age-standardised suicide mortality rate was 62.5 per 100 000 persons per year (95% confidence interval=36.4–88.6), five times higher than the general population suicide rate for England and Wales in 2014 (12.2 per 100 000).
Conclusions:
Suicide attempt was the cause of tSCI in 2.7% of the sample and suicide was the cause of death in 4.2% of all deaths. The overall mortality and death by suicide were significantly higher in persons whose tSCI was caused by an attempted suicide when compared with the rest of the sample. Continued psychological attention following SCI, especially to those who were injured by suicide attempt, is warranted.
Similar content being viewed by others
Introduction
Recently, Kennedy and Garmon-Jones1 published an excellent literature review on suicide before and after spinal cord injury (SCI) and risk factors associated with suicidal behaviour. From their synthesis of 22 relevant articles they concluded that up to 6.8% of all traumatic SCIs were caused by suicide attempts, and that between 4 and 11% of deaths following SCI were due to suicide. They identified the presence of psychiatric disorders as the main risk factor associated with suicide and highlighted the crucial need for risk assessment and psychological intervention for mental health issues following SCI. The authors also emphasised the need for more research into suicide attempts both before and after SCI and into additional risk factors that may contribute to suicide after SCI. Two British studies were included in their review, one from England and one from Scotland, both looking at suicide as a cause of SCI, but there were no British studies reporting on suicide as a cause of death after SCI.2, 3
Since then we have analysed causes of death after traumatic SCI in persons treated at two British spinal centres, Stoke Mandeville and Southport, between 1943 and 2014, and found that suicides accounted for 3.2% of all deaths in our sample. The suicide rates showed an improving trend over the 70-year study period, but were still 2.7 times higher in the latest study period when compared with the general population of England and Wales in 2014.4
The aim of this paper was to look at suicide in more detail, both as a cause of SCI and as a cause of death after SCI, in a subgroup of the above British cohort. We hypothesised that those whose injury was caused by a failed suicide attempt would have higher mortality rates due, at least in part, to a higher successful suicide rate post injury.
Materials and methods
Study design
Retrospective medical records review, and retrospective and prospective mortality data collection for an inception cohort of people with SCI.
Sample
The sample consisted of all patients with traumatic SCI (tSCI) who were newly admitted to Stoke Mandeville and Southport spinal centres between 01 January 1991 and 31 December 2010, who survived the first year post injury, had residual neurological deficit on discharge and were British residents. Their survival status was followed up to the end of 2014. The sample was a subgroup of a larger 70-year British mortality study and included only individuals newly admitted during that study’s last 20-year recruitment period (1991–2010). The original British mortality study database did not distinguish suicide attempts from other aetiologies. Patients newly admitted since 1991 were recently added to the study database and had detailed information collected about suicide attempts causing the SCI, as well as the full suicide mortality information.4
Data collection
Demographic and injury information was collected retrospectively from the medical records at the two spinal centres.
Survival status and death certificates for the deceased were supplied by the Medical Research Information Service, Health and Social Care Information Centre on behalf of the United Kingdom (UK) Office for National Statistics retrospectively for individuals already deceased at the time of sample identification, and prospectively for the rest, up to and including 31 December 2014. Data exchange was done through a secure Health and Social Care Information Centre Data Exchange Service. Causes of death were identified from the death certificates and, when available, from autopsy reports. For those who died at one of the spinal centres, additional information was collected from their medical notes at the centre, where available. The UK Office for National Statistics also produced national mortality figures for the general population of England and Wales.
Data analysis
Data analyses were performed on an anonymised database using Statistical Package for the Social Sciences (SPSS), Version 17 (SPSS Inc., Chicago, IL, USA), SPSS, version 22 (International Business Machines (IBM) Corporation, Armonk, NY, USA) and Statistical Analysis System (SAS Institute Inc., Cary, NC, USA) programmes.
For analysis purposes the sample was divided into five injury severity groups based on the International Standards for Neurological Classification of Spinal Cord Injury.5 The five groups were as follows: (1) those on either full-time or part-time permanent mechanical ventilation or phrenic nerve stimulation (ventilator-dependent); (2) those with high-level tetraplegia and American Spinal Injury Association (ASIA) Impairment Scale (AIS) grade A, B or C (C1–C4 ABC); (3) low-level tetraplegia and AIS grade A, B or C (C5–C8 ABC); (4) paraplegia and AIS grade A, B or C (para ABC); and (5) those with incomplete AIS grade D injuries regardless of the level (all AIS Ds).
The UK Office for National Statistics 2014 definition of suicide was used, by which suicide includes intentional self-harm, as well as injury/poisoning of undetermined intent for persons over 14 years of age. According to the International Classification of Diseases version 9, this includes codes E950-E959 and E980-E989, and according to the International Classification of Diseases version 10, codes X60-X84 and Y10-Y34.6
Descriptive statistics were used for presenting the sample. Suicide attempt as a cause of injury and suicide as a cause of death were expressed as a percentage of all known causes.
A person-year data set was created with each year of follow-up for each person (person-year) being treated as a separate observation. Thus, a person who was followed up for 5 years and had died during the fifth year would contribute five observations to the data set; the person in this example would be considered as alive at the end of each of the first four observations and deceased for the fifth observation.
Unadjusted (crude) suicide rates per 100 000 person-years were calculated for persons whose injury was caused by a failed suicide attempt and for those injured by other means. The risk ratio (RR) and 95% confidence limits were then calculated as the suicide rate for persons injured by a suicide attempt divided by the suicide rate for persons injured by other means. Aetiologic fraction among those whose injury was caused by a suicide attempt (the proportion of subsequent suicides in the attempted suicide group that was directly attributable to the original suicide attempt) was calculated as (RR−1)/RR. Population aetiologic fraction (the proportion of deaths due to suicide in the entire population that could be prevented if no injuries were caused by failed suicide attempts) was calculated using the following formula: ((prevalence of suicide attempt) × (RR−1))/(1+(prevalence of suicide attempt) × (RR−1)).
Following completion of these univariate analyses, multivariate logistic regression analysis of the person-year observations was used to determine overall mortality odds ratios (ORs) and death by suicide ORs, with 95% confidence intervals (CIs), after adjusting for the presence of other risk factors. The risk factors included in the model were current age, post-injury year, calendar year of each follow-up year of observation, gender, neurological grouping and suicide attempt as cause of SCI. CIs not containing the ‘0’ value, as well as P-value of <0.05, indicated statistical significance.
Finally, the age-standardised suicide mortality rate and 95% confidence limits were calculated by applying SCI age-specific suicide mortality rates to the age distribution of the 2013 European Standard Population. The age-standardised suicide rate was then compared with the general population age-standardised suicide rate for England and Wales 2014, which was weighted to match the SCI group gender distribution. Mortality rates were expressed in number of deaths per 100 000 persons at risk per year. This process of direct calculation of an age-standardised suicide rate is analogous to the indirect adjustment of age differences achieved by calculating standardised mortality ratios.
Statement of ethics
This study was approved by Berkshire Research Ethics Committee (REC), REC reference number 11/H0505/1.
We certify that all applicable institutional and governmental regulations concerning the ethical use of patient identifiable data were followed during the course of this research.
Results
Sample characteristics
Between 1991 and 2010 there were 2304 newly admitted individuals with tSCI who fulfilled the study inclusion criteria. The mean age at injury for the entire sample was 38.4 (range 0.5–90.99, median 35.1) years. The gender distribution was 77.6% male and 22.4% female. The neurological grouping of SCI was as follows: 2.8% ventilator-dependent; 9.7% C1–4 tetraplegia AIS grade ABC; 21.2% C5–8 tetraplegia ABC; 37.2% paraplegia ABC; and 29.1% AIS grade D injury of any level. Causes of tSCI were road traffic accidents (42.1%), falls excluding suicide attempts (30.2%), sport injuries (15.1%), violence (4.1%), suicide attempt (2.7%), surgical complications (2.6%), hit by objects (2.1%), other traffic accidents (0.6%) and other trauma (0.4%).
Suicide attempt as cause of SCI
Among the 2304 newly admitted cases of tSCI, suicide attempt was the cause of tSCI in 63 cases (2.7%). All suicide attempts were by jumping from height (windows, balconies, roofs, bridges and cliffs). The majority (52.4%) resulted in functionally complete paraplegia (para ABC), a further 34.9% had functionally incomplete SCI of any level (all Ds), 11.1% had low functionally complete tetraplegia (C5–8 ABC), only one (1.6%) had a high tetraplegia (C4 A) and there were no ventilator-dependent cases. The gender distribution was 55.6% male and 44.4% female.
Demographic and SCI characteristics of those injured in suicide attempts differed significantly from the rest of the sample, as shown in Table 1. Apart from the original suicide attempt, all other known mortality risk factors were lower in those who had attempted suicide when compared with those of other SCI aetiologies: younger age at injury (t-test, P=0.005); younger age at death (t-test, P=0.001); lower percentage of males (χ2-test, P=0.001), no ventilator-dependent cases and lower percentage of those with functionally complete tetraplegia (12.7% vs 34.3%, χ2-test, P=0.007). The subgroups did not differ significantly in time since injury (t-test, P>0.05).
Suicide as cause of death after SCI
At the end of the observation period (31 December 2014), 533 individuals (23.1% of the sample) had died and 7 (0.3%) were lost to follow-up (could not be traced by the Medical Research Information Service). Of the 63 persons whose SCI was due to suicide attempts, 21 (33.3%) died; and of the remaining 2234 successfully traced persons with different SCI aetiology, 512 (22.9%) died in the same time period (χ2-test, P=0.053). For 529 (99.2%) of the deceased, a valid death certificate was provided by the UK Office for National Statistics.
Suicide was the cause of death in 22 cases, which represented 4.2% of all known causes of death. In the suicide attempt group, suicide was the cause of death in 5 (23.8%) of the 21 deaths, and in the rest of the sample in 17 (3.3%) of the deaths (χ2-test, P=0.001; Table 1).
The unadjusted suicide rate among those whose injury was caused by a suicide attempt was 754 per 100 000 persons at risk per year compared with a rate of 73 per 100 000 for those injured in other ways, yielding a RR of 10.32 (95% CI=3.82–27.87). Aetiologic fraction among those whose injury was caused by a suicide attempt was 90.32% (95% CI=73.8–96.4%). Population aetiologic fraction was 20.52% (95% CI=2.53–38.52%).
Table 2 shows the multivariate logistic regression analysis for the overall mortality risk. After controlling for gender, current age, current calendar year, time since injury and neurologic group, persons whose injury was caused by an attempted suicide were 4.32 times more likely to die each year than those whose injury was due to other causes (95% CI=2.70–6.89; P<0.0001). There was no significant gender mortality risk difference (P=0.3189) and no significant trend in overall annual mortality risk throughout the study (P=0.9847). Annual risk of mortality increased by 8% with each year of age (P<0.0001), but decreased by 2% with each year after injury (P=0.0389). Injury severity was also significantly associated with overall annual risk of mortality (P<0.001 for all neurological groups relative to all AIS Ds).
Controlling for the same risk factors identified previously, a separate multivariate logistic regression analysis was performed for the death by suicide risk. Persons whose injury was caused by a suicide attempt were 9.46 times more likely to die by suicide than those whose injury resulted from other causes (95% CI=3.26–27.50; P<0.0001). This adjusted OR is only slightly reduced from the unadjusted RR of 10.32. The annual risk of suicide decreased by 8% per year during the study period, which was of borderline statistical significance (P=0.0618). There were no statistically significant differences in the annual likelihood of suicide for gender, current age, years since injury and injury level, likely due to the small number of suicides committed during the study (n=22).
Table 3 shows the differences among the deceased analysed by cause of death—deaths by suicide vs all other causes of death. Those who died by suicide were significantly younger at injury and at death (t-test, P=0.001), and had proportionally more paraplegic and functionally incomplete (all AIS Ds) lesions among them (χ2-test, P=0.012). They also had a shorter mean time since injury at death, but the difference was not quite statistically significant (t-test, P=0.057).
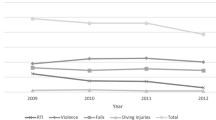
Five of the 22 (22.7%) individuals who died by suicide had incurred their SCI through a suicide attempt. Almost half of all suicides was by overdose (10/22), mainly psychotropic medication or opioid analgesics or the combination, and one by insulin overdose, three suicides were by hanging, three by fire, two by falling (jumping) from height, one by knife, one by firearms, one by drowning and one unspecified, but reported as suicide in the death certificate. Most suicides happened at home, one, caused by drowning, happened in a nursing home, and one person was brought to hospital after falling (jumping) from height, and died in hospital. A total of 10 (45.5%) of all 22 suicides occurred in the first 5 years post injury, 20 (91%) occurred in the first 10 years and only 2 more than 10 years post injury (Figure 1).
The age-standardised suicide mortality rate for the entire tSCI sample for the 1991–2014 observation period was 62.5 per 100 000 persons per year (95% CI=36.4–88.6). The general population age-standardised suicide mortality rate for England and Wales in 2014 was 12.2 per 100 000 persons per year. Because of the small number of suicides, it was not possible to calculate stable estimates of age-standardised suicide rates for neurologic subgroups, gender, length of time post injury or for those whose injury was caused by a suicide attempt.
Discussion
The aim of this study was to analyse suicide both as a cause of tSCI and as a cause of death after tSCI in a cohort of patients from two British spinal centres who survived the first post-injury year.
Suicide attempt was the cause of tSCI in 2.7% of all persons in our study, which is slightly above 1.62 and 1.96%3 previously found in the UK, but well within 0–6.8% reported by Kennedy and Garmon-Jones in their review article.1 Their review also found that suicide was the cause of death in between 4 and 11% of all deaths after SCI in the studies they reviewed, so our finding of suicides representing 4.2% of all deaths falls at the lower end of this range.
The same review found that up to 82% of those who acquired their SCI through a suicide attempt had psychological problems, and identified the presence of psychiatric disorders as the main risk factor associated with suicide. They also found that a previous suicide attempt was reported in between 23 and 64% of those who eventually died from suicide.1 In our sample, of the 22 people for whom suicide was the cause of death, 5 (22.7%) had acquired their SCI through a suicide attempt. According to a recent World Health Organisation publication, risk factors for suicide in the general population include mental disorder (such as depression, personality disorder, alcohol dependence and schizophrenia) and some physical illnesses (such as neurological disorders, cancer and HIV infection), but a previous suicide attempt was singled out as the most important risk factor for suicide.7 Our British mortality study, which includes individuals from the current study, did not include detailed comorbidities in its protocol, so we did not have complete mental health information for all the patients.4 However, suicide attempt could indicate a possible mental health problem, at least at the time of the attempt.
Our recent life expectancy study identified age, gender, SCI level and grade as significant risk factors for mortality after tSCI.8 In the current study, all of these mortality risk factors were lower in the suicide attempt group when compared with the rest of the sample. Still, the overall mortality was higher (borderline significant, P=0.053), and death by suicide was significantly higher (P=0.001), in persons whose tSCI was caused by an attempted suicide when compared with all other aetiologies. The mortality odds analyses showed that after adjusting for age, gender, injury severity, time since injury and calendar year of exposure, the annual risk of dying was more than four times higher, and the risk of dying by suicide was almost 10 times higher in those injured in a suicide attempt than in those with other tSCI aetiologies (both highly statistically significant, P<0.001). Moreover, 20.52% of all suicides after tSCI would be eliminated if no injuries were caused by suicide attempts, and 90.31% of successful suicides among those who previously attempted suicide were directly attributable to the previous suicide attempt.
All other things equal, the difference in annual risk of dying between those persons whose injury was caused by a suicide attempt and those who were injured by other causes (OR=4.32) was greater than the difference between those with a C1–4 ABC injury and those with an AIS D injury at any level (OR=3.85), and was also greater than the difference between a 20-year-old person and a 40-year-old person (OR=3.36) reported in our life expectancy paper.8 Therefore, persons whose injury was due to a suicide attempt will have substantially reduced life expectancy not entirely because of the increased risk of subsequent suicide. Other suicide mortality risk factors were similar to those previously identified (younger age, lower level of SCI and shorter time since injury).9, 10, 11, 12
As to the means of committing suicide, it has been suggested that this often depends on the availability and the ease of access to the means, as well as on the physical ability of people with SCI, particularly higher level SCI, to commit the act.1, 10 In the United States, for instance, firearms are used much more frequently than in Europe.9, 11, 12 Our finding of drug poisoning/overdose being the most frequent method was very similar to that of Hartkopp et al.11
This study also found that suicides after SCI tend to occur more in the early post-injury years, particularly in the first 10 years, and recede with time post injury, similar to findings from the USA SCI Model Systems.9, 12 This is probably why, in the current study, the proportion of suicides among all causes of death and the suicide mortality rates were higher than in our previous causes of death study.4 The longer 70-year observation period in the previous study resulted in longer mean time since injury and lower suicide mortality rates for the same calendar years: 50.2 per 100 000 persons at risk per year for 1990–2004 and 33.0 per 100 000 persons at risk per year for 2005–2014 periods when compared with the rate of 62.5 per 100 000 persons at risk per year for 1991–2014 period in the current study. Compared with the general population of England and Wales in 2014, the suicide mortality rate after tSCI in this study was just over 5 times higher, and in our 70-year study 3–4 times higher.
High suicide mortality rate after SCI suggests that in addition to psychological/psychiatric assessment and intervention, which patients get during their initial rehabilitation, continued attention is warranted after SCI. This particularly applies to the early post-injury years, and to those who were injured by suicide attempt.
Limitations
Seven individuals were lost to follow-up. Four of the deceased did not have a valid death certificate.
Relatively small suicide numbers did not allow more detailed subgroup analyses.
Lack of information on mental health before and after injury was due to the original British mortality study methodology.
Psychological reasons behind suicide were not the topic of this manuscript, but would make an interesting and informative separate study.
Conclusions
Suicide attempt was the cause of tSCI in 2.7% of cases in the sample of the first post-injury year survivors. Suicide was the cause of death in 4.2% of all deaths, with 91% of the suicide deaths occurring in the first 10 years post injury. The age-standardised suicide mortality rate after tSCI was 62.5 per 100 000 persons per year, five times higher than the general population suicide rate for England and Wales in 2014 (12.2 per 100 000 persons per year). Overall mortality and death by suicide were significantly higher in persons whose tSCI was caused by an attempted suicide compared with the rest of the sample. Continued psychological attention is warranted after SCI, particularly in the early post-injury years, and especially to those who were injured by suicide attempt.
Data archiving
There were no data to deposit.
References
Kennedy P, Garmon-Jones L . Self-harm and suicide before and after spinal cord injury: a systematic review. Spinal Cord 2017; 55: 2–7.
Kennedy P, Rogers B, Speer S, Frankel H . Spinal cord injuries and attempted suicide: a retrospective review. Spinal Cord 1999; 37: 847–852.
Anderson J, Allan DB . Vertebral fracture secondary to suicide attempt: demographics and patient outcome in a Scottish spinal rehabilitation unit. J Spinal Cord Med 2011; 34: 380–387.
Savic G, DeVivo MJ, Frankel HL, Jamous MA, Soni B, Charlifue S . Causes of death after traumatic spinal cord injury—a 70 year British study. Spinal Cord 2017; doi:10.1038/sc.2017.64.
American Spinal Injury AssociationInternational Standards for Neurological Classification of Spinal Cord Injury, revised 2011, updated 2015. American Spinal Injury Association: Atlanta, GA, USA.
Office for National Statistics (ONS). Statistical bulletin. Suicides in the United Kingdom: 2014 Registrations. ONS: Newport, UK, 2016. Available at https://www.ons.gov.uk/peoplepopulationandcommunity/birthsdeathsandmarriages/deaths/bulletins/suicidesintheunitedkingdom/2014registrations. Accessed on 03 March 2017.
World Health Organisation (WHO)Preventing suicide: a global imperative. WHO: Geneva, Switzerland, 2014. Available at http://www.who.int/mental_health/suicide-prevention/world_report_2014/en/. Accessed on 16 March 2017.
Savic G, DeVivo MJ, Frankel HL, Jamous MA, Soni B, Charlifue S . Long term survival after traumatic spinal cord injury—a 70 year British study. Spinal Cord 2017; 55: 651–658.
Cao Y, Massaro JF, Krause JS, Chen Y, DeVivo MJ . Suicide mortality after spinal cord injury in the United States: injury cohorts analysis. Arch Phys Med Rehabil 2014; 95: 230–235.
Soden RJ, Walsh J, Middleton JW, Craven ML, Rutkowski SB, Yeo JD . Causes of death after spinal cord injury. Spinal Cord 2000; 38: 604–610.
Hartkopp A, Brønnum-Hansen H, Seidenschnur AM, Biering-Sorensen F . Suicide in a spinal cord injured population: its relation to functional status. Arch Phys Med Rehabil 1998; 79: 1356–1361.
DeVivo MJ, Black KJ, Richards JS, Stover SL . Suicide following spinal cord injury. Paraplegia 1991; 29: 620–627.
Acknowledgements
This study was financially supported by the Buckinghamshire Healthcare NHS Trust Charitable Spinal Fund and the Ann Masson Legacy for Spinal Research Fund, UK. We thank the Medical Records staff at Stoke Mandeville and Southport Spinal Centres, and especially Mrs Pauline Bateman, for their help with medical notes retrieval.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Savic, G., DeVivo, M., Frankel, H. et al. Suicide and traumatic spinal cord injury—a cohort study. Spinal Cord 56, 2–6 (2018). https://doi.org/10.1038/sc.2017.98
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sc.2017.98