Abstract
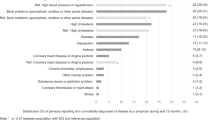
Out of a regional traumatic spinal cord injury population consisting of 379 individuals, 353 (93.1%) participated in the present study. Subjects were individually interviewed using semi-structured protocols. In addition, previous medical records were available for over 96% of subjects, and were used in all these cases to minimise recall bias. Cause of injury, prevalence of present medical symptoms and occurrence of medical complications in the post-acute, post-discharge phase were recorded. Neurological classification was verified by physical examination according to ASIA/IMSOP standards. Many subjects had experienced complications since discharge from initial hospitalisation, especially urinary tract infections, decubitus ulcers, urolithiasis, and neurological deterioration. Prevalence of medical symptoms was also high. More than 41% of subjects with spastic paralysis reported excessive spasticity to be associated with additional functional impairment and/or pain. Almost two-thirds of subjects reported significant pain, with a predominance of neurogenic-type pain. Bladder and bowel dysfunction were each rated by nearly 41% of subjects as a moderate to severe life problem. As expected, sexual dysfunction was also commonly reported. Prevalence of reported symptoms by general systems review was high, particularly fatigue, constipation, ankle oedema, joint and muscle problems, and disturbed sleep. However, lack of adequate normative data precludes comparison with the general population. The frequent occurrence of reported medical problems and complications support advocacy of comprehensive, life-long care for SCI patients. The commonly reported problems of neurogenic pain and neurological deterioration, in particular, require more attention, as these symptoms are not seldom ominous, either by virtue of their impact on quality of life, or because of underlying pathology.
Similar content being viewed by others
Article PDF
References
Guttmann L . Spinal Cord Injuries: Comprehensive Management and Research. 2nd edn. Blackwell Scientific Publications: Oxford, 1976.
Stover S L . Spinal Cord Injury: The Facts and Figures. University of Alabama at Birmingham: Birmingham, AL, 1986.
Stover S L, Fine P R . The epidemiology and economics of spinal cord injury. Paraplegia 1987; 25: 225–8.
Whiteneck G G (ed). Aging with Spinal Cord Injury. Demos Publications: New York, 1992.
Whiteneck G G et al. Mortality, morbidity, and psychosocial outcomes of persons spinal cord injured more than 20 years ago. Paraplegia 1992; 30: 617–30.
Parsons K C, Lammertse D P . Rehabilitation in spinal cord disorders. 1. Epidemiology, prevention, and system of care of spinal cord disorders. Arch Phys Med Rehabil 1991; 72: S293–4.
Burney R E, Maio R F, Maynard F, Karunas R . Incidence, characteristics, and outcome of spinal cord injury at trauma centers in North America. Arch Surg 1993; 128: 596–9.
Dialogdata Information Systems Ltd, Stockholm, Sweden. INREGIA Institute for Regional Analysis, Sweden, 1991.
Levi R, Hultling C, Westgren N . A computer assisted follow-up system for spinal cord injury patients. Paraplegia 1994; 32: 736–742.
Ditunno J F, Young W, Donovan W H, Creasey G . The inter national standards booklet of neurological and functional classification of spinal cord injury. Paraplegia 1994; 32: 70–80.
Klassifikation Av Sjukdomar, Systematisk Forteckning (Inter national Classification of Diseases, Ninth Revision ICD-9). Swedish version, 1987.
Edgar R, Quail P . Progressive post-traumatic cystic and non-cystic myelopathy. Br J Neurosurg 1994; 8: 7–22.
Falcone S et al. Progressive posttraumatic myelomalacic myelo pathy: imaging and clinical features. Am J Neuroradiol 1994; 15: 747–54.
Fenollosa P et al. Chronic pain in the spinal cord injured: Statistical approach and pharmacological treatment. Paraplegia 1993; 31: 722–9.
Svendsen L, Drewes A M, Biering-Sorensen F, Lonnberg F . Chronic pain after spinal cord injury—a descriptive study. Ugeskr Laeger 1993; 155: 3118–22.
Mariano A J . Chronic pain and spinal cord injury. Clin J Pain 1992; 8: 87–92.
Balazy T E . Clinical management of chronic pain in spinal cord injury. Clin J Pain 1992; 8: 102–10.
Kennedy R H . A new viewpoint toward spinal cord injuries. Ann Surg 1946; 124: 1057–1065.
Botetrel E H, Callaghan J C, Jousse A T . Pain in paraplegia: Clinical management and surgical treatment. Proc R Soc Med 1953; 47: 281–288.
Nepomuceno C, Fine P R, Richards J S . Pain in patients with spinal cord injury. Arch Phys Med Rehabil 1979; 60: 605–609.
Rapaport M H . Chronic pain and posttraumatic stress disorder. Am J Psychiatry 1987; 144: 120.
Siösteen A . Adjustment to spinal cord injury: A clinical and experimental study on quality of life, sexuality and fertility. (Doctoral thesis) Departments of Neurosurgery, Neurology and Medicine I/Health Care Research Unit, University of Göteborg, Göteborg, Sweden, 1989.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Levi, R., Hultling, C., Nash, M. et al. The Stockholm spinal cord injury study: 1. Medical problems in a regional SCI population. Spinal Cord 33, 308–315 (1995). https://doi.org/10.1038/sc.1995.70
Issue Date:
DOI: https://doi.org/10.1038/sc.1995.70
Keywords
This article is cited by
-
Practical approaches of PULSE Racing in training their athlete for the Cybathlon Global Edition Functional Electrical Stimulation bike race: a case report
Journal of NeuroEngineering and Rehabilitation (2023)
-
Long-term physical therapy for neuropathic pain after cervical spinal cord injury and resting state electroencephalography: a case report
Spinal Cord Series and Cases (2022)
-
Diffusional kurtosis imaging as a possible prognostic marker of cervical incomplete spinal cord injury outcome: a prospective pilot study
Acta Neurochirurgica (2022)
-
A review of spinal cord perfusion pressure guided interventions in traumatic spinal cord injury
European Spine Journal (2021)
-
Neural pathways for colorectal control, relevance to spinal cord injury and treatment: a narrative review
Spinal Cord (2018)