Abstract
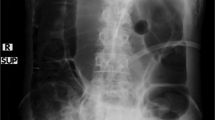
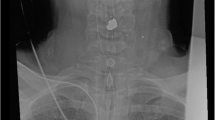
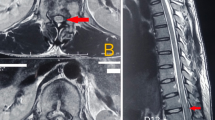
Patients sustaining an injury to the cervical spine at C3/4 level, with extensive cord damage, are difficult to manage. The injury is associated with a high mortality. The respiratory complications, including those associated with tracheostomy and intermittent-positive-pressure ventilation, are well recognised. The initial ileus and its management is also well documented. This report describes the development of acute gastric dilatation occurring 4 weeks after injury. The condition is particularly serious as many complications may have been overcome by this time resulting in a false sense of security. Two case histories are described. It is suggested that to a variable degree this complication probably occurs frequently in these patients. The aetiology of the acute gastric dilatation is discussed and recommendations are made (based on experience with one of the cases described), which may reasonably be expected to minimise the development and progress of the condition.
Similar content being viewed by others
Article PDF
References
Bennett, A & Stockley, H L (1975). The intrinsic innervation of the human alimentary tract and its relation to function. Gut, 16, 443–453.
Birkhahn, J, Joachims, H Z & Kaufman, T (1978). The problem of aerophagy. Anaesthesia, 33, 611–612.
Guttmann, Prof Sir Ludwig (1973). Spinal Cord Injuries—Comprehensive Management & Research. Blackwell Scientific Publications.
Salt, W & Schenker, S (1976). Amylase, its clinical significance: A review of the literature. Medicine, 55, No. 4, 269–289.
Wells, C, Rawlinson, K, Tinckler, L, Jones, H & Saunders, J (1961). Ileus & post-operative intestinal motility. Lancet, July 15, 136.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Sutton, R., Macphail, I., Bentley, R. et al. Acute gastric dilatation as a relatively late complication of tetraplegia due to very high cervical cord injury. Spinal Cord 19, 17–19 (1981). https://doi.org/10.1038/sc.1981.5
Issue Date:
DOI: https://doi.org/10.1038/sc.1981.5