Abstract
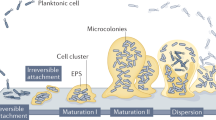
Biofilms have conventionally been perceived as dense bacterial masses on surfaces, following the five-step model of development. Initial biofilm research focused on surface-attached formations, but detached aggregates have received increasing attention in the past decade due to their pivotal role in chronic infections. Understanding their nature sparked fervent discussions in biofilm conferences and scientific literature. This review consolidates current insights on non-attached aggregates, offering examples of their occurrence in nature and diseases. We discuss their formation and dispersion mechanisms, resilience to antibiotics and immune-responses, drawing parallels to surface-attached biofilms. Moreover, we outline available in vitro models for studying non-attached aggregates.
Similar content being viewed by others
Introduction
The surface attached biofilm, as drawn by Stoodley et al.1 and reprinted countless times in theses, reports, and journal articles ever since, is well studied due to its conspicuous nature, ease of handling and phenotype that is in stark contrast to the planktonic lifestyle. Non-attached aggregates have not received the same attention although they have regularly been described in the literature. For example, Pasteur described how floating aggregated bacteria could spoil wine production in 18642. And aggregated bacteria have been described in freshwater and marine environments for close to a century3,4. In 1977, Høiby et al. described so-called heaps of bacteria surrounded by inflammation in chronic pneumonia patients with cystic fibrosis (CF)5, and the following year Bill Costerton published his defining biofilm theory6. In the following decades surface attached biofilms were the focus of numerous studies, and it is only in the last decade that the biology of non-attached aggregates has been intensively studied. Cai recently contributed a review describing non-attached microbial aggregates with focus mostly on microbial ecology aspects7. Here we review our current knowledge of non-attached aggregates focusing on molecular- and microenvironmental aspects with an emphasis on aggregates found in human disease.
Non-attached aggregates are prevalent in nature and disease
In the laboratory, experimental microbiologists will occasionally observe macroscopically visible aggregates in liquid batch cultures. In addition to the visible aggregates, Schleheck et al. described that a considerable part of the biomass in a P. aeruginosa batch culture is bound in microscopic, suspended aggregates ranging from 10 – 400 µm in diameter8, and not only confined to the air-liquid interface as e.g., pellicles9. Moreover, Staphylococcus aureus has been reported to start aggregating in the early exponential phase of growth in batch cultures, resulting in more than 90% of the population being bound in aggregates when they reach the stationary phase10. Such aggregates can have a profound impact on e.g., growth rate and antibiotic tolerance in in vitro experiments11,12.
Flemming et al. compiled a meta-analysis on the occurrence of biofilms in different habitats and reported the presence of aggregates in many environmental habitats13. A prominent example of non-attached aggregates in nature is the pelagic aggregates, often referred to as marine- or lake snow. They have been widely described as a mode for bacteria to colonize the open water column14,15. These aggregates are composed of microbial communities held together by self-produced extracellular polysaccharides or as part of inorganic and organic particles such as clay or sand minerals, fecal pellets, or organic debris. The free-floating aggregated phenotype in limnic and marine environments may confer many of the same attributes to bacteria as often ascribed to classical surface biofilm. E.g., bacteria can attain protection against grazing and live in a stable chemical environment. Further, bacteria bound in pelagic aggregates have been shown to contain elevated amounts of several quorum-sensing related molecules such as N-acyl homoserine lactones compared to their single-celled counterparts16,17. The size of the pelagic aggregates is typically in the range of 500 µm to centimeters.
Microbial aggregates are also prevalent in infections and Bjarnsholt et al.18 compiled a meta-analysis on the distribution of aggregates in chronic infections, and their characteristic sizes. They found non-attached aggregates with a range of 5 to 200 µm in diameter to be dominant in most chronic infections, such as CF-related infections, chronic wounds, otitis media, and chronic osteomyelitis18,19,20,21 (Fig. 1). However, Kolpen et al. recently identified non-attached aggregates in expectorate from patients admitted to the hospital with acute pneumonia, suggesting that biofilm aggregates are not only limited to chronic infections22. The aggregates contained exopolysaccharides and exhibited similar sizes as aggregates found in chronic pneumonia infection in CF or COPD patients. Similar results were recently found in a meta-analysis that revealed the presence of biofilms in acute wounds23. The use of advanced microscopy techniques, such a confocal laser scanning microscopy and electron microscopy, have revealed the structure and positioning of bacteria in several chronic bacterial infections24. A common denominator for many of these is that the bacteria are found positioned in small aggregates surrounded by polymer-rich host secretions and large amounts of inflammatory cells19,25,26 (Fig. 2). These aggregates do not appear to be intimately associated with intact epithelia or other eukaryotic surfaces27.
a, b Biofilm aggregates in debridement material from chronic wounds stained red with PNA-FISH probes. White arrows indicate biofilm aggregates, yellow arrows indicate the surface of the wound. Biofilm aggregates found in sputum from patients diagnosed with either (c) community acquired pneumonia or (d) cystic fibrosis. Red represents cells stained with bacteria specific PNA-FISH. e, f Specimens from chronic otitis media. e Aggregates of Staphylococcus aureus stained with specific PNA-FISH probes (green-yellow) and (f) aggregate stained with a universal bacteria PNA-FISH probe indicated with white arrows. In all panels, host cells were stained blue with DAPI. Adapted with permission from21,22,79.
a HE stained explanted lung tissue from a patient with cystic fibrosis. Image focused on a bronchial lumen. Green arrow indicates a non-attached bacterial aggregate, and the red arrow indicates a host immune cell associated with the aggregates. The unit of the scalebar refers to µm. b Schematic drawing of chronic biofilm infection in CF lungs. Bacteria grows as small non-attached aggregates (green cells), in obstructed bronchia filled with mucus surrounded by a multitude of innate immune cells (pink cells). The aggregates have been found to be unassociated with the epithelial lining (blue cells)27. c The neighboring slide of the image A, stained for P. aeruginosa with specific PNA-FISH probes and counterstained with blue DAPI. The green arrow indicate a red stained P. aeruginosa aggregate and red arrow shows the DAPI stained nucleus of an immune cell. The unit of the scalebar refers to µm. d aggregates of many infections have been found to grow slowly due to limited availability of oxygen due to high consumption from immune cells. a, c are adapted from81 with permission.
Mechanisms of aggregate formation
Microbial aggregates are known to be formed by three different mechanisms: (1) due to restricted motility in high-density gels, (2) by depletion aggregation in polymer-rich environments, and (3) by bridging aggregation caused by bacterial extracellular polymers (Fig. 3).
a–c Aggregate formation due to immobilization in viscous materials. a Single cells are immobilized in a viscous gel. b Over time the single cell proliferates to an immobilized microaggregate. c As the aggregate attains a certain size, its expansion becomes limited due to space restriction and/or resource stratification. d–f Depletion aggregation in polymer-rich environments. d Single bacterial cells found in polymer rich environment. e Cells in proximity of each other will attract due to entropy generated by osmotic imbalance (red arrows) as polymers move out from between the cells (blue arrows). f Depletion aggregation creates the distinct fence pattern aggregate formation. g–i Bridging aggregation. g Preformed aggregates (green cells) are in a biofilm state where they produce extracellular polymers. h Single cells (or other aggregates) are recruited to the aggregate, facilitated by the sticky polymers around the aggregates. i Over time the aggregates increase in size through growth, continuous recruitment, and incorporation of single cells and/or other aggregates.
Staudinger et al. demonstrated that P. aeruginosa can form aggregates in high density gels due to restricted motility28. In addition to wild type cells, aggregates were formed by mutants that were deficient in synthesis of exopolysaccharides and pili, indicating that aggregate formation does not require functions needed for development of surface associated biofilms. In addition, Pabst et al. demonstrated that S. aureus can form aggregates in an agar gel system29. These findings are highly relevant in the context of infections since high density conditions caused by polymer-rich host secretions are thought to be predominant at infectious sites28.
Secor et al. reported a series of in vitro experiments indicating that polymers that are abundant at chronic infection sites can cause P. aeruginosa cells to aggregate by a so-called depletion aggregation mechanism30. Depletion aggregation is mediated by entropic forces between like-charged polymers and the bacteria, and therefore it does not require biofilm formation functions such as self-produced exopolysaccharides.
Examples of the formation of microbial aggregates via bridging aggregation include a study by Kragh et al. who reported that P. aeruginosa aggregates need at least the two well-described exopolysaccharides Pel and Psl to maintain the coherence of aggregates in suspension11. In addition, the adhesin CdrA has been shown to be involved in the formation and maintenance of P. aeruginosa aggregates in liquid culture31,32.
In addition to the three described mechanisms of aggregate formation, it is possible that some non-attached aggregates can originate from surface attached biofilms due to shedding or break-off of a part of the biofilm.
Role of the extracellular matrix of aggregates
The extracellular matrix of non-attached P. aeruginosa aggregates has been shown to be strikingly similar to that of surface attached biofilms33. In addition, self-assembled Staphylococcus epidermidis aggregates in liquid culture had increased expression of proteins related to extracellular matrix production, like polysaccharides and eDNA secretion34. Moreover, in vitro grown S. aureus aggregates were shown to contain substantial amounts of the polysaccharide intercellular adhesin (PIA), well-known for its involvement in the establishment of surface-bound biofilm10.
In suspension, the formation of P. aeruginosa aggregates has been linked to the active recruitment of surrounding single cells to a greater extent than clonal growth within the aggregates11. This recruitment process was meditated through the active secretion of especially Psl. It was speculated that Psl could act as an adhesin enabling the immobilization of planktonic cells on the outside of the aggregate.
Staudinger et al. demonstrated that bacteria can form aggregates independent of matrix components if they grow suspended in gel material that restrict their motility, and this process was suggested to play a role in the formation of aggregates at infectious sites28. Likewise, Secor et al. suggested that matrix-independent depletion aggregation plays a role in the formation of bacterial aggregates in chronic infections30. However, Jennings et al. provided evidence that depletion aggregation does not play a role for the formation of P. aeruginosa aggregates in the CF lung35. This was based on the fact that aggregates formed by depletion aggregation are organized differently than aggregates formed by bridging aggregation. The aggregates found in CF lung sputum had the organization typical of aggregates formed by bridging aggregation, indicating that their formation is mediated by the bacterial extracellular matrix35.
During the course of CF lung infection there is a strong selection for P. aeruginosa mutants that overproduce biofilm matrix components. Overproduction of alginate by P. aeruginosa mucA mutants enable the bacteria to develop persistent infections in the lungs of CF patients5,36. Overproduction of Psl and Pel by P. aeruginosa mutants such as wspF and yfiR also confer a benefit to the bacteria during CF lung infection37,38,39. Similarly, P. aeruginosa wspF mutants overproducing exopolysaccharide developed rapidly in a porcine burn wound model40. Overproduction of these polysaccharide biofilm matrix components may be important for the formation of aggregates at the infectious sites.
Whitchurch et al. reported that eDNA functions as a matrix component in surface-associated P. aeruginosa biofilms grown in vitro41. Investigations of biofilm development in the presence of non-bacterial DNA suggested that P. aeruginosa can incorporate the foreign DNA as an integral part of the extracellular matrix42,43,44. Moreover, the presence of neutrophil immune cells was shown to stimulate P. aeruginosa biofilm formation through release of eDNA that was incorporated in the biofilms44. Alhede et al. showed that the majority of the eDNA surrounding the biofilm aggregates in murine infections and ex vivo lung tissue come from lysed host immune cells45 (Fig. 4). Under in vitro conditions the secretion of eDNA has been shown to be controlled by the Las quorum sensing system through the PQS system46. This Las regulation has primarily been shown in mature surface attached biofilms grown in vitro, so whether this regulation is operating in non-attached aggregates is not known.
a Image of infected murine tissue. Both immune cells and bacteria can be seen as green cells. Eukaryotic DNA was stained purple with antibodies. b Murine immune cells can be seen as large green cells surrounding a large biofilm aggregate. c Antibody stained eDNA can be seen surrounding the biofilm aggregate. Scalebar in (a–c) is 10 µm. d Schematic drawing of the proposed mechanism behind the large amount of eukaryotic eDNA around biofilms. Leukocytes, in this case PMNs, are lysed by bacteria in the aggregates, resulting in expulsion of DNA from the lysed PMNs. Adapted from45 with permission.
Proteins can also play a role as extracellular matrix components of non-attached aggregates. For example, Escherichia coli is prone to aggregation mediated by the adhesin termed Antigen 4347,48,49. Ag43-dependent aggregates exhibit specific properties, including persistence and virulence of uropathogenic E. coli in the mouse bladder48.
Lastly, the host immunometabolism may influence the expression of EPS. For example, it was recently shown that P. aeruginosa and S. aureus can stimulate itaconate production by the host which can induce increased bacterial EPS production50,51. However, the current knowledge on this phenomenon is limited and whether the balance between non-attached vs. surface attached biofilm is affected by this is not known.
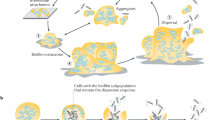
Mechanisms of aggregate dispersal
As described above, aggregates have been shown to form through several active or passive mechanisms. Besides de novo formation of aggregates, non-attached aggregates can also originate by detaching from other aggregates or surface-attached biofilms. Hydrodynamic stress and shear forces can play a significant role in the detachment of bacterial aggregates from biofilms. Studies have shown that the strength of the biofilm matrix and the size and shape of the aggregates can affect their susceptibility to hydrodynamic stress52,53. In other instances, the presence of extracellular matrix-degrading enzymes can also contribute to detachment from surface-attached biofilm as it has been shown for P. putida during starvation54. The upstream detachment of aggregates can provide an advantage for subsequent downstream surface colonization as an aggregate may provide both instant protection and a growth advantage in the initial establishment steps compared to the single-cell attachment to a surface12.
There is some evidence for single-cell dispersal from non-attached aggregates upon starvation as well. In a study by Schleheck et al., it was found that P. aeruginosa preferentially grows as aggregates in liquid batch cultures8. However, upon carbon, nitrogen, or oxygen starvation, the floating aggregates dispersed into single cells8. These findings suggest that P. aeruginosa non-attached aggregates show similar behavior to what has been reported for P. putida surface-associated biofilms54. Interestingly, we observed a decrease in aggregated biomass fraction of P. aeruginosa in chemostatic cultures after 10 days but since these cultures are not limited in electron donors or -acceptors these results contradict the starvation induced dispersal11.
During the last decade it has become evident that many bacteria species employ c-di-GMP signaling to regulate biofilm formation55. Diguanylate cyclase enzymes catalyze formation of the c-di-GMP molecule, whereas c-di-GMP phosphodiesterase enzymes catalyze degradation of c-di-GMP in the bacteria. An elevated cellular level of c-di-GMP upregulates matrix production and drives planktonic bacteria to form biofilms, whereas a reduction in the c-di-GMP level induces dispersal of biofilm bacteria into the planktonic mode of life. In addition to their catalytic domains many of the diguanylate cyclases and phosphodiesterase enzymes have regulatory domains through which they are thought to regulate the bacterial life-style (planktonic versus biofilm) in response to environmental cues. A decrease in the level of c-di-GMP has been shown to result in dispersion of surface-attached biofilms in both in vitro systems and murine biofilm infection models56,57,58,59. However, it is not known whether this mechanism is relevant for dispersion of non-attached aggregates.
Quorum sensing has also been associated with regulation of biofilm dispersal. Changes in the acyl-homoserine lactone levels in P. aeruginosa, Serratia marcescens and Vibrio vulnificus have all been shown to induce dispersal of surface-attached biofilm60,61,62. However, it is not known if this correlation is found in non-attached aggregates. In some infections, bacteria are trapped in highly viscous host material, e.g., CF sputum or wound slough, and we speculate that aggregates that are trapped in such material will likely not be able to disperse via regained flagellar motility.
These studies suggest that the dispersal of bacterial biofilm aggregates is a complex process which is influenced by multiple factors, although more data focusing specifically on biofilm dispersal of the aggregate phenotype are needed. The availability of nutrients, the presence of signaling molecules, and the mechanical forces upon the biofilm aggregates may all play a role in the dispersal of biofilm aggregates.
The aggregate microenvironment
The growth of individual aggregates is determined by environmental factors surrounding the aggregates (Fig. 5a). In viscous environments, bacteria will largely be constrained to their three dimensional position and thus, exchange of metabolic substrate and by-products will follow reaction-diffusion equations. These conditions have been thoroughly reviewed elsewhere63,64,65. But briefly, the occurrence of gradients in aggregates are determined by the reaction rate, diffusion characteristics and local boundary conditions. Example calculations are provided in Lichtenberg et al. (2022) that shows that even small aggregates can have internal hypoxic zones65. This has also been shown experimentally, where aggregates of P. aeruginosa with a radius of only 24 µm showed diminished internal O2 concentrations66. In the study by Wessel et al., gradients inside aggregates were thus seen even at fully oxygenated external conditions but in many environments the O2 concentration will not be at saturation. Hypoxic zones have, for example, been demonstrated in the mucus in lungs of people with cystic fibrosis (CF) as well as in the slough of chronic wounds27,67. Dynamics of the external environment influence the microenvironment of single aggregates and thus their boundary conditions. E.g., the recruitment and activation of PMNs in sputum from CF patients, will lead to local exhaustion of O2 due to production of their oxidative burst68. This releases reactive oxygen radicals that also follow reaction diffusion equation into aggregates63. The microenvironment surrounding aggregates is thus highly dynamic and their growth is not in the slightest restricted to the examples mentioned here but will most likely include several growth factors (e.g., carbon sources, electron acceptors, iron etc.), pH, and external stressors (e.g., antibiotics, ROS, secondary metabolites etc.). Examples of such dynamics has been shown for S. aureus where the transition to anaerobiosis was demonstrated by visualizing the localized expression of the lactate dehydrogenase gene via a ldh::gfp reporter strain29.
Green-red color scale depicts physiological gradients whereas red-blue color scale depicts an environmental gradient. a Non-attached aggregates will experience three dimensional gradient formation in the direction from their surface toward the center (or opposite e.g., for metabolic by-products). This can create a stratification in growth leading to different sub-populations. b For surface attached biofilms, the same diffusion phenomena will occur and will also depend on the three-dimensional structure. Again, sub-populations can form due to gradient formations. c Conceptual figure showing the influence of the immediate microenvironment on biofilm physiological state. Aggregates in the top-right side are close to the external environment and are distant from highly O2-consuming neutrophils. Aggregates in the lower-left are surrounded by neutrophils that creates an anoxic microenvironment.
Non-attached aggregates and surface bound biofilms have the potential to experience similar microenvironments as both are limited by diffusion64. Bacteria inside simple flat biofilms that are attached to a solid surface, rely on diffusion from above the biofilm, while the surfaces of non-attached aggregates are more exposed in three dimensions. However, more complex diffusion patterns can occur in structured surface attached biofilms showing three-dimensional organization, such as flow cell mushroom structures (Fig. 5b). The same applies for the export of metabolic waste products. The gradient formation of metabolic products can lead to a heterogenic distribution of physiological states within the same biofilm29,69,70 which can lead to different subpopulations e.g., displaying different susceptibilities to antibiotics71,72,73. It is important to recognize the scale at which these things are discussed as emphasized by Kirketerp-Møller et al. that described the so-called Zone model that dictates that every single bacterium reacts to its own microenvironment74. In infections, bacterial physiology will thus be more complex and be determined by the immediate microenvironment which could be distinct even between neighboring aggregates (Fig. 5c).
The ability of aggregates to tolerate antibiotics and evade immune responses
The increased tolerance toward antibiotic treatment and immune responses remains one of the defining features of surface attached biofilms75, and the available evidence suggest that these important traits are also common for non-attached aggregates.
For example, Alhede et al. found that P. aeruginosa aggregates grown in liquid media, exhibited tobramycin and colistin tolerance, as well as resilience towards neutrophils, comparable to that found for surface attached biofilms33. Similarly, non-attached aggregates of S. aureus have been shown to be highly tolerant towards both kanamycin, ciprofloxacin, erythromycin, and vancomycin10. Moreover, Pabst et al. demonstrated that gel-entrapped S. aureus aggregates were much more tolerant towards oxacillin, minocycline, and ciprofloxacin than planktonic cells29.
P. aeruginosa mutants that were deficient in the synthesis of Psl, Pel and alginate were shown to form aggregates in high density (0.8%) agar gels, and the bacteria in these aggregates were found to be more antibiotic tolerant than the corresponding strains growing dispersed in low density (0.2%) agar gels28. These results suggested that the biofilm matrix may not be necessary for the antibiotic tolerance of aggregates. However, subsequently it was reported that P. aeruginosa mucA aggregates (overproducing alginate) and P. aeruginosa ΔwspF aggregates (overproducing Pel and Psl) displayed increased tolerance towards tobramycin and ciprofloxacin compared to P. aeruginosa wild-type aggregates76. Recently, however, it was found that overproduction of exopolysaccharides confers a high metabolic burden on the bacteria, and results in subsequent low metabolic activity if the bacteria are situated in a nutrient/oxygen limited environment77. Thus, a difference in antibiotic tolerance between exopolysaccharide-overproducing aggregates and wild-type aggregates could be due to differences in the metabolic state of the bacteria. Accordingly, using an experimental setup where P. aeruginosa aggregates were cultivated under more homogeneous oxygen conditions than in the former study78, found that aggregates formed by alginate-overproducing mutants showed increased tolerance to tobramycin and meropenem, but not increased tolerance to ciprofloxacin. Furthermore, it was found that mutants that overproduce Pel or Psl did not display increased tolerance to tobramycin, meropenem and ciprofloxacin in comparison to wild-type aggregates78,37,38,39.
Since the first in-depth investigation of the phenotype of biofilms in chronic infections, the high local activity of inflammatory cells surrounding the biofilm aggregates has been apparent. However, aggregates and the inflammatory cells appear spatially separated, indicating that immune cells are unable to infiltrate the aggregates79,80,81 (Fig. 10a, b). The size of the aggregates appears to correlate with their ability to evade phagocytosis by innate immune cells. In liquid culture it was shown that aggregates with a diameter of more than 5 µm formed by S. epidermidis, S. aureus, Escherichia coli, and P. aeruginosa were less efficiently phagocytosed by neutrophils than smaller aggregates82. Similarly, it was shown that only surface attached aggregates with an area less than 50 µm2 (corresponding to a diameter of ~8 µm, assuming round aggregates) were efficiently cleared83. Thus, the size of aggregates appears to be a major determinant of the efficiency of clearance by immune cells. Besides the passive inhibition of phagocytosis due to size, P. aeruginosa in non-attached aggregates has been shown to actively kill PMNs through the secretion of the quorum sensing regulated rhamnolipid33. This biosurfactant has previously been attributed to surface-attached biofilms as the ones found in flow cells where it is produced in a density dependent quorum sensing-regulated manner84,85,86.
Resemblance of non-attached aggregates to surface-attached biofilms
A central question is to what extent the bacteria in non-attached aggregates share phenotypic traits with the bacteria in surface-attached biofilms (Fig. 6)?
The consensus on what defines a biofilm is that it consists of a community of microbes living enclosed in extracellular matrix consisting of polysaccharides, proteins, lipids, and eDNA13. The matrix and stratified metabolic activity provide the microbes with an increased tolerance against antibiotics and other environmental stressors compared to planktonic cells and protect them against host immune responses75.
As discussed above, it is currently not clear whether the extracellular matrix is required for microbial aggregate formation in suspension and under conditions found at infectious sites11,31,32,35, as mechanisms of aggregate formation independent of bacterial matrix products also exists28,30. Although wild type aggregates and aggregates formed by mutants unable to produce matrix appear to be equally tolerant to antibiotics28,30, aggregates formed by mutants that overproduce matrix components appear to be more tolerant toward antibiotics than wild type aggregates76. The occurrence of stratified metabolic activity in microbial aggregates is not well explored but recent developments in single cell transcriptomics have suggested diverse physiological states within the same biofilm29,69,70 and between aggregates trapped in a secondary matrix29,69,70,73. Our knowledge from investigations of surface attached biofilms87,88 suggests that stratified metabolic activity occurs in aggregates despite their smaller physical dimensions.
Studies of surface associated P. aeruginosa biofilms have shown that the bacterial c-di-GMP level increases dramatically upon surface contact55,89,90. Using a fluorescent c-di-GMP reporter, based on a fusion between the c-di-GMP-regulated cdrA promoter and gfp91, we have found that the bacteria in agar-embedded P. aeruginosa aggregates have elevated levels of c-di-GMP compared to bacteria in planktonic culture. This is a strong indication that bacteria in non-attached aggregates share phenotypic traits with the bacteria in surface-attached biofilms, although these data are currently unpublished.
A low metabolic activity of the bacteria is a hallmark of biofilms and contributes substantially to the antibiotic tolerance displayed by biofilms75. Using a microcalorimetric approach, we have shown that c-di-GMP signaling is a major determinant of the metabolic activity of P. aeruginosa bacteria in planktonic culture, surface attached biofilms and aggregates77. The high c-di-GMP content of bacteria in biofilms forces them to rapidly spend a large amount of energy on the formation of extracellular matrix products, resulting in subsequent low metabolic activity. This suggests that the low metabolic activity of the bacteria in mature biofilms to some extent is a consequence of a c-di-GMP-regulated persistence strategy.
Although our knowledge on non-attached aggregates is still in its infancy, it appears that bacteria in aggregates share phenotypic traits with bacteria in surface-attached biofilms. Thus, our current knowledge suggests that aggregates should be regarded as a special form of biofilms that can be found across diverse environments.
Selective pressures toward multicellular aggregation
Although the aggregate lifestyle provides numerous benefits, it will also limit the growth and mobility of the cells. The average growth rate for the whole population immobilized in a free floating aggregate is lower than for the same number of planktonic cells33. This is presumably due to the formation of chemical gradients from the surface of the aggregates towards the central regions as discussed above. The surface to volume ratio decreases with increasing aggregate size which will further restrict nutrient- and oxygen uptake, and decrease the potential growth compared to planktonic cells in in vitro cultures.
The biofilm phenotype is typically defined as sessile, and this is also partly true for non-attached aggregates. Cells in aggregates can of course passively be transported by mechanical forces, but an active movement is constrained by the aggregate matrix. If cells which constitute a non-attached aggregate exhibit the same transcriptomic switch as seen among cells in a surface attached biofilm, they will also down-regulate motility related genes. Thus, the movement of biofilm aggregates is largely determined by the local hydrodynamics due to liquid or mechanical forces such as ciliary movements.
In theory, aggregates are therefore not able to migrate to favorable niches during host colonization. However, the question is how frequent single cell migration is within the host. In the rare incidents where, single bacterial cells breach the barrier between skin, intestines or other commensally colonized compartments and enter sterile compartments of the body, it leads to a severe acute immune response92. The fitness trade-off between being organized as single cells or in biofilms is still widely debated and most likely does not have one single explanation. On one hand, single cell lifestyle is associated with fast growth and more even resource exploitation. On the other hand, the population is more vulnerable to environmental stressors where being organized in biofilm offers increased tolerance to many hostile conditions93. In infections, fast growing single cells may also, in very certain circumstances, lead to acute infections where pathogens such as P. aeruginosa or Burkholderia cepacia may migrate to the bloodstream causing bacteremia and possible death of the host within hours or days92. In other cases, the same organism can be found displaying slow growth in aggregates for decades which does not kill the host within hours, but years92,94. Most likely, the environment offers certain cues that bacteria respond to by either dispersing and being allowed to grow fast or by protecting themselves by encasement in biofilm where a rapid growth is then sacrificed.
Likewise, the environment may exert a selective pressure on attached vs. non-attached aggregation. In some infections, non-attached aggregates will be cleared very quickly e.g., in urethra and catheter infections a non-attached aggregate would be flushed away by flow. These are also the infections where surface attached biofilms are normally observed95,96.
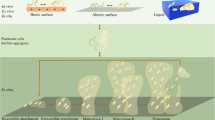
In vitro models for studying non-attached aggregates
The bulk of the current knowledge of biofilms has been gained using in vitro models where bacteria are grown on an innate surface as attached biofilms (Fig. 7). Systems such as the high-throughput microtiter biofilm assay have provided knowledge of the mechanisms of biofilm formation and antimicrobial tolerance and have enabled the screening of thousands of potential anti-biofilm compounds, whereas complex continuous flow cell biofilms have revealed structural mechanisms and regulatory pathways behind the development of surface biofilms97,98,99. Besides these ubiquitous biofilm models, CDC reactors, drip flow reactors, and most other in vitro biofilm models have the common trait of allowing planktonic cells to attach to an abiotic surface100. By providing these cells with liquid growth media the cells will grow into adherent biofilms. These biofilms can grow to be several hundred µm in thickness and often display structured architecture98,101,102.
Schematic breakdown of commonly used surface-attached biofilm models and model systems that aim to model non-attached aggregation. Common to all the models, is that host derived components and interactions is absent, except to some degree for SCFM2 where the chemical composition of CF sputum is mimicked.
Although perfect in vitro model systems rarely exist, an ideal non-attached aggregate in vitro model would aim at emulating in vivo/in situ phenotypic traits. Thus, emulation of the specific physicochemical microenvironment in question, as well as mimicking complex host-microbe interactions seem key in designing successful models.
One crucial aspect to consider, is the expression of extracellular polymeric substances (EPS) produced by biofilm cells but a clear understanding of the in vivo expression of EPS is still lacking. EPS play a critical role in the structure and function of in vitro biofilms, and their correct expression may be essential for accurately reproducing the behavior of biofilm aggregates in vivo where e.g., host derived carboxylates have been shown to impact biofilm development by CF pathogens50. In addition, the level of c-di-GMP which regulates biofilm formation and behavior is important. Finally, another essential factor to consider is antibiotic tolerance and resilience toward immune cells as found in non-attached aggregates100,103.
These characteristics are important for understanding how biofilm aggregates can persist in the presence of antimicrobial treatments and host defenses. Microenvironmental factors such as oxygen and nutrient gradients also play a critical role in the development and behavior of non-attached cells. Low oxygen levels can lead to increased tolerance of non-attached aggregates to antimicrobial treatments and also have an impact on the interactions between biofilm aggregates and host organisms104,105. Similarly, the availability of different nutrients can affect the growth and behavior of non-attached cells. To accurately mimic the in vivo non-attached phenotype, we first need to achieve a better understanding of the microenvironmental factors that are present in vivo, such as oxygen and nutrient gradients, as well as the correct production of EPS, level of c-di-GMP, antibiotic tolerance, and resilience towards immune cells. This will help in increasing our understanding of the complex interactions between microorganisms and their environment and ultimately aid in the development of more effective strategies for biofilm growth control in various environments.
Over the last decades, several model systems have been developed to model non-attached aggregates, primarily with a focus on understanding infectious biofilm aggregates (Fig. 7). Common to several of these model systems is that they use some form of immobilization of single cells with the aim of forcing the cells to propagate into dense aggregate. Wessel et al. used a gelatin-based three-dimensional printing strategy to trap a single cell in so-called microtraps66. These ~50 pL traps could be built on stilts in a flow system with a continuous flow of nutrient media surrounding it. The system was used to study the development of oxygen gradients through aggregates at various sizes. Although limited in clinical application due to the high level of surrounding oxygen and the absence of an immune component, this provided insights into the complex microenvironmental aspects of growth as a pseudo-suspended aggregate66.
Other groups have used low-viscosity gels to immobilize single cells. One example is the alginate bead model where aggregates develop from embedded single cells inside mm-sized beads that are formed in an alginate matrix106,107. An advantage with this model is the ability to form hundreds of beads with hundreds-thousands of individual biofilm aggregates inside73. As aggregates are growing, steep oxygen gradients develop from the edge of the bead towards the center. This creates a very stratified metabolic pattern between the various aggregates, with growth-limiting gradients going from the surface of the bead to the surface of each aggregate rather than gradients forming inside of each aggregate73,106. Aggregates grown in this model were shown to be highly tolerant towards common types of antibiotics, e.g., surviving 100x MIC of tobramycin106. Alginate can be found in abundance in the mucus surrounding biofilms in CF-associated lung infections, but in this model, it mainly serves as the immobilization matrix.
In an effort to capture in vivo chemical complexities, a synthetic CF medium was developed by Palmer et al. (SCFM)108 and further modified by Turner et al. (SCFM2)109 that closely resembles the viscosity and chemical composition of sputum from CF patients108,109. When single cells are seeded in this viscous medium comprised of amino acids, glucose, DNA, lipids, and mucins, these cells will form free-floating biofilm aggregates with a comparable size to that of aggregates found in CF-lung tissue81,109,110. In addition, P. aeruginosa aggregates formed in this model system have been shown to exhibit a comparable transcriptional profile as found in biofilms in CF infection, as well as exhibiting extensive tolerance towards both antibiotic and phage treatment109,110. Crone et al. developed a parallel model system that incorporated a chemically complex environment to model non-attached aggregates in a chronic wound model111. This model was based on growing aggregates in a sandwich of low viscosity agar media with wound-like components such as blood, serum, and animal derived media111. Both models were designed to mimic the highly nutrient-rich, but electron acceptor limited environments found in these infections.
More reductionistic model systems based on LB or minimal media with low percentage agar or agarose have provided insights into how EPS and the polymeric composition provided, can influence the development of antibiotic tolerance for cells in non-attached aggregates76. These simple models provide highly controlled conditions where essential phenotypic mechanisms can be investigated. A high degree of complexity will often compromise the time, effort, and cost of models and may not be necessary in all cases. Depending on the questions asked, more reductionistic approaches may be more optimal and tools for guiding such decisions have been developed112.
Perspectives
With increased attention on non-attached aggregates, numerous questions arise. Do aggregates in infections resemble the ones studied in vitro? Are the mechanisms that operate during in vitro biofilm formation playing a role during aggregate formation in infections? Are the antibiotic tolerance mechanisms disclosed through in vitro biofilm studies relevant for aggregates in infections? Are aggregates in infections formed through recruitment or clonal growth? Does cooperation occur in aggregates, and if so, how do aggregated populations protect against cheating? To answer these questions, and many more, we need to bridge the gap between our in vitro systems and the environments found in the infections we want to mimic. Development of more relevant models should be guided by increased knowledge about infectious microenvironments.
References
Stoodley, P., Sauer, K., Davies, D. G. & Costerton, J. W. Biofilms as complex differentiated communities. Annu. Rev. Microbiol 56, 187–209 (2002).
Pasteur, L. Mémoire sur la fermentation acétique. Annales scientifiques de. l’École Norm. supérieure 1, 113–158 (1864).
Zobell, C. E. The effect of solid surfaces upon bacterial activity1. J. Bacteriol. 46, 39–56 (1943).
Henrici, A. T. Studies of freshwater bacteria: I. A direct microscopic technique. J. Bacteriol. 25, 277–287 (1933).
Hoiby, N. et al. Pseudomonas aeruginosa infection in cystic fibrosis. Diagnostic and prognostic significance of Pseudomonas aeruginosa precipitins determined by means of crossed immunoelectrophoresis. Scand. J. Respir. Dis. 58, 65–79 (1977).
Costerton, J. W., Geesey, G. G. & Cheng, K. J. How bacteria stick. Sci. Am. 238, 86–95 (1978).
Cai, Y. M. Non-surface attached bacterial aggregates: A ubiquitous third lifestyle. Front Microbiol 11, 557035 (2020).
Schleheck, D. et al. Pseudomonas aeruginosa PAO1 preferentially grows as aggregates in liquid batch cultures and disperses upon starvation. PLoS One 4, e5513 (2009).
Hölscher, T. et al. Motility, chemotaxis and aerotaxis contribute to competitiveness during bacterial pellicle biofilm development. J. Mol. Biol. 427, 3695–3708 (2015).
Haaber, J., Cohn, M. T., Frees, D., Andersen, T. J. & Ingmer, H. Planktonic aggregates of Staphylococcus aureus protect against common antibiotics. PLoS One 7, e41075 (2012).
Kragh, K. N. et al. The inoculation method could impact the outcome of microbiological experiments. Appl. Environ. Microbiol 84, e02264–17 (2018).
Kragh, K. N. et al. Role of multicellular aggregates in biofilm formation. mBio 7, e00237 (2016).
Flemming, H. C. & Wuertz, S. Bacteria and archaea on Earth and their abundance in biofilms. Nat. Rev. Microbiol. 17, 247–260 (2019).
Mori, J. F. et al. Sticking together: Inter-species aggregation of bacteria isolated from iron snow is controlled by chemical signaling. ISME J. 11, 1075–1086 (2017).
Alldredge, A. & Silver, M. W. Characteristics, dynamics and significance of marine snow. Prog. Oceanogr. 20, 41–82 (1988).
Zan, J., Liu, Y., Fuqua, C. & Hill, R. T. Acyl-homoserine lactone quorum sensing in the Roseobacter clade. International Journal of Molecular Sciences 15, 654–669 https://doi.org/10.3390/ijms15010654 (2014).
Gram, L., Grossart, H. P., Schlingloff, A. & Kiørboe, T. Possible quorum sensing in marine snow bacteria: Production of acylated homoserine lactones by Roseobacter strains isolated from marine snow. Appl. Environ. Microbiol 68, 4111–4116 (2002).
Bjarnsholt, T. et al. The in vivo biofilm. Trends Microbiol 21, 466–474 (2013).
Fazli, M. et al. Nonrandom distribution of Pseudomonas aeruginosa and Staphylococcus aureus in chronic wounds. J. Clin. Microbiol 47, 4084–4089 (2009).
Alhede, M. et al. Bacterial biofilm formation and treatment in soft tissue fillers. Pathog. Dis. 70, 339–346 (2014).
Homøe, P., Bjarnsholt, T., Wessman, M., Sørensen, H. C. F. & Johansen, H. K. Morphological evidence of biofilm formation in Greenlanders with chronic suppurative otitis media. Eur. Arch. Otorhinolaryngol. 266, 1533–1538 (2009).
Kolpen, M. et al. Bacterial biofilms predominate in both acute and chronic human lung infections. Thorax 77, 1015–1022 (2022).
Patenall, B. L., Ridgley, J. D., Jenkins, A. T. A. & Young, A. E. Evidence of bacterial biofilms within acute wounds: a systematic review. J. Wound Care 32, 273–278 (2023).
Stacy, A., McNally, L., Darch, S. E., Brown, S. P. & Whiteley, M. The biogeography of polymicrobial infection. Nat. Rev. Microbiol. 14, 93–105 (2016).
Bjarnsholt, T. et al. Pseudomonas aeruginosa biofilms in the respiratory tract of cystic fibrosis patients. Pediatr. Pulmonol. 44, 547–558 (2009).
Fazli, M. et al. Quantitative analysis of the cellular inflammatory response against biofilm bacteria in chronic wounds. Wound Repair Regen. 19, 387–391 (2011).
Worlitzsch, D. et al. Effects of reduced mucus oxygen concentration in airway Pseudomonas infections of cystic fibrosis patients. J. Clin. Investig. 109, 317–325 (2002).
Staudinger, B. J. et al. Conditions associated with the cystic fibrosis defect promote chronic Pseudomonas aeruginosa infection. Am. J. Respir. Crit. Care Med 189, 812–824 (2014).
Pabst, B., Pitts, B., Lauchnor, E. & Stewart, P. S. Gel-Entrapped Staphylococcus aureus bacteria as model of biofilm infection exhibits growth in dense aggregates, oxygen limitation, antibiotic tolerance, and heterogeneous gene expression. Antimicrob. Agents Chemother. 60, 6294–6301 (2016).
Secor, P. R., Michaels, L. A., Ratjen, A., Jennings, L. K. & Singh, P. K. Entropically driven aggregation of bacteria by host polymers promotes antibiotic tolerance in Pseudomonas aeruginosa. Proc. Natl. Acad. Sci. USA 115, 10780–10785 (2018).
Borlee, B. R. et al. Pseudomonas aeruginosa uses a cyclic-di-GMP-regulated adhesin to reinforce the biofilm extracellular matrix. Mol. Microbiol 75, 827–842 (2010).
Rybtke, M. et al. The LapG protein plays a role in Pseudomonas aeruginosa biofilm formation by controlling the presence of the CdrA adhesin on the cell surface. Microbiologyopen 4, 917–930 (2015).
Alhede, M. et al. Phenotypes of non-attached Pseudomonas aeruginosa aggregates resemble surface attached biofilm. PLoS One 6, e27943 (2011).
Bottagisio, M. et al. Proteomic analysis reveals a biofilm-like behavior of planktonic aggregates of Staphylococcus epidermidis grown under environmental pressure/Stress. Front Microbiol 10, 1909 (2019).
Jennings, L. K. et al. Pseudomonas aeruginosa aggregates in cystic fibrosis sputum produce exopolysaccharides that likely impede current therapies. Cell Rep. 34, 108782 (2021).
Lam, J., Chan, R., Lam, K. & Costerton, J. W. Production of mucoid microcolonies by Pseudomonas aeruginosa within infected lungs in cystic fibrosis. Infect. Immun. 28, 546–556 (1980).
Evans, T. J. Small colony variants of Pseudomonas aeruginosa in chronic bacterial infection of the lung in cystic fibrosis. Fut. Microbiol 10, 231–239 (2015).
Malone, J. G. et al. YfiBNR mediates cyclic di-GMP dependent small colony variant formation and persistence in Pseudomonas aeruginosa. PLoS Pathog. 6, e1000804 (2010).
Starkey, M. et al. Pseudomonas aeruginosa Rugose small-colony variants have adaptations that likely promote persistence in the cystic fibrosis lung. J. Bacteriol. 191, 3492–3503 (2009).
Gloag, E. S. et al. Pseudomonas aeruginosa interstrain dynamics and selection of hyperbiofilm mutants during a chronic infection. mBio 10, e01698–19 (2019).
Whitchurch, C. B., Tolker-Nielsen, T., Ragas, P. C. & Mattick, J. S. Extracellular DNA required for bacterial biofilm formation. Science 295, 1487 (2002).
Chiang, W.-C. C. et al. Extracellular DNA shields against aminoglycosides in Pseudomonas aeruginosa biofilms. Antimicrob. Agents Chemother. 57, 2352–2361 (2013).
Walker, T. S. et al. Enhanced Pseudomonas aeruginosa biofilm development mediated by human neutrophils. Infect. Immun. 73, 3693–3701 (2005).
Barken, K. B. et al. Roles of type IV pili, flagellum-mediated motility and extracellular DNA in the formation of mature multicellular structures in Pseudomonas aeruginosa biofilms. Environ. Microbiol 10, 2331–2343 (2008).
Alhede, M. et al. The origin of extracellular DNA in bacterial biofilm infections in vivo. Pathog. Dis. 78, ftaa018 (2020).
Allesen-Holm, M. et al. A characterization of DNA release in Pseudomonas aeruginosa cultures and biofilms. Mol. Microbiol 59, 1114–1128 (2006).
Henderson, I. R., Meehan, M. & Owen, P. Antigen 43, a phase-variable bipartite outer membrane protein, determines colony morphology and autoaggregation in Escherichia coli K-12. FEMS Microbiol Lett. 149, 115–120 (1997).
Ulett, G. C. et al. Functional analysis of antigen 43 in uropathogenic Escherichia coli reveals a role in long-term persistence in the urinary tract. Infect. Immun. 75, 3233–3244 (2007).
Ageorges, V. et al. Differential homotypic and heterotypic interactions of antigen 43 (Ag43) variants in autotransporter-mediated bacterial autoaggregation. Sci. Rep. 9, 11100 (2019).
Riquelme, S. A. et al. Pseudomonas aeruginosa utilizes host-derived itaconate to redirect its metabolism to promote biofilm formation. Cell Metab. 31, 1091–1106.e6 (2020).
Tomlinson, K. L. et al. Staphylococcus aureus induces an itaconate-dominated immunometabolic response that drives biofilm formation. Nat. Commun. 12, 1399 (2021).
Krsmanovic, M. et al. Hydrodynamics and surface properties influence biofilm proliferation. Adv. Colloid Interface Sci. 288, 102336 (2021).
Seviour, T. et al. The biofilm matrix scaffold of Pseudomonas aeruginosa contains G-quadruplex extracellular DNA structures. npj Biofilms Microbiomes 7, 1–12 (2021).
Gjermansen, M., Ragas, P., Sternberg, C., Molin, S. & Tolker-Nielsen, T. Characterization of starvation-induced dispersion in Pseudomonas putida biofilms. Environ. Microbiol 7, 894–904 (2005).
Jenal, U., Reinders, A. & Lori, C. Cyclic di-GMP: Second messenger extraordinaire. Nat. Rev. Microbiol. 15, 271–284 (2017).
Christensen, L. D. et al. Clearance of Pseudomonas aeruginosa foreign-body biofilm infections through reduction of the cyclic Di-GMP Level in the Bacteria. Infect. Immun. 81, 2705 (2013).
Gjermansen, M., Ragas, P. & Tolker-Nielsen, T. Proteins with GGDEF and EAL domains regulate Pseudomonas putida biofilm formation and dispersal. FEMS Microbiol Lett. 265, 215–224 (2006).
Gjermansen, M., Nilsson, M., Yang, L. & Tolker-Nielsen, T. Characterization of starvation-induced dispersion in Pseudomonas putida biofilms: genetic elements and molecular mechanisms. Mol. Microbiol 75, 815–826 (2010).
Andersen, J. B. et al. Induction of Native c-di-GMP Phosphodiesterases Leads to Dispersal of Pseudomonas aeruginosa Biofilms. Antimicrob. Agents Chemother. 65, e02431–20 (2021).
Kim, S. M. et al. LuxR homologue smcr is essential for vibrio vulnificus pathogenesis and biofilm detachment, and its expression is induced by host cells. Infect. Immun. 81, 3721–3730 (2013).
Rice, S. A. et al. Biofilm formation and sloughing in Serratia marcescens are controlled by quorum sensing and nutrient cues. J. Bacteriol. 187, 3477–3485 (2005).
Schooling, S. R., Charaf, U. K., Allison, D. G. & Gilbert, P. A role for rhamnolipid in biofilm dispersion. Biofilms 1, 91–99 (2004).
Stewart, P. S. Diffusion in biofilms. J. Bacteriol. 185, 1485–1491 (2003).
Aristotelous, A. C. et al. Diffusive transport through a model host-biofilm system. Phys. Rev. E Stat. Nonlin Soft Matter Phys. 92, 022703 (2015).
Lichtenberg, M. et al. The structure-function relationship of Pseudomonas aeruginosa in infections and its influence on the microenvironment. FEMS Microbiol Rev. 46, fuac018 (2022).
Wessel, A. K. et al. Oxygen limitation within a bacterial aggregate. mBio 5, e00992 (2014).
James, G. A. et al. Microsensor and transcriptomic signatures of oxygen depletion in biofilms associated with chronic wounds. Wound Repair Regen. 24, 373–383 (2016).
Kolpen, M. et al. Polymorphonuclear leucocytes consume oxygen in sputum from chronic Pseudomonas aeruginosa pneumonia in cystic fibrosis. Thorax 65, 57–62 (2010).
Stewart, P. S. & Franklin, M. J. Physiological heterogeneity in biofilms. Nat. Rev. Microbiol 6, 199–210 (2008).
Dar, D., Dar, N., Cai, L. & Newman, D. K. Spatial transcriptomics of planktonic and sessile bacterial populations at single-cell resolution. Science 373, eabi4882 (2021).
Pamp, S. J., Gjermansen, M., Johansen, H. K. & Tolker-Nielsen, T. Tolerance to the antimicrobial peptide colistin in Pseudomonas aeruginosa biofilms is linked to metabolically active cells, and depends on the pmr and mexAB-oprM genes. Mol. Microbiol 68, 223–240 (2008).
Lopatkin, A. J. et al. Bacterial metabolic state more accurately predicts antibiotic lethality than growth rate. Nat. Microbiol 4, 2109–2117 (2019).
Lichtenberg, M., Kvich, L., Larsen, S. L. B., Jakobsen, T. H. & Bjarnsholt, T. Inoculum concentration influences pseudomonas aeruginosa phenotype and biofilm architecture. Microbiol Spectr. 10, e0313122 (2022).
Kirketerp-Møller, K., Stewart, P. S. & Bjarnsholt, T. The zone model: A conceptual model for understanding the microenvironment of chronic wound infection. Wound Repair Regen. 28, 593–599 (2020).
Ciofu, O. & Tolker-Nielsen, T. Tolerance and resistance of Pseudomonas aeruginosa biofilms to antimicrobial agents-how P. aeruginosa can escape antibiotics. Front. Microbiol. 10, 913 (2019).
Goltermann, L. & Tolker-Nielsen, T. Importance of the exopolysaccharide matrix in antimicrobial tolerance of pseudomonas aeruginosa aggregates. Antimicrob. Agents Chemother. 61, e02696–16 (2017).
Lichtenberg, M. et al. Cyclic-di-GMP signaling controls metabolic activity in Pseudomonas aeruginosa. Cell Rep. 41, 111515 (2022).
Liang, Z. et al. The role of individual exopolysaccharides in antibiotic tolerance of Pseudomonas aeruginosa aggregates. Front Microbiol 14, 1187708 (2023).
Kirketerp-Møller, K. et al. Distribution, organization, and ecology of bacteria in chronic wounds. J. Clin. Microbiol 46, 2717–2722 (2008).
Bjarnsholt, T., Tolker-Nielsen, T., Givskov, M., Janssen, M. & Christensen, L. H. Detection of bacteria by fluorescence in situ hybridization in culture-negative soft tissue filler lesions. Dermatol Surg. 35, 1620–1624 (2009).
Kragh, K. N. et al. Polymorphonuclear leukocytes restrict growth of Pseudomonas aeruginosa in the lungs of cystic fibrosis patients. Infect. Immun. 82, 4477–4486 (2014).
Alhede, M. et al. Bacterial aggregate size determines phagocytosis efficiency of polymorphonuclear leukocytes. Med. Microbiol Immunol. 209, 669–680 (2020).
Pettygrove, B. A. et al. Delayed neutrophil recruitment allows nascent Staphylococcus aureus biofilm formation and immune evasion. Biomaterials 275, 120775 (2021).
Jensen, P. Ø. et al. Rapid necrotic killing of polymorphonuclear leukocytes is caused by quorum-sensing-controlled production of rhamnolipid by Pseudomonas aeruginosa. Microbiol. (Read.) 153, 1329–1338 (2007).
Van Gennip, M. et al. Inactivation of the rhlA gene in Pseudomonas aeruginosa prevents rhamnolipid production, disabling the protection against polymorphonuclear leukocytes. APMIS 117, 537–546 (2009).
Alhede, M. et al. Pseudomonas aeruginosa recognizes and responds aggressively to the presence of polymorphonuclear leukocytes. Microbiol. (Read.) 155, 3500–3508 (2009).
Werner, E. et al. Stratified growth in Pseudomonas aeruginosa biofilms. Appl. Environ. Microbiol 70, 6188–6196 (2004).
Sternberg, C. et al. Distribution of bacterial growth activity in flow-chamber biofilms. Appl. Environ. Microbiol 65, 4108–4117 (1999).
Rybtke, M. et al. Gauging and visualizing c-di-GMP levels In pseudomonas aeruginosa using fluorescence-based biosensors. in Methods in Molecular Biology 1657 87–98 (2017).
Güvener, Z. T. & Harwood, C. S. Subcellular location characteristics of the Pseudomonas aeruginosa GGDEF protein, WspR, indicate that it produces cyclic-di-GMP in response to growth on surfaces. Mol. Microbiol 66, 1459–1473 (2007).
Rybtke, M. T. et al. Fluorescence-based reporter for gauging cyclic Di-GMP levels in Pseudomonas aeruginosa. Appl. Environ. Microbiol 78, 5060–5069 (2012).
Furukawa, S., Kuchma, S. L. & O’Toole, G. A. Keeping their options open: acute versus persistent infections. J. Bacteriol. 188, 1211–1217 (2006).
Ciofu, O., Moser, C., Jensen, P. Ø. & Høiby, N. Tolerance and resistance of microbial biofilms. Nat. Rev. Microbiol. 20, 621–635 (2022).
Ciofu, O., Hansen, C. R. & Høiby, N. Respiratory bacterial infections in cystic fibrosis. Curr. Opin. Pulm. Med. 19, 251–258 (2013).
Nickel, J. C., Grant, S. K. & Costerton, J. W. Catheter-associated bacteriuria. Exp. Study Urol. 26, 369–375 (1985).
Pogorelov, A. G., Chebotar, I. V. & Pogorelova, V. N. Scanning electron microscopy of biofilms adherent to the inner catheter surface. Bull. Exp. Biol. Med. 157, 711–714 (2014).
Pitts, B., Hamilton, M. A., Zelver, N. & Stewart, P. S. A microtiter-plate screening method for biofilm disinfection and removal. J. Microbiol Methods 54, 269–276 (2003).
Kragh, K. N., Alhede, M., Kvich, L. & Bjarnsholt, T. Into the well-A close look at the complex structures of a microtiter biofilm and the crystal violet assay. Biofilm 1, 100006 (2019).
Crusz, S. A. et al. Bursting the bubble on bacterial biofilms: a flow cell methodology. Biofouling 28, 835–842 (2012).
Azeredo, J. et al. Critical review on biofilm methods. Crit. Rev. Microbiol 43, 1–39 (2016).
Tolker-Nielsen, T. & Sternberg, C. Growing and analyzing biofilms in flow chambers. Curr. Protoc. Microbiol Chapter 1, Unit 1B.2 (2011).
Goeres, D. M. et al. Statistical assessment of a laboratory method for growing biofilms. Microbiol. (Read.) 151, 757–762 (2005).
Roberts, A. E., Kragh, K. N., Bjarnsholt, T. & Diggle, S. P. The limitations of in vitro experimentation in understanding biofilms and chronic infection. J. Mol. Biol. 427, 3646–3661 (2015).
Hassett, D. J. et al. Pseudomonas aeruginosa hypoxic or anaerobic biofilm infections within cystic fibrosis airways. Trends Microbiol 17, 130–138 (2009).
Folsom, J. P. et al. Physiology of Pseudomonas aeruginosa in biofilms as revealed by transcriptome analysis. BMC Microbiol 10, 294 (2010).
Sønderholm, M. et al. Pseudomonas aeruginosa aggregate formation in an alginate bead model system exhibits in vivo-like characteristics. Appl Environ. Microbiol 83, e00113–e00117 (2017).
Cao, B. et al. Antibiotic penetration and bacterial killing in a Pseudomonas aeruginosa biofilm model. J. Antimicrob. Chemother. 70, 2057–2063 (2015).
Palmer, K. L., Aye, L. M. & Whiteley, M. Nutritional cues control Pseudomonas aeruginosa multicellular behavior in cystic fibrosis sputum. J. Bacteriol. 189, 8079–8087 (2007).
Turner, K. H., Wessel, A. K., Palmer, G. C., Murray, J. L. & Whiteley, M. Essential genome of Pseudomonas aeruginosa in cystic fibrosis sputum. Proc. Natl. Acad. Sci. USA 112, 4110–4115 (2015).
Darch, S. E. et al. Phage inhibit pathogen dissemination by targeting bacterial migrants in a chronic infection model. mBio 8, e00240–17 (2017).
Crone, S., Garde, C., Bjarnsholt, T. & Alhede, M. A novel in vitro wound biofilm model used to evaluate low-frequency ultrasonic-assisted wound debridement. J. Wound Care 24, 64 (2015). 66–9, 72.
Cornforth, D. M., Diggle, F. L., Melvin, J. A., Bomberger, J. M. & Whiteley, M. Quantitative framework for model evaluation in microbiology research using Pseudomonas aeruginosa and cystic fibrosis infection as a test case. mBio 11, e03042–19 (2020).
Drenkard, E. & Ausubel, F. M. Pseudomonas biofilm formation and antibiotic resistance are linked to phenotypic variation. Nature 416, 740–743 (2002).
Tseng, B. S. et al. The extracellular matrix protects Pseudomonas aeruginosa biofilms by limiting the penetration of tobramycin. Environ. Microbiol 15, 2865–2878 (2013).
Flemming, H.-C. & Wingender, J. The biofilm matrix. Nat. Rev. Microbiol 8, 623–633 (2010).
Haagensen, J. A. J. et al. Differentiation and distribution of colistin- and sodium dodecyl sulfate-tolerant cells in Pseudomonas aeruginosa biofilms. J. Bacteriol. 189, 28–37 (2007).
Chiang, W. C., Pamp, S. J., Nilsson, M., Givskov, M. & Tolker-Nielsen, T. The metabolically active subpopulation in Pseudomonas aeruginosa biofilms survives exposure to membrane-targeting antimicrobials via distinct molecular mechanisms. FEMS Immunol. Med. Microbiol 65, 245–256 (2012).
van Gennip, M. et al. Interactions between polymorphonuclear leukocytes and Pseudomonas aeruginosa biofilms on silicone implants in vivo. Infect. Immun. 80, 2601–2607 (2012).
Sønderholm, M. et al. Tools for studying growth patterns and chemical dynamics of aggregated Pseudomonas aeruginosa exposed to different electron acceptors in an alginate bead model. NPJ Biofilms Microbiomes 4, 3 (2018).
Wolfaardt, G. M., Lawrence, J. R., Robarts, R. D., Caldwell, S. J. & Caldwell, D. E. Multicellular organization in a degradative biofilm community. Appl. Environ. Microbiol 60, 434–446 (1994).
Goeres, D. M. et al. A method for growing a biofilm under low shear at the air-liquid interface using the drip flow biofilm reactor. Nat. Protoc. 4, 783–788 (2009).
O’Toole, G. A. Microtiter dish biofilm formation assay. J. Visual. Exp. 47, 2437 (2011).
Ceri, H. et al. The Calgary Biofilm Device: new technology for rapid determination of antibiotic susceptibilities of bacterial biofilms. J. Clin. Microbiol 37, 1771–1776 (1999).
Connell, J. L., Wessel, A. K., Parsek, M. R., Ellington, A. D., Whiteley, M. & Shear, J. B. Probing prokaryotic social behaviors with bacterial “lobster traps”. mBio. 1, e00202-10 (2010).
Behrendt, L. et al. Biofilm growth and near-infrared radiation-driven photosynthesis of the chlorophyll d-containing cyanobacterium Acaryochloris marina. Appl Environ. Microbiol 78, 3896–3904 (2012).
Acknowledgements
This work was supported by grants from the Lundbeck Foundation (R250-2017-633) to M.L., and the Independent Research Fund Denmark (9040-00023B) to T.T.N.
Author information
Authors and Affiliations
Contributions
K.K. and M.L. outlined the review. K.K., T.T.N., and M.L. wrote the review.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Communications Biology thanks Kendra (P) Rumbaugh, Shinya Sugimoto, and the other, anonymous, reviewer(s) for their contribution to the peer review of this work. Primary Handling Editor: George Inglis.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Kragh, K.N., Tolker-Nielsen, T. & Lichtenberg, M. The non-attached biofilm aggregate. Commun Biol 6, 898 (2023). https://doi.org/10.1038/s42003-023-05281-4
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s42003-023-05281-4
This article is cited by
-
Mechanisms of microbial co-aggregation in mixed anaerobic cultures
Applied Microbiology and Biotechnology (2024)
-
Biofilm formation: mechanistic insights and therapeutic targets
Molecular Biomedicine (2023)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.