Abstract
While smartphone usage is ubiquitous, and the app market for smartphone apps targeted at mental health is growing rapidly, the evidence of standalone apps for treating mental health symptoms is still unclear. This meta-analysis investigated the efficacy of standalone smartphone apps for mental health. A comprehensive literature search was conducted in February 2018 on randomized controlled trials investigating the effects of standalone apps for mental health in adults with heightened symptom severity, compared to a control group. A random-effects model was employed. When insufficient comparisons were available, data was presented in a narrative synthesis. Outcomes included assessments of mental health disorder symptom severity specifically targeted at by the app. In total, 5945 records were identified and 165 full-text articles were screened for inclusion by two independent researchers. Nineteen trials with 3681 participants were included in the analysis: depression (k = 6), anxiety (k = 4), substance use (k = 5), self-injurious thoughts and behaviors (k = 4), PTSD (k = 2), and sleep problems (k = 2). Effects on depression (Hedges’ g = 0.33, 95%CI 0.10–0.57, P = 0.005, NNT = 5.43, I2 = 59%) and on smoking behavior (g = 0.39, 95%CI 0.21–0.57, NNT = 4.59, P ≤ 0.001, I2 = 0%) were significant. No significant pooled effects were found for anxiety, suicidal ideation, self-injury, or alcohol use (g = −0.14 to 0.18). Effect sizes for single trials ranged from g = −0.05 to 0.14 for PTSD and g = 0.72 to 0.84 for insomnia. Although some trials showed potential of apps targeting mental health symptoms, using smartphone apps as standalone psychological interventions cannot be recommended based on the current level of evidence.
Similar content being viewed by others
Introduction
As mobile phone usage is ubiquitous, and mobile apps targeted at mental health are flooding the app market, mobile health (mHealth) interventions, which utilize mobile devices and technologies for mental health problems, are gaining popularity.1,2
Mental disorders are highly prevalent worldwide, can often have a detrimental impact on the life of affected individuals, and, to date, remain greatly undertreated.3,4 Although a wide array of evidence-based treatments exist, the majority of individuals with symptoms of mental disorders remain without treatment, even in high-income economies.5,6
Apart from structural treatment barriers such as availability, affordability, and time constraints, attitudinal factors play an even greater role in non-treatment-seeking behavior.7 Contributing factors hindering treatment uptake and treatment continuation include low perceived treatment need, poor mental health literacy, preference for self-reliance, and fear of stigmatization.7,8
Mobile devices could be utilized to overcome some of these issues. mHealth interventions utilizing apps on mobile devices have several benefits: (a) The threshold to use them is generally low and they provide the opportunity to engage individuals in need of treatment timely and anonymously by providing portable and flexible treatment; (b) mHealth might reach individuals who would otherwise not seek treatment;9 (c) most individuals already experience mobile devices to be an integral part of their everyday life and forthcoming generations are growing up as digital natives, where the use of apps for many different areas of life is becoming natural;10 (d) mHealth could be utilized to deliver large-scale interventions in emerging and low-income economies where resources for mental health are greatly limited,4 and (e) individuals can be supported in applying treatment-related skills in real life situations, in which behavior change is at its most vulnerable, and clinicians often struggle to support individuals appropriately.
The app-scape (app landscape) targeting mental health has increasingly been growing. According to a 2017 report, more than 318,000 health-related mobile apps were available for consumers of which 490 unique apps were targeted at mental health and behavioral disorders.11 A 2016 study scanning the app markets found 208 apps related to mental health or stress, most commonly targeting symptom relief (41%, 85/208) or general mental health education (18%, 37/208). The majority of identified apps did not mention any information on its effectiveness (59%, 123/208).12 Another study from 2018 rated the quality of depression apps available in German app stores with only 11% (4/38) showing some face validity, without any evidence on the effectiveness, and safety of any of the apps.13
Apps have been highly praised for their potential towards physical and mental health treatments.14 However, when considering using apps for mental health, there are also potential pitfalls. Disadvantages include technical aspects of delivery, such as screen size, battery life, system updates, technology requirements, as well as usage patterns, such as frequent but brief daily smartphone interactions, attentional competition between apps, short app lifespans, non-private settings, and data-security concerns.15,16,17
Unexpectedly, only very few studies have systematically examined the overall efficacy of mobile apps for mental health. A systematic review from 2013 by Donker et al., only found five apps, of which only three were evaluated in an RCT; targeting depression, anxiety and substance use, and with-in and between-group intention-to-treat effect sizes ranged from 0.29 to 2.28 at post-assessment and 0.01 to 0.48 at follow-up.18
Menon et al., conducted a systematic review on the feasibility of mobile phone apps and other mobile phone-based technology for psychotherapy in mental health disorders.19 Of 24 eligible articles, only eight involved smartphone apps. The eligible apps were found to be feasible and acceptable; however, no statistical analysis on the pooled efficacy was conducted.
There have also been previous systematic and meta-analytic disorder-specific examinations of efficacy, which found small effects for reductions in total anxiety scores from smartphone interventions compared to control conditions (g = 0.33, 95%CI 0.17–0.48, P < 0.01)20 and small effects for reductions in depressive symptoms from smartphone apps compared to control conditions (g = 0.38, 95%CI 0.24–0.52, P < 0.001).21 However, in both reviews, studies were included which did not primarily target depression or anxiety, including apps for memory training and attentional control, so that the effect of apps designed for anxiety and depression remains unclear, as well as the effect of apps individuals explicitly seek as treatment for a specific psychological disorder.
Although apps have been present for approximately ten years and are already being utilized by individuals seeking help for mental health problems, their overall efficacy remains unknown. Therefore, it is crucial to address this issue systematically. The aim of this meta-analysis is to investigate whether standalone psychological interventions for mental health delivered via smartphone apps are efficacious in reducing symptoms of mental disorders and self-injurious thoughts and behaviors (STBs) in adults with heightened symptom severity.
Results
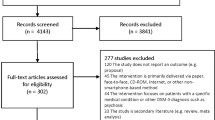
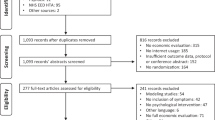
A total of 5921 records were retrieved from the electronic databases. After removal of duplicates and exclusion based on title and abstract, 165 records remained for full text screening. Seventeen publications describing 19 trials fulfilling all inclusion criteria between intervention and control groups remained and were included. Interrater reliability of full text eligibility check was good (κ = 0.64). Figure 1 displays the study flow (reference list of included trials Supplementary References).
All included studies were conducted in high-income countries (k = 11 USA, k = 3 Australia, k = 1 Israel, k = 1 the Netherlands, k = 1 South Korea, k = 1 Sweden, and k = 1 Switzerland). The primary study outcomes of the 19 included studies were depression (k = 6), anxiety (k = 4), posttraumatic stress disorder (k = 2), sleep problems (k = 2), substance use: smoking (k = 3), substance use: drinking (k = 3), and self-injury and suicidal behavior (k = 4). One study addressed smoking and drinking simultaneously. Several studies also assessed anxiety (k = 8) and depression (k = 12), either as primary or secondary outcomes.
All primary study outcomes only utilized self-report measures which were assessed at baseline and at post-assessment. Sample size of the included studies ranged from n = 34 to n = 983. The 19 included studies used different types of comparators: k = 2 no-treatment controls, k = 9 wait-list control groups, k = 3 information only, k = 4 sham group, and k = 1 daily mood chart.
All eligible apps were found to be based on some type of framework: cognitive behavioral therapy (k = 8), therapeutic evaluative conditioning (k = 1),22 attentional bias modification (k = 2), mindfulness (k = 1), behavioral modification (k = 1), theory of planned behavior (k = 1), breathing retraining (k = 1), monitoring with feedback (k = 1), decision aid (k = 1), problem-solving therapy (k = 1), and cognitive control (k = 1) (see Table 1).
An overview of selected study characteristics can be found in Table 1. In total, 3681 participants were included in this study (overview of all trials and effects Supplementary Table 2).
App and intervention components
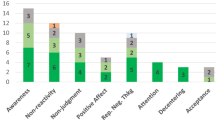
In a further exploration of the studies, we reported the app and intervention components as described. All app features identified in the studies were used as a category to give an overview of how many other studies applied similar techniques. Of the 19 studies, eight (42%, 8/19) employed some type of symptom or behavior monitoring, active participant engagement was utilized in eight interventions which prompted participant engagement by explicitly requesting input (42%, 8/19), eight studies described mechanisms of tailoring based on context sensing, feedback or input (42%, 8/19), some sort of gamification was utilized in six studies (32%, 6/19), five studies sent intervention reminders based on adherence monitoring (26%, 5/19), four studies had some sort of social component added (21%, 4/19), two studies employed some sort of guidance (11%, 2/19), one study used a simulation of situations (5%, 1/19), and one study evaluated an intervention including a wearable device (5%, 1/19) (overview of app components is shown in Table 2).
Quality assessment
The initial interrater reliability between the two independent raters was considered good (κ = 0.67). Overall, risk of bias across trials was considerable. Thirteen (68%, 13/19) reported an adequate sequence generation, while only seven studies (37%, 7/19) reported on adequate allocation concealment. Seven studies (37%, 7/19) were rated as low risk concerning blinding of participants and personnel when participants received some type of sham treatment or app not knowing whether they received the treatment or not. All studies used self-report assessments so that blinding of outcome assessors was rated as not applicable. Twelve studies (63%, 12/19) took adequate measures to deal with missing data and described these methods at least partially. Concerning outcome reporting, only six (32%, 6/19) study registrations were retrievable in which studies had been registered and the outcomes were reported as originally stated. Although all trials were conducted in the last ten years and a priori trial registration has become standard practice, very few studies complied. Only one study (5%, 1/19) was assessed as having an overall low risk of bias (no bias detected) and three studies (16%, 3/19) were assessed with having a risk of bias in only one domain. More than half of the studies (53%, 10/19) were assessed as having some sort of bias in at least three domains (complete risk of bias rating is shown in Supplementary Table 1, Supplementary Figs 1 and 2).
Depression
Data on the primary target depression was pooled from six comparisons (n = 796). A significant pooled effect of smartphone apps compared to controls for depression was found with g = 0.33 (95%CI 0.10–0.57, P = 0.005). This translates to an NNT of 5.43. Heterogeneity between trials was moderate (I2 = 59%, 95%CI 0–83%). Figure 2 shows the forest plot.
Furthermore, depression was assessed in 12 comparisons (n = 1544) as primary or secondary outcome in apps for depression, anxiety, sleep problems, PTSD, and suicidal ideation. The pooled effect was significant in favor of smartphone apps compared to control groups with g = 0.34 (95%CI 0.18–0.49, P ≤ 0.001) which corresponds with an NNT of 5.26. Heterogeneity was moderate (I2 = 53%, 95%CI 10–76%) (forest plot Supplementary Fig. 4).
There was a significant effect of apps compared to controls for overall depression when analyzing trials that employed a wait-list control group (k = 8, g = 0.41, 95%CI 0.24–0.59, P ≤ 0.001, NNT = 4.39, I2 = 47%, 95%CI 0–76%) and a non-significant effect for other form of controls (k = 4, g = 0.17, 95%CI −0.00 to 0.42, P = 0.19, I2 = 36%, 95%CI 0–78%).
Anxiety
Anxiety was investigated in four comparisons (n = 479). Differences between smartphone apps and controls were not significant (g = 0.30, 95%CI −0.1 to 0.7, P = 0.145) and heterogeneity was high (I2 = 75%, 95%CI 31–91%) (forest plot Supplementary Fig. 3).
Anxiety was also assessed in eight comparisons (n = 948) as either primary or secondary outcome of apps for anxiety, depression, and one app for sleep problems. In this analysis, we found smartphone apps to be superior to controls with a pooled effect of g = 0.43 (95%CI 0.19–0.66, P ≤ 0.001) which was significant, and relates to an NNT of 4.2. Heterogeneity was moderate to high (I2 = 66%, 95%CI 28–84%) (forest plot Supplementary Fig. 5).
Trials which employed a wait-list (k = 6) had a significant mean effect for overall anxiety of g = 0.49 (95%CI 0.27–0.71, P ≤ 0.001, NNT = 3.68, I2 = 47%, 95%CI 0–79%). Only two trials (k = 2) employed another type of control group which is why the effects were not pooled.
Self-injurious thoughts and behaviors
Suicidal ideation was assessed in four comparisons (n = 286), of which three used the same intervention, the pooled effect was non-significant with an effect size of g = −0.14 (95%CI −0.37 to 0.1, P = 0.246). Heterogeneity was low (I2 = 0%, 95%CI 0–85%). Self-injury was assessed in three comparisons (n = 225) by the same authors evaluating the same intervention, and the pooled effect was not significant (g = −0.04, 95%CI −0.31 to 0.22, P = 0.746). Heterogeneity was low (I2 = 0%, 95%CI 0–80%) (forest plot Supplementary Figs 9 and 10).
Substance use
Three comparisons (n = 780) investigated the effects on smoking and found a small significant effect of apps compared to control groups (g = 0.39, 95%CI 0.21–0.57, NNT = 4.59, P ≤ 0.001) and low heterogeneity between trials (I2 = 0%, 95%CI 0–93%).
Three comparisons (n = 1040) that investigated the effects on drinking did not find a significant effect of smartphone apps compared to controls (g = −0.03, 95%CI −0.22 to 0.17, P = 0.774, I2 = 48%, 95%CI 0–85%).
Effects on substance use were also pooled for smoking and drinking from five comparisons, with no significant difference between intervention and controls (g = 0.18, 95%CI −0.09 to 0.45, P = 0.2). Heterogeneity was high (I2 = 81%, 95%CI 54–92%) (forest plots Supplementary Figs 6–8).
Posttraumatic stress disorder
Data on PTSD was not pooled over trials due to only two comparisons. Both trials evaluated the same intervention with both trials not finding significant effects in favor of the intervention versus control group (g = 0.14, 95%CI −0.22 to 0.5, n = 120, P = 0.439;23 and g = −0.05, 95%CI −0.6 to 0.51, n = 49, P = 0.87324).
Sleep problems
Due to the limited amount of comparisons (k = 2) data for sleep problems was not pooled over trials. Both trials found significant effects in favor of the intervention group, with medium to large effects on sleep problems (g = 0.84, 95%CI 0.17–1.51, P = 0.014, n = 36, NNT = 2.23;25 and g = 0.72, 95%CI 0.39–1.05, P ≤ 0.001, n = 151, NNT = 2.5626).
Discussion
Only 19 eligible trials were identified which evaluated the efficacy of a smartphone app designed to treat mental health symptoms in a randomized controlled trial, although hundreds of apps for mental health are available in the consumer app markets. This evaluation gap is in line with previous findings.13,27 All trials were conducted in high-income countries.
Significant pooled effects were found for depression (g = 0.33) and smoking (g = 0.39), with small effect sizes and moderate heterogeneity. No significant pooled effects were found for anxiety, alcohol use, and STBs. Additionally, when exploring effects on depression (g = 0.34) and anxiety (g = 0.43), regardless whether this was the primary aim of the intervention, pooled effects were significant, but heterogeneity was moderate to high. These effect sizes are in line with previous research investigating the efficacy of apps for depression and anxiety regardless of whether the app was aimed at depression or anxiety, or another mental health domain.20,21 Both trials targeting PTSD did not find significant effects of the evaluated interventions, whereas both trials on insomniac complaints did, with medium to large effect sizes. Overall, risk of bias was found to be considerate.
Interestingly, effects for most mental health domains were much smaller than what has been found in meta-analytic reviews for digital mental health interventions delivered using the internet (for an overview see e.g. ref. 28). For example, whereas effects on depression were small in the present analysis, the most recent meta-analyses on digital interventions targeting Major Depression found a mean standardized effect size of 0.90.29 Also, the non-significant effects on anxiety are somewhat surprising, given that meta-analytic reviews on internet-based interventions for anxiety found, when compared to passive control conditions, large effects; for example for social anxiety (g = 0.84)30 and general anxiety (g = 0.91)5 as well as for panic disorder (g = 0.83).31 The same goes for PTSD, for which the most recent review found an average pooled effect of 0.95,32 while the two only randomized trials that we were able to include in this study evaluating standalone apps for PTSD did not find significant effects. A different picture emerges when focusing on sleep problems. Although the effects of the two trials evaluating apps for insomniac symptoms were somewhat smaller than the average effects found for internet-based self-help interventions (g = 1.09), their confidence intervals overlap.33
These findings imply that the accumulating evidence for digital mental health interventions delivered through the internet as an effective mean to treat mental health disorders cannot be directly translated to digital interventions delivered via standalone mobile apps for all mental disorders.
Differences between findings in the present study for app-based standalone interventions targeting mental health symptoms and those often found for internet-delivered mental health interventions might be explained by systematic differences in patient, trial, or intervention characteristics. For example, guidance has been associated with higher effect sizes in digital mental health interventions,34 and many of the here included trials evaluated purely self-guided interventions without support from a professional. However, recent trials also indicate significant and moderate to large effects for unguided internet mental health interventions for some disorders such as anxiety or insomnia.35,36 Research has suggested that efficacy of apps is also dependent on long-term adherence to an app, otherwise the impact may be limited, and prompts where shown to increase effectiveness.37 Far fewer than half of the investigated studies employed such strategies; eight studies prompted participant engagement by explicitly requesting input and only five studies sent intervention reminders based on adherence.
Also, considering other app and intervention components utilized in the investigated apps, it seems that only a small portion of the uniquely available features of apps were actually used, which when applied correctly, might have the potential to compensate for other disadvantages of smartphone apps. It might also be helpful for individuals to have a fixed time and space to go through an intervention which might not be compatible with the general manner in which smartphones are used, e.g. when waiting in line or in a public space. The technological advantages of app-based interventions may not yet be so advanced to level out disadvantages of this approach; this might however change in the near future.
Overall, our knowledge of how to design effective mental health apps is very much at the beginning. Unlike established internet interventions, in which manuals for onsite psychotherapy can be directly translated and work very well, clinicians and researchers might need to start thinking outside of the box, and direct greater attention to the technological and persuasive design aspects of app-based interventions. Not being able to detect efficacy in many of the mental health domains might be based on an actual failure to deliver mental health treatment through mobile apps, however, this might also be based on the inefficacious manner in which the treatments were deployed and implemented.
Also, our findings do not refer to the use of apps as an adjunct to evidence-based treatments i.e. blended formats38 such as face-to-face39 or internet-based psychotherapy.9 One possibility to benefit from apps that already show small effects such as for depression, smoking, and sleep problems could be to have them integrated into a clinical setting in which a professional can monitor progress and provide additional support. This is a potentially relevant field which should be investigated systematically.
Limitations
When interpreting the findings, the following limitations should be considered. First, heterogeneity was substantial in most analyses, as was risk of bias. As there were limited studies per disorder, also in the narrative description of study effects, findings should be interpreted with caution. Our findings of limited or non-existent efficacy of standalone treatment delivered by smartphone apps could also be due to the limited amount of studies available. Heterogeneity was not explored in a content-focused manner, nor did we investigate the effects of different features and components on efficacy or engagement. Overall, the limited efficacy does not mean that apps for mental health do not work in general but could also be an indication that the deployment and implementation so far has been unsuccessful. Also, we did not monitor or investigate whether the onboarding process happened in person or virtually which in turn might influence engagement. Engagement should be investigated in future studies.
Furthermore, the search was restricted to publications in English and German language. Due to the small amount of studies per disorder, the number of comparisons per disorder was limited, therefore not all study effects could be pooled, subgroup analyses were restricted, follow-up assessments were not examined, nor was publication bias explored. We originally planned to investigate (1) standalone smartphone apps for mental health and (2) hybrid apps and blended care apps. However, due to differing search strings and the already extensive scope of the primary research question, we decided to no longer investigate the second question within this manuscript.
Future research
Although the potential smartphones bear to deliver mental health treatment is evident, future research needs to clarify whether the present limited efficacy holds true and identify in which circumstances their potential could be increased. The development of digital mental health services should be user-driven and solution-focused, including app developers, researchers and clinicians in the process.37,40,41,42 It is important to investigate app features and components, which make smartphone apps unique delivery modalities, such as context sensing, constant access and availability, high likelihood that prompts are received in daily life, and the combination possibilities with physiological assessments. The feature-driven approach could be helpful to understand working mechanisms of apps for mental health. Therefore, more specific aspects of mobile apps should be investigated and systematically tested, as well as long-term effects. Apps need to be implemented by utilizing persuasive design aspects and by exploiting full technological potential, which might improve effectiveness. It is also very likely that engagement is linked to efficacy of apps for mental health, which is why adherence, user profiles, and usage patterns should be further investigated.
Conclusion
There remains a lack of generalizable evidence to support particular standalone smartphone apps for mental health as a substitute to conventional mental health treatment. Although we found a small effect for depression as well as indications for the use of apps for smoking and sleep problems, heterogeneity was substantial and overall risk of bias was high. Moreover, the insignificant findings on STBs, PTSD as well as alcohol use highlight the need for discussing the potential harm of currently available apps, which might keep users away from evidence-based interventions while bearing a substantial risk of being ineffective.
Methods
The review was conducted in accordance with the Cochrane Handbook for Systematic Reviews of Interventions and reporting is based on PRISMA.43,44 This study was registered in the International Prospective Register of Systematic Reviews of the National Institute for Health Research (https://www.crd.york.ac.uk/prospero/) under the ID CRD42017076515.
Eligibility criteria
We included (a) randomized controlled trials which (b) investigated the effects of a standalone psychological intervention for a specific mental health domain (c) delivered via a standalone smartphone app (d) aiming to reduce symptoms of a mental disorder or STBs (e) which the app was specifically targeted at. The trials must have included (f) an adult (≥18 years) population (g) with heightened symptom severity of a mental disorder according to DSM-IV or DSM-V45,46 or STBs (h) assessed by a diagnostic instrument or a predefined symptom cut-off (i) which was identical to the primary target of the study (j) compared to a control condition. Only (k) published peer-review articles (l) in English and German were considered. We decided to include STBs as they are pervasive among individuals with serious mental disorders.
A psychological intervention was defined as an intervention aimed at behavior change and reduction of mental disorder burden specifically designed and implemented with the intention to treat symptoms of mental disorders.
Search strategy
A systematic literature search was completed (until 8 February 2018) in Pubmed, PsycInfo, SCOPUS, Web of Science, and Cochrane Central Register of Controlled Trials. Key search terms included a combination of three major themes: smartphone apps and mobile health, mental disorders, and randomized controlled trials (search string for Pubmed Supplementary Methods).
Study selection
After duplicate removal, all titles and abstracts were screened for potential eligibility after which full text articles were assessed for eligibility. Study selection was performed by two independent researchers (K.K.W. and L.M.F.). Interrater reliability is reported for the initial agreement on full text eligibility where values of kappa are rated as fair (κ = 0.4–0.59), good (κ = 0.6–0.74), or excellent (κ > 0.75).47 Disagreement was resolved through discussion. If no consensus could be achieved, a third researcher was consulted (D.D.E.).
Data extraction
The following data was extracted: (a) authors, year of publication, citation, (b) study design (sample size, study inclusion criterion, type of control group, target outcomes), (c) sample characteristics (age, gender), (d) treatment (theory basis, app and intervention components), and (e) data for calculation of effect sizes (outcome data preferably intention-to-treat (ITT) data, study dropout rate, handling of missing data). If data was not retrievable from publication, study authors were contacted for clarification.
Quality assessment
Study quality was assessed independently by two researchers (K.K.W. and L.M.F.) based on the six basic criteria of the Cochrane Risk of Bias Assessment Tool: random sequence generation, allocation sequence concealment, blinding of participants and personnel, blinding of outcome assessors, incomplete outcome data, and selective reporting. Based on predefined definitions, studies were rated as “low”, “high”, or “unclear” risk of bias in each of these categories. When self-report measures were used to assess outcomes, blinding of outcome assessors were rated as not applicable (NA). When a study protocol or trial registration was identified and the primary outcome was reported as previously stated, selective outcome reporting was rated as low, if neither existed, selective reporting was rated as unclear. Studies which were rated as low on all available criteria were rated as overall low risk of bias. Interrater reliability of the risk of bias assessment is reported.
Statistical analyses
Trials with the same primary target outcome were pooled to generate a mean effect size for each investigated outcome. If more than one measurement per outcome was assessed, the mean of the effect sizes was used to provide one effect size per study per outcome, to generate a mean effect size, only instruments were used related to the primary measure of the disorder. For each comparison between a smartphone app treatment and a control condition we calculated the effect size Hedges’ g (g), the 95% confidence interval (95%CI) and P-value (P) for each target outcome based on the post-assessment values indicating the difference between the two groups (intervention group versus control group) at post-assessment. For additional interpretability from a clinical perspective the number needed to treat (NNT) is reported for positive significant effects according to the method by Kraemer and Kupfer.48 In cases in which too few comparisons (k < 3) were available to pool data, data is presented in a narrative synthesis. Due to expected heterogeneity between trials, a random effects model was applied in all analyses. If trials were multi-armed, reporting two comparisons to one comparison, we divided the sample size to avoid inflating power.43
Heterogeneity between trials is expressed by I2 and its 95% confidence interval to express the percentage of total variance which can be explained. It can roughly be divided into three thresholds: low (25%), moderate (50%), or high (75%).49 The confidence interval was calculated by using the formula provided by Borenstein.50
In an additional analysis, the overall effects of all comparisons providing data on anxiety and depression after treatment with a smartphone app were each considered, no matter outcome status as primary or secondary. Potential sources of heterogeneity between trials were investigated by conducting subgroup analyses on different types of control groups. The subgroup analyses were conducted according to the mixed-effect model, in this model subgroups are pooled with the random-effects model while tests for significant differences between subgroups are conducted with the fixed-effects model.
Indications for publication bias were explored by investigating the funnel plot visually, and conducting Egger’s test.51 To obtain an estimation of the pooled effect when accounting for missing studies, the Duval and Tweedie trim-and-fill analysis was performed.52
All statistical analyses were calculated with the comprehensive meta-analysis (CMA) software, version 3 (Biostat, Inc.).
Data availability
Data collected and used in this meta-analysis can be requested from the corresponding author.
References
Chan, S., Torous, J., Hinton, L. & Yellowlees, P. Towards a framework for evaluating mobile mental health Apps. Telemed. e-Health 21, 1038–1041 (2015).
Hollis, C. et al. Annual Research Review: digital health interventions for children and young people with mental health problems—a systematic and meta-review. J. Child Psychol. Psychiatry Allied Discip. 58, 474–503 (2017).
Substance Abuse and Mental Health Services Administration. Key Substance Use and Mental Health Indicators in the United States: Results from the 2016 National Survey on Drug Use and Health (2016).
Chisholm, D. et al. Scaling-up treatment of depression and anxiety: a global return on investment analysis. Lancet Psychiatry 3, 415–424 (2016).
Richards, D., Richardson, T., Timulak, L. & McElvaney, J. The efficacy of internet-delivered treatment for generalized anxiety disorder: a systematic review and meta-analysis. Internet Interv. 2, 272–282 (2015).
Barth, J. et al. Comparative efficacy of seven psychotherapeutic interventions for patients with depression: a network meta-analysis. PLoS Med. 10, 1–17 (2013).
Mojtabai, R. et al. Barriers to mental health treatment: results from the National Comorbidity Survey Replication. Psychol. Med. 41, 1751–1761 (2011).
Gulliver, A. et al. Perceived barriers and facilitators to mental health help-seeking in young people: a systematic review. BMC Psychiatry 10, 113 (2010).
Ebert, D. D. et al. Internet- and mobile-based psychological interventions: applications, efficacy, and potential for improving mental health: a report of the EFPA E-Health Taskforce. Eur. Psychol. 23, 167–187 (2018).
The Lancet Child & Adolescent Health. Growing up in a digital world: benefits and risks. Lancet Child Adolesc. Health 2, 90 (2018).
Aitkin, M., Clancy, B. & Nass, D. The Growing Value of Digital Health (IQVIA Institute for Human Data Science, 2017).
Radovic, A. et al. Smartphone applications for mental health. Cyberpsychol. Behav. Soc. Netw. 19, 465–470 (2016).
Terhorst, Y., Rathner, E. -M., Baumeister, H. & Sander, L. ‘Help from the App Store?’: a systematic review of depression apps in German app stores. Verhaltenstherapie https://doi.org/10.1159/000481692 (2018).
Husain, I. & Spence, D. Can healthy people benefit from health apps? BMJ 350, 8–10 (2015).
McCarthy, M. Experts warn on data security in health and fitness apps. BMJ 347, 57216 (2013).
Gostin, L. O., Halabi, S. F. & Wilson, K. Ethical collection, storage, and use of public health data. JAMA 302, 82 (2009).
Lim, S. L., Bentley, P. J., Kanakam, N., Ishikawa, F. & Honiden, S. Investigating country differences in mobile app user behavior and challenges for software engineering. IEEE Trans. Softw. Eng. 41, 40–64 (2015).
Donker, T. et al. Smartphones for smarter delivery of mental health programs: a systematic review. J. Med. Internet Res. 15, e247 (2013).
Menon, V., Rajan, T. & Sarkar, S. Psychotherapeutic applications of mobile phone-based technologies: a systematic review of current research and trends. Indian J. Psychol. Med. 39, 4 (2017).
Firth, J. et al. Can smartphone mental health interventions reduce symptoms of anxiety? A meta-analysis of randomized controlled trials. J. Affect. Disord. 218, 15–22 (2017).
Firth, J. et al. The efficacy of smartphone-based mental health interventions for depressive symptoms: a meta-analysis of randomized controlled trials. World Psychiatry 16, 287–298 (2017).
Franklin, J. C. et al. A brief mobile app reduces nonsuicidal and suicidal self-injury: evidence from three randomized controlled trials. J. Consult. Clin. Psychol. 84, 544–557 (2016).
Kuhn, E. et al. Preliminary evaluation of PTSD Coach, a smartphone app for post-traumatic stress symptoms. Mil. Med. 179, 12–18 (2014).
Miner, A. et al. Feasibility, acceptability, and potential efficacy of the PTSD Coach app: a pilot randomized controlled trial with community trauma survivors. Psychol. Trauma 8, 384–392 (2016).
Clarke, P. et al. Assessing the therapeutic potential of targeted attentional bias modification for insomnia using smartphone delivery. Psychother. Psychosom. 85, 187–189 (2016).
Horsch, C. H. et al. Mobile phone-delivered cognitive behavioral therapy for insomnia: a randomized waitlist controlled trial. J. Med. Internet Res. 19, e70 (2017).
Leigh, S. & Flatt, S. App-based psychological interventions: friend or foe? Evid. Based Ment. Health 18, 97–99 (2015).
Buntrock, C. et al. Effect of a web-based guided self-help intervention for prevention of major depression in adults with subthreshold depression. JAMA 315, 1854–1863 (2016).
Königbauer, J., Letsch, J., Doebler, P., Ebert, D. & Baumeister, H. Internet- and mobile-based depression interventions for people with diagnosed depression: a systematic review and meta-analysis. J. Affect. Disord. 223, 28–40 (2017).
Kampmann, I. L., Emmelkamp, P. M. G. & Morina, N. Meta-analysis of technology-assisted interventions for social anxiety disorder. J. Anxiety Disord. 42, 71–84 (2016).
Andrews, G., Cuijpers, P., Craske, M. G., McEvoy, P. & Titov, N. Computer therapy for the anxiety ad depressive disorders is effective, acceptable and practical health care: a meta-analysis. PLoS ONE 5, 313196 (2010).
Kuester, A., Niemeyer, H. & Knaevelsrud, C. Internet-based interventions for posttraumatic stress: a meta-analysis of randomized controlled trials. Clin. Psychol. Rev. 43, 1–16 (2016).
Zachariae, R., Lyby, M. S., Ritterband, L. M. & O’Toole, M. S. Efficacy of internet-delivered cognitive-behavioral therapy for insomnia—a systematic review and meta-analysis of randomized controlled trials. Sleep Med. Rev. 30, 1–10 (2016).
Baumeister, H., Reichler, L., Munzinger, M. & Lin, J. The impact of guidance on Internet-based mental health interventions—a systematic review. Internet Interv. 1, 205–215 (2014).
Ebert, D. D. et al. Restoring depleted resources: Efficacy and mechanisms of change of an internet-based unguided recovery training for better sleep and psychological detachment from work. Health Psychol. 34, 1240–1251 (2015).
Berger, T. et al. Effects of a transdiagnostic unguided Internet intervention (‘velibra’) for anxiety disorders in primary care: results of a randomized controlled trial. Psychol. Med. 47, 67–80 (2017).
Hickey, E., McMillan, B. & Mitchell, C. Practitioners should embrace, not ignore, health apps. BMJ 350, 2336 (2015).
Erbe, D., Eichert, H.-C., Riper, H. & Ebert, D. D. Blending face-to-face and internet-based interventions for the treatment of mental disorders in adults: systematic review. J. Med. Internet Res. 19, e306 (2017).
Schmädeke, S. & Bischoff, C. Wirkungen smartphonegestützter psychosomatischer Rehabilitationsnachsorge (eATROS) bei depressiven Patienten. Verhaltenstherapie 25, 277–286 (2015).
Hsin, H., Torous, J. & Roberts, L. An adjuvant role for mobile health in psychiatry. JAMA Psychiatry 73, 103–104 (2016).
Torous, J. & Roberts, L. W. Needed innovation in digital health and smartphone applications for mental health transparency and trust. JAMA Psychiatry 74, 437–438 (2017).
Torous, J., Nicholas, J., Larsen, M. E., Firth, J. & Christensen, H. Clinical review of user engagement with mental health smartphone apps: evidence, theory and improvements. Evid. Based Ment. Health ebmental-2018-102891 (2018). https://doi.org/10.1136/eb-2018-102891
Higgins, J. P. T. & Green, S. (editors). Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0 (The Cochrane Collaboration, 2011).
Liberati, A. et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. PLoS Med. 6, e1000100 (2009).
American Psychiatric Association. DSM-IV-TR: Diagnostic and Statistical Manual of Mental Disorders (American Psychiatric Publishing, 2000).
American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders (American Psychiatric Publishing, 2013).
Orwin, R. G. Evaluating coding decisions. In The Handbook of Research Synthesis (eds. Cooper, H. & Hedges, L. V.) 139–162 (Russel Sage Foundation, 1994).
Kraemer, H. & Kupfer, D. Size of treatment effects and their importance to clinical research and practice. Biol. Psychiatry 59, 990–6 (2006).
Higgins, J. P. T., Thompson, S. G., Deeks, J. J. & Altman, D. G. Measuring inconsistency in meta-analyses. BMJ Br. Med. J. 327, 557–560 (2003).
Borenstein, M., Hedges, L., Higgins, J. & Rothstein, H. Introduction to Meta-analysis (John Wiley & Sons, Ltd., 2016).
Egger, S. T. et al. The use of the health of the nation outcome scales for assessing functional change in treatment outcome monitoring of patients with chronic schizophrenia. Front. Public Health 4, 1–6 (2016).
Duval, S. & Tweedie, R. Trim and fill: a simple funnel-plot-based method of testing and adjusting for publication bias in meta-analysis. Biometrics 56, 455–463 (2000).
Arean, P. A. et al. The use and effectiveness of mobile apps for depression: results from a fully remote clinical tria. J. Med. Internet Res. 18, e330 (2016).
BinDhim, N. F., McGeechan, K. & Trevena, L. Smartphone smoking cessation application (SSC App) trial: a multicountry double-blind automated randomised controlled trial of a smoking cessation decision-aid ‘app’. BMJ Open 8, e017105, https://doi.org/10.1136/bmjopen-2017-017105 (2018).
Birney, A. J., Gunn, R., Russell, J. K. & Ary, D. V. Mood Hacker mobile web wpp with email for adults to self-manage mild-to-moderate depression: randomized controlled trial. JMIR mHealth uHealth 4, e8 (2016).
Dar, R. Effect of real-time monitoring and notification of smoking episodes on smoking reduction: a pilot study of a novel smoking cessation app. Nicotine Tob. Res. 20, 1515–1518 (2018).
Enock, P. M., Hofmann, S. G. & McNally, R. J. Attention bias modification training via smartphone to reduce social anxiety: a randomized, controlled multi-session experiment. Cognit. Ther. Res. 38, 200–216 (2014).
Gajecki, M. et al. Mobile phone brief intervention applications for risky alcohol use among university students: a randomized controlled study. Addict. Sci. Clin Pract. 9, 11 (2014).
Hur, J.-W., Kim, B., Park, D. & Choi, S.-W. A scenario-based cognitive behavioral therapy mobile app to reduce dysfunctional beliefsin individuals with depression: a randomized controlled trial. Telemed. e-Health 24, 710–716 (2018).
Kuhn, E. et al. A randomized controlled trial of a smartphone app forposttraumatic stress disorder symptoms. J. Consult. Clin. Psychol. 85, 267–273 (2017).
Pham, Q., Khatib, Y., Stansfeld, S., Fox, S. & Green, T. Feasibility and efficacy of an mHealth game for managing anxiety: “flowy” randomized controlled pilot trial and design evaluation. Games Health J. 5, 50–67 (2016).
Roepke, A. M. et al. Randomized controlled trial of super better, a smartphone-based/internet-based self-help tool to reduce depressive symptoms. Games Health J. 4, 235–246 (2015).
Stolz, T. et al. A mobile app for social anxiety disorder: A three-arm randomized controlled trial comparing mobile and PC-based guided self-help interventions. J. Consult. Clin. Psychol. 86, 493–504 (2018).
Tighe, J. et al. Ibobbly mobile health intervention for suicide prevention in australian indigenous youth: a pilot randomised controlled trial. BMJ Open 7, e013518 (2017).
Witkiewitz, K. et al. Development and evaluation of a mobile intervention for heavy drinking and smoking among college students. Psychol. Addict. Behav. 28, 639–650 (2014).
Acknowledgements
We would like to thank Patricia Arean, Kevin Hallgren, Reuven Dar, and Joseph Franklin for their quick and friendly response in providing original outcome data. This study was registered in the International Prospective Register of Systematic Reviews of the National Institute for Health Research (https://www.crd.york.ac.uk/prospero/) under the ID CRD42017076515. The author(s) received no specific funding for this work.
Author information
Authors and Affiliations
Contributions
K.K.W., D.D.E. and L.M.F. designed the study. K.K.W. and L.M.F. conducted the search, the inclusion decisions, and quality assessment, and D.D.E. provided expertize throughout the process. K.K.W. wrote the first draft of the manuscript under the supervision of D.D.E. and all authors contributed to the final version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
D.D.E. has served as a consultant to/on the scientific advisory boards of Sanofi, Novartis, Minddistrict, Lantern, Schoen Kliniken, Ideamed and German health insurance companies (BARMER, Techniker Krankenkasse) and a number of federal chambers for psychotherapy. D.D.E. and M.B. are also stakeholders of the Institute for Health Training Online (GET.ON), which aims to implement scientific findings related to digital health interventions into routine care. The rest of the authors declare that there are no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Weisel, K.K., Fuhrmann, L.M., Berking, M. et al. Standalone smartphone apps for mental health—a systematic review and meta-analysis. npj Digit. Med. 2, 118 (2019). https://doi.org/10.1038/s41746-019-0188-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41746-019-0188-8
This article is cited by
-
Effectiveness of mobile application interventions for stroke survivors: systematic review and meta-analysis
BMC Medical Informatics and Decision Making (2024)
-
Cognitive Behavioral Therapy for Insomnia Self-Management Mobile Apps: A Review of Efficacy and Quality
Journal of Clinical Psychology in Medical Settings (2024)
-
A Smart Solution? Efficacy of a Self-Management Smartphone App for Panic Disorder and Agoraphobia
Cognitive Therapy and Research (2024)
-
WhatsApp with the Evidence Base for Behavioral Parent Training Apps? A Systematic Review of Mobile Phone Applications
Journal of Child and Family Studies (2024)
-
Emerging Connection of the Mental Health and Well-Being Axis with Digital Technology: A Quantitative and Qualitative Study
Journal of Technology in Behavioral Science (2024)