Abstract
For restoration of extensively damaged teeth preprosthetic treatment measures are necessary. Crown lengthening and extrusion affect the prospective crown-root ratio (CRR). The subject of this in vitro study was to compute CRRs for both treatment approaches. 120 human maxillary central extracted incisors were measured. Measurements were calculated for five treatment groups: C (control), E-2 mm (extrusion of 2 mm), E-4 mm (extrusion of 4 mm), CL-2 mm (crown lengthening of 2 mm), and CL-4 mm (crown lengthening of 4 mm). Tooth (TL), root (RL), and crown lengths (CL) were measured from mesial (m) and facial (f) cemento-enamel junction (CEJ), and respective anatomic (CRR) and effective crown-root ratios (eCRR) were calculated. Following CRR values were computed for C: CRR-m = 0.4 ± 0.1, CRR-f = 0.7 ± 0.1. All crown-root ratios were lower (more favourable) for extrusion compared to crown lengthening (p < 0.001). ECRRs were higher than anatomic CRRs. CRR at mesial CEJ was significantly lower than CRR with facial CEJ as reference (p < 0.001). Mesial measurement-based calculations of CRR typically based on radiographic images should be interpreted with caution as they underestimate the eCRR. CRR can be expected as lower, i.e. more favourable, when teeth are extruded than crown lengthened.
Similar content being viewed by others
Introduction
The restoration of severely destroyed teeth when the clinical crown is lost is challenging. Tooth preservation with endodontic treatment, post-and-core, and crown restoration versus tooth extraction and subsequent implant placement have to be carefully considered and weighed up as equitable treatment alternatives1. As concrete clinical guidelines are not available dental practitioners tend to decide differently2. Due to alveolar bone loss after extraction3 implant placement is in particular in the esthetic zone of the maxillary anterior region regarded as a highly complex procedure4. Moreover, implant borne restorations are cost-intensive5 and post-operative complications such as perimucositis and periimplantitis are considered downsides for implant placement6.
In case of tooth restoration of severely compromised teeth many factors play a role in the treatment planning process: level of defect extension, apical condition of the tooth, tooth mobility score, attachment level, pocket probing depths, quality of endodontic filling, and the prospective crown-root ratio7,8,9. For long-term success of the restoration re-establishment of biologic width10 and a circumferential ferrule-design preparation11 are deemed necessary. Therefore, preprosthetic therapy options such as crown lengthening12 or extrusion13,14,15,16,17 have been suggested in literature for preservation and restoration of severely compromised teeth. Surgical crown lengthening is an operative procedure where surrounding bone level is reduced and “the extent of supragingival tooth structure is increased for restorative purposes”18. It is connected with an inevitable lengthening of the clinical crown in the same amount as the root will be less supported by surrounding alveolar bone12. Particularly in the esthetic zone this procedure may be disadvantageous, since the marginal contour will be disturbed. In contrast, extrusion is the occlusal movement of teeth “beyond the natural occlusal plane that occurs without accompanied movement of their supporting tissues”18. Extrusion allows placement of restorative margins above the gingival level re-establishing biologic width13. Extrusion may be achieved by orthodontic movement of the tooth16 as well as surgical extraction and replantation19. Crown lengthening and extrusion procedures affect the prospective crown-root ratio18. While for crown lengthening both crown and root lengths are altered, for extrusion only the root length within alveolar bone is reduced. The crown length remains constant. The crown-root ratio is defined as “the physical relationship between the portion of the tooth within the alveolar bone compared with portion not within the alveolar bone, as determined radiographically”18. Thereby it is important to differentiate among measurements of the anatomic and the effective crown length (Fig. 1): the anatomic crown is measured from the cemento-enamel junction (CEJ) to the incisal edge18 and does not provide information about the alveolar bone support. Therefore, the effective crown length is the portion of the tooth above the alveolar bone, while the effective root length is the portion within the alveolar bone20. In literature the crown-root ratio is classified by relatively vague terms such as “favourable”, “unfavourable”, “poor” and “unsatisfactory”21. Shillingburg et al. proposed a ratio of 1:1.5 as ideal and a ratio of 1:1 as minimum for abutment teeth22. However, both in vitro and clinical evidence to support this rule on definitive proportions is scarce23,24,25. Additionally, there are only few studies available that investigate the biomechanical impact of the crown-root ratio after extrusion in comparison to crown lengthening procedures20,26,27.
Therefore, this investigation aimed to calculate crown-root ratios with the example of maxillary central incisors after extrusion and crown lengthening procedures according to clinical demands. Null hypotheses tested were, that there is no difference in anatomic or effective crown-root ratio after simulated extrusion and crown lengthening, and irrespective whether calculations based on facial (i.e. “true”) or mesial (i.e. typically radiographic) measurements.
Materials and methods
An in vitro study design was chosen to establish definitive prospective crown-root ratios after simulated extrusion and crown lengthening procedures. Ethical approval was obtained from the local ethics committee at the Charité—Universitätsmedizin Berlin, Germany, at the Department of Prosthodontics, Geriatric Dentistry and Craniomandibular Disorders (approval number: EA1/034/06). Informed consent was obtained from all subjects and/or their legal guardian(s). This research was conducted considering the CRIS Guidelines (Checklist for Reporting In-Vitro Studies). Post-hoc power-analysis was performed with a free-to use software to calculate statistical power (G* Power 3.1.9.7; Heinrich-Heine-Universität Düsseldorf) with a sample size of n = 120, α = 0.05 resulting in a power of 0.99 (99%).
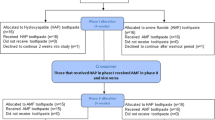
128 human maxillary central extracted incisors were examined from a tooth reservoir at the Department of Prosthodontics, Geriatric Dentistry and Craniomandibular Disorders of the Charité —Universitätsmedizin Berlin, Germany. Maxillary central incisors with sound tooth structures were included. Teeth with root resorptions, restorations, carious lesions, erosive, and wedge-shaped defects were excluded. Figure 1 defines examined variables. Measurements were performed for 128 teeth and calculated for five experimental treatment groups (Fig. 2): C (control), E-2 mm (extrusion of 2 mm), E-4 mm (extrusion of 4 mm), CL-2 mm (crown lengthening of 2 mm), and CL-4 mm (crown lengthening of 4 mm). Tooth lengths (TL) in [mm] were recorded with the aid of a caliper gauge (HSL 246-15; Hammacher, Solingen, Germany) with a measurement error of 0.01 mm from the incisal edge to the apex of the tooth. The most apical point on the facial (f) aspect of the CEJ and the most coronal point of the mesioproximal CEJ served as reference points for measurement. Root and crown lengths (RL/CL) were measured from the mesioproximal and facial CEJ, respectively. Normal distribution was assessed based on RL-measurements. Assuming a biological width of 2 mm effective crown and root lengths (eCL/eRL) were calculated based on following formulas: eCL = CL + 2 mm and eRL = CL-2 mm. Thereafter, anatomic crown-root ratios (CRR) and effective crown-root ratios (eCRR) were calculated for all specimens. Mean values and standard deviations of measurements are displayed in Table 1. Descriptive statistics were performed with the aid of a statistical software (IBM SPSS Statistics 25; IBM, Armonk NY, USA). T-tests were performed for statistical comparison between groups. The significance level was set at p < 0.05.
Results
Root lengths (RL) of 128 teeth were measured. Eight teeth were excluded from further analyses due to their extreme short and long root lengths, respectively. Table 1 summarizes tooth length (TL), crown length (CL) from facial (f), and mesioproximal aspect (m), root length (RL), effective measurements (e), and resulting crown-root ratios (CRR). For maxillary central incisors, the following mean [± SD] anatomic crown-root ratios (CRR) and effective crown-root ratios (eCRR) were recorded: CRR-m = 0.4 [± 0.1], CRR-f = 0.7 [± 0.1], eCRR-m = 0.6 [± 0.1] and eCRR-f = 1.0 [± 0.8]. Comparing measurements for extrusion of 2 mm with crown lengthening of 2 mm all crown-root ratios are lower for extrusion (p < 0.001). For extrusion of 4 mm (E-4 mm) and for crown lengthening of 4 mm (CL-4 mm) all crown-root ratios are lower for extrusion with p < 0.001 (Fig. 3). Values for CRRs were significantly different between all theoretical treatment groups (p ≤ 0.001). Thereby, effective crown-root ratios were higher than anatomic crown-root ratios. CRR referring to mesial CEJ was lower than CRR referring to facial CEJ (Fig. 4).
Discussion
This is the first study that provides “real-life” and exact crown-root ratios after measurement of 120 extracted teeth and compares extrusion with crown lengthening procedures for the assumed clinical case of a missing clinical crown of a maxillary central incisor, i.e. the tooth crown is missing at a gingival level. It was shown, that mesial measurement-based calculations of crown-root ratios typically based on radiographic images should be interpreted with caution as they underestimate (appearing as more favourable) the effective crown-root ratio. Prospective crown-root ratios are lower, i.e. more favourable for extrusion than for crown lengthening procedures. Therefore, both null hypotheses were rejected. The mean effective crown-root ratio measured at the mesial CEJ for maxillary central incisors without preprosthetic treatment measures was 0.6 and the mean effective crown-root ratio measured at the facial CEJ was 1.0, respectively. The eCRR for 2 mm of extrusion was 22% lower compared to the crown lengthening group of 2 mm. For 4 mm of extrusion eCRR was even 30% lower than in the crown lengthening group. Hence, with an inevitable lengthening of the clinical crown due to crown lengthening to enable a reconstruction of the damaged tooth, the crown length is increased while the effective root length, i.e. the part of the root supported by alveolar bone, is decreased. Thus, two parameters have a potential negative impact on the crown-root ratio. In contrast, extrusion changes only one parameter. The effective crown length remains constant, while effective root length decreases. Therefore, in regard to the resulting prospective crown-root ratio extrusion may be favoured over crown lengthening14,15.
The study investigated maxillary central incisors as this region was described as “high risk” area for mechanical failure28 and is functionally and aesthetically of utmost interest. In the anterior region non-axial shear forces occur, whereas in the posterior region axial, compressive forces are more likely. Therefore, anterior restorations are much more susceptible to technical complications.
However, it is one of the limitations of this in vitro study that solely maxillary central incisors were investigated. Crown-root ratios of premolars and molars as well as maxillary and mandibular incisors may be different. Moreover, based on the present results the impact of CRR on long-term clinical success of restorations still remains uncertain, since additional factors play a role. Further, surgical crown lengthening procedures may be contraindicated in the anterior region for aesthetic reasons as they are accompanied by a lengthening of the clinical crown, and an osseous reduction of the alveolar bone is disadvantageous in the context of a possible prospective implant placement. In contrast, for orthodontic extrusion procedures a tendency for marginal bone gain has been observed in a clinical pilot-study investigation29.
Tooth, crown, and root lengths in this study are in line with published data30. They can therefore serve as a reliable basis for calculation of prospective crown-root ratios. Data show that crown-root ratios are highly dependent on measurement methods. The study presented four different measurements with different reference points for the crown-root ratio: crown-root ratios ranging from 0.4 to 2.2, respectively. They are higher if measured from facial in comparison to mesioproximal CEJ in all groups, which would be typically calculated based on X-rays. Effective crown-root ratios exceed a value of 1 in all experimental groups, if measured facially. Data show that crown-root ratios measured at the mesial aspect account to nearly 60% of the crown-root ratios measured at the facial aspect. This finding leads to a miscalculation of the “true” crown-root ratio as the lever arm is much higher than assumed prior to restorative treatment decisions. However, the anatomic “true” crown-root ratio measured from facial aspect may not be determined clinically nor radiographically. Ultimately, the only clinical possible measurement method for determination of CRR is the e-CRR-m as it may be determined radiographically at the proximal marginal bone level31. Therefore, measurements of crown-root ratios based on radiographic images should be interpreted with caution as they underestimate the anatomic crown to root relation.
Scientific evidence on the impact of specific crown-root ratios on biomechanical behaviour is rather low: An in vitro study has demonstrated a reduction of static load failure for decoronated mandibular second premolars after crown lengthening procedures and in presence of a ferrule20. Results are in accordance with another in vitro study showing that extrusion method reduced the crown-root ratio fewer and increased the root-fracture resistance more than crown-lengthening method26,27. However, studies are missing to establish distinctive proportions leaving the general practitioner with vague terms as “unfavourable”, “favourable”, “poor” and “good”. Moreover, clinical studies on the biomechanical impact of altering crown-root ratios are scarce, especially in regard to teeth that underwent extrusion. A review has attributed to a lack of clinical data on the impact of crown-root ratio on long-term prognosis in general23. One of the few longitudinal clinical studies investigated 236 clasp-retained removable partial dentures and found a significant risk for abutment failure with a crown-root ratio exceeding 1.024. Other authors also found a positive correlation between the crown-root ratio and long-term prognosis for patients with periodontitis under maintenance for 5 years32. A clinical study evaluated the impact of the crown-root ratio on the 10-years survival rate of endodontically treated teeth after surgical crown lengthening and concluded that an “inadequate” crown-root ratio exceeding 1.0 has a negative impact on long-term survival25. For orthodontic extrusion long-term clinical data are scarce and mostly limited to case reports and case series13,16,17. Studies, both in vitro and in vivo have to evaluate the biomechanical impact of altering crown-root ratios on both treatment concepts in future.
Conclusions
While for extrusion only root length is reduced (crown length unaltered), for crown lengthening root length is reduced as much as crown length is enlarged. Hence, prospective crown-root ratios are lower, i.e. more favourable for extrusion than for crown-lengthening procedures. Mesial measurement-based calculations of CRR based on radiographic images should be interpreted with caution as they underestimate (appearing as more favourable) the effective CRR.
Data availability
The data presented in this article are available from the corresponding author upon reasonable request.
References
Torabinejad, M. et al. Outcomes of root canal treatment and restoration, implant-supported single crowns, fixed partial dentures, and extraction without replacement: A systematic review. J. Prosthet. Dent. 98, 285–311. https://doi.org/10.1016/S0022-3913(07)60102-4 (2007).
Turp, J. C. et al. Restoring the fractured root-canal-treated maxillary lateral incisor: In search of an evidence-based approach. Quintessence Int. 38, 179–191 (2007).
Tan, W. L., Wong, T. L., Wong, M. C. & Lang, N. P. A systematic review of post-extractional alveolar hard and soft tissue dimensional changes in humans. Clin. Oral Implants Res. 23(Suppl 5), 1–21. https://doi.org/10.1111/j.1600-0501.2011.02375.x (2012).
Buser, D., Chappuis, V., Belser, U. C. & Chen, S. Implant placement post extraction in esthetic single tooth sites: When immediate, when early, when late? Periodontology 2000(73), 84–102. https://doi.org/10.1111/prd.12170 (2017).
Pennington, M. W. et al. Evaluation of the cost-effectiveness of root canal treatment using conventional approaches versus replacement with an implant. Int. Endod. J. 42, 874–883. https://doi.org/10.1111/j.1365-2591.2009.01582.x (2009).
Derks, J. et al. Effectiveness of implant therapy analyzed in a Swedish population: Prevalence of peri-implantitis. J. Dent. Res. 95, 43–49. https://doi.org/10.1177/0022034515608832 (2016).
Reynolds, J. M. Abutment selection for fixed prosthodontics. J. Prosthet. Dent. 19, 483–488. https://doi.org/10.1016/0022-3913(68)90064-4 (1968).
Nyman, S. R. & Lang, N. P. Tooth mobility and the biological rationale for splinting teeth. Periodontology 2000(4), 15–22. https://doi.org/10.1111/j.1600-0757.1994.tb00002.x (1994).
Sorensen, J. A. & Martinoff, J. T. Endodontically treated teeth as abutments. J. Prosthet. Dent. 53, 631–636. https://doi.org/10.1016/0022-3913(85)90008-3 (1985).
Schatzle, M. et al. The influence of margins of restorations of the periodontal tissues over 26 years. J. Clin. Periodontol. 28, 57–64. https://doi.org/10.1034/j.1600-051x.2001.280109.x (2001).
Naumann, M., Schmitter, M., Frankenberger, R. & Krastl, G. Ferrule comes first. Post is second fake! News and alternative facts? A systematic review. J. Endod. 44, 212–219. https://doi.org/10.1016/j.joen.2017.09.020 (2018).
Lanning, S. K., Waldrop, T. C., Gunsolley, J. C. & Maynard, J. G. Surgical crown lengthening: Evaluation of the biological width. J. Periodontol. 74, 468–474. https://doi.org/10.1902/jop.2003.74.4.468 (2003).
Heithersay, G. S. Combined endodontic-orthodontic treatment of transverse root fractures in the region of the alveolar crest. Oral Surg. Oral Med. Oral Pathol. 36, 404–415. https://doi.org/10.1016/0030-4220(73)90220-x (1973).
Assif, D., Pilo, R. & Marshak, B. Restoring teeth following crown lengthening procedures. J. Prosthet. Dent. 65, 62–64. https://doi.org/10.1016/0022-3913(91)90049-3 (1991).
Ivey, D. W., Calhoun, R. L., Kemp, W. B., Dorfman, H. S. & Wheless, J. E. Orthodontic extrusion: Its use in restorative dentistry. J. Prosthet. Dent. 43, 401–407. https://doi.org/10.1016/0022-3913(80)90209-7 (1980).
Ingber, J. S. Forced eruption: Part II: A method of treating nonrestorable teeth—Periodontal and restorative considerations. J. Periodontol. 47, 203–216. https://doi.org/10.1902/jop.1976.47.4.203 (1976).
Reichardt, E. et al. Orthodontic forced eruption of permanent anterior teeth with subgingival fractures: A systematic review. Int. J. Environ. Res. Public Health. https://doi.org/10.3390/ijerph182312580 (2021).
Ferro K.J. et al. The Glossary of Prosthodontic Terms https://doi.org/10.1016/j.prosdent.2016.12.001 (2017). .
Krug, R. et al. Surgical extrusion with an atraumatic extraction system: A clinical study. J. Prosthet. Dent. 120, 879–885. https://doi.org/10.1016/j.prosdent.2018.02.006 (2018).
Gegauff, A. G. Effect of crown lengthening and ferrule placement on static load failure of cemented cast post-cores and crowns. J. Prosthet. Dent. 84, 169–179. https://doi.org/10.1067/mpr.2000.107583 (2000).
Tylman, S.D., Malone, W.F.P, Koth L.D. Tylman's theory and practice of fixed prosthodontics (ed. Tylman, S.D.) 67–8 (MDMI, 1989)67–8 (1989).
Shillingburg, H. T., Hobo, S., Whitsett, L. D., Jacobi, R. & Brackett, S. E. Treatment planning for the replacement of missing teeth. In Fundamentals of Fixed Prosthodontics (ed. Shillingburg, H. S.) 89–90 (Quintessence Publishing Comp. Inc, 1997).
Grossmann, Y. & Sadan, A. The prosthodontic concept of crown-to-root ratio: A review of the literature. J. Prosthet. Dent. 93, 559–562. https://doi.org/10.1016/j.prosdent.2005.03.006 (2005).
Tada, S. et al. The impact of the crown-root ratio on survival of abutment teeth for dentures. J. Dent. Res. 94, 220S-225S. https://doi.org/10.1177/0022034515589710 (2015).
Patil, K., Khalighinejad, N., El-Refai, N., Williams, K. & Mickel, A. The effect of crown lengthening on the outcome of endodontically treated posterior teeth: 10-year survival analysis. J. Endod. 45, 696–700. https://doi.org/10.1016/j.joen.2019.02.006 (2019).
Meng, Q. F. et al. Fracture resistance after simulated crown lengthening and forced tooth eruption of endodontically-treated teeth restored with a fiber post-and-core system. Am. J. Dent. 22, 147–150 (2009).
Meng, Q. F., Chen, Y. M., Guang, H. B., Yip, K. H. & Smales, R. J. Effect of a ferrule and increased clinical crown length on the in vitro fracture resistance of premolars restored using two dowel-and-core systems. Oper. Dent. 32, 595–601. https://doi.org/10.2341/06-169 (2007).
Torbjorner, A. & Fransson, B. Biomechanical aspects of prosthetic treatment of structurally compromised teeth. Int. J. Prosthodont. 17, 135–141 (2004).
Bruhnke, M., Beuer, F., Bose, M. W. H. & Naumann, M. Forced orthodontic extrusion to restore extensively damaged anterior and premolar teeth as abutments for single-crown restorations: Up to 5-year results from a pilot clinical study. J. Prosthet. Dent. 129, 61–68. https://doi.org/10.1016/j.prosdent.2022.08.033 (2023).
Schumacher, G.-H. Odontographie: Anatomie der Zähne und des Gebisses (Dr. Alfred Hüthig Verlag, 1983).
Pepelassi, E. A. & Diamanti-Kipioti, A. Selection of the most accurate method of conventional radiography for the assessment of periodontal osseous destruction. J Clin. Periodontol. 24, 557–567. https://doi.org/10.1111/j.1600-051x.1997.tb00229.x (1997).
McGuire, M. K. & Nunn, M. E. Prognosis versus actual outcome: II: The effectiveness of clinical parameters in developing an accurate prognosis. J. Periodontol. 67, 658–665. https://doi.org/10.1902/jop.1996.67.7.658 (1996).
Funding
Open Access funding enabled and organized by Projekt DEAL.
Author information
Authors and Affiliations
Contributions
M.B. wrote the original draft, supervised and visualized data. I.V. performed formal analysis, data curation and investigation. G.S. was responsible for the conception, design of the work and writing—review and editing. F.B. contributed to the conception and interpretation of data. M.N. developed the conception and contributed to writing—review and editing.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Bruhnke, M., Voß, I., Sterzenbach, G. et al. Evaluating the prospective crown-root ratio after extrusion and crown lengthening procedures in vitro. Sci Rep 13, 18899 (2023). https://doi.org/10.1038/s41598-023-46354-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-023-46354-y
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.