Abstract
Endotracheal tube (ET) misplacement is common in pediatric patients, which can lead to the serious complication. It would be helpful if there is an easy-to-use tool to predict the optimal ET depth considering in each patient’s characteristics. Therefore, we plan to develop a novel machine learning (ML) model to predict the appropriate ET depth in pediatric patients. This study retrospectively collected data from 1436 pediatric patients aged < 7 years who underwent chest x-ray examination in an intubated state. Patient data including age, sex, height weight, the internal diameter (ID) of the ET, and ET depth were collected from electronic medical records and chest x-ray. Among these, 1436 data were divided into training (70%, n = 1007) and testing (30%, n = 429) datasets. The training dataset was used to build the appropriate ET depth estimation model, while the test dataset was used to compare the model performance with the formula-based methods such as age-based method, height-based method and tube-ID method. The rate of inappropriate ET location was significantly lower in our ML model (17.9%) compared to formula-based methods (35.7%, 62.2%, and 46.6%). The relative risk [95% confidence interval, CI] of an inappropriate ET location compared to ML model in the age-based, height-based, and tube ID-based method were 1.99 [1.56–2.52], 3.47 [2.80–4.30], and 2.60 [2.07–3.26], respectively. In addition, compared to ML model, the relative risk of shallow intubation tended to be higher in the age-based method, whereas the risk of the deep or endobronchial intubation tended to be higher in the height-based and the tube ID-based method. The use of our ML model was able to predict optimal ET depth for pediatric patients only with basic patient information and reduce the risk of inappropriate ET placement. It will be helpful to clinicians unfamiliar with pediatric tracheal intubation to determine the appropriate ET depth.
Similar content being viewed by others
Introduction
Pediatric endotracheal intubation is mandatory in elective surgery and critically ill children1,2. However, endotracheal tube (ET) misplacement is common in pediatric patients with short tracheal lengths compared to adults; thus, it is challenging to determine the appropriate depth of ET3,4,5. Deep placement of the tip of the ET can irritate the carina, causing sympathetic stimulation. This may lead to tachycardia, hypertension, and bronchospasm6. Furthermore, endobronchial intubation may result in serious complications such as atelectasis, hypoxemia, barotrauma, and pneumothorax7. By contrast, shallow placement of the tip of the ET increases the risk of accidental extubation during manipulation of surgery or postural change8.
Several methods have been proposed to determine the appropriate ET placement. Methods for determining the appropriate depth of ET include age, height, ET internal diameter (ID)-based formulas, chest X-ray-based methods, and fiberoptic bronchoscopy9,10. Previous studies have shown that these methods have limitations in clinical practice due to the lack of accuracy of formula-based methods and the inconvenience of using the equipment.
Application of machine learning techniques related to this study
With the development of machine learning approaches in recent years, a subfield of artificial intelligence which can automatically learn from big data and then artificially and independently make decisions upon the knowledge, now machine learning is widely applied to the medical field. Machine learning was applied to a broad range of problems in medicine such as medical diagnosis, medical treatment, medical education, and drug development including coronavirus research. For example, in radiological diagnosis, deep learning algorithm, a type of machine learning, was developed for brain tumor segmentation using MRI multi-modalities brain images12. Machine learning-based ultrasonographic image analysis, which was invented by Nguyen DT, showed he best performance for thyroid nodule classification13. In the field of medical treatment, machine learning technology also plays a crucial in the intensive care unit (ICU). For instance, the application of wireless sensor networks based on machine learning can be used to collect patient information, and reduce false alarms ensuring patient data security and patient safety, and lowering the power consumption and price14. Also, artificial intelligence could help scientists develop better medicines faster and improve clinical trial processes and cut down the research and development costs and time period15.
Recently, machine learning (ML) techniques have been applied to diverse areas in anesthesiology16. ML has shown relatively accurate performance in predicting and solving problems such as prediction of clinical outcomes and medical image classification17,18. ML-assisted individualized hemodynamic management in high-risk surgery can reduce the incidence and duration of intraoperative hypotension19,20. An endotracheal intubation training program using virtual reality (VR) has been developed in airway management by applying an ML technique through user feedback21. In addition, our previous study demonstrated that ML could predict the appropriate intubation depth more accurately than the conventional formula-based method in pediatric patients22. However, the sample size used in the study was very small. Thus, it was insufficient to verify the performance and clinical usefulness of the proposed ML model.
Significance of the study
In this study, the ML approaches were employed for predicting endotracheal tube depth compared to formula-based methods based on age, height, and tube. To the best of our knowledge, this is the first study to predict the optimal endotracheal tube depth incorporating four basic patient information by using ML algorithms.
We have assumed that ML methods can reduce the risk of inappropriate ET positioning. Therefore, we have developed a new ML model for predicting the optimal endotracheal tube depth for actual intubation in pediatric patients. The primary objective of this study is to compare the inappropriate positioning incidence rates of the ML model and conventional formula-based methods. The secondary objective is to identify the relative risk of inappropriate locations in formula-based methods compared with the ML model.
Methodology
This study retrospectively collected data from pediatric patients aged < 7 years who underwent chest X-ray examination in an intubated state at Samsung Medical Center from January 1, 2015 to Jan 30, 2022. The Institutional Board of Samsung Medical Center (Seoul, Korea; Chairperson Prof. Hojoong Kim, M.D.; Approval Number: SMC 2021-07-049; July 12, 2021) approved this study. The institutional review board waived the requirement for informed consent from patients owing to the retrospective design. The current study was conducted in accord with ethical guidelines of the Declaration of Helsinki of the world medial association. The exclusion criteria were tracheal or vertebral abnormalities, preoperative tracheostomies, and chest X-rays of insufficient quality.
Data acquisition
Of 1573 pediatric patient records, 30 and 14 were excluded due to preoperative tracheostomies and low-quality chest X-rays, respectively, and 93 with missing data were also excluded. Finally, 1436 data records were used as the prediction model datasets. Patient data, including age, sex, height, weight, the internal diameter of the endotracheal tube (ET ID), and fixed ET depth, were collected from electronic medical records. The distance was measured using the caliper function of the picture archival and communication system (PACS, Centricity Enterprise Web V3.0, GE Healthcare, USA). For chest X-ray data, the distance from the carina to the upper margin of the first thoracic vertebral body (T1), distance from the carina to the lower margin of the third thoracic vertebral body (T3), and distance from the carina to the tip of the ET were measured using PACS. We assumed that the optimal location of the ET tip lies between the T1 upper margin and T3 lower margin23,24.
Data preprocessing and data split
In resuscitation or general anesthesia, endotracheal tube depth is frequently estimated using the Advanced Pediatric Life Support (APLS) guidelines. Various methods have been described for accurate tube positioning including age, height, and ETT internal diameter (ID). Other study have shown that the length of trachea may vary according to gender25. Moreover, weight can be the independent variable for the length of the orotracheal tube in previous study26. Therefore, in this study, only baseline characteristics such as age, gender, height, and weight, which can be easily known before performing intubation, were selected as input values for the model.
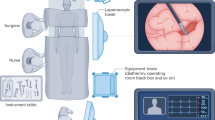
The dataset features included four variables: age, sex, height, and weight (Fig. 1). The target depth of ET was derived using the distance from the carina to the ET tube tip measured on chest radiography and the fixed depth value of ET on electronic medical records. When the tube tip was located at the center between the upper margin of T1 and the lower margin of T3, The fixed ET value was used as the target depth.
Process to estimate optimal depth of endotracheal tube using machine learning model. (A) Acquire the recorded value of (a) fixed ETT depth from the electronic medical record and measure the distance from the carina to the tracheal tube tip (b) on the chest X-ray. Then, assume that the median of the distance from the carina to the upper margin of T1 and the distance from the carina to the lower margin of T3 is the optimal tracheal tube tip position (C). Finally, the ETT optimal depth value is derived by moving (a) as much as the distance that (b) has moved to the position of (c). (B) Applying to machine learning model.
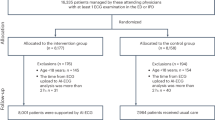
We separated 1436 records into training (1007/1436, 70%) and testing (429/1436, 30%) datasets (Fig. 2). We performed fivefold cross-validation to develop the ML prediction model. The training dataset was used to build the optimal ET depth estimation model, while the test dataset was used to compare the model performance with the formula-based methods. We standardized the training set to maintain the parameters (mean and standard deviation values, respectively) for each feature. These parameters are applied to transform the test set.
Prediction model development
Elastic net
We used an elastic net to develop the ML model for predicting the optimal depth of endotracheal intubation27,28. Regression is widely used to form a model to predict numeric values. Simple linear regression analysis is a technique that assumes a linear relationship between inputs and the target variable. Regularization was added to the loss function of linear regression to enhance the prediction accuracy and interpretability of the resulting predictive model with smaller coefficient values. Elastic net is a regularized regression method that linearly combines two popular penalties, specifically ridge and lasso functions to prevent overfitting the model.29. This is also known as a shrinkage and selection method which contains both the L1 and L2 penalties of the Lasso and Ridge regression. Imposing this penalty means that the coefficient values are reduced towards zero allowing the less contributive variables to have a coefficient close to zero (like ridge regression) or equal zero (like lasso regression). We implemented the models using R, version 4.1.2 (The R Foundation)30.
The elastic net allows tuning of the penalty term of the Eq. (1) requiring the selection of a tuning parameter (α, lambda).
The parameter α determines the type of shrinkage, with Lasso (α = 1 in the equation above) or Ridge (α = 0) regression. A value of α is set between 0 and 1. The amount of shrinkage can be fine-tuned using the penalty parameter λ called lambda (λ).
Prediction of ET depth
Machine learning model
We provided the inputs, including age, sex, height, weight, and the target depth of ET, as the training data in the elastic net algorithm. Therefore, if new patient data (age, sex, height, and weight) were entered into the built model, the ET depth was derived such that the ET was located at the optimal depth.
Formula-based methods
For the formula based on age, the insertion depth was estimated to be 9 cm for those aged 0–6 months, 10 cm for those aged 6–12 months, and 11 cm for those under 2 years31. In children older than 2 years, the tube depth was estimated using the pediatric advanced cardiac life support formula (tube depth [cm] = 12 + age [years]/2)32,33. For the height-based formula, we used the Morgan and Steward formula (tube depth [cm] = height [cm]/10 + 5)34. For the tube ID-based formula, the insertion depth was estimated using the formula: 3 x (tube ID)35.
Performance evaluation
Appropriate predictions of ET depth were defined as ET placed between the T1 upper margin and the T3 lower margin; any other location was an inappropriate prediction. Inappropriate predictions were divided into shallow, deep, and bronchial intubations. Deep intubation was defined as when the tip of the ET was located below the lower border of T3. Bronchial intubation was defined when the tip of the ET was located below the carina. Conversely, if the tip of the ET was located above the T1 upper border, it was defined as shallow intubation.
Performance indices
The Performance of each model was evaluated using five well-known indices i.e., coefficient of correlation (R2), mean square error (MSE), root mean square error (RMSE), mean absolute error (MAE), and variance account for (VAF)36,37. The following Eqs. (2)–(6) represent the formula that was used for calculating the mentioned performance indices for testing data38,39.
where y depicts the measured values, \(\overline{y }\) and y’ indicate mean and predicted of the y, respectively, n is the total number of data.
Statistical analysis
Summary of descriptive statistics includes frequencies (%) and medians [interquartile ranges. Student’s t-test, Wilcoxon rank-sum test, Pearson’s χ2 test, and Fisher’s exact test analyzed the differences between the training and test sets. Relative risks and 95% confidence intervals (CIs) were calculated depending on the scenario. The relative risk and 95% CIs, excluding 1, were considered statistically significant. Differences and 95% CIs, excluding 0, were considered statistically significant. All statistical analyses were performed using MedCalc® Statistical Software version 20.014 (MedCalc Software Ltd, Ostend, Belgium; https://www.medcalc.org; 2021) and R, version 4.1.2 (The R Foundation). We used 2-tailed tests in all analyses, with P values < 0.05 considered statistically significant.
Result and discussion
In this retrospective study, we evaluated 1573 pediatric patients for eligibility, from which 134 records were excluded, as discussed in the above sections. Therefore, 1436 patients were separated into training (70%, n = 1007) and test (30%, n = 429) sets. Patient characteristics are shown in Table 1. The patient characteristics were not statistically different between the training and test datasets.
We evaluated the prediction performance of the elastic net model with the isolated testing data set (n = 429). To compare the prediction performance of our proposed model with those of other ML models, we separately trained the following models: support vector machine, random forest, and artificial neural network. We evaluated the prediction performance of these ML models as well as formula-based methods.
The values of the performance indices of the models are presented in Table 2. The results of the evaluation showed that the elastic net model predicts the optimal depth of endotracheal intubation with lower MSE, RMSE, and MAE, and with a high R2 and VAF in test data. The frequency and percentage of the test datasets predicting the appropriate and inappropriate depth prediction for each method are presented in Table 3 and Fig. 3. The frequency (rate) of inappropriate locations in the machine learning model was 77 (17.9%). The frequency (rate) of inappropriate places was 153 (35.7%), 267 (62.2%), and 200 (46.6%) for the age-based, height-based, and tube ID-based method, respectively. In addition, the relative risk [95% confidence interval, CI] ET location in an inappropriate position in the age-based method, height-based method, and tube ID-based method were 1.99 [1.56–2.52], 3.47 [2.80–4.30], and 2.60 [2.07–3.26], respectively compared to ML models (Table 4). The formula-based method's relative risk of being in an inappropriate position was significantly higher.
Inappropriate ET depths were categorized into shallow, deep, and endobronchial intubations, as shown in Table 3. In the ML model, shallow, deep, and endobronchial intubation rates were 6.8%, 10.3%, and 0.9%, respectively. Among formula-based methods, shallow placement was frequently observed in the age-based method, and deep and endobronchial placement was commonly observed in the height-based and tube ID-based methods. The relative risk [95% CI] of ET location in the shallow was higher as 3.34 [2.26–4.93] in the age-based method compared to the ML model. By contrast, the relative risk of ET location in the deep and endobronchial placement was significantly higher in the height-based method and the tube ID-based method (Table 4).
Additionally, we have developed a web application to predict pediatric patients’ appropriate depth based on the proposed ML model (Fig. 4., web address: https://anurl.shinyapps.io/ETT_depth).
Conventional formula-based methods calculated the insertion depth of the ET based on only one specific variable. Morgan's height formula assumes that the length of the trachea is proportional to the height of the pediatric patient. That height is considered the most critical factor in determining ET depth34. Although the trachea length and height were correlated, the rate at which the appropriate ET depth was observed was only 43%23,40. In addition, in the weight-based method proposed by Gill et al., the ET tube was located in inappropriate positions in 56% of cases, in deep positions in 52% of patients41. The prediction of ET depth using a single biological variable cannot be applied to actual clinical practice due to the low accuracy. Therefore, it is essential to develop a new model for estimating the insertion depth of ET considering the various characteristics of pediatric patients.
The proposed ML model can derive the ET depth by considering four variables: age, gender, height, and weight. As the input values consist of fundamental patient information, it is easy to obtain the required information. In addition, the input value of the optimal ET depth obtained from the chest X-ray, regarded as the gold standard for determining the ET depth, can improve the accuracy of the results. The prediction accuracy was in the range of 38–64% with previous a single variable but increased to 82% with four variables. Furthermore, the relative risk of ET located at an inappropriate depth (shallow, deep, and endobronchial) was significantly lower in the ML model than in formula-based methods.
An ML model is helpful for anesthesiologists who are unfamiliar with pediatric airway management. Artificial intelligence (AI) uses advanced mathematical models to find connections into complex data determined by human intelligence alone. An ML-based intubation-assisted device could identify the creation of label vocal cords and tracheal rings in the airway tract on a real-time video screen, and the sensitivity and specificity were up to 89% and 98%42. In this study, we have also developed an ML model as a web application so that anyone can easily access the prediction model and predict the appropriate ET depth. A potential future application of AI can be recognizing the airway structure of each patient and guiding the proper ET depth in pediatric airway management43.
Conclusion
The appropriate insertion depth of an endotracheal tube (ET) should be determined for pediatric patients because both deep and shallow intubation may result in serious complications related to endotracheal tube misplacement. It would be helpful if there is an easy-to-use tool to predict the optimal ET depth considering in each patient's characteristics. Therefore, we developed and validated ML models to predict the appropriate ET depth in pediatric patients. The proposed ML model accurately predicted the appropriate depth of the ET with adequate accuracy (83%) compared to formula-based methods in pediatric patients below seven years. In addition, our study results demonstrated that the proposed model can reduce the risk of shallow or deep intubation and endobronchial intubation. Applying an ML model can be safe and helpful in determining the appropriate ET depth for pediatric patients.
There are some limitations to this study. First, there may be a difference between the time points of ET fixation and chest radiography. The ET position may not have been the initial depth because the tube position can change after fixation. According to the ICU processes of our institution, during the postoperative period, a chest X-ray examination was performed immediately after confirming tube fixation, and we could use the data that minimized the time difference. Second, it has not been applied to actual ET intubation in pediatric patients. Compared to previous studies, this study used a large amount of data and showed satisfactory performance; however, an actual clinical application process is required for generalization.
In future work, prospective studies may allow comparison of our ML approach to the alternative strategy for clinical assessment. Though the introduction of our proposed elastic net model showed reasonable accuracy, our study used only single center data to develop prediction model. Thus, external validation to verify ML performance is needed. We plan to update and test our model using data from other external institutions in further studies.
A “Key Points” summary is provided, which describes outcome and findings from this study.
-
a.
The elastic net model showed its ability to predict the optimal depth of endotracheal intubation with lower MSE, RMSE, and MAE, and with a higher R2 and VAF compared to other models in test data.
-
b.
The frequency rate of inappropriate locations in the elastic net model was 17.9% in test data. In the elastic net model, shallow, deep, and endobronchial intubation rates were 6.8%, 10.3%, and 0.9%, respectively.
-
c.
This will be helpful in decision-making regarding ET depth to clinicians unfamiliar with tracheal intubation in pediatric patients. However, an actual clinical application process is required for generalization.
Data availability
The datasets used and analyzed during the current study are available from the corresponding author on reasonable request.
References
Ganti, L., Shivdat, J. & Bawany, S. Back to basics: Endotracheal tube too deep, too shallow. Then Just Right. Cureus 10, e2706. https://doi.org/10.7759/cureus.2706 (2018).
Ibarra-Sarlat, M. et al. Endotracheal intubation in children: Practice recommendations, insights, and future directions. In Bedside Procedures (ed. Cismaru, G.) 51–52. https://doi.org/10.5772/intechopen.70356 (InTech, 2018).
Miller, K. A. & Nagler, J. Advances in emergent airway management in pediatrics. Emerg. Med. Clin. N. Am. 37, 473–491. https://doi.org/10.1016/j.emc.2019.03.006 (2019).
Yoon, K.-S., Lee, K.-M., Lim, H.-K. & Um, D.-J. Incidence and contributing factors of malpositioning of the endotracheal tube after endotracheal intubation with chest X-ray. Korean J. Anesthesiol. 33, 98–103 (1997).
Varshney, M., Sharma, K., Kumar, R. & Varshney, P. G. Appropriate depth of placement of oral endotracheal tube and its possible determinants in Indian adult patients. Indian J. Anaesth. 55, 488–493. https://doi.org/10.4103/0019-5049.89880 (2011).
Sharma, K., Varshney, M. & Kumar, R. Tracheal tube fixation: The effect on depth of insertion of midline fixation compared to the angle of the mouth. Anaesthesia 64, 383–386. https://doi.org/10.1111/j.1365-2044.2008.05796.x (2009).
Al-Qahtani, A. S., Messahel, F. M. & Ouda, W. O. Inadvertent endobronchial intubation: A sentinel event. Saudi J. Anaesth. 6, 259–262. https://doi.org/10.4103/1658-354x.101218 (2012).
Weiss, M., Gerber, A. C. & Dullenkopf, A. Appropriate placement of intubation depth marks in a new cuffed paediatric tracheal tube. Br. J. Anaesth. 94, 80–87. https://doi.org/10.1093/bja/aeh294 (2005).
Kumari, S., Prakash, S., Mullick, P., Guria, S. & Girdhar, K. K. Clinical implications of vocal cord-carina distance and tracheal length in the Indian population. Turk. J. Anaesthesiol. Reanim. 47, 456–463. https://doi.org/10.5152/tjar.2019.20856 (2019).
Reyes, G. et al. Use of an optical fiber scope to confirm endotracheal tube placement in pediatric patients. Crit. Care Med. 29, 175–177. https://doi.org/10.1097/00003246-200101000-00035 (2001).
Liu, P. R. et al. Application of artificial intelligence in medicine: An overview. Curr. Med. Sci. 41, 1105–1115. https://doi.org/10.1007/s11596-021-2474-3 (2021).
Ranjbarzadeh, R. et al. Brain tumor segmentation based on deep learning and an attention mechanism using MRI multi-modalities brain images. Sci. Rep. 11, 10930. https://doi.org/10.1038/s41598-021-90428-8 (2021).
Nguyen, D. T., Pham, T. D., Batchuluun, G., Yoon, H. S. & Park, K. R. Artificial intelligence-based thyroid nodule classification using information from spatial and frequency domains. J. Clin. Med. https://doi.org/10.3390/jcm8111976 (2019).
Poncette, A. S. et al. Improvements in patient monitoring in the intensive care unit: Survey study. J. Med. Internet Res. 22, e19091. https://doi.org/10.2196/19091 (2020).
Russo, G., Reche, P., Pennisi, M. & Pappalardo, F. The combination of artificial intelligence and systems biology for intelligent vaccine design. Expert Opin. Drug. Discov. 15, 1267–1281. https://doi.org/10.1080/17460441.2020.1791076 (2020).
Connor, C. W. Artificial intelligence and machine learning in anesthesiology. Anesthesiology 131, 1346–1359. https://doi.org/10.1097/aln.0000000000002694 (2019).
Jang, R. et al. Prediction of osteoporosis from simple hip radiography using deep learning algorithm. Sci. Rep. 11, 19997. https://doi.org/10.1038/s41598-021-99549-6 (2021).
Wang, Y. et al. Predicting postoperative delirium after microvascular decompression surgery with machine learning. J. Clin. Anesth. 66, 109896. https://doi.org/10.1016/j.jclinane.2020.109896 (2020).
Schneck, E. et al. Hypotension Prediction Index based protocolized haemodynamic management reduces the incidence and duration of intraoperative hypotension in primary total hip arthroplasty: A single centre feasibility randomised blinded prospective interventional trial. J. Clin. Monit. Comput. 34, 1149–1158. https://doi.org/10.1007/s10877-019-00433-6 (2020).
Wijnberge, M. et al. Effect of a machine learning-derived early warning system for intraoperative hypotension vs standard care on depth and duration of intraoperative hypotension during elective noncardiac surgery: The HYPE randomized clinical trial. JAMA 323, 1052–1060. https://doi.org/10.1001/jama.2020.0592 (2020).
Xiao, X., Zhao, S., Zhang, X., Soghier, L. & Hahn, J. In 2020 42nd Annual International Conference of the IEEE Engineering in Medicine & Biology Society (EMBC). 2429–2433 (IEEE).
Shim, J. G. et al. Machine learning model for predicting the optimal depth of tracheal tube insertion in pediatric patients: A retrospective cohort study. PLoS ONE 16, e0257069. https://doi.org/10.1371/journal.pone.0257069 (2021).
Koshy, T., Misra, S., Chatterjee, N. & Dharan, B. S. Accuracy of a chest X-Ray-based method for predicting the depth of insertion of endotracheal tubes in pediatric patients undergoing cardiac surgery. J. Cardiothorac. Vasc. Anesth. 30, 947–953. https://doi.org/10.1053/j.jvca.2016.01.031 (2016).
Freeman, J. A., Fredricks, B. J. & Best, C. J. Evaluation of a new method for determining tracheal tube length in children. Anaesthesia 50, 1050–1052. https://doi.org/10.1111/j.1365-2044.1995.tb05949.x (1995).
Ge, X. et al. The lengths of trachea and main bronchus in Chinese Shanghai population. Sci. Rep. 11, 2168. https://doi.org/10.1038/s41598-021-81744-0 (2021).
Lau, N., Playfor, S. D., Rashid, A. & Dhanarass, M. New formulae for predicting tracheal tube length. Paediatr. Anaesth. 16, 1238–1243. https://doi.org/10.1111/j.1460-9592.2006.01982.x (2006).
Leach, J. M. et al. The spike-and-slab elastic net as a classification tool in Alzheimer’s disease. PLoS ONE 17, e0262367 (2022).
Zou, H. & Hastie, T. Regularization and variable selection via the elastic net. J. R. Stat. Soc. Ser. B (Stat. Methodol.) 67, 301–320 (2005).
Bruce, P., Bruce, A. & Gedeck, P. Practical statistics for data scientists: 50+ essential concepts using R and Python. (O'Reilly Media, 2020).
Engebretsen, S. & Bohlin, J. Statistical predictions with glmnet. Clin. Epigenetics 11, 123. https://doi.org/10.1186/s13148-019-0730-1 (2019).
Coté, C. J., Lerman, J. & Todres, I. D. A Practice of Anesthesia for Infants and Children E-book (Elsevier, 2018).
Helfaer, M. A. Advanced paediatric life support, the practical approach. Anesth. Analg. 93, 520–521 (2001).
Lubitz, D. S. et al. A rapid method for estimating weight and resuscitation drug dosages from length in the pediatric age group. Ann. Emerg. Med. 17, 576–581. https://doi.org/10.1016/s0196-0644(88)80396-2 (1988).
Morgan, G. A. & Steward, D. J. Linear airway dimensions in children: Including those from cleft palate. Can. Anaesth. Soc. J. 29, 1–8. https://doi.org/10.1007/bf03007939 (1982).
Phipps, L. M. et al. Prospective assessment of guidelines for determining appropriate depth of endotracheal tube placement in children. Pediatr. Crit. Care Med. 6, 519–522. https://doi.org/10.1097/01.pcc.0000165802.32383.9e (2005).
Kamran, M. A state of the art catboost-based T-distributed stochastic neighbor embedding technique to predict back-break at dewan cement limestone quarry. J. Min. Environ. 12, 679–691 (2021).
Shahani, N. M., Kamran, M., Zheng, X. & Liu, C. Predictive modeling of drilling rate index using machine learning approaches: LSTM, simple RNN, and RFA. Pet. Sci. Technol. 40, 534–555 (2022).
Kamran, M. A probabilistic approach for prediction of drilling rate index using ensemble learning technique. J. Min. Environ. 12, 327–337 (2021).
Shahani, N. M., Kamran, M., Zheng, X., Liu, C. & Guo, X. Application of gradient boosting machine learning algorithms to predict uniaxial compressive strength of soft sedimentary rocks at Thar Coalfield. Adv. Civ. Eng. 2021, 1–19 (2021).
Santos, D. L. S., Andrade, P. D. O. & Gomes, E. Does the endotracheal tube insertion depth predicted by formulas in children have a good concordance with the ideal position observed by X-ray?. Rev. Bras. Ter Intensiva 32, 295–300. https://doi.org/10.5935/0103-507x.20200046 (2020).
Gill, I. et al. Randomised trial of estimating oral endotracheal tube insertion depth in newborns using weight or vocal cord guide. Arch. Dis. Child Fetal. Neonatal. Ed 103, F312-f316. https://doi.org/10.1136/archdischild-2017-312798 (2018).
Matava, C., Pankiv, E., Raisbeck, S., Caldeira, M. & Alam, F. A convolutional neural network for real time classification, identification, and labelling of vocal cord and tracheal using laryngoscopy and bronchoscopy video. J. Med. Syst. 44, 44. https://doi.org/10.1007/s10916-019-1481-4 (2020).
Matava, C., Pankiv, E., Ahumada, L., Weingarten, B. & Simpao, A. Artificial intelligence, machine learning and the pediatric airway. Paediatr Anaesth. 30, 264–268. https://doi.org/10.1111/pan.13792 (2020).
Author information
Authors and Affiliations
Contributions
J.-G.S. and E.-K.L. helped with study design, planning, conduct, data analysis, and drafting of the paper. J.H.A. and E.J.O. helped with data analysis and drafting of the paper. E.-A.C. helped with study design and planning, data analysis and drafting and revision of the paper. J.-H.L. helped with formal analysis. J.P. helped with investigation and methodology.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Shim, JG., Lee, E.K., Oh, E.J. et al. Predicting the risk of inappropriate depth of endotracheal intubation in pediatric patients using machine learning approaches. Sci Rep 13, 5156 (2023). https://doi.org/10.1038/s41598-023-32122-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-023-32122-5
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.