Abstract
Platelet transfusions may lead to more significant risks of infection and septic transfusion reactions that can be fatal to the recipient. Platelet products should be screened to limit or detect bacterial contamination before application to patients to minimise any adverse reactions. This study aimed to develop a helicase-dependent amplification (HDA) technique targeting a universal highly conserved bacterial gene, 16S rRNA, in combination with naked-eye detection using SYBR Green I (HDA/SYBR Green I) to detect bacterial contamination in platelet products. Thirty positive samples were obtained from spiked platelet products by five transfusion-relevant bacterial strains and were screened for bacterial contamination by HDA/SYBR Green I. HDA/SYBR Green I showed an enhanced yield of bacterial contaminant detection when performed with medium to late shelf life, Day 2 of storage or later platelet products (98.67% sensitivity and 100% specificity compared to the BACT/ALERT culture system). The limit of detection of HDA/SYBR Green I was 1 ng, and there was no cross-reaction with other organisms that could likely contaminate platelet products. The developed HDA/SYBR Green I assay is rapid and simplistic and only requires an easy-to-find heat box, available in general blood bank laboratories, for the amplification step. This technique is suitable for further development as an alternative method to detect bacterial contamination in platelet products in the near future.
Similar content being viewed by others
Introduction
Bacterial contamination of blood components is a longstanding concern1. Receiving bacterial contaminated blood components may lead to transfusion-transmitted fatalities due to bacterial infections. The U.S. Food and Drug Administration (FDA) report from 2012 to 2016 showed that transfusion-transmitted bacterial infections were the third cause of death from transfusions after transfusion-related acute lung injury (TRALI) and transfusion-associated circulatory overload (TACO)2. Even the blood collection process is being improved and is well-controlled to reduce the bacterial contamination of blood components3. However, platelet products present a significant risk due to their storage conditions (20–24 °C with agitation), which may support bacteria to multiply and reach clinically harmful levels during their 5-day storage period1.
Regarding the American Association of Blood Banks (AABB) standard 5.1.5.1, platelet products should be screened to limit or detect bacterial contamination before application to patients to minimise any adverse reactions4. Bacterial culture is the gold standard for detecting bacterial contamination from various blood components. However, the traditional culture exhibits some limitations, including an inappropriate practice for bacterial culture in the blood bank working area, time consumption that does not match the short 5-day shelf life of platelets, and high cost-effectiveness of the assay. The BacT/ALERT® culture system is an automated culture-based method for platelet quality control approved by the FDA. Several molecular-based methods have revolutionised the detection of bacterial contamination in platelet products, such as PCR and real-time PCR. However, these techniques are not widely used in routine testing due to a complicated process, high cost-effectiveness, and specific instrument dependence that requires ongoing maintenance1,5.
The isothermal amplification method is an amplification technique that operates under a constant temperature. The most significant advantage of isothermal amplification is that it does not require a thermocycling machine. Therefore, isothermal amplification requires low energy consumption and can be easily integrated into a simple detection platform, such as in the field or instrumentation-free settings. Helicase-dependent amplification (HDA) is one of the most straightforward approaches for isothermal nucleic acid amplification, mimicking an in vivo process of DNA replication, using a helicase instead of heat to isothermally unwind DNA duplexes. The process occurs under an optimum temperature range from 60 to 65 °C and takes 30–120 min. HDA has been previously developed as a novel molecular-based tool for rapid pathogen detection6,7. The aim of this study was to fabricate a simple, rapid, and sensitive screening method for bacterial contaminants in platelet products that can be easily implemented in blood bank service routines. To achieve this objective, HDA amplification targeting 16S rRNA was used with endpoint detection using SYBR Green I (referred to as HDA/SYBR Green I).
Materials and methods
Representative bacterial strains
Five strains of bacteria, including Staphylococcus aureus (ATCC 29,523), Staphylococcus epidermidis, Bacillus cereus, Escherichia coli (ATCC 25,922), and Serratia marcescens, were used as representative strains. All of these strains have been previously reported as common transfusion-relevant bacterial strains of platelet products1,8,9. The ATCC bacterial strains were kindly provided by Assoc. Prof. Dr. Pitak Santanirand, the Microbiology Unit, Faculty of Medicine Ramathibodi Hospital, Mahidol University, Bangkok, Thailand. S. epidermidis, B. cereus, and S. marcescens were clinical isolates obtained from leftover specimens from the Microbiology Unit, Faculty of Medicine Ramathibodi Hospital, Mahidol University, Bangkok, Thailand, and were confirmed at the species level by conventional biochemical tests and PCR sequencing. The bacteria were subcultured on tryptic soy agar (TSA) at 37 °C for 24 h before use. Bacterial genomic DNA was extracted by the boiling method. A single 24 h colony of each strain was resuspended in 1 ml of sterile distilled water and boiled at 95 °C for 10 min, followed by a 5-min centrifugation at 12,000 rpm. The supernatant was used as a DNA template for HDA/SYBR Green I optimisation.
Primer design and screening
An HDA/SYBR Green I assay was developed targeting the highly conserved bacterial 16S rRNA gene, the most widely used marker gene employed to identify bacteria and differentiate between closely related bacterial species. HDA primers were designed from the conserved fragments of 16S rDNA sequences predicted to cover 275,057 eubacterial species derived from the Ribosomal Database Project of a previous study10 using the Primer3 program (version 0.4.0; http://bioinfo.ut.ee/primer3-0.4.0/). This selected 16S rRNA gene fragment is dominant among Firmicutes, Gemmatimonadetes and Proteobacteria, which are the predominant phyla in all microbiomes10. These HDA primer candidates contained 20–32 bases, as recommended by the IsoAmp®II Universal tHDA kit (New England BioLabs, USA). The primer melting temperature ranged from 60 to 74 °C, and the GC% was within the interval of 35–60% 6. The OligoAnalyser 3.1 program (https://eu.idtdna.com/calc/analyser) and BLAST software (https://blast.ncbi.nlm.nih.gov/Blast.cgi) were used to assess the possibility of secondary structure formation and the specificity of the primers, respectively. Four forward and reverse primers were designed in this study. Each forward and reverse primer candidate was paired and preliminarily screened for its ability to amplify specific targets with an IsoAmp®II Universal tHDA kit as recommended by the manufacturer. The most suitable primer pair was selected and finally used in our fabricated HDA/SYBR assay as follows: 16S rRNA forward (5’AGTCCCRYAACGAGCGCAACCC 3’) and 16S rRNA reverse (5’TTGACGTCRTCCCCRCCTTCC 3’), generating an HDA product size of 104 bp.
HDA/SYBR green I optimisation
The optimised HDA/SYBR Green I assay was evaluated using genomic DNA of S. aureus (ATCC 29,523), S. epidermidis, B. cereus, E. coli (ATCC 25,922), and S. marcescens as positive controls to obtain the most appropriate conditions for HDA amplification and endpoint SYBR Green I detection. During HDA/SYBR Green I assay development, the amount of DNA template (1–20 ng), primer concentration (50–200 nM), MgSO4 concentration (3–4.5 mM), NaCl concentration (20–50 mM), incubation temperature (63–69 °C in the heating block) and incubation period (15–90 min) were optimised until the most appropriate conditions were obtained. Sterile distilled water served as a negative control. Amplified 16S rRNA was directly detected by the naked-eye in natural light by adding 1 µL of 100–500 × SYBR to a final volume of 50 µL of HDA products and immediately observing a colour change of the solution. The solution changed from light orange to bright green in the presence of the HDA product, indicating that bacterial DNA was detected. Conversely, the solution remained light orange in the absence of the HDA product, suggesting that no bacterial DNA was detected.
In every optimisation step, the HDA products were examined by SYBR Green I and compared with agarose gel electrophoresis. The condition giving clear readout results when observed with SYBR Green I, without nonspecific bands upon agarose gel electrophoresis, was chosen (data not shown).
Spiked platelet product samples for the performance test
Spiked platelet samples were established to mimic natural bacterial-contaminated platelet products. This study used sterile leukocyte-poor platelet concentrates (LPPC) supplemented with a platelet additive solution (PAS). All the platelet concentrates were due to the expiration of the shelf life (after Day 5 of storage) and were collected from the Regional Blood Centre IV, Thai Red Cross Society. The discarded platelet products were checked for purity by plating out onto blood agar and observed for any growth colony until 7 days of aerobic and anaerobic incubations. The study was approved by the Research Ethics Committee, National Blood Centre, Thai Red Cross Society, Bangkok, Thailand (COA.NBC 15/2019).
Five strains of bacteria, including S. aureus (ATCC 29,523), S. epidermidis, B. cereus, E. coli (ATCC 25,922), and S. marcescens, were grown overnight in tryptic soy broth (TSB) and adjusted to 0.5 McFarland standard (108CFU/ml). Serial tenfold dilutions were prepared in TSB to achieve a concentration of 102 CFU/ml. Then, 3 ml of each bacterial strain was injected into a separate bag containing 297 ml of sterile platelet products, achieving a final bacteria concentration of 1 CFU/ml (One strain per bag). The freshly prepared spiked sample was named Day 0 (representing the collection day). The platelet samples were maintained under standard platelet storage conditions at 20–24 °C under agitation until 5 days and named Day 1 to Day 5, respectively. During storage, platelet products were sampled daily from every bag (Day 0–5) inoculated with each bacterial strain. In total, 30 contaminated samples were obtained and set as the positive samples. Twelve sterile samples were set as the negative samples. Bacterial DNA was extracted from 1 ml of daily aliquoted platelet products using the QIAamp DNA Microbiome Kit (Qiagen, Germany) as recommended by the manufacturer. The DNA was stored at −20 °C until use. All experiments were performed in 5 separate replicates. Another 1 ml of platelet product was aliquoted daily, and tenfold dilutions were prepared in TSB and plated on TSA. Colony counting was performed after 24 h of incubation to determine the bacterial concentration of each strain in the platelet product on each storage day. The experiments were performed in triplicate.
BacT/ALERT® culture system protocol
A 10 ml aliquoted sample was taken from Day 0 to Day 5 platelet products and inoculated into BacT/ALERT® BPA culture bottles (BioMérieux, France). The samples were incubated with the automated BACT/ALERT system for 7 days, and CO2 production indicating bacterial growth was automatically measured via a fluorescent signal. All positive bottles were subcultured, and bacterial colonies were reidentified for confirmation by the matrix-assisted laser desorption/ionization (MALDI-TOF) Microflex series (Bruker Diagnostics, Germany).
HDA/SYBR green I assay protocol
DNA samples derived from Day 0 to Day 5 of platelet products containing 5 individual bacterial strains were used in the HDA/SYBR Green I assay protocol as positive contaminated samples. In contrast, sterile distilled water and sterile platelet product were used as negative samples. The HDA reaction was performed with the IsoAmp®II Universal tHDA kit (New England BioLabs, USA) as recommended by the manufacturer. Each HDA reaction consisted of 5 µM 16S rRNA gene forward and reverse primers, 5 µl 10X annealing buffer II, 2 µl MgSO4, 4 µl NaCl, 3.5 µl IsoAmp dNTPs solution, 3.5 µl IsoAmp enzyme mix, 10 ng of DNA and sterile distilled water up to 50 µl. The HDA reaction mixture was incubated at 65 °C for 60 min in the heating block. After amplification, each reaction was aliquot into two separate tubes for evaluation by different detection methods. The first tube was evaluated by SYBR Green I (HDA/SYBR Green I assay), in which 1 µl of 400 × SYBR Green I (Takara Bio, Japan) was directly added to the 25 µl HDA products. A colour change of the solution in natural light was immediately observed by the naked-eye. The second tube was evaluated by 2% agarose gel electrophoresis. Without prior purification, 2 µl of HDA product was directly mixed with 1 µl of a loading dye before loading into 2% agarose gel electrophoresis. Randomly selected HDA products were confirmed by Sanger DNA sequencing. The sequence reads were compared to gene sequences described in the NCBI database (Blast search http://blast.ncbi.nlm.nih.gov/Blast.cgi). All experiments were performed in 5 replicates. HDA/SYBR Green I was blindly interpreted by two different investigators to eliminate bias. The principles underlying HDA/SYBR Green I assay for the detection of bacterial contamination platelet products are illustrated in Fig. 1.
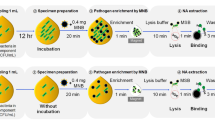
The diagram presentation of the process and reaction principle of HDA/SYBR Green I. (a) DNA extraction. One millilitre of daily aliquoted platelet products was extracted using the QIAamp DNA Microbiome Kit. (b) HDA reaction. Ten nanograms of DNA were used as a template in the HDA reaction under 65 °C for 60 min. (c) SYBR Green I detection. One microlitre of 400 × SYBR Green I was added to HDA products. A colour change was observed by the naked-eye.
Analytical limit of detection
An analytical limit of detection was established to determine the lowest concentration of DNA enabling detection by the HDA/SYBR Green I assay. Genomic colony DNA of S. aureus (ATCC 29,523), S. epidermidis, B. cereus, E. coli (ATCC 25,922), and S. marcescens was tenfold serially diluted from 10 to 0.000001 ng. Each DNA template was amplified by HDA using sterile distilled water and sterile platelet product as negative controls. The HDA products were analysed by SYBR Green I and 2% agarose gel electrophoresis. The experiments were performed in triplicate.
Cross-reaction testing
The specificity of HDA/SYBR Green I was evaluated with DNA extracted from microbial pathogens other than bacteria. These pathogens included the common fungi Candida albicans, Cryptococcus neoformans, Aspergillus spp., Rhizopus spp. (kindly provided with no patient data links by the Microbiology Unit, Faculty of Medicine Ramathibodi Hospital, Mahidol University, Bangkok, Thailand), and bloodborne hepatitis B virus (kindly provided with no patient data links by Prof. Yong Poovorawan, the Centre of Excellence in Clinical Virology, Faculty of Medicine, Chulalongkorn University, Bangkok, Thailand. Human genomic DNA was extracted from a sterile discarded platelet product and included in cross-reaction testing. A total of 10 ng of individual DNA templates was used for HDA amplification. The HDA product was evaluated by SYBR Green I and 2% agarose gel electrophoresis. Sterile distilled water and E. coli colony DNA were used as negative and positive controls, respectively. The experiments were performed in triplicate.
Test performance analyses
The sensitivity and specificity of HDA/SYBR Green I were evaluated with the FDA-recommended BACT/ALERT system. Sensitivity (a true positive rate) was computed from sensitivity (%) = TP/(TP + FN) × 100, where ‘TP’ is the number of positive samples, and ‘FN’ is the number of false negatives when spiked samples were used. Specificity (a true negative rate) was computed from specificity (%) = TN/(TN + FP) × 100, where ‘TN’ is the number of negative samples and ‘FP’ is the number of false-positives when nonspiked samples (sterile distilled water and sterile platelet product) were used. To further evaluate the reliability of HDA/SYBR in detecting bacterial contamination in platelet products, the percent agreement between the two methods (HDA/SYBR Green I and BacT/Alert® system) was calculated. The Kappa result was interpreted as follows: values ≤ 0 indicated no agreement, 0.01–0.20 indicated slight agreement, 0.21–0.40 indicated fair agreement, 0.41–0.60 indicated moderate agreement, 0.61–0.80 indicated substantial agreement, and 0.81–1.00 indicated almost perfect agreement.
Results
Establishment of spiked platelet product samples
The average bacterial concentration in the platelet products from Day 0 to Day 5 of storage is shown in Table 1. A visible colony of every bacterial strain, except S. epidermidis, was initially observed in platelet products collected from Day 1 of storage, with concentrations ranging from 8.8 × 102 to 1.9 × 103 CFU/ml. In contrast, the colony of S. epidermidis was slower on Day 2 of storage, with a concentration of 2.2 × 103 CFU/ml. The number of bacterial cells in platelet products increased during a more extended storage period in a time-dependent manner. The maximum bacterial concentration was 1.2 × 1010 CFU/ml, which was found on Day 5 of storage when inoculated with S. marcescens.
BacT/ALERT® culture system detected bacterial contamination in platelet products
The BacT/ALERT® culture system could detect bacterial contamination in all storage periods of spiked platelet products, starting from the collection day (Day 0). The average processing time of the BacT/ALERT® system from sample incubation until a positive signal was detected ranged from 10 h and 54 min to 18 h and 15 min (Supplement Table 1).
Detection of bacterial contamination by HDA/SYBR green I
After complete optimisation of HDA/SYBR Green I, the appropriate assay conditions were achieved. When evaluated with genomic DNA derived from a colony of 5 representative bacterial strains, SYBR Green I stayed orange in a negative control tube due to the lack of amplification of the HDA product. In contrast, SYBR Green I switched to shining green in the positive control tubes, implying that DNA products were amplified by HDA with 16S rRNA gene-specific primers (Fig. 2). HDA/SYBR Green I concordantly exhibited positive and negative results for agarose gel electrophoresis. The presence of a bottom primer-dimer band on an agarose gel in Fig. 2 (Lanes 1, 2, 7 and 8) did not cause a false-positive or background on SYBR Green I detection or interfere with the assay. When testing with Day 0 to Day 5 of stored (contaminated samples) and sterile platelet products (sterile samples) in 5 replicates, HDA/SYBR Green I could correctly detect positive and negative samples, as described in Table 1. Platelets inoculated with B. cereus, E. coli, and S. marcescens were first detected on Day 1 of storage (average bacterial concentration was 1.9 × 103, 1.8 × 103, and 8.8 × 102 CFU/ml, respectively), whereas almost of the rest of the contaminants started to be detected on Day 2 of storage (bacterial concentration ranged from 7.4 × 104 to 2.0 × 108 CFU/ml). The average test time of HDA/SYBR Green I, from the reaction began until the sample readout, was 1 h and 40 min.
HDA/SYBR Green I detected bacterial contaminants in platelet products. Samples 1 to 6 are DNA samples from Day 0 to Day 5, respectively, of platelet products containing spiked E. coli. Samples 7 and 8 are negative controls (sterile distilled water and sterile platelet product, respectively). Sample 9 is a positive control (E. coli colony DNA). (a) HDA products were naked eye detected by SYBR green I directly in the reaction tubes. Tubes 1, 2, 7, and 8 show an orange colour, which implies a negative amplification result. Tubes 3, 4, 5, 6, and 9 show a green colour, which indicates a positive amplification result. Documented by Canon EOS 760D: ISO 800, aperture f/3.5, and speed shutter 1/125. (b) Cropped gel image demonstrates HDA products that were detected by 2% agarose gel electrophoresis (documented by Gel Doc™ XR ChemiDocTMXRS). Lane L: 100-bp DNA ladder. Reactions in lanes 1, 2, 7, and 8 show no visible target band. Reactions in lanes 3, 4, 5, 6, and 9 show an amplification product size of 104 bp. Original images are presented in Supplementary Fig. 2.
Performance of contaminated bacterial detection by HDA/SYBR Green I
The performance of HDA/SYBR Green I to detect bacterial contamination in platelet products was validated with the BacT/ALERT® culture system. HDA/SYBR Green I could not detect bacterial contamination in freshly prepared Day 0 of storage samples and exhibited a very low sensitivity when tested with Day 1 of storage samples. The sensitivity and specificity of HDA/SYBR Green I when tested with Day 1 of storage samples was 4.00% and 100%, respectively, with slight agreement with a standard method. However, when tested with samples from Day 2 of storage or later, HDA/SYBR Green I showed markedly increased sensitivity of 98.67–100% and specificity of 100% with almost perfect agreement (Table 2).
LOD and cross-reactivity of HDA/SYBR green I
The LOD of the HDA/SYBR Green I assay was 1 ng. When the HDA product was detected by agarose gel electrophoresis, the LOD was as low as 0.1 ng. HDA/SYBR Green I did not cross-react with C. albicans, C. neoformans, Aspergillus spp., Rhizopus spp., hepatitis B virus, or human genomic DNA. Figures 3 and 4 show the LOD and cross-reactivity testing of HDA/SYBR Green I, respectively.
LOD of HDA/SYBR Green I. S. marcescens colony DNA was tenfold serially diluted from 10 to 0.000001 ng (samples 1 to 8, respectively). Samples 9 and 10 are negative controls (sterile distilled water and sterile platelet product, respectively). (a) HDA products were detected by SYBR Green I. Tubes 1 and 2 show a green colour, which indicates a positive amplification result. Tubes 3 to 10 shows an orange colour, which implies a negative amplification result. Documented by Canon EOS 760D: ISO 800, aperture f/4.5, and speed shutter 1/125. (b) Cropped gel image demonstrates HDA products that were detected by 2% agarose gel electrophoresis (documented by Gel Doc™ XR ChemiDocTMXRS). Lane L: 100-bp DNA ladder. Reactions in lanes 1, 2, and 3 show an amplification product size of 104 bp. Reactions in lanes 4 to 10 show no visible target band. Original images are presented in Supplementary Fig. 3.
Cross-reactivity testing of HDA/SYBR Green I. (a) Tubes 1 to 6 are DNA from C. albicans, C. neoformans, Aspergillus spp., Rhizopus spp., hepatitis B virus and human genomic DNA, respectively. Tube 7 is a negative control, showing an orange colour, which indicates no amplification. Tube 8 is a positive control (E. coli colony DNA), showing a green colour, which indicates a positive amplification result. Documented by Canon EOS 760D: ISO 1600, aperture f/4.5, and speed shutter 1/20. (b) Cropped gel image demonstrates HDA products that were detected by 2% agarose gel electrophoresis (documented by Gel Doc™ XR ChemiDocTMXRS). Lane L: 100-bp DNA ladder. No visible target band is seen in lanes 1–7, indicating a negative amplification result. An amplification product size of 104 bp was seen in lane 8, indicating a positive amplification result. Original images are presented in Supplementary Fig. 4.
Discussion
A transfusion with bacterial contaminated platelets can lead to transfusion-transmitted diseases such as transfusion-transmitted bacterial infection (TTBI) and septic transfusion reactions (STRs), which are significant sources of morbidity and mortality. Between 1 in 1000 to 2000 platelet units are bacterially contaminated. Thus, a strategy to relieve the risk of bacterial contamination in platelet products is challenging. Different strategies have been proposed, including preventing bacterial contamination during platelet collection, pathogen reduction/inactivation technologies and testing methods for platelet bacterial contamination11. In 2004, AABB standard 5.1.5.1 instructed that the blood bank or transfusion service should have methods to limit and detect bacterial contamination in platelet products before applying to the patients to minimise any adverse reactions4.
The BacT/ALERT® culture system is the primary automated culture-based method commonly used worldwide and in major transfusion service centres in Thailand. The assay has been approved by the FDA and is regarded as the gold standard for bacterial contaminant screening in platelet products after collection. In our experimental setting, the BacT/ALERT® culture system effectively detected bacterial contamination in collection day (Day 0) and early storage (Day 1) platelet samples inoculated with bacterial strains (e.g., S. aureus, S. epidermidis, B. cereus, E. coli, and S. marcescens) with an incubation time of 10–18 h. A previous study showed that the level of detection of the BacT/ALERT® culture system against those relative bacteria was as low as 1–10 CFU/ml5. The BacT/ALERT® system has been shown to reduce the incidence of TTBI in screening programs for bacterial contamination of platelet products12. However, this current automatic culture system may not effectively detect biofilm-producing organisms13. Moreover, due to high cost-effectiveness, implementing the BacT/ALERT® system may be limited in many transfusion service routines in Thailand. Currently, molecular biology techniques, such as real-time PCR, are being developed to detect bacterial contamination in platelet products targeting highly conserved 16S rRNA and 23S rRNA genes8,14. The analytical sensitivities ranged from 5 to 50 CFU/ml.
However, the ideal screening test should have a high diagnostic sensitivity and specificity and be affordable, reliable, and rapid. Real-time PCR relies on a specific thermocycler, which is not yet widely used in transfusion service routines to detect bacterial platelet contamination. Isothermal-based amplification is a molecular method that depends on a constant temperature during the entire amplification process. Over 15 types of isothermal amplification techniques have been described. However, some techniques have yet to be developed beyond proof of concept or academic research. The most representative and applied isothermal amplification methods, such as loop-mediated amplification (LAMP), recombinase polymerase amplification (RPA), helicase-dependent amplification (HDA), rolling circle amplification (RCA), strand displacement amplification (SDA), nucleic acid sequence-based amplification (NASBA). LAMP has been the most widely used isothermal amplification method, which relies on a Bst DNA polymerase and a set of 4–6 primers for amplification. LAMP is extremely sensitive and has high specificity with an amplification time of less than 1 h at 60–65 °C. Even LAMP is simple to operate, but a higher risk of contamination and complexity in primer design is a disadvantage15. In our pilot study, we focused on an isothermal amplification technique that is simple either in a primer design or an operation step. RPA was attempted in the first period of our development. RPA offers many advantages over other isothermal amplification techniques, such as a simple primer design, a high speed and sensitivity, a broad temperature range (25–45 °C), and multiplexing availability. However, TwistAmp® RPA kits contain a small amount of E. coli DNA due to the manufacturing method16, leading to a false positive in our pilot study (data not shown). According to the manufacturer's instruction manual, RPA reactions are unsuitable for developing diagnostics for E. coli if sequence homology with strains K12 and BL21 is present16. E. coli is one of the most contaminants in platelet products; thus, RPA was considered unsuitable for our developed assay in this study. HDA is one of the most straightforward isothermal amplification schemes7 requiring only 2 primers per target and a double-strand DNA as a template15. HDA is compatible with different detection platforms, including fluorescent DNA intercalator and lateral flow device, which is very practicable to use in general laboratories. Our developed HDA/SYBR Green I assay has an affordable price (~ 7 USD per reaction). However, the assay has a slightly higher cost than LAMP (~ 2 USD per reaction) and RPA (~ 5 USD per reaction). HDA has been successfully developed as a novel molecular-based method for the rapid and sensitive detection of bacteria (e.g., E. coli, S. aureus, Chlamydia trachomatis and Neisseria gonorrhoeae) and viruses (e.g., human papillomavirus 16 and 18)6. The optimum HDA temperature ranges from 60 to 65 °C; thus, the entire reaction can be constantly operated by a simple heating block that is generally used in blood bank laboratories.
Here, HDA was chosen to amplify bacterial target DNA, the 16S rRNA gene, to establish “advanced instrument-free” amplification that depends on a simple heat generating box available in general transfusion service centres. The 16S rRNA gene has been a mainstay of molecular-based bacterial investigation for decades and can be implemented in aerobic, anaerobic, facultative, and fastidious bacteria. The copy numbers of 16S rRNA are diverse among bacterial phyla. They were high in Firmicutes, Gammaproteobacteria and Fusobacteria, with averages greater than five copies per genome. In contrast, most bacterial phyla contain at least a single 16S rRNA copy17. Target selection and primer design are critical in assay development. Therefore, the target sequence and initial primer selection were first verified in silico before the candidate set of primers was experimentally screened with reference strains. However, our 16S rRNA primers were designed in silico to cover 275,057 eubacterial species, including the commonly contaminating bacteria, and the detection of some species may eventually fail10.
The HDA/SYBR Green I assay provided high sensitivity and specificity and was rapid for detecting bacterial contamination in platelet products by the naked-eye. The developed assay was conducted under a constant temperature of 65 °C, and the test time was approximately 1 h and 40 min from sampling to readout. In our study, the early sampling with a small sample volume (1 ml) might have caused false negative results of the HDA/SYBR Green I assay compared with the BacT/ALERT® system, which was processed with a larger sample volume (10 ml). In a previous study, a high-volume extraction (2.4 ml of sample volume) of total DNA by magnetic bead technology was shown to enhance the sensitivity of the 23S rRNA real-time reverse transcription PCR assay for detecting bacterial contamination of platelet products14. HDA/SYBR Green I showed poor sensitivity in detecting bacterial contamination in samples collected from early shelf life, Day 0 and Day 1. However, the assay showed an enhanced yield of detection when performed with medium to late shelf life, Day 2 of storage or later platelet products, with a sensitivity ranging from 98.67 to 100%. The sample collection at an early stage of platelet shelf life can cause a sampling error, owing to a low bacterial contamination number at the start time of storage, mainly when slow-growing bacteria are implicated in the contamination. Previously, the risk of sampling errors continuously decreased during storage; the detection rate of bacterial contamination changed from 14.9% for sampling on Day 1–100% for sampling on Day 718. The bacterial load in platelet products has been suggested to be associated with storage times. One approach to improving the sensitivity of contaminated platelet screening could be to collect samples later in platelet storage (e.g., Day 3–5 of storage)9. Another factor that might interfere with the efficacy of the HDA assay during the amplification process is the presence of human genomic DNA in clinical samples, presumably through binding HDA enzymes. Doseeva et al. showed that more than 200 ng of human genomic DNA per HDA assay significantly interfered with the specific amplification19. Removal of background human genomic DNA originating from platelet cells may increase either sensitivity or specificity of the HDA assay.
Our study has proven a concept to combine isothermal-based amplification, HDA, with naked-eye detection using SYBR Green I to detect bacterial contamination in platelet products. HDA/SYBR Green I is less laborious and expensive (equipment, reagents) than real-time PCR and the BacT/ALERT® system. The total test time of HDA/SYBR Green I is faster than that of culture-based assays, and can be implemented for routine contaminant bacterial screening in platelet products before providing them to a patient. The ideal test to detect bacterial contamination in platelet products should be highly sensitive (1 CFU/ml), specific, rapid (less than 2 h), inexpensive, reliable, and simple20. HDA/SYBR Green I first detected bacteria on Day 1 of storage (1.9 × 103 CFU/ml) as the earliest detection, whereas almost of the rest of the contaminants started to be detected on Day 2 of storage (7.4 × 104 to 2.0 × 108 CFU/ml). The analytical sensitivity of HDA/SYBR Green I was similar to that obtained from real-time PCR for S. epidermidis (2.9 × 104 CFU/ml) and E. coli (2.2 × 104 CFU/ml) in a previous study14. Earlier published surveillance data show that platelet units with bacterial concentrations of < 105 CFU/ml are much less likely to cause severe STRs than units with higher bacterial concentrations21. HDA/SYBR Green I potentially detected bacterial concentrations in platelet products at the minimum clinical significance cut-off of < 105 CFU/ml. Nevertheless, the sensitivity of our HDA/SYBR Green I assay requires further improvement.
Conclusion
In conclusion, the HDA/SYBR Green I assay in combination with late sampling can enhance the possibility of detecting bacteria in platelet products and can be easily adopted in a blood bank service for the routine screening of bacterial contaminants. Our developed HDA/SYBR Green I assay is rapid and simplistic and only requires an easy-to-find heat box, which is available in general blood bank laboratories, for the amplification step. This technique is suitable for further development as an alternative method to detect bacterial contamination in platelet products in the future.
Data availability
The datasets analysed during the current study are available in the DNA Data Bank of Japan (DDBJ) repository, LC730901, LC730902, LC730903, LC730904, and LC746965 for analysed sequences of 16S rRNA of S. aureus, S. epidermidis, B. cereus, E. coli and S. marcescens, respectively, generated in the study.
References
Jerrold, H. L., Matthew, D. N. & Jay, H. H. Bacterial contamination of platelets for transfusion: Strategies for prevention. Crit. Care 22, 271. https://doi.org/10.1186/s13054-018-2212-9 (2018).
Fatalities reported to FDA Following blood collection and transfusion annual summary for FY2016 (Food and Drug Administration, 2016).
Ibáñez-Cervantes, G., Bello-López, J. M., Fernández-Sánchez, V., Domínguez-Mendoza, C. A. & Acevedo-Alfaro, L. I. Prevalence of bacterial contamination in platelet concentrates at the National Center of Blood Transfusion (Mexico). Transfus. Clin. Biol. 24, 56–61. https://doi.org/10.1016/j.tracli.2017.03.003 (2017).
Further guidance on methods to detect bacterial contamination of platelet components: AABB Association Bulletin No. 03–12. (American Association of Blood Banks, 2003).
Störmer, M. & Vollmer, T. Diagnostic methods for platelet bacteria screening: Current status and developments. Transfus. Med. Hemother. 41, 19–27. https://doi.org/10.1159/000357651 (2014).
Barreda-García, S., Miranda-Castro, R., de-Los-Santos-Álvarez, N., Miranda-Ordieres, A. J. & Lobo-Castañón, M. J. Helicase-dependent isothermal amplification: A novel tool in the development of molecular-based analytical systems for rapid pathogen detection. Anal. Bioanal. Chem. 410, 679–693. https://doi.org/10.1007/s00216-017-0620-3 (2018).
Zhao, Y., Chen, F., Li, Q., Wang, L. & Fan, C. Isothermal amplification of nucleic acids. Chem. Rev. 115, 12491–12545. https://doi.org/10.1021/acs.chemrev.5b00428 (2015).
Viana, J. D. et al. Detection of bacterial contamination in platelet concentrates from Brazilian donors by molecular amplification of the ribosomal 16S gene. Transfus. Med. 28, 420–426. https://doi.org/10.1111/tme.12561 (2018).
Sireis, W. et al. Extension of platelet shelf life from 4 to 5 days by implementation of a new screening strategy in Germany. Vox. Sang. 101, 191–199. https://doi.org/10.1111/j.1423-0410.2011.01485.x (2011).
Wang, Y. & Qian, P. Y. Conservative fragments in bacterial 16S rRNA genes and primer design for 16S ribosomal DNA amplicons in metagenomic studies. PLoS ONE https://doi.org/10.1371/journal.pone.0007401 (2009).
Standards for Blood Banks and Transfusion Services: 31th Edition. (American Association of Blood Banks, 2018).
Heaton, W. A., Good, C. E., Galloway-Haskins, R., Yomtovian, R. A. & Jacobs, M. R. Evaluation of a rapid colorimetric assay for detection of bacterial contamination in apheresis and pooled random-donor platelet units. Transfusion 54, 1634–1641. https://doi.org/10.1111/trf.12603 (2014).
Greco-Stewart, V. S. et al. Serratia marcescens strains implicated in adverse transfusion reactions form biofilms in platelet concentrates and demonstrate reduced detection by automated culture. Vox. Sang. 102, 212–220. https://doi.org/10.1111/j.1423-0410.2011.01550.x (2012).
Störmer, M., Kleesiek, K. & Dreier, J. High-volume extraction of nucleic acids by magnetic bead technology for ultrasensitive detection of bacteria in blood components. Clin. Chem. 53, 104–110. https://doi.org/10.1373/clinchem.2006.070987 (2007).
Oliveira, B. B., Veigas, B. & Baptista, P. V. Isothermal amplification of nucleic acids: The race for the next “gold standard”. Front. Sens. 2, 1–22. https://doi.org/10.3389/fsens.2021.752600 (2021).
TwistAmp® Liquid DNA Amplification Kits. Combined Instruction Manual. (TwistDx Limited, 2018).
Veˇtrovsky, T. & Baldrian, P. The variability of the 16S rRNA Gene in bacterial genomes and its consequences for bacterial community analyses. PLoS ONE 8(2), e57923. https://doi.org/10.1371/journal.pone.0057923 (2013).
Palavecino, E. L., Yomtovian, R. A. & Jacobs, M. R. Bacterial contamination of platelets. Transfus. Apher. Sci. 42, 71–82. https://doi.org/10.1016/j.transci.2009.10.009 (2010).
Doseeva, V. et al. Multiplex isothermal helicase-dependent amplification assay for detection of Chlamydia trachomatis and Neisseria gonorrhoeae. Diagn. Microbiol. Infect. Dis. 71, 354–365. https://doi.org/10.1016/j.diagmicrobio.2011.08.021 (2011).
McDonald, C. P. Transfusion risk reduction: Testing for bacteria. ISBT. Sci. Ser. 8, 73–79 (2013).
Jacobs, M. R., Good, C. E., Lazarus, H. M. & Yomtovian, R. A. Relationship between bacterial load, species virulence, and transfusion reaction with transfusion of bacterially contaminated platelets. Clin. Infect. Dis. 46, 1214–1220. https://doi.org/10.1086/529143 (2008).
Acknowledgements
This research was financially supported by the 90th Anniversary Chulalongkorn University Fund and the Chulalongkorn University Ratchadaphiseksomphot Endowment Fund (CU- GR_63_83_37_10). The authors would like to acknowledge the Prof. Yong Poovorawan, the Centre of Excellence in Clinical Virology, Faculty of Medicine, Chulalongkorn University, Bangkok, Thailand, for providing hepatitis B virus DNA, and Assoc. Pitak Santanirand, the Microbiology Unit, Faculty of Medicine Ramathibodi Hospital, Mahidol University, Bangkok, Thailand, for providing bacterial ATCC and clinical strains DNA.
Author information
Authors and Affiliations
Contributions
P.R. created the conceptualisation, conducted the experiments, supervision and did funding acquisition and project administration. W.Y. conducted all the experiments and did the first draft manuscript. P.S. performed BacT/ALERT® culture and reidentified bacteria using MALDI-TOF. P.S. was an essentially intellectual contributor, conducted the experiments and analysed the data. P.R. and W.Y. analysed the statistical data and wrote the manuscript. All the authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Yamket, W., Sathianpitayakul, P., Santanirand, P. et al. Implementation of helicase-dependent amplification with SYBR Green I for prompt naked-eye detection of bacterial contaminants in platelet products. Sci Rep 13, 3238 (2023). https://doi.org/10.1038/s41598-023-30410-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-023-30410-8
This article is cited by
-
A recombinase polymerase amplification–SYBR Green I assay for the rapid and visual detection of Brucella
Folia Microbiologica (2023)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.