Abstract
Acute Stanford type A aortic dissection (ATAAD) with sudden onset and high mortality requiries a standard Bentall operation and a accurate prognosis in common, together with alteration of CO2 combining power (CO2CP) and serum sodium rase concern, hence, we evaluated the prognostic value of CO2CP combined with serum sodium in ATAAD patients. This retrospective study included 183 patients who underwent Bentall operation for ATAAD from 2015 to 2021 in the Fourth Hospital of Hebei Medical University, subsequently followed grouping by the levels of CO2CP and serum sodium. The study endpoint was 30-day all-cause mortality, and the prognostic value of CO2CP combined with serum sodium levels in ATAAD patients were evaluated with multivariate logistic regression method. The postoperative incidence of in-hospital death and adverse events in patients with ATAAD were 18% and 25.7%, respectively. Combination of CO2CP and serum sodium for predicting ATAAD death and adverse events presented a higher predictive value than each single indicator with ROC curve analysis (the AUC of CO2CP combined with serum sodium was 0.786, 95% CI 0.706–0.869, P < 0.001), along with CO2CP < 22.5 mmol/L + serum sodium > 138.5 mmol/L group had the worst prognostic. Multivariate regression analyse showed that CO2CP < 22.5 mmol/L combined with serum sodium > 138.5 mmol/L preferably predicted the prognosis of ATAAD (OR =6.073, 95% CI 2.557–14.425, P < 0.001). Consistently, the cumulative 30-day survival after surgery in ATAAD patients with the low CO2CP and high serum sodium simultaneously was the worst (log-rank P < 0.05). The combination of CO2CP and serum sodium increases the predictive value of prognosis, which is conducive to risk stratification of patients with ATAAD.
Similar content being viewed by others
Introduction
Acute Stanford type A aortic dissection (ATAAD) is a life-threatening cardiovascular disease with high mortality1, and the population-based incidence of ATAAD is stated between 5 and 12 cases/100,000 persons inhabitants/year2,3. Without the only effective surgery treatment, the mortalities at 48 h and 2 weeks from the onset are 50% and 80%, respectively4. ATAAD is also one of the four differential diagnoses of acute chest pain at the emergency department. The pathology department information showed, that only one in two cases of ATAAD was diagnosed3 and the rate of initial misdiagnosis was 16% in previous study5. The wide variety of symptoms, which are associated with acute aortic dissection, make it difficult to establish the correct diagnosis. Timely diagnosis is essential for successful management hat requires quick and accurate diagnosis as a delay in treatment carries a high mortality rate6,7. Variables associated with delayed diagnosis include female sex, the absence of typical historical features (abrupt-onset, chest, or back pain), or high-risk examination findings, including hypotension or pulse deficits8.
Although immediate surgical treatment has greatly reduced the mortality of ATAAD patients, the early postoperative mortality rate of ATAAD patients maintaints high with postoperative in-hospital mortality ranging from 7 to 27%9,10. Numerous mortality-related variables have been identified, such as lymphocyte to monocyte ratio, systolic blood pressure, N-terminal pro-brain natriuretic peptides, C-reactive protein, cardiac troponins, fibrinogen, etc.11,12,13,14,15,16; however, effective variables remained inadiquate, urging us to develop some novel predictors on the ATAAD prognosis in clinical practice.
In clinic, CO2 combing power (CO2CP) as a low cost and time-saving auxiliary diagnosis usually reflects the homeostasis of acidosis and alkalosis. Accumulating evidence shows the low CO2CP level linking with the worse prognosis of patients with olorectal cancer, acute kidney injury, acute ischaemic stroke17,18,19. Similarly, the latest reports also indicates the increased lactic acid as an independent risk factor for ATAAD complications, including postoperative acute kidney and lung injury20,21, thereby driving the application of acid–base balance index on prognosis. Significantly, Liao et al.22 reported that admission low serum level of bicarbonate (HCO3) can predict short-term and long-term mortality in patients with ATAAD. Consistantly, the association between decreased CO2CP level at admission and poor prognosis in patients undergoing Sun’s procedure for ATAAD was observed in our daily work23.
Abnormal serum sodium during hospitalization are risk factors for poor prognosis24,25 . Subsequently, we also verified that admission serum sodium of acute aortic dissection (including Stanford type B) patients play a vital on the postoperative hospital mortality26, whereas the link and interaction of CO2CP and serum sodium levels affecting all-cause death and adverse events of patients with ATAAD in context of different pathological type and surgical treatment is supposed to elaborated comprehensively. In addition, it should be noted that the predictive value of a single serum biomarker for ATAAD patients is usually limited, and it is difficult to simultaneously consider the sensitivity and specificity of prediction.
Therefore, this study focus on facilitating the prognosis prediction and outcome improvement via exploring the effect of admission CO2CP combined with serum sodium levels on the postoperative prognostic after Bentall procedure in patients with ATAAD.
Materials and methods
Study design and participants
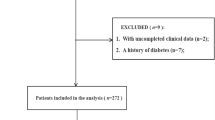
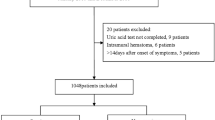
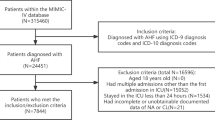
In this retrospective study, patients with ATAAD admitted to the Fourth Hospital of Hebei Medical University from 2015 to 2021 were enrolled and were radiological proven as type A aortic dissection by computed tomographic angiography (CTA) by the Stanford classification, following underwent Bentall procedure for ATAAD repair as well as had a disease course within 14 days with complete clinical information. Patients were excluded from this analysis if: (1) ill for more than 14 days, (2) previous aortic, (3) connective tissue diseases, pregnancy, traumatic dissection, or infection diseases, (4) patients without Bentall procedure, (5) severe preoperative complications (including serum creatinine at admission > 115 µmol/l, a preoperative stroke or unconscious on admission, respiratory insufficiency, and malignant tumor), (6) incomplete clinical data.
Collection and analysis of demographic and clinical data were approved by the ethics committee of the Fourth Hospital of Hebei Medical University (2021k7359). As patient data were anonymized, the ethics committee of the Fourth Hospital of Hebei Medical University waived the written informed consent. All procedures followed were in accordance with the revised Declaration of Helsinki.
Clinical data
Clinical variables of enrolled patients with ATAAD was obtained through review of medical records, including gender, age, medical history (hypertension, diabetes, coronary artery disease, prior surgery, prior trauma, smoking and drinking), complications, vital signs on admission (including systolic blood pressure, diastolic blood pressure, heart rate, etc.) and laboratory testing data on admission (alanine transaminase, aspartate transaminase, creatine, urea nitrogen, serum glucose, white blood cell count, neutrophil count, serum sodium, CO2CP, anion gap, etc.) as well as the duration of in-hospital. The laboratory data were obtained from the patients’ first venous blood samples taken at admission. The outcome of postoperative in-hospital patients with ATAAD was gotten from medical records, including operation selection and complicated with hypoperfusion syndrome etc. Hypoperfusion syndrome was defined as the reduced blood flow to one or more organs, resulting in organ ischemia and dysfunction1. Quality control was carried out in data collection to ensure accuracy.
Surgical techniques
Bentall procedure is a standard technique for complete aortic root replacement and all patients with ATAAD underwent a successful Bentall procedure within 24 h of admission. The surgical technique has been described in the literature27.
Observation endpoints
30-day all-cause mortality during hospitalization was defined as the primary endpoint. 30-day adverse events were served as the secondary endpoint. Adverse events included postoperative acute kidney injury, postoperative hypoxemia, low cardiac output syndrome and arrhythmia.
Statistical analysis
All continuous variables were normality tested by Shapiro–Wilk test. Data that was normally distributed were shown as mean ± SD, one-way ANOVA was applied between four groups. The measurement variables of non-normal distribution were represented by the median (P25, P75) with Kruskal–Wallis test. Categorical variables were presented as frequency (%), and Chi-squared test or Fisher's exact test was used for comparison between groups. Area under curve (AUC) and optimal cut-off value were computed by receiver operating characteristic (ROC) curve to evaluate the prediction value of admission CO2CP and serum sodium level in postoperative all-cause death and adverse events. Optimal cut-off value was determined as the point at which the Youden index (sensitivity + specificity − 1) was maximal. Based on CO2CP and serum sodium optimal cut-off value (22.5 mmol/L, 138.5 mmol/L, respectively), the patients were divided into four groups: group A (CO2CP ≥ 22.5 mmol/L and serum sodium>138.5 mmol/L); group B (CO2CP ≥ 22.5 mmol/L and serum sodium ≤ 138.5 mmol/L); group C (CO2CP < 22.5 mmol/L and serum sodium > 138.5 mmol/L); group D (CO2CP < 22.5 mmol/L and serum sodium ≤ 138.5 mmol/L). Univariate and multivariate logistic regression analysis were performed to examine the influencing factors of postoperative prognostic and to calculate OR and 95% CI. Multivariable analysis was adjusted for potential confounders: age, gender and a statistically significant association at P < 0.05 in univariate regression analysis. The cumulative survival curves in different groups were presented as Kaplan–Meier curves and compared by log-rank test. All statistical analyses were performed using SPSS 25.0 and GraphPad Prism 8.0, and a value of P < 0.05 was considered statistically significant.
Ethics approval and consent to participate
All clinical data related to the study were obtained after approved by the ethics committee of the Fourth Hospital of Hebei Medical University (2021k7359). All procedures followed in accordance with the revised Declaration of Helsinki.
Results
The ROC curve analysis of the CO2CP and serum sodium to predict prognosis in patients with ATAAD
183 patients were enrolled in this study. The postoperative incidence of in-hospital death and adverse events in patients with ATAAD were 18% (n = 33) and 25.7% (n = 47), respectively. Fifteen patients died of aortic root rupture, three died of postoperative infection and six patients died of postoperative acute kidney injury. The predicting efficiency of indicators were shown in Fig. 1A,B and Tables 1 and 2. The results of ROC curve analysis showed a higher predictive value for all-cause death and adverse events in CO2CP + serum sodium combination than each single indicator, seperately.
Preoperative baseline characteristics and postoperative early outcomes of patients with ATAAD
The average age of the participants was 51.3 ± 11.6 (22–82) years old, and about 67.2% (n = 123) of them were male. According to the cut-off value of CO2CP and serum sodium, all patients were divided into four groups (A–D). The demographic and clinical characters of patients with ATAAD were described as in Table 3. Compared with patients in group A, B and D, patients in group C had a higher serum chloride levels, and a higher anion gap (all P < 0.01).
The incidences of adverse events and mortality were significantly the highest in CO2CP < 22.5 mmol/L + serum sodium > 138.5 mmol/L group (all P < 0.01, Fig. 2A,B).
Univariable and multivariable predictors of 30-day all-cause mortality in patients with ATAAD
The results of univariate and multivariate analysis using logistic regression analysis adjusting for other potential predictors of mortality were shown in Tables 4 and 5. Age, gender, serum glucose, preoperative malperfusion, CO2CP and sodium variables were incorporated into the multivariate logistic model. After adjusting for these covariates, results showed that CO2CP < 22.5 mmol/L combined with serum sodium > 138.5 mmol/L was more suitable for predicting the all-casue mortality of ATAAD patients (OR = 6.073, 95% CI 2.557–14.425, P < 0.001, Table 5).
Survival curve analysis
Lastly, we conducted survival analysis of the combination of CO2CP and serum sodium levels of patients with ATAAD using the Kaplan–Meier curves to corroborate the above findings. As shown in Fig. 3A,B, Kaplan–Meier curves showed that combination low CO2CP levels with high serum sodium levels correlated with a higher incidence of all-cause deah and adverse events in ATAAD (log-rank P < 0.05).
Discussion
In this study, we demonstrted that the admission levels of CO2CP combined with serum sodium may be a potential predictive marker for determining the postoperative all-cause mortality and adverse events in patients with ATAAD, this remained significant even after adjusting for confounders. The combination of CO2CP and serum sodium could improve the predictive efficiency of 30-day in-hospital mortality during hospitalization.
The actual mechanisms by which decreased CO2CP leads to adverse outcomes in patients with ATAAD remain unclear. Acidity is a well-characterized factor associated with initiation and development of cardiovascular diseases. Accumulative evidence indicates that lower pH levels in the extracellular space and the circulation promoted the progression of AAD28. Extracellular acidity is generated mainly by aortic vascular smooth muscle cells through production of proton and lactic acid29, which is maintained by a combination of oxygen depletion from malperfusion, increased intracellular H+ efflux and high activity of the carbonic anhydrases, CAIX and CAXII, which results in the acceleration of extracellular CO2 to HCO3− and H+ in context of AAD-produced hypoxia. In turn, severe metabolic acidosis (a lower CO2CP in serum) not only damages the central nervous system but also induces ventricular arrhythmias and myocardial systolic disability. Moreover, acidosis could alter systemic vascular resistance promoting to aggravation of circulatory shock, leading to progressive cellular hypoxia and eventually causing end-organ failure. Patients with aortic dissection initially activate the coagulation fibrinolytic system30, accompanied by d-dimer and micro thrombosis in capillaries, causing abnormal blood flow rate, oxygen exchange obstacle, and glucose transformation into pyruvic acid under anaerobic conditions. The abnormally activated anaerobic glycolysis pathway mediates accumulation of pyruvic acid and lactic acid, ultimately exerting metabolic poisoning31,32. This acidic environment further drives the initiation and progression of complications as well as the poor prognosis. Severe metabolic acidosis not only damages the central nervous system but also induces ventricular arrhythmias and weakened myocardial systolic ability, which is fatal. Several studies verified the association of low HCO3− levels with poor clinical outcomes, including haemodialysis and other treatment33,34,35. Chin Sang Ong et al.36 also found that severe acidosis was associated with higher postoperative mortality (OR = 13.9, P = 0.001) in 298 patients with ATAAD, suggesting that severe acidosis may be a strong predictor of postoperative mortality. In addition, CO2CP as metabolic indicator of acidosis and alkalosis was easier diagnoses than HCO3− level in clinic, suggesting that evaluation of the acid–base homeostasis for patients with ATAAD in the emergency department would be accessible.
Hypoperfusion syndrome is a serious aortic dissection complication caused by the true and false lumen formation after aortic intima tear and the aortic branch vessel blockage by the torn inner membrane, leading to peripheral organ ischaemia and dysfunction before affecting early survival37. Czerny et al.38 revealed that 33.6% of patients were subjected to preoperative malperfusion, and the combined malperfusion syndrome was considered as an independent predictor of poor aortic dissection prognosis in a retrospective analysis of 2137 patients with ATAAD, which is similar to our study (OR = 3.335, 95% CI 1.430–7.777, P = 0.005).
The serological examination is considered as a suitable and simple way to assess a patient’s clinical status. Previous studies reported that serum sodium level change may affect vascular functions39. Experimental studies by Oberleithner40 revealed a 20% strengthened cell stiffness following the increased sodium concentration from 135 to 145 mmol/L and the decreased activity of endothelium-type nitric oxide synthase in endothelial cells, suggesting that alteration of serum sodium concentration also affect vascular endothelial function and vascular tone. In this study, we found that increased serum sodium was associated with in-hospital mortality in patients with ATAAD. More importantly, our data confirmed that the combination of CO2CP and serum sodium strengthened the predictive value for all-cause mortality in ATAAD, enhancing risk discrimination and providing important prognostic information for short-term follow-up after Bentall procedure.
An insight into the biomarker underlying complicated clinical scenarios is critical for developing primary or secondary preventions of ATAAD9, like as CO2CP and serum sodium. In agreement with previous studies, our results suggest that the hazardous effect of low CO2CP and high serum sodium appeared to be prominent in ATAAD patients with preoperative malperfusion, emphasising the requirement for intensive care and therapy. Combination of admission CO2CP and serum sodium, as the readily available parameters, easily simple for routine implementation in clinical practice, which can help clinicians choose more accurate therapies or early interventions for patients with ATAAD. Thus, we illustrates such a scenario that ATAAD patients with low CO2CP level and high serum sodium level at admission should be given more attention, and closely monitored hemodynamic indexes and malperfusion.
Overall, the present study highlights the predictive value of preoperative CO2CP combined with serum sodium in identifying patients with ATAAD who were at high risk of 30-day mortality and adverse events, better than that of a single elevated serum sodium and a single diminished CO2CP. Combination of CO2CP and serum sodium might be a better application in ATAAD managment.
Study limitations
Our study remains several limitations. First, based on a single-centre study with a small sample size, the conclusion will be further verified by a multicenter study. Second, the combination of serum HCO3−, base excess and pH value could be a better supplement. Third, the predictive CO2CP combined with serum sodium for the long-term prognosis in patients with ATAAD should be surveyed. Overall, further investigation of the underlying mechanism is supposed to the multiple-centre, large and prospective studies.
Conclusion
Combination of admission CO2CP and serum sodium levels presented a better predictive value for 30-day all-cause mortality and adverse outcomes of in-hospital patients undergoing Bentall procedure for ATAAD.
Data availability
The datasets generated and analyzed during the current study are available from the corresponding author on reasonable request.
References
Jennifer, S. L. et al. The profound impact of combined severe acidosis and malperfusion on operative mortality in the surgical treatment of type A aortic dissection. J. Thorac. Cardiovasc. Surg. 55(3), 897–904 (2018).
Kurz, S. D. et al. Insight into the incidence of acute aortic dissection in the German region of Berlin and Brandenburg. Int. J. Cardiol. 241, 326–329 (2017).
Maximilian, W. et al. Incidence of acute type A aortic dissection in emergency departments. Sci. Rep. 10, 7434 (2020).
Ke, Ch. et al. Clinical features and risk factors of postoperative in-hospital mortality following surgical repair of Stanford type A acute aortic dissection. BMC Cardiovasc. Disord. 21(1), 392–411 (2021).
Hansen Mark, S., Nogareda Gustavo, J. & Hutchison Stuart, J. Frequency of and inappropriate treatment of misdiagnosis of acute aortic dissection. Am. J. Cardiol. 99, 852–856 (2007).
Lisa, Z. et al. Acute type A aortic dissection: Aortic Dissection Detection Risk Score in emergency care—Surgical delay because of initial misdiagnosis. Eur. Heart J. Acute Cardiovasc. Care 9, S40–S47 (2020).
Kazuhito, H. et al. Clinical predictors for delayed or inappropriate initial diagnosis of type A acute aortic dissection in the emergency room. PLoS ONE 10, e0141929 (2015).
Harris Kevin, M. et al. Correlates of delayed recognition and treatment of acute type A aortic dissection: The International Registry of Acute Aortic Dissection (IRAD). Circulation 124, 1911–1918 (2011).
Okita, Y., Miyata, A. H., Motomura, B. N., Japan Cardiovascular Surgery Database Organization. A study of brain protection during total arch replacement comparing antegrade cerebral perfusion versus hypothermic circulatory arrest, with or without retrograde cerebral perfusion: Analysis based on the Japan Adult Cardiovascular Surgery Database. J. Thorac. Cardiovasc. Surg. 149(2 Suppl), S65-73 (2015).
Jana, T. et al. Left ventricular systolic dysfunction in patients with type-A aortic dissection is associated with 30-day mortality. J. Cardiothorac. Vasc. Anesth. 33(1), 51–57 (2019).
Lin, Y. J. et al. Association of lymphocyte to monocyte ratio and risk of in-hospital mortality in patients with acute type A aortic dissection. Biomark. Med. 13(15), 1263–1272 (2019).
Raimund, E. Hypotensive systolic blood pressure predicts severe complications and in-Hospital mortality in acute aortic dissection. J. Am. Coll. Cardiol. 71(13), 1441–1443 (2018).
Mislav, V., Ana, V. P. & Victor, A. N-terminal pro-brain natriuretic peptide and short-term mortality in acute aortic dissection: A meta-analysis. Clin. Cardiol. 43(11), 1255–1259 (2020).
Vrsalovic, M. & Vrsalovic, P. A. Admission C-reactive protein and outcomes in acute aortic dissection: A systematic review. Croat. Med. 60(4), 309–315 (2019).
Mislav, V. Prognostic effect of cardiac troponin elevation in acute aortic dissection: A meta-analysis. Int. J. Cardiol. 214, 277–288 (2016).
Guan, X. L. et al. Low preoperative fibrinogen level is risk factor for neurological complications in acute aortic dissection. Medicine 97(21), e10830 (2018).
Hu, J. C. et al. Metabolic acidosis as a risk factor for the development of acute kidney injury and hospital mortality. Exp. Ther. Med. 13(5), 2362–2374 (2017).
Sheng, L. S. et al. The significance of CO2 combining power in predicting prognosis of patients with stage II and III colorectal cancer. Biomark. Med. 13(13), 1071–1080 (2019).
Wang, A. et al. CO2 combining power and outcomes in patients with acute ischaemic stroke or transient ischaemic attack. Stroke Vasc. Neurol. 6(2), 252–259 (2021).
Zhang, K. et al. The prognosis and risk factors for acute kidney injury in high-risk patients after surgery for type A aortic dissection in the ICU. J. Thorac. Dis. 13(7), 4427–4437 (2021).
Pan, X. D. et al. Independent factors related to preoperative acute lung injury in 130 adults undergoing Stanford type-A acute aortic dissection surgery: A single-center cross-sectional clinical study. J. Thorac. Dis. 10(7), 4413–4423 (2018).
Tan, L., Xu, Q., Li, Ch., Chen, X. L. & Bai, H. Association between the admission serum bicarbonate and short-term and long-term mortality in acute aortic dissection patients admitted to the intensive care unit. Int. J. Gen. Med. 14, 4183–4195 (2021).
Huang, P. F. et al. Carbon-dioxide-combining-power and postoperative short-term mortality in patients with Stanford type A acute aortic dissection. Asian J. Surg. 45, 2925–2927 (2022).
Ploutarchos, T. et al. Dysnatremia is a predictor for morbidity and mortality in hospitalized patients with COVID-19. J. Clin. Endocrinol. Metab. 106, 1637–1648 (2021).
Patel Yash, R. et al. Prognostic significance of baseline serum sodium in heart failure with preserved ejection fraction. J. Am. Heart Assoc. 7, e007529 (2018).
Huang, P. F. et al. Serum sodium on admission affects postoperative in-hospital mortality in acute aortic dissection patients. PLoS ONE 16, e0261168 (2021).
Xue, Y. X. et al. Root reconstruction for proximal repair in acute type A aortic dissection. J. Thorac. Dis. 11, 4708–4716 (2019).
Shetty, V., Shales, S. & Narayan, P. Lactate levels: A reliable tool to predict mortality in acute type A aortic dissections?. J. Card. Surg. 37(5), 1212–1214 (2022).
Wu, X. et al. LDHA mediated degradation of extracellular matrix is a potential target for the treatment of aortic dissection. Pharmacol. Res. 176, 106051 (2022).
Yoon, S. H., Cho, Y. S., Park, C. Y. & Chung, C. H. Disseminated intravascular coagulation associated with aortic dissecting aneurysm. Korean J. Intern. Med. 19(2), 134–146 (2004).
Nazerian, P. et al. Diagnostic accuracy of the aortic dissection detection risk score plus D-dimer for acute aortic syndromes: The ADvISED prospective multicenter study. Circulation 137(3), 250–258 (2018).
Standards of Medical Care in Diabetes-2016: Summary of revisions. Diabetes Care 39(Suppl 1), S4–S5 (2016).
Menon, V. et al. Serum bicarbonate and long-term outcomes in CKD. Am. J. Kidney Dis. 56(5), 907–914 (2010).
Raphael, K. L., Guo, W., Baird, B. C., Greene, T. & Beddhu, S. Higher serum bicarbonate levels within the normal range are associated with better survival and renal outcomes in African Americans. Kidney Int. 79(3), 356–362 (2011).
Navaneethan, S. D. et al. Serum bicarbonate and mortality in stage 3 and stage 4 chronic kidney disease. Clin. J. Am. Soc. Nephrol. 6(10), 2395–2402 (2011).
Ong, C. S. et al. The strongest risk factor for operative mortality in acute type A aortic dissection is acidosis: Validation of risk model. Semin. Thorac. Cardiovasc. Surg. 32(4), 674–680 (2020).
Crawford, T. C. et al. Malperfusion syndromes in aortic dissections. Vasc. Med. 21(3), 2055–2058 (2016).
Czerny, M. et al. The impact of pre-operative malperfusion on outcome in acute type A aortic dissection: Results from the GERAADA registry. J. Am. Coll. Cardiol. 65(24), 2628–2635 (2015).
Dmitrieva, N. I., Burg, M. B. & Danilo, N. G. Elevated sodium and dehydration stimulate inflammatory signaling in endothelial cells and promote atherosclerosis. PLoS One 10(6), e0128870 (2015).
Hans, O. et al. Plasma sodium stiffens vascular endothelium and reduces nitric oxide release. Proc. Natl. Acad. Sci. U. S. A. 104(41), 16281–16296 (2007).
Acknowledgements
We thank Yong-bo Zhao and Yun-yan Wu doctors from the Cardiac Surgery Department, the Forth Hospital of Hebei Medical University, as well as all the staff during the study.
Funding
Dong Ma was supported by National Natural Science Foundation of China (No.81700416 and No.82270508), Key Laboratory of Neural and Vascular Biology, Ministry of Educational foundation (NV20210006), Natural Science Foundation of Hebei Province of China (H2022206279), and Science and Technology Research Project of Colleges and Universities of Hebei Province (QN2022164). Yong-bo Zhao was supported by 2022 Hebei Provincial Medical Science Research Major Projects (No. 20221293).
Author information
Authors and Affiliations
Contributions
P.H., D.M. and Y.Z. administrated this study with full access to all data and took responsibility for the integrity of the data and the accuracy of the data analysis. P.H. and D.M. conceived and completed the study design. P.H. generated the comprehensive data analysis and drafted the manuscript. Y.Z., X.L., Y.W. and Y.Z. helped in data collection. All authors participated in the revision and review of the manuscript and approved the final version.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Huang, Pf., Zhang, Yj., Lou, Xz. et al. Predictive value of admission CO2 combining power combined with serum sodium for the prognosis in acute Stanford type A aortic dissection patients. Sci Rep 13, 1048 (2023). https://doi.org/10.1038/s41598-022-27099-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-022-27099-6
This article is cited by
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.