Abstract
Circulating adiponectin shows some relationships with the occurrence of cardiometabolic diseases and osteoporotic fracture, but little is known about their causal associations. This two-sample Mendelian randomization (MR) study aims to explore the causal roles of circulating adiponectin in cardiometabolic diseases and osteoporotic fracture. We used 15 single nucleotide polymorphisms associated with circulating adiponectin as the instrumental variables. Inverse variance weighted, weighted median and MR-Egger regression methods were applied to study the causal associations. The results found that high circulating adiponectin was causally associated with reduced risk of type 2 diabetes (beta-estimate: −0.030, 95% CI: −0.048 to −0.011, SE: 0.009, P-value = 0.002) and may be the risk factor of coronary artery disease (beta-estimate: 0.012, 95% CI: 0.001 to 0.023, SE: 0.006, P-value = 0.030). No causal associations were seen between circulating adiponectin and other outcomes including heart failure, atrial fibrillation, cerebral ischemia, intracerebral hemorrhage or osteoporotic fracture. This study found the potential causal roles of high circulating adiponectin in reduced risk of type 2 diabetes and increased risk of coronary artery disease, which may help prevent and treat these two diseases.
Similar content being viewed by others
Introduction
Excess adiposity is widely accepted as the risk factor to cause many diseases such as cardiometabolic diseases and osteoporosis1,2,3,4. In patients with obesity, continued infiltration of immune cells (e.g. macrophages) into adipose tissue affects the secretion of many adipokines such as adiponectin and leptin5. Especially, adiponectin has emerged as an increasingly important factor because of its potential in protecting against type 2 diabetes, anti-inflammatory and anti-atherogenic effects6,7,8.
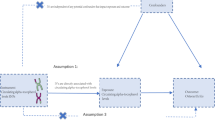
Observational studies reported that circulating adiponectin was associated with cardiometabolic diseases and osteoporotic fracture, but may suffer from confounding factors and reverse causality9,10,11,12,13,14. Their causal associations are not clear, and Mendelian randomization (MR) study has become one effective and powerful approach to explore the causal relationships between exposure phenotype and outcome phenotype15,16,17. Furthermore, two-sample MR analysis is able to greatly improve statistical power of MR study17,18,19,20.
Circulating adiponectin, cardiometabolic diseases and osteoporosis are highly polygenic traits according to the genome-wide association studies (GWASs)19,21,22,23,24. Adiponectin has important potential in regulating inflammatory responses which are associated with the modulation of cardiovascular diseases (e.g. coronary artery disease, heart failure and atrial fibrillation), type 2 diabetes, cerebral ischemia and osteoporosis25,26,27,28,29,30,31. Cardiometabolic diseases and osteoporosis have robust connection of pathogenesis. In addition, our recent MR study provides robust evidence that high circulating adiponectin is causally associated with the increased incidence of osteoporosis and low bone mineral density (BMD)32, but it is unknown whether circulating adiponectin affects the occurrence of osteoporotic fracture. Therefore, this two-sample MR study aims to study the causal influence of circulating adiponectin on the incidence of cardiometabolic diseases and osteoporotic fracture.
Methods
Data source of circulating adiponectin
One recent GWAS meta-analysis aimed to find the adiponectin-associated SNP variants, and included 25 independent studies and 67,739 adult individuals of the following ancestries: (1) European (n ≤ 60,465), (2) East Asian (n ≤ 2568), (3) African American (n ≤ 3271) and (4) Hispanic (n ≤ 1435)33. Different methods were used to measure adiponectin levels and comprised enzyme-linked immunosorbent assay (ELISA), radioimmunoassay (RIA), and dissociation-enhanced lanthanide fluoroimmunoassays (DELFIA). The unit of adiponectin levels was mg/mL. The results was adjusted for age, sex, body mass index (BMI) and principal components (PCs) that may cause population stratification33.
Initially, 18 SNPs were identified to have robust association with circulating adiponectin (P < 5 × 10−8, Supplementary Table S1). Linkage disequilibrium (LD) between selected SNPs was calculated using European samples from the 1000 Genomes project. Three SNPs (rs3087866, rs145119400 and rs3865188) were excluded due to high LD (r2 ≥ 0.001). Finally, we selected 15 SNPs as instrumental variables of circulating adiponectin (Supplementary Table S2).
Outcome data sources
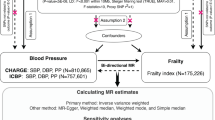
Several largest GWASs reported the summary-level data associated with genetic associations with outcomes (Table 1). Briefly, we studied cardiometabolic diseases including type 2 diabetes (898,130 individuals) from DIAGRAM34, coronary artery disease (547,261 individuals) from UK Biobank and CARDIoGRAMplusC4D35, heart failure (977,323 individuals) from UK Biobank36, atrial fibrillation (587,446 individuals) from one large meta-analysis37, cerebral ischemia (401,937 individuals) and intracerebral hemorrhage (399,717 individuals) from UK Biobank38. Osteoporotic fracture (426,795 individuals) were defined as any fracture apart from the fracture of skull, face, hands, feet, and pathological fractures due to malignancy, atypical femoral fractures, periprosthetic and healed fracture39. All participants in these GWASs were all from European descent except those with atrial fibrillation from predominantly European descent (mixed descents). Supplementary Table S2 demonstrated the SNP summary statistics related to circulating adiponectin and each outcome.
Statistical analyses
We used inverse variance weighted (IVW) meta-analysis of Wald ratio, weighted median and MR-Egger regression methods to assess the causal influence of circulating adiponectin on each outcome. The intercept term in MR-Egger regression was useful to assess the directional horizontal pleiotropy. Cochran’s Q analysis was applied to assess the heterogeneity19. Q statistic represented a chi-square distribution with m−1 degrees of freedom under the null hypothesis of homogeneity and its equation was presented as:
where m was the number of estimates to be pooled, \(w_{k}\) was the weight for the estimate \(\hat{\beta }_{XY}^{(k)}\) and represented the precision (reciprocal of the variance) of the estimate and μF was a weighted mean estimate calculated as \(\mu_{{\text{F}}} = \sum {w_{k} \hat{\beta }_{XY}^{(k)} /\sum {w_{k} } }\).
I2 index was defined as the percentage of total variation in the estimates explained by heterogeneity, and was calculated as:
Heterogeneity p-value < 0.05 indicated significant heterogeneity, while pleiotropy p-value < 0.05 suggested the presence of pleiotropic SNPs40. MR-PRESSO analysis attempted to find the pleiotropic SNPs and then reduce heterogeneity in the causal estimation by removing SNP outliers41.
All methods were carried out in accordance with relevant guidelines and regulations. Because this MR study was conducted by using publicly available GWAS summary data, ethical approval and informed consent obtained from all subjects could be found in the original publications. All analyses were performed in R V.4.0.4 by using the R packages of ‘MendelianRandomization’42, ‘TwoSampleMR’43 and ‘MR-PRESSO’ 44.
Results
Cardiometabolic diseases
We evaluated the causal effect of circulating adiponectin on type 2 diabetes, coronary artery disease, heart failure, atrial fibrillation, cerebral ischemia and intracerebral hemorrhage using multiple MR methods (Table 2). According to the weighted-median analysis, genetically high circulating adiponectin played a significant causal role in reduced risk of type 2 diabetes (beta-estimate: −0.030, 95% CI: −0.048 to −0.011, SE:0.009, P-value = 0.002), but it was not supported by IVW analysis (P-value = 0.590) or MR-Egger result (P-value = 0.426, Fig. 1 and Table 2). Scatter plot of the association between circulating adiponectin and Type 2 diabetes was shown in Supplementary Fig. S1.
In addition, IVW analyses showed that circulating adiponectin demonstrated no obviously causal impact on coronary artery disease (beta-estimate: 0.006, 95% CI: −0.009 to 0.020, SE:0.007, P-value = 0.439, Fig. 2 and Supplementary Fig. S2), heart failure (beta-estimate: 0.001, 95% CI: −0.012 to 0.014, SE:0.006, P-value = 0.023, Fig. 3 and Supplementary Fig. S3), atrial fibrillation (beta-estimate: 0.001, 95% CI: −0.012 to 0.014, SE: 0.007, P-value = 0.929, Fig. 4 and Supplementary Fig. S4), cerebral ischemia (beta-estimate: −0.002, 95% CI: −0.033 to 0.030, SE:0.016, P-value = 0.924, Fig. 5 and Supplementary Fig. S5) or intracerebral hemorrhage (beta-estimate: −0.035, 95% CI: −0.109 to 0.039, SE: 0.038, P-value = 0.173, Fig. 6 and Supplementary Fig. S6), and these results were confirmed by the weighted-median and MR-Egger analyses (P > 0.05, Table 2, Fig. 2–6 and Supplementary Figs. S2–S6).
Osteoporotic fracture
Previous studies have demonstrated that high circulating adiponectin is a risk factor of osteoporosis12,13, but it remains elusive whether circulating adiponectin affects the occurrence of osteoporotic fracture. IVW analysis unraveled that circulating adiponectin showed no causal role in the risk of osteoporotic fracture (beta-estimate: 0.007, 95% CI: −0.003 to 0.016, SE: 0.005, P-value = 0.173), which was also confirmed in weighted-median analysis (P-value = 0.297) and MR-Egger analysis (P-value = 0.970, Table 2 and Fig. 7). Scatter plot of the association between circulating adiponectin and osteoporotic fracture was shown in Supplementary Fig. S7.
Evaluation of assumptions and sensitivity analyses
Little evidence of directional pleiotropy was revealed for all models except the association between circulating adiponectin and atrial fibrillation (MR-Egger intercept P-value = 0.020, Table 2). There was significant heterogeneity for type 2 diabetes, coronary artery disease and atrial fibrillation. Thus, MR-PRESSO method was performed to find the SNP outliers, including 13 outliers (rs2791552, rs2943641, rs2276853, rs13303, rs13133548, rs4311394, rs3735080, rs10861661, rs7134375, rs11057405, rs11057353, rs2925979, rs4805885) for type 2 diabetes, 3 outliers (rs2943641, rs2925979, rs4805885) for coronary artery disease and one outlier (rs10861661) for heart failure (Table 3).
After excluding these SNP outliers, high circulating adiponectin showed the causal effect on increased risk of coronary artery disease (beta-estimate: 0.012, 95% CI: 0.001 to 0.023, SE:0.006, P-value = 0.030, Fig. 2 and Table 3). In addition, the MR association between circulating adiponectin with other outcomes were not changed after excluding the outlying SNP variants (Table 3).
Discussion
In this two-sample MR study, we found that high circulating adiponectin was causally associated with reduced risk of type 2 diabetes, but may be the risk factor of coronary artery disease. In addition, no causal roles of circulating adiponectin were revealed in the incidence of heart failure, atrial fibrillation, cerebral ischemia, intracerebral hemorrhage or osteoporotic fracture. These findings suggested that circulating adiponectin levels may provide new insights to prevent and treat type 2 diabetes and coronary artery disease.
Many studies report the associations between circulating adiponectin and insulin resistance, lipid levels, inflammatory markers, atherosclerosis biomarkers, type 2 diabetes and cardiovascular diseases, but their causal relationships remain elusive25,45,46,47. Observational studies reported the significantly inverse relationship between circulating adiponectin and fasting-insulin level48,49, and the close correlation between adiponectin levels and the incidence of type 2 diabetes was found in one population-based study50. In contrast, another study documented no association between circulating adiponectin and risk of type 2 diabetes51.
Considering these inconsistent results, two-sample MR study has become an increasingly important approach to explore risk factors of diseases19. One recent MR study included GWAS meta-analysis of circulating adiponectin levels (n = 39,883) and GWAS meta-analysis of type 2 diabetes (n = 659,316). The results found no causal effect of circulating adiponectin levels on the risk of type 2 diabetes52. More large-scale patient population were involved in our two-sample MR study, including the GWAS meta-analyses of circulating adiponectin levels (n = 67,739) and type 2 diabetes (n = 89,8130). Our research results revealed the high circulating adiponectin levels displayed a causal role in the decreased risk of type 2 diabetes. This protective effect of adiponectin on type 2 diabetes was attributed to anti-inflammatory properties and improvement in insulin sensitivity53, which were mediated by suppression of tumour necrosis factor alpha (TNF-α)54, inhibition of nuclear factor kappa B (NF-κB) in macrophages55, improved expression of interleukin-10 (IL-10) and promotion to macrophage transformation from M1 to M256.
Various studies reported that high circulating adiponectin levels were associated with low risk of cardiovascular diseases57,58, which were in contrast to other studies59,60,61. In addition, high circulating adiponectin levels may be the risk factor to increase mortality in patients with coronary artery disease62. One recent MR study included the GWASs associated with adiponectin (n = 39,883)63 and coronary artery disease (n = 184,305)64. The results found that high adiponectin was unlikely to be the risk factor of coronary artery disease65. However, our MR study included much larger-scale populations (i.e. 67,739 individuals related to adiponectin33 and 547,261 individuals associated with coronary artery disease35). After excluding these SNP outliers detected by MR-PRESSO method, high circulating adiponectin showed the causal effect on increased risk of coronary artery disease (beta-estimate: 0.012, 95% CI: 0.001 to 0.023, SE:0.006, P-value = 0.030, Fig. 2 and Table 3). These suggested that high circulating adiponectin may be one risk factor of coronary artery disease.
Adiponectin is almost exclusively produced by adipocytes, and its secretion is strongly dependent on cyclic guanosine monophosphate (cGMP)-dependent protein kinase which is activated in response to natriuretic peptide binding to specific receptor66. Thus, high adiponectin may be associated with high natriuretic peptide, which is a risk factor of coronary artery disease67. In addition, overproduction of adiponectin improves cardiac hypertrophy and cardiac function, and protect against ischemic/reperfusion injury in experimental models68,69.
Osteoporosis widely occurs in aging people and post-menopausal women, and is widely accepted to increase the incidence of osteoporotic fracture70,71. High adiponectin levels was documented to be a risk factor of osteoporotic fracture, but the positive finding may be affected by potential confounding factors and reverse causality14. Our recent MR study found that high circulating adiponectin has significantly causal impact on low BMD32, but the causal association between circulating adiponectin and osteoporotic fracture remains elusive. Our multiple analyses confirmed no causal relationship between circulating adiponectin and osteoporotic fracture. In addition, there is limited evidence of associations between circulating adiponectin and heart failure, atrial fibrillation, cerebral ischemia and intracerebral hemorrhage.
We should consider several strengths. Our MR study includes large-scale populations in order to investigate the causal effect of circulating adiponectin on cardiometabolic diseases and osteoporotic fracture. We use strong SNPs as instrumental variables (P < 5 × 10−8), and excluded SNPs in high LD. Multiple sensitivity analyses are used to test the influence of pleiotropy on causal estimates. To increase the reliability of our results, the outlier variants identified by the MR-PRESSO test are removed and causal estimates are recalculated. There are also several important limitations. Firstly, serum adiponectin is measured by various methods including ELISA, RIA and DELFIA, which may produce some heterogeneity. Secondly, participants in the summary GWASs are of predominantly European descent, but we can not perform the MR analyses based on different ancestries. Thus, our findings may not be fully representative of the whole population. Thirdly, the MR association between high serum adiponectin and decreased risk of type 2 diabetes is significant according to the weighted-median analysis, which is not supported by IVW, MR-Egger and MR-PRESSO methods. More large populations are needed to confirm this MR association. Fourthly, the causal role of high circulating adiponectin in low BMD in our previous MR study32, but the detrimental change is not translated to the increase in osteoporotic fracture, and the related mechanisms are still not clear.
Conclusion
In this two-sample MR study, high circulating adiponectin may be causally associated with reduced risk of type 2 diabetes and coronary artery disease, which may help prevent and treat these diseases.
Data availability
Data supporting the findings of this study were available within the paper.
References
Scheja, L. & Heeren, J. The endocrine function of adipose tissues in health and cardiometabolic disease. Nat. Rev. Endocrinol. 15(9), 507–524 (2019).
Goossens, G. H. The metabolic phenotype in obesity: fat mass. Body Fat Distrib Adipose Tissue Funct. Obesity Facts 10(3), 207–215 (2017).
Mechanick, J. I., Farkouh, M. E., Newman, J. D. & Garvey, W. T. Cardiometabolic-based chronic disease, adiposity and dysglycemia drivers: JACC state-of-the-art review. J. Am. Coll. Cardiol. 75(5), 525–538 (2020).
Scott, D., Johansson, J., Ebeling, P. R., Nordstrom, P. & Nordstrom, A. Adiposity without obesity: associations with osteoporosis, sarcopenia, and falls in the healthy ageing initiative cohort study. Obesity 28(11), 2232–2241 (2020).
Coltell, O., Ortega-Azorín, C., Sorlí, J. V., Portolés, O., Asensio, E. M., Saiz, C., Barragán, R., Estruch, R., Corella, D. Circulating adiponectin and its association with metabolic traits and type 2 diabetes: gene-diet interactions focusing on selected gene variants and at the genome-wide level in high-cardiovascular risk mediterranean subjects. Nutrients 13(2) (2021).
Trujillo, M. E. & Scherer, P. E. Adiponectin–journey from an adipocyte secretory protein to biomarker of the metabolic syndrome. J. Intern. Med. 257(2), 167–175 (2005).
Matsuzawa, Y., Funahashi, T., Kihara, S. & Shimomura, I. Adiponectin and metabolic syndrome. Arterioscler. Thromb. Vasc. Biol. 24(1), 29–33 (2004).
Matsuzawa, Y. The metabolic syndrome and adipocytokines. FEBS Lett. 580(12), 2917–2921 (2006).
Diah, M., Lelo, A., Lindarto, D. & Mukhtar, Z. Plasma concentrations of adiponectin in patients with coronary artery disease and coronary slow flow. Acta Med. Indones. 51(4), 290–295 (2019).
Stojanović, S., Ilić, M. D., Ilić, S., Petrović, D. & Djukić, S. The significance of adiponectin as a biomarker in metabolic syndrome and/or coronary artery disease. Vojnosanit. Pregl. 72(9), 779–784 (2015).
Bai, W., Huang, J., Zhu, M., Liu, X. & Tao, J. Association between elevated adiponectin level and adverse outcomes in patients with heart failure: a systematic review and meta-analysis. Braz J Med Biol Res 52(7), e8416 (2019).
Al-Osami, M. H. & Hameed, E. K. Serum adiponectin level in osteoporotic postmenopausal women with type 2 diabetes mellitus. Diabetes Metab Syndrome 12(6), 939–942 (2018).
Tanna, N. et al. The relationship between circulating adiponectin, leptin and vaspin with bone mineral density (BMD), arterial calcification and stiffness: a cross-sectional study in post-menopausal women. J. Endocrinol. Invest. 40(12), 1345–1353 (2017).
Nakamura, Y. et al. Two adipocytokines, leptin and adiponectin, independently predict osteoporotic fracture risk at different bone sites in postmenopausal women. Bone 137, 115404 (2020).
Davies, N. M., Holmes, M. V. & Smith, G. D. Reading Mendelian randomisation studies: a guide, glossary, and checklist for clinicians. BMJ 362, k601 (2018).
Burgess, S., Dudbridge, F. & Thompson, S. G. Combining information on multiple instrumental variables in Mendelian randomization: comparison of allele score and summarized data methods. Stat. Med. 35(11), 1880–1906 (2016).
He, B. et al. Depression and osteoporosis: a mendelian randomization study. Calcif. Tissue Int. https://doi.org/10.1007/s00223-021-00886-5 (2021).
Burgess, S., Scott, R. A., Timpson, N. J., Smith, G. D. & Thompson, S. G. Using published data in Mendelian randomization: a blueprint for efficient identification of causal risk factors. Eur J Epidemiol 30(7), 543–52 (2015).
He, B., Yin, L., Zhang, M., Lyu, Q., Quan, Z., Ou, Y. Causal effect of blood pressure on bone mineral density and fracture: a mendelian randomization study. Front. Endocrinol. 12(910) (2021).
Zhao, J., Zhang, M., Quan, Z., Deng, L., Li, Y., He, B. Systematic influence of circulating bilirubin levels on osteoporosis. Front. Endocrinol. 12(1022) (2021).
Warrington, N. M. et al. Maternal and fetal genetic effects on birth weight and their relevance to cardio-metabolic risk factors. Nat. Genet. 51(5), 804–814 (2019).
Iotchkova, V. et al. Discovery and refinement of genetic loci associated with cardiometabolic risk using dense imputation maps. Nat. Genet. 48(11), 1303–1312 (2016).
Trajanoska, K. & Rivadeneira, F. The genetic architecture of osteoporosis and fracture risk. Bone 126, 2–10 (2019).
Yang, T. L. et al. A road map for understanding molecular and genetic determinants of osteoporosis. Nat. Rev. Endocrinol. 16(2), 91–103 (2020).
Choi, H. M., Doss, H. M., Kim, K. S. Multifaceted physiological roles of adiponectin in inflammation and diseases. Int. J. Mol. Sci. 21(4) (2020).
Yu, B. et al. Wnt4 signaling prevents skeletal aging and inflammation by inhibiting nuclear factor-κB. Nat. Med. 20(9), 1009–1017 (2014).
Ali, M., Girgis, S., Hassan, A., Rudick, S. & Becker, R. C. Inflammation and coronary artery disease: from pathophysiology to Canakinumab Anti-Inflammatory Thrombosis Outcomes Study (CANTOS). Coron. Artery Dis. 29(5), 429–437 (2018).
Adamo, L., Rocha-Resende, C., Prabhu, S. D. & Mann, D. L. Reappraising the role of inflammation in heart failure. Nat. Rev. Cardiol. 17(5), 269–285 (2020).
Hu, Y. F., Chen, Y. J., Lin, Y. J. & Chen, S. A. Inflammation and the pathogenesis of atrial fibrillation. Nat. Rev. Cardiol. 12(4), 230–243 (2015).
Gao, G. et al. Glutaminase 1 regulates neuroinflammation after cerebral ischemia through enhancing microglial activation and pro-inflammatory exosome release. Front. Immunol. 11, 161 (2020).
He, B., Xia, L., Zhao, J., Yin, L., Zhang, M., Quan, Z., Ou, Y., Huang, W. Causal effect of serum magnesium on osteoporosis and cardiometabolic diseases. Front. Nutr. 8(955) (2021).
B. He, J. Zhao, M. Zhang, L. Yin, Z. Quan, Y. Ou, W. Huang, Casual roles of circulating adiponectin in osteoporosis and cancers. Bone (2021) 116266.
Spracklen, C. N. et al. Exome-derived adiponectin-associated variants implicate obesity and lipid biology. Am. J. Hum. Genet. 105(1), 15–28 (2019).
Mahajan, A. et al. Fine-mapping type 2 diabetes loci to single-variant resolution using high-density imputation and islet-specific epigenome maps. Nature Genetics 50(11), 1505–1513 (2018).
van der Harst, P. & Verweij, N. Identification of 64 novel genetic loci provides an expanded view on the genetic architecture of coronary artery disease. Circ. Res. 122(3), 433–443 (2018).
Shah, S. et al. Genome-wide association and Mendelian randomisation analysis provide insights into the pathogenesis of heart failure. Nat. Commun. 11(1), 163 (2020).
Roselli, C. et al. Multi-ethnic genome-wide association study for atrial fibrillation. Nat. Genet. 50(9), 1225–1233 (2018).
Zhou, W. et al. Efficiently controlling for case-control imbalance and sample relatedness in large-scale genetic association studies. Nat. Genet. 50(9), 1335–1341 (2018).
Morris, J. A. et al. An atlas of genetic influences on osteoporosis in humans and mice. Nat. Genet. 51(2), 258–266 (2019).
Greco, M. F., Minelli, C., Sheehan, N. A. & Thompson, J. R. Detecting pleiotropy in Mendelian randomisation studies with summary data and a continuous outcome. Stat. Med. 34(21), 2926–2940 (2015).
Burgess, S. & Thompson, S. G. Multivariable Mendelian randomization: the use of pleiotropic genetic variants to estimate causal effects. Am. J. Epidemiol. 181(4), 251–260 (2015).
Yavorska, O. O. & Burgess, S. MendelianRandomization: an R package for performing Mendelian randomization analyses using summarized data. Int. J. Epidemiol. 46(6), 1734–1739 (2017).
Hemani, G., Zheng, J., Elsworth, B., Wade, K. H., Haberland, V., Baird, D., Laurin, C., Burgess, S., Bowden, J., Langdon, R., Tan, V. Y., Yarmolinsky, J., Shihab, H. A., Timpson, N. J., Evans, D. M., Relton, C., Martin, R. M., Smith, G. D., Gaunt, T. R., Haycock, P. C. The MR-Base platform supports systematic causal inference across the human phenome. eLife 7 (2018).
Verbanck, M., Chen, C. Y., Neale, B. & Do, R. Detection of widespread horizontal pleiotropy in causal relationships inferred from Mendelian randomization between complex traits and diseases. Nat. Genet. 50(5), 693–698 (2018).
Nguyen, T. M. D. Adiponectin: role in physiology and pathophysiology. Int. J. Prev. Med. 11, 136 (2020).
Francischetti, E. A. et al. Insights into the controversial aspects of adiponectin in cardiometabolic disorders. Hormone Metab. Res. 52(10), 695–707 (2020).
A.E. Achari, S.K. Jain, Adiponectin, a therapeutic target for obesity, diabetes, and endothelial dysfunction. Int. J. Mol. Sci. 18(6) (2017).
Stefan, N. et al. Plasma adiponectin concentrations in children: relationships with obesity and insulinemia. J. Clin. Endocrinol. Metab. 87(10), 4652–4656 (2002).
Hotta, K. et al. Plasma concentrations of a novel, adipose-specific protein, adiponectin, in type 2 diabetic patients. Arterioscler. Thromb. Vasc. Biol. 20(6), 1595–1599 (2000).
Zhu, W., Cheng, K. K., Vanhoutte, P. M., Lam, K. S. & Xu, A. Vascular effects of adiponectin: molecular mechanisms and potential therapeutic intervention. Clin. Sci. 114(5), 361–74 (2008).
Kanaya, A. M. et al. Adipocytokines and incident diabetes mellitus in older adults: the independent effect of plasminogen activator inhibitor 1. Arch. Internal Med. 166(3), 350–356 (2006).
Chen, Z. et al. Effects of adiponectin on T2DM and glucose homeostasis: a mendelian randomization study. Diabetes Metab. Syndrome Obesity: Targets Therapy 13, 1771–1784 (2020).
Li, J. et al. Rosiglitazone elicits an adiponectin-mediated insulin-sensitizing action at the adipose tissue-liver axis in otsuka long-evans tokushima fatty rats. J. Diabetes Res. 2018, 4627842 (2018).
Ohashi, K. et al. Adiponectin promotes macrophage polarization toward an anti-inflammatory phenotype. J. Biol. Chem. 285(9), 6153–6160 (2010).
Yamaguchi, N. et al. Adiponectin inhibits Toll-like receptor family-induced signaling. FEBS Lett. 579(30), 6821–6826 (2005).
Wong, W. T. et al. Adiponectin is required for PPARγ-mediated improvement of endothelial function in diabetic mice. Cell Metab. 14(1), 104–115 (2011).
Pischon, T. et al. Plasma adiponectin levels and risk of myocardial infarction in men. JAMA 291(14), 1730–1737 (2004).
Kyrou, I. et al. Adiponectin circulating levels and 10-year (2002–2012) cardiovascular disease incidence: the ATTICA Study. Endocrine 58(3), 542–552 (2017).
Hao, G. et al. Serum total adiponectin level and the risk of cardiovascular disease in general population: a meta-analysis of 17 prospective studies. Atherosclerosis 228(1), 29–35 (2013).
Witberg, G. et al. Relation of adiponectin to all-cause mortality, cardiovascular mortality, and major adverse cardiovascular events (from the dallas heart study). Am. J. Cardiol. 117(4), 574–579 (2016).
Tu, W. J. et al. Elevated levels of adiponectin associated with major adverse cardiovascular and cerebrovascular events and mortality risk in ischemic stroke. Cardiovasc. Diabetol. 19(1), 125 (2020).
Mayer, O. et al. Is there really an association of high circulating adiponectin concentration and mortality or morbidity risk in stable coronary artery disease?. Hormone Metab. Res. 52(12), 861–868 (2020).
Dastani, Z. et al. The shared allelic architecture of adiponectin levels and coronary artery disease. Atherosclerosis 229(1), 145–148 (2013).
Nikpay, M. et al. A comprehensive 1000 genomes-based genome-wide association meta-analysis of coronary artery disease. Nat. Genet. 47(10), 1121–1130 (2015).
Au Yeung, S. L. & Schooling, C. M. Adiponectin and coronary artery disease risk: a bi-directional Mendelian randomization study. Int. J. Cardiol. 268, 222–226 (2018).
Withers, S. B. et al. Mechanisms of adiponectin-associated perivascular function in vascular disease. Arterioscler. Thromb. Vasc. Biol. 34(8), 1637–1642 (2014).
Tsukamoto, O. et al. Natriuretic peptides enhance the production of adiponectin in human adipocytes and in patients with chronic heart failure. J. Am. Coll. Cardiol. 53(22), 2070–2077 (2009).
Shibata, R. et al. Adiponectin protects against myocardial ischemia-reperfusion injury through AMPK- and COX-2-dependent mechanisms. Nat. Med. 11(10), 1096–1103 (2005).
Dadson, K. et al. Adiponectin is required for cardiac MEF2 activation during pressure overload induced hypertrophy. J. Mol. Cell. Cardiol. 86, 102–109 (2015).
Kanis, J. A., Cooper, C., Rizzoli, R. & Reginster, J. Y. European guidance for the diagnosis and management of osteoporosis in postmenopausal women. Osteoporosis Int. 30(1), 3–44 (2019).
He, B. et al. Effect of surgical timing on the refracture rate after percutaneous vertebroplasty: a retrospective analysis of at least 4-year follow-up. Biomed. Res. Int. 2021, 5503022 (2021).
Acknowledgements
The authors acknowledged the GEnetic Factors for OSteoporosis Consortium, the UK Biobank and DIAGRAM consortium for contributing the data used in this work.
Funding
This study was funded by Foundation of The First Affiliated Hospital of Chongqing Medical University (PYJJ2018-13), Natural Science Foundation of Chongqing (cstc2019jcyj-msxmX0836) and Medical Research Project of Luzhou-Southwest Medical University (2019LZXNYDJ37).
Author information
Authors and Affiliations
Contributions
M.Z., X.J.C., Y.Z., .L.Y. and B.H. conducted Study Design, Data Collection, Statistical Analysis. M.Z., X.J.C., Z.X.Q., Y.S.O., Y.Z. and B.H. conducted Data Interpretation, Manuscript Preparation, Literature Search. X.J.C. and B.H. conducted Funds Collection.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Zhang, M., Chen, X., Zhu, Y. et al. Causal associations of circulating adiponectin with cardiometabolic diseases and osteoporotic fracture. Sci Rep 12, 6689 (2022). https://doi.org/10.1038/s41598-022-10586-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-022-10586-1
This article is cited by
-
Inter-organ crosstalk during development and progression of type 2 diabetes mellitus
Nature Reviews Endocrinology (2024)
-
Causal influence of muscle weakness on cardiometabolic diseases and osteoporosis
Scientific Reports (2023)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.