Abstract
Intestinal helminths are highly prevalent in low-SES children and could contribute to poor health outcomes either directly or via alteration of the gut microbiome and gut barrier function. We analysed parasitic infections and gut microbiota composition in 325 children attending high- and low-SES schools in Makassar, Indonesia before and after albendazole treatment. Lactulose/Mannitol Ratio (LMR, a marker of gut permeability); I-FABP (a surrogate marker of intestinal damage) as well as inflammatory markers (LBP) were measured. Helminth infections were highly prevalent (65.6%) in low-SES children. LMR and I-FABP levels were higher in low-SES children (geomean (95%CI): 4.03 (3.67–4.42) vs. 3.22 (2.91–3.57); p. adj < 0.001; and 1.57 (1.42–1.74) vs. 1.25 (1.13–1.38); p. adj = 0.02, respectively) while LBP levels were lower compared to the high-SES (19.39 (17.09–22.01) vs. 22.74 (20.07–26.12); p.adj = 0.01). Albendazole reduced helminth infections in low-SES and also decreased LMR with 11% reduction but only in helminth-uninfected children (estimated treatment effect: 0.89; p.adj = 0.01). Following treatment, I-FABP decreased in high- (0.91, p.adj < 0.001) but increased (1.12, p.adj = 0.004) in low-SES children. Albendazole did not alter the levels of LBP. Microbiota analysis showed no contribution from specific bacterial-taxa to the changes observed. Intestinal permeability and epithelial damage are higher while peripheral blood inflammatory marker is lower in children of low-SES in Indonesia. Furthermore, treatment decreased LMR in helminth-uninfected only.
Similar content being viewed by others
Introduction
Approximately 1.5 billion people suffer from soil-transmitted helminth (STH) infections worldwide1. These infections are caused by different species of worms including Ascaris lumbricoides, Trichuris trichiura, Necator americanus and Ancylostoma duodenale2. Children from lower socioeconomic status (SES) backgrounds are often highly infected with parasitic helminths because of poor sanitation and limited access to clean water facilities3. Untreated, STH infection can cause malnutrition, impaired growth and physical development2,4.
Elevated intestinal permeability, and therefore impaired barrier function, along with gut inflammation and dysbiosis have been observed in various pathological conditions such as in stunting, obesity, and metabolic diseases5,6,7,8. The human intestine, which essentially allows absorptions of dietary products while maintaining a barrier function with selective permeability, prevents intrusion of pathogens or translocation of harmful products9. The intestinal lining is at the interface of interaction between helminths and protozoa that reside in the gastrointestinal tract and their human host and if damaged by parasites, could lead to poor barrier function and poor health outcomes.
To quantify the intestinal permeability in vivo, assays can be used that utilise the absorptive properties of differently sized carbohydrate probes5. The lactulose/mannitol ratio (LMR) is the most commonly used probe combination. As a result of increased intestinal permeability, bacterial products may be able to cross the barrier more easily and end up in the systemic circulation. Therefore, another way to characterize the intestinal permeability is by looking at markers for bacterial translocation. Examples of these include lipopolysaccharide binding protein (LBP)6. Compromised intestinal epithelial integrity and epithelial cell damage can also be assessed by measuring markers of intestinal injury such as intestinal-fatty acid binding protein (I-FABP)10.
Previous studies in low to middle income countries, have shown a difference in gut permeability of children of high and low SES11. Although an association between helminth infections and increased intestinal permeability12 was found in another study, there was no confirmation of causality through treatment. In the current study, we assessed the association between socioeconomic status (SES), intestinal parasitic infections and markers of intestinal barrier function. To this end, the presence of intestinal parasitic infections and the levels of LMR, I-FABP, and LBP were determined in schoolchildren of low- and high-SES, before and after albendazole treatment. In addition, this population has been characterized for baseline gut microbiota to assess the effect of socioeconomic status13. Here, we assessed the alteration of the gut microbiota after albendazole treatment to delineate any contribution to intestinal permeability and barrier function.
Results
Study participants
A total of 325 children (165 and 160 children from low- and high-SES schools, respectively) were recruited. Fifty-four children were lost to follow-up due to migrating out of the study area, absence from school for an extended period of time, or withdrawal of consent as indicated in consort diagram in Supplementary Figure S1. There were no differences in age, sex, SES, or z-BMI between those who remained in the study and those who were lost to follow-up (Supplementary Table S1).
The characteristics of children from low- and high-SES schools are shown in Table 1. The mean age and sex were comparable in both groups. The z-BMI was higher in the high- compared to low-SES children (z-BMI, mean ± SD: 0.27 ± 1.48 vs − 0.97 ± 1.19, p < 0.001). Prevalence of any helminth infection in low- and high-SES was 65.6% and 1.6%, respectively (p < 0.001). In high-SES group, only 2 children (1.6%) were infected with T. trichiura and no other STH infections were detected. In low-SES children, the prevalence of T. trichiura and A. lumbricoides was 65.6% and 39.8%, respectively. No hookworm infection was detected, but 2 children (1.6%) were infected with Hymenolepis diminuta (Table 1).
Similar to STH infections, intestinal protozoa prevalence was higher in low- compared to high-SES children (72.8% vs 39.2%, respectively, p < 0.001). The most prevalent species was G. lamblia followed by D. fragilis and E. histolytica. Infection with Cryptosporidium parvum was only detected in low-SES children (Table 1).
Intestinal barrier function in low-SES and high-SES children at baseline
Markers for intestinal permeability and acute intestinal injury exhibited substantial differences between low- and high-SES children (Figs. 1, 2). LMR was significantly higher in low- compared to high-SES children (geomean(95%CI): 4.03(3.67–4.42) vs. 3.22(2.91–3.57), respectively; adjusted p value (p.adj) < 0.001). I-FABP was also higher in low-SES (1.57(1.42–1.74) vs. 1.25(1.13–1.38); p.adj = 0.02). In contrast, LBP was lower in low- compared to high-SES (19.39(17.09–22.01) vs. 22.74(20.07–26.12); p.adj = 0.01). Additionally, we observed no correlation between any of these measurements (Supplementary Figure S2). To assess the role of parasitic infections in intestinal barrier function, we performed further analysis. Although univariate analysis showed that the presence of A. lumbricoides infection was associated with higher LMR levels (Supplementary Table S2), a subsequent linear regression model including both SES and A. lumbricoides demonstrated that the effect is mainly through SES (Table 2). Infection with D. fragilis was associated with higher LBP levels (Supplementary Table S2) but adding this variable into the model did not alter the effect of SES on LBP.
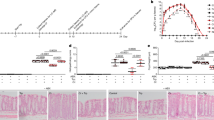
The effect of treatment on the proportion infected with (a) intestinal helminths (by microscopy) and (b) intestinal protozoa (by PCR). SES: socioeconomic status. AL: Ascaris lumbricoides, TT: Trichuris trichiura, HD: Hymenolepis diminuta, EH: Entamoeba histolytica, DF: Dientamoeba fragilis, GL: Giardia lamblia, CR: Cryptosporidium parvum. p values were calculated using a mixed effects logistic model fitted with subject random effects and adjusted for sex, age, and z-BMI.
Geometric means and their 95% confidence intervals for different gut permeability markers at baseline, LMR: Lactulose Mannitol Ratio (a), I-FABP: Intestinal fatty acid binding protein (b), and LBP: Lipopolysaccharide binding protein (c). SES: socioeconomic status. p values derived from linear regression models after adjusting for age, sex, and zBMI.
Furthermore, we observed no association between z-BMI and any of the gut biomarkers (Supplementary Table S3). In addition, the effect of SES on all these markers did not change after adjusting for z-BMI (Table 2).
Effect of albendazole treatment on parasitic infections and gut microbiota
In low-SES group, albendazole treatment resulted in a reduction of proportion of subjects infected with helminths and in infection intensity. Albendazole had the largest effect on A. lumbricoides, followed by T. trichiura (Fig. 1a). Before treatment, the percentage of moderate and light infection intensity for A. lumbricoides were 10.1% and 36.7% while 3.8% and 29.1% for T. trichiura, respectively. Following treatment, only light infections were seen for these two parasites and the proportion of those infected with A. lumbricoides and T. trichiura was reduced to 3.8% and 8.9%, respectively. In high-SES group, we found no helminth-infected children following albendazole administration. Treatment also led to a reduction in the prevalence of G. lamblia (from 51.7% to 31.7%, p.adj = 0.005 in low-SES; from 23.3% to 10.6%, p.adj = 0.04 in high-SES) but changes were not observed for other protozoa (Fig. 1b).
The differences in the diversity and composition of bacterial gut microbiota at baseline between high and low-SES children of this study have been published13. These children shared a core microbiota consisting of Bifidobacterium, Collinsella, and multiple members of Lachnospiraceae and Ruminicoccaceae families, but the diversity and the relative abundance of several taxa differed depending on SES13. At baseline, Shannon diversity index was higher in the low- compared to the high-SES; however, no differences were seen when we compared helminth-infected vs -uninfected in low-SES13. In line with this, after treatment, there were no changes in Shannon diversity index in low-SES children, whether these were helminth-infected or not, nor in high-SES children group (Fig. 3a). Similarly, we observed no alteration in gut microbiota composition in helminth-infected low-SES children after treatment. However, we observed some alteration of several short chain fatty acid (SCFA)-producing bacteria in the uninfected low- and high-SES children. We found decreased Faecalibacterium and Prevotella, but an increased Lactobacillus, Streptococcus, and Clostridiales relative abundance in the low-SES uninfected and high-SES children after albendazole treatment (Fig. 3b). In addition, some other bacteria changed in the same group: a decreased relative abundance of Succinivibrio, Dialister, and Rikenellaceae, and increased relative abundance of Bifidobacteriaceae and Bifidobacterium in low-SES helminth-uninfected children (Fig. 3b).
Effect of triple-dose albendazole treatment on (a) gut microbiota diversity; and b) gut microbiota composition in (i) low-SES helminth-infected, (ii) low-SE helminth-uninfected, and (iii) high-SES children. (a) Shannon diversity index measurements at both timepoints were compared using Wilcoxon signed rank test. Black closed-dots: before treatment; red open-dots: after treatment. (b) Data plotted as log2 fold change derived from differential abundance analysis by DESeq2. Cell colours indicate taxa changes after albendazole treatment: red colour indicate increased relative abundance after treatment and blue colour indicate decreased relative abundance after treatment. Only taxa detected to have significant difference in abundance (adjusted p value < 0.05) are displayed; adjusted p value were determined using Benjamini–Hochberg method. Row annotation showed specific taxa that were assigned under 4 different phylum. SES = Socioeconomic status.
Effect of albendazole treatment on intestinal barrier function
As shown in Fig. 4a, albendazole significantly decreased LMR in helminth-uninfected children. Estimated treatment effect was largest in high-SES children, with a 13% reduction (p.adj < 0.001), while in low-SES uninfected children there was a 11% reduction (p.adj = 0.01). No significant reduction was observed in low-SES children who were helminth-infected at baseline.
Effect of albendazole treatment on (a) LMR and (b) I-FABP in study children stratified by SES and helminth infection at baseline (i) high-SES (ii) low-SES helminth-uninfected; and (iii) low-SES helminth-infected. Analysis was using linear mixed model and adjusted for age, sex, and zBMI. The estimated treatment effects are presented as geometric means ratios with the corresponding 95% confidence interval.
Similar analysis was performed for I-FABP, marker of intestinal damage (Fig. 4b). Firstly, we observed a 9% decrease in I-FABP in high-SES children (p.adj < 0.001). In contrast, there was an increase of 12% (p.adj = 0.004) in I-FABP following albendazole treatment in low-SES helminth-infected children and although a similar increase was seen in the I-FABP in uninfected low-SES children, this fell short of statistical significance (p.adj = 0.08).
Regarding the protozoa, when the model was adjusted for these infections, the effect of albendazole on LMR and I-FABP did not change. Albendazole treatment did not alter the levels of LBP.
To answer the question whether the effect of treatment on LMR and I-FABP was mediated by a specific gut microbiota, we analysed the correlation between the relative abundance of specific taxa and these biomarkers. We could not pinpoint one specific bacterial taxon that might contribute to markers of gut barrier function nor to intestinal damage. (Supplementary Figure S3).
Discussion
In this study, we demonstrated that intestinal barrier function, measured by LMR, I-FABP, and LBP differs between low- and high-SES schoolchildren living in an urban center of Makassar, Indonesia. Low-SES children exhibited higher LMR and I-FABP, yet lower LBP. The higher LMR, indicating increased intestinal permeability and higher I-FABP, a marker of epithelial damage, show that the intestinal barrier function and integrity might be compromised in low- compared to the high-SES children. We had hypothesized that high intestinal permeability might allow bacterial translocation and result in higher LBP levels. Contrary to this, we observed higher LBP values in high SES children that were not associated with zBMI, which could mean that LBP is a better marker of inflammation associated with other factors, such as macronutrient intake. A longitudinal study of healthy lean subjects has shown an increase in LPS and LBP concentrations in subjects given a high-fat, high-carbohydrate meal but not in subjects given a high-fiber and fruit meal14.
In answer to our question whether the differences were due to intestinal parasitic helminths, which were different between low- and high-SES children, we assessed the effect of reducing helminth infections through albendazole treatment. The differences in LMR or I-FABP could not be attributed to current intestinal helminth infections. While LMR decreased after treatment with albendazole, this was restricted to children who were uninfected at baseline. In contrast, I-FABP, increased after albendazole treatment, which might indicate that killing and expulsion of worms, leads to more epithelial damage. In addition, although we observed some changes in microbiota composition after the administration of albendazole, the differences in gut integrity markers could not be explained by differences in microbiota composition. These data indicate that although there are significant differences in gut barrier function of low and high SES children, this could not be accounted for by current parasitic infections.
Despite deworming programs in Indonesia, helminth infections are still widespread, especially in low-SES children. In addition, several parasitic protozoa, such as G. lamblia, are more common in low-SES compared to high-SES children in our urban Indonesian population, in line with other studies15,16,17. Several studies have explored the effect of helminth infections on intestinal permeability, however only one has considered SES as a contributing factor11. A. lumbricoides infection was associated with elevated LMR in Bangladeshi and Malaysian children11,12, consistent with our findings in the crude analysis. However, multivariate analysis including both SES and A. lumbricoides indicated that SES is the main driver of the difference in LMR. Other factors than current A. lumbricoides infections could contribute to increased LMR, for example recurrent gastrointestinal infections that lead to diarrhea18. Intestinal permeability can be assessed by measuring several sugar probes such as lactulose, sucrose and sucralose5. Sucrose is thought to reflect gastroduodenal permeability, meanwhile sucralose indicates colonic permeability5,19. In this study, lactulose mannitol ratio was used to describe the gut function of each participant which reflects paracellular passage in the small intestines where most of the soil-transmitted helminths reside. An important other advantage of LMR over the other markers is that the urine collection is less time-consuming making it, therefore more suitable for use in children.
It should be noted that exercise can also induce intestinal damage or intestinal permeability, especially after a long and intense physical activity such as running or cycling for 90 min20. Several studies have shown that active school transport such as walking have been associated with higher physical activity in general21, which might contribute to the higher LMR in low-SES children.
I-FABP, expressed in mature intestinal epithelial cells, is released into circulation if the cell membranes are damaged22,23. I-FABP has been used as a non-invasive marker for acute intestinal damage or integrity loss24. In our study, we found no influence of Ascaris and Trichuris infections on I-FABP. This is in contrast to studies in subjects infected with hookworm and Strongyloides stercoralis, which reported elevated levels of I-FABP25,26. It is possible that the latter two helminths are more pathogenic, for example, hookworms feed on intestinal mucosa and blood27, which can indeed result in more damage. In our study, the marked increased I-FABP after treatment in helminth-infected children, might suggest that removal of worms leads to local inflammation and damage to epithelial cells, however, as there was a tendency for a similar effect in the helminth-uninfected low-SES children, it is possible that albendazole either directly or indirectly affects gut epithelial homeostasis and damage.
One of the biomarkers generated in response to bacterial translocation is LBP, a class 1 acute phase protein. Unexpectedly, in our study, LBP was found to be lower in low-SES where the intestinal barrier was more disrupted compared to high-SES children. The higher LBP levels in high-SES schoolchildren might be in line with previous observations where elevated LBP levels were linked to obesity, weight gain28,29, high fat and high carbohydrate diet14, as in the high-SES, the children have a different nutritional status and some are obese. However, these differences persisted after controlling for zBMI, suggesting there may be other factors at play, potentially high-fat and high-carbohydrate intake14,30 Another factors to consider is that LPS translocation is not necessarily only through paracellular leakage but also through transcellular transport31, however, the clinical relevance of this transcellular pathway is still unclear.
As published already, gut microbiota composition of Indonesian schoolchildren in our study is associated with socioeconomic status, even when living in the same urban area13. Not only sanitation32 but also differences in diet, hygiene, or helminth infections might be causes of the differences in the gut microbiota profile32,33,34,35. Regarding the diversity of microbiota in our population, we have reported that low-SES children have higher microbial diversity compared to high-SES children, independently of helminth-infection status13. Easton and colleagues showed that 3 weeks after albendazole treatment gut microbiota diversity did not change, yet, microbiota composition was altered with decreased Aeromonodales (Gammaproteobacteria). However, their study did not distinguish the effect of albendazole, between helminth infected and uninfected subjects36. In line with finding of Easton and colleagues, we showed no change in microbiota diversity while microbiota composition was altered 4 weeks after albendazole administration. Nonetheless, larger sample size in our study allowed us to stratify the population based on their SES and helminth status, where the relative abundance of several taxa was altered but only in the uninfected subjects and not in helminth-infected subjects of low-SES group. Moreover, we also observed changes in the high-SES children, indicating that alteration in bacterial taxa was more SES-related and not associated with helminth infections. Further studies should shed light on whether the altered microbiota composition, in a SES-specific manner, is albendazole-related or reflects natural oscillations over time.
An important limitation of our study is the substantial loss to follow-up. Despite our efforts to retain children within the study, 48% of children could not be followed up. However, we report no difference in baseline characteristics between the children that were lost to follow up and those who remained in the study. Furthermore, although we controlled for pre-identified confounders, dietary intake and physical activity was not surveyed, thus, their effect on intestinal permeability and microbiota composition could not be explored. No placebo was used in our study, consequently, we do not have the benefits of controlling for the changes related to time rather than treatment. Due to the lack of data regarding urine volume in this study, we are not able to compare the LMR result with published data and it is not possible to report the level of lactulose or mannitol urinary excretion.
In conclusion, the level of intestinal permeability and acute intestinal injury as measured by LMR, as well as LBP and I-FABP, differed between high- and low-SES children, and these differences were not associated with intestinal parasitic infections. Further research is needed to elucidate the exact mechanisms responsible for the elevated intestinal permeability in low-SES children as well as the off-targets effect of albendazole.
Material and methods
Study population and design
The study was conducted in Makassar, South Sulawesi, Indonesia. Ethical approval was obtained through the local ethics committee of Hasanuddin University (approval number: 1504/H04.8.4.5.31/PP36-KOMETIK/2016). This study was conducted in accordance with the Declaration of Helsinki. Study participants were recruited from two elementary schools that are distinct in SES. The low-SES school was located near the port area where mostly low-skilled labourers lived and worked. Children generally lived in the area surrounding the school site and travelled to school on foot. The high-SES school was located in the city centre. Children attending this school lived in distinct parts of the city, mostly in residential compounds and travelled to school by privately chartered school buses or by private vehicles.
The primary outcome of this study was intestinal permeability, as measured using LMR, while the secondary outcome was the intestinal damage and bacterial translocation, as assessed using I-FABP and LBP; after albendazole treatment in high and low SES schoolchildren. Based on previously reported data, we calculated that around 84 children were required in each group to detect a 25% relative difference in LMR (mean difference of 0.1, SD = 0.02) with a significance level of 5% (2-tailed) and a power of 90%.
Prior to the start of the study, an information letter concerning the study was given to the parents seeking permission for their children to participate in the study. Only children who returned the signed informed consent were included in the study. At baseline, anthropometry data were collected. Blood sample was obtained from median cubital vein by a venipuncturist. The day before, a stool container with enclosed spoon (Sarstedt AG&Co.KG, Nümbrecht, Germany) was given to these children. They were asked to collect stool samples in the morning before school, the same day when the study was conducted.
As soon as samples were gathered by research staff on site, stool, blood and urine samples were stored inside an ice box and transported to the Laboratory of Parasitology Department at Hasanuddin University and Hasanuddin University Medical Research Center laboratory to be aliquoted and kept at − 80˚C for further analyses.
After completion of the baseline visit, all participants received a single albendazole dose (400 mg, PT HoliPharma, Cimahi, Indonesia) given for three consecutive days regardless of their helminth infection status. The follow-up visit took place 4 weeks after treatment at which collection of blood, stool, and urine samples were repeated.
Parasitological examination
A single Kato-Katz slide was prepared from each stool sample37 and examined for the detection of STH Infection. Intensity was determined for each species according to WHO guidelines38. PCR was performed to identify intestinal protozoa. Briefly, DNA was extracted from stool samples followed by a multiplex real-time PCR used for the specific amplification and detection of Entamoeba histolytica, Dientamoeba fragilis, Giardia lamblia, and Cryptosporidium parvum. The procedure has been described elsewhere39,40,41. PCR output was expressed as the cycle threshold (Ct)-value reflecting the load of specific DNA in the sample tested. Protozoa specific DNA load were categorized into low load (35 ≤ Ct < 50), moderate load (30 ≤ Ct < 35), or high load (Ct < 30). Negative DNA results were recoded as Ct = 50.
Urinary lactulose-mannitol ratio (LMR)
Following overnight fasting, a lactulose/mannitol drink, containing 2 g mannitol and 5 g lactulose dissolved in 100 mL drinking water, was administered at school. The following three hours, all urine was collected in a large container together with 1 mL chlorhexidine 2% as a preservative. Urine samples were analysed using liquid chromatography mass spectrometry (LC–MS) as described previously42,43. LMR was calculated by dividing the lactulose concentration by the mannitol concentration in absence of data on the collected urine volumes. These values were multiplied with 100 to create percentages.
ELISA for measurements of I-FABP and LBP
ELISA techniques were used to quantify the concentrations of I-FABP and LBP (Duoset, R&D system, UK), according to the manufacturer’s instruction. For these assays, serum was diluted 8 and 2000 times for I-FABP and LBP, respectively. The results were expressed in ng/ml for I-FABP and µg/ml for LBP.
Microbiota analysis
Microbiota analysis was performed in 140 children from whom sufficient stool samples were available before and after treatment. The procedure for sample processing and microbiota analysis is already described elsewhere13. Raw sequencing data are available in the European Nucleotide Archive (https://www.ebi.ac.uk/ena) under study accession PRJEB38465 (baseline) and PRJEB40889 (follow up).
Statistical analysis
In accordance with the WHO guidelines, age standardized of z-scores of body mass index (z-BMI) were calculated. For the crude analyses, categorical data were compared using chi-square tests, whereas normally distributed continuous data was compared using the student t-test. Correlation between variables was tested using Pearson or Spearman correlation and we considered ρ ≥ 0.4 suggestive for a relevant correlation. To help explore the complex interplay between SES and helminth infection, the analysis was stratified into i) high-SES, ii) low-SES helminth-uninfected, and iii) low-SES helminth-infected. Linear regression models were used to adjust for a priori confounders such as age, sex, and z-BMI in addition to the identified explanatory variables. The data was analysed using IBM SPSS Statistics version 25 (IBM‐SPSS Inc., Chicago, USA), and GraphPad Prism (GraphPad Software, Inc., CA, US) was used for visualisation. Longitudinal data were analysed using mixed models with subject random effects, and fitted using lmerTest package (R software)44. LMR, I-FABP, and LBP were log10-transformed before analysis. Parameter estimates of treatment effects (95%CI) were then back transformed to obtain the geometric mean ratios (GMR). The reported p values were obtained using a likelihood ratio test comparing the model with and without a time effect.
Microbiota data were analysed in R-software (v3.5.1) using the packages phyloseq (v1.26.1)45, vegan (v2.5–4)46, ggplot2 (v3.1.0)47, DESeq2 (v1.22.2)48 and microbiome (v1.4.2)49. Wilcoxon signed rank tests were performed to compare Shannon diversity index before and after treatment groups. For differential abundance testing by DESeq2, the OTU-table was filtered for OTUs present in less than 25% of the samples to minimize zero-variance errors and spurious significance. Outcomes were considered significant when the Benjamini–Hochberg corrected p value was ≤ 0.05. To analyse albendazole-altered taxa in this population, paired analysis was done.
Conference presentation
Keystone Symposia “Helminths: New Insights from Immunity to Global Health”, Cape Town, South Africa, December 2019. Abstract number: 1003 (A.I.A.).
References
WHO. Soil-transmitted helminth infections. Fact sheet updated March 2020, https://www.who.int/news-room/fact-sheets/detail/soil-transmitted-helminth-infections (2020).
Bethony, J. et al. Soil-transmitted helminth infections: ascariasis, trichuriasis, and hookworm. Lancet 367, 1521–1532. https://doi.org/10.1016/S0140-6736(06)68653-4 (2006).
Strunz, E. C. et al. Water, sanitation, hygiene, and soil-transmitted helminth infection: a systematic review and meta-analysis. PLoS Med. 11, e1001620. https://doi.org/10.1371/journal.pmed.1001620 (2014).
Sanya, R. E., Nkurunungi, G., AndiaBiraro, I., Mpairwe, H. & Elliott, A. M. A life without worms. Trans. R. Soc. Trop. Med. Hyg. 111, 3–11. https://doi.org/10.1093/trstmh/trx010 (2017).
Bischoff, S. C. et al. Intestinal permeability–a new target for disease prevention and therapy. BMC Gastroenterol. 14, 189. https://doi.org/10.1186/s12876-014-0189-7 (2014).
Dirajlal-Fargo, S. et al. Altered intestinal permeability and fungal translocation in Ugandan children with HIV. Clin. Infect. Dis. https://doi.org/10.1093/cid/ciz561 (2019).
Guerrant, R. L. et al. Biomarkers of environmental enteropathy, inflammation, stunting, and impaired growth in children in Northeast Brazil. PLoS ONE 11, e0158772. https://doi.org/10.1371/journal.pone.0158772 (2016).
Fasano, A. Gut permeability, obesity, and metabolic disorders: who is the chicken and who is the egg?. Am. J. Clin. Nutr. 105, 3–4. https://doi.org/10.3945/ajcn.116.148338 (2017).
König, J. et al. Human intestinal barrier function in health and disease. Clin. Transl. Gastroenterol. 7, e196. https://doi.org/10.1038/ctg.2016.54 (2016).
Uhde, M. et al. Intestinal cell damage and systemic immune activation in individuals reporting sensitivity to wheat in the absence of coeliac disease. Gut 65, 1930–1937. https://doi.org/10.1136/gutjnl-2016-311964 (2016).
Raj, S. M., Sein, K. T., Anuar, A. K. & Mustaffa, B. E. Effect of intestinal helminthiasis on intestinal permeability of early primary schoolchildren. Trans. R. Soc. Trop. Med. Hyg. 90, 666–669 (1996).
Northrop-Clewes, C. A., Rousham, E. K., Mascie-Taylor, C. N. & Lunn, P. G. Anthelmintic treatment of rural Bangladeshi children: effect on host physiology, growth, and biochemical status. Am. J. Clin. Nutr. 73, 53–60 (2001).
Amaruddin, A. I. et al. The bacterial gut microbiota of schoolchildren from high and low socioeconomic status: A study in an urban area of Makassar, Indonesia. Microorganisms https://doi.org/10.3390/microorganisms8060961 (2020).
Ghanim, H. et al. Increase in plasma endotoxin concentrations and the expression of Toll-like receptors and suppressor of cytokine signaling-3 in mononuclear cells after a high-fat, high-carbohydrate meal: implications for insulin resistance. Diabet. Care 32, 2281–2287. https://doi.org/10.2337/dc09-0979 (2009).
Shrestha, J., Bhattachan, B., Rai, G., Park, E. Y. & Rai, S. K. Intestinal parasitic infections among public and private schoolchildren of Kathmandu, Nepal: prevalence and associated risk factors. BMC. Res. Notes 12, 192. https://doi.org/10.1186/s13104-019-4225-0 (2019).
Rogawski, E. T. et al. Determinants and Impact of Giardia Infection in the First 2 Years of Life in the MAL-ED Birth Cohort. J. Pediat. Infect. Dis. Soc. 6, 153–160. https://doi.org/10.1093/jpids/piw082 (2017).
Silva, R. R. et al. Association between nutritional status, environmental and socio-economic factors and Giardia lamblia infections among children aged 6–71 months in Brazil. Trans. R. Soc. Trop. Med. Hyg. 103, 512–519. https://doi.org/10.1016/j.trstmh.2008.10.019 (2009).
Zhang, Y. et al. Lactulose-mannitol intestinal permeability test in children with diarrhea caused by rotavirus and cryptosporidium. Diarrhea Working Group, Peru. J. Pediat. Gastroenterol. Nutr. 31, 16–21. https://doi.org/10.1097/00005176-200007000-00006 (2000).
van Wijck, K. et al. Novel multi-sugar assay for site-specific gastrointestinal permeability analysis: a randomized controlled crossover trial. Clin. Nutr. 32, 245–251. https://doi.org/10.1016/j.clnu.2012.06.014 (2013).
Karhu, E. et al. Exercise and gastrointestinal symptoms: running-induced changes in intestinal permeability and markers of gastrointestinal function in asymptomatic and symptomatic runners. Eur. J. Appl. Physiol. 117, 2519–2526. https://doi.org/10.1007/s00421-017-3739-1 (2017).
Larouche, R., Saunders, T. J., Faulkner, G., Colley, R. & Tremblay, M. Associations between active school transport and physical activity, body composition, and cardiovascular fitness: a systematic review of 68 studies. J. Phys. Act. Health 11, 206–227. https://doi.org/10.1123/jpah.2011-0345 (2014).
Pelsers, M. M. et al. Intestinal-type and liver-type fatty acid-binding protein in the intestine. Tissue distribution and clinical utility. Clin. Biochem. 36, 529–535. https://doi.org/10.1016/s0009-9120(03)00096-1 (2003).
Adriaanse, M. P. et al. Serum I-FABP as marker for enterocyte damage in coeliac disease and its relation to villous atrophy and circulating autoantibodies. Aliment. Pharmacol. Ther. 37, 482–490. https://doi.org/10.1111/apt.12194 (2013).
van Wijck, K. et al. Exercise-induced splanchnic hypoperfusion results in gut dysfunction in healthy men. PLoS ONE 6, e22366. https://doi.org/10.1371/journal.pone.0022366 (2011).
George, P. J. et al. Evidence of microbial translocation associated with perturbations in T cell and antigen-presenting cell homeostasis in hookworm infections. PLoS Negl. Trop. Dis. 6, e1830. https://doi.org/10.1371/journal.pntd.0001830 (2012).
Rajamanickam, A. et al. Microbial translocation associated with an acute-phase response and elevations in MMP-1, HO-1, and proinflammatory cytokines in strongyloides stercoralis infection. Infect. Immun. https://doi.org/10.1128/iai.00772-16 (2017).
Loukas, A. & Prociv, P. Immune responses in hookworm infections. Clin. Microbiol. Rev. 14, 689–703. https://doi.org/10.1128/cmr.14.4.689-703.2001 (2001).
Moreno-Navarrete, J. M. et al. A role for adipocyte-derived lipopolysaccharide-binding protein in inflammation- and obesity-associated adipose tissue dysfunction. Diabetologia 56, 2524–2537. https://doi.org/10.1007/s00125-013-3015-9 (2013).
Gonzalez-Quintela, A. et al. Determinants of serum concentrations of lipopolysaccharide-binding protein (LBP) in the adult population: the role of obesity. PLoS ONE 8, e54600. https://doi.org/10.1371/journal.pone.0054600 (2013).
Moreira, A. P., Texeira, T. F., Ferreira, A. B., Peluzio Mdo, C. & Alfenas Rde, C. Influence of a high-fat diet on gut microbiota, intestinal permeability and metabolic endotoxaemia. Br. J. Nutr 108, 801–809. https://doi.org/10.1017/s0007114512001213 (2012).
Ghoshal, S., Witta, J., Zhong, J., de Villiers, W. & Eckhardt, E. Chylomicrons promote intestinal absorption of lipopolysaccharides. J. Lipid Res. 50, 90–97. https://doi.org/10.1194/jlr.M800156-JLR200 (2009).
Mello, C. S. et al. Gut microbiota differences in children from distinct socioeconomic levels living in the same urban area in Brazil. J. Pediatr. Gastroenterol. Nutr. 63, 460–465. https://doi.org/10.1097/mpg.0000000000001186 (2016).
Chong, C. W. et al. Effect of ethnicity and socioeconomic variation to the gut microbiota composition among pre-adolescent in Malaysia. Sci. Rep. 5, 13338. https://doi.org/10.1038/srep13338 (2015).
Lee, S. C. et al. Helminth colonization is associated with increased diversity of the gut microbiota. PLoS Negl. Trop. Dis. 8, e2880. https://doi.org/10.1371/journal.pntd.0002880 (2014).
White, E. C. et al. Manipulation of host and parasite microbiotas: Survival strategies during chronic nematode infection. Sci. Adv. https://doi.org/10.1126/sciadv.aap7399 (2018).
Easton, A. V. et al. The impact of anthelmintic treatment on human gut microbiota based on cross-sectional and pre- and postdeworming comparisons in Western Kenya. mBio https://doi.org/10.1128/mBio.00519-19 (2019).
Katz, N., Chaves, A. & Pellegrino, J. A simple device for quantitative stool thick-smear technique in Schistosomiasis mansoni. Rev. Inst. Med. Trop. Sao Paulo 14, 397–400 (1972).
Montresor, A. et al. (World Health Organization, Geneva, 1998).
Kaisar, M. M. M. et al. Improved diagnosis of Trichuris trichiura by using a bead-beating procedure on ethanol preserved stool samples prior to DNA isolation and the performance of multiplex real-time PCR for intestinal parasites. Parasitology 144, 965–974. https://doi.org/10.1017/s0031182017000129 (2017).
Verweij, J. J. et al. Simultaneous detection of Entamoeba histolytica, Giardia lamblia, and Cryptosporidium parvum in fecal samples by using multiplex real-time PCR. J. Clin. Microbiol. 42, 1220–1223. https://doi.org/10.1128/jcm.42.3.1220-1223.2004 (2004).
Verweij, J. J. et al. Real-time PCR for the detection of Dientamoeba fragilis in fecal samples. Mol. Cell. Probes 21, 400–404. https://doi.org/10.1016/j.mcp.2007.05.006 (2007).
Janssen Duijghuijsen, L. M. et al. The effect of endurance exercise on intestinal integrity in well-trained healthy men. Physiol. Rep. https://doi.org/10.14814/phy2.12994 (2016).
van Wijck, K., van Eijk, H. M., Buurman, W. A., Dejong, C. H. & Lenaerts, K. Novel analytical approach to a multi-sugar whole gut permeability assay. J. Chromatogr. B Anal. Technol. Biomed. Life Sci. 879, 2794–2801, https://doi.org/10.1016/j.jchromb.2011.08.002 (2011).
Kuznetsova, A., Brockhoff, P. B. & Christensen, R. H. B. lmerTest package: Tests in linear mixed effects models. 2017 82, 26 %J. J. Stat. Softw., https://doi.org/10.18637/jss.v082.i13 (2017).
McMurdie, P. J. & Holmes, S. phyloseq: an R package for reproducible interactive analysis and graphics of microbiome census data. PLoS ONE 8, e61217. https://doi.org/10.1371/journal.pone.0061217 (2013).
Oksanen J, B. F., Friendly M, Kindt R, Legendre P, McGlinn D, et al. Vegan: Community Ecology Package, https://CRAN.R-project.org/package=vegan. (2018).
H, W. ggplot2: Elegant Graphics for Data Analysis. (2009).
Love, M. I., Huber, W. & Anders, S. Moderated estimation of fold change and dispersion for RNA-seq data with DESeq2. Genome Biol. 15, 550. https://doi.org/10.1186/s13059-014-0550-8 (2014).
Lahti L, S. S., et al. Tools for microbiome analysis in R. http://microbiome.github.com/microbiome. (2017).
Acknowledgements
The authors would like to thank all participants involved in this study as well as all their parents, teachers and principals of schools involved in this study, local government, Hasanuddin University Medical Research Center (HUM-RC) for laboratory facilities, and Hasanuddin University for the support. IPHIC team who were involved in this study as well as our field team are gratefully acknowledged for their tremendous efforts. The authors thank the Joint Scholarship of Directorate General of Resources for Science Technology and Higher Education (DGRSTHE) of Indonesia and Leiden University for providing PhD scholarship to A.A.
Funding
This work was supported by the Ministry of Research, Technology and Higher Education Republic of Indonesia (Kemenristekdikti) [Grant number: 9/E1/KP.PTNBH/2019 to F.H.]; Faculty of Medicine, Hasanuddin University, Indonesia [Grant number: 11146/UN4.6/PT.01.02/2021 to F.H. and A.A.]; and Leiden University Medical Center, The Netherlands. The sponsor of the study had no role in study design, data collection, data analysis, data interpretation, or writing of the report.
Author information
Authors and Affiliations
Contributions
Conceptualisation, M.Y. and F.H.; Funding acquisition, A.I.A, F.H. and M.Y.; Investigation, A.I.A., J.P.R.K., E.A.T.B., A.R.G., M.M., S.W., H.M.H.v.E, K.L, and R.D.Z.; Methodology, A.I.A., J.P.R.K, E.S., L.v.L, K.L and R.D.Z.; Project administration, A.I.A., J.P.R.K., F.H., S.W.; Supervision, E.S., F.H., and M.Y.; Writing—original draft, A.I.A. and J.P.R.K.; Writing— review and editing, A.I.A., J.P.R.K., M.M., H.M.H.v.E, K.L., E.A.T.B., L.v.L., A.R.G., R.D.Z, S.W., E.J.K., E.S., M.Y., and F.H. All authors contributed substantially; approved the submitted version; and agree to be personally accountable for their own contributions and for ensuring that questions related to the accuracy or integrity of any part of the work, even parts in which the author was not personally involved, are appropriately investigated, resolved, and documented in the literature. All authors have read and agreed to the submitted version of the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Amaruddin, A.I., Koopman, J.P.R., Muhammad, M. et al. Intestinal permeability before and after albendazole treatment in low and high socioeconomic status schoolchildren in Makassar, Indonesia. Sci Rep 12, 3394 (2022). https://doi.org/10.1038/s41598-022-07086-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-022-07086-7
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.