Abstract
In patients with acute ischemic stroke, pial collaterals play a key role in limiting neurological disability by maintaining blood flow to ischemic penumbra. We hypothesized that patient with poor pial collaterals will have greater corneal nerve and endothelial cell abnormalities. In a cross-sectional study, 35 patients with acute ischemic stroke secondary to middle cerebral artery (MCA) occlusion with poor (n = 12) and moderate-good (n = 23) pial collaterals and 35 healthy controls underwent corneal confocal microscopy and quantification of corneal nerve and endothelial cell morphology. In patients with MCA stroke, corneal nerve fibre length (CNFL) (P < 0.001), corneal nerve fibre density (CNFD) (P = 0.025) and corneal nerve branch density (CNBD) (P = 0.002) were lower compared to controls. Age, BMI, cholesterol, triglycerides, HDL, LDL, systolic blood pressure, NIHSS and endothelial cell parameters did not differ but mRS was higher (p = 0.023) and CNFL (p = 0.026) and CNBD (p = 0.044) were lower in patients with poor compared to moderate-good collaterals. CNFL and CNBD distinguished subjects with poor from moderate-good pial collaterals with an AUC of 72% (95% CI 53–92%) and 71% (95% CI 53–90%), respectively. Corneal nerve loss is greater in patients with poor compared to moderate-good pial collaterals and may act as a surrogate marker for pial collateral status in patients with ischemic stroke.
Similar content being viewed by others
Introduction
Stroke is a major cause of disability and the second leading cause of death1. Ischemic stroke typically occurs following occlusion of a cerebral artery due to in situ thrombosis or an embolus from the heart or neck vessels2. Several studies have shown that the “leptomeningeal collateral circulation”, or “pial collateral status” determines the neurological outcome following acute ischemic stroke3. Pial collaterals are anastomotic connections located on the pial surface of the cortex that connect distal branches of the anterior, middle and posterior cerebral arteries, which permit blood flow from the territory of an unobstructed artery into the territory of an occluded artery4. Indeed, patients with poor pial collaterals sustain larger infarcts, respond poorly to reperfusion, have increased risk for and severity of intracerebral hemorrhage and suffer increased morbidity and mortality3,5,6,7, whereas those with good collaterals have better reperfusion, smaller infarcts and less hemorrhagic transformation4. A method to help to identify the pial collateral status in stroke patients may allow risk stratification and more aggressive or targeted interventions to reduce neurologic disability.
There is considerable variability in the pial collateral status amongst patients with acute ischemic stroke8,9. Along with genetics factors, several modifiable risk factors such as hypertension10, metabolic syndrome, hyperuricemia11, smoking12 and hyperglycemia13 are associated with poor collaterals. Animal studies have shown that “rarefaction of collaterals” is associated with multiple cardiovascular risk factors14. MR imaging has also shown that the presence of white matter hyperintensities is associated with a poor pial collateral circulation15 and disease severity is associated with poorer outcomes after stroke16.
Corneal confocal microscopy (CCM) is a rapid non-invasive ophthalmic imaging technique that has been used to demonstrate axonal loss in patients with impaired glucose tolerance17, diabetes18,19, and other peripheral neuropathies20. Our recent studies have also demonstrated a significant reduction in corneal nerves21,22,23 and abnormalities in corneal endothelial cells in patients with TIA24 and acute ischemic stroke23. We have also shown that corneal nerve loss is associated with age, HbA1c, lipids and blood pressure19 and the presence of white matter hyperintensities25 in patients with acute ischemic stroke.
The aim of this study was to assess if corneal confocal microscopy-based quantification of corneal nerve and endothelial cell abnormalities could act as surrogate markers for the pial collateral status in patients with acute ischemic stroke.
Results
Thirty-five patients with acute MCA stroke were age-matched with thirty-five healthy controls (years) (51.54 ± 10.50 vs 52.82 ± 17.88, p = 0.717). The systolic blood pressure (mmHg) (144.71 ± 24.44 vs 132.31 ± 16.06, p = 0.014) was higher and HDL (mmol/l) 0.88 ± 0.21 vs 1.32 ± 0.37, p < 0.001) was lower in patients with stroke compared to controls.
Clinical, metabolic and neurological disability according to pial collateral status
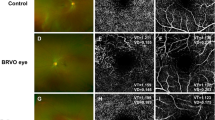
Patients with MCA stroke were classified into those with poor (n = 12) and moderate-good (n = 23) pial collaterals. Age (years) (52.42 ± 8.39 vs 51.09 ± 11.60, p = 0.797), gender (M/F) (21/02 vs 12/00, p = 0.293), BMI (kg/m2) (27.88 ± 3.40 vs 27.73 ± 4.39, p = 0.919), total cholesterol (mmol/l) (4.76 ± 1.26 vs 4.92 ± 0.97, p = 0.694), triglycerides (mmol/l) (1.59 ± 0.75 vs 1.68 ± 0.77, p = 0.632), LDL-cholesterol (mmol/l) (3.14 ± 1.00 vs 3.28 ± 0.89, p = 0.686), HDL-cholesterol (mmol/l) (0.91 ± 0.29 vs 0.87 ± 0.15, p = 0.626), systolic blood pressure (mmHg) (145.00 ± 20.32 vs 144.57 ± 26.76, p = 0.961) and HbA1c (%) (7.29 ± 3.69 vs 6.02 ± 1.16, p = 0.294) did not differ significantly between patients with poor compared to moderate-good pial collaterals (Table 1).
The modified Rankin Scale (mRS) at admission (3.00 ± 1.54 vs 1.68 ± 1.25, p = 0.023) was significantly higher (44%) in patients with poor compared to moderate-good pial collaterals. Although not significant, the mRS at discharge (mRS: 2.22 ± 1.79 vs 0.83 ± 1.04, p = 0.067), and the National Institute of Health Stroke Scale (NIHSS) at admission (14.67 ± 6.31 vs 10.68 ± 5.96, p = 0.065) and at discharge (8.00 ± 6.32 vs 3.76 ± 4.72, p = 0.120) were 63%, 37% and 53% higher in patients with poor compared to moderate-good pial collaterals, respectively (Table 1).
Corneal nerve and endothelial cell parameters in patients with acute ischemic stroke compared to controls
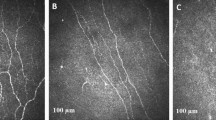
CNFL (mm/mm2;19.22 ± 5.78 vs 24.03 ± 5.21, p < 0.001), CNFD (no/mm2; 30.45 ± 8.41 ± 34.62 ± 6.70, p = 0.025) and CNBD (no/mm2; 64.20 ± 35.70 vs 97.31 ± 48.21, p = 0.002) were 20%, 12% and 34% lower in patients with MCA stroke compared to controls (Fig. 1, Table 2). There was no significant difference in corneal endothelial cell density (ECD) (no./mm2) (2876.61 ± 374.58 vs 2924.95 ± 229.20, p = 0.790), endothelial cell area (ECA) (µm2) (308.91 ± 41.19 vs 300.41 ± 21.57, p = 0.683), endothelial cell perimeter (ECP) (µm) (64.64 ± 4.33 vs 63.75 ± 2.60, p = 0.763), endothelial cell polymegathism (%) (49.62 ± 3.61 vs 52.38 ± 5.87, p = 0.112) or pleomorphism (%) (27.25 ± 4.64 vs 26.95 ± 5.10, p = 0.864) between patients with stroke compared to controls (Fig. 2, Table 2).
Corneal nerve and endothelial cell parameters in patients with poor compared to good pial collaterals
CNFL (mm/mm2) (16.26 ± 5.84 vs 20.76 ± 5.22, p = 0.026) and CNBD (no/mm2) (47.53 ± 30.04 vs 72.89 ± 35.89, p = 0.044) were 22% and 35% lower, with no difference in CNFD (p = 0.231) between patients with poor compared to moderate-good collaterals, respectively (Table 2, Fig. 3). There was no significant difference in ECD (no./mm2) (2697.86 ± 386.66 vs 2974.11 ± 346.57, p = 0.152), ECA (µm2) (329.44 ± 44.37 vs 297.71 ± 36.6, p = 0.133), ECP (µm) (66.67 ± 4.68 vs 63.54 ± 3.9, p = 0.160), endothelial cell polymegathism (%) (49.00 ± 2.6 vs 49.95 ± 4.14, p = 0.621) or pleomorphism (%) (28.28 ± 2.82 vs 26.68 ± 5.43, p = 0.515) between patients with poor compared to moderate-good collaterals (Fig. 2, Table 2).
Diagnostic accuracy for distinguishing patients with poor from moderate-good collaterals
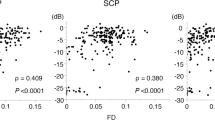
Table 3 and Fig. 4 show the diagnostic accuracy of CCM measures for identifying patients with poor compared to moderate-good collaterals. CNFL and CNBD distinguished subjects with poor from good collaterals with 72% AUC (95% CI 53–92%) and 71% AUC (95% CI 53–90%), respectively. Using an abnormal cutoff of CNFL ≤ 16 the sensitivity and specificity were 96% and 58%, respectively, and using an abnormal cutoff of CNBD ≤ 62 the sensitivity and specificity were 65% and 75% according to the Youden index.
Discussion
In this study, we show evidence of corneal nerve loss in patients with acute MCA stroke which agrees with our recent studies in patients with TIA24, acute21,23 and recurrent stroke22. Moreover, we show that corneal nerve loss was greater and there was good diagnostic accuracy for differentiating patients with poor compared to moderate-good pial collaterals, despite comparable blood pressure, lipids and HbA1c. We have previously shown corneal endothelial cell abnormalities in patients with TIA and stroke23, however, the current study showed no differences between patients with MCA stroke and controls or between patients with good compared to poor pial collaterals.
Although the pial collateral status plays a major role in determining neurological outcomes in acute ischemic stroke it can only be ascertained following the occurrence of large cerebral artery occlusion. White matter hyperintensities (WMH) predict poor stroke outcomes 90 days26,27,28 after thrombectomy and the presence of WMH was associated with greater cerebrovascular dysfunction in patients with large vessel occlusion15, whilst those without WMH had more favorable outcomes in the ASPECT score28. WMH are also associated with endothelial dysfunction29 and poor pial collateral circulation15. Indeed, many of the risk factors and comorbidities associated with WMHs have also been associated with poor pial collateral status. WMH increase with age30, hypertension31,32 and diabetes33,34 and may improve with antiplatelet therapy35 and improved management of hypertension31,32 and diabetes33,34. Of relevance to the current study, these same risk factors have been related to corneal nerve degeneration36 and indeed improvement in blood pressure, lipids and glycemic control is associated with corneal nerve regeneration37,38. Moreover, recently we showed that CCM may act as a surrogate imaging marker for the presence and severity of WMHs in patients with acute ischemic stroke25.
CCM has emerged as a powerful non-invasive ophthalmic imaging endpoint to identify corneal nerve loss as a surrogate marker for neurodegeneration in patients with multiple sclerosis39, Parkinson’s disease40, dementia41and patients with acute ischemic stroke21 and recurrent stroke22. We now show that CCM identifies greater corneal nerve loss in patients with poor compared to moderate/good pial collaterals. This ophthalmic imaging method may therefore act as a surrogate marker for poor pial collaterals and allow the identification of patients who require greater risk factor reduction and more urgent reperfusion after ischemic stroke. Indeed, in the present study patients with poor pial collaterals had a higher mRS and a previous study showed a larger infarct volume and higher mRS and NIHSS in patients with worse pial collateral scores42.
Limitations of the current study include the moderate sample size and the assessment of only patients with moderate disability who could undergo CCM. However, our study broadens the clinical utility of CCM in patients with neurodegenerative disease and patients with ischemic stroke. These data warrant larger studies utilising CCM in patients with or who are at risk of ischemic stroke.
Materials and methods
Thirty-five patients with middle cerebral artery occlusion and 35 age-matched healthy control participants attending the geriatric department at Hamad Medical Corporation were recruited from 2016 to 2018 in Doha, Qatar. In this cross-sectional study, exclusion criteria for participants with ischemic stroke were stroke due to a non-vascular disorder, or intracerebral hemorrhage, a known history of ocular trauma or surgery, high refractive error, and glaucoma. Healthy controls participants without known ocular or systemic co-morbidities including diabetes mellitus were also recruited.
Acute ischemic stroke was confirmed clinically and radiologically using American Heart Association (AHA) criteria43. The pial collateral status was established using multi-modal/dynamic CTA according to the criteria of Tan et al.44 by an investigator who was blinded to the patient’s corneal morphology status. The ordinal collateral score ranges from 0 to 3: 0 = absent collateral supply to the occluded MCA territory, 1 = collateral supply filling ≤ 50% but > 0% of the occluded MCA territory, 2 = collateral supply filling > 50% but < 100% of the occluded MCA territory and 3 = 100% collateral supply of the occluded MCA territory. Patients with pial collateral vessels filling equal to or less than 50% of the occluded middle cerebral artery territory were defined as those with ‘poor collaterals’ whereas patients with collateral vessels filling more than 50% of the occluded middle cerebral artery territory were defined as those with ‘moderate- good collaterals’.
Clinical and demographic data along with blood pressure, HbA1c and lipid profile were obtained at admission. The National Institutes of Health Stroke Scale (NIHSS)45 and modified Rankin Scale (mRS)46 was obtained for all patients at admission and at discharge from hospital. This study adhered to the tenets of the declaration of Helsinki and was approved by the Institutional Review Board of Weill Cornell Medicine (15-00021) and Hamad Medical Corporation (15304/15). Informed, written consent was obtained from all patients/guardians before participation in the study.
Corneal confocal microscopy
All patients underwent CCM (Heidelberg Retinal Tomograph III Rostock Cornea Module; Heidelberg Engineering GmbH, Heidelberg, Germany). CCM uses a 670 nm wavelength helium neon diode laser, which is a class I laser and therefore does not pose any ocular safety hazard. A × 63 objective lens with a numeric aperture of 0.9 and a working distance, relative to the applanating cap (TomoCap; Heidelberg Engineering GmbH) of 0.0 to 3.0 mm, is used. The size of each 2-dimensional image produced is 384 × 384 pixels with a 15° × 15° field of view and 10 μm/pixel transverse optical resolutions. To perform the CCM examination, local anesthetic (0.4% benoxinate hydrochloride; Chauvin Pharmaceuticals, Chefaro, United Kingdom) was used to anesthetize both eyes, and Viscotears (Carbomer 980, 0.2%, Novartis, United Kingdom) was used as the coupling agent between the cornea and the cap. Patients were asked to fixate on an outer fixation light throughout the CCM scan and a CCD camera was used to correctly position the cap onto the cornea20. The examination took approximately 10 min for both eyes. The examiners captured images of the central sub-basal nerve plexus using the section mode. On the basis of depth, contrast, focus, and position, 6 images per patient were selected47.
All CCM images were manually analysed using validated, purpose-written software by an investigator blinded to the collateral status of the participants. Corneal nerve fiber density (CNFD: total number of major nerves/mm2), corneal nerve branch density (CNBD: number of branches emanating from major nerve trunks/mm2), corneal nerve fiber length (CNFL: total length of all nerve fibers and branches mm/mm2) and inferior whorl length (IWL: total length of all nerve fibers in the inferior whorl area mm/mm2) were analyzed using CCMetrics (M. A. Dabbah, ISBE, University of Manchester, Manchester, United Kingdom)18. Corneal endothelial cell images were analyzed using the Corneal Endothelium Analysis System (CEAS), an automated image analysis system48. Endothelial cell density (ECD, cells/mm2), endothelial cell area (ECA, µm2), endothelial cell perimeter (ECP, µm), endothelial cell polymegathism (%) and endothelial cell pleomorphism (%) were quantified. Polymegathism was defined as the standard deviation of the cell area divided by the mean cell area, while pleomorphism was defined as the hexagonality coefficient. Adequate corneal endothelial cells images were available in seventeen patients with poor (n = 6) and moderate-good (n = 11) collaterals and sixteen healthy controls.
Statistical analysis
All statistical analyses were performed using IBM SPSS Statistics software Version 25. Normality of the data was assessed using the Shapiro–Wilk test and by visual inspection of the histogram and a normal Q-Q plot. Data are expressed as mean ± standard deviation (SD). Mann Whitney test (for non-normally distributed variables) and t-test (for normally distributed variables) were performed to find the differences between two groups. Receiver operating characteristic (ROC) curve analysis was performed for corneal nerve parameters to identify patients with poor compared to moderate-good collateral status.
Ethics approval
This study adhered to the tenets of the declaration of Helsinki and was approved by the Institutional Review Board of Weill Cornell Medicine (15-00021) and Hamad General Hospital (15304/15).
Consent to participate
Informed, written consent was obtained from all patients/guardians before participation in the study.
Consent for publication
Written consent was obtained from all patients/guardians for publications.
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Virani, S. S. et al. Heart disease and stroke statistics—2020 update: A report from the American Heart Association. Circulation 141, e139–e596 (2020).
Adams, H. P. Jr. et al. Classification of subtype of acute ischemic stroke. Definitions for use in a multicenter clinical trial. TOAST. Trial of Org 10172 in Acute Stroke Treatment. Stroke 24, 35–41 (1993).
Jung, S. et al. Relevance of the cerebral collateral circulation in ischaemic stroke: Time is brain, but collaterals set the pace. Swiss Med. Wkly. 147, 14538 (2017).
Shuaib, A., Butcher, K., Mohammad, A. A., Saqqur, M. & Liebeskind, D. S. Collateral blood vessels in acute ischaemic stroke: A potential therapeutic target. Lancet Neurol. 10, 909–921 (2011).
Leng, X. et al. Impact of collateral status on successful revascularization in endovascular treatment: A systematic review and meta-analysis. Cerebrovasc. Dis. 41, 27–34 (2016).
Flores, A. et al. Poor collateral circulation assessed by multiphase computed tomographic angiography predicts malignant middle cerebral artery evolution after reperfusion therapies. Stroke 46, 3149–3153 (2015).
Christoforidis, G. et al. Predictors of hemorrhage following intra-arterial thrombolysis for acute ischemic stroke: The role of pial collateral formation. AJNR Am. J. Neuroradiol. 30, 165–170 (2009).
Malhotra, K. & Liebeskind, D. S. Collaterals in ischemic stroke. Brain Hemorrhages 1, 6–12 (2020).
Faber, J. E. et al. Genetic and environmental contributions to variation in the posterior communicating collaterals of the circle of Willis. Transl. Stroke Res. 10, 189–203 (2019).
Fujita, K. et al. Detrimental effect of chronic hypertension on leptomeningeal collateral flow in acute ischemic stroke. Stroke 50, 1751–1757 (2019).
Menon, B. K. et al. Leptomeningeal collaterals are associated with modifiable metabolic risk factors. Ann. Neurol. 74, 241–248 (2013).
Nannoni, S. et al. Determining factors of better leptomeningeal collaterals: A study of 857 consecutive acute ischemic stroke patients. J. Neurol. 266, 582–588 (2019).
van Seeters, T., Biessels, G. J., Kappelle, L. J., van der Graaf, Y. & Velthuis, B. K. Determinants of leptomeningeal collateral flow in stroke patients with a middle cerebral artery occlusion. Neuroradiology 58, 969–977 (2016).
Moore, S. M., Zhang, H., Maeda, N., Doerschuk, C. M. & Faber, J. E. Cardiovascular risk factors cause premature rarefaction of the collateral circulation and greater ischemic tissue injury. Angiogenesis 18, 265–281 (2015).
Mark, I. et al. Leukoaraiosis and collateral blood flow in stroke patients with anterior circulation large vessel occlusion. J. Neurointerv. Surg. 2, 2 (2020).
Huo, L. et al. Impact of leukoaraiosis severity on the association of outcomes of mechanical thrombectomy for acute ischemic stroke: A systematic review and a meta-analysis. J. Neurol. 2, 1–9 (2020).
Asghar, O. et al. Corneal confocal microscopy detects neuropathy in subjects with impaired glucose tolerance. Diabetes Care 37, 2643–2646 (2014).
Petropoulos, I. N. et al. Rapid automated diagnosis of diabetic peripheral neuropathy with in vivo corneal confocal microscopy. Invest. Ophthalmol. Vis. Sci. 55, 2071–2078. https://doi.org/10.1167/iovs.13-13787 (2014).
Ferdousi, M. et al. Diagnosis of neuropathy and risk factors for corneal nerve loss in type 1 and type 2 diabetes: A corneal confocal microscopy study. Diabetes Care 44, 150–156 (2021).
Tavakoli, M. & Malik, R. A. Corneal confocal microscopy: A novel non-invasive technique to quantify small fibre pathology in peripheral neuropathies. J. Vis. Exp. https://doi.org/10.3791/2194 (2011).
Khan, A. et al. Corneal confocal microscopy detects corneal nerve damage in patients admitted with acute ischemic stroke. Stroke 48, 3012–3018. https://doi.org/10.1161/STROKEAHA.117.018289 (2017).
Khan, A. et al. Corneal confocal microscopy identifies greater corneal nerve damage in patients with a recurrent compared to first ischemic stroke. PLoS ONE 15, e0231987 (2020).
Khan, A. et al. Corneal confocal microscopy detects a reduction in corneal endothelial cells and nerve fibres in patients with acute ischemic stroke. Sci. Rep. 8, 17333 (2018).
Gad, H. et al. Corneal nerve and endothelial cell damage in patients with transient ischemic attack and minor ischemic stroke. PLoS ONE 14, e0213319. https://doi.org/10.1371/journal.pone.0213319 (2019).
Kamran, S. et al. Cornea: A window to white matter changes in stroke; corneal confocal microscopy a surrogate marker for the presence and severity of white matter hyperintensities in ischemic stroke. J. Stroke Cerebrovasc. Dis. 2, 1–8 (2020).
Griessenauer, C. J. et al. Effects of white matter hyperintensities on 90-Day functional outcome after large vessel and non-large vessel stroke. Cerebrovasc. Dis. 49, 1–8 (2020).
Mutzenbach, J. S. et al. Severe leukoaraiosis is associated with poor outcome after successful recanalization of M1 middle cerebral artery occlusion strokes. Cerebrovasc. Dis. 49, 253–261 (2020).
Regenhardt, R. W. et al. White matter acute infarct volume after thrombectomy for anterior circulation large vessel occlusion stroke is associated with long term outcomes. J. Stroke Cerebrovasc. Dis. 30, 105567 (2020).
Young, V. G., Halliday, G. M. & Kril, J. J. Neuropathologic correlates of white matter hyperintensities. Neurology 71, 804–811 (2008).
Smith, E. E. et al. Prevention of stroke in patients with silent cerebrovascular disease: A scientific statement for healthcare professionals from the american heart association/american stroke association. Stroke 48, e44–e71. https://doi.org/10.1161/STR.0000000000000116 (2017).
de Leeuw, F. E. et al. Hypertension and cerebral white matter lesions in a prospective cohort study. Brain 125, 765–772. https://doi.org/10.1093/brain/awf077 (2002).
Dufouil, C. et al. Longitudinal study of blood pressure and white matter hyperintensities: The EVA MRI Cohort. Neurology 56, 921–926. https://doi.org/10.1212/wnl.56.7.921 (2001).
McNay, E. C. The impact of recurrent hypoglycemia on cognitive function in aging. Neurobiol. Aging 26(Suppl 1), 76–79. https://doi.org/10.1016/j.neurobiolaging.2005.08.014 (2005).
Geijselaers, S. L. C. et al. The role of hyperglycemia, insulin resistance, and blood pressure in diabetes-associated differences in cognitive performance—The Maastricht Study. Diabetes Care 40, 1537–1547. https://doi.org/10.2337/dc17-0330 (2017).
Gorelick, P. B. et al. Vascular contributions to cognitive impairment and dementia: A statement for healthcare professionals from the american heart association/american stroke association. Stroke 42, 2672–2713. https://doi.org/10.1161/STR.0b013e3182299496 (2011).
Ponirakis, G. et al. Hypertension contributes to neuropathy in patients with type 1 diabetes. Hypertension 32, 796–803. https://doi.org/10.1093/ajh/hpz058 (2019).
Tavakoli, M. et al. Corneal confocal microscopy detects improvement in corneal nerve morphology with an improvement in risk factors for diabetic neuropathy. Diabet. Med. 28, 1261–1267. https://doi.org/10.1111/j.1464-5491.2011.03372.x (2011).
Azmi, S. et al. Early nerve fibre regeneration in individuals with type 1 diabetes after simultaneous pancreas and kidney transplantation. Diabetologia 62, 1478–1487 (2019).
Petropoulos, I. N. et al. Corneal confocal microscopy: An imaging endpoint for axonal degeneration in multiple sclerosis. Invest Ophthalmol. Vis. Sci. 58, 3677–3681 (2017).
Lim, S. H. et al. Corneal confocal microscopy detects small fibre neurodegeneration in Parkinson’s disease using automated analysis. Sci. Rep. 10, 1–7 (2020).
Ponirakis, G. et al. Association of corneal nerve fiber measures with cognitive function in dementia. Ann. Clin. Transl. Neurol. 6, 689–697 (2019).
Christoforidis, G. A., Mohammad, Y., Kehagias, D., Avutu, B. & Slivka, A. P. Angiographic assessment of pial collaterals as a prognostic indicator following intra-arterial thrombolysis for acute ischemic stroke. AJNR Am. J. Neuroradiol. 26, 1789–1797 (2005).
Powers, W. J. et al. 2018 Guidelines for the early management of patients with acute ischemic stroke: A guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 49, e46–e110. https://doi.org/10.1161/STROKEAHA.119.026917 (2018).
Tan, I. et al. CT angiography clot burden score and collateral score: correlation with clinical and radiologic outcomes in acute middle cerebral artery infarct. AJNR Am. J. Neuroradiol. 30, 525–531 (2009).
Brott, T. et al. Measurements of acute cerebral infarction: a clinical examination scale. Stroke 20, 864–870 (1989).
Wilson, J. L. et al. Improving the assessment of outcomes in stroke: use of a structured interview to assign grades on the modified Rankin Scale. Stroke 33, 2243–2246 (2002).
Vagenas, D. et al. Optimal image sample size for corneal nerve morphometry. Optom. Vis. Sci. 89, 812–817. https://doi.org/10.1097/OPX.0b013e31824ee8c9 (2012).
Al-Fahdawi, S. et al. A fully automated cell segmentation and morphometric parameter system for quantifying corneal endothelial cell morphology. Comput. Methods Programs Biomed. 160, 11–23 (2018).
Funding
Supported by Qatar National Research Fund Grant BMRP20038654. The funders had no role in study design, data collection and analysis, decision to publish, or publish, or preparation of the manuscript.
Author information
Authors and Affiliations
Contributions
Conceptualization: A.S., R.A.M. and A.K.; Methodology: A.S., R.A.M., S.K. and A.K.; Software: A.K. & Aj.M.; Validation: A.K., Aj.M.; Formal Analysis: A.K., Aj.M.; Investigation: A.K., Ah.M., G.P., I.N.P., H.G., N.A., A.M.N., F.W., B.B., P.G.B., H.A.H., M.R., P.W., M.Saq., M.San., S.K.; Resources: A.S. and N.A.; Data Curation: A.K., M.Saq.; Writing—Original Draft Preparation: A.K.; Writing Review & Editing: A.S. and R.A.M.; Visualization: M.Saq.; Supervision: A.S. and R.A.M.; Project Administration: A.S. and R.A.M.; Funding Acquisition: A.S. and R.A.M.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Khan, A., Menon, A., Akhtar, N. et al. Corneal nerve loss as a surrogate marker for poor pial collaterals in patients with acute ischemic stroke. Sci Rep 11, 19718 (2021). https://doi.org/10.1038/s41598-021-99131-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-021-99131-0
This article is cited by
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.