Abstract
Mammographic density (MD) of the breast and body mass index (BMI) are inversely associated with each other, but have inconsistent associations with respect to the risk of breast cancer. Skeletal muscle mass index (SMI) has been considered to reflect a relatively accurate fat and muscle percentage in the body. So, we evaluated the relation between SMI and MD. A cross-sectional study was performed in 143,456 women who underwent comprehensive examinations from 2012 to 2016. BMI was adjusted to analyze whether SMI is an independent factor predicting dense breast. After adjustment for confounding factors including BMI, the odds ratios for MD for the dense breasts was between the highest and lowest quartiles of SMI at 2.65 for premenopausal women and at 2.39 for postmenopausal women. SMI was a significant predictor for MD, which could be due to the similar growth mechanism of the skeletal muscle and breast parenchymal tissue. Further studies are needed to understand the causal link between muscularity, MD and breast cancer risk.
Similar content being viewed by others
Introduction
Mammographic density (MD) reflects the relative amount of connective and epithelial tissue (dense area) and fat tissue (non-dense area) in the breast1,2. It is known that the risk of breast cancer varies four to six times, based on the MD1. The difference in MD may reflect the effects of hormones and growth factors and might be related to the causal pathway of breast cancer3. Additionally, because cells at risk of turning malignant are mainly located in the fibro glandular tissue, the total amount of this tissue can also be considered as a risk factor for breast cancer4. Therefore, MD is a significant predictor for the risk of breast cancer, and factors influencing breast density might also contribute to the risk of breast cancer. However, the biological basis for determining MD is still unclear3.
There have been many studies on the factors related to breast density; however, different results have been reported due to heterogeneity and the small number of subjects examined and different statistical methods used for the analysis5,6,7,8,9,10,11,12,13,14. Increasing age and post-menopausal state with decreased estrogen levels is known to be a major determinant of MD15. Anthropometric factors, such as body mass index (BMI), waist–hip ratio, and waist circumference are also known to be related to MD5,6,7,8,9. In epidemiological studies, the most widely used index to evaluate body fat is BMI, which is calculated as the weight (kg) divided by height squared (m2). However, considering the inverse association between BMI and MD and the positive association between MD and breast cancer risk, the positive association between BMI and breast cancer risk remains unexplained in postmenopausal women16,17. The association between obesity and breast cancer risk in premenopausal women is not consistent across studies18,19. We supposed that the inconsistency could be because anthropometric factors used in previous studies are indicators of weight or mass including both muscle and fat, and these parameters do not reflect the respective amounts of each of muscle and adipose tissue.
We obtained the skeletal muscle mass index (SMI) using an equipment that measures the ratio of adipose tissue to muscle and evaluated the association between SMI and MD. Moreover, SMI indicates not only the proportion of skeletal muscle in the body, but are also considered better markers for assessing adiposity and its metabolic consequences compared to BMI. This is because SMI reflects a relatively accurate fat percentage in the body. Therefore, we analyzed whether the SMI can be a better predictor for MD, compared to the other anthropometric parameters used in previous studies. In addition, by attempting to adjust BMI in the analysis of the relationship between SMI and MD, it was intended to identify the cause of the paradoxical relationship between BMI and MD.
Methods
Study population
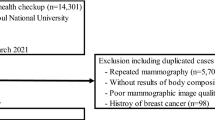
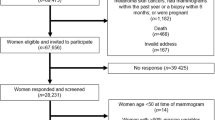
This study was a retrospective analysis of the data of 291,636 patients who underwent comprehensive annual or biennial examinations from 2012 to 2016 at the Samsung Healthcare Center in Seoul and Suwon, South Korea. Mammography was included as a part of the basic examination for all women over 30 years of age. The participants were employees of various companies, and were required to undergo an annual or biennial mandatory screening, which is required by the Industrial Safety and Health Law in Korea. The spouses of some male employees were also included due to the company’s welfare policies, and some women were self-registered. Of the data of 291,636 patients, if any participant underwent multiple examinations through several years (n = 145,898), the data at first year was used for analysis. We also excluded participants with missing anthropometric measures (n = 1387), and those with incomplete mammography (n = 895). Finally, a total of 143,456 women were included in the study. This study was approved by the Institutional Review Board of Kangbuk Samsung Hospital (KBSMC 2018-02-056), which waived the requirement for informed consent due to the use of deidentified data obtained as part of routine health screening exams, retrospectively. All methods were performed in accordance with relevant guidelines and regulations.
Measurement of breast density by mammography
Mammograms were performed using a full-field digital mammography system (Senograph 2000D/DMR/DS, General Electric Company, Milwaukee, WI, USA). MD was assessed from the craniocaudal and mediolateral oblique views of the each breast, using the breast imaging reporting and data system (BI-RADS) with 4 categories: almost entirely fat, scattered fibroglandular densities, heterogeneously dense, or extremely dense by several experienced radiologists20. We defined dense breast tissue as extremely dense, while non-dense breast as almost entirely fat, scattered fibroglandular densities, heterogeneously dense for dichotomous analysis.
Anthropometric measurements
Anthropometric measurements were obtained by the trained staff at the time of mammography. Height was measured to the nearest 0.1 cm using a stadiometer while the participant stood with heels together, arms to the side, legs straight, shoulders relaxed, and the head positioned so the gaze was straight ahead. Body weight was measured to the nearest 0.1 kg using a digital scale, with women in light clothing without shoes. Waist circumference (cm) was measured using a soft tape midway between the lowest rib margin and the iliac crest in a standing position. BMI was calculated as weight in kilograms divided by height in meters square.
The percentage of body skeletal muscle was estimated using a multifrequency bioelectrical impedance analyzer (BIA) with eight-point tactile electrodes (InBody 720, Biospace Co., Seoul, Korea). SMI was calculated as SMI (%) = skeletal muscle mass (kg)/body weight (kg) × 100, based on the methods used by Janssen et al.21.
Other measurements
Data about the history and health-related behaviors, family history, menstrual and reproductive history were collected through a self-administered questionnaire. Blood samples were taken from the antecubital vein by trained staff after the participant had fasted for at least 8 h, to measure the biochemical parameters. Calcium level adjusted to albumin was calculated as serum calcium + 0.8 × (4 − serum albumin).
Statistical analysis
Statistical analyses were performed using the STATA version 13.0 (StataCorp LP, College Station, TX, USA) and R version 4.0.3 with packages for relative weights (RW) analysis and scatter22,23,24. Chi-square test for categorical data and t test for continuous variables were used to compare the baseline characteristics between the groups. The associations of variables with breast density were evaluated using RW, which is a way quantify the relative importance of correlated variables in regression analysis and it could produce clear results even if the predictors have very high collinearity23,25. Pearson correlations and scatter plots were used for understanding the relationship between anthropometric factors, age and SMI24. Logistic regression analyses were conducted to investigate the impact on MD of anthropometric factors by estimating odds ratios (ORs) with 95% confidence internals (CIs). We adjusted for parameters like age, parity, age at menarche, history of estrogen replacement therapy, and calcium level adjusted to albumin. In addition, we adjusted for BMI to evaluate whether SMI was an independent factor for a dense breast. All reported p values are two tailed, and comparisons where p < 0.05 were considered statistically significant.
Results
Patient characteristics
Among the 143,456 participants, there were 115,013 premenopausal women (80.2%) and 28,443 postmenopausal women (19.8%). Table 1 shows the baseline characteristics of the study participants. The prevalence of dense breasts in premenopausal women was higher than that in the postmenopausal women. Dense breasts were positively associated with height, SMI, and estradiol level, and negatively associated with age, weight, BMI, waist circumference, vitamin D level, CA15-3, FSH, parity, and history of breast cancer in the premenopausal women. In postmenopausal women, dense breasts were positively associated with height, amount of alcohol consumption, SMI, estradiol level, and history of estrogen replacement therapy, while it was negatively associated with age, weight, BMI, age at menarche, waist circumference, vitamin D level, FSH, and parity. Regardless of the menopausal status, the factors that had large proportions in dense breast were similar.
Association between anthropometric factors, age and SMI
Pearson correlations and scatter plots between anthropometric factors, age and SMI are presented in Fig. 1. As expected, weight, BMI and waist circumference are strongly related to each other (r = 0.88–0.89), and All of them showed a negative correlation with SMI (r = − 0.73 to − 0.57). In correlation with age, height showed the strongest correlation (r = − 0.4) and weight showed the weakest correlation (r = 0.09), and BMI (r = 0.29), waist circumference (r = 0.32), and SMI (r = − 0.29) showed similar degrees of correlation.
Logistic regression analysis for known risk factors for dense breasts and anthropometric factors
To examine the effect of each factor on MD, we performed a logistic regression analysis of the known risk factors for dense breasts from previous studies and RW analysis. Younger age, nulliparity and low calcium level after adjustment to albumin were significantly associated with dense breasts, regardless menopausal state. Age at menarche, history of estrogen replacement therapy had different effects on dense breasts according to menopausal state (Table 2). RW analysis was used to compare the relative importance of each variable in predicting dense breast (Fig. 2). Among all variables, SMI has the highest RW (RW = 23.62), other anthropometric factors showed relatively high RW values (Waist circumference = 16.55; BMI = 15.78). Age and menopausal state also showed high RW values of 22.74 and 15.02, respectively. Other factors that were known to be related to density had relatively low RW values (Parity = 3.60; Age at menarche = 1.26; Calcium level adjusted to albumin = 1.14; History of estrogen replacement therapy = 0.16; Past history of breast cancer = 0.10; Ovary cancer of family member = 0.02; Breast cancer of family member = 0.01).
Table 3 illustrates the associations between dense breast and anthropometric factors according to menopausal status. Increasing age is well known to be associated with decreasing MD. We therefore corrected age in the analysis of anthropometric factors. Weight, BMI, SMI and waist circumference were statistically significant associated with MD, whereas height was not. These associations remained significant after further adjustment for age at menarche, parity, use of estrogen replacement therapy, and calcium level adjusted to albumin. In both pre and postmenopausal women, weight, BMI, and waist circumference were inversely associated with dense breasts, whereas SMI was positively associated with dense breasts.
Associations between breast density and SMI after stratification or adjustment by BMI
To investigate whether SMI was related to MD independent of BMI, we analyzed the association of MD with SMI after further adjustment for BMI. It was seen that SMI was still a statistically significant factor associated with MD. Premenopausal women in the highest quartile of SMI were 2.65 times more likely to have dense breast tissues than those in the lowest quartile (95% CI 2.52–2.79), while postmenopausal women in the highest quartile of SMI were 2.39 times more likely to have dense breast tissues than those in the lowest quartile (95% CI 2.02–2.82) (Table 4).
Discussion
To our knowledge, this is the first study about the association between skeletal muscularity and MD, and we demonstrated that SMI was the most important predictor among the known predictors of MD by using RW analysis. SMI was also an independent predictor of dense breasts after adjustment for known factors associated with MD, including age and BMI. These results suggest that SMI is a measure to overcome the inconsistency in BMI observed in previous MD-related studies; this could be explained by the strong relationship between skeletal muscularity and breast parenchymal tissue.
In infancy, childhood, puberty, and adulthood, the development of body is affected by a variety of hormones. Among them, gonadal sex steroids, growth hormone and insulin-like growth factor-1 are known to play a major role in development of mammary gland as well as skeletal muscle25. Additionally, the role of epidermal growth factor family of growth factors is known in the development of epithelial tissues, particularly the mammary gland and the gastrointestinal tract, and their role in skeletal tissue growth was also reported26. Thus, based on this growth mechanism, the relationship between SMI and breast parenchymal tissue is highly relevant, and might explain the relationship with MD.
There are many studies on the relationship between MD and adiposity. Easily measurable but potentially inaccurate estimates of adiposity such as weight, BMI, waist circumference, weight gain have proven to be relevant to MD5,6,7,8,9. In our study, as in previous studies, factors representing adiposity, such as BMI, weight, and waist circumference were found to be significantly associated with MD in both pre and postmenopausal women. However, these measurements cannot distinguish between muscle and adipose tissue; hence, it may have a limitation for use as a marker to represent adipose tissue.
Attempts have been made to measure adiposity or muscularity accurately using imaging methods, such as whole-body dual x-ray absorptiometry (DXA) or abdominal computed tomography (CT) scans6,10,11. These studies that suggest that body or abdominal fat assessed by DXA or abdominal CT might have an association with the percentage of dense area in breast, independent of BMI. The eight-polar BIA used in our study was reported to be superior to the DXA or body weight used in other studies, for the accuracy of fat mass and muscle mass measurements27,28. The SMI measured by BIA indicates the ratio of the skeletal muscle and adipose tissue in the body. The significant association between MD and SMI independent of BMI in our study might further strengthen the results of previous studies, and the SMI measured by BIA could be better indicator of predicting MD.
Based on previous studies, although adiposity seems to be highly related to MD and breast cancer, it is still difficult to understand the biological pathway and has different effect according to menopause state. In early-adulthood, estrogen synthesis in subcutaneous fat accounts for only about 5% of the total, but when the fat mass is excessive, negative feedback is received in the hypothalamic-pituitary-axis29. This irregularity of the menstrual cycle induces a decrease in ovarian function, resulting in a decrease of estrogen synthesis. Low level of the sex hormone is associated with inhibition of the growth of the fibroglandular tissue of the breast, resulting in a low MD and a reduced risk of breast cance19. However, in late-adulthood, the increase in adiposity due to weight gain increases only the breast fat tissue (non-dense area) without an increase in the fibroglandular tissue (dense area), resulting in a low MD. Although results vary based on the hormones used or the molecular subtype, it is known that obesity in postmenopausal women increases the risk of breast cancer, which is in contrast to the results in premenopausal women30,31. It could be because an increase in fat mass caused a higher level of estrogen, induced by aromatization of androstenedione32.
Increasing age is strongly associated with declines in MD, which occurs in both pre- and post-menopausal women, regardless of race15. Reproductive hormones that decrease with aging affect MD, which is prominent in the premenopausal period15,33. In particular, the hormonal changes that occur during the menopausal transition are reflected in the drastic decline in MD15,34. In our study, age showed the highest RW value except for SMI, confirming the strong correlation between age and MD. Therefore, in order to more clearly identify the association between SMI and MD, we adjusted for age in analyses.
We also conducted a verification of factors that have been previously associated with MD. Alcohol consumption has been known to be associated with an increased breast cancer and MD in most studies12,13,35,36. In our study, postmenopausal women with dense breasts consumed larger amount of alcohol than those with non-dense breasts, while premenopausal women did not. Vitamin D is known to inhibit estrogen synthesis and its receptor function, and inhibit breast epithelial and stromal proliferation, suggesting an inverse relationship with breast cancer and MD14,37,38. Based on this theory, several studies have examined the association between MD and vitamin D, but the meta-analysis did not yield significant results14. In our study, vitamin D levels were low in women with high MD regardless of the menopausal status. Considering that our study was based on the data from vitamin D measurements of 97,072 participants, which was much larger than the data in a previous meta-analysis (n = 5863), this result could be significant. For a clear conclusion, a further study with correction of the confounding factors might be needed.
The limitation of this study is that quantitative measurements were not used for the measurement of MD. Quantitative measurements are expressed as continuous variables, which might provide more accurate statistical results than the classification based on the BI-RADS method that we used. Second, all participants were Koreans, and they have more dense breasts than other races. Therefore, the results cannot be extrapolated to the general population.
We found a positive correlation between the muscularity and breast density. SMI was independent and strong predictor of dense breast. Considering our results and growth mechanism, the proportion of muscularity in the body are likely to be correlated with the proportion of parenchyma in the breast. It offers the possibility to explain the reason for the paradoxical relationship between BMI, MD and breast cancer risk, and for disagreement between previous studies. Further studies are needed to understand the causal link between muscularity, MD and breast cancer risk.
Data availability
The datasets generated and analyzed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- BIA:
-
Bioelectrical impedance analyzer
- BI-RADS:
-
Breast imaging reporting and data system
- BMI:
-
Body mass index
- CT:
-
Computed tomography
- DXA:
-
Dual x-ray absorptiometry
- MD:
-
Mammographic density
- OR:
-
Odds ratio
- SMI:
-
Skeletal muscle mass index
- RW:
-
Relative weight
References
Boyd, N. F., Lockwood, G. A., Byng, J. W., Tritchler, D. L. & Yaffe, M. J. Mammographic densities and breast cancer risk. Cancer Epidemiol. Biomark. Prev. 7, 1133–1144 (1998).
Boyd, N. F. et al. Mammographic breast density as an intermediate phenotype for breast cancer. Lancet Oncol. 6, 798–808 (2005).
Huo, C. W. et al. High mammographic density is associated with an increase in stromal collagen and immune cells within the mammary epithelium. Breast Cancer Res. 17, 79 (2015).
Trichopoulos, D., Lagiou, P. & Adami, H. O. Towards an integrated model for breast cancer etiology: The crucial role of the number of mammary tissue-specific stem cells. Breast Cancer Res. 7, 13–17 (2005).
Pollán, M. et al. Adult weight gain, fat distribution and mammographic density in Spanish pre- and post-menopausal women (DDM-Spain). Breast Cancer Res. Treat. 134, 823–838 (2012).
Woolcott, C. G. et al. Associations of overall and abdominal adiposity with area and volumetric mammographic measures among postmenopausal women. Int. J. Cancer 129, 440–448 (2011).
Boyd, N. F. et al. The relationship of anthropometric measures to radiological features of the breast in premenopausal women. Br. J. Cancer 78, 1233–1238 (1998).
Tseng, M. & Byrne, C. Adiposity, adult weight gain and mammographic breast density in US Chinese women. Int. J. Cancer 128, 418–425 (2011).
Soguel, L. & Diorio, C. Anthropometric factors, adult weight gain, and mammographic features. Cancer Causes Control 27, 333–340 (2016).
Dorgan, J. F. et al. Height, adiposity and body fat distribution and breast density in young women. Breast Cancer Res. 14, R107 (2012).
Caire-Juvera, G., Arendell, L. A., Maskarinec, G., Thomson, C. A. & Chen, Z. Associations between mammographic density and body composition in Hispanic and non-Hispanic white women by menopause status. Menopause 15, 319–325 (2008).
Flom, J. D., Ferris, J. S., Tehranifar, P. & Terry, M. B. Alcohol intake over the life course and mammographic density. Breast Cancer Res. Treat. 117, 643–651 (2009).
Quandt, Z. et al. The association of alcohol consumption with mammographic density in a multiethnic urban population. BMC Cancer 15, 1094 (2015).
Yaghjyan, L., Colditz, G. A. & Drake, B. Vitamin D and mammographic breast density: A systematic review. Cancer Causes Control 23, 1–13 (2012).
Burton, A. et al. Mammographic density and ageing: A collaborative pooled analysis of cross-sectional data from 22 countries worldwide. PLoS Med. 14, e1002335 (2017).
Neuhouser, M. L. et al. Overweight, obesity, and postmenopausal invasive breast cancer risk: A secondary analysis of the women’s health initiative randomized clinical trials. JAMA Oncol. 1, 611–621 (2015).
Liu, K. et al. Association between body mass index and breast cancer risk: Evidence based on a dose–response meta-analysis. Cancer Manag. Res. 10, 143–151 (2018).
Laudisio, D., Muscogiuri, G., Barrea, L., Savastano, S. & Colao, A. Obesity and breast cancer in premenopausal women: Current evidence and future perspectives. Eur. J. Obstet. Gynecol. Reprod. Biol. 230, 217–221 (2018).
Schoemaker, M. J. et al. Association of body mass index and age with subsequent breast cancer risk in premenopausal women. JAMA Oncol. 4, e181771 (2018).
American College of Radiology. Breast Imaging Reporting and Data System (BI-RADS) (American College of Radiology, 1998).
Janssen, I., Heymsfield, S. B. & Ross, R. Low relative skeletal muscle mass (sarcopenia) in older persons is associated with functional impairment and physical disability. J. Am. Geriatr. Soc. 50, 889–896 (2002).
R Core Team. R: A language and environment for statistical computing. R Foundation for Statistical Computing https://www.R-project.org (2016).
Moon K. R statistics and graphs for medical papers (Hannarae, 2015).
Revelle, W. P. Procedures for psychological, psychometric, and personality research https://CRAN.R-project.org/package=psych (2021).
Veldhuis, J. D. et al. Endocrine control of body composition in infancy, childhood, and puberty. Endocr. Rev. 26, 114–146 (2005).
Xian, C. J. Roles of epidermal growth factor family in the regulation of postnatal somatic growth. Endocr. Rev. 28, 284–296 (2007).
Malavolti, M. et al. Cross-calibration of eight-polar bioelectrical impedance analysis versus dual-energy X-ray absorptiometry for the assessment of total and appendicular body composition in healthy subjects aged 21–82 years. Ann. Hum. Biol. 30, 380–391 (2003).
Tagliabue, A. et al. Appendicular lean body mass. Prediction by bioelectrical impedance analysis. Ann. N. Y. Acad. Sci. 904, 218–220 (2000).
Dowsett, M. & Folkerd, E. Reduced progesterone levels explain the reduced risk of breast cancer in obese premenopausal women: A new hypothesis. Breast Cancer Res. Treat. 149, 1–4 (2015).
Munsell, M. F., Sprague, B. L., Berry, D. A., Chisholm, G. & Trentham-Dietz, A. Body mass index and breast cancer risk according to postmenopausal estrogen–progestin use and hormone receptor status. Epidemiol. Rev. 36, 114–136 (2014).
Huang, Z. et al. Dual effects of weight and weight gain on breast cancer risk. JAMA 278, 1407–1411 (1997).
Hankinson, S. E. et al. Alcohol, height, and adiposity in relation to estrogen and prolactin levels in postmenopausal women. J. Natl. Cancer Inst. 87, 1297–1302 (1995).
Walker, K. et al. Premenopausal mammographic density in relation to cyclic variations in endogenous sex hormone levels, prolactin, and insulin-like growth factors. Cancer Res. 69, 6490–6499 (2009).
Burger, H. G., Hale, G. E., Dennerstein, L. & Robertson, D. M. Cycle and hormone changes during perimenopause: The key role of ovarian function. Menopause 15, 603–612 (2008).
Centers for Disease Control and Prevention (CDC). Prevalence of coronary heart disease—United States, 2006–2010. MMWR Morb. Mortal. Wkly. Rep. 60, 1377–1381 (2011).
Allen, N. E. et al. Moderate alcohol intake and cancer incidence in women. J. Natl. Cancer Inst. 101, 296–305 (2009).
Banerjee, P. & Chatterjee, M. Antiproliferative role of vitamin D and its analogs—A brief overview. Mol. Cell. Biochem. 253, 247–254 (2003).
Krishnan, A. V., Swami, S. & Feldman, D. Vitamin D and breast cancer: Inhibition of estrogen synthesis and signaling. J. Steroid Biochem. Mol. Biol. 121, 343–348 (2010).
Author information
Authors and Affiliations
Contributions
Chae, YL Park and Yun collected and interpreted the patient data. Lee was a major contributor in writing the manuscript. CH Park inspired the topic selection and led the authors. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Lee, K.H., Chae, S.W., Yun, J.S. et al. Association between skeletal muscle mass and mammographic breast density. Sci Rep 11, 16785 (2021). https://doi.org/10.1038/s41598-021-96390-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-021-96390-9
This article is cited by
-
Association of body composition fat parameters and breast density in mammography by menopausal status
Scientific Reports (2022)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.