Abstract
The incidence of kidney stones is increasing in the US population. Oxalate, a major factor for stone formation, is degraded by gut bacteria reducing its intestinal absorption. Intestinal O. formigenes colonization has been associated with a lower risk for recurrent kidney stones in humans. In the current study, we used a clinical trial of the eradication of Helicobacter pylori to assess the effects of an antibiotic course on O. formigenes colonization, urine electrolytes, and the composition of the intestinal microbiome. Of 69 healthy adult subjects recruited, 19 received antibiotics for H. pylori eradication, while 46 were followed as controls. Serial fecal samples were examined for O. formigenes presence and microbiota characteristics. Urine, collected serially fasting and following a standard meal, was tested for oxalate and electrolyte concentrations. O. formigenes prevalence was 50%. Colonization was significantly and persistently suppressed in antibiotic-exposed subjects but remained stable in controls. Urinary pH increased after antibiotics, but urinary oxalate did not differ between the control and treatment groups. In subjects not on antibiotics, the O. formigenes-positive samples had higher alpha-diversity and significantly differed in Beta-diversity from the O. formigenes-negative samples. Specific taxa varied in abundance in relation to urinary oxalate levels. These studies identified significant antibiotic effects on O. formigenes colonization and urinary electrolytes and showed that overall microbiome structure differed in subjects according to O. formigenes presence. Identifying a consortium of bacterial taxa associated with urinary oxalate may provide clues for the primary prevention of kidney stones in healthy adults.
Similar content being viewed by others
Nephrolithiasis (kidney stones) affect up to 9 percent of the US population1, affecting both males and females, with incidence increasing in children and adults2,3. Most stones are composed of calcium oxalate (CaOx)4,5. Oxalate is absorbed in the gut from the diet and also produced endogenously as an end-product of amino acid metabolism6,7. Human intestinal bacteria that degrade oxalate and contribute to its metabolism are considered the oxalobiome8. Increasing evidence suggests gut microbiota roles in nephrolithiasis pathogenesis9,10,11.
Prior antibiotic use has been associated with kidney stone development months or even years later12,13. Although multiple bacterial taxa are able to degrade oxalate in the gut8,14, Oxalobacter formigenes is the only commensal known to use oxalate as its sole energy and carbon source and may be the only specialist oxalate degrader in humans15. The role in overall oxalate metabolism of other high abundance microbiota that have the capability to degrade oxalate but not use it as their primary energy source remains unknown. In our recent work, we showed that in healthy subjects, O. formigenes is the major reservoir of oxalate metabolizing genes at the transcriptional level, greater than all other organisms combined16. In rodent models, colonic colonization with O. formigenes significantly reduced urinary oxalate excretion17,18,19. Intestinal O. formigenes colonization has been associated with lower risk for recurrent kidney stones in humans20.
Epidemiologic studies provide evidence that O. formigenes prevalence in developed countries such as the USA is lower than in developing countries21,22. The prevalence of O. formigenes colonization is very high (> 80%) in uncontacted Amerindians21, and the hunter-gatherer Hadza people22, and was estimated at 60% in India23. Prevalence has been found to be ~ 30% in US and UK populations24. O. formigenes is susceptible to commonly used antibiotics25; an antibiotic course for H. pylori eradication led to loss of colonization for at least six months post-treatment26, but post-treatment examination of urinary analytes and microbiome were not done.
In the current study, we used a study (ESSAY) of the eradication of Helicobacter pylori to assess the effect of an antibiotic course on O. formigenes colonization and on urine electrolytes, including oxalate excretion (Fig. 1A). We also asked whether microbiome structure and composition differed over time with respect to both O. formigenes status and antibiotic exposure.
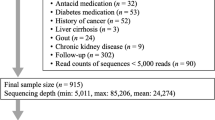
Study design and enrollment. Panel (A) Study design and assessments. From all enrolled subjects, baseline samples (stool and urine) were obtained at time 0. H. pylori-positive subjects received antibiotics for 2 weeks while H. pylori-negative subjects were followed as controls. Follow-up collections were performed at weeks 6, 12, and 24. Urine was collected after fasting (Pre-meal), and for 3 h following a standard meal (Post-meal). Stool samples were tested for O. formigenes using PCR and qPCR and underwent 16S rRNA gene sequencing. Urine was tested for multiple analytes. Panel created by BioRender software (www.biorender.com. Panel (B) Enrollment. Of 139 subjects screened for participation, 87 completed the screening, and 69 subjects underwent baseline assessment. 19 H.pylori-positive subjects were treated with antibiotics ,whereas 46 H.pylori-negative subjects served as controls. Panel created by Lucidchart software (www.lucidchart.com).
Results
Recruitment
Of 69 eligible participants who returned for the baseline visit, 23 (33%) tested positive for H. pylori while 46 tested negative; 65 of the 69 participants also provided fecal samples at the baseline visit. H. pylori-positive participants (n = 19) who consented to the antibiotic treatment received antibiotics based on the standard-of-care. Subjects were given treatment with twice daily amoxicillin (1000 mg) and clarithromycin (500 mg) for 2 weeks. For the two subjects with penicillin allergy, amoxicillin was replaced by metronidazole 500 mg three times daily. Of those, 17 completed the final study visit at 6 months. Four subjects who underwent a baseline assessment and tested positive for H.pylori withdrew from the study before receiving any antibiotics (Fig. 1B).
O. formigenes colonization status and stability over time
Since there is no consensus on the best method to detect O. formigenes in stool samples, we developed a positivity score based on PCR, qPCR and 16S rRNA gene sequencing data at multiple time points to accurately represent O. formigenes positivity in the stool samples of the study subjects. Based on the O. formigenes positivity score, the prevalence of O. formigenes was 50% in the 64 participants at baseline (Figs. 1, 2), similar to prior findings in the USA20,22,24,27. The O. formigenes-positive and negative participants were similar in distributions of age, sex, ethnicity, BMI, mode of birth-delivery, H. pylori status, and place of birth (Table S2). We evaluated O. formigenes colonization status stability over time in both the antibiotic-treated participants and controls. Among the controls, of the 21 O. formigenes-positive subjects at baseline assessed at 6 weeks, 19 (90%) remained positive, vs. 0/20 formigenes-negative participants at baseline becoming positive (p < 0.001, by Fisher’s exact). In contrast, in the antibiotic-treated group, of the eight initially O. formigenes-positive participants, only two (25%) remained positive at 6 weeks vs. 19 (95%) of the 20 who were untreated (p < 0.001, Fisher’s exact test). Only three (37.5%) of the treated subjects remained positive at 24 weeks vs. 20 (83.3%) of 24 in the untreated controls (p < 0.02, Fisher’s exact test). All 11 of the baseline O. formigenes-negative group remained negative (Fig. 2 A, B). Thus, treatment to eradicate H. pylori had a strong effect, largely eliminating O. formigenes, confirming prior studies 26.
O. formigenes colonization status in 45 control subjects and 19 antibiotic-treated subjects over the study period. O. formigenes-positive samples are shown in blue, negative in red, and missing in white. Panel (A) Untreated control subjects. Panel (B) Antibiotic-treated subjects. Figure created by Excel software version 16.44.
O. formigenes detection by high throughput 16S rRNA gene sequencing
Our prior studies showed that O. formigenes abundance can vary in carriers over a range > 3-log10, with some individuals having minimally detectable numbers24,28, which intrinsically limits interpreting positivity.
Using 16S rRNA gene sequencing, we detected O. formigenes in 10 (22%) of the 45 controls at baseline, vs. 24(53%) using the above O. formigenes scoring system. At follow-up, we detected O. formigenes in six other controls by 16S rRNA gene sequencing analysis, but positivity fluctuated for individual subjects (Fig. 3). However, across all the control subjects, the mean % relative abundance was stable over time (0.06 ± 0.0 at baseline and 0.03 ± 0.04 at week 24). At baseline in the antibiotic-treated group, O. formigenes was detected in 4 (21.1%) of 19 participants; after antibiotic treatment, all of these subjects remained O. formigenes negative at 6, 12 and 24 weeks. Two subjects who had undetectable O. formigenes according to the initial16S analysis (but who were positive for O. formigenes by the combined scoring method) had detectable O. formigenes 16S rRNA gene amplification after antibiotic treatment.
Alpha- and beta-diversity of microbiota in 173 fecal samples. from 64 study subjects, according to baseline O. formigenes status. Panel (A) Alpha-diversity measurements. Chao1, phylogenetic diversity, observed OTUs, and Shannon diversity according to Oxf status at baseline. Panel (B) Analysis of Beta-diversity, Unweighted UniFrac distances, according to O. formigenes status. *p < 0.05. Figure created by R software Ggplot2 package.
Urinary parameters according to antibiotic treatment
To assess the differences in urinary electrolytes before and after H. pylori eradication in antibiotic-treated participants and the stability of these electrolytes in untreated controls, we collected a fasting urine sample (pre-meal urine) and then administered a standard 16-oz liquid meal totaling 700 cal (2 cans of Ensure Plus) (Table S1) and collected urine for three hours after the meal (post-meal urine) (Fig. 1A). We used a linear mixed model fitted to the data over the time interval 0–24 weeks in which the changing rates in urine parameters were compared based on baseline treatment status (control, treatment group). In both the controls and the treatment group, pre-meal UOx/Cr increased over the course of the study (p < 0.05), with comparable increases for the two groups. In contrast, post-meal UOx/Cr did not change over time (Table S3, Supplementary Fig. 2). Urine pH levels were unchanged in the untreated controls, as expected, but increased in the treated patients in both the pre- and post-meal comparisons (p = 0.04 and 0.06, respectively). Urine ammonia/Cr differed in their direction of change in controls and treated subjects in pre-meal samples but after the meal increased in both control and antibiotic-treated participants. Urine citrate/Cr was stable over time in pre-meal samples from controls and in post-meal samples from both controls and treated subjects but significantly increased in the treatment group. The ratio to creatinine of urinary sodium, phosphorus, calcium, and urea nitrogen increased pre-meal in both the control and antibiotic-treated subjects, but were unchanged in post-meal comparisons over time (Table S3). These results indicate the effects of antibiotic exposures on urinary electrolyte excretion, pertaining particularly to acid–base homeostasis.
Microbial community structure
Alpha-diversity is used to measure the bacterial diversity within a sample, whereas Beta-diversity provides a measure of the dissimilarity between samples. First, we asked whether the microbiome differed in the study subjects according to O. formigenes status in control subjects or baseline assessments (before antibiotics) in the antibiotic treatment group. Fecal samples from the O. formigenes-positive subjects had higher α-diversity (p < 0.01, by Wilcoxon Rank test) than those from O. formigenes-negative subjects (Fig. 3A). After including subject as random effect in a linear mixed-effect model, we found similarly that O. formigenes is associated with higher α-diversity measurements (p < 0.01). As expected, in the untreated controls, α-diversity remained stable, but after antibiotic treatment, decreased at 6 weeks and later returned to baseline (Fig. 4A). To assess the communities for β-diversity, we examined unweighted UniFrac distances, consistent with our previous analysis of the American Gut Project data24, in 173 samples from 64 participants according to O. formigenes baseline-status; β-diversity significantly differed (p = 0.029 by Adonis test with 999 permutations) in the samples based on O. formigenes status (Fig. 3B). Similar to α-diversity, β-diversity was stable over time in untreated controls, but changed (p = 0.06, by pairwise Permanova testing with 999 permutation) immediately following antibiotic exposure, then returning to baseline (Fig. 4B, C). These studies provide evidence that O. formigenes status correlates with and clinical antibiotic regimen affects overall microbiome community characteristics.
Alpha- and beta-diversity of microbiota in controls and antibiotic-treated subjects over time. Panel (A) Phylogenetic diversity over time in the two groups of subjects; Kruskal Wallace analysis. Panel (B) Unweighted UniFrac distances over time. Panel (C) Comparison of beta diversity between baseline and follow-up specimens in the control and antibiotic treatment groups. Box-and-whisker plots (Tukey) of unweighted UniFrac distance are shown at sequencing depth of 8,000. Comparisons were done between baseline (0) vs. follow up (W6, 3M, 6M), by Pairwise Permanova testing with 999 permutation; no differences were significant at p < 0.05. Panels (A,B) are created by QIIME2 software (version 2-2019.1) while Panel (C) was created by R software Ggplot2 package.
Association between UOx/Cr and specific bacterial taxa
To assess whether any taxa other than O. formigenes were positively or negatively associated with UOx/Cr, we first analyzed the controls (41 participants with 108 measurements at four time points), using a centered log-ratio (CLR) transformation to standardize relative abundances of individual microbial taxa before fitting to a linear mixed model (Table 1). The analyses showed that relative abundance of the phylum Proteobacteria was positively (Adj. p < 0.01) associated with urinary oxalate levels. Genus Dysgonomonas (Adj. p = 0.02) and species D. gadei (Adj. p < 0.01) were inversely associated with post-meal urinary oxalate level, adjusted for age, gender, ethnicity, BMI, and calcium level. Based on our model, in the antibiotic-treated subjects (Table 2), the clr transformed relative abundance of genera Dysgonomonas (Adj. p = 0.02), Epulopiscium (Adj. p = 0.02), and Providencia (Adj. p = 0.02) and species Bacteroides plebeius (Adj. p = 0.03) were inversely associated with pre-meal urinary oxalate level, whereas genus Lachnobacterium (Adj. p = 0.02) and species Faecalitalea cylindroides (Adj. p = 0 < 0.01) were positively associated. Family Barnesiellaceae (Adj. p = 0.01) and species Streptococcus gordonii (Adj. p = 0.05) were negatively associated with post-meal urinary oxalate levels, whereas order Turicibacterales (Adj. p = 0.01) and family Turicibacteraceae (Adj. p = 0.01) were positively associated. In our models, family Oxalobacteraceae was not associated with pre- and post urinary oxalate in both controls and antibiotic-treated subjects.
Discussion
In this study, we confirmed that antibiotic treatment has a strong effect on O. formigenes status26,29. Although most antibiotic-treated participants had durable suppression, lasting > 24 weeks, O. formigenes persisted in some, suggesting either heterogeneity in antibiotic resistance of O. formigenes strains or inability of the active agent(s) to achieve sufficient colonic concentrations. Since O. formigenes colonization has been associated with lower oxaluria30, our observation of treatment effects provides one explanation for why antibiotic treatments have been associated with a higher kidney stone incidence12,31.
This study highlights the difficulty in assessing patients’ O. formigenes status due to the wide range in colonization density that may reflect both diet and competing organisms. This variation confirms our prior work24,28, which provided the rationale for using a formula based on multiple tests to detect colonization. We therefore developed a positivity score based on PCR, qPCR and 16S rRNA gene sequencing data at multiple time points to more accurately represent O. formigenes positivity in our stool samples. This biological variation is likely also in part responsible for the continued uncertainty about whether O. formigenes status is associated with nephrolithiasis or not. Our results may more accurately represent colonization of individual subjects than previously since prior studies used a single assessment types done cross-sectionally, which can underestimate colonization prevalence. Giving subjects an oxalate-rich diet that selects for O. formigenes growth may enhance detection in future cross-sectional analyses. Finding that 16S rRNA gene sequencing has low sensitivity for O. formigenes detection, due to its often low abundance, may be useful in future studies where colonization needs to be confirmed using more sensitive methods.
The standard meal used in this study did not contain a substantial oxalate load because the original trial was not designed to measure our primary outcome. Therefore, urinary oxalate changes might not reach those observed with moderate-high oxalate diets that healthy individuals typically consume. Differences in UOx/Cr (indicated by the standard deviations in Supplementary Fig. 2) emphasize the need for larger trials with high oxalate, low calcium, and controlled diets. However, urinary pH increased after antibiotic treatment but not in controls, indicating possible effects beyond oxalate metabolism affecting acid–base homeostasis. The recent associations between increased stone risk and antibiotic courses did not include urinary chemistry data in one report12, and in the second, the temporal relationship between antibiotic use and urine collection was not standardized13. Our findings provide potential mechanisms for the linkage between prior antibiotic use and nephrolithiasis risk. Higher urinary pH is associated with increased risk for calcium phosphate stones32.
Our community structure findings indicate that O. formigenes presence is a marker for a richer microbiome (consistent with prior studies21,24) and its loss is a marker of important antibiotic-induced microbiome alterations. That no significant recolonization was detected by 6 months, while the overall diversity recovered, is consistent with persistent microbiome disturbance.
We identified a group of bacteria positively or negatively correlated with urinary oxalate level, consistent with the hypothesis that oxalate degradation in the gut is affected by the putative oxalobiome that facilitates oxalate degradation8. This study provides the first analysis of such associations in healthy subjects to potentially identify a microbiome associated with differential potential for stone formation. Since our findings indicate taxa with abundance associated with lower urinary oxalate levels, these could be protective against hyperoxaluria; species from genus Providencia are known to be oxalate-degraders33. Similarly, we identified bacteria associated with higher urinary oxalate levels whose presence could potentially increase kidney stone risk9. Proteobacteria were associated with higher urine oxalate in our study and were enriched in stone formers in two other studies9,11.
The lack of an association of O. formigenes colonization with lower urinary oxalate excretion could reflect its very low abundance in subjects without dietary oxalate enrichment and insensitive detection using 16S rRNA gene sequencing. Future studies with deeper coverage will facilitate identifying low-abundance bacterial taxa.
Our study was limited by the small sample size for the antibiotic-treated participants and lack of information about baseline diets. The standard meal did not contain oxalate, and the 3-h post-meal urine collection did not permit study of less acute colonic bacterial actions on dietary components.
In conclusion, our study found substantial antibiotic effects on O. formigenes colonization, its relationship with other taxa and overall microbiome community structure, and with several urinary parameters, and identified a consortium of bacterial taxa associated with urinary oxalate levels. In the future, understanding metabolic activities of the intestinal taxa may be useful for primary kidney stone prevention.
Materials and methods
Recruitment and subject enrollment
Participants were recruited for the ESSAY study (Eradication Study in Stable Adults/Youths) evaluating the effect of the standard-of-care practice of H. pylori eradication on metabolic profile and anthropometric measures of healthy adults. Participants were identified from the Bellevue Hospital primary care clinic, and community. Healthy young adults who were 18–40 years old were screened by research coordinators for eligibility criteria and then signed an informed consent if meeting those criteria (Fig. 1B). In total, 139 participants were screened for participation. Of the 87 participants who met the eligibility requirements and provided informed consent, 69 completed the baseline visit while 18 were lost to follow-up (Fig. 1B). The clinical study was conducted between April 2012 and July 2016. We excluded participants with diabetes, hyper- or hypothyroidism, prior gastric or bariatric surgery, prior H. pylori treatment, steroid or other immunomodulatory drug use within 4 weeks of the first visit, and antibiotic use within the prior 6 months. Participants completed baseline questionnaires to provide their demographic information, medical history, and current medication use. The study was approved by the Institutional Review Board (IRB) at NYU Langone Health. All research was performed in accordance with the Declaration of Helsinki and our local IRB guidelines. Informed consent was obtained from all participants.
Determination of H. pylori status at baseline and at follow-up and antibiotics regimen
Subjects underwent a non-radioactive 13C Urea Breath Test (Meretek Diagnostics, New York NY) to determine H.pylori status. Subjects (n = 23) who tested H. pylori-positive were offered treatment with a 14-day twice-daily regimen [amoxicillin 1000 mg, clarithromycin 500 mg, and proton pump inhibitor (PPI; omeprazole 20 mg, rabeprazole or esomeprazole 40 mg)], per the then-current standard of care34. In total, 19 subjects received a course of antibiotics, including three who received a second antibiotic course because they failed eradication with the first course, and four other subjects withdrew from the study before receiving antibiotics (Fig. 1). The 46 subjects who were H.pylori negative at baseline did not receive antibiotics and were followed serially as controls.
Study time points and assessments
Subjects fasted overnight at home and then underwent basic assessment at the NYU Clinical and Translational Science Institute (CTSI) at Bellevue Hospital at the baseline and 6, 12, and 24-week timepoints and height and weight obtained. Stool samples were collected and placed immediately on ice at home and brought to the center within 24 h, then immediately frozen at − 80° C. No preservatives were used and the kits were prepared in-house. In total, we obtained fecal samples from 65 subjects at baseline (Fig. 1).
Test meal and urine collections
To assess the differences in urinary electrolytes before and after H. pylori eradication, we collected a fasting urine sample and then administered a standard 16-oz liquid meal totaling 700 cal (2 cans of Ensure Plus) (Table S1). Urine was collected for three hours after the meal. In total, we collected urine samples (pre and post) from 32 controls and 14 treated subjects, (Fig. 1). Urine samples were collected at the CTSI during the study visit.
DNA isolation and 16S rRNA gene sequencing
The fecal DNA was extracted using the PowerSoil-htp 96-Well DNA Isolation Kit (MoBio, Carlsbad CA, USA), following the manufacturer’s instructions which includes mechanical and chemical lysis steps. The V4 region of bacterial 16S rRNA genes was amplified in triplicate reactions using barcoded fusion primers 515F/806R, which amplifies bacterial and archaeal 16S genes35,36. The DNA concentration of the V4 amplicons for each sample was measured using the Quant-iT PicoGreen dsDNA assay kit (Life Technologies, Eugene OR, USA), and samples pooled in equal quantities. These pools were treated with the Qiaquick PCR purification kit (Qiagen) to remove primers, quantified using the high-sensitivity dsDNA assay kit and the Qubit 2.0 Fluorometer (Life Technologies, Eugene OR, USA) and then combined at equal concentrations to form the sequencing library. The ~ 254 bp V4 region was sequenced using the Ilumina MiSeq 2 × 150 bp platform at the New York University Langone Medical Center (NYULMC) Genome Technology Center. We included negative controls during the DNA extraction and library prep that were also sequenced.
Oxalobacter formigenes quantitative PCR
qPCR was used to quantitate the number of copies of O. formigenes oxc using the O. formigenes specific primers (Forward 5′-GTG-TTG-TCG-GCA-TTC-CTA-TC-3′, Reverse 5′-TTG-GGA-AGC-AGT-TGG-TGG-3′). qPCR was performed using the LightCycler 480 SYBR Green I Master Mix, primers targeting oxc, in the LightCycler 480 system (Roche, Pleasanton CA). Melting peak analysis was performed from 65 to 95 °C to confirm amplicon specificity. A positive result was defined by amplification greater than 1.0E2, with melting peak between 86–87 °C.
16S rRNA gene sequencing analysis
Quantitative insights for microbial ecology (QIIME, Version Qiime 2–2019.1) was used for quality filtering and downstream analysis for α-diversity, β-diversity, and compositional analysis37. Sequences were filtered for quality trimmed, de-noised, and merged, and then the chimeric sequences were removed using the DADA2 plugin (version 1.6.0.) using default parameters to generate the feature table containing amplicon sequence variants (ASV)38. QIIME 2 was used to generate a rooted phylogenetic tree to be used for phylogenetic analyses. Phylogenetic diversity, observed features number, Chao1, and Shannon indices were used as α-diversity measures of the intra-individual diversity. The inter-individual (β-) diversity was computed as unweighted UniFrac distances and differences in β-diversity were visualized with principal coordinates analysis (PCoA) plots. Taxonomy was assigned using GreenGenes 13_8 for reference.
Sample diversity analyses
Intra-sample α-diversity was calculated using QIIME2, using phylogenetic diversity, observed OTU number, Chao1, and Shannon indices at rarefaction depths of 8000 sequences/sample. Beta-diversity was assessed using the unweighted UniFrac distance metric24.
Oxalobacter formigenes status determination
We tested each fecal sample for the presence of O. formigenes using PCR in duplicate, qPCR, and 16S rRNA gene sequencing. Based on the known several log-fold biological variations in O. formigenes abundance in human fecal specimens24,28, given the ascertainment variability using different methods, we developed a positivity score based on the 42 control subjects who did not receive antibiotics and who were tested at baseline and at least once in follow-up. The maximum number of assessments for each test subject was 16 if the participant was tested at all 4 time points (baseline, weeks 6, 12, 24) in all four assays; and a minimum of 8 if only tested at two time points. For the 42 control participants, the mean ± SD number of determinations was 14.7 ± 2.6. We computed the positivity score by dividing the number of positive assessments by the total number of assessments for that subject. Since the results were bimodal, as expected (Supplementary Fig. 1) we assigned baseline O. formigenes status as negative with score ≤ 0.2 and positive with score ≥ 0.4. Only one subject had a score of 0.3, which we considered indeterminate and we removed this participant from further analysis (Supplementary Fig. 1). Similarly, per sample positivity score was used to assign O. formigenes status at different time points with the criteria: negative with score ≤ 0.2 and positive with score ≥ 0.4.
Urine testing
Urine aliquots were mixed with either HCl (for oxalate measurements) or with thymol (for all other assessments) and then stored at − 80 °C. Pre-meal (fasting) and the 3-h post-meal urinary samples were analyzed by Litholink Corporation (Chicago IL)39,40. In each urine sample, we measured calcium, chloride, creatinine, magnesium, sodium, potassium, phosphate, and ammonium concentrations by standard techniques by Beckman Synchron AU680 (Beckman Instruments, Brea CA), as described40; pH was measured by glass electrode. Oxalate was measured by enzyme assay using oxalate oxidase (Trinity Biotech, Bray, Ireland). Citrate was measured by enzyme assay using citrate lyase (Mannheim Bohringer, Mannheim, Germany). All urine parameters except pH were normalized by dividing by creatinine concentration to account for hydration status.
Longitudinal analysis of urine parameters
A linear mixed-effects model was fitted for urine parameters over the time interval 0–24 weeks. By involving measurement time as the fixed effect and subject as the random effect, we evaluated the changing rates during this period. Other covariates age, sex, and body mass index (BMI) were also included for adjustment. The p-value < 0.05 was considered significant. Analysis was conducted with R statistical software using the lmerTest package. Satterthwaite approximation was employed to get p-value.
Association between Uox/Cr and bacterial taxa
Linear mixed-effects models were fitted to ascertain which microbial taxa are associated with pre- or post-meal urinary oxalate level (or other urinary parameters), respectively. In all models, the microbial factor of interest, α-diversity for the entire bacterial community, or the centered log-ratio transformed relative abundance of each taxon at a given taxonomic rank (phyla, classes, orders, families, genera, and species), and measurement time were included as fixed effects. The intercept and slope of the linear time trend for each subject were included as random effects. Covariates age, gender, ethnicity, BMI, and calcium level were also involved as fixed effects for adjustment. The Benjamini-Hochberg (BH) procedure was applied for multiple testing correction within each taxonomic level. The p-value or adjusted p-value < 0.05 was considered significant. Analysis was conducted with R statistical software using the lmerTest package. Satterthwaite approximation was employed to get p-value. We included data for the participants in (i) the control group, we analyzed a total of 108 pairs of microbial measurements and urinary oxalate level (pre-/post- dietary) at baseline, 6, 12 and 24 weeks; and (ii), in the antibiotic-treatment group, we analyzed a total of 51 pairs of microbial measurements and urinary oxalate level (pre-/post- dietary) at 6, 12, and 24 weeks. A total of 233 taxa were examined at all taxonomic levels (phylum to species). We Included taxa with mean relative abundances among subjects > 10–5. For the adjusted p-values, the Benjamini–Hochberg procedure was applied for each taxonomic level. Unclassified microbial taxa were not included in the analysis. Analysis was conducted with R statistical software using the lme4 package. Unclassified microbial taxa were not included in the analyses.
References
Scales, C. D. et al. Prevalence of kidney stones in the United States. Eur. Urol. 62(1), 160–165 (2012).
Kittanamongkolchai, W. et al. The changing incidence and presentation of urinary stones over 3 decades. Mayo Clin. Proc. 93(3), 291–299 (2017).
Tasian, G. E. et al. Annual incidence of nephrolithiasis among children and adults in South Carolina from 1997 to 2012. Clin. J. Am. Soc. Nephrol. 11(3), 488–496 (2016).
Lieske, J. C. et al. Renal stone epidemiology in Rochester, Minnesota: An update. Kidney Int. 69(4), 760–764 (2006).
Lieske, J. C. et al. Stone composition as a function of age and sex. Clin. J. Am. Soc. Nephrol. 9(12), 2141–2146 (2014).
Holmes, R. P., Goodman, H. O. & Assimos, D. G. Dietary oxalate and its intestinal absorption. Scann. Microsc. 9(4), 1109–1118 (1995) (discussion 1118–1120).
Holmes, R. P. Oxalate synthesis in humans: Assumptions, problems, and unresolved issues. Mol. Urol. 4(4), 329–332 (2000).
Abratt, V. R. & Reid, S. J. Oxalate-degrading bacteria of the human gut as probiotics in the management of kidney stone disease. Adv. Appl. Microbiol. 72, 63–87 (2010).
Stern, J. M. et al. Evidence for a distinct gut microbiome in kidney stone formers compared to non-stone formers. Urolithiasis 44(5), 399–407 (2016).
Ticinesi, A. et al. Understanding the gut-kidney axis in nephrolithiasis: An analysis of the gut microbiota composition and functionality of stone formers. Gut 67(12), 2097–2106 (2018).
Suryavanshi, M. V. et al. Hyperoxaluria leads to dysbiosis and drives selective enrichment of oxalate metabolizing bacterial species in recurrent kidney stone endures. Sci. Rep. 6, 34712 (2016).
Tasian, G. E. et al. Oral antibiotic exposure and kidney stone disease. J. Am. Soc. Nephrol. 29, 1731–1740 (2018).
Ferraro, P. M. et al. Antibiotic use and risk of incident kidney stones in female nurses. Am. J. Kidney Dis. 74, 736–741 (2019).
Mogna, L. et al. Screening of different probiotic strains for their in vitro ability to metabolise oxalates: Any prospective use in humans?. J. Clin. Gastroenterol. 48(Suppl 1), S91–S95 (2014).
Allison, M. J. et al. Oxalobacter formigenes gen. nov., sp. nov.: Oxalate-degrading anaerobes that inhabit the gastrointestinal tract. Arch Microbiol. 141(1), 1–7 (1985).
Liu, M. et al. Microbial genetic and transcriptional contributions to oxalate degradation by the gut microbiota in health and disease. Elife 10, e63642 (2021).
Canales, B. K. & Hatch, M. Oxalobacter formigenes colonization normalizes oxalate excretion in a gastric bypass model of hyperoxaluria. Surg. Obes. Relat. Dis. 13(7), 1152–1157 (2017).
Li, X. et al. Response of germ-free mice to colonization with O. formigenes and altered schaedler flora. Appl. Environ. Microbiol. 82(23), 6952–6960 (2016).
Hatch, M. et al. Oxalobacter sp. reduces urinary oxalate excretion by promoting enteric oxalate secretion. Kidney Int. 69(4), 691–698 (2006).
Kaufman, D. W. et al. Oxalobacter formigenes may reduce the risk of calcium oxalate kidney stones. J. Am. Soc. Nephrol. 19(6), 1197–1203 (2008).
Clemente, J. C. et al. The microbiome of uncontacted Amerindians. Sci. Adv. 1(3), e1500183 (2015).
PeBenito, A. et al. Comparative prevalence of Oxalobacter formigenes in three human populations. Sci. Rep. 9(1), 574 (2019).
Mittal, R. D. et al. Effect of antibiotics on Oxalobacter formigenes colonization of human gastrointestinal tract. J. Endourol. 19(1), 102–106 (2005).
Liu, M. et al. Oxalobacter formigenes-associated host features and microbial community structures examined using the American Gut Project. Microbiome 5(1), 108–125 (2017).
Lange, J. N. et al. Sensitivity of human strains of Oxalobacter formigenes to commonly prescribed antibiotics. Urology 79(6), 1286–1289 (2012).
Kharlamb, V. et al. Oral antibiotic treatment of Helicobacter pylori leads to persistently reduced intestinal colonization rates with Oxalobacter formigenes. J Endourol 25(11), 1781–1785 (2011).
Kelly, J. P. et al. Factors related to colonization with Oxalobacter formigenes in US adults. J. Endourol. 25(4), 673–679 (2011).
Barnett, C. et al. The presence of Oxalobacter formigenes in the microbiome of healthy young adults. J. Urol. 195(2), 499–506 (2016).
Pebenito, A. M. et al. Development of a humanized murine model for the study of Oxalobacter formigenes intestinal colonization. J. Infect. Dis. 220(11), 1848–1858 (2019).
Siener, R. et al. The role of Oxalobacter formigenes colonization in calcium oxalate stone disease. Kidney Int. 83(6), 1144–1149 (2013).
Nazzal, L. & Blaser, M. J. Does the receipt of antibiotics for common infectious diseases predispose to kidney stones? A cautionary note for all health care practitioners. J. Am. Soc. Nephrol. 29(6), 1590–1592 (2018).
Gault, M. H. et al. Comparison of patients with idiopathic calcium phosphate and calcium oxalate stones. Medicine (Baltimore) 70(6), 345–359 (1991).
Hokama, S. et al. Oxalate-degrading Providencia rettgeri isolated from human stools. Int. J. Urol. 12(6), 533–538 (2005).
Chey, W. D. et al. ACG clinical guideline: Treatment of Helicobacter pylori infection. Am. J. Gastroenterol. 112(2), 212–239 (2017).
Caporaso, J. G. et al. Ultra-high-throughput microbial community analysis on the Illumina HiSeq and MiSeq platforms. ISME J. 6(8), 1621–1624 (2012).
Caporaso, J. G. et al. QIIME allows analysis of high-throughput community sequencing data. Nat. Methods 7(5), 335–336 (2010).
Bolyen, E. et al. Reproducible, interactive, scalable and extensible microbiome data science using QIIME 2. Nat. Biotechnol. 37(8), 852–857 (2019).
Callahan, B. J. et al. DADA2: High-resolution sample inference from Illumina amplicon data. Nat. Methods 13(7), 581–583 (2016).
Cheng, J. W. et al. The effect of lemonade and diet lemonade upon urinary parameters affecting calcium urinary stone formation. J. Endourol. 33(2), 160–166 (2019).
Asplin, J. et al. Supersaturation and stone composition in a network of dispersed treatment sites. J. Urol. 159(6), 1821–1825 (1998).
Acknowledgements
Supported in part by R01 DK090989, R01DK110014, the NYU CTSA grant UL1TR000038 from the National Center for the Advancement of Translational Science (NCATS), and U01 AI22245, all from the NIH, the Oxalosis and Hyperoxaluria Foundation-American Society of Nephrology Career Development Award (to L.N.), the C&D and Zlinkoff Funds, and the Foundation LeDucq Transatlantic Network. This study also was supported by Rare Kidney Stone Consortium grant U54KD083908, a part of the Rare Diseases Clinical Research Network, an initiative of the Office of Rare Diseases Research, the National Center for Advancing Translational Sciences (NCATS), and funded through a collaboration between the NCATS and NIDDK. This work was supported by the National Research Foundation of Korea (NRF) grant funded by the Korea government (MSIT) (NRF-2021R1C1C1013861).
Author information
Authors and Affiliations
Contributions
L.N. and M.J.B. wrote the main manuscript text and prepared the figures. F.F., M.J.B., D.S.G., G.P.P., and L.N. designed the study. L.N. and N.H. performed the study. L.N., M.L., H.L., H.K., C.W., and Z.G. performed the analysis. JRA tested the urine samples. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Nazzal, L., Francois, F., Henderson, N. et al. Effect of antibiotic treatment on Oxalobacter formigenes colonization of the gut microbiome and urinary oxalate excretion. Sci Rep 11, 16428 (2021). https://doi.org/10.1038/s41598-021-95992-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-021-95992-7
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.