Abstract
This study aimed to evaluate the efficacy and safety of bone cement-augmented pedicle screw fixation for stage III Kümmell disease. Twenty-five patients with stage III Kümmell disease who received bone cement-augmented pedicle screw fixation at the First Affiliated Hospital of Guangzhou University of Chinese Medicine between June 2009 and December 2015 were enrolled. All patients were females with a history of osteoporosis. The vertebral Cobb angle (V-Cobb angle), the fixed segment Cobb Angle (S-Cobb angle), pelvic parameters, visual Analogue Scale (VAS) score, and Oswestry Disability Index (ODI) were assessed preoperatively, postoperatively and at the final follow-up. Complications, loosening rate, operation time, and intraoperative bleeding were recorded. The average lumbar vertebral density T-value was − 3.68 ± 0.71 SD, and the average age was 71.84 ± 5.39. The V-Cobb angle, S-Cobb angle, and Sagittal Vertical Axis (SVA) were significantly smaller postoperatively compared to the preoperative values. The VAS and ODI at 1 month after surgery were 3.60 ± 1.00 and 36.04 ± 6.12%, respectively, which were both significantly lower than before surgery (VAS: 8.56 ± 1.04, ODI: 77.80 ± 6.57%). Bone cement-augmented pedicle screw fixation is a safe and effective treatment for stage III Kümmell disease. It can effectively correct kyphosis, restore and maintain sagittal balance, and maintain spinal stability.
Similar content being viewed by others
Introduction
The frequency of Kümmell disease, a complication of osteoporotic vertebral fracture (OVF), is increasing globally1. Since the condition was first described by Herman Kümmell in 1891, the literature has referred to Kümmell disease as being characterized by delayed osteonecrosis after trauma2, nonunion of compression fracture3, delayed collapse of OVF4, intravertebral pseudarthrosis5, and vertebral vacuum sign6. A history of minor trauma was also present in some patients. However, patients without a history of trauma, gradually develop activity-related back pain or lower extremity nerve symptoms after a few weeks or months of an asymptomatic period.
The development of Kümmell disease involves the following 3 stages: Stage I, spinal vertebral bodies are slightly injured due to minor trauma or in the absence of trauma; Stage II, vertebral bodies experience dynamic instability in the cleft area, followed by fracture and bone collapse; and Stage III, the compressed fractured vertebral body compresses the posterior spinal cord, leading to continuous back pain and other neurological symptoms7.
The current treatment strategies for Kümmell disease remain controversial because there are no specific treatment criteria. Various surgical strategies have been developed, including percutaneous kyphoplasty (PKP) or vertebroplasty (PVP), anterior-only, posterior-only, and combined anterior and posterior procedures8,9,10. For stages I and II Kümmell disease, adequate pain relief, vertebral body height restoration, and kyphosis correction are achieved with PKP and PVP11,12. However, stage III Kümmell disease patients with spinal canal stenosis, particularly with nerve damage, PKP or PVP are less effective, with a higher risk of cement leakage, and potential severe neurological damage. The final aim of treatment for patients with mild spinal canal stenosis is to relieve back pain, prevent further collapse of the affected vertebrae, and delay neurological deficits13.
However, for osteoporotic vertebrae, pedicle screw loosening and internal fixation failure are common postoperative complications14. Varieties of internal fixation methods such as the use of expansion screws and the increase of fixed segments have been proposed to reduce the risk of failure of common pedicle screw fixation in osteoporosis patients14. Bone cement-augmented pedicle screw fixation have been paid more and more attention by scholars in recent years because of its good pull-out resistance and fixation. Biomechanical tests have proved that bone cement reinforced pedicle screws can improve the pull-out resistance of 147–278%15,16,17. At present, there is no standard surgical option or single effective treatment. We aimed to address this gap by retrospectively analyzing groups of patients in our hospital to investigate the efficacy of bone cement-augmented pedicle screw fixation for stage III Kümmell disease.
Materials and methods
This study was approved by the Ethics Committee of The First Affiliated Hospital of Guangzhou University of Chinese Medicine.The IRB number is NO. ZYYECK (2017)041. Written informed consent was obtained for each participant. From June 2009 to December 2015, patients with stage III Kümmell disease who visited in our hospital for bone cement-augmented pedicle screws were recruited. The inclusion criteria were: (1) diagnosis with the stage III Kümmell disease by symptoms, signs, and imaging examinations; (2) lumbar vertebral bone mineral density (BMD) of T ≤ − 2.5 SD measured by dual energy X-ray absorptiometry; (3) with or without neurological symptoms. Exclusion criteria included: (1) pathological vertebral fractures such as tumors or infections, and (2) serious medical diseases or intolerance to operation. The research methodology fow chart is shown in Fig. 1.
Operative methods
Through the posterior median approach to the spine, the intersection of the midpoint of the transverse process of the vertebral body and the vertical line of the outer margin of the superior articular process was exposed. Cannulated pedicle screws were inserted into the vertebrae under the monitoring of a C-arm X-ray machine, and then 1.5–2.5 ml of bone cement was injected into each screw channel. The cannulated pedicle screws are hollow and they have some lateral holes in the tip of the screw, thus the bone cement can fill up the cancellous bone around the screws. These screws come from Shanghai Reach Medical Instrument Co. Ltd. The specification of pedicle screw was determined preoperatively by measuring the diameter of the pedicle.
Postoperative management
At early stage after operation, the patients were required to perform both lower limbs exercises on the bed. The drainage tube was removed when the amount of drainage was less than 50 ml/day. All patients began to get out of bed and walk with the protection of waist circumference 3 or 4 days after the operation. Patients were required to wear a waist circumference within first month after operation. Cephalosporin was used once intraoperatively to prevent infection, and antibiotics were not routinely used postoperatively. After operation, standard anti-osteoporosis treatment (calcium, vitamins D and diphosphate).
Data collection and radiographic assessment
Evaluation of clinical efficacy
The VAS and ODI scores were recorded by ward clinicians during outpatient visits or telephone follow-up. The operation time and blood loss were obtained from medical records. The incidence of complications, such as nerve injury, dural tearing, and bone cement leakage were also recorded.
Imaging evaluation
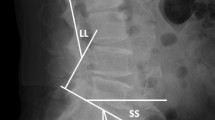
The V-Cobb angle and S-Cobb angle of the injured vertebrae were measured by lateral X-ray and compared at the preoperative, postoperative and final follow-up appointments. Loosening of the pedicle screw was observed on CT or X-ray film during the final follow-up. All spinopelvic parameters were measured twice on total spine photography by two orthopedists, independently, and the mean values were used for analysis. The degree of lumbar lordosis (LL) was assessed from the inferior endplate of T12 to the superior endplate of S118. Pelvic tilt (PT) was defined as the angle subtended by a line drawn from the midpoint of the sacral endplate to the center of the bicoxofemoral axis and a vertical plumb line extending from the bicoxofemoral axis19. Sacral slope (SS) was defined as the angle between the end plate of S1 and the horizontal line19. Pelvic incidence (PI) was defined as the angle between the line perpendicular to the sacral endplate at its midpoint and the line connecting this point to the midpoint of femoral heads axis19. The sagittal vertical axis (SVA) was measured by the horizontal distance from the S1 postero-superior corner to the C7 PL18.
Statistical analysis
IBM SPSS 19.0 Software was used to analyze the data. All data are expressed as mean ± SD. One-way ANOVA followed by the Student–Newman–Keuls post hoc test was used, and p < 0.05 was statistically significant.
Results
There were 34 stage III Kümmell disease patients treated with bone cement-augmented pedicle screw fixation. A total of 25 patients were enrolled in this study (Fig. 2). Four patients died of other diseases, and 9 were lost to follow-up. The follow-up rate was 73.52%. All patients were females with a mean patient age of 71.84 ± 5.39 years and T scores of − 3.68 ± 0.71 SD. Patients were treated with short-segment fixation (n = 11) (Fig. 3) or long-segment fixation (n = 14) (Fig. 4) combined with posterolateral fusion. All methods were carried out in accordance with relevant guidelines and regulations in the manuscript.
Case illustration of a patient. Female, 62 years, BMD (T score) was − 3.8SD. (A2–C2) Preoperative lateral X-ray and CT scan showed L1 vertebral fracture with, MRI showed low signal of the necrotic area on T2-weighted images. Follow-up standing X-ray at 3 months (D2,E2) and 4 year (F2,G2) post T12-L2 bone cement-augmented pedicle screw fixation.
Case illustration of a patient. Female, 80 years, BMD (T score) was − 3.4SD. (A1–C1) Preoperative lateral X-ray and CT scan showed T12 vertebral fracture with, MRI showed low signal of the necrotic area on T2-weighted images. Follow-up standing X-ray at 2 year (D1,E1) and 5 year (F1,G1) post T10-L2 bone cement-augmented pedicle screw fixation.
All patients underwent spinal surgery successfully. Two patients underwent a second surgery on day 6 and 7 after the first surgery because of poor efficacy, and were then discharged successfully. The surgical wound of three patients did not heal well, but they were discharged successfully after extended antibiotic treatment. During the operation, none of the patients experienced nerve injury or dural sac tearing. A total of 178 pedicle screws were used, and all were reinforced with bone cement. Among them, 45 screws showed bone cement leakage beside the vertebra or along the vertebral body vein, with a leakage rate of 25.28%. No patients had serious complications such as nerve compression or pulmonary embolism due to bone cement leakage. During the follow-up, we found 7 fixed segments with adjacent vertebral fractures, however, these were relieved with vertebroplasty. No pedicle screw loosening was found during follow-up. Before surgery, most patients showed signs of nerve compression, but symptoms were significantly recovered after surgery (Table 1). Postoperative and follow-up ODI and VAS scores were significantly lower than preoperative scores (Fig. 5).
Details of the patients’ demographic data are summarized in Table 2. No significant differences were observed in PI, PT, LL, and SS (Table 3).The V-Cobb angle, S-Cobb angle, and SVA of patients at the post-operative and the final follow-up appointments were significantly lower than the pre-operative appointment, no significant difference was observed between the post-operative and final follow-up appointments (Table 4).
Discussion
Kümmell disease was first described in 1891 as an uncommon complication of osteoporotic vertebral fracture, more frequently encountered in patients with severe osteoporosis that have taken long-term courses of corticosteroids or sustained a spinal injury20. Kümmell disease is different from fresh vertebral fracture, and intra-bone clefting is the most important characteristic used to diagnose Kümmell disease. Kümmell disease mostly occurs in women13. The thoracolumbar junction, particularly the T12 vertebra, is the most commonly affected vertebral segment21. In our study, 76% of injured vertebra were in the thoracolumbar segment. Thoracolumbar vertebral body has large range of motion and stress concentration, which easily leads to ischemic necrosis after osteoporotic vertebral fracture.
Different stages of Kümmell disease have unique pathological features. The early stages include avascular necrosis characterized by an accumulation of fluid and inflammatory exudate components21. During stage III, the compressed, fractured vertebral body compresses the posterior spinal cord, leading to continuous back pain and other neurological symptoms. Stage III Kümmell disease is characterized by the collapse of the posterior vertebral body wall, the formation of spinal canal stenosis, and dural sac compression21. Most stage III patients, including 84% of the patients in our study, have preoperative neurological symptoms. In our study, the posterior wall of the fractured vertebral body was fragmented and compressed into the dural sac in all patients.
The treatment of the Kümmell disease remains controversial. Most spinal surgeons suggest that Kümmell disease should be treated by operative interventions because conservative treatments are less effective and are associated with a high risk of complications and delayed neurological deficits22. For early stages patients without neurological symptoms, the aim of treatment is to preserve movement in the diseased vertebrae, and maintain the sagittal balance of the spine. PKP and PVP restore the height of the vertebral body and correct any deformities, which can help achieve satisfactory pain relief23. However, PVP and PKP are less suitable for stage III patients because the surrounding vertebral cortex has already been compromised, as well as a higher risk of severe nerve damage caused by bone cement leakage13. In our study, the bone cement leakage rate was 25.28%, but there were no serious complications, suggesting that short-term leakage is not damaging. Delayed cement displacement and further collapse have been reported in cases of Kümmell disease treated by cement augmentation alone, with poor bone incorporation of cement noted after a long-term follow-up24,25. Therefore, displacement of bone cement and further vertebral collapse may occur after PKP or PVP26. In our study, some patients underwent vertebroplasty for fractured vertebrae, but we did not find cement displacement during follow-up because bone cement-augmented pedicle screw fixation provided stability.
There are alternative treatment strategies for stage III Kümmell disease, but consensus regarding which is most feasible and effective is lacking. For stage III patients with severe stenosis of the spinal canal and neurological symptoms, the objective of surgery is to relieve cord compression, eliminate spinal instability, and restore the sagittal balance of the spine12,27. Many studies have suggested that the main factor contributing to delayed neurological deficits following vertebral collapse in the osteoporotic spine is instability at the fracture site, rather than mechanical compression of the spinal cord by bone fragments28,29. Therefore, maintaining spinal stability is important for treating stage III patients. Other studies suggested that modified posterior vertebral column resection surgery was an effective and safe surgical method to treat stage III Kümmell disease, especially for patients with kyphosis and obvious symptoms of nerve compression; however, the long-term clinical effects require additional evaluation. Anterior reconstruction and posterior osteotomy have also been proposed for the management of stage III Kümmell disease with neurological deficits30. Anterior reconstruction permits direct resection of bony fragments and provides anterior column support. Posterior osteotomy is a common treatment; the advantages include dissection of the posterior cortex by posterior spinal shortening osteotomy and correction of kyphosis31,32. Moreover, these major surgical interventions can be challenging in patients of advanced age, and confer numerous morbid complications and frequent instrumentation failure secondary to severe osteoporosis4. Traditional posterior long-segment fixation was not appropriate for stage III Kümmell disease because the procedure was associated with significant trauma and multiple complications, which are worrisome in elderly patients with comorbidities33. Compared with these methods, on the basis of laminar decompression to improve the neurological symptoms caused by spinal stenosis, and according to the patient’s fracture end reduction, using the bone cement-augmented pedicle screw fixation can further increase the stability and prevent the fracture from collapsing again. Lu et al.34 reported that the use of the bone cement-augmented pedicle screw fixation among the thoracolumbar fractures patients with satisfactory results. In our study, most patients showed signs of nerve compression preoperatively, but symptoms were significantly recovered after surgery. Postoperative and follow-up ODI and VAS scores were significantly lower than preoperative scores.
Leakage of bone cement is a common complication of bone cement-augmented pedicle screw fixation. Jassen et al.35 reported that among the 165 patients who underwent bone cement-augmented pedicle screw fixation, 110 (66.7%) had bone cement leakage without neurological symptoms, and 13 (7.9%) had pulmonary embolism, of which 5 cases (3%) had symptoms of pulmonary embolism requiring treatment, and 2 cases (1.2%) had symptoms of bone cement allergy. In our study, 45 of the 178 screws showed bone cement leakage beside the vertebra or along the vertebral body vein, with a leakage rate of 25.28%. In addition, although all the leakage of bone cement has no obvious clinical symptoms, there are some studies have shown that the leakage of bone cement in the intervertebral disc will increase the risk of secondary fractures of the adjacent vertebral body during the long term follow up36,37.
In order to avoid leakage of bone cement, we can take some measures as follows: (1) select a suitable screw. The data including the pedicle width, vertebral length and introversion angle should be measured before the operation; (2) reduce internal inclination of screw placement to avoid screw appearing in the middle of the vertebral body properly; (3) a proper time to inject the bone cement while the cement becomes at an appropriate timing; (4) X ray or/and CT would be used as monitoring during operation. By using small amount multiple injection method (0.1 ml cement injection per time) before another X-ray examination, we could make sure if the bone cement have leakage or not; (5) it is recommended that the amount of single nail bone cement should be about 1.5–2 ml to control the amount of bone cement injected and the number of reinforcement screws.
There is high risk of pedicle screw loosening because of the osteoporotic vertebra in stage III Kümmell disease. Considering the unsatisfactory performance of traditional pedicle screws in damaged spines, bone cement-augmented pedicle screw fixation strengthens the anti-pullout capability by injecting cement carefully through the screws into the vertebral body. The final follow-up results of SVA, V-Cobb angle and S-Cobb angle were significantly better than those preoperation. The sagittal balance of the spine and the local balance and stability of fractured vertebral body were corrected and maintained by increasing the stability of pedicle screw. In our study, there was no significant difference between postoperative and the final follow-up aboutresults of SVA, V-Cobb angle and S-Cobb angle, which means that bone cement-augmented pedicle screw fixation maintained the stability of the spine and pelvis of the stage III Kümmell disease patients. Posterior screw stress was markedly reduced because of the anterior support provided by the intravertebral cement, which can decrease the risk of internal fixation failure18.
There are some limitations to our study. First, it was a retrospective study at a single center with a small sample size. Thus, further studies with larger samples are needed to confirm our findings. Secondly, we observed long segmental fixation and short segmental fixation together; however, these two fixation methods may have different therapeutic effects.
Conclusions
Bone cement-augmented pedicle screw fixation is a safe and effective treatment for stage III Kümmell disease. It effectively corrects kyphosis, and safely maintains the stability of the spine and sagittal balance. Further prospective and large sample clinical studies are needed to confirm them.
References
Hadjipavlou, A. G., Katonis, P. G., Tzermiadianos, M. N., Tsoukas, G. M. & Sapkas, G. Principles of management of osteometabolic disorders affecting the aging spine. Eur. Spine J. 12(Suppl 2), S113–S131 (2003).
Benedek, T. G. & Nicholas, J. J. Delayed traumatic vertebral body compression fracture; part II: Pathologic features. Semin. Arthritis Rheum. 10, 271–277 (1981).
Tsujio, T. et al. Characteristic radiographic or magnetic resonance images of fresh osteoporotic vertebral fractures predicting potential risk for nonunion: A prospective multicenter study. Spine (Phila) 36, 1229–1235 (2011).
Nakashima, H. et al. Comparative study of 2 surgical procedures for osteoporotic delayed vertebral collapse: Anterior and posterior combined surgery versus posterior spinal fusion with vertebroplasty. Spine (Phila) 40, E120–E126 (2015).
Kim, H. S. & Heo, D. H. Percutaneous pedicle screw fixation with polymethylmethacrylate augmentation for the treatment of thoracolumbar intravertebral pseudoarthrosis associated with Kummell’s osteonecrosis. Biomed. Res. Int. 2016, 3878063 (2016).
Ito, Y., Hasegawa, Y., Toda, K. & Nakahara, S. Pathogenesis and diagnosis of delayed vertebral collapse resulting from osteoporotic spinal fracture. Spine J. 2(2), 101–106 (2002).
Yang, D. L., Yang, S. D., Chen, Q., Shen, Y. & Ding, W. Y. The treatment evaluation for osteoporotic Kummell disease by modified posterior vertebral column resection: Minimum of one-year follow-up. Med. Sci. Monit. 23, 606–612 (2017).
Kanayama, M. et al. Role of major spine surgery using Kaneda anterior instrumentation for osteoporotic vertebral collapse. J. Spinal Disord. Tech. 23(1), 53–56 (2010).
Suk, S. I., Kim, J. H., Lee, S. M., Chung, E. R. & Lee, J. H. Anterior-posterior surgery versus posterior closing wedge osteotomy in posttraumatic kyphosis with neurologic compromised osteoporotic fracture. Spine (Phila) 28, 2170–2175 (2003).
Huang, Y. et al. Clinical efficacy of percutaneous kyphoplasty at the hyperextension position for the treatment of osteoporotic Kümmell disease. Clin. Spine Surg. 29, 161–166 (2016).
Yang, H., Pan, J. & Wang, G. A review of osteoporotic vertebral fracture nonunion management. Spine (Phila) 39, B4–B6 (2014).
Huang, Y. S. et al. Bone cement-augmented short-segment pedicle screw fixation for Kümmell disease with spinal canal stenosis. Med. Sci. Monit. 24, 928–935 (2018).
Funao, H. et al. Comparative study of spinopelvic sagittal alignment between patients with and without degenerative spondylolisthesis. Eur. Spine J. 21, 2181–2187 (2012).
Galbusera, F. et al. Pedicle screw loosening: A clinically relevant complication. Eur. Spine J. 24, 1005–1016 (2015).
Tan, J. S. et al. Cement augmentation of vertebral screws enhances the interface strength between interbody device and vertebral body. Spine (Phila) 32(3), 334–341 (2007).
Bullmann, V., Liljenqvist, U. R., Rödl, R. & Schulte, T. L. Pedicle screw augmentation from a biomechanical perspective. Orthopade 39(7), 673–678 (2010).
Chang, M. C., Kao, H. C., Ying, S. H. & Liu, C. L. Polymethylmethacrylate augmentation of cannulated pedicle screws for fixation in osteoporotic spines and comparison of its clinical results and biomechanical characteristics with the needle injection method. J. Spinal Disord. Tech. 26(6), 305–315 (2013).
Duval-Beaupère, G., Schmidt, C. & Cosson, P. A Barycentremetric study of the sagittal shape of spine and pelvis: The conditions required for an economic standing position. Ann. Biomed. Eng. 20, 451–462 (1992).
Kim, P. & Kim, S. W. Balloon kyphoplasty: An effective treatment for Kummell disease. Korean J. Spine 13, 102–106 (2016).
Laredo, J. D. Expert’s comment concerning Grand Rounds case entitled “Kümmell’s disease: Delayed post-traumatic osteonecrosis of the vertebral body” (by R. Ma, R. Chow, F. H. Shen). Eur. Spine J. 19, 1071–1072 (2010).
Toyone, T. et al. Changes in vertebral wedging rate between supine and standing position and its association with back pain: A prospective study in patients with osteoporotic vertebral compression fractures. Spine (Phila) 31, 2963–2966 (2006).
Fabbriciani, G. et al. Osteoanabolic therapy: A non-surgical option of treatment for Kümmell’s disease. Rheumatol. Int. 32, 1371–1374 (2012).
Huang, Y. S. et al. Comparison of percutaneous kyphoplasty and bone cement-augmented short-segment pedicle screw fixation for management of Kümmell disease. Med. Sci. Monit. 24, 1072–1079 (2018).
Wagner, A. L. & Baskurt, E. Refracture with cement extrusion following percutaneous vertebroplasty of a large interbody cleft. Am. J. Neuroradiol. 27, 230–231 (2006).
Wang, H. S., Kim, H. S., Ju, C. I. & Kim, S. W. Delayed bone cement displacement following balloon kyphoplasty. J. Korean Neurosurg. Soc. 43, 212–214 (2008).
Chen, L., Dong, R., Gu, Y. & Feng, Y. Comparison between balloon kyphoplasty and short segmental fixation combined with vertebroplasty in the treatment of Kümmell’s Disease. Pain Phys. 18, 373–381 (2015).
Li, H., Liang, C. Z. & Chen, Q. X. Kümmell’s disease, an uncommon and complicated spinal disorder: A review. J. Int. Med. Res. 40, 406–414 (2012).
Sudo, H. et al. Anterior decompression and strut graft versus posterior decompression and pedicle screw fixation with vertebroplasty for osteoporotic thoracolumbar vertebral collapse with neurologic deficits. Spine J. 13, 1726–1732 (2013).
Verlaan, J. J. Stabilizing osteoporotic thoracolumbar fractures through an anterior or posterior approach: What works best. Spine J. 13, 1733–1735 (2013).
Li, K. C., Li, A. F., Hsieh, C. H., Liao, T. H. & Chen, C. H. Another option to treat Kümmell’s disease with cord compression. Eur. Spine J. 16(9), 1479–1487 (2007).
Kaneda, K., Asano, S., Hashimoto, T., Satoh, S. & Fujiya, M. The treatment of osteoporotic-posttraumatic vertebral collapse using the Kaneda device and a bioactive ceramic vertebral prosthesis. Spine (Phila) 17(8 Suppl), S295–S303 (1992).
Huang, Y. S. et al. Long-segment or bone cement-augmented short-segment fixation for Kummell disease with neurologic deficits? A comparative cohort study. World Neurosurg. 116, e1079–e1086 (2018).
Pappou, I. P., Papadopoulos, E. C., Swanson, A. N., Cammisa, F. P. Jr. & Girardi, F. P. Osteoporotic vertebral fractures and collapse with intravertebral vacuum sign (Kümmel’s disease). Orthopedics 31(1), 61–66 (2008).
Lu, W. et al. Analysis of percutaneous kyphoplasty or short-segmental fixation combined with vertebroplasty in the treatment of Kummell disease. J. Orthop. Surg. Res. 14(1), 311 (2019).
Janssen, I. et al. Risk of cement leakage and pulmonary embolism by bone cement-augmented pedicle screw fixation of the thoracolumbar spine. Spine J. 17(6), 837–844 (2017).
Xiao, Y. P., Bei, M. J., Yan, C. Q. & Chang, J. Z. Analysis of the effect of percutaneous vertebroplasty in the treatment of thoracolumbar Kümmell’s disease with or without bone cement leakage. BMC Musculoskelet. Disord. 22(1), 10 (2021).
Chen, C., Fan, P., Xie, X. & Wang, Y. Risk factors for cement leakage and adjacent vertebral fractures in kyphoplasty for osteoporotic vertebral fractures. Clin. Spine Surg. 33(6), E251–E255 (2020).
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Mo, Gy., Zhou, Tp., Guo, Hz. et al. Long-term efficacy and safety of bone cement-augmented pedicle screw fixation for stage III Kümmell disease. Sci Rep 11, 13647 (2021). https://doi.org/10.1038/s41598-021-93013-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-021-93013-1
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.