Abstract
This study aimed to assess the psychological impact of the COVID-19 pandemic on guardians of children and adolescents with type 1 diabetes. An online survey was performed to assess the prevalence of pandemic-related emotional burden, mental health disorders and diabetes-specific emotional burden related to diabetes care during the COVID-19 pandemic. Caregivers of children and adolescents with diabetes under the age of 18 and caregivers of youth without diabetes for the non-diabetes group were invited to participate. For the primary outcome, mental health disorders were evaluated using the Self-Reporting Questionnaire (SRQ-20), while pandemic-related emotional burden and diabetes-specific emotional burden related to diabetes care were evaluated in different domains with specific questions. For analyses, a hierarchical testing strategy was performed. A total of 764 participants were included in the study. Regarding the pandemic period, caregivers of youth with type 1 diabetes endorsed significantly more pandemic-related emotional burden for both themselves (OR 1.67; 95% CI, 1.10 to 2.53) and for their child (OR 2.28; 95% CI, 1.54 to 3.38) when compared to the non-diabetes group. The emotional burden evaluation on different age ranges showed that the two groups were similar when the dependent youth was younger than 6 years. Moreover, a positive screening for mental health disorders during social distancing was higher in the diabetes group compared to the non-diabetes group (OR 2.43; 95% CI, 1.70 to 3.47), particularly in those aged under 12 years old. There was no difference between groups in mental health disorders among caregivers of adolescents older than 12 years. Our results allow to conclude that concern, burden and mental health disorders can be present in caregivers of youth with diabetes, and behavioral changes during the COVID-19 pandemic may enhance this situation.
Similar content being viewed by others
Introduction
Caring for children and adolescents with type 1 diabetes mellitus involves daily challenges and can put a psychological strain on those responsible. A study carried out with children under 7 years old shows that caregivers play a fundamental role in controlling the disease and experience the responsibility for its short and long-term consequences, such as episodes of hypoglycemia, future complications, and the impact the disease will have on their children's quality of life1. Another study with children under 8 years old shows that, in addition to the responsibility for optimal glycemic control, parents also suffer from constant concerns about the care for their children while the parents are not present. The difficulty in finding someone reliable and used to the demands of diabetes is also challenging. This makes the role of caregiver a full-time job2. Despite these issues, concerns tend to be child-centered and the psychological demands of family members involved in childcare are often neglected.
The emotional burden experienced by caregivers of children and adolescents with type 1 diabetes may be aggravated by the current COVID-19 pandemic. The change in family dynamics that has occurred since the beginning of COVID-19 is reflected in different aspects of the care of children with diabetes. First, the concern and fear of a potentially serious infection for the child, constitutes a stressful situation3. Second, the suspension of school and extracurricular activities results in more time for children and adolescents at home, requiring greater attention from caregivers. Third, the closing of parks and recreation rooms results in more sedentary habits and, consequently, lower daily energy expenditure4. All these changes may significantly impact the glycemic control of the child, adding even more responsibilities and enhancing the stress on guardians.
Despite everything mentioned above, the psychological repercussion of the current scenario in guardians of children and adolescents with diabetes remains hypothetical. Several studies have shown that the deleterious effects of the caregiver’s psychological distress apply to both caregivers and children, resulting in worse glycemic control and increasing the incidence of depression during adolescence2,5,6,7,8,9,10. The care for caregivers’ mental well-being, however, has received little priority when assessing the impact of stressful situations, such as the current pandemic of COVID-19 and the social distancing it requires11. The present study aims to assess the psychological impact of routine changes and the demands of the disease on caregivers of children and adolescents with type 1 diabetes during the COVID-19 pandemic, and to identify factors that can guide strategies in similar situations in the future.
Methods
Study design and setting
This was a cross-sectional study carried out to evaluate the prevalence of mental health disorders and pandemic-related emotional burden during the COVID-19 pandemic in caregivers of children and adolescents with type 1 diabetes. Caregivers of children and adolescents with a previous diagnosis of type 1 diabetes were recruited to participate in this study as the diabetes group, while caregivers of children and adolescents without diabetes were selected for the non-diabetes group. The invitation to participate in the diabetes group was carried out through the social media of the Juvenile Diabetes Association, a society that integrates associations throughout Brazil meant for children and adolescents with diabetes. The invitation to the non-diabetes group was carried out through social media of medical students across the country. An electronic invitation was sent to access an online survey between May 18th and June 9th of 2020, approximately two months after the beginning of the pandemic in Brazil and after the disclosure from the national ordinance that recommended social distancing for high-risk groups. At the time of the evaluation, Brazil was already considered one of the epicenters of the pandemic. National legislation restricted the functioning of establishments that offer essential services, and which regulated the indication of an exceptional teleworking regime for people with respiratory diseases, immunosuppressed or with chronic disease, upon medical recommendation. Moreover, school activities and non-emergency medical consultations have been suspended. The manuscript description follows the STROBE guideline12.
Participants
Adults of any age who were parents or the primary caregivers of children and adolescents aged less than or equal to 18 years-old with type 1 diabetes were selected for the diabetes group. For the non-diabetes group, adults who were parents or the primary caregivers of children and adolescents aged less than or equal to 18 years-old without diabetes, and who were invited through the social media of student leagues across the country were selected.
Variables and data source
Demographic and clinical data
Sociodemographic information about the caregivers and clinical information about the dependent under their responsibility [such as age, presence of comorbidities, diabetes duration, age at diagnosis, use of medication, last hemoglobin A1c (HbA1c) levels, and presence of diabetes complications] were collected at the beginning of the questionnaire.
Support and relationships
After the gathering of initial information, an evaluation about the participant’s social support and relationships was carried out using specific questions (see supplementary material). Participants were asked to choose, based on the last six months (to evaluate periods in addition to the pandemic period), one of the following options regarding the topics already mentioned: “most of the time”, “occasionally” or “almost never/never”. For analysis, a negative response was considered when participants answered “almost never / never”.
Consequences of social distancing
Regarding the routine during the pandemic, the questionnaire included “yes”, “no” or “partially” response options for the participants’ compliance regarding social distancing since the beginning of the social distancing recommendation, the time spent by the child at home and possible difficulties related to income and medical care. It was considered that family income decreased if the patient answered yes to the reduction of some source of family income since the beginning of the pandemic.
Outcomes
The primary outcomes of this study included the presence of pandemic-related emotional burden, the presence of positive screening for mental disorders, and the presence of diabetes-specific emotional burden related to the diabetes care during the period of social distancing, which was caused by the COVID-19 pandemic.
Pandemic-related emotional burden
The evaluation of pandemic-related emotional burden was carried out for both diabetes and non-diabetes groups and was performed using a 5-point Likert scale for different domains. The domains were evaluated using the following sentences: (1) personal concern—“I often feel worried and afraid of being infected with the coronavirus”; (2) child-related concern—“I often feel worried and afraid that my child may be infected with the coronavirus”; (3) personal emotional burden: “I often feel tired and exhausted due to the changes in routine since the social distancing related to the COVID-19 pandemic started”; (4) child-related emotional burden: “I often feel tired and exhausted from the responsibility to protect my child during the COVID-19 pandemic”. For the analyses, “totally agree” and “agree” were considered affirmative answers.
Screening for mental health disorders during social distancing
The evaluation of mental health disorders was carried out for both diabetes and non-diabetes groups. For tracking mental health disorders such as anxiety-related disorders, depression and somatoform disorders, the Self-Reporting Questionnaire (SRQ—20) was used in a version previously validated to the Brazilian population13. “Yes” or “No” answers were requested for each statement, and a positive screening was considered when the participant answered “Yes” in at least seven of the 20 items13.
Diabetes-specific emotional burden related to diabetes care
The evaluation of diabetes-specific emotional burden was applied only to the diabetes group using a 5-point Likert scale. The following statements were used for the domains evaluated: (1) care sharing: “I feel frustrated because I am the only one responsible for helping my child in using medications and managing glycemic control”; (2) support: “I feel frustrated with the lack of understanding and support I get from my friends and family in relation to taking care of someone with diabetes”; (3) appreciation: “I feel underestimated for all the effort I put into helping my child to take care of diabetes”; (4) exhaustion: “I feel that my child's diabetes is consuming a lot of my physical and mental energy every day”; (5) guilt: “I feel guilty if my child's diabetes is not well controlled”. In order to facilitate interpretation, answers were categorized in (a) it is a problem, if the answer was “totally agree” or “agree”; (b) it is not a problem, if the answer was “strongly disagree” or “disagree”; and (c) not decided, if the answer was “not decided”.
Sample size
The Krejcie and Morgan (1970) formula was used to determine sample size for a given population and for an analysis using a 95% confidence level and a margin of error of 0.0514. Considering the estimate of 95,800 individuals with diabetes and under 18 years of age in Brazil in 2019, 380 responses in the diabetes group was determined to be necessary to obtain the adequate power for the analyses performed15. The strategy was repeated for the non-diabetes group to obtain homogeneity in the procedure performed.
Statistical methods
The data were transcribed from the online platform SurveyMonkey, (San Mateo, CA, U.S.A.; http://www.surveymonkey.com) to the Statistical Package for Social Science (SPSS®) version 20 for analysis. A hierarchical testing strategy was performed to deal with the problem of multiplicity (type I error inflation), and the following outcomes were ranked in descending order of importance: (1) presence of pandemic-related emotional burden, (2) mental health during social distancing and (3) presence of diabetes-specific emotional burden during the COVID-19 pandemic. Just for those outcomes, P values were reported for until the first outcome with a P value greater than 0.05 was obtained and further tests were considered only for exploratory analyses. For all other analyses (baseline characteristics and psychosocial profile during the pandemic), the P value will be reported as usually done. For the diabetes-specific emotional burden related to diabetes care, considering that only the diabetes group was evaluated, P values are not shown.
Descriptive data are presented as mean ± standard deviation (SD) or frequency (%). Statistical analyses of the results include Chi-square tests for categorical variables and t tests for continuous parametric variables. Logistic regressions were used to correct for possible confounders and data are presented as odds ratios (OR) and their respective 95% confidence intervals (CI). Only participants who answered at least 75% of the questionnaire were included on the analyses. The missing values are excluded from the analysis if the participant did not answer the question (listwise deletion). A sensitivity analysis was performed to assess psychosocial aspects in caregivers based on different age groups [preschoolers (< 6 years), young children (between 6 and 12 years), and adolescents (> 12 years)], and the results were adjusted for the youth's age, ethnicity, region of origin and income using multivariable logistic regressions. Moreover, considering that there was a high prevalence of chronic diseases in the non-diabetes group, a sensitivity analysis with a healthy control group was performed, including only the participants in the non-diabetes group who did not report chronic diseases. Finally, subgroup analyses are presented as OR and their respective 95% CI and represent the likelihood of subgroups of interest present diabetes-specific emotional burden. An alpha value < 0.05 was used to determine statistical significance.
Ethics approval and consent participate
The study was done in accordance with the Helsinki Declaration, 2004, and performed in accordance with all relevant guidelines and regulations. The project was approved by the research ethics committee of the main researcher's institution (number 4.045.411). All patients included in the study agreed to the informed consent form available on the online platform before completing the questionnaire.
Results
Characteristics of the participants
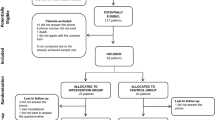
A total of 1011 responses to the online questionnaire were collected: 485 from those responsible for children and adolescents with diabetes (diabetes group) and 526 from those responsible for children and adolescents without diabetes (non-diabetes group). After excluding participants who did not agree with the informed consent, did not meet the inclusion criteria or completed less than 75% of the questionnaire, 381 participants in the diabetes group and 383 in the non-diabetes group were included in the analyses (see supplementary Fig. 1).
Overall, the participants included in the study had a mean age of 39.9 ± 8.5 years; 95.2% were female, 78.3% were white and 47.8% had medium–low family income. Regarding the relationship with the child, 89.1% were mothers, either biological or adoptive. The diabetes and non-diabetes groups did not differ in relation to the participants' age, sex, and relationship with the child. There was a higher prevalence of non-white and low-income participants in the diabetes group (31.2% vs. 12.3%, P < 0.001 and 54.1% vs. 41.5%, P = 0.001, respectively) (see Table 1). Representatives from all regions of Brazil were included, although a high proportion of participants in both groups were from the South-Southeast regions (79.0% in diabetes group and 97.4% in non-diabetes group).
Children and adolescents in the diabetes group were older (11.8 ± 4.3 vs. 8.1 ± 4.7 years, P < 0.001); 28.5% of the participants in the non-diabetes group reported the presence of a chronic illness in the child. Among these participants, 83 had respiratory tract diseases (asthma, bronchitis, cystic fibrosis or rhinitis requiring continuous treatment), 3 had congenital heart disease, 7 had neuro-psychiatric diseases (autism spectrum disorder, attention deficit and hyperactivity or anxiety in need of pharmacological treatment), 1 had epilepsy, 1 polycystic kidney disease, 1 lactose intolerance, 1 deafness and 1 cerebral palsy. Of these, 15.1% used medication daily.
Support, relationships, and consequences of social distancing
Considering the social-demographic differences between the two groups, the OR for the characteristics evaluated in the psychosocial profile were adjusted for age of the child, race/ethnicity, income, and region of origin. Participants in the diabetes group more frequently reported unsatisfactory relationships (18.0% vs. 9.4%, adjusted OR 1.90; 95% CI, 1.16 to 3.12) and regarding family atmosphere, the diabetes group more frequently reported the atmosphere as not-welcoming (8.0% vs. 1.3%, adjusted OR 5.85; 95% CI, 2.09 to 16.43). In addition, a greater purchasing difficulty (38.7% vs. 10.8%, adjusted OR 4.65; 95% CI, 2.93 to 7.38) and a greater difficulty in getting medical assistance when necessary during the pandemic (44.2% vs. 18.5%, adjusted OR 3.36; 95% CI, 2.27 to 4.97) were reported by the diabetes group compared to non-diabetes group. Aspects related to the social distancing, the child being at home full time and reduced family income during the pandemic did not differ between groups (see Table 2). When the evaluation was carried out comparing only to healthy controls, there was no difference between the groups regarding the maintenance of unsatisfactory relationships, but the diabetes group more frequently reported the family atmosphere as not-welcoming (8.0% vs. 0.4%, adjusted OR 17.39; 95% CI, 2.24 to 134.99). There were few differences in the other parameters (see supplementary Table 2).
Pandemic-related emotional burden
The emotional burden evaluation during the COVID-19 pandemic was performed in four domains. Participants in the diabetes group most often expressed personal concern (84.4% vs. 78.3%, P = 0.041), child-related concern (92.6% vs 86.0%, P = 0.005), personal emotional burden (78.2% vs 65.3%, P < 0.001) and child-related emotional burden (75.2% vs. 57.1%, P < 0.001) when compared to the non-diabetes group (see Fig. 1).
The evaluation of pandemic-related emotional burden between the diabetes group and the non-diabetes group was performed in four domains using the Likert scale of 5 points of agreement. The domains were evaluated through the statements: (1) personal concern—“I often feel worried and afraid of being infected with the coronavirus”; (2) concern related to the child—“I often feel worried and afraid that my child may be infected with the coronavirus”; (3) personal emotional burden: “I often feel tired and exhausted due to the change in routine since the social distancing started due to the COVID-19 pandemic”; (4) child-related emotional burden: “I often feel tired and exhausted from the responsibility to protect my child during the COVID-19 pandemic”. It was considered “totally agree” and “agree” as an affirmative answer.The graphs show the percentages of people with affirmative answers to the proposed statements in each group. *P = 0.041; **P = 0.005; ***P < 0.001.
When adjusted by the age of the child, race/ethnicity, region of origin and income, the diabetes group maintained a greater likelihood of personal concern (OR 1.62; 95% CI, 1.01 to 2.58), a greater likelihood of concern for the child (OR 2.01; 95% CI, 1.11 to 3.64), a greater likelihood of personal emotional burden (OR 1.67; 95% CI, 1.10 to 2.53) and a greater likelihood of burden related to childcare (OR 2.28; 95% CI, 1.54 to 3.38).
A sensitivity analysis, adjusted by the same factors and excluding caregivers of youth with chronic disease in the non-diabetes group, was performed. The diabetes group maintained a greater likelihood of personal concern (OR 1.64; 95% CI, 1.02 to 2.64), a greater likelihood of concern for the child (OR 2.49; 95% CI, 1.35 to 4.59), a greater likelihood of personal emotional burden (OR 2.15; 95% CI, 1.41 to 3.27) and a greater likelihood of burden related to childcare (OR 2.62; 95% CI, 1.74 to 3.92) (see Supplementary Fig. 2).
Mental health during social distancing
The presence of a positive screening for mental health disorders was found in 50.3% of the participants in the non-diabetes group and in 69.0% of the participants in the diabetes group (P < 0.001 for the difference between groups). When adjusted for the age of the child, race/ethnicity, income and region of origin, the diabetes group was found to have a significantly higher likelihood of positive screening for mental health disorders when compared to the non-diabetes group (OR 2.43; 95% CI, 1.70 to 3.47).
A sensitivity analysis, adjusted by the same factors and excluding caregivers of youth with chronic disease in the non-diabetes group, was performed. The diabetes group maintained a significantly higher likelihood of positive screening for mental health disorders when compared to the healthy control group (OR 2.68; 95% CI, 1.82 to 3.96) (see Supplementary Table 2).
Diabetes-specific emotional burden related to diabetes care
In the diabetes group, the diabetes-specific emotional burden related to the care of a child/adolescent with diabetes was evaluated in five domains: 40.6% reported discontent in care sharing, 36.0% reported discontent in support, 41.8% reported discontent in appreciation, 48.3% reported exhaustion and 75.7% reported guilt problems (see Fig. 2).
The evaluation of diabetes-specific emotional burden related to diabetes care was performed using the Likert scale of 5 points of agreement. The domains were evaluated through the statements: (1) sharing of care: “I feel frustrated because I am the only one responsible for helping my child use medications and manage glycemic control.”; (2) support: “I feel frustrated with the lack of understanding and support I get from friends and family in relation to taking care of someone with diabetes.”; (3) appreciation: “I feel underestimated for all the effort I put into helping my child to take care of diabetes.”; (4) exhaustion: “I feel that my child's diabetes is consuming a lot of my physical and mental energy every day.”; (5) guilt: "I feel guilty if my child's diabetes is not well controlled." It was considered that it is a problem if the answer was “totally agree” and “agree”, and it is not a problem if the answer was "strongly disagree" or "disagree".
An exploratory analysis of subgroups was performed to identify the likelihood of emotional burden related to care of a child/adolescent with diabetes in certain interest groups. The presence of unsatisfactory relationships and family environment that is not welcoming were predictors of having a greater likelihood of reporting emotional burden related to care sharing, support, appreciation, and exhaustion in diabetes care, while the presence of a positive screening for mental health disorders was a predictor for burden in all areas of diabetes care evaluated (see Table 3).
The impact of the pandemic on different age groups
For the assessment of psychosocial profile and consequences of social distancing on different age groups, the results were adjusted for age of the child, race/ethnicity, income, and region of origin. When considering the different age range, the group of caregivers of youth aged 6 to 12 years with type 1 diabetes most often had unsatisfactory relationships (OR 7.86; 95% CI, 3.59 to 17.22) and had a not-welcoming family atmosphere (OR 5.98; 95% CI, 1.27 to 28.06) in comparison to the non-diabetes group. There was no difference in these aspects in the other age groups. In addition, in all age ranges, caregivers of youth with diabetes had a greater likelihood of having difficulty purchasing during the pandemic. In those aged between 6 and 12 years and those older than 12 years there was a greater likelihood of presenting greater difficulty in getting medical assistance when necessary (OR 3.84; 95% CI, 2.12 to 6.94 and OR 3.69; 95% CI, 1.76 to 7.71, respectively) (see supplementary Table 3).
The emotional burden evaluation on different age ranges was also performed in four domains and adjusted for confounders. The two groups were similar in all domains when the dependent youth was younger than 6 years. On the other hand, there was an increase in likelihood to present child-related concerns (OR 3.19; 95% CI, 1.23 to 8.27 and OR 3.26; 95% CI, 1.22 to 8.71), personal emotional burden (OR 2.05; 95% CI, 1.17 to 3.58 and OR 2.61; 95% CI, 1.34 to 5.10) and child-related emotional burden (OR 2.79; 95% CI, 1.62 to 4.82 and OR 2.56; 95% CI, 1.35 to 4.82) among caregivers of youth with type 1 diabetes aged 6 to 12 years and older than 12 years, respectively (see supplementary Fig. 3).
Regarding mental health disorders, the diabetes group showed greater likelihood of presenting disorders in those aged under 6 years old (OR 2.92; 95% CI, 1.08 to 7.94) and in those aged between 6 and 12 years old (OR 2.89; 95% CI, 1.73 to 4.84). There was no difference between groups in caregivers of adolescents older than 12 years (see supplementary Table 3).
Discussion
Caring for the mental well-being of people responsible for the care of children and adolescents with diabetes has been undervalued. This study was the first to evaluate the psychological impact of routine changes and disease demands on caregivers of children and adolescents with diabetes during the COVID-19 pandemic. When compared to those responsible for children without diabetes, caregivers of children and adolescents with diabetes more often expressed feelings of concern and burden during social distancing. These participants, even when adjusted for potential confounders, had a 60% higher likelihood of presenting feelings of personal concern and burden and up to twice the likelihood of having feelings of concern and burden related to caring for their child during the pandemic. The care of children and adolescents with diabetes has also been associated with a higher likelihood of having a positive screening for mental health disorders during the social distancing period. Moreover, considering the diabetes group, about 3 out of 4 participants reported feeling guilty when the glycemic control of the dependents was not adequate, almost half reported experiencing feelings of exhaustion related to the care of these children and more than a third reported discontent in sharing care, support from family members and appreciation for their dedicated efforts.
The presence of concern, stress and anxiety in relation to glycemic control are part of the routine of the most caregivers of children with diabetes, and behavioral changes during the COVID-19 pandemic seem to enhance this situation16. Participants in the diabetes group more frequently reported the presence of feelings of concern and emotional burden, both personal and related to child care. The longer time at home related to the suspension of non-essential activities may result in an increased demand for those responsible for children with diabetes. Moreover, these individuals are required to coordinate insulin administration and the maintenance of a balanced diet full time.
In our study, those responsible for children and adolescents with diabetes had a higher likelihood of a positive screening for mental health disorders during the social distancing period compared to the non-diabetes group. Previous work has shown that the prevalence of symptoms of depression in the parents of children with newly diagnosed diabetes can reach 74% and, in about 20% of these parents, the symptoms remain for four years after diagnosis6,17. The presence of a potentially fatal pandemic may work as a trigger for the manifestation of latent anxiety and depression symptoms. Caregivers with depressive symptoms may perceive the complexities of diabetes and the challenges associated with its treatment as more negative and distressing, and may lack the necessary coping skills to manage this distress18,19,20. In addition, studies have found depressive symptoms in parents are associated with lower parental involvement, lower family adaptability and higher family conflict, which corroborates the relationships found in the present study6,21,22,23.
Regarding diabetes care during the pandemic, those responsible for this group tended to have a higher prevalence of diabetes-specific emotional burden in different domains related to the demands of the disease. Whittemore et al. found, in a review of studies focused on parents of children with diabetes in usual situations, that those individuals experience considerable stress related to the demands of treatment management. They found that the prevalence of parental psychological distress ranged from 20 to 30% in different studies and, in most of these studies, parents of children with diabetes were found to experience greater distress and problems with parenting than other parents, which may negatively affect their children6. It is difficult to say, based on our study data, how much of the burden found is due to the pandemic and how much is due to the basic conditions of the family members, which may already be weakened. It is possible to imagine, however, that the increase in demands related to social distancing and the anxiogenic context experienced may have contributed to the high levels of diabetes-specific emotional burden reported.
In our study, we chose to use the SRQ-20 questionnaire to assess the prevalence of mental health disorders in caregivers. The choice of this questionnaire was based especially on the wide range of psychiatric disorders assessed (minor disorders) compared to other mental health scores. Other commonly used options, such as the Hospital Anxiety and Depression Scale (HADS) and the Patient Health Questionnaire-9 (PHQ 9), could not be used24,25. The first because its validation for the Brazilian population was performed in hospitalized patients and the second because the evaluation is restricted to depressive disorders alone. All of them have been validated for self-application.
It is necessary to highlight some limitations of the present study. Considering that it is a cross-sectional study, it is not possible to establish cause and effect relationships using the identified associations; reverse causality may occur. The unavailability of validated and translated questionnaires to evaluate anxiety diabetes-specific distress in caregivers has limited the use of these tools in our population. In addition, given that this was an online survey, the results depend on the commitment of the participants and on the veracity of the information provided, which may constitute potential information bias. The dissemination of the questionnaire to the non-diabetes group through medical student leagues may also have selected families with the sickest children in this group and may not be a representative sample of the general population. Regarding the participants sample, although both questionnaires were released at the national level, the diabetes group had a greater representation of different regions of the country. Most participants are from the South and Southeast regions of the country, which limits the generalization of the results. The non-diabetes group also showed less ethnic diversity and greater purchasing power, which may be related to the greater representation of states in Southern Brazil. Although all analyses have been adjusted for the region of origin, purchasing power, youth’s age and ethnicity, these differences in baseline characteristics between groups may reflect a sample bias related to the study design and constitute a limitation of the manuscript. Adjusted analyses for age of the child, skin color, income and region of origin were performed to minimize the effect of these differences. Another aspect that should be highlighted is the high representativeness of female caregivers, which can reduce the validity of the results for male representatives. This high prevalence is in line with other studies conducted in pediatric outpatient care in Brazil, in which the mother plays the role of primary caregiver in 91.0 to 93.7% of cases26,27. Finally, it is necessary to highlight the possibility of selection bias among the participants because family members who are more engaged in childcare may be more interested in participating in the research.
Despite the limitations presented, our study should call attention to mental health and to the diabetes-specific emotional burden related to diabetes care during the pandemic. The evidence found suggests that situations of vulnerability and public calamity may enhance symptoms of concern, burden and mental health disorders in some caregivers of children and adolescents with diabetes, and studies comparing the time periods prior to and after the pandemic should be carried out to better understand this relationship. These results also reveal that additional studies are necessary to understand the burden that these families may be experiencing during the current scenario and to develop new strategies to support these caregivers, especially during the pandemic. The "caregivers and children" binomial approach is fundamental for treating the child's diabetes, and for taking care of the well-being and quality of life of everyone involved.
Data availability
The data collected for the study, including deidentified participant data, will be available for 1 year after publication of the article upon justified request to the e-mail address of the main researcher and with a signed data access agreement.
References
Harrington, K. R. et al. Management and family burdens endorsed by parents of youth <7 years old with type 1 diabetes. J. Diabetes Sci. Technol. 5, 980–987 (2017).
Commissariat, P. V. et al. “I’m essentially his pancreas”: Parent perceptions of diabetes burden and opportunities to reduce burden in the care of children <8 years old with type 1 diabetes. Pediatr. Diabetes 21, 377–383 (2020).
Yang, J. et al. Prevalence of comorbidities and its effects in coronavirus disease 2019 patients: a systematic review and meta-analysis. Int. J. Infect. Dis. 94, 91–95 (2020).
An, R. Projecting the impact of the coronavirus disease-2019 pandemic on childhood obesity in the United States: a microsimulation model. J. Sport Heal. Sci. 4, 302–312 (2020).
Rumburg, T. M., Lord, J. H., Savin, K. L. & Jaser, S. S. Maternal diabetes distress is linked to maternal depressive symptoms and adolescents’ glycemic control. Pediatr. Diabetes. 1, 67–70 (2017).
Whittemore, R., Jaser, S., Chao, A., Jang, M. & Grey, M. Psychological experience of parents of children with type 1 diabetes: a systematic mixed-studies review. Diabetes Educ. 4, 562–579 (2012).
Butler, D. A. et al. The impact of modifiable family factors on glycemic control among youth with type 1 diabetes. Pediatr. Diabetes. 4, 373–381 (2008).
Anderson, B., Ho, J., Brackett, J., Finkelstein, D. & Laffel, L. Parental involvement in diabetes management tasks: relationships to blood glucose monitoring adherence and metabolic control in young adolescents with insulin-dependent diabetes mellitus. J. Pediatr. 2, 257–265 (1997).
Laffel, L. M. B. et al. Impact of ambulatory, family-focused teamwork intervention on glycemic control in youth with type 1 diabetes. J. Pediatr. 4, 409–416 (2003).
Anderson, B. J. et al. Family conflict, adherence, and glycaemic control in youth with short duration type 1 diabetes. Diabet. Med. 6, 480–485 (2002).
Cameron, E. E. et al. Maternal psychological distress and mental health service use during the COVID-19 pandemic. J. Affect. Disord. 276, 765–774 (2020).
von Elm, E. et al. The strengthening the reporting of observational studies in epidemiology (STROBE) statement: Guidelines for reporting observational studies. Int. J. Surg. 4, 344–349 (2014).
Gonçalves, D. M., Stein, A. T. & Kapczinski, F. Avaliação de desempenho do Self-Reporting Questionnaire como instrumento de rastreamento psiquiátrico: Um estudo comparativo com o Structured Clinical Interview for DSM-IV-TR. Cad. Saude Publica. 2, 380–390 (2008).
Krejcie, R. V. & Morgan, D. W. Determining sample size for research activities. Educ. Psychol. Meas. 3, 607–610 (1970).
Patterson, C. C. et al. Worldwide estimates of incidence, prevalence and mortality of type 1 diabetes in children and adolescents: results from the International Diabetes Federation Diabetes Atlas. Diabetes Res. Clin. Pract. 157, 107842 (2019).
Bowes, S., Lowes, L., Warner, J. & Gregory, J. W. Chronic sorrow in parents of children with type 1 diabetes. J. Adv. Nurs. 5, 992–1000 (2009).
Streisand, R. et al. Parental anxiety and depression associated with caring for a child newly diagnosed with type 1 diabetes: Opportunities for education and counseling. Patient Educ. Couns. 2, 333–338 (2008).
Beck, A. T. The evolution of the cognitive model of depression and its neurobiological correlates. Am. J. Psychiatry 8, 969–977 (2008).
Luyckx, K., Vanhalst, J., Seiffge-Krenke, I. & Weets, I. A typology of coping with Type 1 diabetes in emerging adulthood: associations with demographic, psychological, and clinical parameters. J. Behav. Med. 3, 228–238 (2010).
Noser, A. E. et al. Parental depression and diabetes-specific distress after the onset of type 1 diabetes in children. Heal. Psychol. 2, 103–112 (2019).
Jaser, S. S. & Grey, M. A pilot study of observed parenting and adjustment in adolescents with type 1 diabetes and their mothers. J. Pediatr. Psychol. 7, 738–747 (2010).
Jaser, S. S., Whittemore, R., Ambrosino, J. M., Lindemann, E. & Grey, M. Mediators of depressive symptoms in children with type 1 diabetes and their mothers. J. Pediatr. Psychol. 5, 509–519 (2008).
Eckshtain, D., Ellis, D. A., Kolmodin, K. & Naar-King, S. The effects of parental depression and parenting practices on depressive symptoms and metabolic control in urban youth with insulin dependent diabetes. J. Pediatr. Psychol. 4, 426–435 (2010).
De Lima Osório, F., Vilela Mendes, A., Crippa, J. A. & Loureiro, S. R. Study of the discriminative validity of the phq-9 and phq-2 in a sample of brazilian women in the context of primary health care. Perspect. Psychiatr. Care 3, 216–227 (2009).
Botega, N. J., Bio, M. R., Zomignani, M. A., Garcia, C. Jr. & Pereira, W. A. B. Transtornos do humor em enfermaria de clínica médica e validação de escala de medida (HAD) de ansiedade e depressão. Rev. Saude Publica 5, 359–363 (1995).
Barreta, C., de Oliveira, M. A. M., Dias, A. M. & Chesani, F. H. Caracterização dos cuidadores das crianças e dos adolescentes atendidos pelo projeto de extensão de um hospital universitário infantil. Rev. Bras. Tecnol. Sociais 3, 10–15 (2016).
Bertini, G. S. Sobrecarga dos cuidadores informais de pacientes de um serviço de atenção domiciliar - Ribeirão Preto. Dissertação de Mestrado 1, 22–101 (2016).
Acknowledgements
This study received financial support from the National Institute of Science and Technology for Health Technology Assessment (IATS)—CNPq/Brazil (Project: 465518/2014-1). This work was conducted with support from Hospital de Clínicas de Porto Alegre, Programa de Pós Graduação em Ciências Médicas em Endocrinologia da Universidade Federal do Rio Grande do Sul, Faculdade de Medicina da Pontifícia Universidade Católica do Rio Grande do Sul and Hospital São Lucas da Pontifícia Universidade Católica do Rio Grande do Sul.
Author information
Authors and Affiliations
Contributions
J.A. Conceptualization, Methodology, Software, Data curation, Writing—Original draft preparation. G.B.O., G.F. Methodology, Investigation. B.D.S. Supervision, Writing—Reviewing and Editing. G.H.T. Conceptualization, Data curation, Writing—Original draft preparation. Supervision. J.A. is the guarantor of this work and, as such, had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. All authors have reviewed the final version of the manuscript and agreed with the publication of the results presented.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Alessi, J., de Oliveira, G.B., Feiden, G. et al. Caring for caregivers: the impact of the COVID-19 pandemic on those responsible for children and adolescents with type 1 diabetes. Sci Rep 11, 6812 (2021). https://doi.org/10.1038/s41598-021-85874-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-021-85874-3
This article is cited by
-
A prospective analysis of the long-term impact of the COVID-19 pandemic on well-being and health care among children with a chronic condition and their families: a study protocol of the KICK-COVID study
BMC Pediatrics (2023)
-
Exploring the experience of family caregivers of children with medical complexity during COVID-19: a qualitative study
BMC Pediatrics (2023)
-
Eating Problems in Youths with Type 1 Diabetes During and After Lockdown in Italy: An 8-Month Follow-Up Study
Journal of Clinical Psychology in Medical Settings (2023)
-
A systematic review of the international evolution of online mental health strategies and recommendations during the COVID-19 pandemic
BMC Psychiatry (2022)
-
Impact of the COVID-19 pandemic on the kidney community: lessons learned and future directions
Nature Reviews Nephrology (2022)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.