Abstract
The purpose of the present study is to examine the association between toddlers' sleep arrangements and their nighttime sleep duration and other sleep variables. For this investigation, we performed a study in which child activity and sleep levels were recorded using actigraphy. The parents of 1.5-year-old toddlers (n = 106) were asked to attach an actigraphy unit to their child’s waist with an adjustable elastic belt and complete a sleep diary for 7 consecutive days. Questionnaires were used to assess the sleep arrangements of the toddlers. There was a significant negative correlation between nap duration and nighttime sleep duration, suggesting that longer nap sleep induces shorter nighttime sleep duration. Among the sleep arrangements, such as nighttime breastfeeding or co-sleeping, only nighttime breastfeeding predicted shorter nighttime sleep duration. Our findings indicate that shorter naps induce a longer nighttime sleep in 1.5-year-old toddlers while nighttime breastfeeding decreases their nighttime sleep duration.
Similar content being viewed by others
Introduction
Young children experience marked changes in the amount and distribution of nap and nighttime sleep during the first five years of life, in which the frequency of daytime naps decreases and the biphasic sleep–wake pattern gradually disappears to move to a consolidated nighttime sleep like in adults1,2,3,4,5. Sleep problems are commonly found in toddlers, with prevalence estimates of 25% among children across the world6,7. Previous research indicates that sleep arrangements are a strong predictive factor for toddler's sleep problems. For instance, co-sleeping was demonstrated to be associated with persistent child night wakings and bedtime struggles2,8,9,10 and also infants' poor sleep quality10,11,12, according to reports by mothers. In another recent study, falling asleep independently was associated with longer nighttime sleep duration and fewer night wakings, whereas other sleep arrangements, such as co-sleeping or room-sharing, were not13. Another previous study on mother-infant dyads with 3 to 18-month-old children demonstrated that, in comparison to solitary sleep, room-sharing is associated with more objective sleep disturbances in mothers but hardly any in infants13,14. In addition, breastfeeding has been found to be associated with more nocturnal wakings15, but has not been found to be linked to shorter nighttime sleep duration in children13. However, despite the extensive number of studies performed to date, the best sleep arrangements for toddlers is still a much debated issue16.
In a recent study, we investigated the sleep properties of young toddlers approximately 1.5 years of age and reported that nap duration controls the distribution ratio between nap and nighttime sleep17. In the same study, however, we did not examine whether sleep arrangements such as co-sleeping or nighttime breastfeeding influence nighttime sleep. In the current study, to gain an answer to this question, we examined the relationship between the sleep properties and sleep arrangements of 106 toddlers who had been born mature (full term toddlers). Unlike the previous report14, our current study includes data on co-sleeping with parents, which has been less reported in western sleep culture, where bed-sharing is not as common as in Asian countries18. Questionnaires to parents were used to assess the sleep arrangements of the toddlers. This is the first actigraphic study to examine the effects of co-sleeping and/or nighttime breastfeeding on the nighttime sleep of toddlers approximately 1.5 years of age—an age at which a regular child health examination is performed nationwide in Japan.
Results
Sleep properties of the toddlers
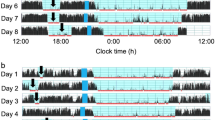
The characteristics of the 106 toddlers are demonstrated in Table 1. The toddlers’ sleep arrangements are shown in Table 2. The toddlers’ sleep variables such as bedtime, wake time, nighttime sleep duration, and nap duration are shown in Table 3. No differences were found between boys and girls in any of the sleep variables (t-test, p > 0.05). Figure 1 shows the representative daily activity-rest patterns of the approximately 1.5-year-old toddlers, indicating the existence of various nap patterns among the toddlers. A significant negative correlation between nap duration and nighttime sleep duration was found (r = − 0.323, p = 0.001), suggesting that longer nap duration induces shorter nighttime sleep duration (Fig. 2a), as we previously reported17. Also, unlike our previous report, no significant correlation was observed between nap end time and nighttime sleep duration (Fig. 2b). In addition, we found a significant correlation between nap onset time and nighttime sleep duration (r = 0.237, p = 0.015), which indicates that earlier nap onset time leads to shorter nighttime sleep duration (Fig. 2c). This correlation between nap onset time and nighttime sleep duration may be affected by the negative correlation between nap onset time and nap duration (r = − 0.362, p = 0.0001), suggesting that earlier nap onset induces longer nap duration which in turn leads to shorter nighttime sleep duration (Fig. 3). To confirm this assumption, we also performed mediation analysis to examine the relationship between nap onset time and nighttime sleep duration mediated by nap duration. As Supplementary Figure 1 illustrates, the standardized regression coefficients between nap onset time and nap duration (a = −0.362, p < 0.001), nap duration and nighttime sleep duration (b = −0.237, p = 0.007), and nap onset time and nighttime sleep duration (c = 0.237, p = 0.015) were statistically significant. Mediation analysis also demonstrated that the indirect effect of the relationship between nap onset time and nighttime sleep duration via nap duration was significant (a x b = 0.099, p = 0.023). However, the direct effect in the absence of the mediator was not significant (c’ = 0.138, p = 0.192). The results showed that shorter nighttime sleep duration in infants with earlier nap onset time was induced by longer nap duration.
The actograms show representative daily activity-rest patterns of toddlers of approximately 1.5 years of age with early nap onset times and long nap duration (a) and late nap onset times and short nap duration (b). The vertical axis shows the 7 consecutive observation days and the horizontal axis shows the course of each 24 h day from 9:00 h (9:00 am). Activity counts per minute are represented by the height of the vertical black bars on each actogram. The red arrows and the blue rectangles indicate naps and bathing periods, respectively. The red underlines are the periods that were automatically judged as sleep periods by the actigraph software. Note that the nap onset times are recognized as relatively early in (a) but as late in (b).
Effects of sleep variables and sleep arrangements on toddlers’ nighttime sleep duration
Before logistic analysis, univariate analysis was performed in order to select possible variables associated with nighttime sleep duration (see Table 4). Next, to evaluate factors contributing to the toddlers’ nighttime sleep duration, we performed a logistic analysis for the effects of gender, perinatal conditions, nap variables, nighttime sleep variables, and sleep arrangements on the nighttime sleep duration of the toddlers (Table 5). According to analysis of nighttime sleep duration in model 1, which was adjusted for birth profile characteristics such as birth order, birth weight, and maternal age, no significant odds ratios (ORs) for toddlers with a nighttime sleep duration of ≥ 8.37 h (mean) were found. In model 2, which adds the sleep variables of nap duration, nap onset time, and wake time to model 1, the ORs for toddlers with a nighttime sleep duration of ≥ 8.37 h (mean) were 0.260 (p = 0.005) for nap duration, indicating that longer nap duration is a significant predictor of shorter nighttime sleep duration in toddlers, but failed to find any significant correlations with nap onset time or wake time. In model 3, which adds the sleep arrangement factors of nighttime breastfeeding, “child having own room”, and putting children to sleep with formula to model 2, the ORs for nighttime sleep duration of ≥ 8.37 h (mean) were 0.233 (p = 0.011) for nap duration, 1.717 (p = 0.038) for nap onset time, and 0.110 (p = 0.0001) for nighttime breastfeeding, indicating that longer nap duration, earlier nap onset time, and nighttime breastfeeding are significant predictors of shorter nighttime sleep duration in toddlers. However, there were no significant correlations between nighttime sleep duration and other sleep arrangement factors.
Discussion
The present study makes two significant findings concerning the sleep properties of toddlers at approximately 1.5 years of age. First, the multivariate analysis (Table 5) indicates that nighttime breastfeeding, rather than sleep arrangements, such as co-sleeping, is significantly associated with the nighttime sleep duration of toddlers. This is also in line with a previous actigraphy study by Yoshida et al.19, which found bed-sharing to be associated only with night wakings and not with nighttime sleep duration. However, previous questionnaire studies by Lo et al.20 reported that co-sleeping was associated with shorter nighttime sleep duration. In addition, questionnaire studies by Mindell et al.21 and Yu et al.13 reported that breastfeeding was not associated with nighttime sleep duration. The reason for the discrepancy between these reports and ours could be because our study employed actigraphy for sleep assessment while the conflicting previous studies did not. Actigraphy is generally regarded as superior to maternal reports in estimating child sleep–wake activity22,23, because some mothers tend to underestimate child waking frequencies and durations1 while others tend to overestimate them14,22.
The second significant finding, also from the multivariate analysis (Table 5) and mediation analysis (Supplementary Figure 1), was a possibility that longer nap duration significantly shortens the nighttime sleep duration of toddlers. This finding is consistent with the results from other studies using questionnaires or actigrapy1,5,24,25,26 and also from our own previous actigraphic study17, which all reported that longer nap duration induces shorter nighttime sleep duration. Although the present study is an association study that shows correlation between nighttime sleep duration and the other sleep variables and sleep arrangement factors, we performed mediation analysis to assess the effect of nap duration on the relationship between nap onset time and nighttime sleep duration. As a result, the analysis indicated that the effect of nap onset time on nighttime sleep duration was significantly mediated by nap duration. Therefore, it may be advantageous for caregivers to avoid setting early nap onset time and late nap end time to reduce the length of toddlers' nap duration, which would result in longer nighttime sleep durations. This result differs from what the results of our previous study suggested, that only a later nap end time induces a shorter nighttime sleep17. This discrepancy in results could be due to the difference in statistical analysis between the two studies. Unlike our current study, our previous study17 did not perform a multivariate analysis which included both sleep variables and sleep arrangement factors.
There are three matters concerning the current study that warrant consideration. First, although the sleep habits of toddlers are affected by those of their parents, especially mothers27, the present study did not investigate the sleep habits of the parent themselves. Secondly, the sleep habits of toddlers are also affected by socio-cultural environments, socioeconomics, individual family ethics, income and the educational backgrounds of parents28. The details of these were not obtained in the present study. Thirdly, the present study was an association study and was not able to fully investigate the effect of nap duration because we did not perform an RCT study, which would require exposing children to at least two different nap durations. Such an RCT study would further strengthen the findings of the present study that indicate that daily naps with short periods would contribute to longer nighttime sleep in toddlers of approximately 1.5 years of age.
During their early developmental stages, young toddlers have bi-phasic sleep patterns which include both napping and nighttime sleep. There is still an ongoing debate whether either nap or nighttime sleep is more valuable to achieve proper physical and cognitive development or if only total sleep duration of nap and nighttime sleep is an important factor for healthy child development (total sleep duration itself in this study was significantly associated with sleep arrangement factors such as nighttime breastfeeding and child having own room as shown in Supplementary Table 1 and 2). Several clinical studies have confirmed positive associations between nighttime sleep duration and toddlers’ physical growth and cognitive development, while other studies have not29,30. However, some recent studies have at least reported that daytime naps improve word learning in toddlers of 12, 15 and 16 months of age31,32,33. Previous clinical studies have also demonstrated a positive association between nighttime sleep duration and the cognitive development of toddlers of 10, 11, and 13 months of age34,35. A further study using additional physiological and psychological parameters will be required to obtain appropriate answers regarding sleep issues in child development.
In summary, our findings suggest that duration-controlled naps and the cessation of nighttime breastfeeding can induce a longer nighttime sleep duration in toddlers without the need to stop co-sleeping. Unlike adult’s nighttime sleep, toddlers’ nighttime sleep is significantly affected by their unique developmental sleep-related factors, i.e., daytime naps and nighttime breastfeeding.
Methods
Participants
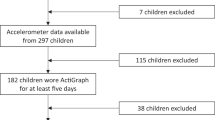
Young toddlers of approximately 1.5 years of age were recruited at the Children’s Clinic of St. Luke’s International Hospital (Tokyo, Japan). Inclusion criteria were as follows: (1) term pregnancy (defined as being born at at least 37 weeks’ gestational age) and (2) the absence of chromosomal or other major genetic abnormalities, suspected neuromuscular disorders or significant chronic lung disease. Exclusion criteria was parental language difficulties. Of 129 eligible toddlers, 23 were excluded because sleep data were invalid due to technical problems with the activity recording devices or incomplete description of sleep diary. The final sample thus consisted of 106 young toddlers (50 boys, 56 girls). The ethics committee of St. Luke’s International Hospital approved the study protocol (UMIN000021153) and all procedures were carried out in accordance with the approved guidelines. Written informed consent was obtained from the parents.
Activity and sleep assessment
Actigraphy
For activity and sleep measurement we used actigraphy, as previously described17. Actigraphy employs a miniature wristwatch-like accelerometer which is attached to the wrist, ankle or waist and continuously records movement for an extended period. The actigraphy device used in the present study was the Actigraph (Micro-mini RC, Ambulatory Monitoring Inc., NY, USA). The parents were asked to attach an Actigraph to their child’s waist with an adjustable elastic belt for 7 consecutive days. Waist attachment was chosen as we found it less disturbing than wrist or ankle attachment. Previous studies have also demonstrated that a minimum of 7 nights was necessary to obtain reliable data36. The actigraphs were removed from the toddlers only for bathing—the average time of which was 29.7 ± 14.2 min.
Motility levels were sampled in the zero-crossing mode in 1-min epochs. The resolution of the Actigraphs was set at 0.01 G/s. The activity data recorded by the Actigraphs was later downloaded using ActMe software (ver. 3.10.0.3, Ambulatory Monitoring Inc.), and then sleep measurements were analyzed with Sadeh’s algorithm37,38, using Action-W software (ver. 2.4.20, Ambulatory Monitoring Inc.).
Sleep diary and questionnaire
Parents were instructed to complete a sleep diary for the 7-day period while their child was wearing the Actigraph. The diary consisted of seven 24-h single-sheet schedules, on which parents were asked to write information such as time of nap, going in/out of bed, bathing and night wakings of which they were aware. At the same time, questionnaires (Supplementary Data 2) given to parents were used to assess the daily sleep arrangements of the toddlers during the same 7-day study period.
The computation of nighttime sleep and nap
The longest sleep period of the day starting after 19:00 was defined as “nighttime sleep”, and all sleep periods of 11 min or more starting before 19:00 were defined as “nap”. Daily nap duration was calculated as the average total nap time per day.
Statistical analysis
Univariate analysis was performed before logistic regression analysis (see Table 4). The degrees of correlation between nighttime sleep duration and gender/birth profiles, sleep variables, and sleep arrangement factors were assessed using the Spearman correlation test. Only variables with relatively significant values (p < 0.2) in the Spearman correlation tests were included in logistic regression analysis. Logistic regression was used to calculate odds ratios (OR) with 95% confidence intervals as estimates of effects, with nighttime sleep duration of toddlers as the outcome variable.
We used 3 models to investigate the effects of gender/birth profiles, sleep variables, and sleep arrangement factors on nighttime sleep duration (see Table 5). Model 1 included gender and perinatal conditions. In model 2, we added the nap variables of nap duration, nap onset time and wake time to model 1. In model 3, we added the sleep arrangement factors of nighttime breastfeeding, putting children to sleep with formula, and “child having own room” to model 2.
Univariate analysis and logistic regression analysis were performed with SPSS Statistics 25.0 (IBM Corp. Armonk, NY, USA). Summary measurements are presented as means ± s.d.s. Spearman correlation was used to assess associations between variables. The gender difference in sleep arrangements and bedtime routine was analyzed using a χ2 test for categorical data and a t-test for continuous data.
We also explored the possible mediating role of nap duration in the relationship between nap onset time and nighttime sleep duration as the outcome. Mediation analysis was conducted using R software 4.0.2 (R Foundation for Statistical Computing, Vienna, Austria, https://www.R-project.org/) with mediation package39. The significance of the direct and indirect (mediation) effects with 95% CI was tested using a non-parametric bootstrapping procedure (10,000 bootstrap samples).
References
Acebo, C. et al. Sleep/wake patterns derived from activity monitoring and maternal report for healthy 1- to 5-year-old children. Sleep 28, 1568–1577 (2005).
Sadeh, A., Mindell, J. A., Luedtke, K. & Wiegand, B. Sleep and sleep ecology in the first 3 years: A web-based study. J. Sleep Res. 18, 60–73. https://doi.org/10.1111/j.1365-2869.2008.00699.x (2009).
Staton, S. et al. Many naps, one nap, none: A systematic review and meta-analysis of napping patterns in children 0–12 years. Sleep Med. Rev. 50, 101247. https://doi.org/10.1016/j.smrv.2019.101247 (2020).
Mindell, J. A. et al. Development of infant and toddler sleep patterns: Real-world data from a mobile application. J. Sleep Res. 25, 508–516. https://doi.org/10.1111/jsr.12414 (2016).
Thorpe, K. et al. Napping, development and health from 0 to 5 years: A systematic review. Arch. Dis. Child. 100, 615–622. https://doi.org/10.1136/archdischild-2014-307241 (2015).
Kohyama, J., Mindell, J. A. & Sadeh, A. Sleep characteristics of young children in Japan: Internet study and comparison with other Asian countries. Pediatr. Int. 53, 649–655. https://doi.org/10.1111/j.1442-200X.2010.03318.x (2011).
Owens, J. A. Sleep in children: Cross-cultural perspectives. Sleep Biol. Rhythms 2, 165–173. https://doi.org/10.1111/j.1479-8425.2004.00147.x (2004).
Mao, A., Burnham, M. M., Goodlin-Jones, B. L., Gaylor, E. E. & Anders, T. F. A comparison of the sleep-wake patterns of cosleeping and solitary-sleeping infants. Child Psychiatry Hum. Dev. 35, 95–105. https://doi.org/10.1007/s10578-004-1879-0 (2004).
Volkovich, E., Ben-Zion, H., Karny, D., Meiri, G. & Tikotzky, L. Sleep patterns of co-sleeping and solitary sleeping infants and mothers: A longitudinal study. Sleep Med. 16, 1305–1312. https://doi.org/10.1016/j.sleep.2015.08.016 (2015).
Shimizu, M. & Teti, D. M. Infant sleeping arrangements, social criticism, and maternal distress in the first year. Infant. Child Dev. https://doi.org/10.1002/icd.2080 (2018).
Sadeh, A., Tikotzky, L. & Scher, A. Parenting and infant sleep. Sleep Med. Rev. 14, 89–96. https://doi.org/10.1016/j.smrv.2009.05.003 (2010).
Touchette, E. et al. Factors associated with fragmented sleep at night across early childhood. Arch. Pediatr. Adolesc. Med. 159, 242–249. https://doi.org/10.1001/archpedi.159.3.242 (2005).
Yu, X. T., Sadeh, A., Lam, H. S., Mindell, J. A. & Li, A. M. Parental behaviors and sleep/wake patterns of infants and toddlers in Hong Kong, China. World J. Pediatr 13, 496–502. https://doi.org/10.1007/s12519-017-0025-6 (2017).
Volkovich, E., Bar-Kalifa, E., Meiri, G. & Tikotzky, L. Mother-infant sleep patterns and parental functioning of room-sharing and solitary-sleeping families: A longitudinal study from 3 to 18 months. Sleep https://doi.org/10.1093/sleep/zsx207 (2018).
Burnham, M. M., Goodlin-Jones, B. L., Gaylor, E. E. & Anders, T. F. Nighttime sleep-wake patterns and self-soothing from birth to one year of age: A longitudinal intervention study. J. Child Psychol. Psychiatry 43, 713–725. https://doi.org/10.1111/1469-7610.00076 (2002).
McKenna, J. J., Ball, H. L. & Gettler, L. T. Mother-infant cosleeping, breastfeeding and sudden infant death syndrome: What biological anthropology has discovered about normal infant sleep and pediatric sleep medicine. Am. J. Phys. Anthropol. Suppl 45, 133–161. https://doi.org/10.1002/ajpa.20736 (2007).
Nakagawa, M. et al. Daytime nap controls toddlers’ nighttime sleep. Sci. Rep. 6, 27246. https://doi.org/10.1038/srep27246 (2016).
Baddock, S. A. et al. The influence of bed-sharing on infant physiology, breastfeeding and behaviour: A systematic review. Sleep Med. Rev. 43, 106–117. https://doi.org/10.1016/j.smrv.2018.10.007 (2019).
Yoshida, M., Shinohara, H. & Kodama, H. Assessment of nocturnal sleep architecture by actigraphy and one-channel electroencephalography in early infancy. Early Hum. Dev. 91, 519–526. https://doi.org/10.1016/j.earlhumdev.2015.06.005 (2015).
Lo, M. J. Relationship between sleep habits and nighttime sleep among healthy preschool children in Taiwan. Ann. Acad. Med. Singap. 45, 549–556 (2016).
Mindell, J. A., Sadeh, A., Kohyama, J. & How, T. H. Parental behaviors and sleep outcomes in infants and toddlers: A cross-cultural comparison. Sleep Med. 11, 393–399. https://doi.org/10.1016/j.sleep.2009.11.011 (2010).
Teti, D. M., Shimizu, M., Crosby, B. & Kim, B. R. Sleep arrangements, parent-infant sleep during the first year, and family functioning. Dev. Psychol. 52, 1169–1181. https://doi.org/10.1037/dev0000148 (2016).
Asaka, Y. & Takada, S. Activity-based assessment of the sleep behaviors of VLBW preterm infants and full-term infants at around 12 months of age. Brain Dev. 32, 150–155. https://doi.org/10.1016/j.braindev.2008.12.006 (2010).
Lam, J. C., Mahone, E. M., Mason, T. & Scharf, S. M. The effects of napping on cognitive function in preschoolers. J. Dev. Behav. Pediatr. 32, 90–97. https://doi.org/10.1097/DBP.0b013e318207ecc7 (2011).
Jones, C. H. & Ball, H. L. Napping in English preschool children and the association with parents’ attitudes. Sleep Med. 14, 352–358. https://doi.org/10.1016/j.sleep.2012.12.010 (2013).
Costanian, C., Abdullah, P., Sawh, N., Nagapatan, A. & Tamim, H. Factors associated with shorter night-time sleep in toddlers: The Survey of Young Canadians. Can. J. Public Health 108, e571–e577. https://doi.org/10.17269/cjph.108.6236 (2018).
Komada, Y. et al. Short sleep duration and irregular bedtime are associated with increased behavioral problems among Japanese preschool-age children. Tohoku J. Exp. Med. 224, 127–136. https://doi.org/10.1620/tjem.224.127 (2011).
Crosby, B., LeBourgeois, M. K. & Harsh, J. Racial differences in reported napping and nocturnal sleep in 2- to 8-year-old children. Pediatrics 115, 225–232. https://doi.org/10.1542/peds.2004-0815D (2005).
Tham, E. K., Schneider, N. & Broekman, B. F. Infant sleep and its relation with cognition and growth: A narrative review. Nat. Sci. Sleep 9, 135–149. https://doi.org/10.2147/NSS.S125992 (2017).
Horváth, K. & Plunkett, K. Spotlight on daytime napping during early childhood. Nat. Sci. Sleep 10, 97–104. https://doi.org/10.2147/NSS.S126252 (2018).
Seehagen, S., Konrad, C., Herbert, J. S. & Schneider, S. Timely sleep facilitates declarative memory consolidation in infants. Proc. Natl. Acad. Sci. USA 112, 1625–1629. https://doi.org/10.1073/pnas.1414000112 (2015).
Gómez, R. L., Bootzin, R. R. & Nadel, L. Naps promote abstraction in language-learning infants. Psychol. Sci. 17, 670–674. https://doi.org/10.1111/j.1467-9280.2006.01764.x (2006).
Horváth, K., Liu, S. & Plunkett, K. A daytime nap facilitates generalization of word meanings in young toddlers. Sleep 39, 203–207. https://doi.org/10.5665/sleep.5348 (2016).
Scher, A. Infant sleep at 10 months of age as a window to cognitive development. Early Hum. Dev. 81, 289–292. https://doi.org/10.1016/j.earlhumdev.2004.07.005 (2005).
Gibson, R. Actigraphic sleep and developmental progress of one-year-old infants. Sleep Biol. Rhythms 10, 77–83. https://doi.org/10.1111/j.1479-8425.2011.00525.x (2012).
Souders, M. C. et al. Sleep behaviors and sleep quality in children with autism spectrum disorders. Sleep 32, 1566–1578 (2009).
Meltzer, L. J., Montgomery-Downs, H. E., Insana, S. P. & Walsh, C. M. Use of actigraphy for assessment in pediatric sleep research. Sleep Med. Rev. 16, 463–475. https://doi.org/10.1016/j.smrv.2011.10.002 (2012).
Schoch, S. F., Kurth, S. & Werner, H. Actigraphy in sleep research with infants and young children: Current practices and future benefits of standardized reporting. J. Sleep Res. https://doi.org/10.1111/jsr.13134 (2020).
Tingley, D., Yamamoto, T., Hirose, K., Keele, L. & Imai, K. mediation: R package for causal mediation analysis. J. Stat. Softw. 59, 1–38. https://doi.org/10.18637/jss.v059.i05 (2014).
Acknowledgements
We thank all the participants and their parents for their generous contributions. This work was supported by Grants-in-Aid for Scientific Research (to H.O. # 26650176, K.C. # 26463369) from the Ministry of Education, Culture, Sports, Science and Technology of Japan and grants (to M.N.) from St. Luke’s Life Science Institute and Public Health Research Foundation.
Author information
Authors and Affiliations
Contributions
M.N., I.K., K.C., H.Y. and H.O. conceived of the study. M.N., I.K., K.C., Y.A., M.T., K.M., M.K., K.K., and H.O. designed the experiments. R.S., T.N., Y.O., M.H., A.A., T.I., Y.Y., Y.M., Y.K., K.M., and M.O. performed and analyzed the experiments. M.N., K.C., Y.A., R.F., and H.O. wrote the paper.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Nakagawa, M., Ohta, H., Shimabukuro, R. et al. Daytime nap and nighttime breastfeeding are associated with toddlers’ nighttime sleep. Sci Rep 11, 3028 (2021). https://doi.org/10.1038/s41598-021-81970-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-021-81970-6
This article is cited by
-
Preterm toddlers have low nighttime sleep quality and high daytime activity
Scientific Reports (2022)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.