Abstract
Antimicrobial peptides (AMPs) are an important part of the human innate immune system for protection against bacterial infections, however the AMPs display varying degrees of activity against Staphylococcus aureus. Previously, we showed that inactivation of the ATP synthase sensitizes S. aureus towards the AMP antibiotic class of polymyxins. Here we wondered if the ATP synthase similarly is needed for tolerance towards various human AMPs, including human β-defensins (hBD1-4), LL-37 and histatin 5. Importantly, we find that the ATP synthase mutant (atpA) is more susceptible to killing by hBD4, hBD2, LL-37 and histatin 5 than wild type cells, while no changes in susceptibility was detected for hBD3 and hBD1. Administration of the ATP synthase inhibitor, resveratrol, sensitizes S. aureus towards hBD4-mediated killing. Neutrophils rely on AMPs and reactive oxygen molecules to eliminate bacteria and the atpA mutant is more susceptible to killing by neutrophils than the WT, even when the oxidative burst is inhibited.These results show that the staphylococcal ATP synthase enhance tolerance of S. aureus towards some human AMPs and this indicates that inhibition of the ATP synthase may be explored as a new therapeutic strategy that sensitizes S. aureus to naturally occurring AMPs of the innate immune system.
Similar content being viewed by others
Introduction
Bacterial pathogens that cause disease in humans remain a serious threat to public health and antibiotics are still our primary weapons in treating many bacterial diseases. The ability to eradicate bacterial infections is however challenged by development of resistance for every type of antibiotic introduced to the clinic1. The majority of the new small molecule antibiotics in clinical development are however inhibiting the same targets as already marketed antibiotics2. As an alternative to small molecule antibiotics, antimicrobial peptides (AMPs) are also explored in clinical trials, however most of the AMPs are only tested for topical applications due to toxicity issues and low metabolic stability3. Here we propose a new strategy to combat bacterial infections, namely to sensitize bacteria to the naturally occurring antimicrobial peptides of the human body and hence boosting the antibacterial capabilities of the innate immune system to eradicate bacterial infections.
Humans are continuously exposed to numerous, and potentially pathogenic, microorganisms, where the innate immune system provides the first line of defense. AMPs constitute an important defense mechanism of the innate immune system against invading microorganisms, due to their antimicrobial and immune stimulatory properties4,5. In humans, several classes of AMPs have been identified, such as α- and β-defensins, the cathelicidin LL-37 and histatins5. The α-defensins consist of six members, which are divided into human neutrophil peptides (HNP1-4) and human α-defensin 5 and 6 (HD5 and HD6). HNP1-4 are highly concentrated in the granules of neutrophils, but are also expressed in monocytes, lymphocytes and natural killer cells. HD5 and HD6 are primarily expressed in Paneth cells of the small intestine4. The β-defensins consist of four members (hBD1-4) and are primarily secreted by mucosal surface epithelia, e.g. by keratinocytes in the human skin6. Histatins comprise a family of cationic, histidine-rich peptides that are present in human saliva and are important for maintaining oral health by limiting infections in the oral cavity5. Several histatins have been characterized, however histatin 5 displays the strongest antimicrobial activity5. LL-37 is an antimicrobial peptide that belongs to the cathelicidin family and is expressed in various epithelial- (e.g. keratinocytes) and immune cells (e.g. neutrophils and macrophages)7. The bactericidal activities of many AMPs have generally been attributed to pore formation in bacterial cytoplasmic membranes, however this mode of action may be too simplistic8,9. The bactericidal activity of hBD3 has for example been associated with lipid II binding, leading to inhibition of cell wall biosynthesis10 and some AMPs also have intracellular targets11. Many antimicrobial peptides display a net positive charge, which is important in the initial electrostatic attraction to negatively charged bacterial phospholipid membranes and negatively charged teichoic acids on the surface of Gram positive bacteria, e.g. Staphylococcus aureus11.
S. aureus is a common colonizer of the human body6, where approximately 30–50% of healthy adults transiently carry this species and approximately 20% are persistently colonized12. The skin, nose and intestinal tract are important ecological niches for S. aureus carriage13. Topical colonization with S. aureus imposes a risk for subsequent infections, if the skin or mucosal barriers are breached and enables transmission of S. aureus cells to the adjacent tissues or the bloodstream12. S. aureus is an opportunistic pathogen that may cause life-threatening diseases, such as sepsis, endocarditis and pneumonia12. Even though keratinocytes express various antimicrobial peptides, such as hBD1-4 and LL-37, S. aureus frequently colonizes human skin6. Among the human β-defensins, only hBD3 displays potent bactericidal activity against S. aureus at physiological conditions14,15,16, and keratinocytes are dependent on hBD3 for killing of S. aureus17. However, it is incompletely understood, why the remaining β-defensins display limited anti-staphylococcal activity. This indicates that sensitizing S. aureus towards the innate immune system AMPs may potentially facilitate eradication of colonizing S. aureus.
Multiple factors affect bacterial susceptibility towards AMPs, such as cell membrane composition, cell surface charge and transmembrane potential8. The positive charge of many AMPs facilitates the interaction with negatively charged bacterial envelopes11. A common resistance mechanism exploited by bacteria is to reduce the net negative charge of the cell envelope, for example by lysinylation of phospholipids18 and D-alanylation of teichoic acids in S. aureus19. Curiously, deficiency of wall teichoic acids selectively confers reduced susceptibility to hBD3, while not affecting susceptibility to LL-37 and HNP1-320. The transmembrane potential affects the ability of cationic AMPs to permeabilize membranes8,21, where an inside-negative transmembrane potential facilitates insertion of some cationic AMPs into bacterial membranes8. Interference with the electron transport chain by inactivation of menaquinone- (men mutants) or hemin (hem mutants) biosynthesis pathways leads to membrane depolarization in S. aureus and in the appearance as small colony variants (SCVs) on agar plates22. Electron transport chain SCVs have been associated with reduced susceptibility towards multiple AMPs, including hBD2-323, thrombin-induced platelet microbicidal protein24 and nisin24. We recently reported that inactivation of genes encoding for multiple subunits of the ATP synthase sensitizes S. aureus towards polymyxins25, a class of cationic AMPs that is used for treatment of Gram-negative infections26. The ATP synthase basically serves two physiological functions, first being synthesis of ATP from ADP and inorganic phosphate by using energy from the proton motive force. Secondly, during conditions with a low proton-motive force the ATP synthase can work in reverse as an ATPase and thereby contributes to the establishment of a cross-membrane proton gradient through ATP hydrolysis27. In S. aureus, the ATP synthase is primarily used to hydrolyze ATP for maintaining the cross-membrane proton gradient both under fermentative and respiratory conditions28. ATP synthase inactivation in S. aureus leads to hyper-polarization of the membrane25,28, which was hypothesized to be the mechanism for sensitizing ATP synthase mutants towards polymyxins25.
Several molecules have been shown to inhibit the ATP synthase in different species29. For example inhibition of the ATP synthase with oligomycin A sensitizes S. aureus towards polymyxin B25 and aminoglycosides30. However, oligomycin A displays similar 50% inhibitory concentration (IC50) between S. aureus and human mitochondrial ATP synthases31, and cannot be used clinically due to toxicity issues32. Resveratrol is a widely used nutraceutical that has been shown to bind to the bovine ATP synthase in the F1-domain33 and also binds reversibly to the ATP synthase in E. coli, partially inhibiting both ATP hydrolysis and ATP synthesis34. Co-administration of resveratrol sensitizes S. aureus towards aminoglycosides30. However, resveratrol is readily metabolized following oral administration, which probably only enables topical use35.
Since ATP synthase inactivation sensitizes S. aureus towards polymyxins, we hypothesize that this strategy also can sensitize S. aureus towards various human AMPs. Potentiation of human AMPs that are currently ineffective against S. aureus may potentially become a new therapeutic strategy, where treatment relies on deprivation of AMP resistance mechanisms and hence boosting of the naturally occurring AMPs of the innate immune system.
Materials and Methods
Bacterial strains, growth conditions and chemicals
The Staphylococcus aureus JE2 wild type (WT) strain and derivative mutants used in this study are highlighted in Table 1. Antimicrobial peptides used in this study included histatin-5 (Innovagen, Sweden), LL-37 (Isca Biochemicals, United Kingdom) and hBD1-4 (Innovagen, Sweden), as well as polymyxin B Etests (bioMérieux, France). We used the ATP synthase inhibitor resveratrol (Santa Cruz Biotechnology). Bacterial strains were routinely cultured at 37 °C in tryptic soy broth (TSB) or on tryptic soy agar (TSA).
Antimicrobial susceptibility assays
Microdilution
The minimum inhibitory concentration for resveratrol was determined using a two-fold broth microdilution assay in TSB (100 µl) with an initial inoculum of approximately 5 × 105 cells/ml. MIC was determined upon incubation at 37 °C for 24 h.
Etest
The MIC for polymyxin B was determined using Etest (bioMérieux, France) in the absence and in the presence of sub-inhibitory concentrations (0.0625x–0.25 × MIC) of resveratrol or menadione (1 µg/ml, Sigma). From overnight cultures, strains were diluted to approximately 108 CFU/ml and then distributed on TSA plates using a sterile cotton swab. MIC was determined upon incubation at 37 °C for 24 h.
Bacterial cell survival assays
From overnight cultures of S. aureus JE2 and mutants, 10 μl was diluted into 990 μl fresh TSB medium in a falcon tube and grown for 2 h for the cells to reach early exponential phase. After 2 h the cultures were re-suspended in 10 mM sodium phosphate buffer (pH 7.4), termed NaPi (Medicago, Sweden). Cells were subsequently diluted in NaPi to approximately 5 × 105 CFU/ml, and combined with antimicrobial peptides and resveratrol when indicated, to a final volume of 100 µl and incubated in 96-well plates with shaking for 2 h at 37 °C. Bacteria were plated for CFU on TSA plates. Following overnight incubation at 37 °C for 24 h, viable cells were enumerated and relative cell survival was calculated as CFUwith peptide/CFUwithout peptide at 2 h post-exposure. Values provided are the mean ± SEM derived from at least three independent biological replicates.
Isolation of PMNs from human blood
Blood was collected from healthy adult volunteers and written informed consent was given. Isolation of neutrophils was performed following the procedure described in36. All methods were carried out in accordance with relevant guidelines and regulations. The institutional review board (IRB) of the University of Tübingen approved the study and all adult subjects provided informed consent. This study was done in accordance with the ethics committee of the medical faculty of the University of Tübingen that approved the study, Approval number 015/2014 BO2. Briefly, heparinized blood was diluted 1:1 (v/v) with PBS containing 0.5% BSA and 2 mM EDTA and layered onto a gradient of Biocoll (density, 1.077 g/ml; Biochrom) and Histopaque (density, 1.119 g/ml; Sigma). After centrifugation for 20 min at 380×g, neutrophils were collected from the Histopaque phase. Cells were subjected to a brief hypotonic shock with ultrapure-water containing 155 mM ammonium chloride, 1 mM potassium hydrogen carbonate and 0.1 mM EDTA at pH 7.4, washed, and suspended at 2.5 × 106 cells/ml in RPMI containing 200 mg/ml HSA, 2 mM glutamine, 2 mM sodium pyruvate and 10 mM HEPES.
Phagocytosis of S. aureus by neutrophils
Starter cultures of S. aureus JE2 and its respective atpA mutant were grown in TSB medium overnight. Main cultures were subsequently inoculated at an OD600 of 0.1 and grown to an OD of 1. 109 CFU of WT and atpA mutant cells were adjusted in PBS, stained with 10 µM carboxyfluorescein succinimidyl ester (CFSE) for 1 h at 37 °C and subsequently washed 3 times with PBS. 108 CFU/ml were opsonized with 10% normal human serum (NHS) in RPMI for 1 h at 37 °C. To check for correct CFUs, the dilution was plated onto TSA agar plates. 2.5 × 106 previously isolated PMNs were seeded in a 96 well round-bottom plate and challenged with opsonized WT and atpA mutant S. aureus JE2 at a MOI of 1. Incubation was performed for 20 min or 1 h at 37 °C. After incubation, the plate was centrifuged at 300×g for 10 min, and the pellet was fixed with 3.7% formaldehyde for 20 min in the dark. The fixed cells were then washed and suspended in PBS. The samples were analyzed with a BD FACSCalibur by measuring 5000 events for each sample.
Killing of S. aureus by neutrophils
Starter cultures of S. aureus JE2 and its respective atpA mutant were grown in TSB medium overnight. Main cultures were subsequently inoculated at an OD600 of 0.1 and grown to an OD of 1. 109 CFU of WT and atpA mutant cells were adjusted in PBS medium, then washed and resuspended in PBS. 108 CFU/ml were opsonized with 10% normal human serum (NHS) in RPMI for 1 h at 37 °C. 2.5 × 106 previously isolated PMNs were seeded in 96 well round-bottom plates and challenged with opsonized WT and atpA mutant S. aureus JE2 at a MOI of 1. Incubation was performed for 1 h at 37 °C in a 96 well round-bottom plate and inoculation controls were included. After incubation, the plate was centrifuged at 300×g for 10 min, the supernatants were collected, and the remaining neutrophil pellets were lysed using cold ddH20 for 10 min on a rocker. The lysed neutrophils and remaining bacteria were resuspended and pooled with the previously collected supernatants. Dilutions of 10–2 were plated on TSA plates with an Eddy Jet 2 W and incubated overnight at 37 °C. Values provided are the mean ± SEM derived from at least seven independent biological replicates.
Statistics
The data were analyzed in GraphPad Prism 7 (GraphPad Software Inc.) using paired t-tests or one-way analysis of variance (ANOVA) with a post hoc analysis of Dunnett’s multiple comparison tests. Log-transformed data was used for bacterial survival. P < 0.05 (*), P < 0.01 (**) and P < 0.001 (***).
Results
ATP synthase mutants are more susceptible to hBD2 and hBD4
Since inactivation of the ATP synthase increases susceptibility of S. aureus towards the antimicrobial peptides, polymyxins25, we wondered if inactivation of the ATP synthase also sensitizes S. aureus towards AMPs of the human innate immune system. Therefore, bacterial killing of the WT S. aureus JE2 and isogenic atpA (ATP synthase subunit alpha) transposon mutant was assessed following 2 h exposure to human cationic AMPs, comprising histatin-5, LL-37 and hBD1-4 at the concentrations highlighted in Fig. 1a. The atpA mutant was more susceptible to hBD4 and hBD2 compared with the WT (Fig. 1a). The atpA mutant displayed a 63-fold greater reduction in viable cells compared with WT upon treatment with hBD4. For hBD2, the atpA mutant displayed a fivefold greater reduction in viable cells compared with WT. A minor increase in bactericidal activity against the atpA mutant was detected for histatin-5 and LL-37, whereas no differences between WT and atpA survival were detected upon treatment with hBD1 nor hBD3.
ATP synthase mutants are more susceptible to specific human AMPs than the WT. (a) The susceptibilities to the different AMPs assayed are presented as the relative survival following 2 h exposure at the indicated AMP concentrations for JE2 (WT) and atpA mutant. (b) Survival of ATP synthase mutants (atpA, atpB and atpG) and menD mutant following 2 h exposure to hBD4 (5 µM). Each survival value provided is the mean ± SEM derived from at least three independent measurements. ★p < 0.05, ★★p < 0.01 and ★★★p < 0.001.
We assessed hBD4-mediated killing of other ATP synthase mutants, namely atpB (ATP synthase subunit A) and atpG (ATP synthase subunit gamma) and both mutants displayed increased susceptibility to hBD4, similarly to the atpA mutant (Fig. 1b).
Since the atpA mutant has a hyperpolarized membrane25, we also assessed hBD4 susceptibility of the menD transposon mutant, which has a depolarized membrane37. The menD mutant was indeed more tolerant to hBD4 compared with WT, as no reduction in viable cell count was observed following 2 h exposure to hBD4 at 5 µM (Fig. 1b), suggesting that the magnitude of the membrane potential is an important determinant for hBD4 susceptibility.
Similarly we observed this correlation between magnitude of membrane potential and polymyxin B susceptibility, where the menD mutant was more resistant towards polymyxin B compared with the WT (Supplementary Table S1). The menD mutant is auxotrophic for menadione and supplementation with the compound re-sensitized the menD mutant to polymyxin B (Supplementary Table S1).
Taken together, inactivation of the ATP synthase sensitizes S. aureus to specific human AMPs and the magnitude of the membrane potential correlates with hBD4 susceptibility. This correlation also applies more broadly to include the non-human AMP, polymyxin B.
The ATP synthase inhibitor resveratrol sensitizes S. aureus towards hBD4
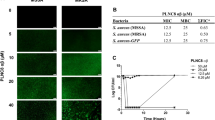
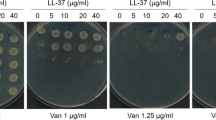
Resveratrol is a putative ATP synthase inhibitor in S. aureus30 and therefore, we assessed if resveratrol could sensitize S. aureus JE2 towards hBD4. Resveratrol has growth-inhibitory properties with a MIC of 256 µg/ml, but at a sub-inhibitory concentration (0.125 × MIC) it had no impact on S. aureus viability (Fig. 2). Importantly, however, when supplemented in combination with hBD4, resveratrol increased killing of WT S. aureus by 20-fold compared with hBD4 alone.
Similarly, supplementation of resveratrol at sub-inhibitory concentrations (0.0625x–0.25 × MIC) sensitized S. aureus JE2 to polymyxin B (Supplementary Table S2).
These result suggests that ATP synthase inhibition with resveratrol may be an attractive approach to sensitize S. aureus towards hBD4.
The atpA mutant is more susceptible to killing by human neutrophils
Log-phase bacteria of the WT and atpA mutant were opsonized with pooled normal human serum, phagocytosed by neutrophils, and subsequently incubated for one hour before determination of surviving cells. The atpA mutant was more susceptible to neutrophil killing than the WT and after one hour of incubation with neutrophils, only 39.2% of the atpA cells survived compared with 49.9% for the WT (P = 0.006) (Fig. 3). The uptake of the strains into the neutrophils was similar (Data not shown), suggesting that the increased killing of the atpA is due to antimicrobial activities of the neutrophils and not due to alterations in phagocytosis rates.
Neutrophil-mediated killing of S. aureus. The percentage of viable opsonized WT and atpA mutant cells following incubation with neutrophils (PMN) for 1 h. Surviving cells are expressed in percentage of the initial counts. Diphenyleneiodonium (DPI) is a NADPH oxidase inhibitor. Each value provided is the mean ± SEM derived from at least seven independent measurements. ★p < 0.05, ★★p < 0.01 and ★★★p < 0.001.
As neutrophils normally use both, oxygen-dependent and non-oxygen-dependent killing mechanisms, including antimicrobial peptides38, we compared survival of atpA and WT in neutrophils treated with the NADPH oxidase inhibitor diphenyleneiodonium (DPI), which suppresses the formation of reactive oxygen species18. Suppression of the oxidative burst limited killing of S. aureus (Fig. 3). After one hour incubation only 74.3% of the atpA cells survived in DPI-treated neutrophils, compared to 91.4% for the WT (P = 0.0196) (Fig. 3). These data suggest that the atpA mutant is more susceptible towards the oxygen-independent antimicrobial activities of neutrophils.
Discussion
Antimicrobial peptides are an important part of the innate immune system and the AMPs display activity against a wide range of bacterial-, fungal- and viral species6. Several human AMPs however display low inhibitory activity against S. aureus14. For example, the human β-defensins 1–4 are produced by keratinocytes and are key in protecting against skin infections6. hBD3 displays greater bactericidal activity against S. aureus than the other β-defensins14,15,16, and hBD3 is important for keratinocytes in killing S. aureus17. Production of AMPs in the skin and in the nasal passages plays a major role in preventing S. aureus persistent colonization and people with defects in hBD3 production have enhanced nasal colonization of S. aureus39. Our results point to a novel type of antimicrobial therapy, whereby the susceptibility of the pathogen is enhanced towards the natural human antimicrobial peptides. Here we demonstrate the potential for S. aureus, but it may be applicable to other human pathogens as well.
The energetic state of bacterial membranes can affect the susceptibility towards AMPs in different bacterial species8 and for some conventional classes of antibiotics as well, i.e. aminoglycosides40. Recently, we demonstrated that ATP synthase mutants of S. aureus become more sensitive towards polymyxins25. ATP synthase inactivation confers hyperpolarization of the membrane25,28 and larger membrane potentials can facilitate AMP insertion into membranes8. In this study, we demonstrate that the activities of certain human AMPs are affected by the magnitude of the membrane potential. ATP synthase mutants have a hyperpolarized membrane25,28 and become more sensitive towards hBD2 and hBD4 and to a minor degree towards LL-37 and histatin-5 (Fig. 1a). Contrarily, a menD mutant with a depolarized membrane is less sensitive towards hBD4 (Fig. 1b).
Our finding that membrane depolarization protects S. aureus from hBD4-mediated killing corroborate previous studies demonstrating that S. aureus SCVs are less susceptible to different AMPs. For S. aureus, electron-transport chain deficient mutants are less susceptible to killing by thrombin-induced PMP-1 (tPMP-1)41, nisin24, lactoferrin B42 and human AMPs, including hBD2, hBD3 and LL-3723. Another study, with genetically defined menD and hemB mutants in different S. aureus genetic backgrounds did however not observe changes in susceptibility to LL-3743. Killing by the human neutrophil defensin 1 (hNP-1) is similar in WT and mutants with impaired electron transport chains24,41,44. These observations indicate that membrane potential changes only affect the activity of specific AMPs.
It has been suggested that membrane depolarization and subsequently increased tolerance towards AMPs of the innate immune system is a survival strategy that enable intracellular persistence of S. aureus in eukaryotic cells45. Here we demonstrate that inactivation of the ATP synthase contrarily sensitizes S. aureus to neutrophil-killing (Fig. 3). The increased susceptibility to neutrophil-killing is also evident when the oxidative burst is suppressed (Fig. 3), suggesting that this effect is mediated by increased susceptibility to AMPs produced by neutrophils38.
It is not only in S. aureus that AMP sensitivity is modulated by the magnitude of the membrane potential. In E. coli, inactivation of the ATP synthase also leads to hyperpolarization of the membrane46 and ATP synthase mutants are more sensitive to colistin47 and aminoglycosides40,47. Deletion of the gene phoP in E. coli conferred hyperpolarization of the membrane and a concomitant increase in activity of polymyxin B, while collapsing the proton gradient with the protonophore carbonyl cyanide m-chlorophenyl hydrazone (CCCP) abrogated this effect48. Dissipation of membrane potential with CCCP also impaired killing of E. coli with the AMP indolicidin49. For Salmonella enterica Typhimurium, impairment of the electron transport chain reduces AMP activity, e.g. a hemB mutant displays a fourfold increase in MIC for colistin50. Even respiration-deficient mutants of the fungus Candida albicans experience reduced sensitivity to histatin-5 and chemical inhibition of the electron transport chain with sodium azide or CCCP treatment also protects C. albicans against histatin-5 killing51,52.
The ATP synthase may potentially be targeted to facilitate killing by AMPs of the innate immune system and hence be essential under in vivo conditions. By employing the Tn-seq methodology, the ATP synthase has been identified in several studies as essential during in vivo conditions, such as in abscess formation or osteomyelitis, while the ATP synthase is dispensable during growth in laboratory medium53,54,55. Recently, Grosser and colleagues demonstrated that an ATP synthase mutant indeed is severely attenuated in a murine skin abscess model28. ATP synthase inactivation confers pleiotropic effects, including attenuated growth under anaerobic conditions, increased sensitivity towards peroxide and nitric oxide stresses28. Whether virulence attenuation of the ATP synthase mutant in the murine skin abscess model is mediated by a single phenotypic trait or a combination thereof remain unexplored in the study28 and here we provide an additional phenotype that may contribute to the attenuated virulence, namely increased sensitivity of S. aureus to different AMPs of the innate immune system.
Inhibition of the ATP synthase may potentially have therapeutic value either as a monotherapy or in combination with AMPs or aminoglycosides. Many ATP synthase inhibitors have been identified29, however several of these, e.g. oligomycin A, are not selective for bacterial ATP synthases and also blocks human mitochondrial ATP synthases31. The ATP synthase has been clinically validated as a druggable target in recent years with the antibiotic bedaquiline that selectively inhibits ATP synthases of Mycobacteria56. We demonstrated that the ATP synthase inhibitor resveratrol, a commonly used nutraceutical57, sensitizes S. aureus towards hBD4 (Fig. 2). Resveratrol has previously been assessed for clearance of acne skin lesions58 and has recently been shown to reduce abscess formation by S. aureus when used as a monotherapy59. It will be important in future animal experiments to elucidate, whether resveratrol in combination with human defensins are superior in treating topical S. aureus infections compared with the respective monotherapies.
It is encouraging that bacterial ATP synthases are sufficiently different from human ATP synthases, which enables identification of selective bacterial ATP synthase inhibitors that are not toxic to human cells32. Selective staphylococcal ATP synthase inhibitors may provide a novel class of antibacterial therapies that is based on sensitizing S. aureus towards the AMPs of the innate immune system. Additionally, such inhibitors can be adjuvants that potentiate the activity of conventional antibiotics, such as aminoglycosides and polymyxins25,30. Several AMPs are in clinical development3, whose activity potentially also can be enhanced by co-administration of ATP synthase inhibitors.
In summary, we have investigated the possibility of sensitizing S. aureus towards human AMPs by targeting the ATP synthase and our results suggest that it may be a novel strategy for development of new antimicrobial therapeutics.
References
Lewis, K. Platforms for antibiotic discovery. Nat. Rev. Drug Discov. 12, 371–387 (2013).
Butler, M. S., Blaskovich, M. A. & Cooper, M. A. Antibiotics in the clinical pipeline at the end of 2015. J. Antibiot. 70, 3–24 (2017).
Mahlapuu, M., Håkansson, J., Ringstad, L. & Björn, C. Antimicrobial peptides: an emerging category of therapeutic agents. Front. Cell. Infect. Microbiol. 6, 194 (2016).
Hancock, R. E., Haney, E. F. & Gill, E. E. The immunology of host defence peptides: beyond antimicrobial activity. Nat. Rev. Immunol. 16, 321 (2016).
De Smet, K. & Contreras, R. Human antimicrobial peptides: defensins, cathelicidins and histatins. Biotech. Lett. 27, 1337–1347 (2005).
Otto, M. Staphylococcus colonization of the skin and antimicrobial peptides. Expert Rev. Dermatol. 5, 183–195 (2010).
Xhindoli, D. et al. The human cathelicidin LL-37—pore-forming antibacterial peptide and host-cell modulator. Biochimica et Biophysica Acta (BBA)-Biomembranes 1858, 546–566 (2016).
Yeaman, M. R. & Yount, N. Y. Mechanisms of antimicrobial peptide action and resistance. Pharmacol. Rev. 55, 27–55 (2003).
Omardien, S., Brul, S. & Zaat, S. A. Antimicrobial activity of cationic antimicrobial peptides against gram-positives: current progress made in understanding the mode of action and the response of bacteria. Front. Cell Dev. Biol. 4, 111 (2016).
Sass, V. et al. Human β-defensin 3 inhibits cell wall biosynthesis in Staphylococci. Infect. Immun. 78, 2793–2800 (2010).
Andersson, D. I., Hughes, D. & Kubicek-Sutherland, J. Z. Mechanisms and consequences of bacterial resistance to antimicrobial peptides. Drug Resist. Updates 26, 43–57 (2016).
Lowy, F. D. Staphylococcus aureus infections. N. Engl. J. Med. 339, 520–532 (1998).
Gordon, R. J. & Lowy, F. D. Pathogenesis of methicillin-resistant Staphylococcus aureus infection. Clin. Infect. Dis. 46, S350–S359 (2008).
Midorikawa, K. et al. Staphylococcus aureus susceptibility to innate antimicrobial peptides, β-defensins and CAP18, expressed by human keratinocytes. Infect. Immun. 71, 3730–3739 (2003).
Chen, X. et al. Synergistic effect of antibacterial agents human β-defensins, cathelicidin LL-37 and lysozyme against Staphylococcus aureus and Escherichia coli. J. Dermatol. Sci. 40, 123–132 (2005).
Kubicek-Sutherland, J. Z. et al. Antimicrobial peptide exposure selects for Staphylococcus aureus resistance to human defence peptides. J. Antimicrob. Chemother. 72, 115–127 (2017).
Kisich, K. O. et al. The constitutive capacity of human keratinocytes to kill Staphylococcus aureus is dependent on β-defensin 3. J. Investig. Dermatol. 127, 2368–2380 (2007).
Peschel, A. et al. Staphylococcus aureus resistance to human defensins and evasion of neutrophil killing via the novel virulence factor MprF is based on modification of membrane lipids with l-lysine. J. Exp. Med. 193, 1067–1076 (2001).
Peschel, A. et al. Inactivation of the dlt operon in Staphylococcus aureus confers sensitivity to defensins, protegrins, and other antimicrobial peptides. J. Biol. Chem. 274, 8405–8410 (1999).
Koprivnjak, T., Weidenmaier, C., Peschel, A. & Weiss, J. P. Wall teichoic acid deficiency in Staphylococcus aureus confers selective resistance to mammalian group IIA phospholipase A2 and human β-defensin 3. Infect. Immun. 76, 2169–2176 (2008).
Kagan, B. L., Selsted, M. E., Ganz, T. & Lehrer, R. I. Antimicrobial defensin peptides form voltage-dependent ion-permeable channels in planar lipid bilayer membranes. Proc. Natl. Acad. Sci. 87, 210–214 (1990).
Proctor, R. A. et al. Small colony variants: a pathogenic form of bacteria that facilitates persistent and recurrent infections. Nat. Rev. Microbiol. 4, 295–305 (2006).
Gläser, R., Becker, K., von Eiff, C., Meyer-Hoffert, U. & Harder, J. Decreased susceptibility of Staphylococcus aureus small-colony variants toward human antimicrobial peptides. J. Investig. Dermatol. 134, 2347–2350 (2014).
Koo, S.-P., Bayer, A. S., Sahl, H.-G., Proctor, R. A. & Yeaman, M. R. Staphylocidal action of thrombin-induced platelet microbicidal protein is not solely dependent on transmembrane potential. Infect. Immun. 64, 1070–1074 (1996).
Vestergaard, M. et al. Inhibition of the ATP Synthase Eliminates the Intrinsic Resistance of Staphylococcus aureus towards Polymyxins. mBio 8, e01114–e01117 (2017).
Zavascki, A. P., Goldani, L. Z., Li, J. & Nation, R. L. Polymyxin B for the treatment of multidrug-resistant pathogens: a critical review. J. Antimicrob. Chemother. 60, 1206–1215 (2007).
Deckers-Hebestreit, G. & Altendorf, K. The F0F1-type ATP synthases of bacteria: structure and function of the F0 complex. Annu. Rev. Microbiol. 50, 791–824 (1996).
Grosser, M. R. et al. Genetic requirements for Staphylococcus aureus nitric oxide resistance and virulence. PLoS Pathog. 14, e1006907 (2018).
Hong, S. & Pedersen, P. L. ATP synthase and the actions of inhibitors utilized to study its roles in human health, disease, and other scientific areas. Microbiol. Mol. Biol. Rev. 72, 590–641 (2008).
Nøhr-Meldgaard, K., Ovsepian, A., Ingmer, H. & Vestergaard, M. Resveratrol enhances the efficacy of aminoglycosides against Staphylococcus aureus. Int. J. Antimicrob. Agents 52, 390–396 (2018).
Balemans, W. et al. Novel antibiotics targeting respiratory ATP synthesis in Gram-positive pathogenic bacteria. Antimicrob. Agents Chemother. 56, 4131–4139 (2012).
Haagsma, A. C. et al. Selectivity of TMC207 towards mycobacterial ATP synthase compared with that towards the eukaryotic homologue. Antimicrob. Agents Chemother. 53, 1290–1292 (2009).
Gledhill, J. R., Montgomery, M. G., Leslie, A. G. & Walker, J. E. Mechanism of inhibition of bovine F1-ATPase by resveratrol and related polyphenols. Proc. Natl. Acad. Sci. 104, 13632–13637 (2007).
Dadi, P. K., Ahmad, M. & Ahmad, Z. Inhibition of ATPase activity of Escherichia coli ATP synthase by polyphenols. Int. J. Biol. Macromol. 45, 72–79 (2009).
Vestergaard, M. & Ingmer, H. Antibacterial and antifungal properties of resveratrol. Int. J. Antimicrob. Agents 53, 716–723 (2019).
Troelstra, A. et al. Dual effects of soluble CD14 on LPS priming of neutrophils. J. Leukoc. Biol. 61, 173–178 (1997).
Vestergaard, M. et al. Novel pathways for ameliorating the fitness cost of gentamicin resistant small colony variants. Front. Microbiol. 7, 1866 (2016).
Amulic, B., Cazalet, C., Hayes, G. L., Metzler, K. D. & Zychlinsky, A. Neutrophil function: from mechanisms to disease. Annu. Rev. Immunol. 30, 459–489 (2012).
Zanger, P., Nurjadi, D., Vath, B. & Kremsner, P. G. Persistent nasal carriage of Staphylococcus aureus is associated with deficient induction of human β-defensin 3 after sterile wounding of healthy skin in vivo. Infect. Immun. 79, 2658–2662 (2011).
Lobritz, M. A. et al. Antibiotic efficacy is linked to bacterial cellular respiration. Proc. Natl. Acad. Sci. 112, 8173–8180 (2015).
Yeaman, M. R., Bayer, A. S., Koo, S.-P., Foss, W. & Sullam, P. M. Platelet microbicidal proteins and neutrophil defensin disrupt the Staphylococcus aureus cytoplasmic membrane by distinct mechanisms of action. J. Clin. Investig. 101, 178–187 (1998).
Samuelsen, Ø et al. Staphylococcus aureus small colony variants are resistant to the antimicrobial peptide lactoferricin B. J. Antimicrob. Chemother. 56, 1126–1129 (2005).
Zhang, P., Wright, J. A., Tymon, A. & Nair, S. P. Bicarbonate induces high-level resistance to the human antimicrobial peptide LL-37 in Staphylococcus aureus small colony variants. J. Antimicrob. Chemother. 73, 615–619 (2017).
Sadowska, B. et al. Characteristics of Staphylococcus aureus isolated from airways of cystic fibrosis patients, and their small colony variants. FEMS Immunol. Med. Microbiol. 32, 191–197 (2002).
Kahl, B. C. Small colony variants (SCVs) of Staphylococcus aureus—a bacterial survival strategy. Infect. Genet. Evolut. 21, 515–522 (2014).
Jensen, P. R. & Michelsen, O. Carbon and energy metabolism of atp mutants of Escherichia coli. J. Bacteriol. 174, 7635–7641 (1992).
Liu, A. et al. Antibiotic sensitivity profiles determined with an Escherichia coli gene knockout collection: generating an antibiotic bar code. Antimicrob. Agents Chemother. 54, 1393–1403 (2010).
Alteri, C. J., Lindner, J. R., Reiss, D. J., Smith, S. N. & Mobley, H. L. The broadly conserved regulator PhoP links pathogen virulence and membrane potential in Escherichia coli. Mol. Microbiol. 82, 145–163 (2011).
Falla, T. J., Karunaratne, D. N. & Hancock, R. E. Mode of action of the antimicrobial peptide indolicidin. J. Biol. Chem. 271, 19298–19303 (1996).
Pränting, M. & Andersson, D. I. Mechanisms and physiological effects of protamine resistance in Salmonella enterica serovar Typhimurium LT2. J. Antimicrob. Chemother. 65, 876–887 (2010).
Gyurko, C., Lendenmann, U., Troxler, R. F. & Oppenheim, F. G. Candida albicans mutants deficient in respiration are resistant to the small cationic salivary antimicrobial peptide histatin 5. Antimicrob. Agents Chemother. 44, 348–354 (2000).
Koshlukova, S. E., Lloyd, T. L., Araujo, M. W. & Edgerton, M. Salivary histatin 5 induces non-lytic release of ATP from Candida albicans leading to cell death. J. Biol. Chem. 274, 18872–18879 (1999).
Ibberson, C. B. et al. Co-infecting microorganisms dramatically alter pathogen gene essentiality during polymicrobial infection. Nat. Microbiol. 2, 17079 (2017).
Wilde, A. D. et al. Bacterial hypoxic responses revealed as critical determinants of the host-pathogen outcome by TnSeq analysis of Staphylococcus aureus invasive infection. PLoS Pathog. 11, e1005341 (2015).
Valentino, M. D. et al. Genes contributing to Staphylococcus aureus fitness in abscess-and infection-related ecologies. MBio 5, e01729-e1714 (2014).
Mahajan, R. Bedaquiline: first FDA-approved tuberculosis drug in 40 years. Int. J. Appl. Basic Med. Res. 3, 1 (2013).
Aschemann-Witzel, J. & Grunert, K. G. Resveratrol food supplements: a survey on the role of individual consumer characteristics in predicting the attitudes and adoption intentions of US American and Danish respondents. BMC Public Health 15, 110 (2015).
Fabbrocini, G. et al. Resveratrol-containing gel for the treatment of acne vulgaris. Am. J. Clin. Dermatol. 12, 133–141 (2011).
Duan, J. et al. Subinhibitory concentrations of resveratrol reduce alpha-hemolysin production in Staphylococcus aureus isolates by downregulating saeRS. Emerg. Microbes Infect. 7, 1–10 (2018).
Fey, P. D. et al. A genetic resource for rapid and comprehensive phenotype screening of nonessential Staphylococcus aureus genes. MBio 4, e00537-e512 (2013).
Acknowledgements
The work is funded by the Danish Research Council for Independent Research, Technology and Production nr. 7017-00079B for HI and by grants from the German Research Foundation (PE 805/5-2, TRR156, and SFB766 [to A. P.] and TRR34 [to D. K. and A. P.]) and the German Center for Infection Research (DZIF) to A.P. and D.K. The authors acknowledge infrastructural support by the Cluster of Excellence EXC2124 Controlling Microbes to fight Infections.
Author information
Authors and Affiliations
Contributions
MV, AP, DK and HI conceived and designed the study. Experiments were performed by MV, LL, KNM and CB. All authors contributed in analysis of data and writing of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Liu, L., Beck, C., Nøhr-Meldgaard, K. et al. Inhibition of the ATP synthase sensitizes Staphylococcus aureus towards human antimicrobial peptides. Sci Rep 10, 11391 (2020). https://doi.org/10.1038/s41598-020-68146-4
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-020-68146-4
This article is cited by
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.