Abstract
The aims of this randomized controlled double-blind clinical trial were to assess the impact of vitamin D supplementation on calcium metabolism and non-calcemic broad gene expression by relating them to the individual’s responsiveness to varying doses of vitamin D3. Thirty healthy adults were randomized to receive 600, 4,000 or 10,000 IU/d of vitamin D3 for 6 months. Circulating parathyroid hormone (PTH), 25(OH)D, calcium and peripheral white blood cells broad gene expression were evaluated. We observed a dose-dependent increase in 25(OH)D concentrations, decreased PTH and no change in serum calcium. A plateau in PTH levels was achieved at 16 weeks in the 4000 and 10,000 IU/d groups. There was a dose-dependent 25(OH)D alteration in broad gene expression with 162, 320 and 1289 genes up- or down-regulated in their white blood cells, respectively. Our results clearly indicated that there is an individual’s responsiveness on broad gene expression to varying doses of vitamin D3. Vitamin D3 supplementation at 10,000 IU/d produced genomic alterations several fold higher than 4,000 IU/d even without further changes in PTH levels. Our findings may help explain why there are some inconsistency in the results of different vitamin D’s clinical trials.
Similar content being viewed by others
Introduction
Vitamin D sufficiency, insufficiency and deficiency are defined as serum levels of 25-hydroxyvitamin D [25(OH)D] as 30–100 ng/mL (75–250 nmol/L), 21–29 ng/mL (51–74 nmol/L) and <20 ng/mL (<50 nmol/L) respectively by the Endocrine Society’s Practice Guidelines on Vitamin D1,2,3. The influence of vitamin D in maintaining skeletal balance is clearly explained1,2,3. In addition to its important role in calcium balance, a long list of acute and chronic medical conditions including cardiovascular disease4, autoimmune diseases5, neurocognitive dysfunction6, type 2 diabetes7, infectious diseases and deadly cancers have been connected to vitamin D deficiency1,2,8. Debate continues on what an “optimal” serum concentration of 25(OH)D is and how much supplementation is required to achieve it. The Institute of Medicine (IOM) recommended that 600 IU/d as adequate to sustain a serum concentration of 25(OH)D above 20 ng/mL for most children and adults and prevent negative outcomes for their bone health1,3.
Although the IOM’s upper limit of vitamin D for adults is 4000 IU/d, the IOM and the Endocrine Society recognize that up to 10,000 IU/d is completely safe in healthy adults for up to 5 months1,3,9. Ekwaru et al.10 reported that receiving up to 20,000 IU/d for at least one year did not achieve serum concentration of 25(OH)D above 100 ng/mL in adults10. Many reference laboratories11 as well as the Endocrine Society suggested this serum concentration of 25(OH)D (100 ng/mL) as the upper limit of normal. The most epidemiological studies indicated that serum 25(OH)D > 30 ng/mL were related with immune function improvement and reduced risk of many chronic illnesses8,12. However studies evaluating supplementation with vitamin D up to 2000 IU/d with an average of 5 years of follow-up did not find benefit for reducing risk for cardiovascular disease or cancer13. In the Vitamin D and Omega-3 Trial (VITAL)13, a large primary-prevention trial, supplementation with vitamin D3 (at a dose of 2,000 IU/d) did not show any significant association with lower occurrence of cardiovascular events or invasive cancer than placebo13. Despite that vitamin D supplementation did not associate with a lower occurrence of total deaths from cancer than placebo, yet found that mortality due to cancer was significantly lower with vitamin D supplementation13. Patients’ quality of life in hospital was improved after supplementation with vitamin D3 at 10,000 IU/d over 6 months and improved hormonal factors b-type natriuretic peptide (BNP) and PTH as well as inflammation14. These findings suggest possible health benefits of doses of vitamin D above the RDA.
However, the influence of vitamin D supplementation on genome-wide expression remains largely unexplored in vivo, particularly with respect to dose. We previously evaluated the influence of vitamin D supplementation on genome-wide expression and found differential regulation of about 300 genes because of supplementation with vitamin D38. This randomized controlled double-blinded study included healthy young adults who received either 400 IU/d of vitamin D3 (the study occurred in 2010 before the IOM released its new recommendation of 600 IU/d) or 2,000 IU/d for 2 months. The alteration of gene regulation in the 400 IU/d group was the same as 2,000 IU/d8. However, we detected a greater change in gene regulation in the subjects of the 2,000 IU/d group in comparison the 400 IU/d group8. Pathway and functional analysis of the target genes indicated that vitamin D supplementation may be connected with some pathways related to epigenetic modification, immune system and response to stress8. Many of these activities of vitamin D have been hypothesized to play roles in disease susceptibility including autoimmune disease and cancer8,12. The current clinical trial was designed to evaluate the responsiveness of different doses of vitamin D supplementation (600 IU/d, 4,000 IU/d and 10,000 IU/d) on serum calcium, PTH and broad gene expression in white blood cells. Our previous study supported the theory that higher doses of vitamin D could have important biologic functions at least on the immune cells8. The hypothesis that was tested was that as serum concentration of 25(OH)D increased as a result of vitamin D supplementation that there would be a significant decline in PTH levels. Furthermore, we expected that there would be continued alterations in gene expression when the dose was increased to 10,000 IUs daily whereas the PTH levels would plateau at a dose of 4000 IUs daily.
Results
Baseline characteristics
Participants were recruited between November 2016 and March 2018. The baseline examination was performed in November 2016 and October 2017. After consideration criteria for inclusion and exclusion, a total of 33 adult subjects recruited. Thirty participants (90%) completed the 6-month trial. The CONSORT flow diagram is shown in Fig 1.
Depicts the CONSORT flow diagram, the adverse events as well as the reasons for withdrawal. With 3 participants withdrawing from the study, the overall dropout rate was 10% with one subject resigning from the arm 1 (to receive 600 IUs of vitamin D3), and 2 subjects from the test arm 3(to receive 600 IUs of vitamin D3).
Baseline serum concentrations of calcium, PTH and total 25(OH)D are shown in Table 1.
Influence of the supplementation with vitamin D3 on circulation levels of PTH and 25(OH)D
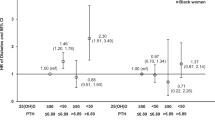
The average increase in 25(OH)D over 24 weeks was 7 ng/mL (18 nmol/L), 18 ng/mL (45 nmol/L) and 61 ng/mL (153 nmol/L) for 600 IU/d, 4000 IU/d and 10,000 IU/d, respectively (Table 1). Figure 2 depicts serum concentrations of 25(OH)D and PTH by dose group.
Total concentration of calcium, PTH and 25(OH)D during vitamin D3 supplementation at baseline and every eight weeks for 24 weeks. Total 25(OH)D, PTH and calcium levels during vitamin D3 supplementation are evaluated at baseline and every eight weeks for 24 weeks. The p-value in the figure represents the difference between in each time point with the baseline.
Mean serum concentrations of 25(OH)D at baseline were 17.1 ± 5.9 ng/mL (43.8 ± 14.8 nmol/L). After 24 weeks on 600 IU/d serum 25(OH)D significantly (p = 0.01) increased to 24.3 ± 4.1 ng/mL (60.8 ± 10.3 nmol/L) at end-of-study. The 600 IU/d dose was sufficient to correct vitamin D deficiency (25(OH)D above 20 ng/ml) in 71% of subjects but did not result in sufficiency (25(OH)D above 30 ng/ml) and 86% of subjects were still remain insufficient. There was no significant change in serum concentrations of PTH or calcium in the 600 IU/d group (p > 0.05).
The mean serum 25(OH)D level that was achieved for the groups that ingested 4,000 and 10,000 IU/d vitamin D3 daily for 24 weeks was 40.8 ± 3.8 ng/mL (102 ± 9.5 nmol/L) and 78.6 ± 13.5 ng/mL (196.5 ± 33.8 nmol/L), respectively. All participants in the 4000 and 10,000 IU/d groups achieved 25(OH)D levels >30 ng/ml (>75 nmol/L). There was no significant change in serum calcium for either group (Table 1). Significant decreases in PTH levels of 17.5% and 33.3% at 16 weeks were found for the 4000 and 10,000 IU/d group, respectively (p = 0.04). PTH levels remained at that level for the remaining 8 weeks (Fig. 2). There were no significant differences between men and women with respect to changes in serum concentration of calcium, 25(OH)D or PTH in response to supplementation with vitamin D3.
Influence of supplementation with vitamin D3 on genome wide expression in buffy coat
Differential expression analysis was performed using fold change >1.5 to identify a total of 162, 320 and 1289 differentially expressed genes (DEGs) that were influenced after vitamin D3 supplementation with dose of 600, 4,000 and 10,000 IU/d, respectively. The recognized target genes are shown in Supplementary Tables 1 and 2.
The microarray results of gene expression alterations were confirmed by real-time PCR for 7 genes including HIST1H2BB, TLR1, CYP24A1, LRRN3, RPL3, OCLM and HBE1 (Table 2).
An evaluation of genome-wide gene expression of genes being influenced by vitamin D3 supplementation revealed a greater change in the gene expression for the subjects who received 10,000 IU/d compared to the other two groups. There was a dose-dependent influence on the total number of differentially expressed genes (Table 3).
Whereas 162 (86 up-regulated, 76 down-regulated) genes in the peripheral white blood cells were influenced the adults who took 600 IU/d for 6 months, there was 2- and 8-fold increase in the number of genes that were influenced in the groups that received 4000 IU/d and 10,000 IU/d, respectively (Table 3).
We compared gene expression between the 3 groups and related them to changes in serum concentrations of PTH and 25(OH)D. Broad gene expression analysis revealed that all groups who received vitamin D3 supplementation had a significant number of genes that were differentially expressed. The subjects in the 600 IU/d group did not have any significant change in their serum levels of PTH but demonstrated a change in 162 genes after 6 months of supplementation (Fig. 3).
Gene expression alterations in response to 600 IU/d vitamin D3 supplementation. The gene-expression alterations are demonstrated by different colors. Upregulation and downregulation of gene expression after 6-months of vitamin D3 supplementation are shown by red and blue respectively. Trends in gene expression are seen by a range of colors from light blue to dark red. The red, white and blue represents high, average and low gene expression respectively.
A similar pattern of variable genomic response to vitamin D3 supplementation was detected in the 2 groups treated with higher doses of vitamin D3 supplements (4,000 IU/d and 10,000 IU/d). The gene expression alterations in the group of 4,000 IU/d is shown in Supplementary Fig. 1. A similar observation was made for those subjects in the 10,000 IU/d group (Fig. 4). The statistical analysis showed that 1,289 genes were differentially expressed after vitamin D3 supplementation. Among these DEGs, 800 genes were upregulated and 489 genes were downregulated after vitamin D3 supplementation (Fig. 5).
Gene expression alterations in response to 10,000 IU/d of vitamin D3 supplementation. The gene-expression alterations are demonstrated by different colors. Upregulation and downregulation of gene expression after 6-months of vitamin D3 supplementation are shown by red and blue respectively. Trends in gene expression are seen by a range of colors from light blue to dark red. The red, white and blue represents high, average and low gene expression respectively.
Volcano plot of target genes in the10,000 IU/d group. Log2 fold change was plotted against the p-value (−log base 10). This statistical analysis showed that 1289 genes were differentially expressed after vitamin D3 supplementation. Among these DEGs, 800 genes were upregulated and 489 genes were downregulated after 6 months supplementation with vitamin D3. Volcano plot of differentially expressed genes (DEGs) between, before and after 24 wks vitamin D3 supplementation (10,000 IUs/d). Log2 fold change was plotted against the p-value (−log base 10). Differential expression analysis using a p < 0.05 cutoff identified 1289 DEGs after vitamin D3 supplementation. Among these DEGs, 800 genes were upregulated and 489 genes were downregulated after vitamin D3 supplementation.
Variable pattern of genomic wide expression in response to supplementation with Vitamin D3
We compared gene expression between dose groups and related this data to changes in circulating levels of 25(OH)D and PTH to provide a clearer understanding of the biologic responsiveness to different doses of vitamin D3. The pattern of gene expression in response to vitamin D3 supplementation showed an inter-individual variation. Approximately 30% of the adults who received different doses of vitamin D3 supplement (600, 4000 or 10000 IU/d) for 6 months and raised serum 25(OH)D levels to the same degree as the other 70% demonstrated much less of a genomic response, despite similar increases in 25(OH)D. This variable pattern of expression is shown in Figs. 3 and 4, which displays some subjects with a very strong genomic response to vitamin D3 supplementation when compared to others with a weak response. Although after receiving vitamin D3 the broad gene expression significantly was changed in all subjects, the fold change of gene expression and the number of the differently expressed gene were different between these two groups of subjects with very strong genomic response comparing weak genomic response to vitamin D3.
Figure 3 depicts gene expression changes in subjects on 600 IU/d, and demonstrated that five subjects (ID# 6, 17, 30, 49 and 69) had a very strong genomic response to vitamin D3 supplementation when compared to two subjects (ID: 50 and 67) with a weak response. Figure 4 depicts gene expression changes in subjects on 10,000 IU/d, and demonstrated that three subjects (ID: 34, 46 and 68) had a very strong genomic response to vitamin D3 supplementation with many genes being up or down regulated, in comparison with one subject (ID: 73) with a moderate response and two subjects (ID: 56 and 66) with a weak response. Subject 34 had a baseline 25(OH)D of 20 ng/mL (50 nmol/L) which increased to 56 ng/mL (140 nmol/L). This subject had a robust gene expression in response when comparing this subject’s heat map at baseline and at 6 months (Fig. 4). Subject 56 had a baseline 25(OH)D of 21 ng/mL (52 nmol/L) that was comparable to subject 34. After 6 months on 10,000 IU/d this subject achieved a higher blood level of 25(OH)D (87 ng/mL ;218 nmol/L) yet had a much more subdued genomic response (Fig. 4). Approximately one third of the 10,000 IU/d group achieved similar serum 25(OH)D and PTH levels as the other two thirds of subjects, but had much less of a genomic response (Fig. 4).
This suggests that there are other factors involved in an individual’s responsiveness to the non-calcemic actions of vitamin D beyond vitamin D dose and achieved 25(OH)D concentration.
There was no significant change in expression of genes involved in vitamin D metabolism including vitamin D receptor (VDR), vitamin D binding protein (DBP or GC) and Cytochrome P450, family 24, subfamily A, polypeptide 1 (CYP24A1). There was no significant change from baseline expression after vitamin D3 supplementation between subjects with strong or weak genomic response to vitamin D3. Interestingly, when we compared baseline broad gene expression between subjects with a strong or weak genomic responses, the expression of 6 genes dramatically were different. These genes include Major histocompatibility complex, class II, DR beta 5 (HLA-DRB5) and DR beta 1 (HLA-DRB1), Purinergic receptor P2Y, G-protein coupled, 14 (P2RY14), Ribosomal protein S4, Y-linked 1(RPS4Y1), small nucleolar RNA, C/D box 33 (SNORD33), and two domains of Killer cell immunoglobulin-like receptor, long cytoplasmic tail, 1 (KIR2DL1) and Early growth response 2 (EGR2).
Pathway and functional analysis of the genes that are differentially expressed
The important applicable molecular pathways resulting from the alteration of gene regulation in response to 6 months of supplementation with vitamin D3 is shown in Fig. 6. Protein-protein interaction (PPI) network was created from the target genes8. We mapped upregulated genes to the STRING database8 and selected high confidence for interactions score. The result was significant for PPI enrichment (p-value = 9.33e−14). The key genes in these clusters were HIST1H2B, JUN, NFKB, TNF, IL8, HSPA8, EIF4A and PRS (Fig. 6).
Protein-protein interaction (PPI) network was created from significantly upregulated genes after 6-months of supplementation with vitamin D3. Protein-protein interaction (PPI) network was constructed from differentially upregulated genes after vitamin D3 supplementation. We mapped differentially upregulated genes to the STRING database (the hub protein was selected according to the node degree) and screened significant interactions with a score >0.7. The key genes in these clusters were HIST1H2B, JUN, NFKB, TNF, IL8, HSPA8, EIF4A and PRS. Network nodes represent proteins. Each node represents all the proteins produced by a single protein-coding gene locus. Edges represent protein-protein associations. Associations are meant to be specific and meaningful, i.e. proteins that jointly contribute to a shared function; this does not necessarily mean they are physically binding each other. Line color indicates the type of interaction evidence. The navy, cornflower and Olympic-blue lines indicate predicted gene co-occurrence, known interactions from curated databases and protein homology respectively. The red and purple lines indicate gene fusions and known experimentally determined interactions. Also, the green and light green lines indicate predicted gene neighborhood and textmining. Finally, the black line indicates co-expression. Line thickness indicates the strength of data support and line shape indicates the predicted mode of action17,18. Furthermore, the network is clustered to 4 specified clusters by kmeans clustering17,18 of which one is related to histone modification (red circle).
These significant interactions in our molecular network indicated that these proteins might be associated to a specific pathway and biologically should be connected8,15. This network includes 4 clusters of which one is related to histone modification (red circle in Fig. 6). Epigenetic modification such as histone modification and chromatin regulation are necessary mechanisms to control gene expression15. Gene Ontology showed that these genes in this network may regulate DNA accessibility and stability of chromosomes (red circle in Fig. 6) via histone modification as well as remodel the nucleosomes17. This finding may explain the role of vitamin D supplementation on chromatin accessibility. Furthermore, the accessibility of chromatin and vitamin D supplementation might be considered as a factor involved in individual alteration pattern of broad gene expression. The other clusters in this network are related to signaling pathways of NF-kappa B, TNF, NOD-like receptor, T cell receptor, mTOR, Chemokine, MAPK, Toll-like receptor and pathways in cancer.
PPI network was also constructed from differentially downregulated genes. The key genes in this network are TLR1, CD180 and LRRN3 (Supplementary Fig. 2).
Adverse events
There was no significant change in the serum calcium levels in any dose group. There was no sign of toxicity over 24 weeks of the study.
Discussion
This broad gene expression study describes the first insight into the genome wide regulation activity of different doses of vitamin D3 supplementation in human white blood cells. As shown in Table 3, differential expression analysis was performed using fold change >1.5 to identify a total of 162, 320 and 1,289 differentially expressed genes (DEGs) that were affected after vitamin D3 supplementation with doses of 600, 4,000 and 10,000 IU/d, respectively. These genes are related to epigenetic modification and immune function (Fig. 6). This observation is consistent with our previous study that showed that supplementation with vitamin D3 influenced the regulation of about 300 genes that were related to epigenetic modification and immune function (Fig. 7)8.
Venn diagram for comparing the number of affected genes between current study and our previous study8. (A) Differential expression analysis identified 1289 DEGs (differentially expressed genes) after 24 wks vitamin D3 supplementation (10,000 IUs/d). (B) Differential expression analysis identified 291 DEGs after 8 wks vitamin D3 supplementation (400 or 2,000 IUs/d). Venn diagram for comparing the number of differentially expressed genes (DEGs) between current study and our previous study4. (A) Differential expression analysis identified 1289 DEGs after 24 wks vitamin D3 supplementation (10,000 IUs/d). (B) Differential expression analysis identified 291 DEGs after 8 wks vitamin D3 supplementation (400 or 2,000 IUs/d).
The effectiveness of vitamin D3 supplementation is connected to its ability to produce adequate substrate [25(OH)D] for its metabolism to 1,25-dihydroxyvitamin D [1,25(OH)2D] in the kidneys and other tissues2,4,8.
In vitro studies showed that 1,25(OH)2D3 regulated about two hundred genes that are involved in immune function, cellular proliferation and differentiation as well as angiogenesis18,19,20. Our results confirm previous findings that have indicated that VDR stimulation may affect genome-wide expression18,19,20,21,22,23. A human genome study showed that there are about 2,776 VDREs by the length of the human genome22,23.
There continues to be controversy as to whether reaching blood concentrations of 25(OH)D above 30 ng/mL would have any additional health benefits3,12. Our results demonstrated that PTH plateaued when 25(OH)D ≥ 30 ng/mL (75 nmol/L) and confirms previous observations that serum concentrations of PTH continued to decrease and reach a plateau when circulating levels of 25(OH)D > 30 ng/mL24,25,26. The effect of increasing vitamin D3 from 4,000 IU/d to 10,000 IU/d had no significant additional effect on the PTH levels (Fig. 2). However, the gene expression analysis demonstrated a dose dependent effect. Even for subjects who took 600 IU/d of vitamin D3 for 24 weeks, a dose that had little effect on PTH levels, this dose significantly affected the expression of more than 100 genes. In comparison, the groups who received vitamin D3 supplement 4,000 and 10,000 IU/d for 24 weeks had a similar effect on lowering the blood levels of PTH, but the group who received 10,000 IU/d had 4-fold greater effect on gene expression, influencing ~1,200 genes compared to the group who took 4,000 IU/d (about 300 genes). These results indicated that even a small increase in vitamin D3 intake of 600 IU/d for 24 weeks, a dose that did not alter the PTH levels, exerted significant genomic effects. Therefore, randomized controlled trials that include a “placebo” group receiving the RDA of 600 IU/d are confounded by unanticipated changes in gene expression. Our findings showed that there was a dissociation between the calcemic and non-calcemic biologic actions of vitamin D3, especially on functions involved in immune activity.
These results may help explain the disparity of conclusions regarding the studies that have evaluated the impact of supplementation with vitamin D3 on serum 25(OH)D improvement and clinical outcomes. An individuals response to vitamin D3 is related to the individual’s ability to convert vitamin D to its active metabolite and 1,25(OH)2D’s interaction with its receptor and response elements8,27,28.
Similar to our findings, two recent studies (VitDmet and VitDbol trials) indicated that there are individual differences in response to supplementation with vitamin D23,27,28. Based on their conclusion, this response to vitamin D is explain by epigenetic and genetic individual differences27,28. Our results support this conclusion that indicated in subjects with a lower genomic response to vitamin D3 supplementation and there was a response in ~2–5% of the genome while in more responsive subjects >5% of the genome responded to vitamin D3.
The most pronounced vitamin D response occurred in genes involved in genetic regulation (Fig. 5 and Supplementary Fig. 2). The major upregulated genes were HIST1H2B, JUN, NFKB, TNF, IL8, HSPA8, EIF4A and PRS and the major down regulated genes were TLR1, CD180 and LRRN3. The upregulated genes were involved in 4 main clusters, one of which is related to histone modification (red circle in Fig. 6). Epigenetic modification, such as histone modification and chromatin regulation, are essential parts of gene regulation16,17. These findings are consistent with our previous study8 and several other studies29,30 that showed that vitamin D supplementation caused alteration in some genes related to epigenetic modification.
The small sample size of participants is a major limitation of the current clinical trial. In spite of this small sample size, the results of broad genomic expression are associated with an acceptable FDR. The use of microarray technology for evaluating gene expression is another limitation of our study. RNA-sequencing is more popular than microarray for evaluating broad gene expression. Nevertheless, RNA-sequencing has been associated with some limitations and biases31.
Peripheral white blood cells are an acceptable source of RNA for evaluating gene expression in response to drug or other biological exposure32. The changes in gene regulation patterns in the peripheral white blood cells, as a result of the 6-month supplementation of vitamin D3, represented alterations in cells that were short lived and that were constantly replenished by bone marrow precursors. Thus, changes in gene expression patterns after 6 months does not related to the same cells, due to the short life-cycle of circulating white blood cells.
However, there are several published transcriptome studies of peripheral white blood cells and purified monocytes obtained from adults that relate gene expression to vitamin D33,34,35.
In addition, the influence of vitamin D3 active metabolite, 1,25(OH)2D3, on broad gene expression in monocytes was evaluated by RNA-seq36,37. The study showed that about 9% of gene expression profile of monocytes were altered by of 1,25(OH)2D336.
This research program emphasizes the importance of personalized medicine. Vitamin D supplementation at 10,000 IU/d for 6 months was safe, had optimally regulated PTH levels and a pronounced effect on genetic expression of more than 1,200 genes. Furthermore, broad gene expression may predict individual responsiveness to vitamin D3 supplementation.
Methods
The protocol of the current study approved by the Institutional Review Board (IRB) of Boston University Medical Campus (H-35506) and was completed in accordance with the CONSORT statement38.
This clinical trial is listed at the ClinicalTrials.gov (NCT02856776; date of registration 05/08/2016). All participants provided written informed consent.
A deidentified bottle that contained 60 capsules of vitamin D3 was given to each participant that was formulated with one of the doses of vitamin D3 (600 IU/d, 4,000 IU/d or 10,000 IU/d). All vitamin D3 supplements were provided by Solgar Inc (Leonia, NJ) and the contents evaluated by HPLC as previously described5 and were found to contain concentrations within 10% of their specified content. The bottles were returned at each visit when the vitamin D3 capsules were counted to track compliance.
The participants were randomized by a computer-generated randomization program into one of the three study groups (Fig. 1)35.
Recruitment
Healthy young adult males and non-pregnant females were prescreened for serum concentrations of 25(OH)D deemed insufficient (below 30 ng/mL). Inclusion criteria included healthy young healthy black and white adults with a BMI <30 kg/m2 without disorders or medications affecting vitamin D metabolism. To reduce the effect on 25(OH)D levels recruitment started in October and supplementation was completed by March. All subjects signed an informed accepted by the IRB of Boston University Medical Campus.
The exclusion criteria consistent with our previous study8 were: history of elevated serum calcium (>10.5 mg%); vitamin D supplementation with a dose of 600 IU/d or more; direct exposure to artificial UVB or solar radiation during the past month for greater than eight hours; any kind of malabsorption; history of chronic or acute renal or hepatic disease; current antiseizure medications or glucocorticoids; pregnant/lactating women; and reluctance to consent to the study.
Study visits and blood sample collection
All participants visited in the GCRU (a unit for clinical research at Boston University Medical Campus). At baseline and every eight weeks, blood was drawn from each subject to determine serum calcium, albumin, creatinine, PTH and total 25(OH)D concentrations. At baseline and after 24 weeks additional blood was obtained for collecting the buffy coat for the RNA extraction to evaluate broad gene expression by microarray analysis. Buffy coat including peripheral white blood cells isolated as soon after the blood draw as possible (usually <30 minutes after the blood drawn) to obtain total RNA. Quest Diagnostics performed the 25(OH)D and PTH assays as previously described4. The other blood biochemistries were performed by Boston Medical Center Clinical Laboratory.
Microarray analysis
RNA extraction was performed by using a QIAGEN RNA extraction kit (QIAGEN’s RNeasy kit; Qiagen, Valencia, CA). The isolated RNA kept at −80 degrees Celsius till using for expression analysis. All stored RNA sent to the Boston University Microarray Resource Facility for analysis. All procedures are described in the GeneChip® Whole Transcript (WT) Sense Target Labeling Assay Manual (Affymetrix, Santa Clara, CA) and also in our previous article8 and supplementary information.
Real time –PCR verification
The microarray results of gene expression alterations were confirmed by real-time PCR using the Quant Studio 7 Real-Time PCR system. Total 7 genes including HIST1H2BB, TLR1, CYP24A1, LRRN3, RPL3, OCLM and HBE1 selected for validation based on their differential expression in the Microarray analysis and 2 housekeeping genes (Table 2).
For 7 genes (Table 2). All procedures described in our previous article8 and supplementary information.
Safety and compliance
The amount of vitamin D3 that given was within the guidelines recommended by the Institute of Medicine (now National Academy of Medicine) and the Endocrine Society Guidelines1,3. Serum calcium, albumin and creatinine were determined every 8 weeks to evaluate for potential toxicity. Any participant discovered to have serum calcium level above 10.5 mg/dL or serum creatinine increased by >20% would immediately be removed from the study and the primary care physician informed.
A deidentified bottle containing 60 capsules of vitamin D3 was given to each participant who had one of the doses of vitamin D3 (600 IU/d, 4,000 IU/d or 10,000 IU/d). The bottles were returned at each visit when the vitamin D3 capsules were counted to track compliance.
Statistical and functional analysis
The microarray data were normalized by using RMA method and the quality control and similarity was checked by using Principal Component Analysis (PCA) method as described previously8. To compare the differentially expressed genes between groups, a 2-way ANOVA in the linear model was applied. A p value threshold of 0.05 and also a False Discovery Rate (FDR) of 0.1 considered as significant results. Pathway enrichment analysis was performed as previously described8,39,40.
Power
The sample size of current clinical trial was calculated based on the data of our previous study of the impact of vitamin D on broad gene expression8. By considering 0.05 of a type 1 error(α) and power of 80%) and changing 2-fold change in gene expression based on previous results8 with a standard deviation of 1, the sample size (N) for was estimated to N = 4 for each arm. Assuming a 2-fold difference in gene expression between the groups being compared, 2 time points for comparison (baseline, and 24 weeks), with N = 4/arm, we are able to achieve >80% power. Assuming a dropout rate of 10–20% and design effect 1.5, we enrolled a minimum of 8 subjects per arm.
Data availability
The datasets are available in the Microarray & Sequencing Resource Core Facility repository and directly accessible at http://microarray.bu.edu/~yurik/HolickM/2018-02-27_Holick_Hu1-0ST.zip.
References
Holick, M. F. et al. Evaluation, treatment, and prevention of vitamin D deficiency: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab. 96, 1911–30 (2011).
Hossein-nezhad, A. & Holick, M. F. Vitamin D for Health: A Global Perspective. Mayo Clin Proc. 88, 720–755 (2013).
Institute of Medicine. Dietary Reference Intakes for Calcium and Vitamin D (ed. Ross, A. C., Taylor, C. L., Yaktine, A. L. & Del Valle, H. B.) 185–255 (The National Academies Press, 2011).
Al-Ishaq, R. K. et al. Health implication of vitamin D on the cardiovascular and the renal system. Arch Physiol Biochem. 10, 1–15 (2019).
Harrison, S. R., Li D., Jeffery L. E., Raza K. & Hewison M. Vitamin D, Autoimmune Disease and Rheumatoid Arthritis. Calcif Tissue Int., https://doi.org/10.1007/s00223-019-00577-2 (2019 Jul 8).
Goodwill, A. M. & Szoeke, C. A Systematic Review and Meta-Analysis of The Effect of Low Vitamin D on Cognition. J Am Geriatr Soc. 65(10), 2161–2168 (2017).
Grammatiki, M., Karras, S. & Kotsa, K. The role of vitamin D in the pathogenesis and treatment of diabetes mellitus: a narrative review. Hormones (Athens). 18(1), 37–48 (2019).
Hossein-nezhad, A. & Holick, M. F. Influence of vitamin D status and vitamin D3 supplementation on genome wide expression of white blood cells: A randomized double-blind clinical trial. PlosONe. 8, e58725 (2013).
Heaney, R. P., Davies, K. M., Chen, T. C., Holick, M. F. & Barger-Lux, M. J. Human serum 25-hydroxycholecalciferol response to extended oral dosing with cholecalciferol. Am J Clin Nutr. 77, 204–210 (2003).
Ekwaru, E., Zwicker, J. D., Holick, M. F., Giovannucci, E. & Veugelers, P. J. The importance of body weight for dose response relationship of oral vitamin D supplementation and serum 25-hydroxyvitamin D in healthy volunteers. PLOS ONE. 9, e111265 (2014).
Dudenkov, D. V., Mara, K., Petterson, T., Maxson, J. & Thacher, T. Serum 25-hydroxyvitamin D values and risks of all cause and cause-specific mortality: A population-based-based cohort study. Mayo Clin Proc. 90, 77–86 (2015).
Bouillon, R. et al. Skeletal and extra-skeletal actions of vitamin D: Current evidence and outstanding questions. Endocr Rev. 40(4), 1109–1151 (2019).
Manson, J. E. et al. Vitamin D Supplements and Prevention of Cancer and Cardiovascular Disease. N Engl J Med. 380, 33–44 (2018).
Moretti, H. D., Colucci, V. J. & Berry, B. D. Vitamin D3 repletion versus placebo as adjunctive treatment of heart failure patient quality of life and hormonal indices: a randomized, double-blind, placebo-controlled trial. BMC Cardiovasc Disord. 30, 274 (2017).
Bubier, J. A. et al. Integration of heterogeneous functional genomics data in gerontology research to find genes and pathway underlying aging across species. PLoS One. 14(4), e0214523 (2019).
Zhang, G. & Pradhan, S. Mammalian epigenetic mechanisms. IUBMB Life. 66(4), 240–56 (2014).
Fenley, A. T., Anandakrishnan, R., Kidane, Y. H. & Onufriev, A. V. Modulation of nucleosomal DNA accessibility via charge-altering post-translational modifications in histone core. Epigenetics Chromatin. 11(1), 11 (2018).
Adams, J. S. & Hewison, M. Update in Vitamin D. J Clin Endocrinol Metab. 95, 471–478 (2010).
Rosen, C. J. et al. The nonskeletal effects of vitamin D: an Endocrine Society Scientific statement. Endocr Rev. 33, 456–92 (2012).
Montecino, M. et al. Vitamin D control of gene expression: temporal and spatial parameters for organization of the regulatory machinery. Crit Rev Eukaryot Gene Expr 18, 163–72 (2008).
Tarroni, P. et al. Microarray analysis of 1,25(OH)2D3 regulated gene expression in human primary osteoblasts. J Cell Biochem. 113, 640–9 (2012).
Ramagopalan, S. V. et al. A ChIP-seq defined genome-wide map of vitamin D receptor binding: associations with disease and evolution. Genome Res. 20, 1352–60 (2010).
Ahn, J. et al. Genome-wide association study of circulating vitamin D levels. Hum Mol Genet 19(13), 2739–45 (2010).
Holick, M. F. et al. Prevalence of vitamin D inadequacy among postmenopausal North American women receiving osteoporosis therapy. J Clin Endocrinol Metab. 90, 3215–3224 (2005).
Chapuy, M. C. et al. Vitamin D3 and calcium to prevent hip fractures in elderly women. N Engl J Med. 327, 1637–1642 (1992).
Thomas, K. K. et al. Hypovitaminosis D in medical inpatients. N Engl J Med. 338, 777–783 (1998).
Carlberg, C. & Haq, A. The concept of the personal vitamin D response index. J Steroid Biochem Mol Biol. 175, 12–17 (2018).
Carlberg, C. Nutrigenomics of Vitamin D. Nutrients., 21;11(3), E676 (2019).
Wei, R., Dhawan, P., Baiocchi, R. A., Kim, K. Y. & Christakos, S. PU.1 and epigenetic signals modulate 1,25-dihydroxyvitamin D3 and C/EBPα regulation of the human cathelicidin antimicrobial peptide gene in lung epithelial cells. J Cell Physiol., 10.1002/jcp.27702 (2018).
Hossein-nezhad, A. & Holick, M. F. Optimize dietary intake of vitamin D: an epigenetic perspective. Curr Opin Clin Nutr Metab Care. 15, 567–79 (2012).
‘t Hoen, P. A. et al. Reproducibility of high-throughput mRNA and small RNA sequencing across laboratories. Nat Biotechnol. 31(11), 1015–22 (2013).
Dumeaux, V. et al. Deciphering normal blood gene expression variation–The NOWAC post genome study. PLoS Genet. 12, e1000873 (2010).
Carlberg, C. et al. Primary vitamin D target genes allow a categorization of possible benefits of vitamin D3 supplementation. PLoS One. 29;8(7), e71042 (2013).
Vukić M. et al. Relevance of vitamin D receptor target genes for monitoring the vitamin D responsiveness of primary human cells. PLoS One. 13;10(4), e0124339 (2015).
Standahl Olsen, K., Rylander, C., Brustad, M., Aksnes, L. & Lund, E. Plasma 25- hydroxyvitamin D level and blood gene expression profiles: a cross-sectional study of the Norwegian Women and Cancer Post-genome Cohort. Eur J Clin Nutr. 67(7), 773–8 (2013).
Seuter, S., Neme, A. & Carlberg, C. Epigenome-wide effects of vitamin D and their impact on the transcriptome of human monocytes involve CTCF. Nucl. Acids Res. 44(9), 4090–4104 (2016).
Neme, A., Nurminen, V., Seuter, S. & Carlberg, C. The vitamin D-dependent transcriptome of human monocytes. J Steroid Biochem Mol Biol. 164, 180–187 (2016).
Schulz, K. F., Altman, D. G., Moher, D. & Group, C. CONSORT 2010 Statement: updated guidelines for reporting parallel group randomised trials. BMC medicine. 8, 18 (2010).
Hossein-Nezhad, A. et al. Transcriptomic Profiling of Extracellular RNAs Present in Cerebrospinal Fluid Identifies Differentially Expressed Transcripts in Parkinson’s Disease. J Parkinsons Dis. 6, 109–117 (2016).
Maghbooli, Z. & Hossein-Nezhad, A. Transcriptome and Molecular Endocrinology Aspects of Epicardial Adipose Tissue in Cardiovascular Diseases: A Systematic Review and Meta-Analysis of Observational Studies. Biomed Res Int. 2015, 926567 (2015).
Acknowledgements
We would like to thank the Boston University Microarray and Sequencing Resource Core Facility for microarray of the samples and their data analysts Adam C. Gower, Ph.D. and Andrés Bretón, M.S for microarray data analysis. This trial was funded by institutional resources. The vitamin D3 supplements are provided by Solgar LLC.
Author information
Authors and Affiliations
Contributions
Study design: A.S., T.K. and M.H. Data acquisition: A.S., T.K., A.S. and M.H. Analysis: A.S. and M.H. All authors, A.S., T.K., A.S. and M.H., reviewed and edited the manuscript. M.H. is the guarantor of this work, and, as such, had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis.
Corresponding author
Ethics declarations
Competing interests
The A.S., T.K. and A.S. declare no competing interests. M.H. is a consultant for Quest Diagnostics Inc., and was on the speaker’s Bureau for Abbott Inc. and Hayat Pharmaceutical Industries Company PLC.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Shirvani, A., Kalajian, T.A., Song, A. et al. Disassociation of Vitamin D’s Calcemic Activity and Non-calcemic Genomic Activity and Individual Responsiveness: A Randomized Controlled Double-Blind Clinical Trial. Sci Rep 9, 17685 (2019). https://doi.org/10.1038/s41598-019-53864-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-019-53864-1
This article is cited by
-
Transcriptomics identifies blunted immunomodulatory effects of vitamin D in people with multiple sclerosis
Scientific Reports (2024)
-
Vitamin D status of the Russian adult population from 2013 to 2018
Scientific Reports (2022)
-
Photoprotective Properties of Vitamin D and Lumisterol Hydroxyderivatives
Cell Biochemistry and Biophysics (2020)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.