Abstract
Anti-Retroviral Therapy (ART) is the recommended first line therapy for patients with HIV. Since 2004, Chinese government has provided free Chinese herbal medicine (CHM) for Chinese HIV/AIDS patients. Data of living patients with HIV from the NFTCMP database and Center for Disease Control (CDC) database during 2003–2016 in Guangxi province was obtained and compared. Patients were divided into 3 groups according to their recorded treatment regimens. A total of 2954 patients with their treatment recorded in the two databases were included for analysis, their median age was 46 years (IQR = 36–59), and 64.63% were male. CHM regimens users had baseline CD4 cell counts (380.11 ± 240.59 cell/μL), approximately 100 cell/μL significantly higher than patients receiving CHM combined with ART regimens or only ART regimens. There was no significant difference in mortality among groups. All three regimens improved patients’ CD4 cell counts. Compared to the sharp improvement in ART group during the first 6 months, CD4 cell counts of patients in CHM group and CHM combined with ART group showed a smooth and steady rise. CD4 cell counts of the combined group remained much lower than ART group in the first 3 years, but overtook ART group in the fourth year.
Similar content being viewed by others
Introduction
Human immunodeficiency virus (HIV) is a retrovirus that can destroy or impair the function of the immune system and which can later progress to Acquired Immune Deficiency Syndrome (AIDS), the most advanced stage of HIV infection. HIV/AIDS remains one of the most important public health problems in the world, particularly in low-income and middle-income countries. According to the World Health Organization (WHO) report1, at the end of 2015, there were 36.7 million [34.0 million–39.8 million] people living with HIV, and more than 18 million people were receiving antiretroviral treatment (ART) by mid-2016. Due to treatment, the global annual HIV-related all-cause mortality has continually decreased in recent years. By 2015 the number had reduced to 1.1 million [940 000–1.3 million]. According to the recent report of China Centers for Disease Control (CDC), on October 31, 2017, China’s population of people living with HIV was about 750,0002. HIV/AIDS remains one of the most important public health problems in China and no longer restricted to blood donors and drug users but increasingly spreading through the general population due to unsafe sex, especially among men who have had sex with men3,4,5.
Chinese herbal medicine (CHM) was firstly used to treat patients living with HIV in 1987 when Chinese medicine practitioners from China provided medical assistance in Tanzania, Africa6. In China, there are three main strategies for treating HIV, which include ART alone, CHM alone, and CHM combined with ART. A pilot project, the National Free CHM HIV/AIDS Treatment Program (NFCHMP), was initiated in 2004 and expanded rapidly. NFCHMP was supported by the State Administration of Traditional Chinese Medicine (SATCHM) and the Ministry of Finance, and the program has provided tens of thousands of HIV/AIDS patients with free Chinese medicine treatment.
A double-blind randomized controlled trial7 found CHM could significantly improve CD4 cell counts and symptoms (anorexia, diarrhea, fatigue, nausea, and emesis). In Henan province, a retrospective cohort study based on the database of NFCHMP observed CHM could decrease the disease progression, reduce the mortality of PLHIV, and improve life expectancy. However, the major limitation was that they chose the world mortality rate over the same period as a comparison8. A 7-year observational study suggested long-term use of CHM could maintain or slow the pace of CD4 cell counts declining. However, this study did not address bias, potential confounders and the possibility that results may have occurred by chance9. CHM has also been reported to relieve HIV/AIDS patients’ clinical symptoms (e.g., fatigue, pain, sleep disturbance, shortness of breath, coughing) and significantly decrease opportunistic infections in before and after studies10,11,12. Although there is some evidence to indicate there was an observable effect of CHM therapy on HIV, most studies had a small sample size and did not address confounding factors. To confirm the effect and safety of CHM, analysis of more longitudinal data is required to analyze the characteristics of the patients who receive CHM therapy, and statistically adjust for confounding factors. Obtaining longitudinal data is expensive, time-consuming, and the data is difficult to analyze, the advantage of longitudinal data is that the individual development of a certain outcome variable can be studied over time. However, when evaluating the effect of CHM for HIV/AIDS, most studies have ignored individual disease progression. With the development of statistical techniques, such as generalized estimating equations (GEE) and random coefficient analysis, it has become possible to analyze longitudinal relationships using all available longitudinal data, without summarizing the longitudinal development of each subject into one value13.
Guangxi, a province located in southwestern China that borders Myanmar, has the second highest HIV prevalence in the whole country due to its specific geographical location and cultural environment14. Therefore, this study aimed to utilize and explore longitudinal data from the registries established by SATCHM in Guangxi province to analyze the effect of CHM on patients with HIV.
Methods
Data sources
The Ethics Committee of Beijing University of Chinese medicine granted ethical approval for analyzing data from two registries (BZYYYDX-LL20160215). This study complied with the Declaration of Helsinki and Good Clinical Practice Guidelines in China. All participants provided their written informed consent and allowed their medical data to be used for researches. To protect participants’ privacy, we extracted all available data without names and other identifiers on HIV patients from two registries (CHM registry and CDC registry) in Ruikang Hospital, which is located in the Guangxi province of southern China. We excluded 29 records that only had an ID number and had no other information.
CHM database collected data HIV/AIDS patients who participated in the NFCHMP and received CHM therapy. In this registered database, all participants were identified from 16 clinical centers across 14 cities. The CDC database in Nanning, the capital of Guangxi province, was also included to compare the effectiveness of CHM therapy and ART therapy. All patients in the two registries had been diagnosed with HIV infection via virus detection.
Procedure
In the 16 NFCHMP clinical centers, the patients diagnosed with HIV infection would have been informed that NFCHMP could provide free CHM. Patients who had a previous record of severe cerebrovascular disease, severe kidney and hematopoietic system disease, and mental disease were excluded. The NFCHMP participants would have been registered on the CHM registry and would have completed the pre-CHM treatment examination, which we defined as a baseline.
Participants were provided with medication and assessed every three months via an interview and laboratory testing. Doctors identified the CHM therapy according to the infection stage of patients and used the Clinical practice proposal of Traditional Chinese medicine treatment for patients living with HIV/AIDS issued by SATCM. CHM therapy could include Chinese patent medicines such as Tangcao tablets, Shenling Fuzheng capsules, Qingdu capsules, Aifukang capsules, as well as other herbal recipes, depending on patients’ symptoms and according to TCM hospital clinical practice. Whether to take a combined treatment of CHM and ART were decided based on patients’ wishes and symptoms.
According to the CHM registry, all patients took CHM. To compare the effectiveness of CHM with ART, we also accessed the CDC registry and extracted the data of HIV patients who took ART alone in Ruikang hospital.
Outcome measures
Demographic characteristics included participants’ gender and age were recorded in two registries. CHM registry recorded more demographic information, including marital status, educational levels, and possible route of infection. Mortality rate, CD4, CD8 cell counts, and white blood cell (WBC) counts were extracted to evaluate the effectiveness. We used the abnormal rate of liver and kidney function to evaluate safety. Alanine transaminase (ALT) and aspartate aminotransferase (AST) were used to evaluate liver function. Blood urea nitrogen (BUN) and creatinine (Cr) were used to evaluate kidney function.
Statistics
The data analyses were performed using SAS version 9.4. We divided participants into different groups by treatment. At baseline, descriptive statistics were used to examine the demographic and clinical characteristics of all participants and in different groups. Continuous variables were summarized as means, standard deviations, median, interquartile range (IQR), range (minimum value to maximum). For categorical variables, the number and percentages of patients in each category were calculated and the proportions of participants who had dropped out, and the meantime of drop-out.
This study provided longitudinal data, in which the outcome variables were repeatedly measured. We used analysis of covariance (ANCOVA) and GEE statistical methods to adjust confounding factors13.
Our first approach was an analysis of changes in outcomes between two points in time. Differences between groups were tested for statistical significance using chi-square and Wilcoxon-Mann-Whitney tests for categorical and continuous variables, respectively. Besides, differences between groups were estimated using a one-way analysis of variance (ANOVA) followed by the Student-Newman-Keuls (SNK) test for all pairwise comparisons. Results were considered statistically significant at 0.05 p-value.
ANCOVA used to adjust confounding factors (gender, age, CD4 cell counts at baseline), furthermore, we used GEE to investigate the relationship between the outcome variable CD4 cell counts and the predictor variables (gender, age, group and time), and in the model used in this study, we assumed a linear relationship with time.
Ethical approval and informed consent
The Ethics Committee of Beijing University of Chinese medicine granted ethical approval for the study.
Results
Demographic characteristics
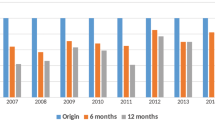
Two thousand nine hundred fifty-four individuals recorded in two registries were extracted for analyses. Of these, 1374 individuals used CHM alone, 1198 individuals used CHM combined with ART, and 382 individuals used ART alone. Participants registered on the databases between 2003 and 2016, the highest proportion (25.84%) were in 2013.
One hundred ten patients dropped out from CHM alone group with the mean drop-out time of 9.11 months. Reasons for dropping out were migrating from the area for work (n = 11), unwilling to take medications (n = 24), patients voluntarily withdrawing from the project (n = 39), travel issues (n = 4), other reasons including: lost touch, compulsory detoxification, being put in prison (n = 32).
Sixty-seven patients dropped out from CHM combined with ART group, and the meantime of drop-out was 17.78 months. They dropped out for the following reasons: migrating from the area for work (n = 3), unwilling to take medications (n = 21), patients voluntarily withdrawing from the project (n = 23), travel issues (n = 4), other reasons including compulsory detoxification and lost-to-follow-up (n = 16).
Of the participants who used CHM therapy and provided demographic characteristics, most participants were married (64.07%), 18.00% were single, 8.10% were divorced, and it is noted that 9.83% were widowed. Further analysis found that, for female patients, the proportion of the widowed (16.86%) was much higher than that of the single (7.58%). On the contrary, for males, the proportion of those who were single (21.24%) was much higher than that of widowed (8.75%). Most participants (40.45%) only received junior middle school education, and few (4.72%) had college or further college education. Most participants (84.38%) considered their possible HIV-infected route was sexual behavior, and drug taking (10.79%) was the second leading possible infection route (Table 1). Individuals used CHM combined with ART had similar but slightly different demographic characteristics. The demographic characteristics of the CHM group and CHM combined with ART group could be compared, but the CDC registry (individuals used ART alone) did not record information on the potential infection route.
After data filtering, we analyzed 2637 patients with effective or safety information. The average age of the whole sample was 47.35 ± 14.24, the median age was 45 years (IQR = 36–59), and 65.25% were male (Table 2).
Effectiveness evaluation
During the study period, there were no statistical differences between the groups in mortality (p = 0.24). Seven patients (0.51%) in the CHM group, eight patients (0.67%) in CHM combined with ART group, and five patients (1.31%) in the ART group, died.
The baseline clinical characteristics of the whole cohort were stratified by therapy (Table 2). At baseline, there were significant differences across the three groups regarding age and sex. However, all three were more likely to contain male patients and patients were mostly 30 to 49 years old. CHM regimens users had better baseline status of CD4 cell counts (376.80 ± 213.53 cell/μL, median 371, IQR = 235.5–488.5 cell/μL), around 100 cell/μL higher than the patients with CHM combined with ART regimens (271.45 ± 181.54, median 237, IQR = 148–347 cell/μL) and ART regimens (258.17 ± 133.01, median 255, IQR = 166–348 cell/μL), and there was no significant difference between CHM combined with ART group and ART group. Participants were categorized according to whether the CD4 cell count was greater than 350 per μL. The CHM group had a significantly higher proportion (55.64%) of participants with higher CD4 counts when compared to CHM combined with ART group (24.60%) and ART group (24.78%).
Changes in CD4 cell counts of the three cohorts were explored. As most participants had been registered in databases since 2011, four years of data were available. Figure 1 reflected the change curves of CD4 cell counts over a 48-months period for all three groups. All three regimens demonstrated improvements in patients’ CD4 cell counts. Compared to the initial sharp improvement in the ART group, the CD4 cell counts of patients in CHM group and CHM combined with ART group rose steadily and smoothly and respectively peaked at 499.49 ± 199.25 (median 502, IQR = 365–620) and 438.38 ± 200.68 (median 412.5, IQR = 305–535) cell/μL by 48 months. Compared to CHM group and CHM combined with ART group, participants used ART alone had rapidly increasing CD4 cell counts when treatment was initiated and was more likely to slow down their improvement of CD4 cell counts after six months. In the ART group, CD4 cell counts reached a peak at 36 months, before beginning its gradual decline to 414.15 ± 213.68 (median 386.5, IQR = 255–477) cell/μL in 48 months.
We calculated the change of CD4 cell counts from baseline value during the 4-years follow-up period, ANCOVA was used to adjust major confounding factors (age, sex) and compared the differences among groups (Table 3).
Table 4 shows the results of a GEE analysis that was applied to investigate the relationship between the outcome variable CD4 cell counts and the four predictor variables, including gender, age, group, and time. For each of the predictor variables the regression coefficient, the standard error of the coefficient and the corresponding p-value were given. In this model, time was added as a continuous variable coded as [1 to 15], and respectively corresponded to the baseline and the 16 follow-ups during four years.
Gender was significantly related to the development of outcome variable CD4 cell counts. The regression coefficient (β = 48.73, p < 0.01) for gender indicates that there was a greater increase in CD4 counts for females over time. For age, a negative association was found (β = −2.11, p < 0.01). The results also showed that there was a significant linear increase over time in CD4 cell counts (β = 9.43, p < 0.01). The change in CD4 over time was significantly different among groups.
Table 5 shows the laboratory data for each cohort. CD8 cell counts were compared between the three groups by adjusting for age, sex, and baseline values, and there was no significant difference detected during the first 4-year follow-up periods except the 2.5-year.
At baseline, comparing to participants used ART alone (5.16 ± 1.73, median 4.97, IQR = 3.97–6.1 × 109/L), participants in CHM group (5.71 ± 1.85, median 5.4, IQR = 4.55–6.53 × 109/L) and CHM combined with ART group (5.5 ± 2.26, median 5.2, IQR = 4.1–6.54 × 109/L) were more likely to have higher white blood cell (WBC) counts. After one year of treatment, there were no statistical differences in WBC counts among groups, and the mean and median WBC counts were all within normal limits.
Safety evaluation
Figure 2 shows the abnormal rate of liver and kidney function throughout the 4-years for the three groups. For liver function, at baseline, the abnormal rate of AST in CHM combined with ART group (19.79%) was significantly (χ2 = 7.73, P = 0.02) higher than the ART group (13.61%). The abnormal rate of ALT had significant differences among groups. In the first three months of ART treatment, liver function abnormal rate significantly increased and significantly higher than the other two treatments. However, after more than three months of treatment, no significant difference was detected among groups. Regarding kidney function, BUN and Cr were not significantly different at baseline between the groups. For patients taking CHM and CHM combined with ART, and ART, the baseline BUN abnormal rate was 4.54%, 4.06%, and 4.56% respectively. There was no significant difference. During four years of treatment, only at 48 months was a significant difference detected between CHM combined with ART and ART alone. Three groups had similar Cr at baseline. During the treatment, the abnormal rate for the CHM group was significantly higher than for the CHM combined with ART at 3 months. Additionally, at 33 months, CHM had a significantly higher abnormal rate than ART.
Discussion
This preliminary analysis showed that CHM gradually and continuously improved CD4 cell counts of patients with a relatively better baseline CD4 status. Compared to patients who only took the ART regimen, the patients who combined CHM were more likely to have a steady and continuous growth in CD4 cell counts. This phenomenon indicated there might be some drug interactions between two therapies. We found that for the patients who had relatively higher CD4 cell counts (>350 cell/μL) and did not take ART before, CHM could steadily increase CD4 cell counts and improved immunity levels. Compared to using ART alone, the CD4 cell counts of participants using CHM combined with ART increased slower in the first three years. It may relate to the potential effect of CHM on promoting immune reconstitution and counteracting the adverse side effects of antiviral drugs15. A study has suggested that the asymptomatic stage is the optimal time to take CHM, for it could help to maintain and enhance the immune function so as to delay the progression to the AIDS stage. For those patients who have a diagnosis of AIDS, CHM focuses on relieving symptoms of patients having AIDS-related opportunistic infection16. There was no statistical difference in the death rate among the three groups, and it may relate to the generally low death rate of patients with HIV.
In China, governments provide patients with free antiviral drug including nucleoside reverse transcriptase inhibitor (NRTI), non-nucleoside reverse transcriptase inhibitor (NNRTI), and protease inhibitor (PI), such as inhibitor didanosine (ddI), lamivudine (3TC), stavudine (d4T), zidovudine (AZT, ZDV), nevirapine (NVP), and indinavir (IDV). Using a combination of d4T, 3TC and NVP are recommended as the first-line treatment for patients who had not received ART. For those patients who had accepted ART before, experts decide whether they need to change by considering their condition and personal willingness17.
As a chronic disease, the safety of long-term medication is an important issue that both patients and doctors concerned with. In this study, long-term CHM alone or ART combined regimens seemed safety. After the first three months of treatment, only patients who used ART alone had a significant increase in the abnormal rate of liver function. While patients used CHM alone and CHM combined with ART had no significant change in liver function.
The strength of our study was our use of both traditional statistical methods and GEE to analyze longitudinal data. This study has some limitations. The CHM database was based on the patients who had agreed to take part and who completed the full four years follow up and possibly did not reflect all those taking CHM. There may also have been some selection bias with those who accepted CHM as a treatment or as part of their treatment regimen. This was not a randomized controlled trial, and therefore, potential selection bias of whether or not to consent to the study may have influenced the results.
Conclusions
Three therapies appeared to improve CD4 cell counts of patients in the first three years. After three years, CHM alone or combined with ART could still improve CD4 cell counts. There was no evidence to suggest CHM could decrease mortality. It is noteworthy that compared to patients who only took ART, patients taking CHM were more likely to have a steady rise in CD4 cell counts.
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
World Health Organization. Progress Report 2016: Prevent HIV, Test and Treat All. WHO support for country impact, http://www.who.int/hiv/pub/progressreports/2016-progress-report/en/ (2016).
National Center for AIDS/STD Control and Prevention, China CDC, http://www.chinaaids.cn/zyxz/.
Lu, L. et al. The changing face of HIV in china. Nature 455(7213), 609–611 (2008).
Chow, E. P. F., Wilson, D. P. & Zhang, L. The next era of hiv in china: rapidly spreading epidemics among men who have sex with men. Journal of Acquired Immune Deficiency Syndromes 55(4), e32–3 (2010).
Zhang, L. et al. HIV prevalence in China: integration of surveillance data and a systematic review. Lancet Infect Dis. 13(11), 955–63 (2013).
Micollier, E. & Black, M. Management of the AIDS epidemic and local/global use of Chinese medicine. Chin Perspect. 1(77), 67–78 (2009).
Wang, J. et al. Clinical observations on 100 HIV/AIDS cases treated with Chinese herb Aining granule plus ART. Chinese Journal of AIDS & STD. 14(2), 101–4, 107 (2008).
Jin, Y. et al. Survival of people living with HIV after treatment with traditional Chinese medicine in Henan province of China: a retrospective cohort study. J Tradit Chin Med. 34(4), 430–6 (2014).
Wang, J. et al. An 84-month observational study of the changes in CD4 T-lymphocyte cell count of 110 HIV/AIDS patients treated with traditional Chinese medicine. Front Med. 8(3), 362–367 (2014).
Tian, S. Z. et al. Summarization of 3-year clinical efficacy of Ai Ke Fu Zheng Pian on 112 cases of HIV/AIDS. World J Integr Tradit West Med. 4(1), 23–5 (2009).
Zou, W., Wang, J. & Liu, Y. Effect of traditional Chinese medicine for treating human immunodeficiency virus infections and acquired immune deficiency syndrome: Boosting immune and alleviating symptoms. Chin J Integr Med. 22(1), 3–8 (2016).
Liu, Z. B. et al. Treatment of acquired immunodeficiency syndrome with Chinese medicine in China: opportunity, advancement and challenges. Chin J Integr Med. 19(8), 563–567 (2013).
Twisk, J. W. R. Applied Longitudinal Data Analysis for Epidemiology-A Practical Guide. (Cambridge University Press, 2003)
Zhao, T. et al. Cognitive disorders in HIV-infected and AIDS patients in Guangxi, China. J Neurovirol. 21(1), 32–42 (2015).
Liu, Z. B., Yang, J. P. & Xu, L. R. Effectiveness and safety of traditional Chinese medicine in treating acquired immune deficiency syndrome: 2004–2014. Infect Dis Poverty. 4(1), 59 (2015).
Wang, L. et al. HIV epidemic among drug users in China: 1995–2011. Addiction. 110(Suppl 1), 20–8 (2015).
Wang, J. & Zou, W. Recent Advances of HIV/AIDS Treatment with Traditional Chinese Medicine in China. J Tradit Chin Med. 30(4), 305–8 (2010).
Acknowledgements
We would like to thank Professor Dan-hui Yi for her professional advice on the statistics. This work was supported by the Natural Science Foundation of China (Grant No.: 81673828), Capacity building in evidence-based Chinese medicine and internationalization project (No.: 1000061020008).
Author information
Authors and Affiliations
Contributions
Jian-ping Liu, Xin Deng and Jin Sun Conceived and designed the study. Jiang Feng, Zhen-wei Liu and Bin Wen supervised the data collection. Jin Sun and Jing Li did data cleaning. Jin Sun, Ying Zhang and Wen-yuan Li extracted and analyzed the data. Jin Sun and Jian-ping Liu wrote the first draft. Nicola Robinson helped drafting the manuscript and correcting any language issues. Mei Han, Nuala McGrath, and Yu-tong Fei reviewed the report and approved the final draft. All authors have read, and confirm that they meet, ICMJE criteria for authorship.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Sun, J., Jiang, F., Wen, B. et al. Chinese herbal medicine for patients living with HIV in Guangxi province, China: an analysis of two registries. Sci Rep 9, 17444 (2019). https://doi.org/10.1038/s41598-019-53725-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-019-53725-x
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.