Abstract
Acetaminophen (APAP) is a worldwide commonly used painkiller drug. However, high doses of APAP can lead to acute hepatic failure and, in some cases, death. Previous studies indicated that different factors, including life-style and metabolic diseases, could predispose to the risk of APAP-induced liver failure. However, the molecular process that could favor APAP hepatotoxicity remains understood. Here, we reported that a short-term high fat-enriched diet worsens APAP-induced liver damage, by promoting liver accumulation of lipids that induces the activation of peroxisome proliferator-activated receptor gamma coactivator 1-beta (PGC-1β). Therefore, we challenged mice with hepatic-specific PGC-1β overexpression on a chow diet with a subtoxic dose of APAP and we found that PGC-1β overexpression renders the liver more sensitive to APAP damage, mainly due to intense oxidative stress, finally ending up with liver necrosis and mice death. Overall, our results indicated that during high fat feeding, PGC-1β adversely influences the ability of the liver to overcome APAP toxicity by orchestrating different metabolic pathways that finally lead to fatal outcome.
Similar content being viewed by others
Introduction
Overdose of Acetaminophen (APAP) is the most frequent cause of acute and severe liver injury in the Western Countries. APAP is one of the most common analgesic drugs worldwide, safe when used at therapeutic dosage. Nevertheless, its ingestion only 2- or 3-fold over the maximum daily recommended dose can be fatal, due to hepatotoxicity and centrilobular hepatic necrosis1. The mechanism of APAP toxicity has been well studied. In normal conditions, APAP is mainly metabolized by glucuronidation and sulfation process. However, during an overdose these pathways become saturated and APAP is mostly metabolized by the Cytochrome P450 CYP2E1 and CYP3A4 isoenzymes into its reactive intermediate NAPQI (N-acetyl-p-benzoquinone imine)2. At subtoxic level, NAPQI is detoxified by conjugation with reduced glutathione (GSH), both non-enzymatically and in a reaction catalyzed by glutathione S-transferases. Under APAP overdose conditions, a GSH severe depletion together with a significant increase of NAPQI occurs, leading to mitochondrial dysfunction, ATP depletion, oxidative stress, DNA damage and, finally, cell death.
Even when used at low dose, APAP causes the impairment of mitochondrial respiratory chain, decreasing ATP reservoir and promoting reactive oxygen species accumulation3. Together with the reversible mitochondrial dysfunctions, this xenobiotic could exacerbate hepatic fat accretion by inhibiting fatty acids oxidation and intensifying de novo lipogenesis, finally inducing steatosis4,5. One of the factors that can increase the risk and the severity of APAP-induced liver injury is malnutrition and related metabolic diseases. Indeed, the APAP hepatotoxicity seems to be more frequent in obese or NAFLD (Non-Alcoholic Fatty Liver Disease) patients, even if some studies reported contradictory results, in which obese subjects show similar or decreased risk of APAP-induced hepatic injury compared to non-obese one6,7,8,9. Most likely, the risk and the severity of APAP toxicity in obese individuals depend on a fragile equilibrium between multiple metabolic processes that can either provide protection or be harmful to the patient itself. Therefore, the identification of pathophysiological molecular factors implied in APAP hepatoxicity is mandatory in order to prevent unintentional hazards to the health of users.
To address this issue, we reported here our results identifying the peroxisome proliferator-activated receptor gamma coactivator 1-beta (PGC-1β) as an important contributor to APAP-induced hepatic failure. The coregulator PGC-1β belongs to the PGC-1s family, whose members play a key role in the control of energy metabolism in many tissues and have been so far recognized as master regulators of mitochondrial biogenesis and antioxidant response10,11,12,13. Beside its role in oxidative metabolism, in the liver PGC-1β is mainly involved in de novo lipogenesis and hepatic triglycerides secretion through very low-density lipoproteins14,15. However, despite several studies have been conducted to dissect the role of this coactivator in healthy and pathological conditions, a clear picture of the PGC-1β contribution to liver disease is still missing16. By using a gain of function mouse model, we unravel the knot of an intricate scenario where PGC-1β is the mastermind able to orchestrate different hepatocellular processes that increase APAP sensitivity, finally leading to acute hepatic failure.
Results
High fat diet fed mice are more prone to APAP hepatotoxicity and mortality
Obesity and related complications arise as a consequence of wrong lifestyle, including malnutrition. Although, usually, several months of high caloric diet are necessary to develop these morbid conditions, short-term exposition to this type of diet is sufficient to induce metabolic changes that can favor liver injury susceptibility.
To explore the effects of a short-term high fat diet on APAP-induced liver injury, we subjected 4-weeks old wild type mice to a diet containing 58% fat-derived calories (HFD) for one month. Mice fed with HFD display higher body weight increase compared to control mice (mice fed with Chow Diet, CD) (Supplementary Figure 1A). Thereafter, we intraperitoneally injected the mice with a toxic dose of APAP (300 mg/kg) and we monitored their survival until 24 hours post-injection. The mortality rate in HFD fed mice was much higher compared to CD fed mice throughout the observation period. At 12 hours after APAP injection, the surviving rate of HFD fed mice was less than 10%, whereas over 80% of mice under control diet remained alive (Fig. 1A), suggesting that even a short-term exposition to HFD worsened the APAP-induced hepatotoxicity and mortality.
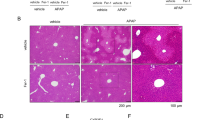
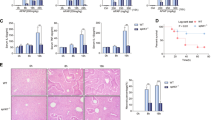
High fat diet fed mice are more prone to APAP hepatotoxicity and mortality. Eight weeks old FVB/N mice fed with HFD or chow diet for 1 month were intraperitoneally injected with either APAP (300 mg/Kg body weight) or equal volume of saline as vehicle control. Survival rate (A) of WT mice fed either with high fat or control diet at different time points after APAP injection. ALT (B) and AST (C) analysis from serum collected 6 hours after injection. Gross morphology (D) of livers in mice of indicated treatments and staining of relative liver sections with H&E (E), and Oil Red O’ (F). Comparison of different groups (n = 6 mice/group) was performed using Two-way ANOVA followed by Bonferroni post-test. Data from groups sharing the same lowercase letters were not significantly different, whereas data from groups with different case letters were significantly different (p < 0.001).
Correspondingly, HFD-APAP treated mice sacrificed 6 hours later displayed higher levels of both alanine aminotransferase (ALT) and aspartate transaminase (AST) (Fig. 1B,C) compared to CD-APAP treated ones. Gross morphology and histological analysis of the liver revealed a worse phenotype in HFD-APAP-treated mice compared to controls, with clear necrotic areas and massive accumulation of large lipid droplets as indicated by H&E and Oil Red O staining, respectively (Fig. 1D–F).
Then, we evaluated GSH and ROS content in liver tissue isolated from CD and HFD mice treated with or without APAP. HFD fed mice injected with saline displayed lower levels of GSH than controls, supporting the idea that fat accumulation conditions per se may contribute to deplete GSH reservoir (Fig. 2B). When injected with APAP, HFD fed mice showed three-times less GSH than chow diet fed ones. Notably, hepatic GSH determination after 30 min displayed the same rate of glutathione depletion between the two groups (Supplementary Figure 1B). Consistently, the analysis of ROS damage to DNA, proteins and lipids (8-Oxo-2′-deoxyguanosine, Nitrotyrosine and 4-Hydroxynonenal, respectively) confirmed the presence of a mild oxidative stress in saline injected mice exposed to HFD. APAP administration worsened the hepatic oxidative stress condition, as indicated by the higher accumulation of oxidized derivatives in APAP-treated HFD fed mice compared to CD fed ones (Fig. 2A). Moreover, the expression of antioxidant genes involved in glutathione metabolism were severely downregulated after HFD and APAP challenge. Specifically, the consumption of diet with high fatty acids content negatively affected the quantity of the catalytic subunit of glutamate cysteine ligase (Gcl-c), coding for the rate limiting enzyme of glutathione synthesis, both after saline and APAP injection (Fig. 2D). Also, when challenged with APAP, mice exposed to HFD showed a significantly downregulation of cytoprotective enzymes coding genes glucose 6-phosphate dehydrogenase (G6pdh) and NAD(P)H dehydrogenase 1 (Nqo1) as compared to their CD counterparts (Fig. 2E–F).
High fat diet fed mice treated with APAP display increase oxidative damage. Eight weeks old FVB/N mice fed with HFD or chow diet for 1 month were intraperitoneally injected with either APAP (300 mg/Kg body weight) or equal volume of saline as vehicle control. Liver tissues were collected 6 hours after injection. (A) Staining of the liver sections with 8-Oxo-DG, NITT, and HNE. (B) GSH determination on liver tissues. Relative PGC-1β expression (C), and of genes related to GSH metabolism, Gcl-c (D), G6pdh (E) and Nqo1 (F) were evaluated by Real Time qPCR. Relative Gene Expression was evaluated in liver specimens from different groups, using TBP as housekeeping gene. Comparison of different groups (n = 6 mice/group) was performed using Two-way ANOVA followed by Bonferroni post-test. Data from groups sharing the same lowercase letters were not significantly different, whereas data from groups with different case letters were significantly different (p < 0.001).
Since one of the major regulators of both hepatic lipids and ROS metabolism is the coactivator Pgc-1β16, we analyzed its expression in our liver specimens. HFD fed mice display a significative induction of hepatic Pgc-1β expression compared to CD ones, that is preserved after APAP treatment (Fig. 2C, Supplementary Figure 1C). Notably, when sacrificed 3 hours after APAP injection, CD fed mice displayed halved Pgc-1β mRNA levels (Supplementary Figure 1D).
Hepatic PGC-1β overexpression exacerbates APAP-induced hepatotoxicity and mortality in mice
Since Pgc-1β is one of the master regulators of liver metabolism and given its increased expression observed when mice were challenged with HFD, we decide to decipher whether PGC-1β induction could contribute to the worsening of APAP-induced hepatotoxicity. Previously generated mice overexpressing PGC-1β specifically in the liver, LivPGC-1β, were subjected to a single dose injection of APAP (300 mg/Kg) 8 weeks after birth, together with matched age control mice.
We monitored the survival of both WT and LivPGC-1β mice for 24 hours after the i.p. injection with 300 mg/kg of APAP. Consistently, we observed a higher mortality rate in transgenic mice compared to WT ones (Fig. 3A). Indeed, three-hours post APAP-injection all the mice overexpressing PGC-1β in the liver died, whereas the survival of WT mice decreased to about 80% only after 24 hours from APAP administration. Accordingly, LivPGC-1β mice displayed significantly higher concentration of serum ALT than control ones (Fig. 3B).
Hepatic PGC-1β overexpression exacerbates APAP-induced hepatotoxicity and mortality in mice. Eight weeks old WT and age matched LivPGC-1β mice were intraperitoneally injected with either APAP (300 mg/Kg body weight) or equal volume of saline as vehicle control and sacrificed. Survival rate (A) of either WT and LivPGC-1β at different time points after APAP injection. Serum levels of ALT (B) measures at various time point. (C) Relative PGC-1β expression evaluated by Real Time qPCR in liver specimens from different groups, using TBP as housekeeping gene. ALT (D) and AST (E) analysis from serum collected 3 hours after injection. Gross morphology of livers in mice of indicated treatments (F) and relative section staining with H&E (G). Comparison of different groups (n = 6 mice/group) was performed using Two-way ANOVA followed by Bonferroni post-test. Data from groups sharing the same lowercase letters were not significantly different, whereas data from groups with different case letters were significantly different (p < 0.001).
To analyze the factors that may affect LivPGC-1β mortality after APAP treatment, we sacrificed 3 hours post-APAP injection. LivPGC-1β mice displayed high PGC-1β expression in the liver also after APAP challenge (Fig. 3C, Supplementary Figure 2). Serum analysis showed that transaminases levels raised in LivPGC-1β mice treated with APAP, confirming that a more severe hepatic liver failure occurred in transgenic mice compare to WT ones (Fig. 3D,E). Liver gross morphology revealed alterations of hepatic parenchyma of WT mice injected with APAP, whereas LivPGC-1β under the same treatment displayed a necrotic liver (Fig. 3F). These observations were further confirmed by histological analysis, indicating a worse liver appearance in transgenic mice challenged with APAP, characterized by the complete loss of lobular structure (Fig. 3G).
Overall, these data suggest that the overexpression of PGC-1β in the liver renders mice more prone to acetaminophen-induced liver injury.
Hepatic PGC-1β overexpression markedly increases lipogenic genes even under APAP challenge
In the liver, PGC-1β plays a major role in the synthesis of new fatty acids and VLDL excretion. To dissect if the hepatic PGC-1β overexpression may heighten APAP response interfering with de novo lipogenesis process, we examined lipid profiles in the four groups. APAP challenge intensified the differences observed in serum lipids profile, being serum triglycerides and cholesterol lower in LivPGC-1β treated mice compared to controls (Fig. 4A,B). Conversely, gene expression analysis displayed increased levels of Fatty Acids Synthase (Fasn) and Acetyl-CoA Carboxylase (Acc) together with the two isoforms of the Diacylglycerol acyltransferase (Dgat1 and Dgat2, respectively) in LivPGC-1β mice compared to controls (Fig. 4C). Thus, the ability of PGC-1β in fostering de novo lipogenesis and triglycerides production is further induced when transgenic mice are challenged with APAP, with concomitant lowered excretion of triglycerides and cholesterol.
Hepatic PGC-1β overexpression markedly increases lipogenic genes even under APAP challenge. Eight weeks old WT and age matched LivPGC-1β mice were intraperitoneally injected with either APAP (300 mg/Kg body weight) or equal volume of saline as vehicle control. Liver tissues were harvested 3 hours later. Analysis of serum triglycerides (A) and cholesterol (B) collected from mice. (C) Relative expression of genes involved in fatty acids synthesis and excretion. Relative Gene Expression was evaluated by Real Time qPCR in liver specimens from different groups, using TBP as housekeeping gene. Comparison of different groups (n = 6 mice/group) was performed using Two-way ANOVA followed by Bonferroni post-test. Data from groups sharing the same lowercase letters were not significantly different, whereas data from groups with different case letters were significantly different (p < 0.01).
Hepatic PGC-1β overexpression increases APAP-induced ROS accumulation due to altered glutathione metabolism
Lipid accumulation per se has been often associated with an increased ROS content. Thus, in the context of acetaminophen hepatoxicity, lipid accretion may aggravate the oxidative status of the liver. However, one of the fundamental roles of PGC-1β relies on the promotion of the antioxidant response, thus limiting the ROS content within a narrow range. Therefore, to understand if PGC-1β was still able to induce ROS scavenger after APAP injection, we analyzed the relative expression of antioxidant genes. LivPGC-1β mice displayed a significative increase of Superoxide dismutase 2 (Sod2), Thioredoxin 2 (Txn2) and Peroxiredoxin 3 (Prdx3) mRNA levels, that was still preserved after APAP injection. On the contrary, WT mice showed a small but significant reduction of these mRNA levels when challenged with the drug (Fig. 5A). ROS scavengers induction lowered the oxidative stress in LivPGC-1β mice compared to controls after saline injection. Indeed, the evaluation of ROS-mediated lipid damage exhibited prominent HNE accumulation in WT mice, with clear marked nuclei, possible due to HNE covalent adducts with nucleophilic functional groups in nucleic acids17. Surprisingly, this protective effect was completely lost after treatment with APAP, with the transgenic mice displaying a remarkable HNE deposition (Fig. 6A). The greater extent of oxidative damage in LivPGC-1β mice treated with APAP compared to WT ones is also indicated by the 8-Oxo-2′-deoxyguanosine and the Nitrotyrosine staining, markers of ROS-byproducts affecting DNA and proteins, respectively (Fig. 6A).
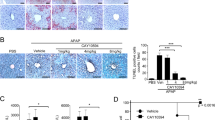
Hepatic PGC-1β overexpression exacerbates APAP-toxic damage due to altered glutathione metabolism. Gene expression analysis on liver specimens isolated from eight weeks old WT and age matched LivPGC-1β mice 3 hours after APAP (300 mg/Kg body weight) or saline treatment. Relative expression of antioxidant genes involved in ROS detoxification (A), of different Cytochrome P isoforms involved in APAP bioactivation (B), of Glutathione S-transferase (C) and of genes implicated in GSH biosynthesis (D). Relative Gene Expression was evaluated by Real Time qPCR in liver specimens from different groups, using TBP as housekeeping gene. Comparison of different groups (n = 6 mice/group) was performed using Two-way ANOVA followed by Bonferroni post-test. Data from groups sharing the same lowercase letters were not significantly different, whereas data from groups with different case letters were significantly different (p < 0.01).
Hepatic PGC-1β overexpression increases APAP-induced ROS byproducts accumulation. Analysis of oxidative stress on liver specimens isolated from eight weeks old WT and age matched LivPGC-1β mice 3 hours after APAP (300 mg/Kg body weight) or saline treatment. 8-Oxo-DG, NITT and HNE staining (A) of liver sections isolated from WT and LivPGC-1β mice subjected to different treatments. (B) GSH determination from liver tissues. Comparison of different groups (n = 6 mice/group) was performed using Two-way ANOVA followed by Bonferroni post-test. Data from groups sharing the same lowercase letters were not significantly different, whereas data from groups with different case letters were significantly different (p < 0.01).
In line with these observations, we found halved concentration of hepatic GSH in APAP-treated LivPGC-1β mice compared to control ones (Fig. 6B). To explore whether the loss of GSH reservoir, the major scavenger system against oxidative stress caused by APAP, was attributable to an increased acetaminophen metabolization or to a decreased glutathione synthesis, we investigated the relative expression of the main genes involved in these processes. The analysis of different isoforms of cytochrome P450 (Cyp2E1, Cyp3A1 and Cyp4A10), involved in bioactivation of APAP into NAPQI, revealed a significant higher expression in transgenic mice challenged with APAP compared to control ones (Fig. 5B). Remarkably, the overexpression of PGC-1β fostered the increase of Glutathione S-transferases (Gstt, Gstp), involved in the detoxification of NAPQI by conjugation with GSH (Fig. 5C). Therefore, it is possible that overexpression of PGC-1β not only induced a faster metabolization of the drug, with a concomitant accumulation of highly reactive intermediates, but also contributed to a rapid GSH depletion by Glutathione S-transferases.
Nonetheless, after APAP treatment the expression of antioxidant genes with a prominent role in the glutathione metabolism (Gcl-c, G6pdh and Nqo1) raised in WT mice, while only modestly increased in LivPGC-1β littermates (Fig. 5D). Particularly, the mRNA levels of Gcl-c, the first-rate limiting enzyme of glutathione synthesis, were already low in LivPGC-1β injected with saline, suggesting a possible negative correlation between coactivator and enzyme expression. Overall, these data suggested that mice overexpressing PGC-1β display deleterious effects when challenged with APAP, since they failed in the induction of genes involved in GSH synthesis, thereby limiting the GSH reservoir to contrast acetaminophen overdose.
Discussion
Acetaminophen (APAP) is a painkiller drug, extensively used worldwide. However, high dosage of APAP induces rapid necrosis of hepatic tissue, that could end up with ill-fated outcome and patients’ death. Although it is well known that these adverse events of acetaminophen use are mostly attributable to the depletion of GSH reservoir18, it is still to be defined why some people are more sensitive to the APAP side effects and how to predict the fatal end.
Recent observations pointed out that obesity and related metabolic diseases may affect APAP liver injury. However, both clinical investigations and experimental studies reported contradictory results, in which obese and NAFLD subjects displayed either higher or lower hepatotoxicity after APAP administration6,9,19,20,21. Thus, an unequivocal mechanism whereby APAP could be more toxic in obese condition and related disorders is still to be determined.
It is well known that malnutrition plays a fundamental role in overweight and obesity. Diets containing an excess or imbalance of energy can lead to overnutrition and fat accumulation, that predispose to body weight increase. Here, we showed that a short but extreme oversupply of fatty acids with the diet is able to worsen APAP administration. Mice rapidly died due to a drastic lowering of GSH supply, possibly ascribable to the decreased expression levels of several enzymes involved in glutathione biosynthesis. Interestingly, we found high hepatic expression of PGC-1β in mice that received high fat diet independent of drug treatment, whereas APAP per se halved the mRNA levels of PGC-1β in a chow diet background, thus implying a kind of protective mechanism exerted in normal conditions.
The coactivator PGC-1β belongs to the family of PGC-1s coactivators, generally considered as master regulators of mitochondrial biogenesis and oxidative metabolism as well as of antioxidant response22. In the liver, PGC-1β has been shown to play a key role in the de novo lipogenesis and triglycerides metabolism12,14,15. Former experiments on LivPGC-1β mice indicate that hepatic overexpression of PGC-1β may differently impact on metabolic pathways. Indeed, selective activation of PGC-1β within the hepatocytes protects the liver from lipids overload and progression to fibrosis, due to its ability to induce mitochondrial oxidative phosphorylation, fatty acids β-oxidation and citrate cycle, while decreasing oxidative stress and promoting triglycerides excretion in the bloodstream15. On a different angle, when subjected to DEN-induced hepatocarcinogenesis, overexpression of PGC-1β renders mice more prone to hepatocarcinoma development possibly by enhancing the expression of genes involved in fatty acids and triglycerides synthesis as well as by limiting ROS accumulation via increased antioxidant response12.
Previous studies demonstrated that the other member of the PGC-1’s family, PGC-1α, protects the liver from acetaminophen-induced liver injury by inducing the expression of Nrf2-regulated anti-oxidant genes23. Moreover, the induction of PGC-1α after APAP hepatotoxicity promotes mitochondrial biogenesis that finally attenuates the injury and stimulates liver regeneration24. Of notice, the hepatic overexpression of PGC-1β leads to an acute liver failure after subtoxic dose of APAP, inducing mice death three hours post-injection. These evidences highlighted once more the divergent role of the two coactivators in the liver, with PGC-1α being more involved in catabolic pathways and PGC-1β inducing anabolic processes, such as the synthesis of new fatty acids.
If APAP injection is able to stimulates fatty acids accretion per se4, the overexpression of PGC-1β boosts the expression of genes involved in de novo lipogenesis and triglycerides synthesis, thus contributing to the impairment of normal liver functions. Moreover, PGC-1β overexpression induces higher hepatotoxicity also exacerbating the oxidative stress that finally leads to liver failure and mice death.
Hepatic oxidative stress is the principal mediator of APAP induced liver injury. N-Acetyl-p-benzoquinone imine (NAPQI), the toxic metabolite of APAP, besides its intrinsic ability to form aspecific chemical adducts with proteins, promotes the excessive accumulation of ROS mostly depleting the GSH pool that it is required for its detoxification. This, in turn, can cause alterations of mitochondria and nucleic acids, ceasing the ATP production and contributing to liver necrosis1,25,26. We demonstrated that PGC-1β overexpression leads to an increase of cytochrome P450 isoforms (Cyp) which results in the intensification of NAPQI production, with consequent rising of the oxidative stress. Beside NAPQI, Cyp can also directly increase oxidative stress by consuming NADPH during their catalytic cycle.
At the same time, PGC-1β failed to induce the expression of enzymes involved in glutathione biosynthesis. The glutamate-cysteine ligase catalytic subunit (Gcl-c), the main controlling step of GSH synthesis is less expressed in mice overexpressing PGC-1β at basal conditions. Moreover, whereas its mRNA levels rapidly rise in WT mice after APAP injection, in LivPGC-1β we detected just a feeble increase of Gcl-c, probably not sufficient to enrich the GSH supply useful to limit APAP damage. Surprisingly, one of the inducers of Gcl-c expression is 4-Hydroxynonenal (HNE), the major end product of lipid peroxidation27,28. HNE covalently binds to functional groups of proteins, nucleic acids and membrane lipids, driving to serious cell damage, and, ultimately, cell death17. In mice with hepatic overexpression of PGC-1β, HNE amount is kept low in basal conditions, thus contributing to the reduced expression levels of Gcl-c observed. Conversely, after APAP injection in hepatic specific PGC-1β overexpressing mice, the high expression of primary ROS scavengers is not able to counteract the hepatic oxidative stress induced by APAP, due to the collapse of GSH reservoir caused by the lowered Gcl-c expression and by the massive utilization of GSH for NAPQI detoxification performed by Glutathione S-Transferases.
Despite the enhanced HNE staining observed in our samples, we have to highlight on one hand that lipid peroxidation per se is not always recognized as relevant in APAP hepatotoxicity, and its contribution to liver injury after acetaminophen exposure is still debated3,29,30,31,32. Also, it may be possible that the increased HNE staining is a specific consequence of the mouse strain used in our experiments, given the fact that FVBN mouse strain might be more sensitive than C57BL/6 J one33,34. However, it is also plausible that the enhanced lipid peroxidation observed is the resultant of a combined effect of APAP and predisposition to liver steatosis and its sequelae that once more contribute to liver failure35. Thereby, even if lipid peroxidation per se is insufficient to cause cell death, it may be considered as evidence for oxidative stress that contribute to liver injury. Indeed, when hepatic PGC-1β levels are high, mice liver appeared intensely affected by oxidative stress, as depicted by extensive accumulation of ROS byproducts (8-Oxo-DG, NITT and HNE), that is suggestive of the prelude to hepatic necrosis and death.
Notably, two of the most important transcription factors coactivated by PGC-1β are Nrf2 (Nuclear Factor E2-Related Factor 2) and LXRs (Liver X Receptors)16. Nrf2 is mainly implicated in antioxidant response, whereas LXR controls lipid metabolism36,37. Though, recently it has been pointed out that the molecular pathways controlled by these two transcription factors not only are highly overlapping, with Nrf2 able to modulate genes involved in lipid metabolism and LXR involved in the promotion of glutathione transferase, but they are also mutually interconnected38,39,40. In the present study, high level of PGC-1β induced the expression of genes involved in lipid metabolism and detoxification, but failed to promote the expression of Nrf2 regulated genes involved in glutathione synthesis. Lastly, it has been described that hepatic injury caused by APAP is lower in mice with elevated expression of Nrf2 and in those with constitutive activation of LXR39,41. Therefore, it is plausible that the effect of PGC-1β overexpression we observed did not rely only on these two transcription factors, but that it was mediated also by other factors, that finally contributed to the deleterious outcome.
Overall, in the present study we highlight that short-term consumption of diets enriched in fatty acids may worsen the risk of hepatic failure due to APAP consumption. Lipidic metabolites or intermediate ligands can be able to activate PGC-1β, mimicking our transgenic mouse model, thus contributing to exacerbate the risk of APAP hepatotoxicity. Unfortunately, the impossibility to study the direct effect on humans, due to obvious reasons, is one of the major limitations of this study. However, a healthy life style, characterized by proper consumption of lipids and carbohydrates that would limit PGC-1β induction, might be a preventive strategy to reduce APAP induced liver damage in human. Our data depict an interesting scenario, in which coactivator PGC-1β is able to increase APAP sensitivity, finally leading to acute hepatic failure.
Materials and Methods
Study design
This study was firstly designed to test the hypothesis that the administration of a diets enriched in fatty acids for a short period of time has the potential to worsen APAP-induced liver injury. Since we showed that HFD consumption induces PGC-1β expression, and shortly after injection, APAP treatment halved PGC-1β levels, to validate the PGC-1β as a putative biomarker we examined the effect of APAP treatment on hepatic-specific transgenic mouse model. We demonstrated that PGC-1β limits glutathione production and negatively affect oxidative stress, finally resulting in a severe liver damage. Sample sizes and P values are indicated in the text, figure legends, or figures. The sample sizes of the experiments were selected on the basis of previous experience. Data reported included all samples analyzed. No samples or data were excluded after analysis. Experiments were carried out in an unblinded fashion except for analyses of immunohistochemistry images.
Animal studies
All animals were housed in a controlled environment with 12 hours light and dark cycles, with free access to food and water. For high fat feeding, four weeks-old wild type (WT) FVBN male mice were switched on diet containing 58% fat-derived calorie (D12331, Research Diets) for one month. A total of four groups of 6/7 male mice each has been tested. Mice were randomized prior treatment with the diet and then allocated in different cages (3/4 mice per cage).
Male LivPGC-1β mice15 and wild type (WT) controls in FVBN background were used for study the effect of PGC-1β overexpression. A total of four groups of 6/7 male mice each has been tested. Mice were randomized at 4 weeks of age and then allocated in different cages (3/4 mice per cage).
To induce APAP hepatotoxicity, 8 weeks-old animals were fasted for 16 hours before the experiments. An APAP solution freshly-prepared by dissolving with heating acetaminophen (Sigma-Aldrich) in saline solution was administrated into mice by intraperitoneal injection at 300 mg/Kg. Saline solution (0.90% w/v of NaCl) was used as control. The experimental protocol was approved by the Ethical Committee of the Consorzio Mario Negri Sud and also was certified by the Italian Ministry of Health according to internationally accepted guidelines and regulation for the animal care.
RNA extraction and quantitative real-time PCR analysis
All the tissues were harvested at indicated time points after APAP injection. Liver were snapped freezing under liquid nitrogen and homogenized in QIAzol reagent (Qiagen) using Tissue Lyser (Qiagen). Total RNA was isolated by following the manufacture’s instruction. To avoid possible DNA contaminations, RNA was treated with DNase (ThermoScientific). cDNA was synthesized retro-transcribing 4 μg of total RNA in a total volume of 400 μl using High Capacity DNA Kit (TehrmoScientific) in accordance to the manufacture’s instruction. Real Time qPCR was performed using SybrGreen Master Mix (ThermoScientific) with various sets of primers for specific genes. The PCR reactions were performed on the Studio Quant5 (ThermoScientific). Relative gene expression levels were analyzed using the ΔΔCt method, using TBP as housekeeping gene.
GSH assay
For GSH assay in vivo, liver specimens were collected at different time points as indicated. Detection of GSH abundance was performed using Glutathione Assay kit (Sigma-Aldrich) following the manufacturer’s instructions. For GSH determination 30 minutes after APAP injection, liver tissue (50 mg) was homogenized with 20 volumes of 5% 5-Sulfosalicylic Acid Dihydrate (500 µL) (Sigma-Aldrich) and centrifuged at 12,000 g for 10 minutes at 4 °C. Total glutathione levels were measured from the supernatants using a glutathione detection kit according to the manufacturer’s instructions (Enzo Life Sciences)42.
Serum analysis
At the time of sacrifice, blood samples were collected in lithium-heparin collection tubes and subsequently centrifuged to obtain serum. Serum levels of ALT and AST were measured using a colorimetric kit (BioQuant, Heidelberg, Germany) according to manufacturer’s instructions.
Histological and immunohistochemical analysis
Tissue specimens were fixed in 10% formalin for 12 to 24 h, dehydrated, and paraffin embedded. Liver sections were stained with H&E following standard protocols. For immunohistochemistry, sections were subjected to antigen retrieval by boiling the slides in sodium citrate pH 6 (Sigma Aldrich) for 15 min and then permeabilized in phosphate-buffered saline (PBS) with 0.25% TritonX-100 for 5 min. Subsequently, after 10 min incubation at room temperature in protein blocking solution (Dako, Glostrup, Denmark), sections were incubated at 4 °C for 48 hours with the anti-8-Hydroxyguanosine antibody (LifeSpan Bioscience Inc, Seattle, Washington, USA). Sections were washed in PBS for 15 min and incubated for 25 min at room temperature with DAKO real EnVision detection system Peroxidase/DAB + (Dako) according to manufacturer’s instruction. Coverslips were mounted with Permount and evaluated under a light microscope. To evaluate lipid accumulation, serial 4.5 μm cryosections from liver specimens embedded in OCT compound (Tissue-Tek Sakura, Torrance, CA) were stained with Oil Red O (Sigma-Aldrich) and hematoxylin to counterstain nuclei.
Western blot analysis
Total liver protein lysates were separates on 10% and 12% SDS–polyacrylamide gel and transferred on nitrocellulose membrane. Membranes were blocked with 5% BSA in TBS–0.01% Tween 20 and probed with specific antibodies against PGC-1β (ab176328) and GCL-c (ab53179) purchased from Abcam. Nuclear encoded β-actin (Abcam) were used as loading control. Membranes were finally incubated with HRP conjugated secondary antibodies and developed with a chemiluminescent reagent (Biorad, California, USA).
Statistical analysis
The results are expressed as mean ± SEM. All the statistical analyses were performed using GraphPad Prism software (v5.0; GraphPad Software Inc). Comparisons of two groups were performed using Mann-Whitney U test. Comparison of four groups were performed using two-way ANOVA followed by Bonferroni post-test. At least p-value < 0.05 was considered statistically significant.
References
Hinson, J. A., Roberts, D. W. & James, L. P. Mechanisms of acetaminophen-induced liver necrosis. Handb.Exp.Pharmacol., 369–405, (2010).
Dahlin, D. C., Miwa, G. T., Lu, A. Y. & Nelson, S. D. N-acetyl-p-benzoquinone imine: a cytochrome P-450-mediated oxidation product of acetaminophen. Proceedings of the National Academy of Sciences of the United States of America 81, 1327–1331 (1984).
Du, K., Ramachandran, A. & Jaeschke, H. Oxidative stress during acetaminophen hepatotoxicity: Sources, pathophysiological role and therapeutic potential. Redox.Biol. 10, 148–156 (2016).
Fromenty, B. Drug-induced liver injury in obesity. J.Hepatol. 58, 824–826 (2013).
Begriche, K., Massart, J., Robin, M. A., Borgne-Sanchez, A. & Fromenty, B. Drug-induced toxicity on mitochondria and lipid metabolism: mechanistic diversity and deleterious consequences for the liver. J.Hepatol. 54, 773–794 (2011).
Michaut, A., Moreau, C., Robin, M. A. & Fromenty, B. Acetaminophen-induced liver injury in obesity and nonalcoholic fatty liver disease. Liver Int. 34, e171–e179 (2014).
Aubert, J. et al. Differences in early acetaminophen hepatotoxicity between obese ob/ob and db/db mice. J.Pharmacol.Exp.Ther. 342, 676–687 (2012).
A., vR. et al. Morbidly Obese Patients Exhibit Increased CYP2E1-Mediated Oxidation of Acetaminophen. Clin.Pharmacokinet. 55, 833–847 (2016).
Myers, R. P. & Shaheen, A. A. Hepatitis C, alcohol abuse, and unintentional overdoses are risk factors for acetaminophen-related hepatotoxicity. Hepatology 49, 1399–1400 (2009).
Villena, J. A. New insights into PGC-1 coactivators: redefining their role in the regulation of mitochondrial function and beyond. FEBS J. 282, 647–672 (2015).
Bellafante, E. et al. PGC-1beta promotes enterocyte lifespan and tumorigenesis in the intestine. Proc.Natl.Acad.Sci.USA 111, E4523–E4531 (2014).
Piccinin, E. et al. Hepatic peroxisome proliferator-activated receptor gamma coactivator 1beta drives mitochondrial and anabolic signatures that contribute to hepatocellular carcinoma progression in mice. Hepatology 67, 884–898 (2018).
Gali Ramamoorthy, T. et al. The transcriptional coregulator PGC-1beta controls mitochondrial function and anti-oxidant defence in skeletal muscles. Nat.Commun. 6, 10210 (2015).
Lin, J. et al. Hyperlipidemic effects of dietary saturated fats mediated through PGC-1beta coactivation of SREBP. Cell 120, 261–273 (2005).
Bellafante, E. et al. Hepatic-specific activation of peroxisome proliferator-activated receptor gamma coactivator-1beta protects against steatohepatitis. Hepatology 57, 1343–1356 (2013).
Piccinin, E., Villani, G. & Moschetta, A. Metabolic aspects in NAFLD, NASH and hepatocellular carcinoma: the role of PGC1 coactivators. Nature reviews. Gastroenterology & hepatology 16, 160–174 (2019).
Huang et al. HIF-1-mediated suppression of acyl-CoA dehydrogenases and fatty acid oxidation is critical for cancer progression. Cell Rep. 8, 1930–1942 (2014).
Saito, C., Zwingmann, C. & Jaeschke, H. Novel mechanisms of protection against acetaminophen hepatotoxicity in mice by glutathione and N-acetylcysteine. Hepatology 51, 246–254 (2010).
Kucera, O. et al. Susceptibility of rat non-alcoholic fatty liver to the acute toxic effect of acetaminophen. Journal of gastroenterology and hepatology 27, 323–330 (2012).
Rutherford, A. et al. Influence of high body mass index on outcome in acute liver failure. Clinical gastroenterology and hepatology: the official clinical practice journal of the American Gastroenterological Association 4, 1544–1549 (2006).
Ito, Y., Abril, E. R., Bethea, N. W., McCuskey, M. K. & McCuskey, R. S. Dietary steatotic liver attenuates acetaminophen hepatotoxicity in mice. Microcirculation 13, 19–27 (2006).
Lin, J., Handschin, C. & Spiegelman, B. M. Metabolic control through the PGC-1 family of transcription coactivators. Cell Metab 1, 361–370 (2005).
Ye, D. et al. Fibroblast growth factor 21 protects against acetaminophen-induced hepatotoxicity by potentiating peroxisome proliferator-activated receptor coactivator protein-1alpha-mediated antioxidant capacity in mice. Hepatology 60, 977–989 (2014).
Du, K. et al. Induction of mitochondrial biogenesis protects against acetaminophen hepatotoxicity. Food and chemical toxicology: an international journal published for the British Industrial Biological Research Association 108, 339–350 (2017).
Jaeschke, H., McGill, M. R. & Ramachandran, A. Oxidant stress, mitochondria, and cell death mechanisms in drug-induced liver injury: lessons learned from acetaminophen hepatotoxicity. Drug Metab Rev. 44, 88–106 (2012).
Masubuchi, Y., Suda, C. & Horie, T. Involvement of mitochondrial permeability transition in acetaminophen-induced liver injury in mice. J.Hepatol. 42, 110–116 (2005).
Zhang, H., Court, N. & Forman, H. J. Submicromolar concentrations of 4-hydroxynonenal induce glutamate cysteine ligase expression in HBE1 cells. Redox report: communications in free radical research 12, 101–106 (2007).
Iles, K. E. & Liu, R. M. Mechanisms of glutamate cysteine ligase (GCL) induction by 4-hydroxynonenal. Free Radic.Biol.Med. 38, 547–556 (2005).
Wendel, A., Feuerstein, S. & Konz, K. H. Acute paracetamol intoxication of starved mice leads to lipid peroxidation in vivo. Biochemical pharmacology 28, 2051–2055 (1979).
Knight, T. R., Fariss, M. W., Farhood, A. & Jaeschke, H. Role of lipid peroxidation as a mechanism of liver injury after acetaminophen overdose in mice. Toxicological sciences: an official journal of the Society of Toxicology 76, 229–236 (2003).
Jaeschke, H. & Ramachandran, A. Oxidant Stress and Lipid Peroxidation in Acetaminophen Hepatotoxicity. Reactive oxygen species 5, 145–158 (2018).
James, L. P., Mayeux, P. R. & Hinson, J. A. Acetaminophen-induced hepatotoxicity. Drug metabolism and disposition: the biological fate of chemicals 31, 1499–1506 (2003).
Haluzik, M. et al. Genetic background (C57BL/6J versus FVB/N) strongly influences the severity of diabetes and insulin resistance in ob/ob mice. Endocrinology 145, 3258–3264 (2004).
Pugh, P. L., Ahmed, S. F., Smith, M. I., Upton, N. & Hunter, A. J. A behavioural characterisation of the FVB/N mouse strain. Behavioural brain research 155, 283–289 (2004).
Morita, M. et al. Fatty liver induced by free radicals and lipid peroxidation. Free radical research 46, 758–765 (2012).
Nguyen, T., Nioi, P. & Pickett, C. B. The Nrf2-antioxidant response element signaling pathway and its activation by oxidative stress. The Journal of biological chemistry 284, 13291–13295 (2009).
Wang, B. & Tontonoz, P. Liver X receptors in lipid signalling and membrane homeostasis. Nature reviews. Endocrinology 14, 452–463 (2018).
Huang, J., Tabbi-Anneni, I., Gunda, V. & Wang, L. Transcription factor Nrf2 regulates SHP and lipogenic gene expression in hepatic lipid metabolism. American journal of physiology. Gastrointestinal and liver physiology 299, G1211–1221 (2010).
Saini, S. P. et al. Activation of liver X receptor increases acetaminophen clearance and prevents its toxicity in mice. Hepatology 54, 2208–2217 (2011).
Kay, H. Y. et al. Nrf2 inhibits LXRalpha-dependent hepatic lipogenesis by competing with FXR for acetylase binding. Antioxidants & redox signaling 15, 2135–2146 (2011).
Chan, K., Han, X. D. & Kan, Y. W. An important function of Nrf2 in combating oxidative stress: detoxification of acetaminophen. Proceedings of the National Academy of Sciences of the United States of America 98, 4611–4616 (2001).
Vergara, D. et al. Resveratrol Modulation of Protein Expression in parkin-Mutant Human Skin Fibroblasts: A Proteomic Approach. Oxidative medicine and cellular longevity 2017, 2198243 (2017).
Acknowledgements
We thank A. Sciacovelli, A. Contursi and M. Cariello for their invaluable help during the study. We also thank J. Hardfeldth for carefully reading the manuscript. Antonio Moschetta is funded by Italian Association for Cancer Research (AIRC, IG 18987), MIUR PRIN 2017J3E2W2_002, JPI-EU FATMAL.
Author information
Authors and Affiliations
Contributions
E.P. contributed to study design, performed experiments, analyzed data and wrote the paper; S.D. contributed to study design, performed experiments and data analysis; C.P., M.A., M.C.V., and A.F. performed experiments; E.B. generated the transgenic mouse model; G.V. contributed to paper writing; A.M. designed the study, supervised the project and contributed to paper writing.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Piccinin, E., Ducheix, S., Peres, C. et al. PGC-1β Induces Susceptibility To Acetaminophen-Driven Acute Liver Failure. Sci Rep 9, 16821 (2019). https://doi.org/10.1038/s41598-019-53015-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-019-53015-6
This article is cited by
-
Unraveling the effect of intra- and intercellular processes on acetaminophen-induced liver injury
npj Systems Biology and Applications (2022)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.