Abstract
Joint deterioration and associated chronic pain are common among people with haemophilia (PWH), having an impact on quality-of-life. Though non-pharmacological strategies are recommended, psychological interventions to promote pain control and quality-of-life have scarcely been tested in haemophilia. This randomised controlled pilot trial aimed to assess feasibility, acceptability and effectiveness of hypnosis for pain management and promotion of health-related quality-of-life (HRQoL) among PWH. Twenty adults were randomised either to four weekly hypnosis sessions plus treatment-as-usual (experimental group; EG) or treatment-as-usual only (control group; CG). Participants completed sociodemographic and clinical assessment, measures of pain, HRQoL and emotional distress before (T1) and after (T2) intervention. Changes were analysed by calculating the differences between T1 and T2, and the groups were compared through independent-sample t tests (or chi-squared). Retention rates (90%) and analysis of patient satisfaction showed good acceptability and feasibility of the intervention. The EG (n = 8) had a higher reduction on pain interference than the CG (n = 10) (d = −0.267). A higher improvement on HRQoL (EQ-5D index: d = 0.334; EQ-5D VAS: d = 1.437) and a tendency towards better haemophilia-related quality-of-life (A36-Hemofilia QoL) were also evident in the EG. This is the first study showing the effectiveness of hypnosis to reduce pain interference and promote HRQoL among PWH.
Similar content being viewed by others
Introduction
Haemophilia is an X-linked rare bleeding disorder, resulting from a deficiency in blood coagulation factor VIII (haemophilia A) or IX (haemophilia B), and characterized by a pattern of spontaneous bleeding episodes that most often occur in the muscles (haematomas) or joints (haemarthrosis)1. The frequency of spontaneous bleeds is associated with disease severity, which is classified according to plasma levels of clotting factor activity (severe: <1% of normal factor level; moderate: 1 to 5%; mild: 5 to 40%)2. Intravenous administration of factor replacement concentrate is the mainstay of treatment, delivered to stop bleeds (on-demand) or to prevent its occurrence (prophylaxis)3. Prophylaxis can potentially prevent bleeds altogether, but its use as a routine treatment since childhood has only been considered a standard of care during the last two decades. As a consequence, most adults with severe haemophilia did not benefit from prophylaxis while growing up and are now afflicted with some degree of joint damage, due to frequent haemarthrosis and lifelong accumulation of intraarticular blood4.
Haemarthrosis are painful events that, if repeated, progressively contribute to the development of chronic haemophilic arthropathy, characterized by irreversible joint damage, disability and chronic pain5. Pain is therefore a very relevant issue among people with haemophilia (PWH), with studies reporting a prevalence of chronic pain ranging from 35 to 66%6,7,8,9, and about half the participants in some investigations complaining of daily arthritic pain10,11. In addition, it has been demonstrated that PWH who experience more intense or frequent pain have lower quality-of-life8,10,12,13, further highlighting the unquestionable relevance of an adequate pain management in this field. Yet, haemophilia-related pain is still under-recognized and suboptimally treated14,15, and several authors have called on the need to improve its assessment and management, advocating for a combination of pharmacological and non-pharmacological techniques7,16,17.
Besides clinical variables (e.g. bleeding rate, joint status, pain), health-related quality-of-life (HRQoL) is a valuable outcome of research to capture patients perspective on their health. This is even more relevant in such burdensome conditions like haemophilia, with lifelong complications and demanding treatments18. Indeed, research on this topic has shown that PWH have lower HRQoL than the general population12,19,20,21. This has contributed to current haemophilia guidelines, which emphasize quality-of-life promotion as a relevant endpoint of comprehensive care22. However, the few interventional studies assessing HRQoL outcomes among adult PWH have mainly focused on the effects of physical exercise and physiotherapy interventions23,24, or on the impact of different factor replacement treatment modalities25,26. To our knowledge, the efficacy of psychological interventions specifically aiming at improving pain management and quality-of-life among PWH has never been tested, leaving a significant gap in evidence-based treatments targeting these outcomes.
The existing research focusing on psychological interventions among PWH is outdated and has focused mainly on hypnosis, showing positive results for disease management27,28,29. Indeed, the medical use of hypnosis is approved since 1955 by the British Medical Association30 and is recognized as an effective intervention to help manage chronic pain31, also contributing to improve HRQoL across distinct medical fields32,33,34. In haemophilia, the promising results that have been reported using hypnosis make the discontinuity of this line of research somewhat surprising, and thus encourage the development of investigations to further explore its usefulness.
The aim of this work was to assess the effectiveness of a hypnosis intervention for pain management and promotion of HRQoL among people with haemophilia. Since this is a rare disease, with an estimated number of 700 cases in Portugal35, we conducted a pilot trial to address if a future randomised controlled trial (RCT), with a larger sample, would be feasible and well-accepted by patients.
Results
Feasibility and acceptability
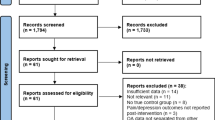
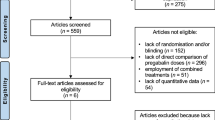
Patient screening and assessment (pre and post-intervention) occurred from January to June 2018. The flow of patients through the study, reasons for ineligibility and refusals are shown in Fig. 1. Thirty-five adult patients with haemophilia were identified as eligible. Of these, 20 accepted to participate and met the inclusion criteria, and were therefore randomised to one of the study groups. One participant from the CG was excluded because he underwent orthopaedic surgery during the duration of the trial, and one participant in the EG dropped out of the intervention after one session due to unavailability to attend the remaining sessions. Another participant who had been initially allocated to the EG also expressed unavailability to attend the intervention sessions, but was willing to change to the CG. Thus, the final analysed sample included 8 participants in the EG and 10 participants in the CG.
Retention rate in the pilot trial was 90%, with participants in the EG (n = 8) attending all hypnosis sessions. Concerning satisfaction with intervention, 2 (25%) participants in the EG revealed to be “satisfied” and 6 (75%) “very satisfied” with the intervention. All participants (8, 100%) stated they felt “a lot” better after the four sessions, said they “agree” that these interventions would be useful in haemophilia centres and also “agree” that they would wish to participate in further sessions, if available.
No unanticipated harm or detrimental effects of intervention were reported.
Sociodemographic and clinical characteristics
Baseline sociodemographic and clinical participant characteristics are summarized in Table 1. The groups were not statistically different on any of these variables, although a large effect size (ES) was found for the differences on age (d = −0.879) and number of affected joints (d = −0.985); and a medium ES for the number of painful locations (d = −0.770).
No statistically significant differences were found between the groups at baseline on the analysed outcomes, except on the “treatment difficulties” subscale of the A36 Hemofilia-QoL (t(16) = 2.52; p = 0.023; d = 1.27) (results not shown). This subscale score revealed higher difficulties for the EG.
Comparison of pre/post-intervention changes among groups
Table 2 shows the differences from baseline to post-intervention in each outcome for each group, comparing them. Concerning work absences, the number of days missed from work in the previous month decreased in the EG (Δ = 5.80 days; SD = 13.57) and had a slight increase in the CG (Δ = −0.83; SD = 2.04), corresponding to a medium ES (d = −0.656).
Regarding the clinical parameters under assessment, pain interference yielded significant results (d = −0.267), decreasing in both groups, but with a higher reduction in the EG (Δ = 0.75; SD = 1.53) than in the CG (Δ = 0.41; SD = 0.99). The differences on pain intensity from pre to post intervention were not significant (d = 0.195) between the groups.
In what concerns general HRQoL, there was a statistically significant difference between groups on EQ-5D VAS (t(16) = 3.03, p = 0.008, d = 1.437), with a mean 13.75 (SD = 10.94) point improvement in the EG and a mean 7.50 (SD = 17.20) decrease in the CG. EQ-5D index scores increased in both groups, yet with a slightly higher improvement in the EG (small ES, d = 0.334). Concerning haemophilia-related quality-of-life, the EG revealed a global tendency towards better HRQoL at post-intervention, with a higher difference (larger improvements) than the CG on the global score (ES = 0.335) and in 4 of the 9 specific dimensions. The higher effect sizes for these improvements in the EG were found on “treatment difficulties” (large ES, d = 0.852) and “daily activities” (medium ES, d = 0.581). Despite having small effect sizes, “physical health” (d = 0.296) and “joints” (d = 0.297) also yielded higher improvements in the EG, compared with the CG. Finally, the magnitude of the differences concerning depression and anxiety was not significant (depression, d = 0.097; anxiety, d = 0.009).
Discussion
This manuscript reports a randomised controlled pilot trial aiming to assess the feasibility, acceptability and effectiveness of a hypnosis intervention among people with haemophilia (PWH). Findings revealed, for the first time, the specific benefits of hypnosis in diminishing pain interference and in improving health-related quality-of-life (HRQoL) among PWH.
Important practical insights were also retrieved from this study, namely concerning the feasibility of a future randomized controlled trial (RCT). Considering the rarity of this disease and the inclusion criteria for participation, the main challenge in implementing a future RCT would be the recruitment of a big enough sample size to guarantee statistical power. In this case, implementing a multi-centre trial could be a potential solution. From this pilot study, it also became clear that time availability to participate in the intervention sessions is a relevant constraint, particularly for participants who have a full-time occupation. In this sense, it seems that accounting for individual allocation preferences could be advantageous to guarantee bigger sample sizes, namely by adopting patient preference designs. In these, participants with a strong preference for one of the arms are assigned to it, while the others are randomised between the groups. This approach contributes to improve recruitment rates and is more advantageous when active involvement of patients is warranted, without compromising internal and external validity36,37.
Globally, this study showed that it is feasible to develop and implement an RCT with PWH that is based on hypnosis. The participants in the experimental group (EG) attended all sessions (except one person that discontinued the intervention after the first session and was thus excluded from the study), demonstrating good acceptability of the intervention. All participants reported to be satisfied with the intervention and expressed the wish to keep attending, if more sessions were available.
Former studies have previously reported the implementation of hypnosis among PWH, with positive results in controlling bleeding, reducing pain and alleviating stress27,28,29. Other investigations, describing imagery and relaxation techniques similar to hypnosis, have also achieved reductions in arthritic pain for PWH undergoing intervention38,39. These were encouraging results for the use of hypnosis as an adjunctive strategy for haemophilia care, but the fact that most conclusions were based on case studies and lacked a rigorous methodology warrants further research to establish more definitive conclusions40. Surprisingly, the last reports of studies analysing the efficacy of hypnosis in the haemophilia field date from the early 90’s. To our knowledge, no more recent research was conducted on this subject, hence the relevance of further exploring this issue.
Previous research has described reductions on pain intensity following hypnosis across a variety of other chronic pain conditions41,42,43,44,45,46,47,48. Nevertheless, and despite the good results yielded by the present study on pain interference, similar improvements on pain intensity were not found. One possible explanation for this result might be the long duration of pain within this sample of patients. As far as we are aware, there are no studies investigating hypnosis effectiveness among patients with such a long pain duration as in this pilot trial, with around 70% of the participants having pain for over 20 years. In the literature reviewed on this subject, the highest mean pain duration identified was 13 years47. This is particularly significant since continuous and prolonged painful inputs from the damaged joints may cause an amplification of the responses of peripheral nociceptors (peripheral sensitization) and central nervous system neurons (central sensitization), resulting in an over activation of the nociceptive system49. Indeed, central and peripheral sensitization have been demonstrated in PWH17, and since the level of sensitization is dependent on pain duration50, these phenomenon may help to understand the non-significant changes in pain intensity found in the present study. In addition to physiological mechanisms, cognitive and emotional factors could also help explain the results, as these also play an important role in pain modulation51. Future trials with adequate sample sizes should therefore control for the potential moderator effect of psychological variables on intervention outcomes.
Additionally to a very long pain duration, it is possible that 4 sessions of hypnosis might have been insufficient to produce a significant decrease on pain intensity. Although some studies have achieved positive results with only 3 or 4 sessions41,42,45, most chronic pain trials include more sessions. It is true that brief interventions have been proven effective in conditions such as surgical acute pain52, but it is likely that the specificities of chronic pain demand a higher number of sessions. For example, Tan et al.43 showed that 2 self-hypnosis training sessions were effective in reducing pain intensity and interference, but these were followed by six weekly reminder telephone calls that possibly accounted for the positive results. Indeed, it has been recommended that a full hypnosis treatment should comprise 8 or more sessions53, and the question of the ideal number of sessions to achieve a clinically significant improvement in symptoms should be further analysed in future studies. Lastly, and given the low sample size, it is also important to consider the contribution of individual results for the group averages54. In this scope, it should be noted that one participant in the hypnosis sessions had a fall during the treatment period, with a later X-ray revealing a displacement of his knee prosthesis, which understandably influenced pain intensity ratings increase between pre and post-test.
Though pain intensity is traditionally the most valued outcome of pain research, it is also important to analyse the effects of treatments on other pain-related outcomes, to shed a more comprehensive light over the burden of pain48. Corroborating other reports42,43, the current study suggests that hypnosis intervention is effective in decreasing the perception of pain interference. Though there was a reduction on pain interference in both groups, it was higher in the EG, accounting for a significant effect size. The relevance of this finding is underscored by the high prevalence of pain in haemophilia and the recognition that it can be highly disruptive, particularly for patients with chronic pain8. Indeed, pain has been associated with lower HRQoL among PWH8,10,12,13, yielding a global negative impact on daily life. For instance, an international survey reported that as much as 89% of the participants had pain that interfered with daily activities12, mainly on physical functioning domains, but also having an impact on mood and enjoyment of life55. Congruently, previous findings of our team have shown that the greatest pain interference reported by Portuguese PWH was on dimensions related to daily activities, such as work and mobility, but also on mood13. In this scope, a positive association between pain interference and distress was also found among PWH, heightening the relevance of interventions that target pain interference in this population56. This body of evidence and our current findings add to recent publications calling for an improvement on pain management among PWH, namely through a broader adoption of non-pharmacological strategies7,14,16,17. Given the acknowledged negative impact of pain and these recent calls to improve its management in the haemophilia field, we would advocate for an urgent shift on research, from collection of observational data towards the implementation and testing of pain management interventions.
Notwithstanding the encouraging results showing reductions on pain interference, the most notable findings from this intervention concern HRQoL. In this sample, baseline EQ-5D VAS scores were lower (worse perception of health status) than those described in other haemophilia studies8,20,25. However, the effect of age has to be considered when comparing these figures, since those studies included data from younger samples (mean ages ranging from 29.7 to 37 years old). Research has indeed demonstrated that HRQoL scores tend to be lower among older PWH12,19,57, which has been at least partially explained by increased joint deterioration in this age group19,57. Congruent data was found in the present sample, with participants in the EG having a higher mean age and more affected joints. Nonetheless, these participants had a higher increase in EQ-5D index scores than those in the CG and an unequivocal improved assessment of their overall health status (EQ-5D VAS) at post-test, with participants in the CG even presenting a reduction in EQ-5D VAS scores. This is even more noteworthy considering the older mean age of participants in the EG, suggesting that hypnosis is an effective way to improve the subjective evaluation of health, even among older PWH who present more joint deterioration.
Concerning haemophilia-related quality-of-life, the improvements were higher for the EG on most dimensions, with the largest effect sizes on global HRQoL, “daily activities”, “treatment difficulties”, “physical health” and “joints”. These data show a more marked benefit of the intervention on dimensions related to the perception of physical health, which indeed tends to be more affected in PWH, comparing to mental health dimensions21,55. In this scope, it is also relevant to note that there were no significant reductions on “pain” scores (A36 Hemofilia-Qol). However, the 2 items composing this subscale refer only to pain frequency, which was not a specific target of the intervention sessions. Therefore, no changes were expected in this dimension.
As outlined in the introduction section, there are no published controlled trials specifically aiming to test psychological interventions that promote HRQoL among adult PWH, despite the acknowledgment that it is impaired in these patients12,19,20,21. Only one of the former reports of hypnosis in haemophilia makes a reference to quality-of-life, affirming that it is improved among patients using self-hypnosis, though it is not clear whether it was formally assessed29. Despite the absence of interventional studies with PWH, some comparisons can be drawn from investigations analysing the utility of hypnosis in other conditions that, like haemophilia, are associated with disabling symptoms. Corroborating the findings from this paper, those have shown that hypnosis is effective in improving HRQoL among patients with irritable bowel syndrome32, fibromyalgia33 and breast cancer34. This body of evidence further supports the utility of hypnosis to promote HRQoL and favours the pursuit of this line of research, encouraging the adoption of strategies that can improve the well-being, and thus the quality-of-life, of patients with chronic conditions.
Lastly, it is also relevant to note that the present results revealed a reduction in work absences in the EG, which could be related to the significant findings concerning global pain interference. Also, fewer missed days from work could be associated with the improved perception of HRQoL among participants in the EG.
This investigation has some limitations to consider. Although this was a pilot study, the small sample size hinders the establishment of definitive conclusions concerning the effectiveness of the intervention, which should be overcome in a future, adequately powered RCT. Additionally, specific measures should be adopted to avoid treatment contamination between the groups (i.e. the possibility that participants in the EG may disseminate information concerning the intervention to participants in the CG). However, the significant effect sizes obtained indicate treatment effectiveness and cannot be dismissed as a promising research direction58. In addition, the demographic and clinical differences between groups at baseline may have influenced the outcomes. Namely, patients in the EG have more affected joints and more painful locations which, as discussed above, can impact HRQoL and pain experience. Similarly, it would also be relevant to consider the role of other clinical variables, such as prophylaxis status or inhibitor development, and to control for their influence on the studied outcomes.
Another important variable to account for in a future RCT would be hypnotic susceptibility, since it has been suggested that highly susceptible individuals derive increased benefits from hypnotic pain interventions59. In this scope, it might be plausible that hypnotic susceptibility levels could at some degree account for the lack of a significant decrease on pain intensity levels in this study. However, it has also been argued that, in clinical settings, the success or failure of hypnotic interventions is not dependent on hypnotisability, which would only explain a small percentage of variance in outcomes60. Studies with chronic pain patients have reached inconsistent conclusions on this matter, with some findings revealing increased reductions on pain intensity scores among highly susceptible individuals46, others concluding that susceptibility was not related to outcomes43,44,45,48, and one study even reporting an inverse relationship between hypnotic susceptibility and reduction on pain intensity42. Undoubtedly, the inconsistent findings on this matter54,60 and the potential impact of hypnotic susceptibility on intervention outcomes justify the need to consider its inclusion as a potential moderator, or as a criteria for group stratification, in hypnotic intervention studies58.
Another suggestion for further studies would be a thorough record of self-hypnosis teaching and home practice, as a possible mean to explain clinically significant changes and long-term results. Also relevant to consider is the inclusion of an active control group besides the treatment-as-usual condition (e.g. attention group, relaxation training), in order to compare the relative efficacy of hypnosis and to rule out placebo effects as an explanation for the results obtained.
In conclusion, this pilot trial showed that it would be feasible to conduct an RCT to analyse the effectiveness of a hypnosis intervention among PWH. This was, to our knowledge, the first study suggesting that hypnosis is effective in decreasing pain interference and in improving the perception of HRQoL among PWH, providing a promising research direction that should be replicated with larger sample sizes and more homogenous groups, in order to establish more definitive conclusions.
Methods
Design
This was a two-arm randomised controlled pilot trial, with one experimental (intervention) group (EG) and one control group (CG), and three assessment moments: baseline (before intervention), post-test (after intervention) and 3 months after intervention. This manuscript reports the results from baseline (T1) and post-test (T2) assessment moments.
This investigation was approved by the Portuguese National Data Protection Agency, the Life Sciences and Health Ethics Subcommittee (University of Minho) and the Ethics Committee from São João University Hospital Centre —E.P.E.. All procedures were carried out in accordance with the Declaration of Helsinki and relevant guidelines for clinical research with human participants, and reported following the Consolidated Standards of Reporting Trials (CONSORT). This pilot trial is part of a larger study, registered at clinicaltrials.gov (NCT02870452) on August 17th, 2016.
Participants
Participants were recruited from the European Haemophilia Comprehensive Care Centre (EUHANET certified centre) and Reference Centre for Congenital Coagulopathies (certified by the Portuguese Health Ministry) at São João University Hospital Centre, Porto, Portugal. Eligible patients were identified and approached by the clinicians of the haemophilia centre to be referred to the investigators, who made a later telephone call for a more comprehensive evaluation of inclusion criteria. These included (a) male gender; (b) age ≥18 years; (c) moderate or severe haemophilia A or B, with or without inhibitors; (d) chronic pain (as defined by the European Haemophilia Therapy Standardisation Board7; and (e) ability to consent voluntary participation to the study. The exclusion criteria were (a) severe and debilitating neurological conditions (e.g., dementia); (b) severe organic or psychiatric conditions (e.g., cancer, schizophrenia); (c) undergoing any form of psychotherapy at time of enrolment; (d) having had orthopaedic surgery less than six months before study start or having it scheduled for the following six months; and e) unavailability to commit to four weekly intervention sessions.
During a visit to the haemophilia centre, participants signed the informed consent, performed baseline assessment and were randomly allocated either to intervention or control group. At this time, the four weekly intervention sessions were scheduled for participants in EG. Five weeks after baseline all participants completed the post-test assessment.
Since this was a pilot study, a formal sample size calculation was not performed.
Hypnotic intervention
Patients in the EG attended four consecutive weekly individual 60-min hypnotic sessions while maintaining treatment-as-usual. The hypnotic scripts were adapted from different sources61,62,63,64,65 and the intervention was conducted verbatim by one of the authors (PRP), who is a PhD Clinical Health Psychologist with certified advanced training in clinical hypnosis.
In order to engage patients in hypnosis, the first step is to explain its principles, providing patients with a rationale for its learning and use. In all sessions, theoretical-educative contents were provided and discussed before hypnotic induction. These focused on pain education, namely through the use of metaphors based on the gate control theory, emphasizing that pain results from a complex and dynamic interplay between biological processes and psychological factors (cognitive and emotional), as well as on contents regarding the relaxation response.
The hypnosis sessions comprised the following stages: (1) introduction/preparation of the patient (explaining the rationale underlying hypnosis, including dispelling potential myths, misconceptions and doubts; this step only in the first session); (2) hypnotic induction (suggestions to promote a state of relaxation and focused awareness); (3) deepening procedure (further suggestions for achieving a more deeply relaxed and focused state); (4) symptom-specific therapeutic suggestions (specific for haemophilia, aiming to change or improve symptoms and/or maladaptive behaviors, such as pain); (5) posthypnotic suggestions (to extend the benefits obtained beyond the session setting) and, finally (6) “waking up” the patient. On the first session, all the patients were taught self-hypnosis61 in order to be provided with means to perform hypnosis independently by themselves, thus reinforcing the posthypnotic suggestions. Self-hypnosis constitutes a powerful resource that guarantees the practice of the technique, independently and in an autonomous fashion, thereby empowering patients and giving them a sense of control and mastery over their problems and their lives53,63.
Regarding the hypnotic scripts, these consisted of an initial standardized hypnotic induction procedure (“Hartland’s Progressive Relaxation”)64, embracing suggestions to eye closure, concentration on breathing and promotion of a state of relaxation and focused awareness. It was then followed by the deepening procedure entitled “Special-Place Deepening Technique”65. This technique was directed to the selection of a comfortable and peaceful place, according to the personal preference of each participant (e.g. beach, garden, an autobiographical event…), wherein patients are suggested to experience several sensorial details of the place, along with allusions to safety and control. After induction and deepening procedures, specific hypnotic techniques were administered. In the first session, the “Healing White Light”64 technique was used to promote natural healing of the body against haemophilia usual symptoms (swellings, bleeds, bodily pains), intending to induce a general sense of well-being and health fitness. In the remaining three sessions, the “Pain Switch” technique, along with “Direct Therapeutic Suggestions For Pain Control” were employed61. All sessions included the “Ego Strengthening Technique”, which is potentially powerful because it increases the patients’ ability to access inner resources, improving their stress management skills and fostering a sense of control over the illness65. All suggestions were made on a repetitive basis at each session and all sessions ended with post-hypnotic suggestions before waking up the patient. These underscored that any experience of well-being, healing and comfort obtained would remain with the patient and last beyond the sessions, becoming a permanent part of how the patient lives and copes with disease and problematic issues.
An overview of the sessions, with further description of the techniques, is in Table 3.
Control group
Patients in the control group received medical treatments and standard care as usual, with the assessments being made in the same time points as the intervention group, but without receiving any psychological intervention.
Outcomes and data collection
Feasibility and acceptability were evaluated by analysis of recruitment and retention rates, adherence to study protocol, and satisfaction with the intervention. The latter was assessed using four questions specifically developed for this study. These ask about overall satisfaction with the intervention (rated from 1 = very dissatisfied to 5 = very satisfied), perception of improvement in well-being after attending the four sessions (rated from 1 = nothing to 5 = totally), perception of the utility of this type of interventions in haemophilia centres and desire to participate in further sessions (both rated from 1 = disagree to 3 = agree).
To evaluate the effectiveness of the intervention, the following primary outcomes were considered: pain experience (intensity and interference) and HRQoL. To ensure the quality of self-reported data and avoid inter-assessor subjectivity, all assessments were performed in-person, by the same investigator, using the Portuguese version of the following measures:
-
Socio-demographic and clinical questionnaire: Collects sociodemographic (e.g. age, education, employment) and haemophilia-related information (e.g. type and severity, bleeding episodes, treatment regimen).
-
Multidimensional Haemophilia Pain Questionnaire (MHPQ)66: Assesses haemophilia-related pain, focusing on painful locations, duration, frequency, triggering factors, intensity, interference, strategies for pain control, pain specialists and satisfaction with treatment. Pain intensity [Cronbach’s alpha (α) = 0.65] is assessed for six triggers/situations: bleeding episodes; during physical efforts and/or movement; using stairs; after resting or staying still; during rest, sitting or lying down; and accidental or “wrong” movements. Interference (α = 0.82) is rated in 7 domains, using the Brief Pain Inventory subscale67 (general activity, mood, walking ability, normal work, relations with others, sleep and enjoyment of life). Pain intensity and interference items are rated on a numerical rating scale, ranging from 0 (no pain/no interference) to 10 (worst imaginable pain/completely interferes), with a mean score being computed for each scale.
-
EQ-5D-5L68: Participants rate their overall HRQoL on five dimensions (mobility, self-care, usual activities, pain/discomfort and anxiety/depression) according to a five level scale (1 = no problems; 5 = extreme problems), with a summary index being calculated for each participant (range: 0–1; where 1 is the best possible score) (α = 0.58). Overall health status is evaluated by patients on a 0–100 visual analogic scale (VAS), with higher scores indicating a better health status.
-
A36 Hemofilia-QoL69: This is a disease-specific measure to assess haemophilia-related quality-of-life. The 36 items are rated on a 5 point Likert scale, generating a global HRQoL score (possible range: 0–144; α = 0.90) and nine subscale scores (physical health, daily activities, joints, pain, treatment satisfaction, treatment difficulties, emotional functioning, mental health and relationships and social activity). Higher scores translate better HRQoL.
-
Hospital Anxiety and Depression Scale (HADS)70: Used to evaluate emotional distress, according to two separate anxiety (α = 0.61) and depression (α = 0.92) scores (ranging from 0–21). Items are rated on a 4 point Likert scale (0–3), with higher results translating more symptomatology, and a score >8 being indicative of clinically significant symptoms71.
Randomisation
Participants were randomly allocated to intervention or control group (1:1 ratio), with the different randomisation steps being performed independently by two investigators. The randomisation sequence was computer-generated and concealed until official patient enrolment, after consenting to participate and performing baseline assessment. Due to the differences in procedure, blinding of the patients to intervention versus control group was impossible. The clinicians from the haemophilia centre and the investigator performing the assessments were blind to patient allocation.
Data analysis
Data analyses were performed using IBM SPSS Statistics version 23 (Chicago, IL, USA). Participants’ characteristics are expressed as absolute and relative frequencies (n, %) for categorical data or mean and standard deviation (SD) for continuous variables.
To adjust for between-group baseline differences, changes from pre to post-test assessment were analysed by calculating the difference between the two moments (Δ = T1 score-T2 score). The normality assumption of the Δ variables was checked for the two groups (CG and EG) through Shapiro-Wilk test. Normality was guaranteed for all variables, except for “number of bleeds” and “missed work days” in both groups; and for the “joints”, “pain” and “relationships and social activity” subscales of the A36 Hemofilia QoL, in the EG. For these cases, the corresponding non-parametric tests were used, and since the results were concordant with the corresponding parametric procedures, we decided to report the latter.
The groups were compared through chi-squared tests (χ2, for categorical variables) or independent-sample t tests (for continuous variables), accounting for the equality of variances (Levene’s test). If the variances were not homogeneous, the Welch’s correction was used. Statistical significance was set at p < 0.05.
Since null hypothesis significance testing and, consequently, p values, depend on sample size, the meaningfulness of differences was determined through the associated effect sizes (ES). These were expressed as Cohen’s d for continuous variables and Pearson’s phi (φ) coefficient for nominal variables. Cohen’s d score above 0.80 is considered a large effect, between 0.50 and 0.80 a medium effect and between 0.20 and 0.49 a small effect72. The interpretation of Pearson’s phi (φ) coefficient is analogous to the correlation coefficient, expressing the strength of association between two variables. The internal consistency of responses to the questionnaires was assessed using the Cronbach’s alpha coefficient (α)73.
Data Availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Ling, G., Nathwani, A. C. & Tuddenham, E. G. D. Recent advances in developing specific therapies for haemophilia. Br J Haematol 181, 161–172 (2018).
Blanchette, V. S. et al. Definitions in hemophilia: communication from the SSC of the ISTH. J Thromb Haemost 12, 1935–1939 (2014).
Bolton-Maggs, P. H., Pasi, K. J. & Haemophilias, A. and B. Lancet 361, 1801–1809 (2003).
Bossard, D. et al. Management of haemophilic arthropathy. Haemophilia 14(Suppl 4), 11–19 (2008).
Valentino, L. A. Blood-induced joint disease: the pathophysiology of hemophilic arthropathy. J Thromb Haemost 8, 1895–1902 (2010).
Forsyth, A. L. et al. Haemophilia Experiences, Results and Opportunities (HERO) Study: survey methodology and population demographics. Haemophilia 20, 44–51 (2014).
Holstein, K. et al. Pain management in patients with haemophilia: a European survey. Haemophilia 18, 743–752 (2012).
Witkop, M. et al. Self-reported prevalence, description and management of pain in adults with haemophilia: methods, demographics and results from the Pain, Functional Impairment, and Quality of life (P-FiQ) study. Haemophilia 23, 556–565 (2017).
Pinto, P. R. et al. Sociodemographic, Clinical, and Psychosocial Characteristics of People with Hemophilia in Portugal: Findings from the First National Survey. TH Open 02, e54–e67 (2018).
Elander, J., Robinson, G., Mitchell, K. & Morris, J. An assessment of the relative influence of pain coping, negative thoughts about pain, and pain acceptance on health-related quality of life among people with hemophilia. Pain 145, 169–175 (2009).
Wallny, T. et al. Pain status of patients with severe haemophilic arthropathy. Haemophilia 7, 453–458 (2001).
Forsyth, A. L. et al. Associations of quality of life, pain, and self-reported arthritis with age, employment, bleed rate, and utilization of hemophilia treatment center and health care provider services: results in adults with hemophilia in the HERO study. Patient Prefer Adherence 9, 1549–1560 (2015).
Pinto, P. R., Paredes, A. C. & Almeida, A. Pain prevalence, characteristics and impact among people with haemophilia: findings from the first Portuguese survey and implications for pain management. Pain Med (in press).
Young, G., Tachdjian, R., Baumann, K. & Panopoulos, G. Comprehensive management of chronic pain in haemophilia. Haemophilia 20, e113–120 (2014).
Tagliaferri, A. et al. Pain assessment and management in haemophilia: A survey among Italian patients and specialist physicians. Haemophilia 24, 766–773 (2018).
Humphries, T. J. & Kessler, C. M. Managing chronic pain in adults with haemophilia: current status and call to action. Haemophilia 21, 41–51 (2015).
Roussel, N. A. Gaining insight into the complexity of pain in patients with haemophilia: State-of-the-art review on pain processing. Haemophilia 24, 3–8 (2018).
Bullinger, M., Globe, D., Wasserman, J., Young, N. L. & von Mackensen, S. Challenges of patient-reported outcome assessment in hemophilia care-a state of the art review. Value Health 12, 808–820 (2009).
von Mackensen, S., Gringeri, A., Siboni, S. M. & Mannucci, P. M. Health-related quality of life and psychological well-being in elderly patients with haemophilia. Haemophilia 18, 345–352 (2012).
Cavazza, M. et al. Social/economic costs and quality of life in patients with haemophilia in Europe. Eur J Health Econ 17(Suppl 1), 53–65 (2016).
Carvalhosa, A. M., Henrard, S., Lambert, C. & Hermans, C. Physical and mental quality of life in adult patients with haemophilia in Belgium: the impact of financial issues. Haemophilia 20, 479–485 (2014).
Srivastava, A. et al. Guidelines for the management of hemophilia. Haemophilia 19, e1–e47 (2013).
Cuesta-Barriuso, R., Gomez-Conesa, A. & Lopez-Pina, J. A. Manual therapy in the treatment of ankle hemophilic arthropathy. A randomized pilot study. Physiother Theory Pract 30, 534–539 (2014).
Runkel, B., Von Mackensen, S. & Hilberg, T. RCT - subjective physical performance and quality of life after a 6-month programmed sports therapy (PST) in patients with haemophilia. Haemophilia 23, 144–151 (2017).
Manco-Johnson, M. J. et al. Effect of late prophylaxis in hemophilia on joint status: a randomized trial. J Thromb Haemost 15, 2115–2124 (2017).
Oldenburg, J. et al. Emicizumab Prophylaxis in Hemophilia A with Inhibitors. New England Journal of Medicine 377, 809–818 (2017).
Lucas, O. N. The use of hypnosis in haemophilia dental care. Ann N Y Acad Sci 20, 263–266 (1975).
Swirsky-Sacchetti, T. & Margolis, C. G. The effects of a comprehensive self-hypnosis training program on the use of factor VIII in severe hemophilia. Int J Clin Exp Hypn 34, 71–83 (1986).
LaBaw, W. The use of hypnosis with hemophilia. Psychiatric medicine 10, 89–98 (1992).
British Medical Association. Medical use of hypnotism: report of a subcommittee appointed by the Psychological Medicine Group Committee of the British Medical Association. BMJ Suppl 23, 190–193 (1955).
Adachi, T., Fujino, H., Nakae, A., Mashimo, T. & Sasaki, J. A meta-analysis of hypnosis for chronic pain problems: a comparison between hypnosis, standard care, and other psychological interventions. Int J Clin Exp Hypn 62, 1–28 (2014).
Keefer, L. & Keshavarzian, A. Feasibility and acceptability of gut-directed hypnosis on inflammatory bowel disease: a brief communication. Int J Clin Exp Hypn 55, 457–466 (2007).
Zech, N., Hansen, E., Bernardy, K. & Hauser, W. Efficacy, acceptability and safety of guided imagery/hypnosis in fibromyalgia - A systematic review and meta-analysis of randomized controlled trials. Eur J Pain 21, 217–227 (2017).
Forester-Miller, H. Self-Hypnosis Classes to Enhance the Quality of Life of Breast Cancer Patients. Am J Clin Hypn 60, 18–32 (2017).
World Federation of Haemophilia. Report on the Annual Global Survey 2017 (2018).
King, M. et al. Impact of participant and physician intervention preferences on randomized trials: a systematic review. JAMA 293, 1089–1099 (2005).
Kowalski, C. J. & Mrdjenovich, A. J. Patient preference clinical trials: why and when they will sometimes be preferred. Perspect Biol Med 56, 18–35 (2013).
Varni, J. W. Behavioral medicine in hemophilia arthritic pain management: two case studies. Arch Phys Med Rehabil 62, 183–187 (1981).
Varni, J. W. & Gilbert, A. Self-regulation of chronic arthritic pain and long-term analgesic dependence in a haemophiliac. Rheumatol Rehabil 21, 171–174 (1982).
Pinnell, C. M. & Covino, N. A. Empirical findings on the use of hypnosis in medicine: a critical review. Int J Clin Exp Hypn 48, 170–194 (2000).
Ardigo, S. et al. Hypnosis can reduce pain in hospitalized older patients: a randomized controlled study. BMC Geriatrics 16, 14 (2016).
Tan, G., Fukui, T., Jensen, M. P., Thornby, J. & Waldman, K. L. Hypnosis treatment for chronic low back pain. Int J Clin Exp Hypn 58, 53–68 (2010).
Tan, G. et al. A randomized controlled trial of hypnosis compared with biofeedback for adults with chronic low back pain. Eur J Pain 19, 271–280 (2015).
Jensen, M. P. et al. Effects of self-hypnosis training and EMG biofeedback relaxation training on chronic pain in persons with spinal-cord injury. Int J Clin Exp Hypn 57, 239–268 (2009).
Abrahamsen, R., Zachariae, R. & Svensson, P. Effect of hypnosis on oral function and psychological factors in temporomandibular disorders patients. J Oral Rehabil 36, 556–570 (2009).
Abrahamsen, R., Baad-Hansen, L. & Svensson, P. Hypnosis in the management of persistent idiopathic orofacial pain-clinical and psychosocial findings. Pain 136, 44–52 (2008).
Gay, M. C., Philippot, P. & Luminet, O. Differential effectiveness of psychological interventions for reducing osteoarthritis pain: a comparison of Erikson hypnosis and Jacobson relaxation. Eur J Pain 6, 1–16 (2002).
Jensen, M. P. et al. Hypnotic analgesia for chronic pain in persons with disabilities: a case series. Int J Clin Exp Hypn 53, 198–228 (2005).
Latremoliere, A. & Woolf, C. J. Central sensitization: a generator of pain hypersensitivity by central neural plasticity. J Pain 10, 895–926 (2009).
Arendt-Nielsen, L. Joint pain: more to it than just structural damage? Pain 158(Suppl 1), S66–s73 (2017).
Bushnell, M. C., Ceko, M. & Low, L. A. Cognitive and emotional control of pain and its disruption in chronic pain. Nat Rev Neurosci 14, 502–511 (2013).
Montgomery, G. H. et al. A randomized clinical trial of a brief hypnosis intervention to control side effects in breast surgery patients. J Natl Cancer Inst 99, 1304–1312 (2007).
Jensen, M. & Patterson, D. R. Hypnotic treatment of chronic pain. J Behav Med 29, 95–124 (2006).
Jensen, M. P. & Patterson, D. R. Hypnotic approaches for chronic pain management: clinical implications of recent research findings. Am Psychol 69, 167–177 (2014).
Kempton, C. L. et al. Impact of pain and functional impairment in US adults with haemophilia: Patient-reported outcomes and musculoskeletal evaluation in the pain, functional impairment and quality of life (P-FiQ) study. Haemophilia 24, 261–270 (2018).
Pinto, P. R. et al. Emotional distress in haemophilia: Factors associated with the presence of anxiety and depression symptoms among adults. Haemophilia 24, e344–e353 (2018).
Fischer, K., Bom, J. G., Mauser-Bunschoten, E. P., Roosendaal, G. & Berg, H. M. Effects of haemophilic arthropathy on health-related quality of life and socio-economic parameters. Haemophilia 11, 43–48 (2005).
Lynn, S. J., Kirsch, I., Barabasz, A., Cardena, E. & Patterson, D. Hypnosis as an empirically supported clinical intervention: the state of the evidence and a look to the future. Int J Clin Exp Hypn 48, 239–259 (2000).
Milling, L. S. Is high hypnotic suggestibility necessary for successful hypnotic pain intervention? Curr Pain Headache Rep 12, 98–102 (2008).
Montgomery, G. H., Schnur, J. B. & David, D. The impact of hypnotic suggestibility in clinical care settings. Int J Clin Exp Hypn 59, 294–309 (2011).
Hammond, D. C. Handbook of Hypnotic Suggestions and Metaphors. (WW Norton & Company, 1990).
Jensen, M. Hypnosis for Chronic Pain Management (Oxford University Press, 2011).
Jensen, M. P. The neurophysiology of pain perception and hypnotic analgesia: implications for clinical practice. Am J Clin Hypn 51, 123–148 (2008).
Heap, M. & Aravind, K. Hartland’s Medical and Dental Hypnosis. (Churchill Livingstone 2001).
Frederick, C. & McNeal, S. Inner strengths: Contemporary ego-strengthening in hypnotic and non-hypnotic psychotherapy. (Lawrence Erlebaum and Associates, 1999).
Paredes, A. C., Costa, P., Almeida, A. & Pinto, P. R. A new measure to assess pain in people with haemophilia: The Multidimensional Haemophilia Pain Questionnaire (MHPQ). PLoS One 13, e0207939 (2018).
Cleeland, C. S. & Ryan, K. M. Pain assessment: global use of the Brief Pain Inventory. Ann Acad Med Singapore 23, 129–138 (1994).
Herdman, M. et al. Development and preliminary testing of the new five-level version of EQ-5D (EQ-5D-5L). Qual Life Res 20, 1727–1736 (2011).
Remor, E. et al. Psychometric field study of the new haemophilia quality of life questionnaire for adults: The ‘Hemofilia-QoL’. Haemophilia 11, 603–610 (2005).
Zigmond, A. S. & Snaith, R. P. The hospital anxiety and depression scale. Acta Psychiatr Scand 67, 361–370 (1983).
Bjelland, I., Dahl, A. A., Haug, T. T. & Neckelmann, D. The validity of the Hospital Anxiety and Depression Scale: An updated literature review. J Psychosom Res 52, 69–77 (2002).
Cohen, J. Statistical Power Analysis for the Behavioural Sciences. 2nd edn, (Lawrence Erlbaum Associates, 1988).
Cronbach, L. J. Coefficient alpha and the internal structure of tests. Psychometrika 16, 297–334 (1951).
Acknowledgements
This work is supported by a grant from the Novo Nordisk HERO Research Grant 2015. P. R. Pinto has a post-doctoral grant (SFRH/BPD/103529/2014) from the Portuguese Foundation of Science and Technology.
Author information
Authors and Affiliations
Contributions
P.R.P., A.C.P. and A.A. designed the research. M.C., M.L. and S.F. contributed for the refinement of the design with clinical expertise and were responsible for patient selection. P.R.P. conducted the hypnosis sessions and A.C.P. performed outcome assessments. P.R.P., A.C.P. and P.C. conducted the statistical analysis and interpreted the data. P.R.P., A.C.P. and A.A. wrote the manuscript and M.C., M.L., S.F. and P.C. critically revised it. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Paredes, A.C., Costa, P., Fernandes, S. et al. Effectiveness of hypnosis for pain management and promotion of health-related quality-of-life among people with haemophilia: a randomised controlled pilot trial. Sci Rep 9, 13399 (2019). https://doi.org/10.1038/s41598-019-49827-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-019-49827-1
This article is cited by
-
Chronischer Schmerz – eine psychosomatische Sichtweise
Manuelle Medizin (2020)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.