Abstract
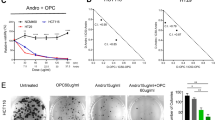
The objective was to assess anti-progression and stimulatory immune response effects among anthocyanins (ANC) and their metabolites on human colorectal cancer cells in vitro and in silico. Pure phenolics including delphinidin-3-O-glucoside (D3G) and its metabolites, delphinidin (DC) and gallic acid (GA), were tested alone or in combination, on HCT-116 and HT-29 human colorectal cancer cells (100–600 µg/mL). HCT-116 and HT-29 50% inhibition concentrations (µg/mL) were 396 ± 23 and 329 ± 17 for D3G; 242 ± 16 and >600 for DC; and 154 ± 5 and 81 ± 5 for GA, respectively. Using molecular docking, cyanidin-3-O-glucoside (C3G) showed the highest potential to inhibit immune checkpoints: programmed cell death protein-1 (PD-1) (−6.8 kcal/mol) and programmed death-ligand-1 (PD-L1) (−9.6 kcal/mol). C3G, D3G, DC, GA, and D3G-rich extracts decreased PD-L1 protein expression in HCT-116 cells. C3G decreased PD-L1 fluorescence intensity by 39%. ANC decreased PD-1 expression in peripheral blood mononuclear cells in monoculture by 41% and 55%, and co-culture with HCT-116 and HT-29 cells by 39% and 26% (C3G) and 50% and 51% (D3G), respectively. D3G and C3G, abundant in plant foods, showed potential for binding with and inhibiting immune checkpoints, PD-1 and PD-L1, which can activate immune response in the tumor microenvironment and induce cancer cell death.
Similar content being viewed by others
Introduction
In the United States, colorectal cancer deaths in 2018 were estimated at 50,6301. Currently, regional and distant stages represent 35% and 21% of the total colorectal cancer cases, and five-year survival rates are 71.1% and 13.8%, respectively, emphasizing the impact of metastasis on survival1. Three categories of drug therapies are used for metastatic colorectal cancer treatment: chemotherapy, targeted therapy, and immunotherapy. Chemotherapy drugs target highly proliferating cells while approved targeted therapies aim to inhibit proteins in the angiogenesis pathway, such as vascular endothelial growth factor (VEGF)2. More recently, VEGF has been shown, in addition to its proangiogenic effects, to hinder immune function in the tumor microenvironment by impacting infiltration of T cells3,4.
Immunotherapy drugs are the newest addition to combat colorectal cancer. In 2017, the first two immunotherapies (nivolumab and pembrolizumab) that target programmed cell death protein 1 (PD-1) were approved by the FDA for colorectal cancer with microsatellite instability-high or deficient mismatch repair solid tumors5. Microsatellites are short repeated sequences in the genome, and microsatellite instability indicates a disruption in the mismatch repair system and greatly increased mutations6. PD-1 is part of a group of immune checkpoints, which are negative regulators of the immune system and are targeted in immunotherapy to help activate T cell response against tumors5. Other immune checkpoints, including programmed death-ligand 1 (PD-L1), the ligand for PD-1, and cytotoxic T-lymphocyte-associated antigen 4 (CTLA-4), are also being targeted for treatment in colorectal cancer7. PD-L1 is typically overexpressed in tumor cells, contributing to the tumor cells’ ability to avoid immune destruction; when it binds to PD-1 on T cells, they are deactivated and unable to destroy the cancer cells7. In July of 2018, a combination treatment of nivolumab and ipilimumab, a CTLA-4 inhibitor, was approved by the FDA8. More successful therapies and the use of combination therapies are needed to enhance the highly complex mechanisms of the immune system in the tumor microenvironment4,9.
A diet high in non-starchy vegetables, fruits, and whole grains is recommended for decreasing the risk of developing colorectal cancer10. Anthocyanins (ANC) are phenolic compounds and natural pigments that provide blue, purple, or red color to fruits, vegetables, cereals, and legumes. ANC have been shown to have anti-carcinogenic properties including an impact on autophagy regulation in tumor development11,12,13,14. ANC metabolites, including phenolic acids, have been shown to reach the colon during in vivo studies on bioavailability15. Assessment of ANC and immune response related to carcinogenesis has not been well examined. ANC from black rice promoted an immune response by increasing T cell and macrophage populations in a leukemia in vivo model16. In vitro and in silico analyses of compounds present in ANC-rich extracts can provide more information on their mechanisms of action as it applies to the immune response in the tumor microenvironment.
Our previous studies with colorectal cancer and ANC-rich extracts have shown the potential for such extracts to inhibit colorectal cancer cell growth in vitro, with effects on markers of apoptosis, cell cycle, and angiogenesis17,18. However, in the present study we focused on pure ANC and their metabolites and extensively evaluated their effects on immune checkpoints. The objective of this research was to compare the anti-progression and stimulatory immune effects among ANC and their metabolites on human colorectal cancer cell lines, HCT-116 and HT-29. We employed a co-culture set-up in addition to the monoculture analyses to test ANC in a more representative model of the tumor microenvironment. Our findings support the potential for ANC to inhibit immune-suppressing markers, providing a basis for additional studies on the impact of other plant phenolics on immune response.
Materials and Methods
Materials
Human colorectal cancer cells, HCT 116 and HT-29, were purchased from the American Type Culture Collection (Manassas, Virginia) and human peripheral blood mononuclear cells (PBMC) from BioIVT (Hicksville, New York). The CellTiter 96® AQueous One Solution Cell Proliferation Assay was purchased from Promega Corporation (Madison, WI) and the Pierce LDH Cytotoxicity Assay Kit from ThermoFisher Scientific (Waltham, MA). Delphinidin-3-O-glucoside (D3G), cyanidin-3-O-glucoside (C3G), malvidin-3-O-glucoside (M3G), delphinidin chloride (DC), procyanidin B1 (PB1), naringenin-7-O-glucoside, eriodictyol-7-O-glucoside, and quercetin-3-O-glucuronide (Q3G) all with >95% purity were purchased from ExtraSynthese (France). Red grape extract (RGE) was obtained from San Joaquin Valley Concentrates (Fresno, CA) and the black lentil extract (BLE) from the Kraft Heinz Company (Chicago, IL); both extracts were further purified as described in our previous publication18. Primary antibodies programmed cell death ligand-1 (1C10) (sc-293425), VEGF (F-5) (sc-365578), and GAPDH (sc-25778), and the radioimmunoprecipitation (RIPA) buffer were purchased from Santa Cruz Biotechnology (Santa Cruz, CA). Secondary antibody, anti-mouse IgG horseradish peroxidase conjugated, was obtained from GE Healthcare (Buckinghamshire, UK). Anti-PD-L1 antibody [EPR19759] (ab213524) was purchased from Abcam (Cambridge, UK). Atezolizumab and pembrolizumab were bought from BioVision, Inc. (Milpitas, CA). DC protein assay materials were obtained from Bio-Rad (Hercules, CA). All other chemicals used in this study were purchased from Sigma- Aldrich (St. Louis, MO) unless otherwise stated.
Cell culture
HCT 116 and HT-29 cells were cultured in Minimum Essential Medium Eagle and PBMC in Roswell Park Memorial Institute (RPMI) medium both with 10% FBS, 1% penicillin/streptomycin, and 1% sodium pyruvate at 37 °C in 5% CO2 and 95% air. When HCT 116 cells were co-cultured with PBMC they were grown in RPMI medium. As microsatellite stability is important in the treatment of colorectal cancer, one cell line with a microsatellite instable phenotype (HCT 116) and another cell line with chromosomal instability (HT-29) were selected to allow for comparison of immune response effects19.
HCT 116 and HT-29 cell viability with phenolics
The CellTiter 96® AQueous One Solution Cell Proliferation Assay was used to determine the most potent of the pure phenolics and the concentration for 50% inhibition (IC50) values for the ANC and metabolites on the HCT 116 cells based on the method described in our previous publication17. Briefly, cells were seeded in a 96 well plate at 1 × 104 cells per well for 24 h. Pure phenolics alone or in combinations were added up to 600 µg/mL (50, 100, 200, 400, and 600 µg/mL) and incubated with the cells for 24 h. Ratios (percentages) for the phenolic combinations were based on the three main phenolics discovered in three extracts previously found to be potent at colorectal cancer cell inhibition: D3G, M3G, and Q3G (57:33:10) representing red grape; PB1, D3G, and Q3G (42:40:18) for black lentil; and PB1, eriodictyol 7-O-glucoside, and naringenin 7-O-glucoside (40:34:26) for sorghum18. Because cyanidin is the most ubiquitous anthocyanidin in fruits and vegetables and C3G was present in at least small amounts in all of the extracts tested in our previous study, it was tested individually, as well20. Some of the phenolics tested in the combinations are not water-soluble (Q3G, eriodictyol 7-O-glucoside, naringenin 7-O-glucoside) and had to be dissolved in DMSO, so they were not tested individually. A maximum of 0.5% DMSO was used on the cells, and an untreated control at the same percentage was always used for comparison. Additionally, two metabolites of D3G were tested: DC and gallic acid (GA). These were identified as metabolites based on the literature21,22. Absorbance using the CellTiter assay was calculated and compared at 515 nm with an ELX808IU Ultra Microplate Reader (BioTek, Winooski, VT). Then, IC50 values were calculated using Prism 6 software (GraphPad Software, La Jolla, CA).
Interaction analysis of delphinidin-3-O-glucoside and anthocyanin-rich extracts with oxaliplatin
Oxaliplatin is a commonly used chemotherapy drug for colorectal cancer, so it is important to learn about potential chemical interactions. Isobolograms were utilized to analyze the effect of ANC-rich extracts, BLE and RGE, and D3G on oxaliplatin inhibition. To determine if there was an antagonistic, additive, or synergistic effect, extracts were tested in combination with oxaliplatin. IC50 values were utilized: BLE (1.2 mg/mL), RGE (1.4 mg/mL), D3G (395.8 μg/mL), and oxaliplatin (13.5 μg/mL). Extracts (or D3G) were combined with oxaliplatin in a 1:1 ratio of the IC50 concentrations as the highest concentration and step-wise dilutions were tested to determine the IC50 of the combination. Then, using the expected and observed IC50, the type of effect the extracts and D3G had on oxaliplatin inhibition effectiveness was determined based on the calculated V values23.
Metabolism of phenolics analysis with HPLC and colorimetry
HPLC analysis at 520 and 280 nm of the pure ANC (D3G, C3G, and M3G) was performed in duplicate with pure compounds before application to the cells and in the media following 24 h treatment on HCT 116 cells. A Hitachi HPLC System (Hitachi High Technologies America, Inc., Schaumburg, IL) equipped with a multi-wavelength detector L-7100 pump was utilized with a Prevail C18 column (5 µm, 250 × 4.6 mm, Columbia, MD)24.
A Hunter Lab LabScan II (Hunter Associates Laboratory, Inc., Reston, VA) was used to analyze color parameters: L*, a*, and b using CIELAB 10°/D65 for D3G, C3G, and M3G in the media before and after being applied to HCT 116 cells for 24 h in the incubator at 37 °C and 5% CO2. This was to confirm the visual color changes seen and offer quantitative data for each ANC treatment. The initial color was compared to the final color of the media that was collected 24 h after treatment on the cells. Calculations were made as described previously25.
Evaluation of apoptosis induction by delphinidin-3-O-glucoside and its metabolites using flow cytometry
Since the pure compounds tested were more effective on HCT 116 cells, apoptosis induction was determined for these cells. For apoptosis measurement, HCT 116 cells were seeded at 3 × 105 cells per well in a six-well plate as described before17. After 24 h, they were treated with D3G, DC, GA, red grape combination (RGC: D3G, M3G, and Q3G (57:33:10), and oxaliplatin for 24 h at the IC50 determined values (ranging from 13.5–395.8 µg/mL). A BD LSR II Flow Cytometry Analyzer (BD Biosciences, San Jose, CA) was used to evaluate the state of 10,000 cells. Duplicate readings of each well were taken, and two independent experiments were analyzed. Total apoptotic cells was a combination of late and early apoptotic cells in quadrants two and four, respectively analyzed through FCS Express 5 Software.
Immune response analysis
Co-culture with PBMC and HCT 116 cells
Day one PBMC were seeded in a 24-well plate at 0.5–1 × 106 cells per mL untreated or with treatments for 48 h: C3G or D3G at 100 μM or pembrolizumab at 6.7 nM. The concentration of 100 μM was used after a pretest (data not shown) showed it had the highest induced cancer cell inhibition even with higher concentrations tested in pretreatment with the PBMC. HCT 116 cells were seeded at 1 × 104 cells per well in a 96 well plate on day two. Day three PBMC from each treatment or untreated cells were centrifuged at 200 g for 15 min. Regular media was added to bring to 1 × 106 cells per mL so that when adding 200 μL to each 96 well of HCT 116 cells, there would be a 10:1 PBMC to HCT 116 cell ratio. After 24 h, viability was determined using a Pierce LDH Cytotoxicity Assay Kit. A visual summary of the method is shown in Supplementary Fig. 1.
Effect of pure phenolics and D3G-rich plant extracts on VEGF and PD-L1 protein expression
Western blots for VEGF and PD-L1 were run using a protocol based on that used by Dia and Gonzalez de Mejia26. The PD-L1 antibody is a mouse monoclonal IgG2b raised against amino acids 18-238 which represents the partial length of human PD-L1. Briefly, HCT 116 and HT-29 cells were seeded in a six-well plate at 3 × 105 cells per well for 24 h. Then, cells were either left untreated or treated with pure phenolics or the D3G-rich plant extracts (BLE or RGE) at their IC50. After another 24 h, cell lysates were obtained to be used in the SDS-PAGE electrophoresis.
PD-L1 analysis through ELISA
Human PD-L1 ELISA kit (Abcam ab214565) was used to analyze the effect of the phenolics and extracts in a non-denatured condition with a higher scale of sensitivity. The PD-L1 antibody was rabbit monoclonal with an immunogen of a recombinant full-length protein of human PD-L1 containing the extracellular domain (Phe19-Thr239). The manufacturer’s instructions were followed. Briefly, HCT 116 and HT-29 cells were seeded in a six-well plate at 4 × 105 cells per well for 24 h. Then, cells were left untreated or treated with pure phenolics (D3G, DC, GA, and RGC) or plant extracts (BLE and RGE) at their IC50 values. C3G was tested at the same concentration as D3G since it did not have high enough inhibition to have an IC50 value. Atezolizumab, a PD-L1 inhibitor drug, was used as a positive control at 6.9 nM (1 μg/mL) as suggested by the manufacturer; ELISA was the only method in which atezolizumab was recommended to be used because of the non-denatured conditions. After another 24 h, cell lysates were obtained by following the Abcam protocol for adherent cells. PD-L1 calculations for samples were based on the standard curve and translated to pg of PD-L1 per μg of protein based on their protein concentration.
PD-1 analysis through ELISA in peripheral blood mononuclear cells
Human PD-1 ELISA kit (Invitrogen BMS2214) was used to analyze the effect of C3G and D3G on PD-1 in PBMC in a monoculture and co-culture with HCT 116 and HT-29 cells. PBMC were seeded in a 24-well plate 0.5–2 × 106 cells per mL for 24 h either untreated or treated with C3G or D3G (100 μM). Pembrolizumab, a PD-1 inhibitor drug, was used as a positive control at 6.7 nM (1 μg/mL) as suggested by the manufacturer. After 48 h, the cell culture supernatant was collected post-centrifugation (200 g for 15 min). The media was then centrifuged at 20,817 g (Eppendorf Centrifuge 5417 R, 30 1.5–2 mL tubes) for 10 min at 4 °C and supernatant was collected. To analyze in co-culture with HCT 116 and HT-29 cells, at the step where media was collected post-centrifugation, media was also added to the cell pellet to be added at a 10:1 ratio of PBMC to colorectal cancer cells in a 96-well plate. After 24 h of co-culture, the media was collected, centrifuged, and the supernatant collected as described above. The DC protein assay was used to determine the concentration of protein for all supernatants. For the ELISA, the manufacturer’s instructions were followed. PD-1 calculations for samples were based on the standard curve and translated to pg of PD-1 per μg of protein.
PD-L1 analysis through confocal microscopy
Due to higher expression of PD-L1 in HCT 116 cells, further analysis with confocal microscopy was tested in these cells. The PD-L1 antibody was a rabbit monoclonal with an immunogen of a synthetic peptide within amino acids 250 to the C-terminus of human PD-L1. HCT 116 cells were seeded on 8-well immunofluorescence and high-end microscopy slide at 1.5 × 104 cells per well. After 24 h, pure compounds were added, with one untreated well; for D3G and DC, the IC50 concentrations were used, and C3G was used at the same concentration as D3G. Following 24 h, cells were washed with PBS and fixed in 4% paraformaldehyde for 30 min. They were permeated with 0.5% Triton X100 after PBS washes for 15 min. Then they were incubated in cold methanol for 15 min at −20 °C and then for 30 min in PBS at room temperature. After 30 min in ITsignal FX, the primary PD-L1 antibody was added at a 1:50 dilution and left overnight at 37 °C. The next day, cells were washed and incubated for 3 h in the secondary antibody at a 1:200 dilution. Cells were washed and drained before adding Prolong Gold. After 24 h in the dark, slides were kept at 4 °C until analyzed using a Zeiss LSM 880 laser-scanning confocal microscope at the Carl R. Woese Institute for Genomic Biology at the University of Illinois. Zen 2 (blue edition) software (Carl Zeiss Microscopy) was used to obtain pictures and measure fluorescence by taking the mean intensity of the PD-L1 signal divided by the mean DAPI signal with the histogram tool.
In silico studies of phenolics and immune response related proteins
In silico analysis was utilized to screen the potential for phenolic compounds to inhibit immune response related proteins. The 3D structures of PD-1 (5WT9), PD-L1 (5N2D), and VEGF (5FV1) were obtained from Protein Data Bank. Phenolic structures were downloaded from the PubChem Compound database (National Center for Biotechnology Information, Bethesda, MD): C3G (CID: 44256715), PB1 (CID: 11250133), D3G (CID: 443650), M3G (CID: 44257034), DC (CID: 68245), and GA (CID: 370). Water molecules and ligands that accompanied the protein structures were removed in BIOVIA Discover Studio Client 2016. The protein structures were then uploaded to AutoDock Tool where partial Gasteiger charges were automatically implemented and the search space was configured to be a cube with sides measuring 20 angstroms centered on the protein binding sites for each drug and respective ligand. Two sites were tested for each protein with each phenolic ligand: PD-1 at the nivolumab and PD-L1 binding sites; PD-L1 at the atezolizumab and 8J8 small molecule inhibitor site; and VEGF at the VEGFR1 and VEGFR2 binding sites. The search space for the PD-1/PD-L1 binding site was centered to be near VAL64, ILE124, and LEU128 on PD-127. VEGF binding sites to its receptors were estimated to be near ASP63, GLU64, and GLU67 for VEGFR1, and near ARG82, LYS84, and HIS86 for VEGFR228. A related small molecule inhibitor of each protein was used as a comparison. The small molecule 8YZ accompanied by 5NIU was used for PD-1 and PD-L1 sites. For the 8J8 site on PD-L1, the 8J8 molecule that accompanied the 5N2D structure was selected. The control chosen for VEGF at VEGFR1 was vatalanib, obtained from PubChem (CID: 151194). Using MarvinSketch, a structure of PTC-858, a reported VEGF inhibitor, was replicated from ChemSpider (CID: 4501829)29. Protein structures were transferred to AutoDock Tools as rigid molecules. Each phenolic and small molecule inhibitor was also uploaded to AutoDock Tools as a ligand and their number of flexible bonds was reduced to half their maximum torsions. After these alterations, all molecules were saved as PDBQT files before docking experiments were run. The data received from AutoDock Vina was analyzed in BIOVIA Discovery Studio 2016 Client to determine the nature of each docking interaction and 3D configuration.
Fluorescence quenching of anthocyanins and immune checkpoint proteins
To confirm docking predictions seen with C3G and D3G and immune checkpoints, fluorescence spectroscopy analysis was used to determine whether an interaction occurs and if it is static or dynamic. A FluoroMax-3 spectrofluorometer (HORIBA Jobin Yvon, Edison, NJ) was used with C3G and D3G and recombinant human PD-L1 protein and human PD-1 protein combinations. The PD-L1 protein was kept constant at 10 nM and PD-1 at 100 fM in distilled deionized water. Excitation wavelength was set to 280 nm, increment at 2 nm, integration time of 0.5 s, excitation and emission slits at 5 nm, scan start at 310 nm, and scan end at 500 nm. The peak at 354 nm was determined to be the main peak of the PD-L1 and PD-1 proteins. Concentrations of anthocyanins (1000, 500, 250, 100, and 10 µM) were incubated with the fixed concentrations of the proteins to read fluorescence intensity. The Stern-Volmer equation system was utilized as described previously30. The lifetime of the fluorophore of protein in the absence of a quencher, τ0, used was 10−8.
Statistical analysis
Statistical analyses were conducted using one-way ANOVA to compare experimental to control values with JMP version 8.0. Comparisons between groups for viability and apoptosis were performed using the Tukey- Kramer test; differences were considered significant at p < 0.05. For western blots and confocal microscopy, comparisons between the untreated control and treatments were performed using Student’s test; differences were considered significant at p < 0.05. At least two independent experiments run with at least duplicate data points were performed for every study.
Results
HCT 116 and HT-29 cell viability inhibition by delphinidin-3-O-glucoside and its metabolites
Of the three ANC (D3G, C3G, and M3G) and PB1 tested on HCT 116 cells, only D3G showed a dose-response inhibitory effect with an IC50 at 395.8 μg/mL. Figure 1 shows the inhibition curves, IC50’s, and inhibition at 400 μg/mL of the pure phenolics for comparison. Both of the D3G metabolites tested, DC and GA, inhibited HCT 116 cells with IC50 of 242.4 and 154.2 μg/mL for DC and GA, respectively (Fig. 1a–c). For the phenolic combinations (Fig. 1d,e), pure compounds from red grape had the highest potency with an IC50 at 394.3 μg/mL, not statistically different from D3G alone at 395.8 μg/mL (p = 0.9671). Since the RGC was the most potent, it was also tested on HT-29 cells and had an IC50 of 589.9 μg/mL, statistically higher (p = 0.0021) than that for HCT 116 cells. D3G and GA had IC50 for HT-29 cells of 329.1 and 80.6 μg/mL, respectively; DC had up to 43.5% inhibition at 600 μg/mL (Fig. 1f,g). The IC50 for D3G on HT-29 cells was not statistically different from its IC50 for HCT 116 cells (p = 0.0608).
Inhibition curves with standard error bars. (a) Pure anthocyanins on HCT 116 cells. (b) Pure phenolics on HCT 116 cells. (c) The 50% viability inhibition concentrations (IC50) of the pure anthocyanins and phenolics on HCT 116 cells (mean ± SEM) and their percent inhibition compared at 400 μg/mL. (d) Inhibition curves of the pure phenolic combinations on HCT 116 cells. (e) The IC50 values of the pure phenolic combinations on HCT 116 cells (mean ± SEM). (f) Inhibition curves of the pure phenolics and red grape combination on HT-29 cells. (g) The IC50 values of the pure phenolics and red grape combination on HT-29 cells (mean ± SEM). Letters indicate statistical difference between phenolics per column as determined by the Tukey test (p < 0.05). Table c presents the statistics for the IC50 inhibitions of HCT 116 cells by phenolics and anthocyanins. Table (e) presents the statistics for the IC50 inhibitions of HCT 116 cells by combination of phenolics and anthocyanins present in represented extracts. Table (g) presents the statistics for the IC50 inhibitions of HT-29 cells by phenolics and anthocyanins; statistics are compared within the table only for each column. At least two independent experiments were run with triplicate data points. *Inhibition for delphinidin chloride at 600 μg/mL was 43.9%. GA, gallic acid; DC, delphinidin chloride; D3G, delphinidin-3-O-glucoside; PB1, procyanidin B1; C3G, cyanidin-3-O-glucoside; M3G, malvidin-3-O-glucoside; RG, red grape; BL, black lentil; SH, sorghum; NA, not applicable; ND, not able to be determined.
Black lentil and red grape extracts had an additive effect on oxaliplatin inhibition of HCT 116 cells, but delphinidin-3-O-glucoside had a slightly antagonistic effect
Figure 2 shows that both BLE and RGE had an additive effect with oxaliplatin. The V values were 0.84 and 0.90 for BLE and RGE respectively, putting them in the additive range (0.7–1.3)23. However, D3G had a V value of 0.61, which just put it in the antagonistic range (V < 0.7).
Isobolograms of anthocyanin-rich extracts or delphinidin-3-O-glucoside and oxaliplatin with their V values and the type of effect based on the V value ranges. (a) Red grape. (b) Black lentil. (c) Delphinidin-3-O-glucoside. D3G, delphinidin-3-O-glucoside. Two independent experiments were performed with triplicate data points.
Transformation of anthocyanins that inhibited cell viability after incubation with HCT 116 cells
When performing the cell viability tests with ANC, notable color changes in the culture media occurred after 24 h of treatment on HCT 116 cells as shown in Supplementary Fig. 2. D3G had a more drastic color change (Supplementary Fig. 2a), while C3G and M3G (Supplementary Fig. 2b,c) had dulling of the color, but the media appeared to better retain its hue angle. Supplementary Fig. 2 shows that D3G is no longer present (at 520 nm) in media, after the 24 h treatment on the cells, as there was no peak at the D3G retention time detectable by the HPLC software. However, for C3G and M3G the major peak remains after 24 h treatment, at lower peak intensity. Colorimeter tests in Supplementary Table 1 show a similar decrease in saturation, dulling of the color, for all three ANC but a larger change in L*, a*, and b* parameters for D3G.
Delphinidin-3-O-glucoside and its metabolites induced apoptosis in HCT 116 cells
Figure 3 shows the results of apoptosis induction by D3G, its metabolites (DC and GA), and the pure compound combination RGC, in comparison to untreated cells. There was a significant increase in apoptotic cells due to D3G, DC, and GA (p values of 0.0075, 0.0035, and <0.0001, respectively). GA had the highest percentage of apoptotic cells (41.5%), followed by DC (27.9%) and D3G (25.8%). The increase of apoptotic cells caused by RGC was not statistically higher than the untreated DMSO control (p = 0.1735). The basis for the quadrant placements is shown in Supplementary Fig. 3.
Flow cytometry plots (propidium iodide (PI) vs annexin V FITC (fluorescein isothiocyanate) and percentages of total apoptotic HCT 116 human colon cancer cells. The total of apoptotic cells is the combined percentage of early and late apototic cells, quadrants two and four, respectively. (a) Untreated. (b) Delphinidin-3-O-glucoside. (c) Delphinidin chloride. (d) Gallic acid. (e) Percent of apoptotic cells for all tested treatments. The results are expressed as mean ± SEM. Different letters indicate statistical difference among all treatments as determined by Tukey test p < 0.05. At least two independent experiments with duplicate data points were performed. D3G, delphinidin-3-O-glucoside; DC, delphinidin chloride; OX, oxaliplatin; RGC, red grape combination; UNT, untreated; UNT D, untreated DMSO. RGC was compared to UNT D; both had 0.3% DMSO.
Cyanidin-3-O-glucoside treatment of peripheral blood mononuclear cells prior to co-culture with HT-29 cells increased LDH activity
Supplementary Fig. 4 shows the LDH activity results for the co-culture. Compared to the untreated HCT 116 monoculture, LDH activity increased for each co-culture of PBMC with HCT 116 cells by 53.3% for the untreated, 47.0% for the D3G pretreated, 49.5% for the C3G pretreated, and 74.5% for the pembrolizumab pretreated (p values of 0.0114, 0.0242, 0.0303, and 0.0034, respectively) (Supplementary Fig. 4a). There was no statistical difference between the untreated PBMC and the pre-incubation of PBMC with C3G, D3G, or pembrolizumab (p values of 0.3254, 0.9229, and 0.9799, respectively). Compared to the untreated HT-29 monoculture, LDH activity increased for each co-culture of PBMC with HT-29 cells by 51.1% for the untreated, 61.0% for the D3G pretreated, 93.8% for the C3G pretreated, and 118.0% for the pembrolizumab pretreated (p values of 0.0141, 0.0101, 0.0009, and 0.0002, respectively). There was a significant increase induced by C3G and pembrolizumab compared to the untreated co-culture (p values of 0.0489 and 0.0098, respectively) (Supplementary Fig. 4b).
Delphinidin-3-O-glucoside, its metabolites, and D3G-rich plant extracts decreased expression of VEGF and PD-L1
Figure 4 shows the western blot results for D3G, DC, GA, RGC, RGE, and BLE with VEGF for both HCT 116 and HT-29 cells. In HCT 116 cells (Fig. 4a), all treatments decreased VEGF expression significantly compared to the untreated cells except BLE, with D3G decreasing the protein expression 57.2%. In HCT 116 cells, all treatments decreased the expression of PD-L1 compared to the untreated control, with RGC reducing the protein expression by 68.7%. C3G did not significantly decrease the PD-L1 expression with 20.7% inhibition compared to the untreated control (p > 0.05) (data not shown in the figure). In HT-29 cells (Fig. 4b), all treatments reduced VEGF expression compared to the control, with RGE inducing the largest decrease (64.6%) and not statistically different than DC (59.1%). PD-L1 expression was too low in HT-29 cells to evaluate the effect of the treatments through western blots since well-developed bands could not be elucidated.
Comparison of the percent of protein expression relative to the untreated (UNT) control normalized to GAPDH for vascular endothelial growth factor (VEGF) and programmed death-ligand 1 (PD-L1) for delphinidin-3-O-glucoside (D3G), delphinidin chloride (DC), red grape combination (RGC), red grape extract (RGE), and black lentil extract (BLE) and the associated protein band examples for (a) HCT 116 human colon cancer cells. (b) HT-29 human colon cancer cells (VEGF only). RGC was compared to untreated DMSO (UNTD); both had 0.3% DMSO. Western blot pictures were cropped and full-length blots are shown in Supplementary Figs 6 and 7. The results are expressed as mean ± standard error. Different letters indicate statistical difference between treatments and the untreated control (100%) as determined by Student’s T-test (p < 0.05) per protein tested per cell line. At least two independent experiments were run. c. ELISA results for PD-L1 and programmed cell death protein 1 (PD-1) in terms of percent inhibition compared to the untreated control in monoculture or co-culture. The results are expressed as mean ± standard error. Asterisks indicates statistical difference from the untreated control as determined by Student’s T-test (p < 0.05) compared within each monoculture or coculture tested. GAPDH, glyceraldehyde 3-phosphate; MW, molecular weight; C3G, cyandin-3-O-glucoside; PBMC, peripheral blood mononuclear cells; ATZ, atezolizumab; PMB, pembromolizumab.
Cyanidin-3-O-glucoside was the only non-pharmaceutical treatment to inhibit PD-L1 expression through ELISA analysis
Results are shown for D3G, C3G, and atezolizumab in Fig. 4c.
In both HCT 116 and HT-29 cells, there were no significant inhibitions of PD-L1 by any of the D3G related pure compounds or extracts. However, C3G significantly inhibited PD-L1 in HCT 116 cells at 39.5% (p = 0.0110). Atezolizumab had high inhibition of PD-L1 in both cell lines: 85.9% for HCT 116 and 79.1% for HT-29 cells compared to the untreated control cells. It was also shown that the expression of PD-L1 was much higher in pg per µg of total protein in HCT 116 cells vs. HT-29 cells with 3.7 times the amount of PD-L1 protein in HCT 116 cells.
Cyanidin-3-O-glucoside and delphinidin-3-O-glucoside inhibit PD-1 through ELISA analysis in both monoculture and co-culture
C3G and D3G decreased PD-1 expression in peripheral blood mononuclear cells in a monoculture by 41.0% and 54.8% (p = 0.0339 and 0.0152, respectively), and in a co-culture with HCT 116 and HT-29 cells by 38.7% and 25.6% (p = 0.0007 and 0.0093, respectively), and 49.5% and 51.0% (p = 0.0378 and 0.0345, respectively), respectively, compared to the untreated control as show in Fig. 4c.
Cyanidin-3-O-glucoside decreased fluorescence intensity of PD-L1 in HCT 116 cells
Figure 5 shows examples of microscopy pictures from untreated HCT 116 cells and C3G, D3G, and DC treated cells revealing more intense fluorescence of PD-L1 in the untreated cells. C3G, D3G, and DC decreased intensity compared to the control by 39.2%, 19.1%, and 16.7%, respectively (p values of 0.0346, 0.2455, and 0.3193, respectively). Visually, there appears to be higher intensity of the PD-L1in the membrane for the untreated HCT 116 cells.
Effect of anthocyanins and delphindin chloride (DC) on programmed death-ligand 1 (PD-L1) localization in the cell and fluorescence intensity. Examples of confocal microscopy pictures of cells. (a) Untreated (UNT), (b) Cyanidin-3-O-glucoside (C3G), (c) Delphinidin-3-O-glucoside (D3G). (d) DC. (e) The relative fluorescence intensity of PD-L1 for treatments of C3G, D3G, and DC compared to the untreated control. The results are expressed as mean ± SEM. Different letters indicate statistical difference between treatments and the untreated control (100%) as determined by Student’s T-test (p < 0.05). At least two independent experiments were run. At least three sections of a well were used to quantify the expression of PD-L1 in Zen 2 (blue edition) software. White arrows indicate visualization of membrane localization of the protein.
Delphinidin-3-O-glucoside and cyanidin-3-O-glucoside show potential to inhibit VEGF and immune checkpoints in silico
All tested phenolics (D3G, C3G, DC, M3G, GA, and PB1) were predicted to bind to immune checkpoints (PD-1 and PD-L1) and VEGF (Fig. 6). For the drug binding sites of PD-1 and PD-L1, C3G and D3G (−5.9 kcal/mol) had the highest binding affinity. For PD-1 at the binding site of PD-L1, C3G and PB1 had a binding affinity of −6.8 and −6.1 kcal/mol, respectively. For PD-L1 at a small molecule inhibitor site, C3G and DC had the most negative predicted free energy of binding with −9.6 and −8.4 kcal/mol, respectively. For VEGF, C3G, PB1, and D3G had the highest binding affinity for both the VEGFR1 and VEGFR2 binding sites. Common interactions between C3G and the small molecule inhibitor for PD-L1 were a polar interaction with SER93 and a hydrophobic interaction with LEU50 (Supplementary Table 4). D3G shared a polar interaction with GLN99 with the small molecule inhibitor for PD-1. The immune checkpoint CTLA4 was also modeled with the phenolics at the site of the drug ipilimumab (data not shown). D3G and C3G also had highest binding affinity of the phenolics, with −5.6 and −5.3 kcal/mol, respectively; GA had the lowest at −3.6 kcal/mol. The two-dimensional modeling pictures of the ANC ligands in the immune checkpoint proteins and VEGF are shown in Fig. 6 and the three-dimensional pictures in Supplementary Fig. 5. There were several similar amino acid interactions not only among the phenolics but also among the phenolics and the small molecule inhibitor used as a comparison for each protein. These interactions are shown in Supplementary Tables 2, 3 and 4 for PD-1, PD-L1, and VEGF, respectively.
Two-dimensional figures including distances of interactions between an immune checkpoint or vascular endothelial growth factor (VEGF) protein and a phenolic ligand for (a) Procyanidin B1(PB1) and programmed cell death protein 1 (PD-1). (b) Delphinidin-3-O-glucoside (D3G) and programmed death-ligand 1(PD-L1). (c) Cyanidin-3-O-glucoside (C3G) and VEGF. (d) Free energy of binding for two sites on PD-1, PD-L1, or VEGF with phenolic ligands: C3G, PB1, D3G, malvidin-3-O-glucoside, delphinidin chloride, gallic acid, and a small molecule inhibitor. The top two or three phenolics with the highest binding affinities are bolded. *The small molecule 8YZ was used for PD-1 and PD-L1 sites except for the 8J8 site. For the 8J8 site on PD-L1, the actual 8J8 molecule was selected. Vatalanib was utilized for VEGF at VEGFR1 and PTC-858 for VEGFR2. Lengths given in the figures are in angstroms.
Delphinidin-3-O-glucoside and cyanidin-3-O-glucoside demonstrate static quenching of immune checkpoints
Figure 7 shows the fluorescence spectra of anthocyanins, D3G and C3G, with immune checkpoints, PD-1 and PD-L1. F0/F was plotted against concentration to obtain the Ksv and then kq values. The calculated kq values for each interaction demonstrate a static quenching indicating a formation of a complex between the immune checkpoint proteins and anthocyanins based on the kq values being higher (320–488 times) than the diffusion-limited quenching in water of 1010 mol−1 s−1 30.
Fluorescence quenching of immune checkpoints programmed cell death protein 1 (PD-1) and programmed death-ligand 1 (PD-L1) by anthocyanins. Representative fluorescence spectra for (a) Delphinidin-3-O-glucoside (D3G) with PD-1 (b) D3G with PD-L1 (c) Cyanidin-3-O-glucoside (C3G) and PD-1 and (d) C3G and PD-L1. (e) Table showing Ksv and kq values given as the mean ± standard error of mean, with two independent replicates of each concentration (1 mM, 500 µM, 250 µM, 100 µM, 10 µM). No statistical difference among Ksv values (p > 0.05) for each protein and anthocyanin interaction as determined by Tukey-Kramer. (f) The Stern-Volmer equation where F0 is the fluorescence intensity of the protein peak at 354 nm without a quencher, F is the fluorescence intensity at a given concentration of quencher [Q], Ksv is theh Stern–Volmer quenching constant, kq is the bimolecular quenching constant, and 𝜏0 is the average lifetime of protein without quencher, value as defined in the figure.
Discussion
Recent in vitro and in vivo studies have reported the inhibitory effects of ANC-rich extracts from a wide range of sources on proliferation and progression of colon cancer cells; however, little has been shown on ANC-rich extracts on the immune response in the tumor microenvironment31,32,33,34. Additionally, a lesser number of studies have analyzed the ability of pure ANC to inhibit colorectal cancer progression in vitro35,36. We discovered that the only ANC tested that was effective at colorectal cancer cell inhibition in HCT 116 cells was D3G. Another study found that M3G was not effective, but metabolites, GA, 3-O-methylgallic acid, and 2,4,6-trihydroxybenzaldehyde were successful inhibiting HCT 116 cells, as well as other colorectal cancer cells37. In our study, we found that GA had a dose-dependent inhibition in both cell lines, HCT 116 and HT-29. It was expected that combining ANC and phenolics in ratios representative of phenolic-rich extracts would result in synergistic effects on the inhibition of HCT 116 cells. However, this was not seen in either cell line as determined by the RGC not being statistically better than D3G in HCT 116 cells; in HT-29 cells, D3G was significantly more effective than RGC. A study testing berry anthocyanidins (aglycones of ANC) on lung cancer cell inhibition found delphinidin as the only anthocyanidin that did not have a significantly higher inhibition with a mixture of phenolics compared to single anthocyanidin38. In the animal portion of the study, the mixture and delphinidin both exerted antitumor activity that was not statistically different. Delphinidin was the only anthocyanidin that was effective inhibiting the two lung cancer cell lines tested alone, similar to the trend in our study where D3G was the only effective ANC. D3G and its metabolites appear to play a key role in the anti-carcinogenic activity of the plant extracts.
It was demonstrated that the ANC-rich extracts did not negatively affect the ability of oxaliplatin to decrease colorectal cancer viability; however, D3G did have a slightly antagonistic effect. In a study looking at the effects of the phenolic compound quercetin on cisplatin (also in the platinum-containing family of drugs) in ovarian cancer models, it was concluded that quercetin had an antagonistic effect on cisplatin at low concentrations39. However, quercetin and its related glycoside, rutin, have been reported to decrease peripheral neuropathy, a common side effect of oxaliplatin treatment in mice that received biweekly injections of oxaliplatin40.
Significant color changes and lack of HPLC peak retention coincided with greater efficacy of D3G to inhibit HCT 116 viability in comparison to C3G and M3G. These observations led us to believe that cell uptake and transformation of D3G was occurring in the HCT 116 cells, the metabolites of D3G were having an impact on viability, or a combination of both. Comparing the structure of C3G versus D3G, the difference is that D3G has an additional hydroxyl group on its B-ring. More hydroxyl groups have been connected to less stable pigment but also to higher antioxidant capacity41. A study using Caco-2 cells testing black currant anthocyanins found that delphinidins were both less stable and had higher initial absorption efficiency than the cyanidin derivatives42. These studies corroborate our findings of a more considerable color change and reduction of cancer cell viability induced by D3G versus C3G. Additionally, with a higher degradation of D3G, it is likely that the degradation products of D3G were also impacting the reduction in cell viability.
We found that D3G, DC, and GA induced apoptosis significantly, providing further mechanistic knowledge. A study that analyzed grape and strawberry ANC-rich extracts found that the extracts and one of the metabolites induced apoptosis43. Additionally, a java plum extract containing glucosides of delphinidin was shown to increase apoptosis in HCT 116 cells44. These studies provide evidence that ANC-rich extracts can stimulate apoptosis, including those that have D3G or its derivatives as a main component of the ANC profile. Here, we looked at individual components and metabolites and showed that D3G alone can induce apoptosis, as well as its metabolites, DC and GA. Analysis continued in relation to angiogenesis and immune response by determining VEGF expression effects. In both HCT-116 and HT-29 cells, VEGF expression decreased due to D3G, DC, GA, and D3G-rich treatments (RGC, BLE, and RGE). A study discovered that pomegranate juice extract that contained 3-glucosides and 3,5-diglucosides of delphinidin, cyanidin, and pelargonidin was successful at reducing VEGF expression in HT-29 cells45. In the in silico analysis, we found that C3G, PB1, and D3G had the most potential to inhibit VEGF at the VEGFR1 and VEGFR2 sites of the protein, but ANC and metabolites may have more of an affinity at the VEGFR1 site. Previously, we demonstrated that D3G and C3G had a high binding affinity with VEGFR218. Also, research on ellagic acid, a phenolic compound abundant in plant foods, showed anti-angiogenic potential through docking analysis by revealing strong bonds at the ATP site of the VEGFR-2 kinase domain46. We build on the in silico angiogenesis and immune response analysis to show that these ANC also have a potential to inhibit VEGF, a ligand of VEGFR1 and VEGFR2.
Immunotherapy techniques have been identified as pivotal strategies to implement in combination with other therapies, to combat cancer progression and resistance47. D3G, DC, GA, and D3G-rich treatments (RGC, BLE, and RGE) reduced PD-L1 protein expression compared to the untreated HCT 116 cells. Based on the docking results, C3G was shown to have the highest potential of all the pure compounds to inhibit PD-L1 at the small inhibitor site. At the sites of the drug inhibitors for both PD-1 and PD-L1, C3G and D3G had the same predicted binding energy. This was confirmed in fluorescence quenching analysis, where C3G and D3G showed static quenching with both PD-1 and PD-L1 with no statistical difference in Stern-Volmer constants. These results confirmed the potential of C3G and D3G to form complexes with immune checkpoint proteins. C3G was able to inhibit PD-L1 expression in the ELISA and as shown through lowering fluorescence intensity of PD-L1 where D3G and its metabolites did not. Despite higher expression of PD-L1 in HCT 116 cells and the microsatellite stability differences (HCT 116 instable and HT-29 stable), atezolizumab was successful at inhibiting the expression in both cell lines. D3G, its related metabolites and extracts, and C3G inhibited PD-L1, which could decrease the binding of PD-L1 to PD-1 resulting in activation of T cells in the tumor microenvironment. D3G and C3G also inhibited PD-1 expression not only in PBMC cells in a monoculture but as pretreatments in a co-culture model with both HCT 116 and HT-29 cells; this showed their potential to block both immune suppressive proteins. Additionally, C3G pre-treated PBMC increased cytotoxicity of HT-29 cells in a co-culture. An in vivo hepatocellular cancer study with Lonicera caerulea ‘Beilei’ fruit showed this ANC-rich extract was able to alter the immunoregulatory activity48. ANC-rich black raspberries were researched in an in vivo esophageal cancer model and were reported to positively modulate cytokine and immune cell response, focusing on the innate immune response49. These studies showed a potential of ANC-rich extracts to promote an immune response in other cancers. A recent in vivo study using aronia berry demonstrated the ability of ANC-rich extracts to hinder colitis progression through T cell modulation50. Here, we add to the potential mechanisms of how ANC and ANC-rich extracts may affect the immune response, specifically demonstrating their impact on immune checkpoints.
In summary, this study showed that D3G and its metabolites, DC and GA, inhibited HCT 116 and HT-29 human colon cancer cell viability in a dose-dependent manner and induced apoptosis. D3G treatment on HCT 116 cells, produced significant changes in chromatographic profile and color parameters in cell media correlating with its inhibition ability. In silico screening showed potential for ANC and their metabolites to inhibit immune checkpoints and VEGF, with C3G indicating overall more favorable binding energies. Despite C3G not reducing the viability of either colorectal cancer cell line directly, PBMC pre-treated with C3G increased cytotoxicity of HT-29 cells, and C3G inhibited PD-L1 in vitro. D3G, its metabolites, and D3G-rich treatments (RGC, BLE, and RGE) decreased the expression of PD-L1 and VEGF proteins. C3G and D3G inhibited PD-1 expression in both a monoculture of PBMC, as well as through pre-incubation of PBMC in a co-culture with HCT 116 and HT-29 cells. A summary of the pure phenolic effects seen in this study are shown in Fig. 8. The results of this research demonstrated the potential of ANC to promote immune destruction of colorectal cancer cells by inhibiting negative regulators, immune checkpoints, of the adaptive response in both colorectal cancer cells and immune cells. To our knowledge this research shows for the first time, the potential for pure ANC and their metabolites to inhibit immune checkpoints. This contributes to the understanding of the anti-carcinogenic potential of ANC-rich foods, opening further exploration of their stimulatory effects on the immune response.
Summary of the effects of anthocyanins and metabolites on the immune response markers tested. Inhibition (bar-headed lines) or promotion (arrows) shown if effects were seen through western blots, ELISA, confocal microscopy, and/or in silico analysis. C3G, cyanidin-3-O-glucoside; D3G, delphinidin-3-O-glucoside; DC, delphinidin chloride; GA, gallic acid; MHC, major histocompatibility complex; PD-1, programmed cell death protein 1; PD-L1, programmed death-ligand 1; TCR, T cell receptor; VEGF, vascular endothelial growth factor.
Data Availability
Availability of data and material: All data generated or analyzed during this study are included in this published article [and its supplementary information files].
References
National Institutes of Health. Colorectal Cancer - Cancer Stat Facts. Available at: https://seer.cancer.gov/statfacts/html/colorect.html (Accessed: 22nd June 2018) (2019).
PDQ Adult Treatment Editorial Board. Colon Cancer Treatment (PDQ®): Health Professional Version. PDQ Cancer Information Summaries (2002).
Li, Y.-L., Zhao, H. & Ren, X.-B. Relationship of VEGF/VEGFR with immune and cancer cells: staggering or forward? Cancer Biol. Med. 13, 206–14 (2016).
Chen, D. S. & Mellman, I. Elements of cancer immunity and the cancer–immune set point. Nature 541, 321–330 (2017).
Lynch, D. & Murphy, A. The emerging role of immunotherapy in colorectal cancer. Ann. Transl. Med. 4(16), 305 (2016).
Boland, C. R. & Goel, A. Microsatellite instability in colorectal cancer. Gastroenterology 138, 2073–2087.e3 (2010).
Passardi, A., Canale, M., Valgiusti, M. & Ulivi, P. Immune Checkpoints as a Target for Colorectal Cancer Treatment. Int. J. Mol. Sci. 18, 1324 (2017).
National Cancer Institute. Combination of Immunotherapy Drugs Approved for Metastatic Colorectal Cancer. Available at: https://www.cancer.gov/news-events/cancer-currents-blog/2018/fda-ipilimumab-nivolumab-colorectal-dna-repair (Accessed: 20th November 2018) (2018).
Mckee, A. S., Macleod, M. K. L., Kappler, J. W. & Marrack, P. Immune mechanisms of protection: can adjuvants rise to the challenge? BMC Biol. 8, 1–10 (2010).
American Institute for Cancer Research. Learn About Colorectal Cancer. Available at: http://www.aicr.org/learn-more-about-cancer/colorectal-cancer/ (Accessed: 22nd June 2018) (2018).
Wang, L.-S. & Stoner, G. D. Anthocyanins and their role in cancer prevention. Cancer Lett. 269, 281–290 (2008).
Amin Moosavi, M. et al. Phytochemicals as potent modulators of autophagy for cancer therapy. Cancer Lett. 424, 46–69 (2018).
Choe, Y.-J. et al. Anthocyanins in the black soybean (Glycine max L.) protect U2OS cells from apoptosis by inducing autophagy via the activation of adenosyl monophosphate-dependent protein kinase. Oncol. Rep. 28, 2049–2056 (2012).
Mazewski, C. & De Mejia, E. G. Impact of anthocyanins on colorectal cancer. In Advances in Plant Phenolics: From Chemistry to Human Health, https://doi.org/10.1021/bk-2018-1286.ch0019 (American Chemical Society, 2018).
Fernandes, I., Faria, A., Calhau, C., de Freitas, V. & Mateus, N. Bioavailability of anthocyanins and derivatives. J. Funct. Foods 7, 54–66 (2014).
Fan, M. J. et al. Anthocyanins from black rice (Oryza sativa) promote immune responses in leukemia through enhancing phagocytosis of macrophages in vivo. Exp. Ther. Med. 14, 59–64 (2017).
Mazewski, C., Liang, K. & Gonzalez de Mejia, E. Inhibitory potential of anthocyanin-rich purple and red corn extracts on human colorectal cancer cell proliferation. in vitro. J. Funct. Foods 34, 254–265 (2017).
Mazewski, C., Liang, K. & Gonzalez de Mejia, E. Comparison of the effect of chemical composition of anthocyanin-rich plant extracts on colon cancer cell proliferation and their potential mechanism of action using in vitro, in silico, and biochemical assays. Food Chem. 242, 378–388 (2018).
Ahmed, D. et al. Epigenetic and genetic features of 24 colon cancer cell lines. Oncogenesis 2, e71 (2013).
Khoo, H. E., Azlan, A., Tang, S. T. & Lim, S. M. Anthocyanidins and anthocyanins: colored pigments as food, pharmaceutical ingredients, and the potential health benefits. Food Nutr. Res. 61 (2017).
Xie, L. et al. Bioavailability of anthocyanins and colonic polyphenol metabolites following consumption of aronia berry extract. Food Chem. 211, 860–868 (2016).
Stalmach, A., Edwards, C. A., Wightman, J. D. & Crozier, A. Colonic catabolism of dietary phenolic and polyphenolic compounds from Concord grape juice. Food Funct. 4, 52–62 (2013).
Timbrell, J. Principles of Biochemical Toxicology, Fourth Edition., https://doi.org/10.3109/9781420007084 (CRC Press, 2008).
Li, Q., Somavat, P., Singh, V., Chatham, L. & Gonzalez de Mejia, E. A comparative study of anthocyanin distribution in purple and blue corn coproducts from three conventional fractionation processes. Food Chem. 231, 332–339 (2017).
Mojica, L., Berhow, M. & Gonzalez de Mejia, E. Black bean anthocyanin-rich extracts as food colorants: Physicochemical stability and antidiabetes potential. Food Chem. 229, 628–639 (2017).
Dia, V. P. & de Mejia, E. G. Lunasin induces apoptosis and modifies the expression of genes associated with extracellular matrix and cell adhesion in human metastatic colon cancer cells. Mol. Nutr. Food Res. 55, 623–634 (2011).
Zak, K. M. et al. Structure of the Complex of Human Programmed Death 1, PD-1, and Its Ligand PD-L1. Struct. Des. 23, 2341–2348 (2015).
Walsh, T. P. & Grant, G. H. Computer modelling of the receptor-binding domains of VEGF and PIGF. Protein Eng. 10, 389–98 (1997).
Cao, L. et al. Discovery of Novel Small Molecule Inhibitors of VEGF Expression in Tumor Cells Using a Cell-Based High Throughput Screening Platform. PLoS One 11, 1–20 (2016).
Luna-Vital, D., Cortez, R., Ongkowijoyo, P. & Gonzalez De Mejia, E. Protection of color and chemical degradation of anthocyanin from purple corn (Zea mays L.) by zinc ions and alginate through chemical interaction in a beverage model, https://doi.org/10.1016/j.foodres.2017.11.009 (2018).
Kubow, S. et al. Effects of Simulated Human Gastrointestinal Digestion of Two Purple-Fleshed Potato Cultivars on Anthocyanin Composition and Cytotoxicity in Colonic Cancer and Non-Tumorigenic Cells. Nutrients 9, 953 (2017).
Choi, Y. J. et al. Açaí Berries Inhibit Colon Tumorigenesis in Azoxymethane/Dextran Sulfate Sodium-Treated Mice. Gut Liver 11, 243–252 (2017).
Fernández, J., García, L., Monte, J., Villar, C. & Lombó, F. Functional Anthocyanin-Rich Sausages Diminish Colorectal Cancer in an Animal Model and Reduce Pro-Inflammatory Bacteria in the Intestinal Microbiota. Genes (Basel). 9, 133 (2018).
Venancio, V. P. et al. Cocoplum (Chrysobalanus icaco L.) anthocyanins exert anti-inflammatory activity in human colon cancer and non-malignant colon cells. Food Funct. 8, 307–314 (2017).
Anwar, S. et al. Berry anthocyanins reduce proliferation of human colorectal carcinoma cells by inducing caspase-3 activation and p21 upregulation. Mol. Med. Rep. 14, 1397–1403 (2016).
Jing, P. et al. Effect of glycosylation patterns of Chinese eggplant anthocyanins and other derivatives on antioxidant effectiveness in human colon cell lines. Food Chem. 172, 183–189 (2015).
Forester, S. C., Choy, Y. Y., Waterhouse, A. L. & Oteiza, P. I. The anthocyanin metabolites gallic acid, 3-O-methylgallic acid, and 2,4,6-trihydroxybenzaldehyde decrease human colon cancer cell viability by regulating pro-oncogenic signals. Mol. Carcinog. 53, 432–439 (2014).
Kausar, H. et al. Berry anthocyanidins synergistically suppress growth and invasive potential of human non-small-cell lung cancer cells. Cancer Lett. 325, 54–62 (2012).
Li, N. et al. Low Concentration of Quercetin Antagonizes the Cytotoxic Effects of Anti-Neoplastic Drugs in Ovarian Cancer. PLoS One Nat. Sci. Found. Hubei Prov. 9(7), e100314 (2014).
Azevedo, M. I. et al. The Antioxidant Effects of the Flavonoids Rutin and Quercetin Inhibit Oxaliplatin-Induced Chronic Painful Peripheral Neuropathy. Mol. Pain 9, 1744-8069-9–53 (2013).
Hernández-Herrero, J. A. & Frutos, M. J. Degradation kinetics of pigment, colour and stability of the antioxidant capacity in juice model systems from six anthocyanin sources. Int. J. Food Sci. Technol. 46, 2550–2557 (2011).
Steinert, R. E., Ditscheid, B., Netzel, M. & Jahreis, G. Absorption of Black Currant Anthocyanins by Monolayers of Human Intestinal Epithelial Caco-2 Cells Mounted in Ussing Type Chambers. J. Agric. Food Chem. 56, 4995–5001 (2008).
López de las Hazas, M.-C., Mosele, J. I., Macià, A., Ludwig, I. A. & Motilva, M.-J. Exploring the Colonic Metabolism of Grape and Strawberry Anthocyanins and Their in Vitro Apoptotic Effects in HT-29 Colon Cancer Cells. J. Agric. Food Chem. 65, 6477–6487 (2017).
Charepalli, V. et al. Eugenia jambolana (Java Plum) Fruit Extract Exhibits Anti-Cancer Activity against Early Stage Human HCT-116 Colon Cancer Cells and Colon Cancer Stem Cells. Cancers (Basel). 8, 1–11 (2016).
Banerjee, N., Kim, H., Talcott, S. & Mertens-Talcott, S. Pomegranate polyphenolics suppressed azoxymethane-induced colorectal aberrant crypt foci and inflammation: possible role of miR-126/VCAM-1 and miR-126/PI3K/AKT/mTOR. Carcinogenesis 34, 2814–2822 (2013).
Wang, N. et al. Ellagic acid, a phenolic compound, exerts anti-angiogenesis effects via VEGFR-2 signaling pathway in breast cancer. Breast Cancer Res. Treat. 134, 943–955 (2012).
Greaves, M. Nothing in cancer makes sense except …. BMC Biol. 16, 22 (2018).
Zhou, L. et al. Anti-tumor properties of anthocyanins from Lonicera caerulea ‘Beilei’ fruit on human hepatocellular carcinoma: In vitro and in vivo study. Biomed. Pharmacother. 104, 520–529 (2018).
Peiffer, D. S. et al. Dietary consumption of black raspberries or their anthocyanin constituents alters innate immune cell trafficking in esophageal cancer. Cancer Immunol. Res. 4, 72–82 (2016).
Pei, R. et al. Dietary Prevention of Colitis by Aronia Berry is Mediated Through Increased Th17 and Treg. Mol. Nutr. Food Res. 63(5), 1800985 (2018).
Acknowledgements
This work was partially supported by USDA National Institute of Food and Agriculture Hatch project 1014457.
Author information
Authors and Affiliations
Contributions
C.M. was the major contributor in writing the manuscript. She completed all experiments, analyzed the data, and created the figures and tables except those related to in silico docking. S.K. aided in numerous experiments including cell lysates and western blots. His major contribution was performing the in silico analysis and constructing the related figures and tables. He contributed to writing the methods and results related to the docking experiments and helped with the editing process of the document. E.D.M. contributed to the idea and design of the study and interpretation of all results. She assisted with writing and editing the manuscript and provided scientific guidance throughout the study. E.D.M. also provided all sources of funding. All authors have read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Mazewski, C., Kim, M. & Gonzalez de Mejia, E. Anthocyanins, delphinidin-3-O-glucoside and cyanidin-3-O-glucoside, inhibit immune checkpoints in human colorectal cancer cells in vitro and in silico. Sci Rep 9, 11560 (2019). https://doi.org/10.1038/s41598-019-47903-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-019-47903-0
This article is cited by
-
Dietary factors and their influence on immunotherapy strategies in oncology: a comprehensive review
Cell Death & Disease (2024)
-
Medicinal plants cultivated in Egypt with anticancer potential; a systematic review
Phytochemistry Reviews (2024)
-
Anticancer potential of delphinidin and its derivatives: therapeutic and mechanistic insights
Medicinal Chemistry Research (2024)
-
Artichoke extracts in cancer therapy: do the extraction conditions affect the anticancer activity?
Future Journal of Pharmaceutical Sciences (2020)
-
ST2 and regulatory T cells in the colorectal adenoma/carcinoma microenvironment: implications for diseases progression and prognosis
Scientific Reports (2020)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.