Abstract
Androgens are known to be an essential regulator of male health. Androgen receptor (AR) is widely expressed throughout the adrenal cortex, yet the wider role for androgen signalling in the adrenal remains underexplored. To investigate AR-dependent and AR-independent androgen signalling in the adrenal, we used a novel mouse model with a specific ablation of androgen receptor in the adrenal cortex with or without reduction of circulating androgen levels by castration. Our results describe AR expression in the human and mouse adrenal and highlight that the mouse is a viable model to investigate androgen signalling in the adrenal cortex. We show androgen signalling via AR is required for X-zone regression during puberty. Furthermore, cortex measurements define differences in X-zone morphology depending on whether circulating androgens or AR have been removed. We show androgens promote both cortical cell differentiation and apoptosis but are dispensable for the formation of the definitive cortex. Additionally, investigation of aged mice with AR ablation reveals severe cortex disruption, spindle cell hyperplasia and X-zone expansion. The data described herein demonstrates AR-signalling is required to facilitate X-zone regression, cell clearance and to protect against adrenal degeneration during ageing.
Similar content being viewed by others
Introduction
Androgens are essential regulators of male health, primarily in the maintenance and development of male sexual characteristics1. A decline in circulating androgens has been associated with co-morbidities such as obesity2 cardiac disease3 and metabolic syndrome4. Androgen production in men occurs predominantly in the testis (~90%) with a small proportion produced in the zona reticularis (ZR) of the adrenal cortex5,6. Androgens primarily exert their effects through their cognate androgen receptor (AR), a nuclear receptor to testosterone and dihydrotestosterone. Upon binding, AR undergoes translocation into the nucleus to regulate gene transcription7. Androgens and AR have also been shown to act independently of each other to regulate cellular processes8.
Previous research has focussed upon the body-wide impact of adrenal androgens9. However, whilst AR is abundantly expressed in the adrenal cortex of both rodents10,11, and humans12,13, surprisingly little is known about androgen action on the adrenal cortex itself. This gap in our understanding is at least in part due to the perceived lack of suitable animal models. Mice have largely been overlooked as a model system for the human adrenal as mouse adrenals are unable to produce androgens due to the silencing of Cyp17a1 early in development. This lack of expression results in no 17α hydroxylase and 17, 20 lyse activity and consequently the rodent adrenal does not have a zona reticularis14,15. The fetal adrenal is thought to give rise to the adult adrenal cortex in both humans and mice16,17, so understanding the mechanisms that underpin its regulation is essential. In the mouse, these fetal cells are maintained for a period postnatally and regress in a sex dependent manner. In the human, this zone is known as the ‘fetal zone’, with the mouse homologue termed the ‘X-zone’18,19. Historical studies using castrated mice show that removal of circulating androgens leads to the redevelopment of an additional cortex zone known as the transient X-zone20. The redevelopment of the X-zone following castration and the abundant expression of AR in the mouse adrenal suggests that androgens are important regulators of the adrenal cortex and that despite not producing adrenal androgens, the mouse has utility for dissecting the role of androgen signalling within the adrenal. Previous global knockouts have ablated AR from the adrenal21, however, the caveats of this, like many global knockout models, is that the adrenals both produce and respond to multiple endocrine stimuli. For these reasons, it is difficult to attribute any phenotype to perturbed endocrine signalling locally rather than disruption of the wider hypothalamic-pituitary-axis.
For these reasons, we generated an adrenal-specific androgen receptor knockout model (Ad-ARKO) that ablates AR from the adrenal cortex in fetal and adult life22, permitting investigation of adrenal AR signalling. Due to the ability of AR and androgens to act independently of each other, additional models of castrated wild-type and castrated AR-ablated animals were investigated in parallel with the Ad-ARKO model, allowing us to independently dissect both androgen and AR action in the adrenal. We show that androgen signalling via the androgen receptor required for X-zone regression, furthermore, that androgens and androgen receptor also work independently to regulate multiple aspects of adrenal cortex function and morphology.
Results
Androgen receptor is widely expressed throughout the human and mouse adrenal cortex
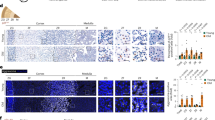
AR mRNA has been shown to be present in human and mouse adrenals12,23, however AR localisation in the adrenal cortex in human and mice has yet to be defined. To establish AR location within the adrenal cortex, human and mouse adrenals were examined using immunohistochemistry. Expression of human AR can be seen in the definitive cortex in fetal adrenals and in the zona reticularis of the adult adrenal. Unexpectedly, despite AR being a nuclear receptor, localisation of AR in human tissue is observed in the cytoplasm (Fig. 1a). Analysis of the mouse fetal adrenal shows nuclear AR protein expression throughout the adrenal at (e)13.5 (Fig. 1b). AR protein is also present in the postnatal male mouse adrenal when examined at d12, d21, d35 and d80. AR is localised in cells at the cortex-medulla boundary at d12; by d21 AR is localised in cells throughout the zona fasciculata (ZF), and from d35 onward AR can be seen in cells in the ZF and zona glomerulosa (ZG) (Fig. 1c). These data confirm the expression of AR in both human and mouse adrenals during development and in adulthood, although differing in cellular location in the human and mouse, this suggests that despite a lack of androgen production, the mouse adrenal has human relevance as a model system for the study of the within-adrenal response to androgen stimulation. For these reasons, we generated an adrenal-specific mouse model to investigate the role of androgen receptor in the adrenal cortex.
Androgen receptor expression in the adrenal cortex. (a) AR immunostaining details AR expression in the cytoplasm of the definitive zone in fetal (19 weeks) and in the cytoplasm of the zona reticularis in adult human adrenals (N = 2). Human fetal and adult adrenal samples are male. (b) AR localisation can be detected at e13.5 in mouse embryonic adrenals, with staining in the central region of the fetal adrenal (N = 3). (c) Expression of AR observed during development shows changes in localisation from the inner most cortex/medulla boundary at d12 to be present in the ZF at d21 and d35 and at d80 AR can be seen in the ZF and ZG (N = 5) (red = androgen receptor, green = sytox counterstain). PC = positive control, DZ = Definitive zone, ZR = Zona reticularis M = Medulla, ZF = Zona fasciculata, ZG = Zona glomerulosa. Scale bars 100 µm.
Confirmation of ablation of androgen receptor from the mouse adrenal
We have previously described a novel method to ablate target genes from steroidogenic cell types through the development of a GFP-Cre-GC targeted to the mouse Cyp11a1 locus to drive Cre Recombinase expression22. We established that this Cre line targets less than 20% of testicular Leydig cells22 and that loss of AR from Leydig cells has no discernible impact on circulating testosterone levels24. However, the GFP-Cre-GC line targets 100% of adrenal cortical cells, and immunostaining for AR in Ad-ARKO mice confirmed complete ablation of AR protein throughout the adrenal cortex (Fig. 2a). Interestingly, the adrenal capsule does not express Cyp11a1, therefore, Cyp11a1-Cre does not target these cells. This results in AR expression still being maintained in the capsule22,25, an important internal positive control for downstream studies. Initial observations of body weight, testis weight, and anogenital distance (AGD) show no differences in Ad-ARKO mice when compared to controls (Supplementary Fig. 1A–C).
Ad-ARKO mice show increased adrenal weight and size and have an additional cortical zone that persists into adulthood. (a) Immunofluorescence staining confirms ablation of AR from adrenal cortex (red = androgen receptor, green = sytox counterstain). (b) Observations of whole tissue at d35 and d80 demonstrate Ad-ARKO males have larger adrenals (Scale bar 1 mm). (c) Weight analysis reveals Ad-ARKO males have significantly larger adrenals from d35, this difference in size is maintained into adulthood (Two-Way ANOVA; **p < 0.001, n = 5, ****p < 0.0001, n = 5, Tukey’s post-hoc analysis, error bars SEM) (d) Adrenal histology in d12 and d21 mice appear morphologically normal compared to control males. Full regression of the X-zone is usually complete by d35 which is demonstrated in controls, however there is an additional inner cortical zone still present in Ad-ARKO males at this time point. This inner cortical zone can again be observed in d80 males, with this extra cortical zone occupying a large proportion of the adrenal cortex. M = Medulla, X = X-zone, ZF = Zona fasciculata, ZG = Zona glomerulosa. Scale bars 50 µm.
Ad-ARKO mice have enlarged adrenals and failed X-zone regression
Postnatal day 9 to 35 is a crucial remodelling period for the adrenal. During this time, the definitive cortex forms and the X-zone regresses26. Following AR ablation, we observe a fully formed definitive cortex in Ad-ARKO mice, demonstrating AR is dispensable for adrenal and definitive cortex formation. However, in line with previous studies suggesting androgens are essential for regression of the X-zone, we see a retained X-zone in Ad-ARKO mice. This is confirmed through adrenal weight and morphology analysis. Ad-ARKO adrenal weights are similar to controls in d12 or d21 male mice, however, at d35 and d80 there is a significant increase in adrenal weight compared to controls (Fig. 2c). Examination of adrenal morphology reveals the presence of a visibly more defined X-zone in d12 and d21 male Ad-ARKO adrenals compared to controls. Analysis at d35 and d80 shows X-zone retention in Ad-ARKOs (Fig. 2d). These results demonstrate that AR is essential for X-zone suppression.
Confirmation of X-zone cells in Ad-ARKO adult males
Due to the time period in which the mouse X-zone regresses, it has long been established that regulation of the adrenal by androgens does not occur until puberty26. Investigation of 20-α-hydroxysteroid dehydrogenase (20 alpha-HSD, produced by the mouse Akr1c18 gene), an X-zone specific marker27,28, at d12, d21 and d35 shows that the X-zone in Ad-ARKO mice is more advanced in developmental stage than controls before, during and after puberty (Fig. 3). This challenges the current paradigm that suggests that androgen regulation of the adrenal cortex does not occur until later in postnatal development.
20 alpha-HSD demonstrates a more developed X-zone in Ad-ARKO mice. Protein localisation of 20 alpha-HSD (Red) in the developing postnatal adrenal. It can be seen that from d12 that the X-zone in Ad-ARKO mice is more developed compared to controls. M = Medulla, X = X-zone, ZF = Zona fasciculata, ZG = Zona glomerulosa. Scale bars 100 µm.
Removal of circulating androgen results in X-zone development
It is known that castration can induce development of an X-zone in males20, and that AR and androgens can work independently of each other29,30,31,32. To provide a comprehensive overview of androgen action in the adrenal, we included additional wild-type (WT) C57BL/6J (Bl6) ‘BL6 castrated’, and ‘Ad-ARKO castrated’, cohorts in our study to determine receptor and ligand-independent effects on adrenal regulation in young adult mice (d80). These additional cohorts also show a significant increase in adrenal weight compared to controls (Fig. 4a). Morphology and 20 alpha-HSD immunolocalisation analysis conforms X-zone re-development in Bl6 castrated, and a change in the morphology of the X-zone in Ad-ARKO castrated mice (Fig. 4b,c). Furthermore, we confirm the presence of AR in WT female, and WT castrated male X-zones (Supplementary Fig. 1D). Although all experimental cohorts display an X-zone, there are clear differences in the distribution of 20 alpha-HSD localization and X-zone morphology (Fig. 4e). This suggests that the X-zone and cortex could be impacted differently depending whether circulating androgens or AR have been ablated.
Analysis of additional androgen manipulation models. In all experimental cohorts an increase in weight is detected when compared to controls (one-way ANOVA; n = 8, ***p < 0.0001, ****p < 0.0001, Tukey’s post-hoc analysis, error bars SEM). (b) Morphology analysis confirms experimental cohorts have developed an additional cortical zone. (c) qRT-PCR data shows up regulation of 20 alpha HSD expression in castrated, Ad-ARKO and Ad-ARKO castrated mice (one-way ANOVA; n = 7–8, *p < 0.05, Tukey’s post-hoc analysis, error bars SEM). (d) Immunostaining for 20 alpha-HSD confirms X-zone cells in adult cortex (Green = 20alpha-HSD, Blue = sytox counterstain). (e) Investigation of X-zones present in these cohorts show morphological differences in cell shape and size. All cohorts were collected at d80. M = Medulla, X = X-zone, ZF = Zona fasciculata, ZG = Zona glomerulosa. Scale bars 50 µm.
Morphologies of X-zones in Bl6 castrated, Ad-ARKO and Ad-ARKO castrated show distinct characteristics
Following the observation of differing X-zone morphologies after loss of AR or androgens, depth and cell density measurements were performed to distinguish differences in cortex composition between experimental cohorts. Measurements consisted of X-zone depth, X-zone cell density, ZG depth and ZF depth. X-zones in Ad-ARKO and Ad-ARKO castrated mice are significantly larger than Bl6 castrated mice (Fig. 5a). X-zones in Bl6 castrated and Ad-ARKO castrated have significantly denser X-zones per 2000 µm2 than Ad-ARKO mice (Fig. 5b). For analysis of cortex zones, a WT male adrenal has also been included for comparison. Measurements of the ZG reveals no changes in depth upon androgen manipulation between any cohorts (Fig. 5c). ZF depth is significantly smaller in Ad-ARKO mice compared to castrated cohorts however are similar in size to WT male adrenals (Fig. 5d). Measurements of complete cortex depth (ZG, ZF and X-zone) show all experimental cohorts have a larger overall cortex compared to WT male adrenals. A significant increase is also detected in Ad-ARKO castrated mice when compared to Bl6 castrated and Ad-ARKO mice (Fig. 5e). These data coupled with our morphological analysis suggest that AR and circulating androgens are able to act on the adrenal gland independently of each other, as well as in concert.
X-zones in BL6 Castrated, Ad-ARKO, and Ad-ARKO Castrated mice have distinct morphological differences. (a) Measurements of X-zone depth reveal that Ad-ARKO and Ad-ARKO Castrated mice have a significantly larger X-Zone than BL6 Castrated mice (one-way ANOVA; ***p < 0.0001, ****p < 0.0001, Tukey’s post-hoc analysis, error bars SEM). (b) The X-zone in BL6 Castrated mice is significantly denser than in Ad-ARKO mice, however upon castration of Ad-ARKO males, this cell density changes to be similar to Bl6 castrated mice (one-way ANOVA; ****p < 0.0001, Tukey’s post-hoc analysis, error bars SEM). (c) There is no significant difference in ZG depth between the four cohorts. (d) A significantly smaller ZF depth is observed in WT male adrenals and Ad-ARKO mice compared to both castrated cohorts (one-way ANOVA; *p < 0.05, **p < 0.001, Tukey’s post-hoc analysis, error bars SEM). (e) All experimental cohorts have a significantly larger overall cortex size compared to WT male adrenals (one-way ANOVA; ****p < 0.0001, ***p < 0.0001, Tukey’s post-hoc analysis, error bars SEM). Ad-ARKO castrated mice have a larger overall cortex (ZG, ZF and X-zone) compared to Bl6 castrated and Ad-ARKO mice (one-way ANOVA; *p < 0.05, **p < 0.001, Tukey’s post-hoc analysis, error bars SEM). All cohorts were collected at d80.
Transcript analysis reveals changes in key adrenal regulators
Following the observation of fluctuations in cortex zone size, we wanted to ascertain if this results in changes of known adrenal and X-zone regulators. Two well described transcription factors that have been shown to be key regulators of adrenal development are the nuclear receptors, steroidogenic factor-1 (SF1, NR5A1, also known as Ad4BP) and Dax1 (Dosage sensitive sex reversal, Adrenal hypoplasia congenita, critical region on the X chromosome, gene-1, NR0B1/AHC). Ablation or mutations in Sf1 results in adrenal agenesis, and adrenal failure in Dax1 ablation models, so determining if these are impacted following loss of androgen signalling is essential33,34,35. Furthermore a recent study has shown ablation of Prkar1a in aged mice results in the maintenance of an X-zone in adulthood in males and following a pregnancy in females36. Due to a similar phenotype being observed in Ad-ARKO mice, we investigated transcript levels of Sf1, Dax1 and Prkar1a. Transcript analysis of Sf1 shows a significant increase in all experimental cohorts when compared with controls at d80 (Fig. 6a). Dax1, shows no increase in Bl6 castrated or Ad-ARKO mice, however, there is a significant increase in transcript in Ad-ARKO castrated mice (Fig. 6b). Results show a significant downregulation of Prkar1a in all of our cohorts when compared with controls (Fig. 6c). In addition to the aforementioned key regulators, transcript analysis of Ctnnb1, Gata6, Gli1 and Wnt4, additional known regulators of the adrenal were also investigated (Supplementary Table 3A). No changes are detected in these genes in Ad-ARKO mice compared to controls. Due to the variation in cortex zones, we also confirmed that there was no impact on Actb our house-keeping gene or influence from genotype (Supplementary Fig. 1E,F). Together these data demonstrate an important role for androgens during adrenal homeostasis and suggest that genes thought to be regulating the X-zone are likely to be direct or indirect downstream targets of AR signalling.
Loss of androgen signalling results in changes in key developmental genes. (a) Sf1 gene expression analysis shows an increase in all experimental cohorts (one-way ANOVA; n = 8, **p < 0.001, ***p < 0.0001, Tukey’s post-hoc analysis, error bars SEM), however this increase was not observed in Ad-ARKO castrated males. (b) Dax1 gene expression has increased in Ad-ARKO castrated males, however this is not observed in BL6 castrated or Ad-ARKO mice (one-way ANOVA; n = 8, ***p < 0.0001, Tukey’s post-hoc analysis, error bars SEM). (c) Prkar1 gene expression has decreased in all experimental cohorts compared to controls (one-way ANOVA; n = 8, *p < 0.05, ***p < 0.0001, Tukey’s post-hoc analysis, error bars SEM). (d) Cleaved caspase 3 immunostaining shows cell death at the cortex medulla boundary. Cleaved caspase 3 staining is not present in Bl6 castrated mice or Ad-ARKO animals. In Ad-ARKO castrated mice cell death can be seen throughout the cortex. All cohorts were collected at d80. M = Medulla, X = X-zone. Scale bars 50 µm.
Immunohistochemistry analysis reveals changes in cell death marker
Due to failed regression of X-zone cells from the cortex during puberty, we investigated whether there is any disruption to normal adrenal cell apoptosis via immunostaining of cleaved caspase 3. Immunostaining of cleaved caspase 3 shows that in control mice, cortical cells undergo apoptosis at the cortex-medulla boundary, conversely, BL6 castrated and Ad-ARKO mice show no cleaved caspase-positive cells. However, Ad-ARKO castrated mice show aberrant apoptosis throughout the cortex (Fig. 6d). However, we see no differences in PCNA localisation across these cohorts compared to controls (Supplementary Fig. 1G). These results suggest that, in the absence of androgens and/or AR, the adrenal fails to appropriately differentiate its cortex zones, in addition to disruption to cell clearance from the cortex.
Disruption to AR signalling in the adrenal cortex does not impact the HPA-axis
The maintenance of an X-zone, changes in adrenal regulators and changes in morphology following AR ablation would suggest and influence adrenal function. To assess this, we examined key biomarkers of the stress response pathway; circulating corticosterone concentration37, adrenal Mc2r expression38 and circulating pituitary ACTH concentrations39. Corticosterone analysis reveals no changes in any cohort compared with controls (Fig. 7a). We show a significant increase in Mc2r expression in all experimental cohorts compared to controls (Fig. 7b). However, consistent with no changes in corticosterone, circulating ACTH shows no changes in any cohort examined (Fig. 7c). These results reveal that HPA-axis control is independent of androgen signalling in these mice.
Disruption to androgen signalling does not affect circulating corticosterone levels. (a) Circulating corticosterone levels are unchanged in all experimental cohorts compared to controls at d80. (b) Mc2r gene expression shows an increase in all cohorts compared to controls (one-way ANOVA; n = 8, ***p < 0.0001, *p < 0.05, **p < 0.001, Tukey’s post-hoc analysis, error bars SEM). (c) Circulating ACTH levels shows no changes in experimental cohorts compared to controls. (d) 3βHSD immunostaining (Red) shows the X-zone in castrated mice still positive for 3βHSD, however expression in Ad-ARKO X-zones is more sporadic with fewer positive cells and Ad-ARKO castrated mice show no expression in their X-zones. A 3βHSD negative X-zone is also noted in WT females. All cohorts were collected at d80. M = Medulla, X = X-zone. Scale bars 50 µm.
In addition to the analysis of stress hormones, mass spectrometry was used to analyse circulating androstenedione, testosterone, 17-OHP and progesterone in all cohorts (Supplementary Fig. 2A–D). The results show no changes in any cohort analysed when compared to controls. However, we do see fluctuations in several adrenal steroid enzymes and steroid receptors. Investigation of steroidogenesis markers revealed that in all experimental cohorts, CYP21A1 (protein essential for cholesterol conversion), is localised in all cortex zones compared to controls where protein is solely localised to the ZF40 (Supplementary Fig. 3A,B). This could lead to overactive steroidogenesis in the adrenal glands. Additionally, analysis of ZF marker AKR1B7 immunolocalisation revealed no positive cells in the adrenal cortex in Bl6 castrated and Ad-ARKO castrated mice. Interestingly, AKR1B7 is still expressed in Ad-ARKO mice (Supplementary Fig. 3C,D) suggesting androgens promote this expression via an AR-independent mechanism. We also noted a significant increase in glucocorticoid receptor (GR) in castrated cohorts, however, no changes in GR localisation was observed (Supplementary Fig. 3E,F). Furthermore, we also note a significant increase in AR in castrated mice (Supplementary Fig. 3G,H). We considered the possibility of AR directly regulating GR in the adrenal cortex, however, AR and GR are found in separate cell populations in the adrenal cortex, suggesting the results observed are independent or in-direct effects of AR-signalling (Supplementary Fig. 3I). A significant increase in expression of Srd5a1 was detected in Ad-ARKO castrated mice, although not significant, we also see an increase in BL6 castrated mice. This increase is potentially in response to compensate for the removal of circulating androgens (Supplementary Fig. 3J).
Of particular interest, analysis of steroidogenesis marker 3β-Hydroxysteroid dehydrogenase (3β-HSD) reveals differential staining patterns in the X-zones of all experimental cohorts. BL6 castrated mice have 3β-HSD positive X-zones, suggesting these cells have come from a definitive cortex lineage. Ad-ARKO mice have sporadic 3β-HSD cells in their X-zone, however, following castration, no positive cells can be seen in the X-zone. This suggests that some cells in the X-zone of Ad-ARKO mice are steroidogenic and lose this capability following removal of androgens (Fig. 7d). This coincides with the denser X-zones of Ad-ARKO castrated mice noted in Fig. 5b. Wild-type (WT) females have 3β-HSD positive cells throughout their cortex but do not express 3β -HSD in their X-zone. This highlights that a WT X-zone in adulthood does not express 3β-HSD and suggests the presence of androgens without AR is driving X-zone cells down a steroidogenic cell lineage that is alleviated upon castration.
Aged Ad-ARKO mice show increased disruption to the adrenal cortex
Despite X-zone maintenance, mice appear to be healthy with no major adverse phenotype, however, mice are analysed at d80 and are therefore still young. Due to the presence of an X-zone in all our experimental cohorts in addition to the downregulation of Prkar1, (Fig. 7d), we aged a cohort of Bl6 castrated, Ad-ARKO and Ad-ARKO castrated mice to 12 months (m). This is to determine if we observe a similar phenotype or additional disruption to the adrenal cortex following the prolonged loss of AR or circulating androgens.
Adrenal weight was unchanged in Bl6 castrated and Ad-ARKO castrated mice following the prolonged loss of circulating androgens, but a significant increase in adrenal weight is observed in 12 m Ad-ARKO mice compared to d80 Ad-ARKO mice (Fig. 8a). Consistent with this, analysis of adrenal morphology revealed no obvious visual difference in structure in 12 m WT controls when compared to d80 WT controls (Fig. 8b). Prolonged loss of circulating androgens in 12 m Bl6 castrated mice also show no major disruption to the adrenal cortex compared to d80 Bl6 castrated mice (Fig. 8b). Likewise, analysis of 12 m Ad-ARKO castrated mice show no disruption to the ZG and ZF regions of the adrenal cortex compared to d80 Ad-ARKO castrated mice (Fig. 8b). In addition, the X-zone in both these cohorts is significantly smaller than at d80 and is visibly breaking down (Fig. 8c). This phenotype is observed in aged virgin female mice, with eventual vacuolization of the X-zone41.
Aged Ad-ARKO mice display large cell clusters in capsule and large eosinophilic cells. (a) Adrenal weight analysis shows a significant increase in 12 m Ad-ARKO mice compared to d80 Ad-ARKO mice (two-way ANOVA; n = 5–8 ***p < 0.0001, Tukey’s post-hoc analysis, error bars SEM), with no weight changes observed in any other cohort. (b) Morphology analysis at 12 m reveals that cohorts with no circulating androgens have no major cortex disruption, and no visible X-zone regression. 12 m Ad-ARKO mice have severe cortex disruption, with presence of large spindle cell lesions and enlarged X-zone. (c) Measurement of X-zone depth show a significant increase in 12 m Ad-ARKO mice compared to d80 Ad-ARKO mice (two-way ANOVA; n = 5–8 ****p < 0.0001, Tukey’s post-hoc analysis, error bars SEM). In contrast, 12 m Ad-ARKO castrated mice show a significant decrease in X-Zone depth when compared to d80 Ad-ARKO mice (two-way ANOVA; n = 5–8 ****p < 0.0001, Tukey’s post-hoc analysis, error bars SEM). (d) Circulating corticosterone analysis shows 12 m Ad-ARKO mice have no changes in corticosterone compared to 12 m WT controls. M = Medulla, X = X-zone, ZF = Zona fasciculata, ZG = Zona glomerulosa. Scale bars 50 µm.
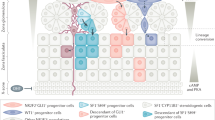
In accordance with the increase in adrenal weight, severe cortex disruption is observed in 12 m Ad-ARKO animals compared to d80 Ad-ARKO mice (Fig. 8b). Large spindle cell lesions can be observed in the adrenal capsule, that extend down into the ZF. Additionally, these mice have an X-zone that is significantly larger than the X-zone that is observed in d80 Ad-ARKO mice (Fig. 8c). Consistent with d80 cohorts, no changes in corticosterone are observed in aged cohorts compared to controls (Fig. 8d). Together these data show that, whilst chronic loss of androgens does not exacerbate the phenotype established earlier in life, continued AR signalling is essential to prevent age-related degeneration of the adrenal cortex associated with further X-zone expansion and the development of spindle cell lesions. A summary diagram highlights these findings and the differences observed between androgen and androgen receptor loss in the adrenal cortex (Fig. 9a,b).
Diagram explaining the role of androgen receptor in the male adrenal cortex. (a) Summary of the differences described following loss of androgens or androgen receptor over the key time-points investigated in this study. Our data demonstrates over time, the loss of AR but not androgens results in spindle cell formation and X-zone expansion. (b) Diagram describing the role of androgens in X-zone cells. Androgens binding to AR promote X-zone regression and normal adrenal zonation in WT male mice. GDX results in the development of an X-zone with regression in aged male mice, phenocopying what is observed in the aging female. Loss of AR but not androgens results in adrenal degeneration in ageing male mice with aberrant AR independent androgen signalling driving X-zone expansion and differentiation.
Discussion
To examine the role of androgen action in the adrenal, we utilised a novel mouse model with a specific ablation of androgen receptor in the adrenal cortex compounded with additional reduction of circulating androgen levels by castration. Our results describe AR expression in the human and mouse adrenal suggesting the mouse has utility as a model system with which to investigate androgen signalling in the adrenal cortex. AR ablation does not disrupt the formation of the definitive cortex and does not result in any adverse sexual or behavioural phenotypes, however, androgen signalling via AR is required for X-zone regression in males during puberty. Cortex measurements defined differences in X-zone morphology depending on whether circulating androgens or adrenal cortex AR have been targeted, suggesting the presence of a more complex signalling network linked to androgens. Prolonged loss of circulating androgens in aged Bl6 castrated and Ad-ARKO castrated revealed X-zone regression, in a manner that phenocopies previous observations in ageing female adrenals41. However, aged males with AR ablation alone revealed severe cortex disruption, spindle cell hyperplasia and X-zone expansion. The data described herein demonstrates AR-signalling is integral for adrenal cortex function throughout life.
The current paradigm regarding X-zone regression suggests that the surge in testosterone at puberty drives X-zone involution42. However, our investigation of morphology and 20 alpha-HSD expression in Ad-ARKO mice adrenals demonstrates that X-zone cells are already more developed in size and abundance compared to controls at d12, d21 and d35. This tells us, contrary to the literature, that the negative regulation of the X-zone by androgens or androgen receptor is occurring prior to puberty. Although not the focus of the study, Hershkovitz et al. noted a decrease in adrenal 20 alpha-HSD activity prior to the increase in testosterone that occurs during puberty in male mice28. This fits with our hypothesis that androgen signalling is regulating X-zone cells prior to the peak in testosterone. However, due to the minimal amount of circulating androgens at this time point, it would appear that AR is able to regulate the X-zone with low levels of circulating androgens or independently of androgens during adrenal postnatal development. In recent years, there has been a drive to identify the molecular mechanisms that govern the switch between fetal/adult adrenal cells and the pathways involved in adrenal cortex remodelling. Zubair et al. demonstrated via lineage tracing studies that AD4BP/SF-1 (64) is essential for adrenal formation, confirming that understanding the mechanisms that control the X-zone is essential to understanding adrenal regulation. Furthermore, they hypothesised that there is still an unidentified adult adrenal enhancer that activates during a key developmental stage to switch development from fetal to adult cells. The challenge surrounding understanding X-zone control is undoubtedly due to a number of genes identified as potential regulators. A study conducted by Sahut-Bernola et al. showed that the X-zone remains when Prkar1a is ablated from the adrenal cortex36. Consistent with their model, we note that Ad-ARKO mice also have X-zone maintenance that expands through the cortex with age and development of lesions in the outer cortex. However, we do not see the development of Cushing’s syndrome nor the switching on of Cyp17a1 in the adrenal cortex. Interestingly, we do note a significant downregulation in the transcript of Prkar1a. This suggests a relationship between AR and Protein Kinase A (PKA)43. The same group has recently extended these studies to look at castration and DHT treatment in their Prkar1a ablation models and found that androgen signalling is able to inhibit the PKA pathway via the RSPO/WNT/β-catenin pathway in the adrenal44.
Ablation of Dax1 in the adrenal cortex also results in maintenance of the X-zone34. It was for this reason that Dax1 was thought to control the switch between fetal and adult cells. With a similar phenotype being observed in Ad-ARKO mice, demonstrates that the switch from adult to fetal cells is a complex mechanism and that Dax1 could be involved in the same pathway as androgens and PKA to drive adult cortex cell differentiation and X-zone regression. Additionally, Dax1 ablation results in eventual adrenal failure as the pool of adrenocortical progenitor cells cannot be replenished. This is not something that is observed in our Ad-ARKO or castration models suggesting that AR does not regulate definitive cortex differentiation. However, unlike the Dax1 ablation model, our Ad-AKRO model does not target AR in the adrenal capsule22, which is essential for coordination of ZG to ZF transition and maintaining the pool of progenitor cells45,46, so the authors cannot comment on the rolf of AR in this cell population.
A significant upregulation in Sf1 transcript in all experimental cohorts was also observed. It has previously been shown that androgens act as a repressor of Sf1 (52), an important mechanism to regulate Sf1 and its target genes (52). Sustained elevated expression of Sf1 has been implicated in conditions such as childhood adrenocortical tumours (53). Whilst it is speculation at this stage, our data imply that perturbed androgen signalling could be a contributory factor in Sf1-associated adrenal disease, this requires further investigation. To determine the exact nature of the relationship between these signalling pathways, it would be pertinent to look at the androgen response elements in the promoter regions of these genes to determine if AR is directly upstream or if the changes observed are an off-target effect caused by general disruption to the adrenal cortex. The genes investigated in this study following AR ablation are by no means an exhaustive list of known cortex and X-zone regulators. We have in the first instance, focused on a sub set of key regulators, however, following the results of this study and demonstrating the importance of AR in the adrenal, it would be essential to investigate other known regulators. There is avenue for future research into the role of AR and their interactions with TRβ147 shown to be important in X-zone maintenance but not development, and activin, shown to promote X-zone apoptosis48,49. Further study would also seek to examine cohorts castrated at additional time points. This study examined absence of circulating androgens from the point of castration onwards in acute (14 days) and chronic (6 months) androgen loss, post puberty. A potential caveat of this is that there is still the potential for stimuli from steroid hormones. This has been shown to occur through memorized histone modification and DNA methylation50,51. This may be particularly pertinent for long terms castrated mice that will have had circulating androgens for 6 months. Future work would seek to perform castration before the onset of puberty to determine is this could be a potential confounder.
The maintenance of the X-zone in adulthood in Ad-ARKO mice brings into question cell clearance from the adrenal cortex. Under normal conditions adrenocortical cells migrate towards the cortex-medulla boundary and undergo apoptosis48. Protein localisation of Cleaved caspase 3 showed no apoptotic cells in BL/6 castrated or Ad-ARKO mice, suggesting androgen signalling is important for cell clearance from the adrenal through apoptosis. This phenotype has been documented previously in a global AR knockout model, however, this was thought to be a result of the loss of AR signalling from the pituitary21, our results show that this is a within-adrenal role for androgen-signalling.
Sahut-Bernola et al. described an increase in severity in adrenal cortex disruption with age in Prkar1a knockout mice, showing X-zone expansion and the development of primary pigmented adrenocortical disease (PPNAD) with age36. Due to the overlapping phenotype, we hypothesised that the severity of the phenotype in our androgen manipulation models would progress with age. Again, we noted a disparity between our models depending on whether AR or androgens have been targeted. Both castrated cohorts show no major adverse phenotypes, there is no increase in corticosterone, cortex disruption or X-zone expansion. X-zone measurements show X-zone regression, phenocopying what is observed in an ageing female, this phenotype is well described in the literature41,42,52,53,54. Conversely, the Ad-ARKO shows X-zone expansion and spindle cell hyperplasia. This result is of particular interest as it demonstrates that AR but not androgens are needed to protect against age-related degeneration of the cortex. Furthermore, that androgens are potentially still able to stimulate the adrenal in Ad-ARKO mice and without the presence of AR to bind to, could result in the aberrant stimulation of off target pathways. AKR1B7 and 3βHSD staining and X-zone measurements taken in our d80 cohorts further strengthen this. Measurements of the X-zone demonstrated significant morphological and size differenced depending on whether, androgens or AR has been targeted. Furthermore, AKR1B7 localisation is still observed in Ad-ARKO mice compared to castrated cohorts with no AKR1B7 expression. Additionally, 3βHSD showed localisation in Ad-ARKO adrenals but not in either castrated cohorts. This suggests that again, without the presence of AR to bind to, there is activation of off target signalling pathways in the adrenal cortex that requires further investigation.
The presence of AR in both human and mouse adrenal suggests that the mouse could provide a suitable model to investigate human conditions, however, due to the differences in localisation of adrenal AR in the human and rodent this could potentially suggest that although present in both, could have varying roles. This would need to be taken into consideration in future studies regarding adrenal androgen signalling and would be an avenue for future research.
In conclusion, this study not only highlights many new roles for androgen signalling in the adrenal but shows that the mouse has utility as a model to explore androgen action within the adrenal, opening up a novel entry point towards further increasing our understanding of adrenal function. Through cortex measurements, we demonstrate androgens and AR can act independently of each other and show that AR in mouse and human display similar spatiotemporal expression. Furthermore, we demonstrate that androgens act via AR to regress the X-zone and influence both cortical cell differentiation and apoptosis. We highlight that AR is potentially upstream of key adrenal-developmental genes but is dispensable in the formation of the definitive cortex. Finally, we demonstrate that androgens acting via AR protects against age-related degeneration of the adrenal cortex, with implications for our understanding in preventing adrenal degeneration and tumour development.
Methods
Ethics statement
All mice used in experiments were under a strict standard of care and experimental planning covered by licensed approval from the UK Home Office (License Number 80/7704) and adhere to the ARRIVE (Animal Research: Reporting of In Vivo Experiments) guidelines55. Ethical approval was obtained for the use of archived human fetal adrenal tissue from the East Scotland Research Ethics Committee (Reference Number: LREC08/S1101/1). Ethical approval was obtained for the use of archived human adult adrenal tissue from the Danish regional ethics committee (Reference Number: H-1-2012-007).
Targeted ablation of AR from the adrenal cortex using Cyp11a1-GC Cre
To specifically ablate AR from the adrenal cortex, Cre/loxP technology was used. Male C57BL/6 mice carrying a random insertion of the Cyp11a1-GC Cre22 were mated to C57BL/6 female mice homozygous for floxed AR56. Male offspring were either Cyp11a1+/GC; ARfl/y mice with adrenal androgen receptor ablation termed ‘Ad-ARKO’ or Cyp11a1+/+; ARfl/y ‘control’ littermates.
PCR genotyping of mice
Mice were genotyped for the inheritance of Cre recombinase as previously described57. PCR amplification products were resolved using the QIAxcel capillary system (QIAGEN, Crawley, United Kingdom). An amplicon of 102 bp indicated the inheritance of the Cre recombinase transgene.
Removal of circulating androgen through castration
Isoflurane was administered via inhalation. A single 1 cm incision was made into the scrotum and testes exposed and removed. Following removal of testes, the site of incision was closed with sterile sutures. Mice were injected subcutaneously with Buprenorphine 0.05 mg/kg, whilst anaesthetized, and allowed to recover whilst being monitored. Mice were closely monitored over 24 hours for any welfare problems, and twice daily from then onwards. At the end of the experiment, mice were culled by inhalation of CO2 until unconscious, followed by cervical dislocation. These animals were termed ‘BL6 castrated’ and ‘Ad-ARKO castrated’.
Two castration time points are used in this study, short term and long term. Short-term castrations were performed on postnatal day 64, allowed to age for 14 days and collected at postnatal day 80. Long-term castrations were performed on 6-month-old mice, left to age another 6 months and collected at 12 months old.
Tissue collection and processing
Body weight was measured, and adrenals were removed and weighed. Reproductive organs were also examined, removed and weighed. Tissues were fixed in Bouin’s fixative (Clin-Tech, Guildford, UK) for 4 hours (adrenals). Bouin’s-fixed tissues were processed and embedded in paraffin wax, and 5 µm sections were used for histological analysis. Sections of adrenals were stained with haematoxylin and eosin using standard protocols and examined for histological abnormalities.
Immunohistochemistry
Immunolocalization was performed either by a single antibody colourimetric (DAB) immunostaining method, as described previously58 a single or double antibody tyramide fluorescent immunostaining method, as described previously22,59, or automated Bond immunostaining method, as described previously58. Exceptions to this protocol are the H2O2 concentration washes performed at 3% H2O2 TBS. Antibodies used are listed in Table 1. A minimum of five individual sections for each age and genotype were immunostained in each experiment.
Quantitative RT-PCR
RNA was obtained from frozen adrenals from n = 8 d80 BL6 castrated, n = 8 Ad-ARKO, n = 8 Ad-ARKO castrated and n = 8 control mice, using the RNeasy Mini extraction kit with RNase-free DNase on the column digestion kit (Qiagen, Crawley, UK) according to the manufacturer’s protocol. RNA yield was quantified using a NanoDrop 1000 spectrophotometer (Thermo Fisher Scientific, Waltham, MA, USA). Random hexamer primed cDNA was prepared using the SuperScript VILO cDNA synthesis kit (Life Technologies) according to manufacturers’ protocols. Quantitative PCR was performed on d80 BL6 castrated, Ad-ARKO, Ad-ARKO castrated and control adrenals for the genes of interest listed in Table 2 using an ABI Prism 7900 Sequence Detection System (Applied Biosystems) and the Roche Universal Probe Library (Roche, Welwyn, UK). The expression of each gene was related to internal housekeeping gene assay Actb (Roche, Welwyn, UK).
Extraction of steroid hormones from plasma
Immediately after culling, blood was collected from mice via cardiac puncture with a syringe and needle, blood was collected in EDTA coated tubes to prevent coagulation. Mice were collected at 10:00 am following minimal handling. Handling, culling and blood collection was performed in under two minutes. Plasma was separated by centrifugation and stored at −80.
Quantification of hormone levels
Corticosterone in 12 m aged mice was measured using a mouse corticosterone ELISA kit (KO14-H5) according to manufacturer’s instructions. ACTH was measured using a mouse ACTH ELISA kit (ABIN415571) according to manufacturer’s instructions. All samples were run as a single assay for each hormone.
Serum analysis of d80 corticosterone and circulating androgens was achieved through the use of a new and sensitive isotope-dilution TurboFlow-LC-MS/MS method. Using this method, we are able to quantify androstenedione, testosterone, 17α-hydroxyprogesterone (17-OHP) progesterone, and corticosterone in human and mouse serum as previously described60, without modifications. However, since the steroid concentration in several of the mouse samples were higher than the normal analytical range for steroids in human serum, the linearity of calibration curves was investigated by preparing calibration materials in synthetic serum expanded in the high concentration area by including a total of 23 different dilutions of the standard stock solution. The linear range of calibration curves for regression analysis are shown in Supplementary Tables 1 and 2(A). All control material was based on different pools of human serum from children and adults, spiked in respectively low and high levels and not spiked serum pool. Samples were analyzed in 7 batches and each batch included standards for calibration curves, about 60 blind samples, one blank, three un-spiked serum pool samples, three pool controls spiked at respectively low and high levels. The inter-day variation, expressed as the relative standard deviation (RSD) was ≤8% for all analytes in both spike levels. The recovery was >89% for all analytes. Supplementary Tables 1 and 2(B) shows the limit of quantification60, the linear range for each individual calibration curves, and the inter-day validation. All chemical analyses were performed at the Dept. of Growth and Reproduction, Rigshospitalet, Copenhagen University Hospital.
Quantification of cortex zones
Comparison of adrenal cortex zones was performed by serially sectioning the whole adrenal at 5 µm, which produced on average 50 slides, per one adrenal, with one section per slide. To account for the shape of the adrenal and allow for consistent measurements, counts were performed on slides 15, 25 and 35 in Ad-ARKO and BL6 castrated animals. X-Zone depth was measured from the medulla boundary to the outer edge of the X-zone, with 5 measurements per slide, across sections 15, 25 and 35 in 5 castrated, 5 Ad-ARKO and 5 Ad-ARKO castrated samples. X-zone depth was measured by placing a 5 × 5 square grid over an ×40 magnification image of the X-zone. Five 2000 µm squares were chosen at random and cells within each box were counted across sections 15, 25 and 35 in 5 castrated, 5 Ad-ARKO and 5 Ad-ARKO castrated samples. Zona Fasciculata/Zona Glomerulosa (ZF/ZG) depth was measured from the X-zone boundary to the capsule, with 5 measurements per slide, across sections 15, 25 and 35 in 5 castrated, 5 Ad-ARKO and 5 Ad-ARKO castrated samples. Overall capsule depth was measured from the medulla boundary to the capsule, with 5 measurements per slide, across sections 15, 25 and 35 in 5 castrated, 5 Ad-ARKO and 5 Ad-ARKO castrated samples. All individual counts can be seen in Supplementary Fig. 4A–C.
Statistical analysis
Statistical analysis was performed using GraphPad Prism (version 7; GraphPad Software Inc., San Diego, CA, USA) using a two-tailed unpaired t-test (if comparing two groups), a one-way ANOVA with Tukey’s post-hoc test (if comparing multiple groups groups), or a two-way ANOVA with Tukey’s post-hoc test (if comparing multiple groups and variables) Values are expressed as means ± S.E.M.
Data Availability
All data generated as part of this study has been included in this manuscript in either the main body or in Supplementary Figures.
References
Laughlin, G. A., Barrett-Connor, E. & Bergstrom, J. Low serum testosterone and mortality in older men. The Journal of Clinical Endocrinology & Metabolism 93, 68–75 (2008).
Murashimaa, A., Kishigami, S., Thomsonc, A. & Yamadaa, G. Androgens and mammalian male reproductive tract development. Biochimica et Biophysica Acta (BBA) - Gene Regulatory Mechanisms (2014).
Isidori, A. M. et al. Leptin and androgens in male obesity: Evidence for leptin contribution to reduced androgen levels 1. The Journal of Clinical Endocrinology & Metabolism 84, 3673–3680 (1999).
Kupelian, V., Hayes, F. J., Link, C. L., Rosen, R. & McKinlay, J. B. Inverse association of testosterone and the metabolic syndrome in men is consistent across race and ethnic groups. The Journal of Clinical Endocrinology & Metabolism 93, 3403–3410 (2008).
Franchimont, P. Regulation of gonadal androgen secretion. Hormone Research in Paediatrics 18, 7–17 (1983).
Meikle, A., Daynes, R. & Araneo, B. Adrenal androgen secretion and biologic effects. Endocrinology and metabolism clinics of North America 20, 381–400 (1991).
Gottlieb, B., Lombroso, R., Beitel, L. K. & Trifiro, M. A. Molecular pathology of the androgen receptor in male (in) fertility. Reproductive biomedicine online 10, 42–48 (2005).
Foradori, C., Weiser, M. & Handa, R. Non-genomic actions of androgens. Frontiers in neuroendocrinology 29, 169–181 (2008).
Lois, K., Kassi, E., Prokopiou, M. & Chrousos, G. Adrenal Androgens and Aging (2000).
Bentvelsen, F., McPhaul, M., Wilson, C., Wilson, J. & George, F. Regulation of immunoreactive androgen receptor in the adrenal gland of the adult rat. Endocrinology 137, 2659–2663 (1996).
Sar, M., Lubahn, D. B., French, F. S. & Wilson, E. M. Immunohistochemical localization of the androgen receptor in rat and human tissues. Endocrinology 127, 3180–3186 (1990).
Simental, J. A., Sar, M., Lane, M. V., French, F. S. & Wilson, E. M. Transcriptional activation and nuclear targeting signals of the human androgen receptor. Journal of Biological Chemistry 266, 510–518 (1991).
Almeida, M. Q. et al. Increased expression of ACTH (MC2R) and androgen (AR) receptors in giant bilateral myelolipomas from patients with congenital adrenal hyperplasia. BMC endocrine disorders 14, 1 (2014).
Dunn, T. B. Normal and pathologic anatomy of the adrenal gland of the mouse, including neoplasms. Journal of the National Cancer Institute 44, 1323–1389 (1970).
Van Weerden, W., Bierings, H., Van Steenbrugge, G., De Jong, F. & Schröder, F. Adrenal glands of mouse and rat do not synthesize androgens. Life sciences 50, 857–861 (1992).
Lerario, A. M., Finco, I., LaPensee, C. & Hammer, G. D. Molecular Mechanisms of Stem/Progenitor Cell Maintenance in the Adrenal Cortex. Frontiers in Endocrinology 8 (2017).
Kim, A. C. et al. In search of adrenocortical stem and progenitor cells. Endocrine reviews 30, 241–263 (2009).
Ozisik, G., Achermann, J. C., Meeks, J. J. & Jameson, J. L. SF1 in the Development of the Adrenal Gland and Gonads. New Insights into Adrenal Pathophysiology (2003).
Lanman, J. T. The fetal zone of the adrenal gland: its developmental course, comparative anatomy, and possible physiologic functions. Medicine 32, 389–430 (1953).
Hirokawa, N. & Ishikawa, H. Electron microscopic observations on the castration-induced X zone in the adrenal cortex of male mice. Cell and tissue research 162, 119–130 (1975).
Miyamoto, J. et al. The pituitary function of androgen receptor constitutes a glucocorticoid production circuit. Molecular and cellular biology 27, 4807–4814 (2007).
O’Hara, L., York, J. P., Zhang, P. & Smith, L. B. Targeting of GFP-Cre to the mouse Cyp11a1 locus both drives cre recombinase expression in steroidogenic cells and permits generation of Cyp11a1 knock out mice. PloS one 9 (2014).
Crocoll, A., Zhu, C. C., Cato, A. C. & Blum, M. Expression of androgen receptor mRNA during mouse embryogenesis. Mechanisms of development 72, 175–178 (1998).
O’Hara, L. et al. Autocrine androgen action is essential for Leydig cell maturation and function, and protects against late-onset Leydig cell apoptosis in both mice and men. The FASEB Journal 29, 894–910 (2015).
Laufer, E., Kesper, D., Vortkamp, A. & King, P. Sonic hedgehog signaling during adrenal development. Molecular and cellular endocrinology 351, 19–27 (2012).
Rosol, T. J., Yarrington, J. T., Latendresse, J. & Capen, C. C. Adrenal gland: structure, function, and mechanisms of toxicity. Toxicologic pathology 29, 41–48 (2001).
Huang, C.-C. J., Kraft, C., Moy, N., Ng, L. & Forrest, D. A Novel Population of Inner Cortical Cells in the Adrenal Gland That Displays Sexually Dimorphic Expression of Thyroid Hormone Receptor-β1. Endocrinology 156, 2338–2348 (2015).
Hershkovitz, L., Beuschlein, F., Klammer, S., Krup, M. & Weinstein, Y. Adrenal 20α-hydroxysteroid dehydrogenase in the mouse catabolizes progesterone and 11-deoxycorticosterone and is restricted to the X-zone. Endocrinology 148, 976–988 (2007).
Benten, W. P. M. et al. Testosterone signaling through internalizable surface receptors in androgen receptor-free macrophages. Molecular Biology of the Cell 10, 3113–3123 (1999).
Heinlein, C. A. & Chang, C. Androgen receptor (AR) coregulators: an overview. Endocrine reviews 23, 175–200 (2002).
Koryakina, Y., Ta, H. Q. & Gioeli, D. Phosphorylation of the Androgen Receptor. Endocrine-related cancer 21, T131–T145, https://doi.org/10.1530/ERC-13-0472 (2014).
Xie, N. et al. The expression of glucocorticoid receptor is negatively regulated by active androgen receptor signaling in prostate tumors. International journal of cancer 136 (2015).
Lin, L. et al. Analysis of DAX1 (NR0B1) and steroidogenic factor-1 (NR5A1) in children and adults with primary adrenal failure: ten years’ experience. The Journal of Clinical Endocrinology & Metabolism 91, 3048–3054 (2006).
Scheys, J. O., Heaton, J. H. & Hammer, G. D. Evidence of adrenal failure in aging Dax1-deficient mice. Endocrinology 152, 3430–3439 (2011).
Ozisik, G., Achermann, J. C., Meeks, J. J. & Jameson, J. L. SF1 in the development of the adrenal gland and gonads. Hormone Research in Paediatrics 59, 94–98 (2003).
Sahut-Barnola, I. et al. Cushing’s Syndrome and Fetal Features Resurgence in Adrenal Cortex–Specific Prkar1a Knockout Mice. PLoS Genet 6, e1000980 (2010).
Gong, S. et al. Dynamics and correlation of serum cortisol and corticosterone under different physiological or stressful conditions in mice. PloS one 10, e0117503 (2015).
Belgardt, B. F. et al. PDK1 deficiency in POMC-expressing cells reveals FOXO1-dependent and-independent pathways in control of energy homeostasis and stress response. Cell metabolism 7, 291–301 (2008).
Sapolsky, R. M. & Meaney, M. J. Maturation of the adrenocortical stress response: neuroendocrine control mechanisms and the stress hyporesponsive period. Brain Research Reviews 11, 65–76 (1986).
Chang, S.-P. et al. Cell proliferation, movement and differentiation during maintenance of the adult mouse adrenal cortex. PloS one 8, e81865 (2013).
Holmes, P. & Dickson, A. X-zone degeneration in the adrenal glands of adult and immature female mice. Journal of anatomy 108, 159 (1971).
Siuda, S. The occurrence of X-zone in the adrenal glands of two rodent species. Acta Theriologica 18, 471–480 (1973).
Sarwar, M., Sandberg, S., Abrahamsson, P.-A. & Persson, J. L. In Urologic Oncology: Seminars and Original Investigations. 25, e21–25.e12 (Elsevier)(2017).
Dumontet, T. et al. PKA signaling drives reticularis differentiation and sexually dimorphic adrenal cortex renewal. JCI insight 3 (2018).
Pihlajoki, M., Dörner, J., Cochran, R. S., Heikinheimo, M. & Wilson, D. B. Adrenocortical zonation, renewal, and remodeling. Frontiers in endocrinology 6 (2015).
Pihlajoki, M., Heikinheimo, M. & Wilson, D. B. (Oxford University Press, 2013).
Huang, C.-C. J. & Forrest, D. In HPT Axis Biology and Thyroid Hormone Action SUN-0471-SUN-0471 (Endocrine Society, 2014).
Beuschlein, F. et al. Activin induces x-zone apoptosis that inhibits luteinizing hormone-dependent adrenocortical tumor formation in inhibin-deficient mice. Molecular and cellular biology 23, 3951–3964 (2003).
Hofland, J. & de Jong, F. H. Inhibins and activins: their roles in the adrenal gland and the development of adrenocortical tumors. Molecular and cellular endocrinology 359, 92–100 (2012).
Zhang, X. & Ho, S.-M. Epigenetics meets endocrinology. Journal of molecular endocrinology 46, R11–R32 (2011).
Prins, G. S. Estrogen imprinting: when your epigenetic memories come back to haunt you. Endocrinology 149, 5919–5921 (2008).
Beuschlein, F. et al. The adrenal X-zone is involved in progesterone inactivation. Experimental and Clinical Endocrinology & Diabetes 114, OR2_09 (2006).
Daughaday, W. A comparison of the X-zone of the adrenal cortex in two inbred strains of mice. Cancer research 1, 883–885 (1941).
Starkey, W. F. & Schmidt, E. C. Jr. The effect of testosterone-propionate on the x-zone of the mouse adrenal. Endocrinology 23, 339–344 (1938).
Kilkenny, C., Browne, W., Cuthill, I. C., Emerson, M. & Altman, D. G. Animal research: reporting in vivo experiments: the ARRIVE guidelines. British journal of pharmacology 160, 1577–1579 (2010).
De Gendt, K. et al. A Sertoli cell-selective knockout of the androgen receptor causes spermatogenic arrest in meiosis. Proceedings of the National Academy of Sciences of the United States of America 101, 1327–1332 (2004).
Welsh, M., Saunders, P. T., Atanassova, N., Sharpe, R. M. & Smith, L. B. Androgen action via testicular peritubular myoid cells is essential for male fertility. The FASEB Journal 23, 4218–4230 (2009).
O’Hara, L., Welsh, M., Saunders, P. T. & Smith, L. B. Androgen receptor expression in the caput epididymal epithelium is essential for development of the initial segment and epididymal spermatozoa transit. Endocrinology 152, 718–729 (2010).
O’Hara, L. & Smith, L. B. Androgen receptor signalling in Vascular Endothelial cells is dispensable for spermatogenesis and male fertility. BMC research notes 5, 16 (2012).
Søeborg, T., Frederiksen, H., Johannsen, T. H., Andersson, A.-M. & Juul, A. Isotope-dilution TurboFlow-LC-MS/MS method for simultaneous quantification of ten steroid metabolites in serum. Clinica Chimica Acta 468, 180–186 (2017).
Acknowledgements
We thank Nathan Jeffery, Mike Dodds, Will Mungal, Mike Millar, and Dr. Forbes Howie for technical support. This work was funded by a Medical Research Council Program Grant Award (MR/N002970/1) (to L.B.S.).
Author information
Authors and Affiliations
Contributions
Conceived and designed the study: A.L.G.; L.O.; L.B.S. Carried out experiments: A.L.G.; L.O.; S.S.; L.M. Analyzed the results: A.L.G.; L.O.; J.I.M.; L.B.S. Provided novel resources: R.T.M.; A.J.; H.F. Wrote the paper: A.L.G.; L.B.S.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Gannon, AL., O’Hara, L., Mason, J.I. et al. Androgen receptor signalling in the male adrenal facilitates X-zone regression, cell turnover and protects against adrenal degeneration during ageing. Sci Rep 9, 10457 (2019). https://doi.org/10.1038/s41598-019-46049-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-019-46049-3
This article is cited by
-
Conditional disruption of Nr5a1 directed by Sox9-Cre impairs adrenal development
Scientific Reports (2024)
-
Elevated luteinizing hormone receptor signaling or selenium treatment leads to comparable changes in adrenal cortex histology and androgen-AR/ZIP9 signaling
Protoplasma (2024)
-
Adrenal cortex renewal in health and disease
Nature Reviews Endocrinology (2021)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.