Abstract
Plasmodium transmission success depends upon the trade-off between the use of host resources to favour parasite reproduction and the negative effects on host health, which can be mediated by infection intensity. Despite its potential influence on parasite dynamics, the effects of infection intensity on both, birds and vectors, and on Plasmodium transmission success are still poorly understood. Here, we experimentally reduced the Plasmodium load in naturally infected wild house sparrows with the antimalarial primaquine to assess the effects of intensity of infection in the vertebrate hosts on Plasmodium transmission to and by mosquitoes. We monitored the survival of Culex pipiens mosquitoes throughout the development of the parasite and the infection status of the mosquitoes by analysing the head-thorax and saliva at 13 days post-exposure to birds. The proportion of mosquitoes infected by Plasmodium and the presence of Plasmodium in saliva were not associated with the medication treatment of birds. However, the experimental treatment affected vector survival with mosquitoes fed on medicated birds showing a higher survival rate than those fed on control individuals. These results provide strong experimental evidence of the impact of parasite load of vertebrate hosts on the survival probability of malaria vectors.
Similar content being viewed by others
Introduction
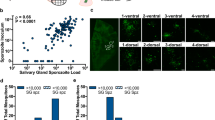
Parasites depend on their hosts to survive and to maximise their fitness1. Avian Plasmodium are vector-borne parasites that reproduce asexually in birds but requires mosquitoes to complete their sexual reproduction and development of sporozoites before being successfully transmitted. In mosquitoes, during sporogony, numerous sporozoites, i.e., parasite forms with elongated bodies, are formed in the oocyst. After maturation of the oocysts, the sporozoites move into the haemocoele and then penetrate the salivary glands of the vector. Transmission occurs when sporozoites, the infective forms of the parasites, are injected during a vector blood meal into the vertebrate hosts2. Thus, parasite sexual and asexual reproduction occur in two phylogenetically distant organisms and give rise to complex interactions between hosts, vectors, and parasites, while promoting constant coevolution between them3,4. In birds, Plasmodium infection is characterised by an acute phase, in which high parasite loads are reached soon after infection, followed by a chronic phase characterised by lower intensities that usually continue their course as lifelong infections5. Greater infection intensity has often been associated with a higher transmission rate6, but could reduce the transmission success of the parasite by killing either its vertebrate or invertebrate host6. Parasite virulence may thus be considered as a balance between increasing parasite transmission and reducing the costs imposed on their hosts1.
Different factors may influence the transmission success of vector-borne pathogens that cause major diseases, such as malaria, Lyme or bluetongue diseases7,8,9. Among them, the mosquito survival rate is particularly important10. Mosquitoes must be able to survive long enough for the Plasmodium sporozoites to develop (7–13 days2,11) to guarantee subsequent parasite transmission. Therefore, the lifespan of infected mosquitoes will have drastic consequences for the Plasmodium transmission success12,13. Avian malaria infections may impact the mosquito longevity14 (but see Pigeault and Villa15) and the development of parasites (i.e. mosquito latent period16). Although the impact of Plasmodium on the survival of birds has been experimentally demonstrated17,18, much less is known about the effects of infection on vector survival16. Mosquito survival may be reduced by Plasmodium due to tissue damage during the development and migration of parasites from the midgut to the salivary glands19 and the activation of a costly immune response against the infection20. However, positive14, negative21 and no effects15 of the infections by avian Plasmodium on mosquito survival have all been reported. The infection intensity in hosts may determine the successful development of the parasite in the mosquito22,23, although, in the case of Plasmodium falciparum, this relationship is not linear24. Likewise, a quadratic relation between parasitaemia in bird hosts and oocyst burden in mosquitoes has been found for the case of avian Plasmodium25.
Here, we used birds naturally infected by avian Plasmodium parasites to experimentally test the effect of the infection intensity of vertebrate hosts on mosquito survival, infection rate and Plasmodium transmission rate. Culex pipiens, the main vector of avian Plasmodium2,26, were allowed to bite Plasmodium-infected birds that had been either medicated with the antimalarial primaquine, which reduces infection intensity, or non-medicated control birds.
Results
The primaquine treatment significantly reduced the infection intensity in medicated birds compared to the controls (mean±SE control = 1.69 ± 0.26, medicated = 0.79 ± 0.23, F1,35 = 5.77, p = 0.02). Mosquitoes fed on birds infected by four different parasite lineages: Plasmodium relictum lineages SGS1 (18 birds) and GRW11 (3 birds), and the lineages PADOM02 (3 birds) and COLL1 (1 bird). The mosquitoes that fed on medicated birds (N = 102 mosquitoes) had a higher daily survival probability than those that fed on control birds (N = 95 mosquitoes) (daily survival probability = 0.99 and 0.96, respectively, Z = −3.17, p = 0.002; Table 1; Fig. 1). The presence of Plasmodium in the head-thoraxes of surviving mosquitoes was evaluated in 76 and 46 individuals that fed on medicated and control birds, respectively. Plasmodium was detected in 31 and 12 mosquitoes that had fed on medicated and control birds, respectively, and the presence of Plasmodium was screened in the saliva of these mosquitoes (Table 1). Overall, two out of 12 (16.67%) and 11 out of 31 (35.48%) head-thoraxes-positive mosquitoes were also positive in their saliva. The medication treatment did not affect the proportion of mosquitoes with Plasmodium-positive head-thorax (est = 0.89, Z = 0.92, p = 0.36, Table 1) or saliva (est = 1.31, Z = 1.66, p = 0.10, Table 1). Plasmodium lineages isolated from the head-thorax of mosquitoes and their saliva were identical. With the exception of the Plasmodium lineage COLL1, all Plasmodium lineages infecting house sparrows were isolated from mosquito saliva.
Discussion
The insect vector survival and infection rate may greatly affect the epidemiology of vector-borne parasites. Through an experimental manipulation of the infection intensity in wild birds, we assessed the impact of Plasmodium parasitaemia on mosquito survival, infection rate (i.e., presence of parasites in the head-thorax) and Plasmodium transmission rate (i.e., presence of parasites in the saliva). Medication reduced the infection intensity in birds, which in turn influenced mosquito survival, since higher Plasmodium intensities gave rise to greater mortality rates. Consequently, the mosquitoes that fed on medicated birds had a higher lifespan than those that fed on control birds. This result should be considered with caution as we estimated the survival of mosquitoes at only 13 days post-exposure and not along its complete lifetime. This period was selected based on the capacity of parasites to develop in mosquitoes between 7–13 days after infection2. The alternative interpretation that the greater survival rates in the mosquitoes that fed on medicated birds was in fact due to an effect of the drug itself on mosquito survival is poorly supported as the biological half-life of primaquine in plasma is 4–9 h27, and mosquitoes fed on birds 10 days after medication. Even if the drug had been active when ingested by the vectors, it could have not favoured mosquito survival28.
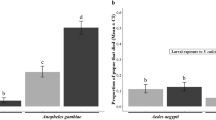
The costs of Plasmodium infection on mosquito survival are still a subject of intense debate19,29. Vézilier et al.14 reported increased longevity in Cx. pipiens infected by P. relictum; Pigeault and Villa15, by contrast, found that there were no effects on mosquito survival when using the same mosquito–parasite assemblage. However, these effects could be driven by the access to nutritional resources other than blood and the cost of Plasmodium infection on mosquito survival may only be detected in the event of nutritional stress21. The consumption of glucose has been found to be higher in infected mosquitoes than in uninfected ones30, which could be associated with the increased resources required by mosquitoes to fight off infections31. In addition, although Motta et al.32 did not find differences in the glucose concentration between Plasmodium infected and uninfected birds, avian malaria infection could affect the quality of the host blood through changes in the micronutrient composition and a decrease in red blood cell density. This potential decrease in host blood quality is expected to be a function of host parasitaemia33,34. Therefore, we cannot rule out the possibility that the observed lower survival rate of mosquitoes fed on control birds was due to the lower quality of these bloodmeals, and not exclusively to the costs of the parasite infections. However, since our mosquitoes were fed ad libitum with sugar solution after the bloodmeals, we suggest the lower survival of control mosquitoes was an effect of parasite infections and not due to the lower concentration of micronutrients in control birds’ blood. Parasites may impose additional costs on mosquitoes by producing tissue damage during their development, thereby increasing their susceptibility to bacterial infections and diseases35. An important factor likely affecting mosquito survival is the immune response of insects against parasite infection, which may also vary depending on the parasite species. For instance, Michel et al.36 found that the immune response of Anopheles gambiae performed differently against Plasmodium falciparum and P. berghei, which in turn affected the mosquito lifespan. The presence of four different Plasmodium lineages in our study could have potentially influenced our results on mosquito survival. This potential limitation is due to the fact that naturally infected birds were used in this experiment, thus providing an overview of the natural processes occurring in the wild. In fact, a diversity of parasite lineages circulate between birds and mosquitoes under natural conditions, with 12 different Plasmodium lineages infecting house sparrows in the study area37. Unfortunately, the sample size of individuals infected by each Plasmodium lineage was insufficient as to test for differences in the effect of the different parasite lineage on mosquito survival.
The infection intensity by Plasmodium might determine the success of parasite development in the insect vector and, consequently, its capacity for parasite transmission. In humans, the density of Plasmodium gametocytes has been found to be positively associated with the proportion of mosquitoes harbouring oocysts. However23, and in agreement with our findings, Pigeault et al.25 failed to find any association between avian Plasmodium infection intensity and the probability of mosquito infection. The absence of significant associations between the experimental reduction of Plasmodium infection intensity and the proportion of infected mosquitoes reported here could be due to the ability of Plasmodium to develop in mosquitoes that have fed on vertebrate hosts with infection intensities that are low or undetectable by microscopy24,38. This may also explain the absence of any significant effect of the reduction of infection intensity on the presence of Plasmodium in mosquito saliva 13 days after ingestion, a period which is enough for Plasmodium to reach the salivary glands2,26,39. However, the absence of significant differences could be due, at least in part, to the reduced sample size, as the prevalence was much higher in mosquitoes fed on control than on medicated birds (Table 1).
In wild bird populations, infections by avian Plasmodium usually pass through an acute phase of infection with high parasite loads followed by a chronic phase with low infection intensities5. Previous studies found that the prevalence of infection observed in mosquitoes fed on birds with acute infections was higher than in those mosquitoes fed on birds with chronic infections25,40. According to our results, and owing to the negative effects of high infection intensities on mosquito survival, Plasmodium transmission may be more effective during the chronic phase of infection than during the acute phase. Interestingly, Cornet et al.39 found that mosquitoes prefer biting avian hosts in a chronic phase of infection to biting uninfected birds or birds with infections in an acute phase, which is further support for how chronically infected birds affect the epidemiology of avian Plasmodium. Considering differences in host attraction by mosquitoes according to their infectious status and the impact on mosquito survival, as we did here, would provide a more realistic view of the epidemiology of avian malaria parasites in the wild.
Material and Methods
Mosquito collection and rearing
Culex pipiens larvae were collected in July 2014 in the natural reserve La Cañada de los Pájaros (Seville, Spain; 6°14′W, 36°57′N). Larvae were transferred to the laboratory and maintained in fresh water in plastic trays at uniform density, and fed ad libitum (Mikrozell 20 ml/22 g; Dohse Aquaristik GmbH & Co. KG, D-53501, Gelsdorf, Germany). Larvae and adult mosquitoes were maintained at 28 ± 1 °C, 65–70% relative humidity and 12:12 h light:dark cycle. Adult mosquitoes were anesthetised with ether, sexed and identified to species level under a stereo-microscope (Nikon SM7645) on chilled Petri dishes using morphological keys41. Female mosquitoes were placed in insect cages (BugDorm-43030F, 32.5 × 32.5 × 32.5 cm) and fed ad libitum with 1% sugar solution. Sugar solution was replaced with water 24 h prior to each experiment and the water was removed from the cages 12 hours before the experiment begins. The experiment was conducted using 7–15-days old female mosquitoes.
Bird trapping and sampling
Yearling house sparrows (Passer domesticus) were captured using mist nets in July 2014 (6°50′W, 37°18′N). Birds were individually ringed and blood was sampled (0.2 ml) from the jugular vein using sterile syringes to assess their Plasmodium infection status using molecular methods (see details below). Birds were transported to the laboratory in the Doñana Biological Station (EBD-CSIC) and kept in birdcages (58.5 × 25 × 36 cm) in a vector-free room under controlled conditions (22 ± 1 °C, 40–50% RH and 17:7 h light:dark cycle). Birds were housed for 24 days before the exposing to mosquitoes and were fed ad libitum with a standard mixed diet for seed-eating and insectivorous birds (KIKI, GZM S.L., Alicante, Spain). It was not possible to discriminate the stage of Plasmodium infection (i.e. acute or chronic stage) of the birds. However, avian malaria infections reached its maximum after 10–13 days, while the chronic phase start after 20–25 days post infection42. Birds in our study were captured and maintained in a vector-free environment during 24 days before exposing them to mosquitoes, thus infections are expected to be in a chronic stage.
Experimental procedure
The bird’ infection status was determined by the amplification and sequencing of a fragment of the parasite cytochrome b gene (see details below)43. Thirty-six house sparrows, naturally infected by Plasmodium, were randomly assigned to one of two experimental groups: medicated birds (the experimentally reduced infection intensity group, N = 17) or control birds (non-medicated group, N = 19). Medicated birds were injected subcutaneously with 0.1 mg of the antimalarial drug primaquine (Sigma, St. Louis, MO, USA) diluted in 0.1 ml saline solution while control birds were injected subcutaneously with the same volume of saline solution44. Primaquine was previously used to reduce the intensity of infection by avian malaria and malaria-like parasites in different bird species, including house sparrows17,45,46. In vertebrates, high doses of primaquine produces non-desirable side effects, such as gastrointestinal disturbances and the development of methaemoglobinaemia47. Thus, only a single and low–concentration dose of primaquine was administered to minimize these side effects. A single dose will clear most of the gametocytes within seven days after treatment, as reported in humans48. Ten days after the treatment, each bird was immobilized (using a cylinder of 1 × 1 cm mesh, allowing mosquitoes can bite through) and exposed individually to 80 unfed female Cx. pipiens in an insect cage (BugDorm-43030F 32.5 × 32.5 × 32.5 cm) for 30 minutes. Although previous studies allowed mosquitoes to fed on domestic birds during a longer period40, the duration of the exposure period was chosen to obtain a sufficient number of engorged mosquitoes while reducing stress levels experienced by wild birds, as those used in this study. Using this procedure, a mean of 8.5 mosquitoes fed on bird blood (range: 0 to 22 mosquitoes). This value is similar (mean = 14.2) to that obtained with Cx. pipiens allowed to feed on birds exposed overnight44.
Immediately after the trials, engorged mosquitoes fed on the same individual bird were captured and placed together in a single insect cage under the same standard conditions detailed above. Mosquitoes were fed ad libitum with 1% sugar solution. Mosquito survival was monitored every 12 h for 13 days post-exposure to allow for parasite development. At the end of this period, saliva from the surviving mosquitoes was obtained by introducing the mosquitoes’ proboscis into a 1 μl disposable capillary (Einmal-Kapillarpipetten, Hirschmann® Laborgeäte, Germany) with 1 μl of foetal bovine serum. One μl of 2% pilocarpine (Novartis 2012, Alcon Cusí S.A. Barcelona, Spain) was applied to the mosquito thorax to stimulate salivation. After 45 min, the medium containing the saliva was placed in 1.5 ml Eppendorf tubes with 10 μl of MQ water26. We chose the isolation of saliva over other conventional methods such as the analysis of mosquito salivary glands because it allows the use of molecular methods for parasite detection and it has been widely used in studies on the competence of mosquitoes to transmit pathogens, such as West Nile virus49, Dengue virus50, Zika virus51, human malaria parasites52 and avian malaria26. This method, however, required the mosquitoes to be alive, which implied stopping the monitoring of mosquito survival at 13 days post exposure. The alternative extraction of salivary glands may become difficult in dead mosquitoes because the tissues dry soon after death. Samples were kept at −80 °C until further molecular analyses.
One day after the trial, the birds’ blood was sampled again (0.2 ml) to confirm the blood parasite lineages infecting individuals at this stage. This procedure allowed us to identify any potential parasite lineage that was not detected during the first sampling. After sampling, a drop of blood was immediately smeared, air-dried, fixed in absolute methanol and stained with Giemsa for 45 min53. The intensity of infection by haemosporidian parasites was estimated as the percentage of infected red blood cells detected after scanning 10,000 erythrocytes from each blood smear at high magnification (x10,000). Birds were not blood-sampled immediately before or during the mosquito exposure period in order to reduce the stress caused by the blood extraction and mosquito bites. Birds were released after the completion of the experiments at the site of capture.
Molecular detection and identification of blood parasites
DNA was isolated from blood samples and the head-thorax of each mosquito using a semiautomatic procedure (MAXWELL® 16 LEV Blood DNA Kit)54. The Qiagen DNeasy® Kit Tissue and Blood (Qiagen, Hilden, Germany) was used to isolate DNA from mosquito saliva. Based on a previous study showing that saliva from uninfected mosquitoes tested negative26, we considered absence of Plasmodium DNA in the saliva of those mosquitoes with uninfected head-thoraxes. Therefore, we only analysed those saliva samples from mosquitoes with Plasmodium positive head-thoraxes. Plasmodium infections were recorded following Hellgren et al.43. The presence of amplicons was verified in 1.8% agarose gels and positive samples were sequenced using the Macrogen sequencing service (Macrogen Inc., Amsterdam, The Netherlands). Sequences were edited using the software Sequencher™ v 4.9 (Gene Codes Corp., © 1991–2009, Ann Arbor, MI 48108) and assigned to parasite lineages through blast comparison with those deposited in the GenBank (National Center for Biotechnology Information) and Malavi databases55.
Statistical analyses
An ANOVA test was used to assess differences in the Plasmodium infection intensity (log-transformed) between medicated and control birds. We fitted a Cox mixed-effect model by maximum likelihood to mosquito survival data (number of surviving mosquitoes /12-hours-period) to test the effect of counted the medication treatment on mosquito survival. The medication treatment was considered as a fixed factor, using censored survival data and bird identity as a random or ‘frailty’ effect. Two similar Generalized Mixed Linear Models (GLMMs) with binomial error and logit link function were performed in which the infection status by Plasmodium of the head-thorax or the saliva samples were included as the dependent variable, respectively. The medication treatment was included as a fixed factor and bird identity as a random term. Initially, 36 birds were included in the study comprising 17 medicated birds and 19 control birds. However, six of these birds, including two medicated birds and four controls, showed evidence of co-infections. To avoid any potential effect of parasite coinfection on mosquito survival56, those insects fed on co-infected birds (n = 51) were excluded from the analyses. Thus, the final sample size included 30 birds comprising 15 medicated birds and 15 controls. Mosquitoes fed on blood from all birds but two medicated and three control birds. Statistical analyses were performed in R software 3.2.5 (R Core Development Team, 2016) with the packages survival57 and lme458.
Ethics statements
All experiments involving animals adhered to the guidelines included in the Spanish Legislative Decree “Real Decreto 53/2013 de 1 de Febrero” on protection of animals used for experimentation and other scientific purposes, with the guidelines established by the European Community Council Directive n° 2010/63/UE on Laboratory Animal Protection. The project was approved by the Regional Authorities and the CSIC Ethics Committee (project code assigned by the CSIC Ethical Committee CEBA-EBD-12-40).
Data Availability
The data generated and/or analysed during the current study are available from the corresponding author on reasonable request. Supplementary material are included in the manuscript.
References
De Roode, J. C., Yates, A. J. & Altizer, S. Virulence-transmission trade-offs and population divergence in virulence in a naturally occurring butterfly parasite. Proc Natl Acad Sci USA 105, 7489–7494 (2008).
Valkiūnas, G. Avian malaria parasites and other haemosporidia (CRC Press, 2005)
Ewald, P. W. Host-parasite relations, vectors, and the evolution of disease severity. Annu Rev Ecol Evol Syst. 14, 465–485 (1983).
Cohuet, A., Harris, C., Robert, V. & Fontenille, D. Evolutionary forces on Anopheles: what makes a malaria vector? Trends Parasitol. 26, 130–136 (2010).
Asghar, M. et al. Primary peak and chronic malaria infection levels are correlated in experimentally infected great reed warblers. Parasitology. 139, 1246–1252 (2012).
Mackinnon, M. J. & Read, A. F. Genetic relationships between parasite virulence and transmission in the rodent malaria Plasmodium chabaudi. Evolution. 53, 689–703 (1999).
Parham, P. E. & Michael, E. Modeling the effects of weather and climate change on malaria transmission. Environ Health Perspect. 118, 620–626 (2010).
Hartemink, N. A., Randolph, S. E., Davis, S. A. & Heesterbeek, J. A. P. The basic reproduction number for complex disease systems: Defining R 0 for tick-borne infections. Am Nat. 171, 743–754 (2008).
Gubbins, S., Carpenter, S., Baylis, M., Wood, J. L. & Mellor, P. S. Assessing the risk of bluetongue to UK livestock: uncertainty and sensitivity analyses of a temperature-dependent model for the basic reproduction number. J R Soc Interface. 5, 363–371 (2008).
Macdonald, G. The measurement of malaria transmission. Proc R Soc Med. 48, 295–301 (1955).
Macdonald, G. The analysis of the sporozoite rate. Trop Dis Bull. 49, 569–586 (1952).
Smith, D. L. et al. Ross, Macdonald, and a theory for the dynamics and control of mosquito-transmitted pathogens. PLoS Pathog. 8, e1002588 (2012).
Garrett-Jones, C. & Grab, B. The assessment of insecticidal impact on the malaria mosquito’s vectorial capacity, from data on the proportion of parous females. Bull World Health Organ. 31, 71 (1964).
Vézilier, J., Nicot, A., Gandon, S. & Rivero, A. Plasmodium infection decreases fecundity and increases survival of mosquitoes. Proc Biol Sci. 279, 4033–4041 (2012).
Pigeault, R. & Villa, M. Long-term pathogenic response to Plasmodium relictum infection in Culex pipiens mosquito. PloS One. 13, e0192315 (2018).
Dawes, E. J., Zhuang, S., Sinden, R. E. & Basáñez, M. G. The temporal dynamics of Plasmodium density through the sporogonic cycle within Anopheles mosquitoes. Trans R Soc Trop Med Hyg. 103, 1197–1198 (2009).
Martínez-de la Puente, J. et al. The blood parasite Haemoproteus reduces survival in a wild bird: a medication experiment. Biol Lett. 6, 663–665 (2010).
Asghar, M. et al. Hidden costs of infection: chronic malaria accelerates telomere degradation and senescence in wild birds. Science. 347, 436–438 (2015).
Ferguson, H. M. & Read, A. F. Why is the effect of malaria parasites on mosquito survival still unresolved? Trends Parasitol. 18, 256–261 (2002).
Moret, Y. & Schmid-Hempel, P. Survival for immunity: the price of immune system activation for bumblebee workers. Science. 290, 1166–1168 (2000).
Lalubin, F., Deledevant, A., Glaizot, O. & Christe, P. Natural malaria infection reduces starvation resistance of nutritionally stressed mosquitoes. J Anim Ecol. 83, 850–857 (2014).
Griffin, J. T. et al. Reducing Plasmodium falciparum malaria transmission in Africa: a model-based evaluation of intervention strategies. PLoS Med. 7, e1000324 (2010).
Bousema, T. & Drakeley, C. Epidemiology and infectivity of Plasmodium falciparum and Plasmodium vivax gametocytes in relation to malaria control and elimination. Clin Microbiol Rev. 24, 377–410 (2011).
Churcher, T. S. et al. Predicting mosquito infection from Plasmodium falciparum gametocyte density and estimating the reservoir of infection. Elife. 2, e00626 (2013).
Pigeault, R. et al. Avian malaria: a new lease of life for an old experimental model to study the evolutionary ecology of Plasmodium. Philos Trans Biol Sci. 370, 20140300 (2015).
Gutiérrez-López, R. et al. Do mosquitoes transmit the avian malaria-like parasite Haemoproteus? An experimental test of vector competence using mosquito saliva. Parasit Vectors. 9, 609 (2016).
Baird, J. K. & Hoffman, S. L. Primaquine therapy for malaria. Clin Infect Dis. 39, 1336–1345 (2004).
Butcher, G. A. Antimalarial drugs and the mosquito transmission of Plasmodium. Int J Parasitol. 27, 975–987 (1997).
Martínez-de la Puente, J., Gutiérrez-López, R. & Figuerola, J. Do avian malaria parasites reduce vector longevity? Curr Opin Insect Sci. 28, 113–117 (2018).
Hurd, H., Taylor, P. J., Adams, D., Underhill, A. & Eggleston, P. Evaluating the costs of mosquito resistance to malaria parasites. Evolution. 59, 2560–2572 (2005).
Ahmed, A. M. & Hurd, H. Immune stimulation and malaria infection impose reproductive costs in Anopheles gambiae via follicular apoptosis. Microbes Infect. 8, 308–315 (2006).
Motta, R. O. C. et al. Does haemosporidian infection affect hematological and biochemical profiles of the endangered Black-fronted piping-guan (Aburria jacutinga)? PeerJ. 1, e45 (2013).
Palinauskas, V., Valkiūnas, G., Križanauskienė, A., Bensch, S. & Bolshakov, C. V. Plasmodium relictum (lineage P-SGS1): further observation of effects on experimentally infected passeriform birds, with remarks on treatment with Malarone™. Exp Parasitol. 123, 134–139 (2009).
Townsend, A. K., Wheeler, S. S., Freund, D., Sehgal, R. N. & Boyce, W. M. Links between blood parasites, blood chemistry, and the survival of nestling American Crows. Ecol Evol. 8, 8779–8790 (2018).
Vaughan, J. A. & Turell, M. J. Facilitation of Rift Valley fever virus transmission by Plasmodium berghei sporozoites in Anopheles stephensi mosquitoes. Am J. Trop Med Hyg. 55, 407–409 (1966).
Michel, K., Budd, A., Pinto, S., Gibson, T. J. & Kafatos, F. C. Anopheles gambiae SRPN2 facilitates midgut invasion by the malaria parasite Plasmodium berghei. EMBO Rep. 6, 891–897 (2005).
Ferraguti, M. et al. Ecological determinants of avian malaria infections: An integrative analysis at landscape, mosquito and vertebrate community levels. J Anim Ecol. 87, 727–740 (2018).
Lin, J. T., Saunders, D. L. & Meshnick, S. R. The role of submicroscopic parasitemia in malaria transmission: what is the evidence? Trends Parasitol. 30, 183–190 (2014).
LaPointe, D. A., Goff, M. L. & Atkinson, C. T. Thermal constraints to the sporogonic development and altitudinal distribution of avian malaria Plasmodium relictum in Hawaii. J Parasitol. 96, 318–324 (2010).
Cornet, S., Nicot, A., Rivero, A. & Gandon, S. Malaria infection increases bird attractiveness to uninfected mosquitoes. Ecol Lett. 16, 323–329 (2013).
Schaffner, E. et al. The mosquitoes of Europe: an identification and training programme. (IRD Editions, 2001).
Cornet, S., Nicot, A., Rivero, A. & Gandon, S. Evolution of plastic transmission strategies in avian malaria. PLoS Pathog 10, e1004308 (2014).
Hellgren, O., Waldenström, J. & Bensch, S. A new PCR assay for simultaneous studies of Leucocytozoon, Plasmodium, and Haemoproteus from avian blood. J Parasitol. 90, 797–802 (2004).
Yan, J. et al. Avian malaria infection intensity influences mosquito feeding patterns. Int J Parasitol. 48, 257–264 (2018).
Merino, S., Moreno, J., Sanz, J. J. & Arriero, E. Are avian blood parasites pathogenic in the wild? A medication experiment in blue tits (Parus caeruleus). Proc Biol Sci. 267, 2507–2510 (2000).
Garcia-Longoria, L., Møller, A. P., Balbontín, J., de Lope, F. & Marzal, A. Do malaria parasites manipulate the escape behaviour of their avian hosts? An experimental study. Parasitol Res. 114, 4493–4501 (2015).
Mayorga, P., Deharo, E., Puisieux, F. & Couarraze, G. Interpretation and prediction of plasma levels of primaquine following transdermal delivery in Swiss mice. Int J Pharm. 155, 99–107 (1997).
Burgess, R. W. & Bray, R. S. The effect of a single dose of primaquine on the gametocytes, gametogony and sporogony of Laverania falciparum. Bull World Health Organ. 24, 451–546 (1961).
Ebel, G. D., Rochlin, I., Longacker, J. & Kramer, L. D. Culex restuans (Diptera: Culicidae) relative abundance and vector competence for West Nile virus. J Med Entomol. 42, 838–843 (2005).
Schaffner, F., Vazeille, M., Kaufmann, C., Failloux, A. B. & Mathis, A. Vector competence of Aedes japonicus for chikungunya and dengue viruses. J Eur Mosq Control Assoc. 29, 141–142 (2011).
Gutiérrez-López, R. et al. Vector competence of Aedes caspius and Ae. albopictus Mosquitoes for Zika Virus, Spain. Emerg Infect Dis. 25, 346 (2019).
Brugman, V. A. et al. Detection of malaria sporozoites expelled during mosquito sugar feeding. Sci Rep. 8, 7545 (2018).
Gering, E. & Atkinson, C. T. A rapid method for counting nucleated erythrocytes on stained blood smears by digital image analysis. J Parasitol. 90, 879–881 (2004).
Gutiérrez-López, R., Martínez-de la Puente, J., Gangoso, L., Soriguer, R. C. & Figuerola, J. Comparison of manual and semi‐automatic DNA extraction protocols for the barcoding characterization of hematophagous louse flies (Diptera: Hippoboscidae). J Vector Ecol. 40, 11–15 (2015).
Bensch, S., Hellgren, O. & Pérez-Tris, J. MalAvi: a public database of malaria parasites and related haemosporidians in avian hosts based on mitochondrial cytochrome b lineages. Mol Ecol Resour. 9, 1353–1358 (2009).
Marzal, A., Bensch, S., Reviriego, M., Balbontin, J. & De Lope, F. Effects of malaria double infection in birds: one plus one is not two. J Evol Biol. 21, 979–987 (2008).
Fox, J. Cox proportional-hazards regression for survival data. An R and S-PLUS companion to applied regression, http://cran.r-project.org/doc/contrib/Fox-Companion/appendix-cox-regression.pdf (2002)
Bates, D., Maechler, M., Bolker, B. & Walker, S. Fitting Linear Mixed-Effects Models Using lme4. J. Stat Softw. 67, 1–48 (2015).
Acknowledgements
Special thanks to Alberto Pastoriza for his help during the fieldwork and with mosquito capture and identification, and to Isabel Martín and Laura Gómez for their help with the laboratory analyses. We thank Plácido and Maribel for allowing us to sample mosquitoes at “La Cañada de los Pájaros”. We would also like to thank anonymous reviewers for constructively revising this manuscript. This study was funded by projects CGL2012-30759, CGL2015-65055-P and PGC2018-095704-B-100 from the Spanish Ministry of Science and Innovation. R.G.L. was funded by a FPI grant (BES-2013-065274). J.M.P. was partially supported by a 2017 Leonardo Grant for Researchers and Cultural Creators, BBVA Foundation. The Foundation accepts no responsibility for the opinions, statements and contents included in the project and/or the results thereof, which are entirely the responsibility of the authors. L.G. was supported by a postdoctoral contract of project P11-RNM-7038 from the Junta de Andalucía and by a Marie Curie Fellowship of the European Commission (grant number 747729, “EcoEvoClim”). J.Y. was supported by the State Scholarship Found from the China Scholarship Council.
Author information
Authors and Affiliations
Contributions
R.G.L., J.M.P., L.G., R.S. and J.F. designed the study. R.G.L., J.M.P. and J.Y. conducted the experimental work. R.G.L. and J.M.P. performed the laboratory analysis. R.G.L., J.M.P., L.G., J.Y., R.S. and J.F. contributed in the redaction and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Gutiérrez-López, R., Martínez-de la Puente, J., Gangoso, L. et al. Experimental reduction of host Plasmodium infection load affects mosquito survival. Sci Rep 9, 8782 (2019). https://doi.org/10.1038/s41598-019-45143-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-019-45143-w
This article is cited by
-
Evaluation of sustainable susceptibility to Plasmodium vivax infection among colonized Anopheles darlingi and Anopheles deaneorum
Malaria Journal (2022)
-
Plasmodium relictum infection in Culex quinquefasciatus (Culicidae) decreases diel flight activity but increases peak dusk flight activity
Malaria Journal (2022)
-
Experiment in semi-natural conditions did not confirm the influence of malaria infection on bird attractiveness to mosquitoes
Parasites & Vectors (2022)
-
Culex quinquefasciatus (Diptera: Culicidae) survivorship following the ingestion of bird blood infected with Haemoproteus sp. parasites
Parasitology Research (2021)
-
From Africa to Europe: evidence of transmission of a tropical Plasmodium lineage in Spanish populations of house sparrows
Parasites & Vectors (2019)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.