Abstract
Overlap in morphologic features between malignant and benign myogenic tumors, such as leiomyosarcoma (LMS) vs. leiomyoma as well as rhabdomyosarcoma (RMS) vs. rhabdomyoma, often makes differential diagnosis difficult and challenging. Here the expressions of Enhancer of Zeste Homolog 2 (EZH2), Suppressor of Zeste 12 (SUZ12), retinoblastoma protein associated protein 46 (RbAp46), Embryonic Ectoderm Development (EED) and ki-67 protein were detected by immunohistochemistry to evaluate their values in differential diagnosis. The expression of EZH2 mRNA was investigated by analyzing the Gene Expression Omnibus Datasets. The results demonstrated that EZH2 protein was detected in 81.25% (26/32) of LMS and 70.58% (36/51) of RMS, whereas none of leiomyoma (n = 16), rhabdomyoma (n = 15) and normal tissues (n = 31) showed positive immunostaining (p < 0.05). EZH2 protein was found to have a sensitivity of 91.30% and specificity of 100% in distinguishing well-differentiated LMS from cellular leiomyoma, and a sensitivity of 92.86% and specificity of 100% in distinguishing well-differentiated embryonal rhabdomyosarcoma (ERMS) from fetal rhabdomyoma. Besides, the expression of EZH2 mRNA was higher in LMS and RMS than in benign tumors (p < 0.05). The expressions of SUZ12 and RbAp46 protein were higher in RMS than in rhabdomyoma (p < 0.05). Conclusively, the high expression of EZH2 is a promising marker in distinguishing well–differentiated LMS from cellular leiomyoma, or well–differentiated ERMS from fetal rhabdomyoma, and the upregulation of EZH2 protein expression may occur at transcriptional level.
Similar content being viewed by others
Introduction
Overlap in morphologic features between malignant and benign myogenic tumors, such as well-differentiated leiomyosarcoma (LMS) vs. cellular leiomyoma as well as well-differentiated rhabdomyosarcoma (RMS) vs. fetal rhabdomyoma, often makes differential diagnosis difficult and challenging. LMS mainly occurs in the pelvic retroperitoneum/abdomen of adults, with hypercellularity, nuclear atypia and active mitosis. However, well-differentiated LMS, with no excessive mitotic activity and undue nuclear atypia, often shows histological features similar to cellular leiomyoma. Cellular leiomyoma often shows the morphology features of increased cellularity, large tumor size and active mitotic activity. RMS is one of the most common sarcomas with high recurrence rates in infants and children. Embryonal rhabdomyosarcoma (ERMS) is a subtype of RMS. The well-differentiated ERMS is sometimes indistinguishable from fetal rhabdomyoma for lacks of cytologic atypia and active mitosis. Fetal rhabdomyoma is rare and often considered to be a mimic of well-differentiated ERMS. Immunohistochemical markers used for clinical diagnoses, such as MAS, vimentin, calponin, SMA and desmin, are not effective in differentiating these malignant tumors from benign tumors. To address this issue, highly sensitive and specific new markers are needed for differential diagnosis.
Enhancer of Zeste Homolog 2 (EZH2) is a key subunit of polycomb repressive complex 2 (PRC2) and represses its target genes by catalyzing histone methylation through the coordinate action of three other components of PRC2, including Suppressor of Zeste 12 (SUZ12), Embryonic Ectoderm Development (EED) and retinoblastoma protein associated protein 46 (RbAp46). Previous studies have reported that high expression of EZH2 was found in various kinds of cancers, which contributed to tumor progression and poor prognosis1,2,3,4,5,6,7,8,9. In recent years, upregulation of EZH2 expression was also discovered in certain sarcomas, including Ewing sarcoma, RMS, synovial sarcoma, osteosarcoma and chondrosarcoma. Ewing sarcoma and RMS are common pediatric sarcomas with high malignance. Ramaglia10 found that EZH2 was expressed with a different degree in 60% of 17 patients with Ewing sarcoma or RMS and it was significantly higher in patients presenting lymph node and/or distant metastases. Moreover, overexpression of EZH2 was positively relative to lower probability of survival. EZH2 expression can be induced by the fusion gene of EWS/FLI1 via binding to its promoter in Ewing sarcoma in vivo11. It was also demonstrated that EZH2 was aberrantly overexpressed in RMS primary tumors and cell lines, and downregulation of it in vitro can lead to muscle-like differentiation of RMS cells12,13,14. Some studies exist on synovial sarcoma revealed that EZH2 expressed in 76% of patients15. EZH2 mRNA and protein were highly expressed in poorly differentiated subtype. Even in the monophasic and biphasic subtypes, patients with high EZH2 score was characterized by high proliferation rate, large tumor size, distant metastasis and poor outcomes16. EZH2 overexpression was also detected in osteosarcoma17 and high grade chondrosarcomas18, which was significantly associated with aggressive behavior and poor prognosis. However, the expression of EZH2 in malignant myogenic tumors, such as LMS and RMS, remains unknown. Specifically, the difference of its expression in malignant and benign tumors has not been elucidated yet.
In this study, we detected the expression of EZH2 and three other components of PRC2 in 32 LMS, 51 RMS, 16 uterine leiomyoma, 15 rhabdomyoma as well as 31 normal tissues to evaluate the application value of EZH2 in differential diagnosis. In addition, the association between EZH2 expression and clinicopathological characteristics, and the correlation of EZH2 with ki-67 protein were assessed to identify the significance in these malignant tumors. We also investigated EZH2 mRNA expression by analyzing the Gene Expression Omnibus (GEO) Datasets.
Results
The EZH2 protein was highly expressed in LMS
In this study, immunohistochemical analysis was performed in 64 specimens, including 32 LMS, 16 uterine leiomyoma and 16 normal myometrial to quantify and localize the expression of EZH2 protein. Microscopy pictures showed nuclear localization of EHZ2 in LMS (Fig. 1).
EZH2 expression in LMS, uterine leiomyoma and normal myometrium. LMS (a, H&E staining) showed positive staining for EZH2 protein (b,c). Brown color in nuclei indicates strong positive staining. In contrast, uterine leiomyoma (d, H&E staining) and normal myometrium (g, H&E staining) exhibited negative staining (e,f: uterine leiomyoma; h,i: normal myometrium) (a,b, d,e and g,h, original magnification x100; c,f and i, original magnification x400).
Totally, EZH2 protein expression was observed in 26 of 32 (81.25%) LMS, whereas none was found in uterine leiomyoma and normal myometrium (p < 0.05, Table 1). Of 32 LMS cases, 4 were scored 0 (negative staining), 2 were scored 1 (weak staining not exceeding 24% of tumor cells), 13 were scored 2 (weak staining between 25% to 49%), 16 were scored 2+ (moderate to strong staining exceeding 50%, Supplementary Table 1). Further subgroup analysis showed that EZH2 expression was found in 21 of 23 (91.30%) well-differentiated and significancently higher than that in cellular uterine leiomyoma (p < 0.05) (Table 2). According to the tumor sites, LMS were divided into two groups: uterine LMS and extra-uterine LMS. No significant difference in EZH2 protein expression level was found between the two groups (Table 3 and Supplementary Table 2).
The EZH2 protein was highly expressed in RMS
In this study, the expression of EZH2 protein was measured in 81 cases, 51 from RMS and 15 from fetal rhabdomyoma, as well as in 15 specimens of tumor adjacent skeletal muscle (TASM). Microscopy pictures showed nuclear localization of EHZ2 in RMS (Fig. 2). EZH2 protein expression was detected in 36 of 51 (70.58%) RMS, but not in rhabdomyoma and TASM (p < 0.05, Table 4). Of 51 RMS cases, 10 were scored 0 (negative staining), 5 were scored 1 (weak staining not exceeding 24%), 12 were scored 2 (weak staining between 25% to 49%), 24 were scored 2+ (moderate to strong staining exceeding 50%, Supplementary Table 3). Subgroup analysis indicated that EZH2 protein was found in 26 of 28 (92.86%) of well-differentiated ERMS and significantly higher than that in fetal rhabdomyoma (p < 0.05, Table 5).
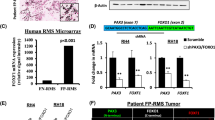
EZH2 expression in ERMS, fetal rhabdomyoma and TASM. ERMS (a, H&E staining) showed positive staining for EZH2 protein (b,c). Brown color in nuclei indicates strong positive staining. In contrast, fetal rhabdomyoma (d, H&E staining) and TASM (g, H&E staining) showed negative staining for EZH2 protein (e,f: fetal rhabdomyoma; h-i: TASM) (a,b, d,e and g,h, original magnification x100; c, f and i, original magnification x400, Scale bar,100 μm).
High expression levels of EZH2 mRNA in LMS
The data set GSE64763 (Fig. 3A) showed the relative expression levels of EZH2 mRNA in LMS (n = 25), uterine leiomyoma (n = 25) and normal myometrium (n = 28) were 1.56, 1.11 and 1, respectively. EZH2 mRNA expression in LMS were significantly higher than those in uterine leiomyoma and normal myometrium (p < 0.05).
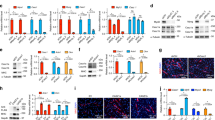
The expression of EZH2 mRNA in human LMS, uterine leiomyoma and myometrium is detected by bioinformatics analysis in GEO datasets. (A) The data set from GSE64763 shows the relative expression level of EZH2 mRNA in normal myometrium, uterine leiomyoma and LMS. (B) The data set from GSE764 shows the relative expression level of EZH2 mRNA in myometrium, uterine leiomyoma, uterine LMS and extra-uterine LMS. (C) The data set from GSE36610 shows the expression level of EZH2 mRNA in late secretory myometrium, proliferative myometrium and uterine LMS. (One-way ANOVA).
The data set GSE764 (Fig. 3B) showed the relative expression levels of EZH2 mRNA in uterine LMS (n = 9), extra-uterine LMS (n = 4), uterine leiomyoma (n = 9) and normal myometrium (n = 4) were 2.54, 5.15, 0.64 and 1, respectively. The expression of EZH2 mRNA in uterine and extra-uterine LMS were higher than those in uterine leiomyoma and normal myometrium (p < 0.05), respectively. And there was no difference in expression levels between uterine LMS and extra-uterine LMS.
As we known that the different stages of uterus depend on the changes of physiolgical characteristics of endometrium, not myometrium. In order to understand whether EZH2 mRNA expression in myometrium was affected by different statuses of endometrium, we investigated it in two phases of endometrium, including late secretory phase and proliferative phase. The data set GSE36610 (Fig. 3C) showed the relative expression levels of EZH2 mRNA in uterine LMS (n = 12), myometrium which adjacent endometrium was at the stage of proliferation (n = 5) and myometrium which adjacent endometrium was at the stage of late secretory (n = 5) were 1.36, 1.02 and 1, respectively. It was significantly higher in EZH2 mRNA expression level in uterine LMS than that in the two latter (p < 0.05). No difference was found between the two different stages of endometrium.
High expression levels of EZH2 mRNA in RMS
The data set from GSE28511 was utilized to analyze the relative expression levels of EZH2 mRNA in RMS, TASM and skeletal muscle. The result showed that the relative expression level of EZH2 mRNA in ERMS (n = 8), alveolar rhabdmyosarcoma (ARMS) (n = 10), TASM (n = 3) and normal skeletal muscle (n = 3) were 3.44, 2.55, 1.28 and 1, respectively. EZH2 mRNA expression in ERMS and ARMS were significantly higher than those in TASM and skeletal muscle, respectively (p < 0.05). And there were no significant differences in expression levels between ERMS and ARMS, or between TASM and skeletal muscle (Fig. 4).
Expression levels of EZH2 mRNA in other sarcomas at tissue and cellular levels
In order to know the difference in expression level of EZH2 mRNA between LMS and other sarcomas, we investigated EZH2 mRNA in 8 kinds of sarcoma tissues. The data set GDS2736 (Fig. 5A) showed the expression level of EZH2 mRNA in LMS (n = 6) was higher than that in well-differentiated liposarcoma (n = 3) (p < 0.05). And there was no significant difference in expression levels between LMS and synovial sarcoma (n = 16), myxoid liposarcoma (n = 19), dedifferentiated liposarcoma (n = 15), myxofibrosarcoma (n = 15), fibrosarcoma (n = 4), malignant peripheral nerve sheath tumor (MPNST, n = 3) and malignant fibrous histiocytoma (MFH, n = 21).The data set GSE71121 (Fig. 5B) revealed that the expression level of EZH2 mRNA in LMS (n = 90) was higher than that in differentiated liposarcoma (n = 44), undifferentiated sarcoma (n = 88) and other unclassified sarcoma (n = 45) (p < 0.05). And no significant difference was found between LMS and myxoid liposarcoma (n = 42).
The expression of EZH2 mRNA in LMS and other sarcomas at tissue level is detected by bioinformatics analysis in GEO datasets. (A) The data set from GDS2736 shows the expression level of EZH2 mRNA in LMS and 8 kinds of other sarcomas. (B) The data set from GSE71121 shows the expression level of EZH2 mRNA in LMS, myxofibrosarcoma, differenctiated liposarcoma and undifferentiated sarcoma and other types. (One-way ANOVA).
Additionally, EZH2 mRNA in cell lines of other sarcomas was also investigated. The data set GSE68591-3078349 (Fig. 6A) showed the expression level of EZH2 mRNA in LMS was significantly lower than Ewing’s sarcoma (p < 0.05). And there was no significant difference in expression levels between LMS and chondrosarcoma, fibrosarcoma, osteosarcoma, uterine sarcoma, synovial sarcoma, differentiated liposarcoma, MPNST and giant/spindle cell sarcoma. It also indicated that the expression level of EZH2 mRNA in RMS was lower than Ewing’s sarcoma (p < 0.05). And no significantly difference was found between RMS and the above nine kinds of cell lines of sarcomas. The data set GSE39262 (Fig. 6B) showed that the expression level of EZH2 mRNA in LMS was higher than that in osteosarcoma, fibrosarcom and Ewing sarcoma (p < 0.05). And there was no significant difference in expression level between LMS and chondrosarcoma, neuroblastoma and other six kinds of sarcoma (liposarcoma, MFH, malignant primitive neuroectodermal tumor, desmoplastic round cell tumor, poorly differentiated liposarcoma cell line and synovial sarcoma). It also revealed that the expression level of EZH2 mRNA in RMS was higher than that in osteosarcoma, chondrosarcoma and fibrosarcoma (p < 0.05). No significant difference was found between RMS and chondrosarcoma, neuroblastoma and the above six sarcomas.
The expression of EZH2 mRNA in LMS, RMS and other sarcomas at cellular level is detected by bioinformatics analysis in GEO datasets. (A) The data set from GSE68591-3078349 shows the expression level of EZH2 mRNA in LMS, RMS and 10 kinds of cell lines of other sarcomas. (B) The data set from GSE39262 shows the expression level of EZH2 mRNA in LMS, RMS and 12 kinds of cell lines of sarcomas.
The expression of EZH2 protein was highly sensitive and specific to LMS and RMS
Totally, EZH2 protein was found to have a sensitivity of 81.25% and specificity of 100% in distinguishing LMS from leiomyoma. Subgroup analysis showed the sensitivity and specificity of EZH2 protein were 91.30% and 100% in well-differentiated LMS. The accuracy is 96.36% in differentiating well-differentiated LMS from cellular leiomyoma.
The sensitively and specificity of RMS is 70.58% and 100% respectively. Further analysis revealed that EZH2 protein was found to have a sensitivity of 92.86% and specificity of 100% in well-differentiated ERMS. The accuracy of is 94.12% in differentiating well-differentiated ERMS from fetal rhabdomyoma (Table 6).
Association of EZH2 protein with clinicopathological features of LMSand RMS
The correlation between EZH2 protein expression in LMS and RMS and clinicopathological characteristics was analyzed (Table 7).
The age of patients with LMS ranged from 28 to 83 years, and the maximum diameter of tumors ranged from 3 to 15 cm. In 32 LMS cases, 14 (43.75%) patients developed the tumor in uterus and 18 (56.25%) in extra-uterus. 51 patients with RMS were also included in this study. The ages of patients ranged from 3 months to 66 years. As RMS usually occurs in infants and children, age of 18 was picked as an age cut off for RMS. The maximum diameter of the tumors ranged from 0.5 to 13 cm. No significant association was found between EZH2 expression and clinicopathological features of LMS and RMS, including gender, age, tumor size, tumors site and lymphatic metastasis.
In previous studies, EZH2 protein was highly expressed and significantly associated with overexpression of ki-67 protein in some solid tumors, such as breast cancer19,20 and gastric cancer21,22. To clarify the correlation between them in LMS and RMS, we further investigated the expression of ki-67 protein and no association was observed.
The expression of SUZ12, EED and RbAp46 in LMS and RMS
EZH2 is a methyltransferase that acts in coordination with three other components of PRC2, including SUZ12, RbAp46 and EED. In this study, we also investigated the expression of these proteins in LMS, RMS as well as benign tumors.
SUZ12 and EED protein were detected in 18 of 32 (56.25%) and 14 of 32 (43.75%) LMS, respectively, and they were lower than that in uterine leiomyoma (16/16,100%) and normal myometrium (16/16,100%) (p < 0.05). No difference of RbAp46 expression was found between LMS and leiomyoma.
SUZ12 and RbAp46 protein expression were observed in 37 of 51 (72.55%) and 35 of 51 (68.63%) RMS, respectively, and they were significantly higher than that in rhabdomyoma and TASM (p < 0.05). No significant difference in EED expression was found between RMS and rhabdomyoma (Table 8). The sensitivity and specificity of SUZ12, RbAp46 and EED in LMS and RMS was analyzed (Table 9).
Discussion
Generally, the main pathological criteria for differentiating malignant tumors from benign tumors include cytologic atypia, mitotic figures and necrosis. However, overlapping pathological features are frequently seen between malignant and benign myogenic tumors, which often make differential diagnosis difficult and challenging.
Well-differentiated LMS is sometimes indistinguishable from cellular leiomyoma for lacking of hypercellularity, active mitosis and excessive cytologic atypia. However, cellular leiomyoma in deep soft tissue is easily misdiagnosed with well-differentiated LMS for the similar histopathological characteristics. The present study demonstrated the utility of EZH2 immunohistochemistry for differentiating well-differentiated LMS from cellular leiomyoma. EZH2 protein was found to have a sensitivity of 81.25% and specificity of 100% in distinguishing LMS from leiomyoma. Further subgroup analysis showed that the sensitivity and specificity of EZH2 in well-differentiated LMS were 91.30% and 100%, respectively, which indicated that high expression of EZH2 is highly sensitive and specific to LMS, especially to well-differentiated LMS. The transcriptional level analysis showed that the expression of EZH2 mRNA in LMS is higher than that in leiomyoma and myometrium, which suggested that the upregulation of EZH2 expression in LMS may occur at the transcriptional level. RMS is a highly aggressive sarcoma with high recurrence rates in infants and children. ERMS, composed of primary-differentiated blastema cells and rhabdomyoblasts, often show similar pathological features to fetal rhabdomyoma. Fetal rhabdomyoma is rare and pathologists from basic hospitals do not have enough diagnostic experience, which may increase the risk of misdiagnosis. Under-treatment or over-treatment is unavoidable once misdiagnosis is made. In this study, EZH2 protein expression was detected in 70.58% of RMS, but none was found in rhabdomyoma and TASM. The subtype analysis showed the sensitivity and specificity of EZH2 protein in ERMS were 89.47% and 100%, respectively, which illustrated that EZH2 expression is highly sensitive and specific to ERMS and it can be utilized as a reliable marker for differentiating ERMS from rhabdomyoma. The transcriptional level analysis indicated that EZH2 mRNA expression in RMS was higher than that in TASM and skeletal muscle.
The mechanisms of high EZH2 protein expression in malignant tumors are mainly due to the overexpression of the oncogenes and down-regulation of the suppressors of EZH2. RAS/KARS mutation promotes the expression of EZH2 by activating the MEK-ERK-ELK1 and PI3K-AKT signaling pathways of pancreatic cancer and non-small cell lung cancer23,24. The Rb-E2F signaling pathway up-regulates EZH2 expression by binding to the promoter of EZH2 in bladder cancer and small cell lung cancer25,26. Similarly, the fusion gene EWS/Friend leukemia integration 1 transcription factor (FLI1) induced EZH2 expression by directly binding to its promotor in Ewing’s sarcoma cell lines11.When the expression levels of micro-RNAs, such as miRs-25, -26a, -101, -138 and -214, were decreased, the expression of EZH2 was increased by interacting directly with the 3′-UTR of EZH2 in malignant tumors27,28,29,30.
The associations between EZH2 expression and the clinicopathological features of LMS and RMS were analyzed. Contrary to previous studies19,20,21,22, we found no correlation between EZH2 and ki-67 proteins either in LMS or RMS. We do not know what the mechanism is, and it perhaps lacks the reaction sites in the signal pathway.
EZH2 can’t play the role as a methyltransferase without the synergistic action of SUZ12, RbAp46 and EED. Thus, we further investigated the expression of those three proteins both in malignant and benign tumors. SUZ12 and EED protein expression in LMS was deceased comparing with leiomyoma and myometrium. Recent studies reported that mutations of SUZ12 and EED had occurred in malignant peripheral nerve sheath tumors as well as head and neck high-grade malignant peripheral nerve sheath tumors had led to the loss of trimethylation at lysine 27 of histone H3 (H3K27me3), a downstream gene of EZH231,32. We plan to explore the mechanism of down-regulation of the expression of SUZ12 and EED in LMS. Moreover, the expression of SUZ12 and RbAp46 in RMS was higher than that in rhabdomyoma and TASM. The sensitivity of SUZ12 and RbAp46 in ERMS was 72.55% and 68.63%, respectively, and the specificity was 93.33% and 86.67% respectively, which illustrated that SUZ12 and RbAp46 were highly specific to RMS and they may become supplementary indicators together with EZH2 for differentiating RMS from rhabdomyoma.
In conclusion, EZH2 was highly expressed in LMS and RMS and it may be utilized as a new marker for differentiating well–differentiated LMS from cellular leiomyoma, or ERMS from rhabdomyoma. In addition, the upregulation of EZH2 protein expression in LMS and RMS may occur at transcriptional level. SUZ12 and RbAp46 may be used as supplementary indicators together with EZH2 for differentiating RMS from rhabdomyoma.
Materials and Methods
Patients and tissue samples
A total of 145 cases were collected from the Department of Pathology of Shanghai University of Medicine and Health Science. 32 LMS, 16 cellular and mitotically active uterine leiomyoma, 16 smooth muscle of myometrial, 51 RMS, 15 fetal rhabdomyoma (extracardiac) and 15 tumor-adjacent skeletal muscle (TASM) were selected and identified. Among 32 LMS cases, sites of involvement are as following: 6 were located in the retroperitoneum, 6 in the lower extremity, 2 in the orbit, 4 in the arteries, and 14 in the uterus. According to the degree of differentiation, LMS were divided into two subgroups: well-differentiated LMS (n = 23) and moderately-poorly differentiated LMS (n = 9). And the former were selected to compare with cellular leiomyoma at expression level of EZH2 protein.
Two histopathologic subtypes of RMS, including ERMS (n = 38) and ARMS (n = 13) were involved in this experiment. In group of ERMS, 28 cases of well-differentiated, 6 cases of moderately-differentiated and 4 cases of poorly-differentiated ERMS were included and the case of well-differentiated ERMS were selected to compare with fetal rhabdomyoma at the expression level of EZH2 protein. 12 cases of myxoid variant and 3 cases of intermediate form were included in the group of fetal rhabdomyoma.
Patients had given their written informed consent. Clinical information was collected from medical records. Then, the tissue microarrays, composed of core areas of 1.5-mm diameters taken from paraffin-embedded tissues using a Quick Ray Manual Tissue Microarrayer (UNITMA, Korea), were prepared by Wuhan Iwill Biological Technology Co., Ltd. The study was approved by the Ethics Committee of Shanghai University of Medicine and Health Sciences and experiments were performed in accordance with the relevant guideline and regulation of this committee.
Immunohistochemistry
Tissue microarrays of 4-μm thickness were deparaffinized, hydrated and rinsed in PBS. After antigen retrieval by exposure to microwaves for 10 minutes, peroxide blocking was performed with 3% H2O2 at room temperature for 30 minutes. The sections were blocked with goat serum and incubated with EZH2 antibody (1:200; catalog number: 5246, Cell Signaling Technology, MA, U.S.), SUZ12 antibody (1:100; catalog number: ab12073, Abcam, Cambridge, UK), RbAp46 antibody (1 µg/ml; catalog number: ab3535, Abcam, Cambridge,UK), EED antibody (1:200; catalog number: ab96801, Abcam, Cambridge, UK) and ki-67 antibody (1:400, catalog number: 12202, Cell Signaling Technology, MA, U.S.) at 4 °C overnight. Then, the samples were probed with biotinylated secondary antibody and high-sensitivity HRP-conjugated streptavidin (kit catalog number: 9710, Fuzhou Maixin Biotech, China) at room temperature for 20 minutes each. All slides were stained with 3, 30-diaminobenzidine and counterstained with hematoxylin. Colorectal cancer tissue was used as a positive control. A negative control for antibodies was carried out by replacing the primary antibody with PBS.
Evaluation of staining
The immunostained sections were evaluated by two independent pathologists and the expression of EZH2, SUZ12, EED, RbAp46 and ki-67 protein of each sample was scored according to the percentage of tumor cells with positive nuclear immunostaining and staining intensity. The score of each sample was the average score from the two observers’ evaluations. The percentage of positive tumor cells was scored as 0–4 (0 ≤ 10%, 1 = 10–24%, 2 = 25–49%, 3 = 50–74%, and 4 ≥ 75%), and the intensity of positive staining was quantified as 0–3(0 = negative, 1 = weak, 2 = moderate, and 3 = strong). The final score was obtained by multiplying these two scores. For statistical purposes, scores less than 2 were regarded as negative, and scores equal or more than 2 were considered to be positive.
GEO database analysis
The mRNA data sets of LMS, RMS, other sarcomas as well as benign myogenic tumors and normal controls were downloaded from Gene Expression Omnibus (GEO) Datasets (https://www.ncbi.nlm.nih.gov/gds/), which is a publicly available gene expression database. Three independent data sets from GSE64763, GSE764 and GSE36610 were utilized to analyze the relative expression levels of EZH2 mRNA in LMS, uterine leiomyoma and myometrium. One independent data set from GSE28511 was used to analyze the relative expression level of EZH2 mRNA inRMS, TASM and skeletal muscle. Two independent data sets from GDS2736 and GSE71121 were utilized to analyze the difference in expression level of EZH2 mRNA between LMS and other sarcomas in tissue level. And two data sets from GSE68591-3078349 and GSE39262 were used to analyze the difference in expression level of EZH2 mRNA between LMS, RMS and other sarcomas in cellular level.
Statistical analysis
All experimental data were analyzed by SPSS 19.0 statistical software (SPSS, Inc., Chicago, IL, USA). The expression difference of EZH2, SUZ12, RbAp46 and EED between malignant tumors and benign tumors, as well as the association between EZH2 expression and clinicopathological parameters, were investigated by Chi-square tests or Fisher’s exact tests. The analysis of expression of EZH2 mRNA in GEO datasets was performed by Student’s two tailed t test or one-way ANOVA. P < 0.05 was considered to be statistically significant for the analyses performed.
References
Varambally, S. et al. The polycomb group protein EZH2 is involved in progression of prostate cancer. Nature 419, 624–629 (2002).
Kleer, C. G. et al. EZH2 is a marker of aggressive breast cancer and promotes neoplastic transformation of breast epithelial cells. Proc. Natl. Acad. Sci. 100, 11606–11611 (2003).
Behrens, C. et al. EZH2 protein expression associates with the early pathogenesis, tumor progression, and prognosis of non-small cell lung carcinoma. Clin. Cancer Res. 19, 6556–6565 (2013).
Sato, T. et al. PRC2 overexpression and PRC2-target gene repression relating to poorer prognosis in small cell lung cancer. Sci. Rep. 3, 1911 (2013).
Matsukawa, Y. et al. Expression of the enhancer of zeste homolog 2 is correlated with poor prognosis in human gastric cancer. Cancer Sci. 97, 484–491 (2006).
Kondo, Y. et al. Alterations of DNA methylation and histone modifications contribute to gene silencing in hepatocellular carcinomas. Hepatol. Res. 37, 974–983 (2007).
Ougolkov, A. V., Bilim, V. N. & Billadeau, D. D. Regulation of pancreatic tumor cell proliferation and chemoresistance by the histone methyltransferase enhancer of zeste homologue 2. Clin. Cancer Res. 14, 6790–6796 (2008).
Wagener, N. et al. Enhancer of zestehomolog 2 (EZH2) expression is an independent prognostic factor in renal cell carcinoma. BMC Cancer 10, 524 (2010).
Takawa, M. et al. Validation of the histone methyltransferase EZH2 as a therapeutic target for various types of human cancer and as a prognostic marker. Cancer Sci. 102, 1298–1305 (2011).
Ramaglia, M. et al. High EZH2 expression is correlated to metastatic disease in pediatric soft tissue sarcomas. Cancer Cell Int. 16, 59–68 (2016).
Richter, G. et al. EZH2 is a mediator of EWS/FLI1 driven tumor growth and metastasis blocking endothelial and neuro-ectodermal differentiation. Proc. Natl. Acad. Sci. 106, 5324–5329 (2009).
Ciarapica, R. et al. ThePolycomb group (PcG) protein EZH2 supports the survival of PAX3-FOXO1 alveolar rhabdomyosarcoma by repressing FBXO32 (Atrogin1/MAFbx). Oncogene 33, 4173–4184 (2014).
Ciarapica, R. et al. Pharmacological inhibition of EZH2 as a promising differentiation therapy in embryonal RMS. BMC Cancer 14, 139 (2014).
Marchesi, I. et al. 12-O-tetradecanoylphorbol-13-acetate and EZH2 inhibition: A novel approach for promoting myogenic differentiation in embryonal rhabdomyosarcoma cells. J. Cell Physiol. 233, 2360–2365 (2018).
Shen, J. K. et al. Targeting EZH2-mediated methylation of H3K27 inhibits proliferation and migration of Synovial Sarcoma in vitro. Sci. Rep. 6, 25239 (2016).
Changchien, Y. C. et al. Poorly differentiated synovial sarcoma is associated with high expression of enhancer of zeste homologue2 (EZH2). J. Transl Med. 10, 216 (2012).
Ranran, S. et al. Overexpression of EZH2 is associated with the poor prognosis in osteosarcoma and function analysis indicates a therapeutic potential. Oncotarget 7, 38333–38346 (2016).
Girard, N. et al. 3-Deazaneplanocin A (DZNep), an inhibitor of the histone methyltransferase EZH2, induces apoptosis and reduces cell migration in chondrosarcoma cells. PLoS One 9, e98176 (2014).
Inari, H. et al. Expression of enhancer of zeste homolog 2 correlates with survival outcome in patients with metastatic breast cancer: exploratory study using primary and paired metastatic lesions. BMC Cancer 17, 160 (2017).
Jang, S. H. et al. High EZH2 Protein Expression Is Associated with Poor Overall Survival in Patients with Luminal A Breast Cancer. J. Breast Cancer 19, 53–60 (2016).
Mattioli, E. et al. Immunohistochemical analysis of pRb2/p130, VEGF, EZH2, p53, p16(INK4A), p27(KIP1), p21(WAF1), Ki-67 expression patterns in gastric cancer. J. Cell Physiol. 210, 183–191 (2007).
Choi, J. H. et al. Enhancer of zeste homolog 2 expression is associated with tumor cell proliferation and metastasis in gastric cancer. APMIS 118, 196–202 (2010).
Fujii, S. et al. RAS oncogenic signal upregulates EZH2 in pancreatic cancer. Biochem. Biophys. Res. Commun. 417, 1074–1079 (2012).
Riquelme, E. et al. Modulation of EZH2 Expression by MEK-ERK or PI3K-AKT Signaling in Lung Cancer Is Dictated by Different KRAS Oncogene Mutations. Cancer Res. 76, 675–685 (2016).
Santos, M. et al. In vivo disruption of an Rb-E2F-Ezh2 signaling loop causes bladder cancer. Cancer Res. 74, 6565–6577 (2014).
Coe, B. P. et al. Genomic deregulation of the E2F/Rb pathway leads to activation of the oncogene EZH2 in small cell lung cancer. PLoS One 8, e71670 (2013).
Völkel, P., Dupret, B., Le Bourhis, X. & Angrand, P. O. Diverse involvement of EZH2 in cancer epigenetics. Am. J. Transl. Res. 7, 175–193 (2015).
Chang, C. J. & Hung, M. C. The role of EZH2 in tumour progression. Br. J. Cancer 106, 243–247 (2012).
Zhu, Z. et al. MiR-138 Acts as a Tumor Suppressor by Targeting EZH2 and Enhances Cisplatin-Induced Apoptosis in Osteosarcoma Cells. PLoS One 11, e0150026 (2016).
Zhuang, C. et al. A double-negative feedback loop between EZH2 and miR-26a regulates tumor cell growth in hepatocellular carcinoma. Int. J. Oncol. 48, 1195–1204 (2016).
Cleven, A. H. et al. Loss of H3K27 tri-methylation is a diagnostic marker for malignant peripheral nerve sheath tumors and an indicator for an inferior survival. Mod Pathol. 29, 582–590 (2016).
Owosho, A.A. et al. A Clinicopathologic Study of Head and Neck Malignant Peripheral Nerve Sheath Tumors. Head Neck Pathol. https://doi.org/10.1007/s12105-017-0841-y (2017).
Acknowledgements
This work was supported by grant from the National Natural Science Foundation of China (No. 81602535; No. 81760223), by Shanghai Municipal Commission of Health and Family Planning (no. 201740161), by Science and Technology Commission of Shanghai Municipality (no. 15ZR1421800), and by Natural Science Foundation of Yunnan Province (No. FB2016121).
Author information
Authors and Affiliations
Contributions
Peng Huang and Ning Zhang conceived and designed this study; Zhi Zeng, Shaobo Li and Fei Wang conducted the study; Ning Zhang and Zhi Zeng analyzed data; Shaobo Li prepared figures; Ning Zhang drafted manuscript; Peng Huang and Ning Zhang edited and revised manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Zhang, N., Zeng, Z., Li, S. et al. High expression of EZH2 as a marker for the differential diagnosis of malignant and benign myogenic tumors. Sci Rep 8, 12331 (2018). https://doi.org/10.1038/s41598-018-30648-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-018-30648-7
This article is cited by
-
Differential Expression of EZH2 and H3K27me3 in Oral Verrucous Carcinoma and Oral Verrucous Hyperplasia
Head and Neck Pathology (2021)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.