Abstract
Magnesium has been shown to effectively prevent vascular calcification associated with chronic kidney disease. Magnesium has been hypothesized to prevent the upregulation of osteoblastic genes that potentially drives calcification. However, extracellular effects of magnesium on hydroxyapatite formation are largely neglected. This study investigated the effects of magnesium on intracellular changes associated with transdifferentiation and extracellular crystal formation. Bovine vascular smooth muscle cells were calcified using β-glycerophosphate. Transcriptional analysis, alkaline phosphatase activity and detection of apoptosis were used to identify transdifferentiation. Using X-ray diffraction and energy dispersive spectroscopy extracellular crystal composition was investigated. Magnesium prevented calcification in vascular smooth muscle cells. β-glycerophosphate increased expression of osteopontin but no other genes related to calcification. Alkaline phosphatase activity was stable and apoptosis was only detected after calcification independent of magnesium. Blocking of the magnesium channel TRPM7 using 2-APB did not abrogate the protective effects of magnesium. Magnesium prevented the formation of hydroxyapatite, which formed extensively during β-glycerophosphate treatment. Magnesium reduced calcium and phosphate fractions of 68% and 41% extracellular crystals, respectively, without affecting the fraction of magnesium. This study demonstrates that magnesium inhibits hydroxyapatite formation in the extracellular space, thereby preventing calcification of vascular smooth muscle cells.
Similar content being viewed by others
Introduction
Vascular calcifications are common in chronic kidney disease (CKD) and their presence is associated with increased cardiovascular mortality, which is the primary cause of death in CKD patients1. When glomerular filtration rate decreases, phosphate (Pi) levels rise and cause severely disturbed mineral and bone metabolism affecting vascular integrity and function2. Recently, several epidemiological studies showed a significant inverse relationship between serum magnesium (Mg2+) and survival in CKD patients3,4,5.
Mg2+ has been shown to effectively prevent mineralization in multiple experimental models of vascular calcification6,7,8,9,10,11,12,13. To date, experimental research has been focused on the role Mg2+ in the medial layer of the vessel wall, where vascular smooth muscle cells (VSMC) actively contribute to the calcification process. VSMCs transdifferentiate from contractile into osteoblast-like cells, which results in mineral deposition in the extracellular matrix, loss of contractile properties and apoptosis14. Typically, this process is characterized by the expression of genes normally restricted to bone tissue such as bone morphogenetic protein 2 (BMP2) and Runt-related transcription factor 2 (RUNX2) and increased alkaline phosphatase (ALP) activity15. Several studies suggest that Mg2+ directly prevents the upregulation of osteoblastic gene expression and thereby blocks VSMC transdifferentiation and subsequent mineralization6,7,8,11,16,17. However, extracellular inhibition of Mg2+ on calcium (Ca2+)-Pi particle formation, which is an important driving force for the onset of calcification, has largely been neglected18. Interestingly, it has been suggested that Ca2+-Pi nanocrystals, rather than Pi, may drive osteoblastic transdifferentation of VSMC19, illustrating the relevance of crystal inhibiting effects of Mg2+. Though poorly studied in detail in the context of VSMC calcification, the extracellular crystal inhibitory properties of Mg2+ are profound and well known in both biological and non-biological systems20,21,22.
This study aimed to investigate the effects of Mg2+ on both intracellular changes associated with vascular calcification and crystal formation in the extracellular space. Therefore, in addition to mapping the effects of Mg2+ on gene expression patterns associated with osteoblastic transdifferentiation in VSMC, we studied the effects of Mg2+ on the formation of crystals in the extracellular space by scanning electron microscopy and X-ray diffraction.
Materials and Methods
Cell culture and vascular smooth muscle cell identification
Bovine aortic VSMC (bVSMC) were set up from explant culture of bovine aortic segments according to standard protocols and cultured in M199 culture medium (Lonza, Basel, Switzerland) supplemented with 10% (v/v) fetal bovine serum (FBS, HyClone, GE Healthcare Life Sciences, Illinois, USA), ciprofloxacine (Fresenius Kabi, Zeist, The Netherlands) at 37 °C in a humidified incubator with 5% (v/v) CO2. Standard culture medium contained 0.8 mM MgSO4, 1.02 mM NaH2PO4 and 1.8 mM CaCl2. VSMC were not used beyond the 16th passage and VSMC identity was confirmed by α-smooth muscle actin (α-SMA) immunofluorescent stainings. α-SMA staining was performed on cells that were cultured on coverslips (18 mm in diameter) until 80% confluent. After fixation in 4% (w/v) paraformaldehyde and blocking with 16% (v/v) normal goat serum, the cells were stained overnight (4 °C) with a mouse monoclonal primary anti-α-SMA antibody diluted (1:400, A5228, Sigma, Missouri, USA) in a buffer containing phosphate buffered saline (PBS) and normal goat serum. Subsequently, cells were stained with a goat-anti mouse IgG Alexa 488 conjugated polyclonal antibody (1:250, A-11029, Invitrogen, Massachusetts, USA) and visualized using an Axio Imager M (Zeiss, Oberkochen, Germany).
Experimental design
For calcification, medium was supplemented with 5% (v/v) FBS and 10 mM β-glycerophosphate (BGP, Merck Millipore, Massachusetts, USA). BGP requires cellular activity for its cleavage to free Pi, and was chosen in this setup to increase the medium Pi concentration to minimize Mg2+-Pi interactions prior to cellular exposure. In the high Mg2+ treatment medium, MgCl2 (Merck Millipore) was supplemented to reach a final concentration of 2 mM MgCl2. At 80% confluence, cells grown in a 12-wells plate were incubated with designated media for 14 days, which was changed every 2–3 days.
TRPM7 inhibition by 2-APB
Transient receptor potential melastatin 7 (TRPM7) was inhibited by incubation with 10 μM of 2-Aminoethyl diphenylborinate (2-APB, Sigma). At 80% confluence, 2-APB was supplemented in combination with the different culture media as outlined in the previous section during 14 days in a 24-wells plate.
Pi concentration of the cell culture supernatant
Pi was measured in the cell culture supernatant (or culture medium) calorimetrically using the malachite green method as described elsewhere23. Briefly, a reaction mix consisting of molybdate and malachite green was added to the samples and standards and incubated for 30 minutes at room temperature. The absorbance was measured at 620 nm using a Benchmark Plus Microplate Spectrophotometer System (Bio-Rad, California, USA).
Quantification of Ca2+ deposition
Cells were decalcified with 0.1 M HCl for 5 minutes at room temperature with gentle rocking, which effectively dissolved all Ca2+ deposits present. The Ca2+ concentration in the supernatant was determined by the o-cresophthalein complexone method. o-cresophthalein color reagent (Sigma) was incubated with the samples and standards and the absorbance was measured immediately at 570 nm, as described previously24. Subsequently, the cells were neutralized in PBS and lysed in 0.1 M NaOH/0.1% (w/v) sodium dodecyl sulfate for total protein isolation. Ca2+ concentrations were normalized for total protein as determined by Pierce BCA protein detection kit according to the manufacturer’s instructions (Fisher Scientific, Massachussets, USA).
Alizarin Red staining
Calcification was visualized by the Alizarin Red S staining method for Ca2+. Cultures were washed with PBS, fixed in 4% (v/v) formalin for 15 minutes and washed with demineralized H2O before staining with 2% (w/v) aqueous Alizarin Red (Sigma) for 5 minutes.
RNA isolation and real-time polymerase chain reaction (RT-qPCR)
Total RNA was extracted from VSMC using TRIzol (Invitrogen) and treated with DNAse (1 U/μg RNA, Promega, Wisconsin, USA) to remove genomic DNA. cDNA was synthesized from 1.5 μg total RNA by Moloney Murine Leukemia Virus reverse transcriptase (Invitrogen) for one hour at 37 °C. The primers used for PCR amplification are shown in Table 1 and were equally efficient. RT-qPCR was executed in duplicate using IQ SYBRGreen Mix according to the manufacturers protocol (Bio-Rad), using a Bio-Rad thermos-cycler (Bio-Rad). The expression of target genes was normalized to GAPDH expression levels.
Alkaline phosphatase activity assay
Cells grown in 12-well plates and cultured in designated media for 2, 8 and 14 days were lysed with 1% (v/v) Triton X-100 in PBS containing protease inhibitors. ALP activity was determined in the total lysate as the hydrolysis of p-nitrophenyl phosphate (sigma) into p-nitrophenol in a basic buffer by ALP by p-nitrophenol production. The reaction was incubated for 30 minutes at 37 °C and the absorbance for p-nitrophenol was measured at calorimetrically at 410 nm for both p-nitrophenol (Sigma) standards and samples. One unit (U) was defined as the production of 1 µmol p-nitrophenol per minute per gram protein.
Detection of apoptosis
Occurrence of apoptosis was measured using the Annexin V-FITC Apoptosis Detection Kit (ab14085 Abcam, Cambridge, UK). Due to the presence of calcifications, the method for adherent cells was used according to the manufacturer’s instructions. Briefly, cells were incubated with Annexin-V-FITC and propidium iodide in binding buffer for 5 minutes at room temperature. Apoptotic cells were detected by immunofluorescence microscopy using a FITC and Texas Red filter on an Axio Imager M (Zeiss). Apoptosis was quantified using ImageJ software (NIH, Maryland, USA) by calculating the ratio of the area positive for FITC signal versus total area, as the mean of multiple captures in 3 replicates per treatment per time-point.
Crystal isolation for X-ray diffraction, scanning electron microscopy and energy-dispersive spectroscopy analysis
Cell culture supernatants of BGP-treated cells in 6-well plates with and without 2 mM MgCl2 were collected and purified. Supernatants were centrifuged for one hour at 16 000 × g19. The pellets containing the nanocrystals were washed with demineralized H2O and then re-centrifuged. Subsequently, the crystal pellets were dried and used for analysis. One measurement represents the crystals formed in a total of 7 wells containing 2 ml of culture medium in the BGP treated cultures. As less material was formed in the BGP cultures supplemented with Mg2+, one measurement represents the crystals formed in a total of 21 wells containing 2 ml of culture medium in order to reach sufficient amounts to detect by X-ray diffraction. For X-ray diffraction analysis, diffractograms were measured on a PANalytical Empyrean (PANalytical, Almelo, the Netherlands) in transmission mode with fine-focus sealed tube, focusing mirror and PIXcel3D detector, using CuKα radiation. The samples were measured in a capillary, using 0.5 mm soda glass capillaries with a wall thickness of 0.01 mm. For scanning electron microscopy (SEM) (GeminiSEM, Zeiss) in combination with energy-dispersive spectroscopy (EDX) for elemental analysis (QUANTAX 200, Bruker) the crystal pellets were transferred onto copper tape and coated with carbon. High-resolution pictures were obtained using an Everhart-Thornley SE detector. Accelerating voltage was 5 kV for morphological observations and 15 kV for micro-elemental analyses. Due to the use of BGP as calcification inducer, a cell-free control could not be included as cellular presence is necessary to cause Pi accumulation in the medium (data not shown).
Statistics
Parametric data were analyzed by One-Way ANOVA with Tukey’s post-hoc test to correct for multiple comparisons using PRISM software (GraphPad, San Diego, CA). Non-parametric data as identified by Shapiro-Wilk test for normality were analyzed using Kruskall-Wallis analysis with Dunn’s correction for multiple analysis. Time-course data was analyzed using a Two-Way ANOVA. All data are shown as mean ± SEM. P < 0.05 was considered statistically significant.
Results
β-glycerophosphate supplementation resulted in increased medium Pi concentration
BGP is a Pi-donor that requires enzymatic cleavage in order to release Pi. As Pi exposure is one of the decisive factors in the calcification process, the Pi concentration of the cell culture supernatant was assessed after 2, 8 and 14 days of treatment (Fig. 1). 10 mM BGP treatment resulted in gradual increase in Pi concentration over time, reaching 4.6 ± 0.3 mM after 14 days. 2 mM Mg2+ supplementation led to significantly higher Pi concentrations of 7.6 ± 0.8 mM after 14 days. In contrast, BGP treatment in cell-free conditions did not lead to increased Pi concentrations under the same conditions (data not shown).
BGP increased medium Pi concentration. bVSMC were cultured with 10 mM BGP and the Pi concentration in the cell culture supernatant was measured in whole media at 2 (white bars), 8 (striped bars) and 14 (black bars) days. Data are shown as the mean of 3 individual experiments (each consisting of 3 replicates) ±SEM. Unless shown otherwise, *Indicates P < 0.05 versus control. BGP, β-glycerophosphate; bVSMC, bovine vascular smooth muscle cells; Pi, inorganic phosphate; SEM, standard error of the mean.
Mg2+ prevents vascular smooth muscle cell mineralization
The effect of BGP on the development of calcifications was studied using cellular Ca2+ measurements and visualized by Alizarin Red staining (Fig. 2). 10 mM BGP treatment of bVSMC resulted in variable but pronounced calcification after 14 days (146 ± 93 versus 2.5 ± 0.2 µg Ca2+ per gram protein in the control condition, p < 0.05). Ca2+ deposition was completely prevented by 2 mM Mg2+ in our model (3.5 ± 0.3 µg/g protein Ca2+).
High Mg2+ prevented mineralization, despite high medium Pi concentrations. Quantification of calcification by cellular calcium deposition at 2 (white bars), 8 (striped bars) and 14 (black bars) days during calcification by BGP supplementation (a) and Alizarin Red staining for calcium (b). Calcium deposition data are shown as the mean of 3 individual experiments (each consisting of 3 replicates) ±SEM. *Indicates P < 0.05 versus control. Scale bar corresponds with 100 µm. BGP, β-glycerophosphate; Pi, inorganic phosphate; SEM, standard error of the mean.
β-glycerophosphate supplementation upregulated OPN gene expression but did not result in changes in mRNA expression of calcification activators
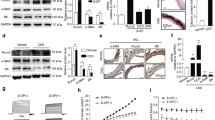
To assess the effects of Mg2+ involved in the prevention of VSMC calcification, gene expression levels of ACTA2 and osteogenic transcription factors RUNX2 and BMP2 were assessed after 2, 8 and 14 days (Fig. 3a–c). 10 mM BGP treatment did not result in expression changes of ACTA2, RUNX2 and BMP2 over the time course of calcification. 2 mM Mg2+ supplementation did not affect these expression levels. Both ACTA2 and BMP2 mRNA expression significantly increased over time in all conditions, independent of BGP treatment (Fig. 3a–c). In addition, mRNA expression levels of calcification inhibitors OPG, OPN and MGP were assessed (Fig. 3d–f). OPG expression was significantly downregulated by Mg2+ supplementation compared all other treatments after 8 days. No effect of BGP was observed at all time-points. MGP gene expression showed a significant increase over time in all treatment groups, while no effect of BGP was observed. After 14 days, BGP significantly increased OPN expression, which was prevented by Mg2+. In addition to osteogenic transcription factors, ALP is a well-known indicator for osteoblastic maturation. Therefore, ALP mRNA expression and activity were measured to assess the effect of Mg2+ on the development of an osteoblastic phenotype after 2, 8 and 14 days. BGP did not change ALPL mRNA expression and ALP activity, which remained stable after Mg2+ supplementation (Fig. 3g,h).
Bovine VSMC did not underdo osteogenic transdifferentiation after BGP treatment. mRNA expression of ACTA2 (a), osteogenic transcription factors RUNX2 (b) and BMP2 (c) and calcification inhibitors OPG (d), OPN (e) and MGP (f) were measured after 2 (white bars), 8 (striped bars) and 14 (black bars) days of BGP supplementation in presence or absence of Mg2+. mRNA levels were normalized for GAPDH expression and are shown relative to the 2-day control. ALP activity (g) and mRNA expression (h) remained stable during BGP treatment. Data are shown as the mean of 3 individual experiments (each consisting of 3 replicates) ±SEM. Unless shown otherwise, significance is indicated versus control (*Indicates P < 0.05). ACTA2, α-smooth muscle actin; ALPL, alkaline phosphatase; BGP, β-glycerophosphate; BMP2, bone morphogenetic protein 2; bVSMC, bovine vascular smooth muscle cells; GAPDH, glyceraldehyde 3-phosphate dehydrogenase; MGP, matrix gla protein; OPG, osteoprotegerin; OPN, osteopontin; RUNX2, Runt-related transcription factor 2; SEM, standard error of the mean.
VSMC mineralization preceded apoptosis
As apoptosis accelerates VSMC calcification in vitro25, the occurrence of apoptosis was assessed in VSMC at 2, 8 and 14 days (Fig. 4). 10 mM BGP treatment did not result in increased apoptosis before the onset of calcification at 2 and 8 days. After 14 days, apoptosis was observed in calcified regions. Mg2+ prevented calcification at all time-points as apoptosis was not detected in the Mg2+-supplemented BGP cells.
Calcification preceded bVSMC apoptosis. Apoptosis was detected on adherent cells by Annexin-V FITC conjugated antibody quantified at 2 (white bars), 8 (striped bars) and 14 (black bars) days of BGP supplementation in presence or absence of Mg2+ (a). Nuclei are stained with DAPI (blue), Annexin-V positive cells (green) indicate apoptosis (arrows), which was observed only after onset of calcification at 14 days. Images represent 3 individual experiments. Scale bars correspond to 200 µm (upper panel) and 100 µm (lower panel). Prior to calcification, as represented by 2-day and 8-day treated samples, no apoptosis was detected (b). *Indicates P < 0.05 versus control. BGP, β-glycerophosphate.
TRPM7 was not involved in the protective effect of Mg2+ against β-glycerophosphate-induced calcification
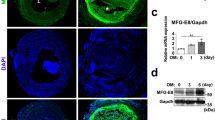
TRPM7 is the main Mg2+ channel in VSMCs26. To examine whether a TRPM7-mediated increasing intracellular Mg2+ concentration prevents VSMC calcification, VSMCs were treated with 10 µM 2-APB, which is a TRPM7 blocker11. 2-APB treatment of Mg2+ supplemented BGP cultures did not reverse the protective effect of Mg2+ on BGP-induced VSMC calcification (Fig. 5a). Furthermore, 10 mM BGP treatment did not affect TRPM7 mRNA expression levels in cultured VSMC (Fig. 5b).
Inhibition of TRPM7 did not abrogate the protective effects of Mg2+. Ca2+ deposition was measured in calcifying bVSMC supplemented with Mg2+ cultured with 10 µM 2-APB, a TRPM7 inhibitor, for 14 days (a). In calcifying bVSMC, mRNA expression levels of TRPM7 were not affected after 2 (white bars), 8 (striped bars) and 14 days (black bars) (b). Data are shown as the mean of 3 individual experiments (each consisting of 3–4 replicates) ± SEM. *Indicates P < 0.05 versus control. 2-APB, 2-Aminoethyl diphenylborinate; BGP, β-glycerophosphate; bVSMC, bovine vascular smooth muscle cells; TRPM7, transient receptor potential melastatin.
Mg2+ prevented β-glycerophosphate-induced formation of extracellular hydroxyapatite crystals
To investigate the potential role of Mg2+ in crystal growth and formation, the cell culture supernatants of BGP-treated cells in the presence or absence of Mg2+ were analyzed for the incidence of crystals using X-ray powder diffraction. In the BGP-treated samples, the X-ray diffraction patterns revealed the presence of a considerable amount of hydroxyapatite crystals (Fig. 6). The broadening of the hydroxyapatite diffraction peaks, compared to the NaCl peaks, indicate that the hydroxyapatite crystals are nano-sized. Both crystals isolated from the cell culture supernatants and a synthetic hydroxyapatite standard, that was used as positive control, matched with a reference diffraction pattern specific for hydroxyapatite crystals (see Supplemental Fig. 2). Hydroxyapatite diffraction peaks were absent in the Mg2+-supplemented BGP supernatants. Of note, no crystals other than hydroxyapatite and NaCl were identified. As X-ray diffraction exclusively detects crystalline material and not amorphous material, isolated particles were analyzed by SEM-EDX for morphology and elemental composition (Fig. 7). EDX analysis revealed a reduced Ca2+ and Pi fraction in crystal clusters of 68% and 41% after Mg2+ supplementation, respectively, without increasing the fraction of Mg2+ present in the crystal clusters (Fig. 7b,c).
Impact of Mg2+ on BGP-induced Ca2+-apatite formation. X-ray powder diffraction analysis of cell culture supernatants show presence of NaCl (*) and Ca-apatite (arrows) in BGP treated cultures (black line), but not in BGP cultures supplemented with Mg2+ (gray line). Of note: as the BGP culture supplemented with Mg2+ contained less precipitates; one measurement represents 21 cultures (6-well format) compared to 7 in the BGP condition in order to reach the detection threshold. BGP, β-glycerophosphate.
Crystal or particle clusters formed in BGP cell culture supernatant are morphologically and chemically distinct. Morphology of crystal clusters formed in BGP and in BGP supplemented with Mg2+ cell culture supernatants, as overview (upper) and focused (lower) for EDX analysis (a). The averaged EDX-spectrum and resulting quantification of the crystal cluster isolated from Mg2+ supplemented culture supernatant reveals reduced Ca (green) and P (purple), as visualized in the elemental map (c) compared to crystal clusters found in BGP treated cultures (b). In addition, Mg2+ supplemented crystal clusters showed increased Na (blue) and Cl (orange) compared to BGP crystal clusters. Data are presented as mean of the analyses of ten individual crystal clusters. BGP, β-glycerophosphate; CPS, counts per second; EDX, energy dispersive spectroscopy; (k)eV, (kilo)-electron volt.
Discussion
Here, we demonstrate that Mg2+ inhibits bVSMC mineralization through inhibition of Ca-apatite formation in the extracellular space, independent of VSMC transdifferentiation. Our most important finding is the absence of hydroxyapatite crystals in the medium of BGP-treated bVSMCs supplemented with Mg2+. Characterization by SEM-EDX confirmed the reduction of Ca-apatite crystals in Mg2+-supplemented supernatants, without incorporation of Mg2+ in the formed crystals. Underlining the strong capacity of Mg2+ to block crystal formation, 2 mM Mg2+ was sufficient to prevent the calcification process, even though extracellular Pi levels rise to 7 mM in Mg2+-BGP treated bVSMCs. Moreover, intracellular action of Mg2+ is not likely in our setup, because when cellular Mg2+ uptake was impaired using TRPM7-blocker 2-APB, Mg2+ still prevented vascular calcification11. Accordingly, we propose that Mg2+ prevents VSMC mineralization through the inhibition of hydroxyapatite formation in the extracellular space, blocking its deposition on VSMC.
Hydroxyapatite (Ca10(PO4)6(OH)2) is the most abundant type of crystal in uremic arterial calcifications and its formation has been shown to be essential for VSMC transdifferentiation and vascular calcification19,27. Although it has been suggested that the potential incorporation of Mg2+ in Ca-apatite crystals (whitlockite, Ca9Mg(HPO4)(PO4)6), may reduce crystal pathogenicity and increase solubility, we did not identify any whitlockite after Mg2+ treatment. Our data suggest that Mg2+ most likely prevents crystal nucleation, rather than affecting crystal content. These findings are in line with previous studies that exclusively identified hydroxyapatite, and not whitlockite, in deposits on calcifying VSMC supplemented with Mg2+ 28. Indeed, high concentrations of Mg2+ led to less hydroxyapatite deposition in a study by Louvet et al.29. Given the lack of crystals after Mg2+ supplementation, our results indicate that Mg2+ inhibits the early phases of crystal assembly in high Pi-media. Moreover, we hypothesize that the incorporation of Pi in hydroxyapatite in the BGP condition explains the lower free Pi concentration in BGP-treated compared to the Mg2+-BGP-treated culture media.
Initial Ca-Pi particle formation in response to elevated Pi-levels has shown to occur in a cell-independent manner, subsequently initiating VSMC transdifferentiation when native VSMC inhibitory capacities diminish19,30. Though poorly studied in the context of VSMC mineralization, Mg2+ is known to stabilize amorphous Ca-Pi particles and therefore inhibit Ca-apatite maturation in acellular systems31,32,33,34,35,36. While the exact mechanisms remain unknown, evidence suggests that Mg2+ may stabilize extracellular ATP. Hydrolysis of ATP is necessary for hydroxyapatite nucleation21. The importance of crystal maturation in the initiation of VSMC transdifferentiation and vascular calcification has been frequently emphasized18,19,30,37. Recently, Ca-Pi-containing soluble nanoparticles or calciprotein particles (CPP) were shown to stimulate calcification37. Interestingly, Mg2+ delays CPP maturation in uremic serum38. These findings support that Mg2+ prevents mineralization by directly inhibiting Ca-apatite crystal formation or maturation in the extracellular space.
Mg2+ supplementation has repeatedly shown to prevent osteogenic gene expression. As a result, osteogenic gene expression has been repeatedly considered as Mg2+ target to prevent osteoblastic transdifferentiation39. In line with this hypothesis, previous research showed that Mg2+ concentrations as low as 0.8 mM reversed established calcification in human VSMC, which could be abrogated by 2-APB treatment17. These results suggest that cellular Mg2+ uptake via TRPM7 prevents VSMC calcification7,11,17. However the role of TRPM7 is controversial, as recent evidence suggests that interleukin-18 enhanced VSMC calcification through TRPM7 activation40. In our model, TRPM7 inhibition by 2-APB did not affect the Mg2+ rescue.
bVSMC are characterized by high basal expression levels of ALP, which makes them prone to calcification. Despite their susceptibility to calcify, the bVSMCs are contractile and do not present any signs of osteoblastic transdifferentiation, as high levels of ACTA2 expression and α-SMA protein expression were preserved in response to BGP supplementation. Although our bVSMCs strongly calcified, BGP treatment did not result in osteogenic conversion as demonstrated by stable expression of BMP2, RUNX2 and ALPL among treatments14. Interestingly, both mRNA expression of BMP2 and ACTA2 increased over time. However, these observations were irrespective of treatment and are therefore not related to osteoblastic transdifferentiation of the bVSMC. The only transcriptional response observed during BGP-induced calcification was upregulation of the OPN gene after 14 days, which was prevented by Mg2+. Increased OPN expression is associated with calcification19,41,42. OPN is an inhibitor of calcification and potently inhibits hydroxyapatite growth and OPN upregulation has been shown to reflect a protective mechanism in response to the phosphate- and hydroxyapatite-rich environment by VSMC43,44,45. The absence of OPN upregulation in Mg2+-supplemented BGP cultures may therefore be explained by the lack of Ca-Pi formation. Moreover, OPN is only increased at 14 days after calcification was already manifested, suggesting it to be resulting from calcification rather than causing. In addition to osteoinductive signaling, apoptosis has been shown to induce the progression of calcification25. Our results indicate that calcification precedes apoptosis, as apoptosis was only detected after 14 days of BGP treatment when calcification was already manifested. In our setup, apoptosis is likely the result of exposure to Ca-Pi crystals, rather than a causative factor for calcification46.
In human, rodent and bovine calcification models evidence strongly suggests that calcification is a result of VSMC undergoing osteogenic transdifferentiation and that Mg2+ effectively abrogates this through upregulation of calcification inhibitors and downregulation of osteogenic genes6,7,8,11,16,17,47,48. Indeed, we show the effective inhibition of Mg2+ in VSMC calcification. However, in contrast to previous studies, our results suggest that calcification is driven by extracellular hydroxyapatite formation independent of osteogenic transdifferentiation in bVSMCs. While many studies show the association between osteogenic transdifferentiation and vascular calcification, it remains debatable whether this transdifferentiation is an undisputable prerequisite for the development of mineralization49. Calcification represents the final common pathway of multiple pathological vascular processes50. Our results do not contradict intracellular Mg2+ effects on osteoblastic transdifferentation. However, they do highlight the presence of alternative extracellular effects on crystal formation. Overall, it is important to note that potential intracellular and extracellular pathways involved in the calcification-inhibiting capacity of Mg2+ are not mutually exclusive. Given the strong effect of Mg2+ on calcification independent of osteogenic pathways, however, the relative contribution of crystal inhibition compared to any intracellular targets may be considerable and underestimated to date.
An important strength of this study is that our model favored to study the effects of Mg2+ on extracellular crystal growth, independent of genetic VSMC transdifferentiation. Although it has been reported previously that Mg2+ inhibits calcification, most study set-ups do not allow to discriminate between extracellular reduction of crystal formation and intracellular inhibition of osteogenic conversion6,7,8,11,17. A limitation of this study is that while we show that TRMP7 seems not to be involved in calcification, we cannot exclude that other Mg2+ channels than TRPM7 facilitate Mg2+ entry into the bVSMCs. However, it was shown previously that TRPM7 is the main Mg2+ channel in VSMCs26. Therefore, the contribution of other transporters is likely minor. In addition, we show the effectiveness of Mg2+ primarily through extracellular mechanisms involving hydroxyapatite. In contrast to other studies, the driving force of calcification in our model is not osteoblastic transdifferentiation but mainly hydroxyapatite formation and deposition. Therefore, any intracellular effects of Mg2+ involving modification of osteogenic genes such as BMP2 and RUNX2 cannot be excluded.
In conclusion, our findings demonstrate a role for Mg2+ in preventing VSMC mineralization involving direct extracellular Ca-apatite crystal inhibition. An increasing body of studies now report that Mg2+ prevents vascular calcification by extracellular Pi binding. Mg2+ has been shown to reduce both vascular and non-vascular calcifications and to improve calcification propensity, favoring a non-cellular mechanism of action38,51. Therefore, Mg2+ may be considered an important and realistic approach to potentially reduce the risk for vascular calcification and subsequent cardiovascular complications in CKD patients. Clinical trials are warranted to further assess the clinical relevance of Mg2+ in relation to vascular calcifications.
References
London, G. M. et al. Arterial media calcification in end-stage renal disease: Impact on all-cause and cardiovascular mortality. Nephrol Dial Transplant 18, 1731–1740 (2003).
Shanahan, C. M., Crouthamel, M. H., Kapustin, A. & Giachelli, C. M. Arterial Calcification in Chronic Kidney Disease: Key Roles for Calcium and Phosphate. Circ Res 109, 697–711 (2011).
Kieboom, B. C. T. et al. Serum Magnesium and the Risk of Death From Coronary Heart Disease and Sudden Cardiac Death. J Am Heart Assoc 5, e002707 (2016).
De Roij van Zuijdewijn, C. L. M. et al. Serum Magnesium and Sudden Death in European Hemodialysis Patients. PLoS One 10, e0143104 (2015).
Sakaguchi, Y. et al. Association between Density of Coronary Artery Calcification and Serum Magnesium Levels among Patients with Chronic Kidney Disease. PLoS One 11, e0163673 (2016).
Bai, Y. et al. Magnesium prevents β-glycerophosphate-induced calcification in rat aortic vascular smooth muscle cells. Biomed Reports 3, 593–597 (2015).
Louvet, L., Büchel, J., Steppan, S., Passlick-Deetjen, J. & Massy, Z. A. Magnesium prevents phosphate-induced calcification in human aortic vascular smooth muscle cells. Nephrol Dial Transplant 28, 869–78 (2013).
Kircelli, F. et al. Magnesium reduces calcification in bovine vascular smooth muscle cells in a dose-dependent manner. Nephrol Dial Transplant 27, 514–521 (2012).
Kingman, J., Uitto, J. & Li, Q. Elevated dietary magnesium during pregnancy and postnatal life prevents ectopic mineralization in Enpp1asj mice, a model for generalized arterial calcification of infancy. Oncotarget 8, 38152–38160 (2016).
Gorgels, T. G. M. F. et al. Dietary magnesium, not calcium, prevents vascular calcification in a mouse model for pseudoxanthoma elasticum. J Mol Med 88, 467–475 (2010).
Montezano, A. C. et al. Vascular smooth muscle cell differentiation to an osteogenic phenotype involves TRPM7 modulation by magnesium. Hypertension 56, 453–462 (2010).
de Baaij, J. H. F., Hoenderop, J. G. J. & Bindels, R. J. M. Magnesium in Man: Implications for Health and Disease. Physiol Rev 95, 1–46 (2015).
Ter Braake, A. D., Shanahan, C. M. & De Baaij, J. H. F. Magnesium Counteracts Vascular Calcification: Passive Interference or Active Modulation? Arterioscler Thromb Vasc Biol 37, 1431–1445 (2017).
Shanahan, C. M. Mechanisms of vascular calcification in renal disease. Nat Rev Nephrol 63, 146–57 (2013).
Tyson, K. L. et al. Osteo/Chondrocytic Transcription Factors and Their Target Genes Exhibit Distinct Patterns of Expression in Human Arterial Calcification. Arterioscler Thromb Vasc Biol 23, 489–494 (2003).
Louvet, L., Metzinger, L., Büchel, J., Steppan, S. & Massy, Z. A. Magnesium Attenuates Phosphate-Induced Deregulation of a MicroRNA Signature and Prevents Modulation of Smad1 and Osterix during the Course of Vascular Calcification. Biomed Res Int 2016, 1–11 (2016).
De Oca, A. M. et al. Magnesium inhibits wnt/b-catenin activity and reverses the osteogenic transformation of vascular smooth muscle cells. PLoS One 9, 1–10 (2014).
Proudfoot, D. & Shanahan, C. M. Nanocrystals seed calcification in more ways than one. Kidney Int 79, 379–382 (2011).
Sage, A. P., Lu, J., Tintut, Y. & Demer, L. L. Hyperphosphatemia-induced nanocrystals upregulate the expression of bone morphogenetic protein-2 and osteopontin genes in mouse smooth muscle cells in vitro. Kidney Int 79, 414–22 (2011).
Boskey, A. L. & Posner, A. S. Magnesium stabilization of amorphous calcium phosphate: A kinetic study. Mater Res Bull 9, 907–916 (1974).
Blumenthal, N. C., Betts, F. & Posner, A. S. Stabilization of amorphous calcium phosphate by Mg and ATP. Calcif Tissue Int 23, 245–250 (1977).
Tenhuisen, K. S. & Brown, P. W. Effects of magnesium on the formation of calcium-deficient hydroxyapatite from CaHPO4 2H2O and Ca4(PO4)2O. Calcif Tissue Int 4, 538–546 (1996).
Harder, K. W. et al. Characterization and kinetic analysis of the intracellular domain of human protein tyrosine phosphatase beta (HPTP bèta) using synthetic phosphopeptides. Biochem J 298, 395–401 (1994).
Hoenderop, J. G. et al. Calcitriol controls the epithelial calcium channel in kidney. J Am Soc Nephrol 12, 1342–1349 (2001).
Proudfoot, D. et al. Apoptosis Regulates Human Vascular Calcification In Vitro: Evidence for Initiation of Vascular Calcification by Apoptotic Bodies. Circ Res 87, 1055–1062 (2000).
He, Y., Yao, G., Savoia, C. & Touyz, R. M. Transient receptor potential melastatin 7 ion channels regulate magnesium homeostasis in vascular smooth muscle cells: Role of angiotensin II. Circ Res 96, 207–215 (2005).
Lee, J. S., Morrisett, J. D. & Tung, C. H. Detection of hydroxyapatite in calcified cardiovascular tissues. Atherosclerosis 224, 340–347 (2012).
De Schutter, T. M. et al. Effect of a magnesium-based phosphate binder on medial calcification in a rat model of uremia. Kidney Int 83, 1109–17 (2013).
Louvet, L. et al. Characterisation of Calcium Phosphate Crystals on Calcified Human Aortic Vascular Smooth Muscle Cells and Potential Role of Magnesium. PLoS One 10, e0115342 (2015).
Villa-Bellosta, R., Millan, A. & Sorribas, V. Role of calcium-phosphate deposition in vascular smooth muscle cell calcification. AJP Cell Physiol 300, C210–C220 (2010).
Eanes, E. D. & Posner, A. S. Kinetics and mechanism of conversion of non-crystalline calcium phosphate to hydroxyapatite. Trans N Y Acad Sci 28, 233–241 (1965).
Termine, J. D., Peckauskas, R. A. & Posner, A. S. Calcium phosphate formation in vitro. Arch Biochem Biophys 140, 318–325 (1970).
Boistelle, R., Lopex-Valero, I. & Abbona, F. Cristallisation des phosphates de calcium en présence de magnésium. Nephrologie 14, 265–269 (1993).
Apfelbaum, F., Mayer, I., Rey, C. & Lebugle, A. Magnesium in maturing synthetic apatite: a Fourier transform infrared analysis. J Cryst Growth 144, 304–310 (1994).
Boskey, A. L. et al. The Mechanism of bèta-glycerophosphate Action in Mineralizing Chick Limb-Bud Mesenchymal Cell Cultures. J Bone Miner Res 11, 1694–1712 (1996).
Salimi, M. H., Heughebaert, J. C. & Nancollas, G. H. Crystal growth of calcium phosphates in the presence of magnesium ions. Langmuir 1, 119–122 (1985).
Aghagolzadeh, P. et al. Calcification of vascular smooth muscle cells is induced by secondary calciprotein particles and enhanced by tumor necrosis factor-α. Atherosclerosis 251, 1–11 (2016).
Pasch, A. et al. Nanoparticle-Based Test Measures Overall Propensity for Calcification in Serum. J Am Soc Nephrol 23, 1744–1752 (2012).
Massy, Z. A. & Drüeke, T. B. Magnesium and cardiovascular complications of chronic kidney disease. Nat Rev Nephrol 11, 1–11 (2015).
Zhang, K. et al. Interleukin-18 Enhances Vascular Calcification and Osteogenic Differentiation of Vascular Smooth Muscle Cells Through TRPM7 Activation. Arterioscler Thromb Vasc Biol 37, 1933–1943 (2017).
Shioi, A. et al. beta-Glycerophosphate Accelerates Calcification in Cultured Bovine Vascular Smooth Muscle Cells. Arterioscler Thromb Vasc Biol 15, 2003–2009 (1995).
Ahmed, S., Neill, K. D. O.’, Hood, A. F., Evan, A. P. & Moe, S. M. Calciphylaxis Is Associated With Hyperphosphatemia and Increased Osteopontin Expression by Vascular Smooth Muscle Cells. Am J Kidney Dis 37, 1267–1276 (2001).
Chen, N. X., O’neill, K. D., Duan, D. & Moe, S. M. Phosphorus and uremic serum up-regulate osteopontin expression in vascular smooth muscle cells. Kidney Int 62, 1724–1731 (2002).
Hunter, G. K. Role of osteopontin in modulation of hydroxyapatite formation. Calcif Tissue Int 93, 348–354 (2013).
Paloian, N. J., Leaf, E. M. & Giachelli, C. M. Osteopontin protects against high phosphate-induced nephrocalcinosis and vascular calcification. Kidney Int 89, 1027–1036 (2016).
Ewence, A. E. et al. Calcium phosphate crystals induce cell death in human vascular smooth muscle cells: A potential mechanism in atherosclerotic plaque destabilization. Circ Res 103, 28–35 (2008).
Alesutan, I. et al. Inhibition of osteo/chondrogenic transformation of vascular smooth muscle cells by MgCl2 via calcium-sensing receptor. J Hypertens 35, 523–532 (2016).
Xu, J. et al. Magnesium modulates the expression levels of calcification-associated factors to inhibit calcification in a time-dependent manner. Exp Ther Med 9, 1028–1034 (2015).
Leopold, J. A. Vascular calcification: Mechanisms of vascular smooth muscle cell calcification. Trends Cardiovasc Med 25, 267–274 (2014).
Vervloet, M. & Cozzolino, M. Vascular calcification in chronic kidney disease: different bricks in the wall? Kidney Int 91, 808–817 (2016).
Jiang, Q. & Uitto, J. Restricting dietary magnesium accelerates ectopic connective tissue mineralization in a mouse model of pseudoxanthoma elasticum (Abcc6−/−). Exp Dermatol 21, 694–699 (2012).
Acknowledgements
We thank Robert Hayward from the BHF Centre of Research Excellence, Cardiovascular Division, James Black Centre, King’s College, London, United Kingdom and Huib Croes from the Department of Cell Biology, Radboud Institute for Molecular Life Sciences, Radboud university medical center, Nijmegen, The Netherlands for their technical support. This work was financially supported by grants from the Netherlands Organization for Scientific Research (NWO Rubicon 825.14.021 and VICI 016.130.668) and the Dutch Kidney Foundation (Kolff 14OKG17 and 15OP02).
Author information
Authors and Affiliations
Contributions
Study conception and design: A.D.t.B., J.H.F.d.B., C.M.S., J.G.J.H. Acquisition of data: A.D.t.B., P.T.T. Critical revision: A.D.t.B., P.T.T., J.H.F.d.B., C.M.S., J.G.J.H.
Corresponding author
Ethics declarations
Competing Interests
Catherine M. Shanahan has a consultancy agreement with OPKO Health. The other authors declare no conflict of interest.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
ter Braake, A.D., Tinnemans, P.T., Shanahan, C.M. et al. Magnesium prevents vascular calcification in vitro by inhibition of hydroxyapatite crystal formation. Sci Rep 8, 2069 (2018). https://doi.org/10.1038/s41598-018-20241-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-018-20241-3
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.