Abstract
In absence of direct comparison, we conducted an indirect-comparison meta-analysis to evaluate the efficacy and safety of thrombopoietin-receptor agonists(TPO-RAs) in treatment of pediatric persistent or chronic immune thrombocytopenia(ITP). PubMed, Embase, Cochrane Library, Clinical Trials.gov, China National Knowledge Infrastructure, and Chinese Biomedical Literature Database were searched from their earliest records to May 2017. Randomized controlled trials comparing the TPO-RAs with placebo in pediatric ITP were included. Outcomes included overall response rate(primary), durable response, overall or clinically significant bleeding, the proportion of patients receiving rescue medication, and safety. Five randomized placebo-controlled studies(N = 261) were analyzed. The overall response[Risk Ratio(RR) 0.57, 95% confidence interval(CI) 0.21–1.56], the incidence of adverse events (RR 0.96, 95%CI 0.66–1.39), durable response(RR 2.48, 95%CI 0.31–19.97), and the proportion of patients receiving rescue treatment(RR 0.73, 95%CI 0.20–2.73) were similar between eltrombopag and romiplostim group. Nevertheless, eltrombopag might have lower risk of overall bleeding(RR 0.43, 95%CI 0.23–0.80) and clinically significant bleeding(RR 0.33, 95%CI 0.12–0.89) than romiplostim. This meta-analysis suggests that eltrombopag might be similar to romiplostim in efficacy and safety, but seems to reduce the risk of bleeding compared to romiplostim. Furthermore, cost of the treatment, comorbidity of patients and drug compliance should also be considered in clinical decision making.
Similar content being viewed by others
Introduction
Immune thrombocytopenia (ITP) is an immune-mediated disease characterized by transient or persistent decrease in the platelet count and increased risk of bleeding1. The pediatric ITP incidence reported in recent population-based studies varied greatly in different countries: 1.91 per 105 in Japan2, 2.83 per 105 in France3, 4.2 per 105 in the United Kingdom4 and 14.5 per 105 in Korea5, respectively. Most children with ITP achieve remission spontaneously over time, however, 23.1%~47.3% of them develop a disease course of more than 6 months6.
For management of pediatric ITP, the first-line treatments include observation, corticosteroids, intravenous immunoglobulin (IVIg) and anti-D immunoglobulin7,8,9. If previous treatments fail, subsequent treatments may include splenectomy, rituximab, thrombopoietin receptor agonists (TPO-RAs), or more potent immunosuppression7. Eltrombopag (ELT), an oral non-peptide TPO-RA which could facilitate the proliferation and differentiation of megakaryocytes and increase platelet production10, has been approved by the United States Food and Drug Administration (FDA) for pediatric patients (≥1 year old) with chronic ITP who have “not achieved an appropriate response using other ITP medicines or splenectomy”11. Romiplostim (ROM), a subcutaneously administered peptide mimetic TOP-RA, was found effective in children with chronic ITP by randomized clinical trials and observational studies12,13,14,15,16,17,18,19. A systematic review including both adult and pediatric patients concluded that TPO-RAs substantially increased the rates of platelet response or durable response in children subgroup20.
Nevertheless, ROM binding to the extracellular TPO-receptor and ELT binding to a transmembrane site of the TPO-receptor have different mechanisms of action21,22. They also have different ways of administration, as ROM is given by subcutaneous injection, while ELT is given orally. Therefore, their efficacy and safety might be different. Unfortunately, there are no head-to-head randomized controlled trials (RCTs) comparing ROM with ELT in treatment of pediatric ITP. Hence indirect comparisons of the therapeutic outcomes across separate RCTs are recommended in the UK National Institute for Health and Clinical Excellence (NICE) methods guide23. The indirect comparison method proposed by Bucher preserves within-trial randomization by comparing treatment effects (RR) relative to a common comparator (placebo) from each trial, rather than comparing individual treatment arms from different trials24, and thus becomes a standard source of comparative evidence. An indirect comparison between ROM and ELT in treatment of adult patients with ITP was previously conducted25, but these conclusions may not be applicable for children due to different disease characteristics. This study aims to evaluate the efficacy and safety of ELT versus ROM for children with ITP using an indirect-comparison meta-analysis.
Results
Search result and characteristics of included studies
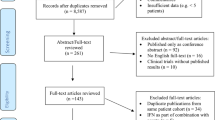
A total of 3,499 citations were obtained from the literature search and Fig. 1 showed the selection process. Five randomized, placebo-controlled studies (261 participants)18,19,26,27,28 were included in this systematic review. Agreement between two reviewers for study selection was excellent (K = 0.89). As shown in Table 1, four multicenter studies were conducted in 16 countries or regions (USA, UK, Canada, Spain, France, the Netherlands, Argentina, Czech Republic, Germany, Hong Kong, Israel, Italy, Russia, Taiwan, Thailand and Australia)18,19,27,28 except one single-center study conducted in Egypt26.
All participants were aged 1–17 years old, with disease duration more than 6 months and baseline platelet count less than 30 × 109/L. Two studies (159 participants) evaluated the efficacy and safety of ELT in comparison to placebo27,28 (Table 2). The initial dose of ELT was based on age and weight, and the following dose was adjusted according to individual platelet counts, with a target of 50–200 × 109/L27. The initial dosage and adjustment were shown in Table 3. Three studies evaluated the efficacy and safety of ROM18,19,26. It was administrated at the initial dose of 1 μg/kg and was also adjusted according to platelet counts (Table 3). The double-blind phase of included studies ranged from 7 to 24 weeks.
Risk of Bias assessment
As shown in Fig. 2, four studies18,19,27,28 had low risk of selection bias for central randomization while the other one26 was unclear because the method of randomization and allocation concealment were not reported. Four studies18,19,27,28 had low risk of performance bias and detection bias, as both participants and study personnel were masked, however, this risk was not clear in one study26 for failing to report who was blinded. All studies18,19,26,27,28 had low risk of attrition bias, as there was no loss to follow-up or they dealt with the missing data properly (e.g. applying intention-to-treat analysis which could underestimate the efficacy of the interventions). Four studies18,19,27,28 had low risk of reporting bias since they were registered in ClinicalTrials.gov and had reported all predesigned outcome, however, the other study26 did neither mention registration information nor have an available protocol, so it was unclear whether all the pre-designed outcomes in this study had been reported. Four studies18,19,27,28 were supported by pharmaceutical industry, the bias caused by conflict of interest was unclear.
Overall Platelet Response
The overall platelet response was reported in all studies (two18,19 for ELT and three26,27,28 for ROM) including 261 participants. The heterogeneity was not statistically significant (I2 = 26%, P = 0.24 and I2 = 0%, P = 0.55, respectively). The pooled results with a fixed-effect model (Table 4) showed that proportion of participants achieving overall response was significantly higher in the TPO-RAs group than in the placebo group (RR = 2.64, 95%CI: 1.58–4.44, P < 0.05 for ELT and RR = 5.05, 95%CI: 2.21–11.53, P < 0.05 for ROM). The result of indirect comparison (Fig. 3) indicated that the overall response between ELT and ROM was not significantly different (RR = 0.57, 95%CI: 0.21–1.56, P > 0.05).
Adverse events (AEs)
Four studies (197 participants)19,26,27,28 reported the overall incidence of any adverse events reported in participants receiving TPO-RAs or placebo. The pooled analysis (Table 4) showed that the incidence was not significantly different between two groups (RR = 0.97, 95%CI: 0.72–1.29, P > 0.05 for ELT and RR = 1.00, 95%CI: 0.69–1.45, P > 0.05 for ROM). And the result of indirect comparison (Fig. 4) also showed that the overall incidence of any AEs in ELT group was similar to that in ROM (RR = 0.96, 95%CI: 0.66–1.39, P > 0.05).
SAEs were reported in all studies18,19,26,27,28, and the results of both direct and indirect comparison (Table 4 and Fig. 3) indicated that the incidences of SAEs of ELT, ROM and placebo were not significantly different (ELT vs Placebo: RR = 0.70, 95%CI: 0.26–1.86, P > 0.05; ROM vs Placebo: RR = 3.28, 95%CI: 0.65–16.60, P > 0.05; ELT vs ROM: RR = 0.24, 95%CI: 0.03–1.65, P > 0.05; respectively).
The most common AEs in TPO-RAs and placebo were headache, vomiting, upper respiratory tract infection, pyrexia, cough, epistaxis, oropharyngeal pain, abdominal pain, and upper abdominal pain. However, the results of head-to-head comparison (Table 4) of the incidences demonstrated no significant difference between TPO-RAs and placebo, except that vomiting was less likely to occur in ELT than in placebo (RR = 0.31, 95%CI: 0.12-0.82, P < 0.05). According to the result of indirect comparison (Fig. 4), the incidences of these AEs in ELT were similar to that in ROM, except that cough was more frequent in ELT than in ROM (RR = 14.40, 95%CI: 1.21–171.13, P < 0.05).
Durable Platelet Response
Three studies (221 participants)18,27,28 reported durable platelet response. The direct and indirect comparison analyses (Table 4 and Fig. 3) showed that the proportion of participants achieving durable platelet response in TPO-RAs was significantly higher than placebo (RR = 13.14, 95%CI: 2.76–64.64, P < 0.05 for ELT and RR = 5.24, 95%CI: 1.36–20.13, P < 0.05 for ROM), while there was no significant difference between ELT and ROM (RR = 2.48, 95%CI: 0.31–19.97, P > 0.05).
Clinically significant bleeding
Four studies (242 participants)18,19,27,28 reported the incidence of clinically significant bleeding (grade 2~4). According to the direct comparison (Table 4), the incidence was significantly lower in participants receiving ELT than those receiving placebo (RR = 0.37, 95%CI: 0.15–0.93, P < 0.05), while the incidence was not significantly different between ROM and placebo (RR = 1.11, 95%CI: 0.78–1.58, P > 0.05). As to indirect comparison (Fig. 3), the incidence was significantly lower in ELT group than in ROM group (RR = 0.33, 95%CI: 0.12–0.89, P < 0.05).
All bleeding events
Four studies (242 participants)18,19,27,28 reported the incidence of all bleeding events (grade 1–4). The pooled results (Table 4) demonstrated that the incidence was significantly lower in ELT group compared with placebo group (RR = 0.50, 95%CI: 0.29–0.87, P < 0.05), while the incidence was not statistically different between ROM and placebo (RR = 1.22, 95%CI: 0.89–1.66, P > 0.05). According to the indirect comparison (Fig. 3), the incidence was significantly lower in ELT group than in ROM group (RR = 0.43, 95%CI: 0.23–0.80, P < 0.05).
Rescue treatment
All studies (261 participants)18,19,26,27,28 reported the proportion of participants receiving rescue treatment in TPO-RAs or placebo group. The results of both direct and indirect comparison (Table 4 and Fig. 3) indicated that the proportion was not significantly different between ELT, ROM and placebo. (ELT vs Placebo: RR = 0.46, 95%CI: 0.16–1.34, P > 0.05; ROM vs Placebo: RR = 0.70, 95%CI: 0.41–1.20, P > 0.05; ELT vs ROM: RR = 0.73, 95%CI: 0.20–2.73, P > 0.05; respectively).
Discussion
This is the first systematic review incorporating an indirect-comparison meta-analysis summarizing the evidence of efficacy and safety of TPO-RAs in children with persistent or chronic ITP. Our study suggests that the use of TPO-RAs may improve the durable and overall platelet response compared with placebo, while ELT resembles ROM in efficacy. It’s shown that ELT might be superior to ROM or placebo in reducing bleeding risk (including clinically significant bleeding). The incidences of AEs (including SAEs) of ELT, ROM and placebo were similar. Neither ELT nor ROM could reduce the need for rescue treatment.
A systematic review on the efficacy and safety of TPO-RAs in adults and children concluded that TPO-RAs were effective and safe second-line options for primary ITP patients20. According to its subgroup analysis for children, TPO-RAs could significantly improve platelet response (RR = 2.49, 95%CI: 1.46–4.23, P < 0.05) and durable response (RR = 7.64, 95%CI: 2.73–21.36, P < 0.05), without increasing the incidence of AEs (including SAEs) compared with placebo or standard care. Those findings are mostly consistent with the results of this review on children. However, our research indicated that ELT might reduce the risk of bleeding compared to ROM or placebo, and the TPO-RAs did not reduce the need for rescue treatment, which are inconsistent with previous study results. These differences might be caused by the different ways in pooling data: the previous study pooled the results from studies on ELT and ROM together, while our study conducted analysis on the two drugs separately.
An indirect comparison conducted in adult ITP patients demonstrated that ROM significantly improved overall platelet response compared to ELT, while the durable platelet response of the two TPO-RAs was similar25,29. Our research drew a different conclusion that ELT and ROM were similar in overall or durable platelet response for children with persistent or chronic ITP, probably due to population difference.
In addition, a multicenter retrospective study including 87 pediatric ITP patients (36 in ELT and 51 in ROM, respectively)17 found that the durable platelet response (RR = 1.00, 95%CI: 0.76–1.30, P > 0.05), overall platelet response (RR = 0.93, 95%CI: 0.77–1.13, P > 0.05), the incidence of AEs (RR = 2.83, 95%CI: 0.27–30.07, P > 0.05), and the proportion of patients receiving rescue treatment (RR = 0.89, 95%CI: 0.46–1.72, P > 0.05) were not significantly different between ELT and ROM, which are also consistent with the results of our study. Similar findings were also reported in other small sample observational studies30,31.
Nonetheless, an updated systematic review and meta-analysis of RCTs suggested that TPO-RAs were associated with higher risk of thromboembolic events compared with placebo or standard care32. And another meta-analysis of three large, population-based observational studies concluded that the risk of arterial and venous thromboembolism should be considered when evaluating the risk of thromboembolism attributed to ITP treatments (e.g. TPO-RAs)33. A disproportionality analysis in the World Health Organization global individual case safety report (ICSR) database (VigiBase) suggested the presence of a signal for an increased risk of thrombosis with ELT compared to ROM (adjusted reporting odds ratio = 1.72, 95%CI 1.47–2.02, P < 0.05)34. Although these AEs were not reported in the RCTs due to small sample size, physicians should be cautious when administering TPO-RAs to patients with higher risk of thromboembolism, especially for ELT.
In spite of increasing pharmacoeconomic studies revealing the advantage of ELT in cost-effectiveness for adult patients with ITP35,36,37, further studies are still needed to compare the benefits and cost of different TPO-RAs for pediatric persistent or chronic ITP to facilitate better clinical decision making.
There are several limitations in this study. As we only included RCTs in this review, the results may not have good generalizability for strict inclusion criteria and small sample size in those studies. These studies were also not sensitive enough to find rare AEs related to the drugs, as the sample size was relatively small. On the other hand, the results of indirect comparisons between ELT and ROM should be interpreted with caution because of low power of test and heterogeneity caused by different study designs, patient populations, and outcome definitions.
In summary, ELT and ROM might lead to similar overall and durable platelet response and incidence of adverse events in children with persistent or chronic ITP, but patients receiving ROM might have lower risk of bleeding compared to those receiving ROM. Cost of treatments, comorbidity and drug compliance should also be considered when making decisions in the management of pediatric persistent or chronic ITP with thrombopoietin-receptor agonists.
Methods
We followed the standard set by Preferred Reporting Items for Systematic reviews and Meta-Analyses (PRISMA) in this systematic review (Table 1). The study was registered in PROSPERO International Prospective Register of Systematic Review (PROSPERO 2017: CRD42017068657).
Searching
Pubmed, Embase, and Cochrane Central Register of Controlled Trials (CENTRAL) published in Cochran Library were searched using the search strategies detailed in Table S2, from their earliest records to May 2017. Clinical Trials.gov was searched using the terms “immune thrombocytopenia”, “children”, “eltrombopag”, and “romiplostim”. The China National Knowledge Infrastructure(CNKI) and Chinese Biomedical Literature Database(CBM) were also searched in Chinese.
Eligibility Criteria
All included studies met the following criteria: (1) randomized controlled studies; (2) participants were children <18 years with ITP lasting for 6 months or longer; (3) the intervention was ELT or ROM irrespective of dosage and schedule; (4) the comparison was placebo; (5) studies included at least one of the following outcomes: overall platelet response (primary outcome), defined as achieving at least once platelet response (50 × 109/L or more) during treatment; incidence of overall and serious adverse events (SAEs); durable platelet response, defined as achieving platelet counts of 50 × 109/L or more for 4 or more weeks; incidence of clinically significant bleeding (WHO Grade 2~4); all bleeding events; and the proportion of patients who received rescue treatment[e.g. receiving any unscheduled or new treatment (including new drugs, increase the dose of a concomitant drug from baseline, platelet transfusion or splenectomy) for immediate risk or treatment failure]; (6) publication written in English or Chinese. We excluded the patients with Evans syndrome or secondary ITP and the studies including both children and adults when children data could not be extracted separately.
Study Selection and Data Extraction
Two authors independently screened the titles and abstracts of all studies identified by the search strategies, and assessed the studies using predetermined inclusion criteria. The full texts of all potentially relevant articles were retrieved for detailed review. We resolved any disagreements by discussion until consensus was achieved. We used a pre-designed data collection form to extract data from each eligible study. The following data were extracted: (1) authors; (2) year of publication; (3) country or region where the study conducted; (4) study design and use of control; (5) number of participants randomized into each group; (6) gender, age, and disease duration of participants; (7) baseline platelet count, previous ITP medication, and splenectomy status; (8) dose and schedule of TPO-receptor agonists; (9) outcomes of each study and their definitions; (10) numerical data for assessment of included outcomes; (11) sources of funding.
Risk of Bias Assessment
Two authors independently assessed the risk of bias of each included study using the checklist developed by Cochrane Collaboration38. The items included random sequence generation, allocation concealment, blinding, incomplete outcome data, selective outcome reporting, and other bias. We categorized the judgments as low, high or unclear risk of bias and created plots of risk of bias assessment in Review Manager Software (RevMan 5.3).
Statistical Synthesis
We calculated a kappa statistic for measuring the agreement level between two authors making decisions on study selection. The value of kappa (K) between 0.40 and 0.59 was considered as fair agreement, between 0.60 and 0.74 as good and 0.75 or more as excellent.
If more than one study reported the same outcome, the pairwise meta-analysis was conducted to calculate the pooled estimate of the risk ratio (RR) of different TPO-RAs versus placebo by RevMan 5.3. Statistical heterogeneity among studies was examined by the Chi-square test and quantified by the I2 statistic39. We used a fixed-effect model to synthesize data when heterogeneity was not significant (P > 0.1 and I2 < 50%). When heterogeneity was significant (P ≤ 0.1 and I2 ≥ 50%) and could not be explained by subgroup analyses or in terms of clinical or methodological features of the trials, the random-effect model was used. If both the ELT-placebo and ROM-placebo trials reported the same outcome, the relative treatment effect (RR) for ELT versus ROM was estimated using indirect procedure of Stata12.0 software40, with the formula as follow:
The subgroup analysis was also conducted according to the different types of adverse events.
References
Rodeghiero, F. et al. Standardization of terminology, definitions and outcome criteria in an international working group immune thrombocytopenic purpura of adults and children: report from an international working group. Blood 113, 2386–2393 (2009).
Kurata, Y., Fujimura, K., Kuwana, M., Tomiyama, Y. & Murata, M. Epidemiology of primary immune thrombocytopenia in children and adults in Japan: a population-based study and literature review. Int J Hematol 93, 329–335 (2011).
Moulis, G. et al. Epidemiology of incident immune thrombocytopenia: a nationwide population-based study in France. Blood 124, 3308–3315 (2014).
Yong, M. et al. Epidemiology of paediatric immune thrombocytopenia in the General Practice Research Database. Br J Haematol 149, 855–864 (2010).
Lee, J. Y. et al. Epidemiology and management of primary immune thrombocytopenia: A nationwide population-based study in Korea. Thromb Res 155, 86–91 (2017).
Kühne, T. et al. A prospective comparative study of 2540 infants and children with newly diagnosed idiopathic thrombocytopenic purpura (ITP) from the Intercontinental Childhood ITP Study Group. J Pediatr 143(5), 605–608 (2013).
American Society of Hematology. Clinical practice guideline on the evaluation and management of immune thrombocytopenia(ITP). https://www.hematology.org/Clinicians/Guidelines-Quality/Quick-Ref/526.aspx (2011).
Neunert, C. et al. American Society of Hematology. The American Society of Hematology 2011 evidence-based practice guideline for immune thrombocytopenia. Blood 117, 4190–4207 (2011).
Provan, D. et al. International consensus report on the investigation and management of primary immune thrombocytopenia. Blood 115, 168–186 (2010).
Garzon, A. M. & Mitchell, W. B. Use of Thrombopoietin receptor agonists in childhood immune thrombocytopenia. Front Pediatr 3, 70 (2015).
U.S. Food & Drug Administration(FDA). FDA extends use of promacta in young children with rare blood disorder. http://www.fda.gov/NewsEvents/Newsroom/PressAnnouncements/ucm459430.htm (Accessed on September 09, 2015).
Bussel, J. B., Hsieh, L. & Buchanan, G. R. Long-Term Use of the thrombopoietin-mimetic romiplostim in children with severe chronic immune thrombocytopenia (ITP). Pediatr Blood Cancer 62, 208–213 (2015).
Mokhtar, G. M., Tantawy, A. A. & El Sherif, N. H. Romiplostim therapy in children with unresponsive chronic immune thrombocytopenia. Platelets 23, 264 (2012).
Vilaplana, V. E. et al. Use of romiplostim for primary immune thrombocytopenia in children. Pediatr Hematol Oncol 29, 197–205 (2012).
Pasquet, M. et al. Romiplostim in children with chronic immune thrombocytopenia (ITP): the French experience. Br J Haematol 164, 266–271 (2014).
Ramaswamy, K. et al. Thrombopoietic agents for the treatment of persistent and chronic immune thrombocytopenia in children. J Pediatr 165, 600–605 (2014).
Neunert, C., Despotovic, J., Haley, K. & Lambert, M. P. et al. Thrombopoietin Receptor Agonist Use in Children: Data From the Pediatric ITP Consortium of North America ICON2 Study. Pediatr Blood Cancer 63, 1407–1413 (2016).
Tarantino, M. D. et al. Romiplostim in children with immune thrombocytopenia: a phase 3, randomised, double-blind, placebo-controlled study. Lancet 388, 45–54 (2016).
Bussel, J. B. et al. A randomized, double-blind study of Romiplostim to determine its safety and efficacy in children with immune thrombocytopenia. Blood 118, 28–36 (2011).
Wang, L. et al. Efficacy and safety of thrombopoietin receptor agonists in patients with primary immune thrombocytopenia: a systematic review and meta-analysis. Sci Rep-UK 6, 39003 (2016).
Imbach, P. & Crowther, M. Thrombopoietin-receptor agonists for primary immune thrombocytopenia. N Engl J Med 365, 734–741 (2011).
Erhardt, J. A. et al. Comparative analyses of the small molecule thrombopoietin receptor agonist eltrombopag and thrombopoietin on in vitro platelet function. Exp Hematol 37, 1030–1037 (2009).
National Institute for Health and Clinical Excellence (NICE). Guide to the methods of technology appraisal. www.nice.org.uk/aboutnice/howwework/devnicetech/guidetothemethodsoftechnologyappraisal.jsp (2008).
Jansen, J. P. et al. Interpreting indirect treatment comparisons and network meta-analysis for health-care decision making: Report of the ISPOR Task Force on Indirect Treatment Comparisons Good Research Practices: Part 1. Value in Health 14, 417–428 (2011).
Cooper, K. L., Dillingham, K., Helme, K., Fitzgerald, P. & Akehurst, R. Romiplostim and eltrombopag for immune thrombocytopenia: methods for indirect comparison. Int J Technol Assess 28, 249–258 (2012).
Elalfy, M. S., Abdelmaksoud, A. A. & Eltonbary, K. Y. Romiplostim in children with chronic refractory ITP: randomized placebo controlled study. Ann Hematol 90, 1341–1344 (2011).
Grainger, J. D. et al. Eltrombopag for children with chronic immune thrombocytopenia (PETIT2): a randomised, multicentre, placebo-controlled trial. Lancet 386, 1649–1658 (2015).
Bussel, J. B. et al. Eltrombopag for the treatment of children with persistent and chronic immune thrombocytopenia (PETIT): a randomised, multicentre, placebo-controlled study. Lancet Haematol 2, e315–e325 (2015).
Cooper, K., Matcham, J., Helme, K. & Akehurst, R. Update on romiplostim and eltrombopag indirect comparison. Int J Technol Assess 30, 129–130 (2014).
Elena, V. S. et al. Bleeding tendency and platelet function during treatment with romiplostim in children with severe immune thrombocytopenic purpura. Int J Hematol 105, 841–848 (2017).
Leven, E. et al. Safe and effective use of romiplostim and eltrombopag in children with ITP. Blood 122, 3541–3541 (2013).
Catala-Lopez, F. et al. Risk of thromboembolism with thrombopoietin receptor agnonists in adult patients with thrombocytopenia: An updated systematic review and meta-analysis of randomized controlled trials. Medical Clinica 145, 511 (2015).
Langeberg, W. J., Schoonen, W. M., Eisen, M., Gamelin, L. & Stryker, S. Thromboembolism in patients with immune thrombocytopenia(ITP): a meta-analysis of observational studies. Int J Hematol 103, 655–664 (2016).
Thi-Thanh, L. N., Aurore, P., Francois, M., Maryse, L. M. & Guillaume, M. Signal for thrombosis with eltrombopag and romiplostim: a disproportionality analysis of spontaneous reports within Vigi Base. Drug Saf 38, 1179–1186 (2015).
Marzal, A. M. B., Marguinez, A. I., Escudero, V. V., Pernia, L. S. & Sanjurjo, S. M. Cost-minimization analysis of immune thrombocytopenia treatment with romiplostim and eltrombopag. Int J Clin Pharm-Net 35, 975–976 (2013).
Frolov, M., Pyadushkina, E. & Avxentyeva, M. Eltrombopag vs romiplostim in adult patients with chronic immune trombocytopenia: Economic evaluation. Value in Health 19, A583–A583 (2016).
Allen, R., Bryden, P., Grotzinger, K. M., Stapelkamp, C. & Woods, B. Cost-effectiveness of eltrombopag versus romiplostim for the treatment of chronic immune thrombocytopenia in England and Wales. Value in Health 19, 614–622 (2016).
Higgins, J. & Green, S. The Cochrane Collaboration.Cochrane handbook for systematic reviews of interventions version 5.1.0. http://handbook.cochrane.org/ (2011).
Higgins, J. P. & Thompson, S. G. Quantifying heterogeneity in a meta-analysis. Stat Med 21, 1539–1558 (2002).
Li, S., Zhang, C., Yuan, R. X., Xu, C. & Zeng, X. T. Brief introduction of indirect comparison software. Clin J Evid-based Med 15, 362–366 (2015).
Acknowledgements
We thank Prof. Jing Li and Prof. Deying Kang from the Chinese Cochrane Center in West China Hospital of Sichuan University for providing methodology and statistic support for this review.
Author information
Authors and Affiliations
Contributions
Jiaxing Zhang, Yi Liang and Youping Li performed the research. Jiaxing Zhang, Yi Liang, Youping Li, Yuan Ai, and Juan Xie designed the research study. Xiaosi Li, Wenyi Zheng and Rui He contributed essential reagents or tools. Jiaxing Zhang, Yi Liang, Yuan Ai, and Juan Xie analysed the data. Jiaxing Zhang, Yi Liang, Xiaosi Li, Wenyi Zheng, and Rui He wrote the paper. Conceived and designed the experiments: Youping Li; Jiaxing Zhang; Juan Xie.
Corresponding author
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Zhang, J., Liang, Y., Ai, Y. et al. Eltrombopag versus romiplostim in treatment of children with persistent or chronic immune thrombocytopenia: a systematic review incorporating an indirect-comparison meta-analysis. Sci Rep 8, 576 (2018). https://doi.org/10.1038/s41598-017-19099-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-017-19099-8
This article is cited by
-
Immune Thrombocytopenia in Children: Consensus and Controversies
The Indian Journal of Pediatrics (2020)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.